Ring around mouth
Perioral Dermatitis: Treatment, Symptoms & Causes
Overview
What is perioral (periorificial) dermatitis? What does it look like?
Perioral (periorificial) dermatitis is a red rash that circles your mouth. Your skin can be scaly, dry and flaky with swollen, inflamed bumps called papules. It is one of many types of dermatitis. Perioral dermatitis can look like acne and is often mistaken for it.
Some people report that perioral dermatitis itches or burns. Sometimes it spreads up to the nose and eyes and, very rarely, the genitals.
In the word perioral, “peri” means “around” and “oral” means “mouth.” The word literally means “around the mouth.” In the word periorificial, “orifical” means orifice or “an opening.” “Around an opening” is the meaning of periorificial. The two words refer to the same condition.
What are the types of perioral dermatitis?
There is typical perioral dermatitis, and then there is granulomatous perioral dermatitis. Granulomatous is not a type perioral dermatitis, but an irregular version of it. If you have granulomatous dermatitis then you’ll see yellowish bumps instead of red ones. Children are more prone to have granulomatous dermatitis than adults.
Where does perioral (periorificial) dermatitis most commonly occur?
Perioral dermatitis is easily recognizable by the location of the rash around your mouth. It can also go on your eyelids or around your eyes and nose. Rarely, it will appear on your genitals. Rarer still, it may move to the ears, neck, scalp, trunk and extremities.
Can perioral dermatitis become rosacea?
Perioral dermatitis can return after treatment. This happens even when it was successfully treated. Many cases that return can turn into rosacea, a skin condition that causes red papules in the middle of your face, including on your nose.
Who is at risk of getting perioral dermatitis?
You’re most at risk if you’re a woman between 25 and 45 who uses topical steroids, face creams and more (see the Causes section). However, children and men can develop perioral dermatitis, too.
However, children and men can develop perioral dermatitis, too.
Is perioral dermatitis contagious?
No. No type of dermatitis is contagious. It can’t be spread to another person.
Is perioral dermatitis a fungal infection?
Overuse of topical steroids is the most likely cause of perioral dermatitis. However, there are a number of theories and the exact cause is yet to be determined. One theory is that perioral dermatitis is caused by candida albicans. Candida albicans is a yeast, which is a type of fungus.
Is perioral dermatitis (periorificial) a bacterial infection?
The exact cause of perioral dermatitis is unknown, but there are many theories. One theory is that this skin condition is caused by follicular fusiform, a type of bacteria.
Symptoms and Causes
What causes perioral dermatitis?
The exact cause is to be determined, but experts have noted 13 possible causes of perioral dermatitis:
Steroids:
- Topical steroid creams.

- Inhaled prescription steroid sprays.
Lifestyle choices:
- Moisturizers and heavy face creams.
- Fluorinated toothpaste.
- Gum chewing.
- Dental fillings.
Other:
- Hormonal changes (or oral contraceptives).
- Dysfunction of the epidermal barrier.
- Problems with the immune system.
- Altered cutaneous microflora.
- Bacteria – follicular fusiform.
- Candida albicans.
- Demodex mites.
What are the symptoms of perioral dermatitis?
The primary symptom of perioral dermatitis is a red rash around your mouth. The rash may be scaly or dry and flaky. Often there are inflamed bumps that are called papules. Additionally, you may develop vesicles (clear fluid-filled bumps) or pustules (white fluid-filled bumps). Although it is usually found around the mouth, perioral dermatitis can also move to your eyelids, or around your eyes and nose. It can also appear on your genitals, scalp, ears, neck, extremities and trunk.
The rash can cause an itching or burning sensation.
Some people experience conjunctivitis (pink eye) when they have perioral dermatitis. If you have pink eye then your healthcare provider may refer you to an eye doctor (an ophthalmologist).
Can perioral dermatitis be caused by stress?
Yes. Stress can sometimes cause some types of dermatitis.
Does perioral dermatitis hurt?
Sometimes it itches, and sometimes it burns. This is not true for all people.
What aggravates perioral dermatitis?
Triggers for perioral dermatitis may differ for different people. If you continue doing what is causing your personal perioral dermatitis (using topical steroids, etc.) then your condition may worsen.
Do certain foods worsen or improve perioral (periorificial) dermatitis?
No food or drink is known to cause or worsen perioral dermatitis. However, in some cases, chewing gum has been linked to the rash. Work with your healthcare provider to figure out the cause of your perioral dermatitis so that you can avoid that cause in the future – if possible.
Is perioral dermatitis permanent?
Perioral dermatitis may be permanent if you don’t get treatment. Most cases eventually resolve, but this can take weeks to years. If you do get treatment, your symptoms and rash are likely to go away much sooner. However, there is no known reproducible cure for perioral dermatitis. (It might return.)
Diagnosis and Tests
How is perioral dermatitis diagnosed? What tests are done?
A visual examination by your healthcare provider is usually all you’ll need for a diagnosis of perioral dermatitis. Once in a while a skin biopsy is taken to distinguish perioral from other types of dermatitis such as atopic dermatitis (eczema) and contact dermatitis.
What questions might my healthcare provider ask to diagnose perioral (periorificial) dermatiti
s?- Is there a rash somewhere other than your face?
- How long have you had the rash?
- Do you use topical steroids?
- Does your rash itch?
- Does your rash burn?
- Do you have any other types of dermatitis or other skin conditions?
- Do you see a dermatologist?
Management and Treatment
How is perioral dermatitis treated? What medicines help?
First, you must stop using any products that might be causing your perioral dermatitis. Stop the following:
Stop the following:
- Topical and inhaled steroids. This includes both over-the-counter and prescribed steroids. If your healthcare provider has prescribed a steroid, ask if you can switch to a different medication.
- Face creams, including moisturizers.
- Cosmetics (makeup).
- Sunscreen.
- Fluorinated toothpaste (toothpaste without fluoride can be found at health food stores).
- Chewing gum.
Your perioral dermatitis might flare up after you stop a topical steroid. Some experts recommend going back on a topical steroid that is not as strong as what you may be using. Discuss this with your healthcare provider. Your perioral dermatitis may get worse before it gets better.
There are several medications that can help your perioral dermatitis. Unfortunately, these medications may not fix the problem for weeks or months. Your healthcare provider may recommend one or more of the following:
Topical (applied to the skin) medications:
- Erythromycin gel.

- Clindamycin lotion or gel.
- Metronidazole cream or gel.
- Pimecrolimus.
- Azelaic acid.
- Sulfur preparations.
- Tacrolimus ointment.
- Pimecrolimus.
- Adapalene.
- Photodynamic therapy using a 5-aminolevulinic acid as a photosensitizer.
Sometimes oral antibiotics are prescribed. They help with inflammation. Oftentimes, topical medications are used at the same time as the antibiotics.
Oral (by mouth) antibiotic medications:
- Tetracycline.
- Doxycycline.
- Minocycline.
- Oral erythromycin. (For preadolescents and pregnant women.)
- Oral low-dose isotretinoin.
Is there a cure for perioral dermatitis?
Perioral dermatitis may be with you for months or even years. There is no cure, but long-term remissions are possible. Sometimes the rash disappears, then reappears. The same treatments that worked the first time are likely to work again.
Are there complications/side effects of treatment?
Your rash might get worse after you stop using a topical steroid. This is normal. Don’t resume using it unless your healthcare provider tells you to do this. The flare-up will fade with time.
Should I see a dermatologist?
You might need the help of a dermatologist if your rash doesn’t disappear after you’ve stopped topical steroids.
How soon after treatment will my symptoms improve?
It may take days, weeks, or months for your symptoms to go away.
Prevention
How can I reduce my risk of perioral (periorificial) dermatitis?
Avoid topical steroids and face creams. See your healthcare provider as soon as possible after you notice symptoms of a rash around your mouth, especially if the rash causes itchiness and burning.
After the rash is gone, only use a mild soap (fragrance-free) or soap substitute when you wash. Don’t go back to using products you used before the rash.
What medicines can I take to possibly prevent perioral dermatitis?
There are no known medicines that can prevent perioral dermatitis, but there are some that can cause it. Topical steroids are the most likely cause of the rash.
What foods can I eat or avoid to reduce my risk of perioral dermatitis?
At this time there are no known foods that can help your perioral dermatitis, or worsen it.
Outlook / Prognosis
What can I expect if I’ve been diagnosed with perioral dermatitis?
Expect that you’ll have to abide by a treatment plan worked out with your healthcare provider. Every treatment plan is different. You might need topical medications or oral medications, or you might simply need to stop doing what’s causing the rash (such as stop taking topical steroids). However, most of the time a treatment regimen that effectively controls the perioral dermatitis can be found.
Remember — your perioral dermatitis will get worse before it gets better when you stop taking topical steroids. This is normal, and expected.
This is normal, and expected.
How long will I have perioral (periorificial) dermatitis?
Perioral dermatitis may stay with you for months or even years.
Can perioral dermatitis go away on its own?
This can happen. If you stop all steroids, you might find that the rash and symptoms disappear.
Can perioral dermatitis get worse?
Yes, perioral dermatitis can get worse if you do not follow your healthcare provider’s treatment plan.
Living With
How do I take care of myself?
Once your rash clears, don’t go back to using the steroids, face creams, or other products that possibly caused it.
When you have the rash, just wash with warm water. Don’t use soap until after it’s gone.
Listen to your healthcare provider’s instructions.
When should I see my healthcare provider?
See your healthcare provider as soon as you see a rash or have symptoms of perioral dermatitis. You’ll want to get treatment before the rash and/or symptoms become severe.
What questions should I ask my healthcare provider about perioral (periorificial) dermatitis?
- Why do I have perioral dermatitis?
- Do I have perioral dermatitis or another type of dermatitis?
- Do you think this will go away on its own, or do I need treatment?
- What medications should I stop taking?
- What over-the-counter products should I stop using?
- Do I need to see a dermatologist?
- Are there any other specialists I should see?
- What treatment would be best?
A note from Cleveland Clinic
There are many types of dermatitis. Some have an obvious cause while others, like perioral dermatitis, are unclear. It can be frustrating to have a rash and not know for sure where it comes from. Although topical steroids is thought to be the most likely cause, there are a variety of other theories. Work with your healthcare provider to narrow down what the cause might be. This will help you and your healthcare provider determine a treatment plan.
Perioral dermatitis is common, and there are effective treatments. Don’t hesitate to ask questions, follow your healthcare provider’s instructions and remember that your rash might get worse before it gets better.
Perioral dermatitis: Causes, symptoms, treatment, prevention
Perioral dermatitis is a skin condition that causes a rash around the mouth. The rash may also occur around the eyes, nose, or genitals, but this is much less common.
A note about sex and gender
Sex and gender exist on spectrums. This article will use the terms “male,” “female,” or both to refer to sex assigned at birth. Click here to learn more.
Dermatitis refers to an inflammation of the skin, while perioral means around the mouth.
Perioral dermatitis is most common in females between the ages of 20 and 45 years. Older adults, males, and children can also have the condition, but it happens less frequently.
Perioral dermatitis belongs to the broader category of periorificial dermatitis, which can affect the skin predominantly around the eyes, the nostrils, the mouth, and occasionally the genitals.
However, when medical professionals discuss the condition affecting specifically the skin around the mouth, they use the term perioral dermatitis.
In most cases, perioral dermatitis affects young adults and adult females up to the age of 45. But when it affects children, health experts call it childhood perioral dermatitis.
Lupoid perioral dermatitis is a more severe version that results in a person developing denser groupings of bumps that can be red and brown on both light and darker skin tones.
Another related type of condition is granulomatous periorificial dermatitis. While it primarily occurs in children with darker skin tones, it can also present in children with light skin tones. It usually appears as flesh-colored, yellow-brown papules.
Perioral dermatitis is a rash that develops around the mouth and tends to be bumpy or scaly.
These bumps generally do not affect the skin right next to the mouth but appear a short distance away from the lips. They may also form a ring around the mouth.
They may also form a ring around the mouth.
Sometimes the rash can appear around the nose or eyes. It can occasionally appear around the genitals too, but this is rare.
What does it look and feel like?
Some people with perioral dermatitis may only get a few bumps, and their rash may not be very discernible. Others may have many lumps forming a noticeable rash.
The bumps may be skin colored or hyperpigmented and may appear red or pink in people with fair skin. Although they might resemble pimples, the bumps are not the same as acne. The rash may look inflamed, with the underlying and surrounding skin appearing red, pink, or flesh toned.
The rash may be itchy or non-itchy, but it does not usually hurt. Some people with perioral dermatitis may feel tightness or mild burning in the affected skin, which may be dry or flaky.
Granulomatous periorificial dermatitis is more common in darker-skinned people, who may experience less evident skin flushing and color changes. This condition has associations with burning, so individuals with darker skin may experience this symptom more frequently.
This condition has associations with burning, so individuals with darker skin may experience this symptom more frequently.
Share on PinterestPerioral dermatitis is a common facial skin problem.
Photo by DermNet New Zealand
Share on PinterestIt presents as tiny red papules around the mouth and chin.
Photo by DermNet New Zealand
Share on PinterestThe condition is commonly treated with facial ointments and creams.
Photo by DermNet New Zealand
Share on PinterestThe skin is usually dry and itchy, with the papules presenting in clusters.
Miroslav Lukic/Shutterstock
Share on PinterestThe condition can be caused by many things, including creams, soaps, and other external exposures.
© 2021, Diehl et al/NCBI
Share on PinterestHealing time varies for each individual but usually takes 2–4 weeks.
The Korean Dermatological Association and The Korean Society for Investigative Dermatology/NBCI
There is no underlying condition that causes perioral dermatitis, and it is not contagious.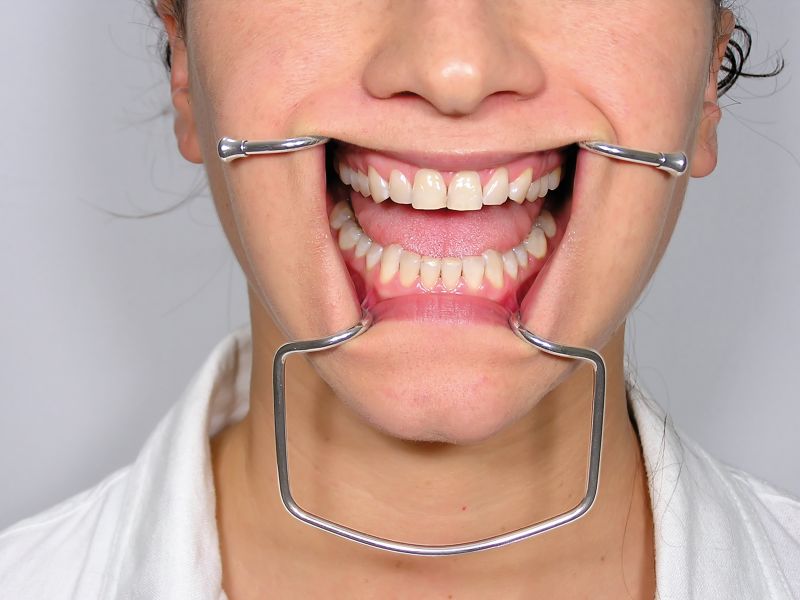 Although the exact cause is unknown, researchers think it may relate to the use of topical corticosteroids.
Although the exact cause is unknown, researchers think it may relate to the use of topical corticosteroids.
Topical corticosteroids are steroid ointments, creams, or gels that people use to treat skin conditions. However, individuals should only ever use topical corticosteroids as a short-term treatment, and most of them are not suitable for applying on the face. Sometimes, a person uses corticosteroids for longer than they should or use them on their face. This can result in skin damage.
A 2021 study showed that topical corticosteroids may have a link to a variety of skin conditions, including perioral dermatitis. Research from 2017 that explored the effects of the misuse of topical corticosteroids on facial skin also showed that perioral dermatitis was one of the adverse effects.
Additional possible causes of perioral dermatitis may include:
- a problem with the skin’s protective barrier
- a change in the bacteria on the skin
- bacteria getting into the hair follicles
- an allergic reaction
- irritation resulting from a skin care product or fluorinated toothpaste
- hormonal changes
- strong winds
- UV light
- in children:
- lip licking and chewing
- thumb sucking
- drooling
- chewing gum
- inhaling nasal steroids
More research is necessary to understand the exact causes of perioral dermatitis, but using heavily-scented toiletries or skin care products or wearing heavy makeup can trigger the condition.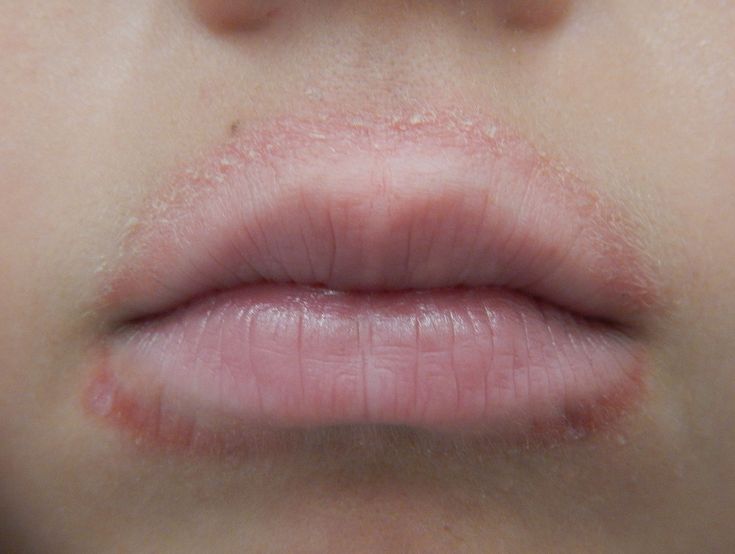
Other possible risk factors can include young age, being female, hormonal imbalance, topical steroid use, and a history of allergies.
Symptomatically, periorificial dermatitis and its subcondition perioral dermatitis can appear quite similar to rosacea. Both cause red bumps, which may also appear yellowish-brown on darker skin colors, around the nose, mouth, and central area of the face, as well as scaling or peeling skin. Both conditions can also cause a sensation of burning.
However, the causes of the conditions are different. Rosacea is a chronic inflammatory condition. Its exact cause is unknown, but experts believe it has links to genetics, immune reaction, microorganisms, environmental factors, and neurovascular dysregulation.
People with rosacea often have more prominent blood vessels, which can lead to flushing easily. In contrast, perioral dermatitis is a rash that occurs primarily due to using topical corticosteroids, cosmetics, skin care products, fluorinated toothpaste, or other oral care products.
However, because of the similarities in symptoms, some researchers consider periorificial and perioral dermatitis a variant of rosacea.
As topical corticosteroids seem to be a primary risk factor for perioral dermatitis, it is essential to stop using them on the skin. This includes hydrocortisone.
If a doctor has prescribed corticosteroids, it is best to explore alternatives, as continuing to use them could cause the rash to worsen.
When a person stops using corticosteroids, their rash may worsen before it improves. A dermatologist may offer someone specific medications to help ease inflammation during this time.
Medical treatments for perioral dermatitis
The first medications a doctor may prescribe include:
- metronidazole cream or gel
- clindamycin lotion or gel
- erythromycin gel
- topical sulfur ointment
- azelaic acid gel
It is important to consult a dermatologist if the rash does not get better on its own. The dermatologist may also prescribe oral or topical antibiotics or a cream that suppresses the immune response.
Natural treatments for perioral dermatitis
The following home remedies and lifestyle changes may help manage symptoms:
- avoiding topical steroids
- washing the face with warm water alone
- using fragrance-free skin care products
- avoiding the sun
- avoiding fluorinated toothpaste
A 2018 study notes that coconut oil is a safe and effective skin moisturizer. Research suggests that it can benefit the skin by:
- reducing inflammation
- fighting bacteria
- promoting wound healing
- repairing the skin barrier
Due to these properties, coconut oil may help perioral dermatitis. However, some people may find that it can clog their skin pores. Researchers also need to carry out more studies into its effectiveness as a treatment for this skin condition.
Are there any side effects or complications of treatment?
Without treatment, a person can develop significant facial scarring from perioral dermatitis. This is more likely to occur if they have the more severe lupoid form of the condition.
The medications that a doctor may prescribe to treat the conditions can potentially cause skin irritation or an allergic reaction. A severe reaction can include anaphylaxis, a life threatening condition.
They may also cause skin dryness, burning, itching, or hypopigmentation. Using the topical drug Metronidazole may increase the risk of cancer and antibiotic resistance, so a person should use it only under guidance from a doctor.
Is there a perioral dermatitis cure?
There is no cure for perioral dermatitis, but many home remedies that can help relieve perioral dermatitis may also help prevent it.
First, people should only use topical steroids as a doctor advises. A person should limit using heavy makeup and fluorinated oral care products and choose fragrance-free, oral care, soap, and other skin care products suitable for sensitive skin.
Avoiding the sun and strong winds may also promote skin health.
If someone has perioral dermatitis that does not go away when they stop using topical steroids, they should speak with their doctor.
They may receive a referral to consult a dermatologist, a specialist in skin conditions. They can recommend the best course of treatment. And if a person has Medicare, they likely will not need a referral in most cases.
Some private health insurance companies, and especially Health Maintenance Organization plans, may require a referral or prior authorization before the visit.
How to prepare
A doctor will usually be able to diagnose perioral dermatitis according to the symptoms. They may ask a person questions about their lifestyle to determine the cause and differentiate the diagnosis from rosacea.
They will likely ask if an individual has been using corticosteroids or any fragrance- or fluoride-based products. A person may wish to bring information on their skin and oral care routine and any medications they are taking.
Medication side effects
If a person is already taking medications for perioral dermatitis, and their symptoms do not improve or get worse, they may be reacting to the medication. They should revisit their dermatologist for another evaluation to see if a change in treatment is necessary.
If a person experiences symptoms of a serious allergy or anaphylaxis after using topical medications, they should call 911 and get medical treatment immediately as this is a life threatening condition.
Anaphylaxis is a severe allergic reaction that can be life threatening. The symptoms develop suddenly and include:
- hives
- swelling of the face or mouth
- wheezing
- fast, shallow breathing
- a fast heart rate
- clammy skin
- anxiety or confusion
- dizziness
- vomiting
- blue or white lips
- fainting or loss of consciousness
If someone has these symptoms:
- Check whether they are carrying an epinephrine pen.
 If they are, follow the instructions on the side of the pen to use it.
If they are, follow the instructions on the side of the pen to use it. - Dial 911 or the number of the nearest emergency department.
- Lay the person down from a standing position. If they have vomited, turn them onto their side.
- Stay with them until the emergency services arrive.
Some people may need more than one epinephrine injection. If the symptoms do not improve in 5–15 minutes, or they come back, use a second pen if the person has one.
Perioral dermatitis often clears up on its own a few weeks after a person stops using topical steroids, but medical treatment may still be necessary. Using fragrance-free products helps avoid irritating the skin while it heals.
As a doctor examines the healing skin, they should begin to see less inflammation and decreased redness, skin bumps, and scaling. Other symptoms should also gradually decrease.
This skin condition may flare up if a person starts using topical steroids again. Flares can also occur with other triggering agents, such as fluorinated toothpaste or heavy, scented cosmetics. It is best to discuss alternative options with a doctor.
It is best to discuss alternative options with a doctor.
Yellow ring around the mouth - what is it?
Yellow ring around …
Wisdom of the forum: Women's health
-
If you removed the uterus
69 212 answers
-
Blood under sexual intercourse
255 answers
-
How to postpone menstruation for 3-4 days?
624 responses
-
Water leaking from the vagina
284 answers
-
Stomach pain like menstruation.
2,015 responses
-
Menstruation twice a month
500 responses
-
Are pieces of meat during menstruation or miscarriage?
577 answers
-
Pimple or bump on inner labia
750 answers
-
How to get rid of the vaginal smell
974 Reply
-
Strong abdominal stomach during the monthly
583 Reply
-
Small lam
Pieces of mucus from the vagina between periods
43 answers
24 answers
Last - Removing
#1
#2
Guest
Author YOU KITH KIRITH?
usually from smoking.
#3
#4
5
#5
#6
#7
#8
Guest
This is carrots
#9
Guest
Do you like scrambled eggs?
#10
#11
20 20 210006
#12
#13
#14
#15 #15
#16
#17
9000 #18
Gost
222 Your text is what kind of carrot?
#18
#18
Ira
+
usually from smoking. #19
#19
#20
Woman.ru experts
-
Rich Vyacheslav
Certified practitioner...
234 answers
-
Maxim Sorokin
Practicing psychologist
604 answers
-
Julia Lekomtseva
Cosmetologist
243 answers
-
Egor Mazurok
Clinical psychologist
11 answers
-
Alla Buraya
Psychologist
33 answers
-
Nidelko Lyubov Petrovna
Practicing psychologist
219 answers
-
Dotsenko Vsevolod
Psychologist
175 answers
-
Daria Gorbunova
Practicing psychologist
134 answers
-
Novikova Olga Dmitrievna
Practicing psychologist in.
 ..
.. 10 answers
-
Nina Babanakova
Nutritionist, consultant on...
78 answers
#21
Person
I have the same problem, yellowness around the mouth and stickiness of the lips, I went to the dermatologist, he diagnosed seboric dermatitis, but the treatment did not help, and by the way I love scrambled eggs and after it there is a strong itch, and almost no I eat chocolate, etc.
#24
#25,0003
attention
No answers
Vaginal pain after surgery
No answers
pain in the Prima Nadovs.
 Who had it?
Who had it? 8 answers
Who wears glasses?
4 answers
Thrush. Nothing helps
10 answers
I have mycoplasma and HPV, my boyfriend doesn't. Is it possible?
2 answers
Search for ovulation
3 answers
How to refuse contraceptives
2 Answer
Unexpected Vitamin D
9000 9000 7.Pharmaceutical decoction or collection
3 answers
Popular topics for the day:
-
Who treated hemorrhoids
18 answers
-
Metroal bowl
15 answers
-
can be acne in 36?
13 answers
-
female consultation
11 answers
-
0014
11 answers
-
Who has taken hormone tests can this be done for free?
10 answers
-
Thrush.
 Nothing helps
Nothing helps 10 answers
-
Who made the Visual Laser Correction
9 answers
-
Regarding menstruation
9 Responses
-
The preparation for pain in the shin and spin
9 answers
Editor's choice
-
Is it possible to take a bath with burning in the veins?
20 answers
Next topic
-
Clostilbegit and Side effects!!!
37 answers
0018
Perioral dermatitis - BIOSPHERE - Beauty Industry Experts
04/08/2020
“Recently I noticed that a few small red pimples formed on my chin - I began to use the
acne cream and wash my face more often, but this only made it worse. Within a few weeks, the skin around the mouth and on the chin became just red, and acne kept appearing
and appearing, the skin began to peel off and become covered with crusts, "- if you heard something like this from your client, most likely we are talking about perioral dermatitis.
Signs and causes of appearance
Perioral dermatitis is an inflammatory skin disease characterized by the appearance of erythema (redness), against which small papular or papulo-vesicular rashes and peeling appear. Typical localization - the area around the mouth, chin, less often - the periorbital region. A characteristic sign of dermatitis is the presence of intact skin in the immediate vicinity of the red border of the lips. Sometimes rashes are accompanied by a burning sensation, tightness, soreness. More common in women
aged 20-40.
Perioral dermatitis must be differentiated from the following diseases:
1. Rosacea . With rosacea, the process develops gradually: at first, hyperemia appears, then papules, pustules, etc. Perioral dermatitis develops quickly and has no staging. The presence of telangiectasias is characteristic only for rosacea.
2. Seborrheic dermatitis . Rashes are more often localized on the scalp, the border of hair growth, eyebrows, eyelashes, the mustache and beard area, nasolabial folds, the skin of the external auditory canals and behind the ear areas and are accompanied by the appearance of shiny, greasy yellowish scales. The feeling of itching is characteristic. It occurs more often in men.
The feeling of itching is characteristic. It occurs more often in men.
3. Acne (acne) . Erythema is usually absent. The skin of the face is oily, with a large number of comedones and conical papules. It often occurs at a younger age.
4. Contact dermatitis . There is a connection between the onset of the disease and exposure to irritants and allergens. The main difference is a pronounced itching, not characteristic of perioral dermatitis.
Factors contributing to the development of perioral dermatitis:
- Uncontrolled use of glucocorticoids (creams, ointments and other products)
- Regular use of dense decorative cosmetics and cosmetic products
with an occlusive effect
- Excessive sun exposure
including the use of contraceptives), diseases of the gastrointestinal tract – Carrying out aggressive cosmetic procedures (peelings, laser resurfacing, etc.)
without proper preparation and rehabilitation
- Decreased immunity, increased sensitivity to bacterial agents (mites of the genus Demodex, fungi of the genus Candida)
Treatment, correction and prevention
When prescribing treatment, it is necessary to take into account the severity of the disease.