Normal vaginal ultrasound
Transvaginal Ultrasound | Cedars-Sinai
Ultrasound is a safe and painless procedure that uses sound waves to "see" inside your body and create detailed images which the physician can study. At the Cedars-Sinai S. Mark Taper Foundation Imaging Center, we have an expert team of physicians, nurses and technologists who are highly trained in ultrasound imaging.
- Why choose the S. Mark Taper Foundation Imaging Center for an ultrasound?
- Directions and parking information
Before Your Exam
- This exam can be performed during menstruation. If you are menstruating and wearing a tampon, you will need to remove the tampon before the test.
- Drink 32 ounces of any liquid one hour before your examination time. Try to drink all the liquid within 30 minutes.
- Do not urinate before the exam. Arrive for your exam with a full bladder.
- If your doctor gave you an order, please bring it with you.
- We want to make your waiting time as pleasant as possible. Please consider bringing your favorite magazine, book or music player to help you pass any time you have to wait.
- Although there are lockers with locks for your use, we recommend that you leave your jewelry and valuables at home.
During Your Exam
- Upon arrival, you will be asked to change into a hospital gown.
- Once in the examination room, the diagnostic medical sonographer will explain your procedure and answer any questions you may have.
- You will be positioned on your back on the exam table, with your legs raised — just like for a pelvic exam.
- A small, lubricated probe, called a transducer, will be inserted into your vagina. The transducer is inserted like a tampon. The transducer is larger than a tampon, but smaller than the speculum that your doctor uses for a pelvic exam.
- During the exam you will feel a light amount of pressure.
 You may be requested to lie still, change positions, hold your breath or just breathe normally.
You may be requested to lie still, change positions, hold your breath or just breathe normally. - Sound waves will pass harmlessly through the skin from the transducer. The sound waves bounce off certain organs and tissue in the body. This creates "echoes." The echoes are reflected back to the transducer. A television monitor shows images as the transducer converts the echoes to electrical signals. These moving images may be viewed immediately, recorded and/or photographed for physician review.
- Occasionally the radiologist may request additional images.
- Your procedure will take approximately 30 to 60 minutes.
After Your Exam
Your study will be reviewed by a imaging physician and the results sent to your doctor. Your doctor will discuss these results with you and explain what they mean in relation to your health.
If you have problems related to your procedure, please call 310-423-8000.
To request a copy of your images on a CD or film, or a copy of your report, please call 310-423-8000, option 2 or submit an online request.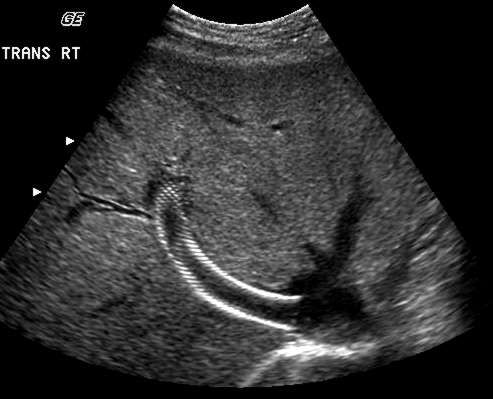
For more information or to schedule an appointment, please call 310-423-8000.
If you have uterine fibroids, call 310-423-2468 today for a consult about uterine fibroid embolization, a minimally invasive treatment for uterine fibroids.
Transvaginal Ultrasound Images
Conventional ultrasound images of the pelvis and ovary structures.
Transvaginal ultrasound images showing the pelvis and ovary structures with far greater clarity. The colored areas show blood flow.
A transvaginal ultrasound showing the heartbeat of a fetus early in a pregnancy. The lines at the bottom are called M Mode, which is how imaging specialists detect and document heart motion.
An adnexal mass in the pelvis shown with traditional ultrasound. Below right: an adnexal mass shown more clearly with a transvaginal ultrasound.
The S. Mark Taper Foundation Imaging Center provides a full range of advanced imaging, both radiology and cardiology, as well as interventional radiology and interventional tumor (oncology) treatments to the greater Los Angeles area, including Beverly Hills, Encino, Mid-Cities, Santa Monica, Sherman Oaks, Silver Lake, Studio City, Toluca Lake and West Hollywood.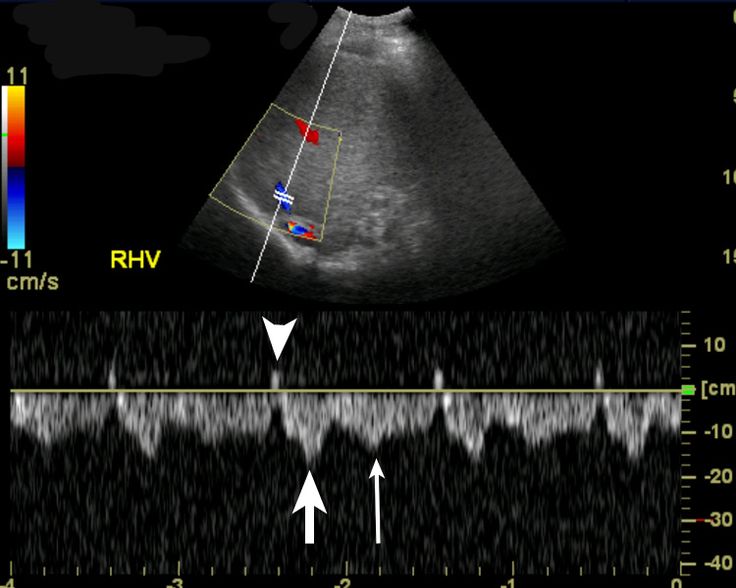
Sonography Transvaginal Assessment, Protocols, And Interpretation - StatPearls
Continuing Education Activity
A transvaginal ultrasound offers an invaluable avenue of imaging of the female pelvic anatomy. It augments transabdominal ultrasound for a more complete evaluation of the ovaries, adnexa, uterus, cervix, and surrounding pelvic regions. Typically, an ultrasound technician will conduct the scanning and take images of the normal structures, with more dedicated images or cine clips obtained of aberrant anatomy, pathologic processes, or pregnancy. The images are read by a radiologist, guiding the treatment by an interprofessional team.
Objectives:
Review the purpose of the transvaginal ultrasound.
Explain how to perform the endovaginal ultrasound.
Outline the utilities and limitations of the transvaginal ultrasound.
Describe the basics of interpreting an endovaginal ultrasound by an interprofessional team.

Access free multiple choice questions on this topic.
Introduction
Transvaginal ultrasound imaging of the female pelvic organs is unique in its ability to closely visualize the organs that would otherwise be difficult to see on transabdominal ultrasound. Additionally, unlike computer tomography (CT), this is a more up-close imaging modality without the utilization of ionizing radiation. There are many indications for this, both diagnostic and interventional. An ultrasound technician first conducts a transabdominal scan for a thorough exam and follows it with a transvaginal ultrasonographic exam. Images are uploaded to a picture archiving and communication system or PACS system for the radiologist to interpret.
Adnexal/ovarian masses and cysts, endometrial pathologies, fibroids, pregnancy (ectopic and intrauterine) as well as evaluation of developmental anomalies are a non-exhaustive list of indications that are ideally evaluated with ultrasound.
Anatomy and Physiology
The ability to properly evaluate the female pelvis sonographically requires proficiency in anatomy. An ultrasonographer will always position the probe so that a marker that propagates on every image consistently indicates cephalad on sagittal imaging and right side on transverse imaging. Beginning externally, the introitus gives way to the vaginal canal, which ends at the cervix. The cervix has two portions: the ectocervix, which protrudes out into the vagina, and the supravaginal portion connects with the uterus.[1]
The endocervical canal connects the vagina and uterine cavity. Circumferentially to the cervix, the fornices are invaginations of the mucosa. A transvaginal ultrasound probe may be placed anteriorly, posteriorly, or on either side of the cervix by placement within the fornix. The posterior fornix creates the inferior border of the Pouch of Douglas, while the anterior fornix borders the vesicouterine pouch inferiorly.
The external os of the cervix gives rise to the endocervical canal and terminates at the internal cervical os.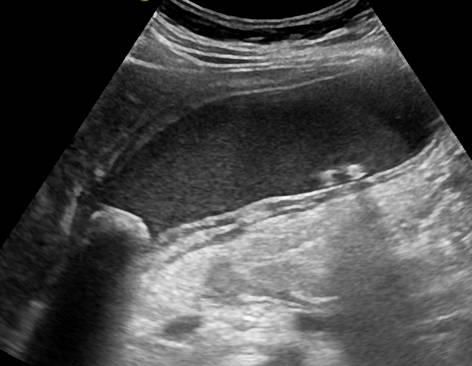 This marks the entrance to the uterus. The fallopian tubes are located on either side of the uterus and are composed of three regions. The portion of the fallopian tube closest to the uterus is called the isthmus, followed by the ampullary segment and then the infundibulum. On the ends of the infundibulum, there are finger-like projections called fimbriae that move like cilia and are responsible for drawing an ovulated ovum into the fallopian tubes. The junction between the uterus and the fallopian tube is termed the cornu.[2]
This marks the entrance to the uterus. The fallopian tubes are located on either side of the uterus and are composed of three regions. The portion of the fallopian tube closest to the uterus is called the isthmus, followed by the ampullary segment and then the infundibulum. On the ends of the infundibulum, there are finger-like projections called fimbriae that move like cilia and are responsible for drawing an ovulated ovum into the fallopian tubes. The junction between the uterus and the fallopian tube is termed the cornu.[2]
The ovary is suspended to the pelvic sidewall by the infundibulopelvic ligament (suspensory ligament of the ovary), containing the ovarian vessels.[2] The utero-ovarian ligament extends from the uterus to the ovaries and carries a blood supply from the uterine artery.[3]
Indications
Indications for ultrasonographic evaluation of the female pelvis includes, but is not limited to the following:[4]
Evaluation of pregnancy
Fetal evaluation
Intrauterine
Ectopic
Abortive process
Infertility
Abnormal uterine bleeding
Amenorrhea
Dysmenorrhea
Menorrhagia
Metrorrhagia
Incontinence
Presence of pelvic mass
Presence of infection
Evaluation of anomalous anatomy
Aid in performing an interventional procedure
Other non-gynecologic entities may be evaluated as well as listed below:[5]
Bladder:
Neoplasms
Calculi
Fistulas
Cystitis
Urethra:
Small bowel
Rectosigmoid colon
Pelvic vasculature
Adhesions
Contraindications
Contraindications to the transvaginal ultrasound are the following[4]:
Rupture of membranes in a pregnant patient, as they are at an increased risk of chorioamnionitis
Imperforated hymen
Vaginal obstruction
Woman with no history of vaginal intercourse
Recent vaginal surgery
Lack of patient's consent
Contraindications in pregnant women are premature rupture of membranes and bleeding from placenta previa.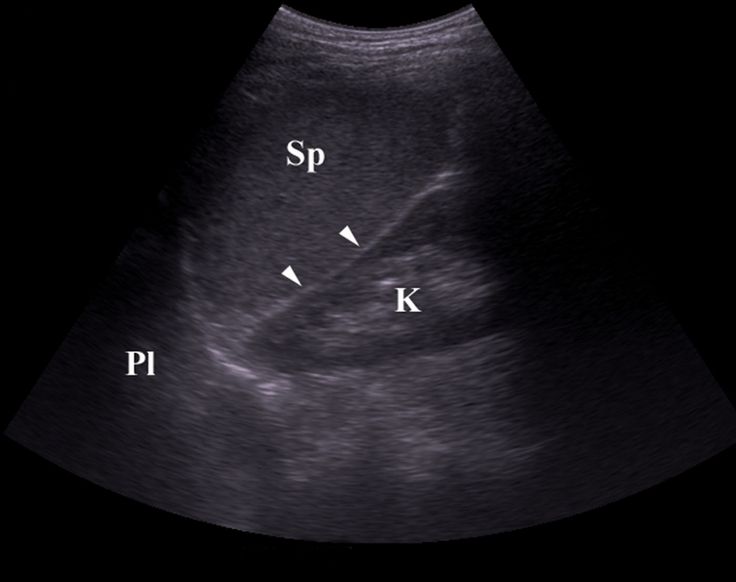
Equipment
Ultrasound machine with a transvaginal ultrasound probe
Ultrasound gel
Probe Cover
Table: The table may be specialized for patient placement in the lithotomy position with stirrups. If this specialized table is unavailable, the patient may lie on a flat table and have a rolled towel or pillow under her pelvis to allow for probe maneuverability.[4]
Personnel
An ultrasound technician conducts a transabdominal ultrasound and then follows with a transvaginal sonographic exam. Images are uploaded to a PACS system which is made available to the radiologist for review and interpretation. The image quality and thoroughness of evaluation are largely dependent on the technician's proficiency and perspective to identify pathology and relay the images in a way that sufficiently allows the radiologist to interpret the ultrasound. A chaperone may be offered to the patient as this decreases misinterpretation or miscommunication during the exam.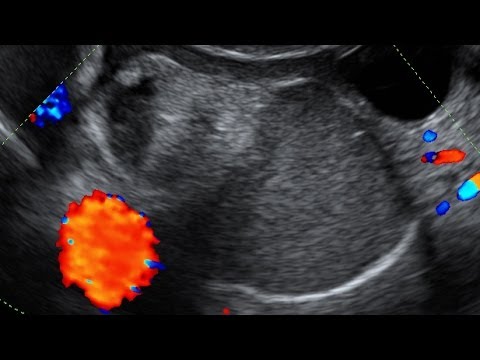 [6]
[6]
Preparation
The patient is asked to undress from the waist down and cover themselves with a gown. Lying supine, transabdominal ultrasound is first performed. A full bladder is recommended as this displaces the adjacent bowel loops that would otherwise distort the image and create an acoustic window, illuminating the organs behind it. Once completed, the patient is asked to empty their bladder. A disinfected transvaginal ultrasound probe is prepared by placing lubricant gel within the tip of the probe cover and then inserting the probe into it. Careful attention should be made to eliminate any bubbles which may interfere with imaging quality as an artifact.
Technique
The transvaginal transducer is inserted, with special attention being made to the orientation of the image. A marker on the screen may be used to indicate cephalad from caudad on sagittal imaging or right from left on transverse imaging, though various protocols are institution-specific.
The probe is placed in the distal vagina or against the external cervical os. Changing the depth of the ultrasound probe will create a different focal point and thus bring different areas within view.[4] Sagittal imaging is obtained with side-to-side movements of the probe, from one adnexa to the other. Turning the probe to 90° will give us a transverse/semi-coronal orientation.[4] The transverse on endovaginal imaging is more of a coronal plane, while the true transverse image is done transabdominally.[1] Subsequent imaging is performed by moving the probe anterior to posterior. A general survey is first performed as an initial evaluation by sweeping the probe from the midline to the lateral margins at the bilateral adnexa. The probe is then rotated 90° and swept in the anterior-posterior direction.[7] The cervix, internal os, endocervical canal, and occasionally the external os is imaged in both sagittal (long-axis) and transverse (short-axis) orientations.
Changing the depth of the ultrasound probe will create a different focal point and thus bring different areas within view.[4] Sagittal imaging is obtained with side-to-side movements of the probe, from one adnexa to the other. Turning the probe to 90° will give us a transverse/semi-coronal orientation.[4] The transverse on endovaginal imaging is more of a coronal plane, while the true transverse image is done transabdominally.[1] Subsequent imaging is performed by moving the probe anterior to posterior. A general survey is first performed as an initial evaluation by sweeping the probe from the midline to the lateral margins at the bilateral adnexa. The probe is then rotated 90° and swept in the anterior-posterior direction.[7] The cervix, internal os, endocervical canal, and occasionally the external os is imaged in both sagittal (long-axis) and transverse (short-axis) orientations.
The cervix is normally 2.5 to 3 cm and may be measured if there is an indication for it, such as recurrent second-trimester miscarriages in the setting of incompetent cervix.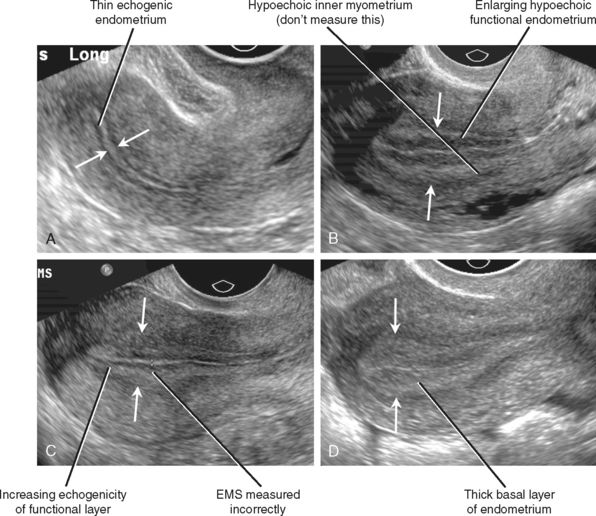 [1] Benign nabothian cysts may be seen here, which are small and anechoic. Concerning the uterus, size, orientation, contour irregularity, and myometrial pattern should be addressed. The length of the uterus is measured on sagittal orientation, from the fundus to the external cervical os if able to image. Transverse/semi-coronal images should also be obtained with anteroposterior and transverse diameters measured. Volume may be calculated from these values. An anteverted uterus, which is the most frequently seen presentation, rests its fundus forward on the bladder, best appreciated on sagittal imaging with the fundus oriented towards the top of the image. A retroverted uterus displays a fundus that orients posteriorly towards the rectum. To see a retroverted uterus may not have any clinical significance, though it may be associated with deep infiltrating endometriosis in the posterior cul-de-sac or abdominal adhesions, particularly if it is fixed in this position.[8] The myometrial pattern should be homogeneous, and the uterine contour should be smooth.
[1] Benign nabothian cysts may be seen here, which are small and anechoic. Concerning the uterus, size, orientation, contour irregularity, and myometrial pattern should be addressed. The length of the uterus is measured on sagittal orientation, from the fundus to the external cervical os if able to image. Transverse/semi-coronal images should also be obtained with anteroposterior and transverse diameters measured. Volume may be calculated from these values. An anteverted uterus, which is the most frequently seen presentation, rests its fundus forward on the bladder, best appreciated on sagittal imaging with the fundus oriented towards the top of the image. A retroverted uterus displays a fundus that orients posteriorly towards the rectum. To see a retroverted uterus may not have any clinical significance, though it may be associated with deep infiltrating endometriosis in the posterior cul-de-sac or abdominal adhesions, particularly if it is fixed in this position.[8] The myometrial pattern should be homogeneous, and the uterine contour should be smooth.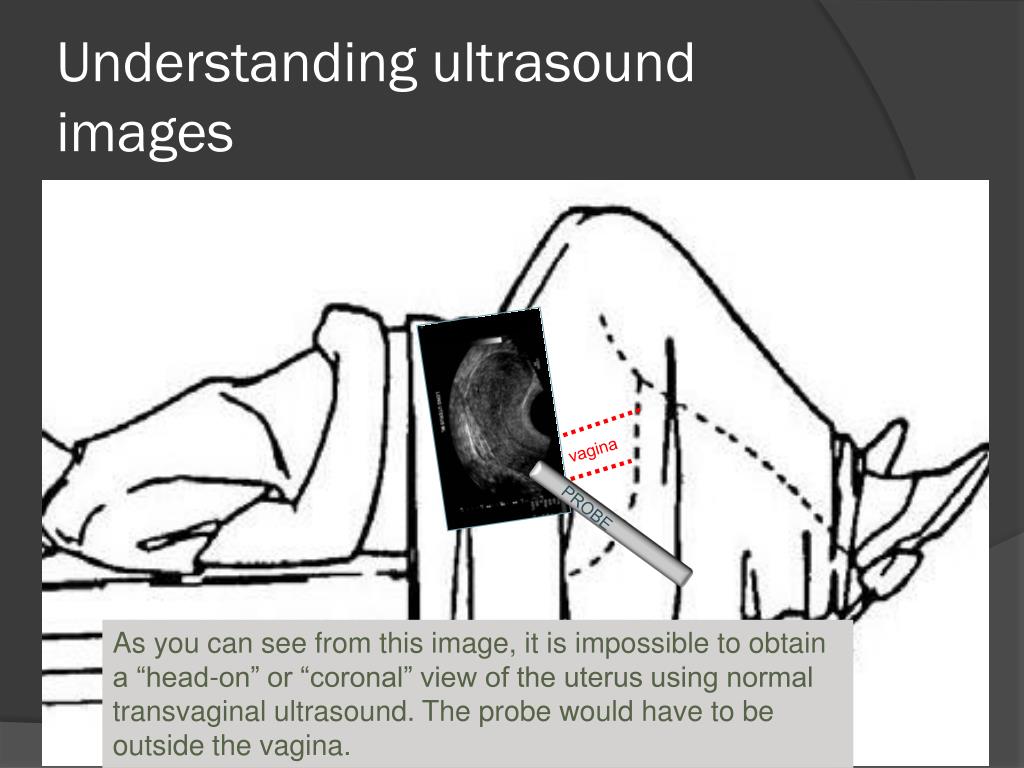 Heterogeneous parenchyma is non-specific though it may be attributable to adenomyosis or fibroids. Not all fibroids need to be measured, but the ones that are measured should be measured in at least 2 dimensions.[8] The location within the layers of the uterus (subserosal, mucosal, submucosal) and which area of the uterus (left wall, fundus, lower segment, etc.) should be reported.
Heterogeneous parenchyma is non-specific though it may be attributable to adenomyosis or fibroids. Not all fibroids need to be measured, but the ones that are measured should be measured in at least 2 dimensions.[8] The location within the layers of the uterus (subserosal, mucosal, submucosal) and which area of the uterus (left wall, fundus, lower segment, etc.) should be reported.
The endometrium, also referred to as the endometrial stripe, is delineated by its normal echogenic nature surrounded by the hypoechoic uterine myometrium. The thickest portion on true sagittal imaging should be measured. If the endometrial cavity has contents such as fluid or an intrauterine device, then it should be documented.[8] The sum of the thickness of the two parallel endometrial lines is recorded as the endometrial thickness in these cases.[9] Normal thickness varies for a premenopausal woman, which may be 3-5 mm during the proliferative phase of the cycle, with an upper limit of 6-12mm during the secretory phase. A maximum thickness of 5 mm is normal in a postmenopausal woman, even in women on hormonal replacement therapy or tamoxifen.[10] Endometrial irregularity, thickening, or cysts may be seen in the setting of adenomyosis. Endometrial thickness may also provide clinically useful information. Saline-infused sonohysterography is a technique to augment visualization of the endometrial lining and cavity and evaluate fallopian tube patency.[11]
A maximum thickness of 5 mm is normal in a postmenopausal woman, even in women on hormonal replacement therapy or tamoxifen.[10] Endometrial irregularity, thickening, or cysts may be seen in the setting of adenomyosis. Endometrial thickness may also provide clinically useful information. Saline-infused sonohysterography is a technique to augment visualization of the endometrial lining and cavity and evaluate fallopian tube patency.[11]
Ultrasonography is the best way to identify the location of early pregnancy in the setting of an elevated beta-hCG; however, a very early intrauterine pregnancy may be missed.[12] Furthermore, an ectopic pregnancy cannot be excluded. Hence a follow-up transvaginal ultrasound and b-hCG are advised [13]. An ectopic pregnancy may occur almost anywhere along with the female reproductive system; however, the majority (95%) implant within the fallopian tubes.[14]
The bilateral ovaries should be measured in three dimensions with the calculation of the volumes.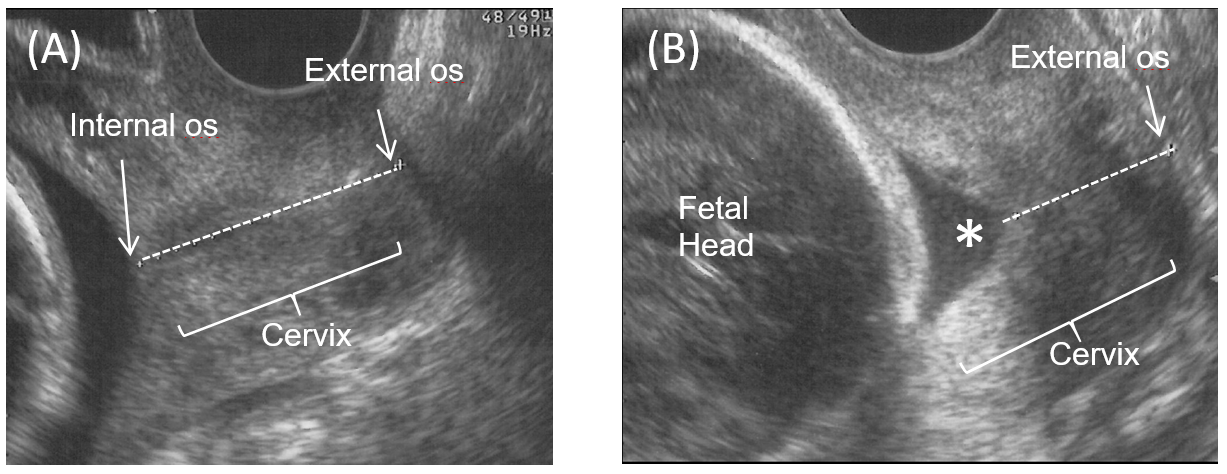 Any masses or prominent cysts should be measured as well. Physiologic follicles in a reproductive-aged woman may be seen. Masses, dilated tubular structures, and other abnormalities should be evaluated in the adnexal regions.[15] However, the fallopian tubes are not typically visualized if there is no pathology present.[7]
Any masses or prominent cysts should be measured as well. Physiologic follicles in a reproductive-aged woman may be seen. Masses, dilated tubular structures, and other abnormalities should be evaluated in the adnexal regions.[15] However, the fallopian tubes are not typically visualized if there is no pathology present.[7]
Dynamic imaging may be performed by a sonographer via placing a hand over the lower abdomen, palpating, and observing the mobility of the internal organs in real-time. “Slide sign” is when the organs move relatively freely against one another. When they are more fixed during palpation, this is indicative of adhesions.[8] Additionally, regional sensitivity to probe maneuvers and anterior abdominal palpation may be pertinent to identify pathology.[7] Another form of dynamic imaging may be performed by taking a cine-loop (video clip). When an area of interest is identified, a cine-clip will allow the interpreting radiologist to characterize pathology more accurately than static images alone.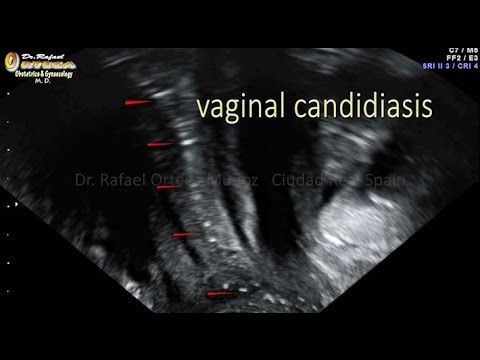 Some protocols have cine-clip imaging as a part of their requirements.[16] The use of color doppler has many utilities. It can assess the vascularity of an identified lesion, assess for hyperemic states such as infection, or assess for lack of flow, such as in the case of ovarian torsion. When color doppler is utilized, this must be mentioned in the reporting technique and findings.
Some protocols have cine-clip imaging as a part of their requirements.[16] The use of color doppler has many utilities. It can assess the vascularity of an identified lesion, assess for hyperemic states such as infection, or assess for lack of flow, such as in the case of ovarian torsion. When color doppler is utilized, this must be mentioned in the reporting technique and findings.
Once the examination is complete, the probe cover is removed, running water and soap are used to remove any gel. After drying the probe, the utilization of a high-level disinfectant is recommended.[17]
Complications
Typically, there are no major complications with this procedure. The patient may experience some discomfort but should not feel any pain.
Clinical Significance
Ultrasound is a tool that is widely available, relatively inexpensive, and timely, which makes it invaluable in evaluating emergency situations. One of these medical emergencies is ovarian torsion, in which there is twisting about the vascular pedicle of the infundibulopelvic ligament and utero-ovarian ligament.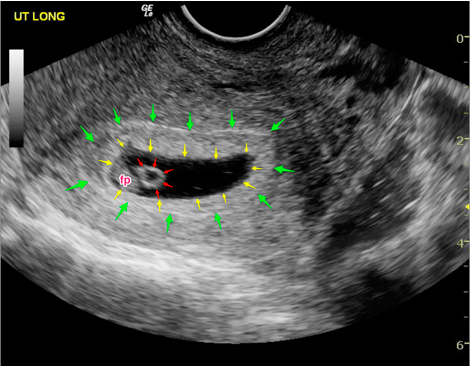 [15] Venous wave-forms are expected to initially become absent because vein walls are thinner and more compressible than their arterial counterparts.[15]
[15] Venous wave-forms are expected to initially become absent because vein walls are thinner and more compressible than their arterial counterparts.[15]
Because of variability in blood flow appearance secondary to setting adjustment, the contralateral normal ovary should be compared.[15] The ovary will appear enlarged, and edematous and pelvic free fluid may be seen.[15] A hallmark characteristic is the whirlpool sign, which is torsion at the infundibulopelvic ligament is evaluated in cross-section.[18]
Seeing some or all of these findings on ultrasound will strongly suggest ovarian torsion. However, there are a few caveats. Due to the dual blood supply from both the ovarian artery running through the infundibulopelvic ligament and the uterine artery from the abdominal aorta, a patient without symptoms may demonstrate an apparent lack of blood flow to the ovary.[15]
Furthermore, the ovary may alternate between being torsed and reconfigured to its original position, which means that some of the aforementioned signs may not be present at the time of the ultrasound.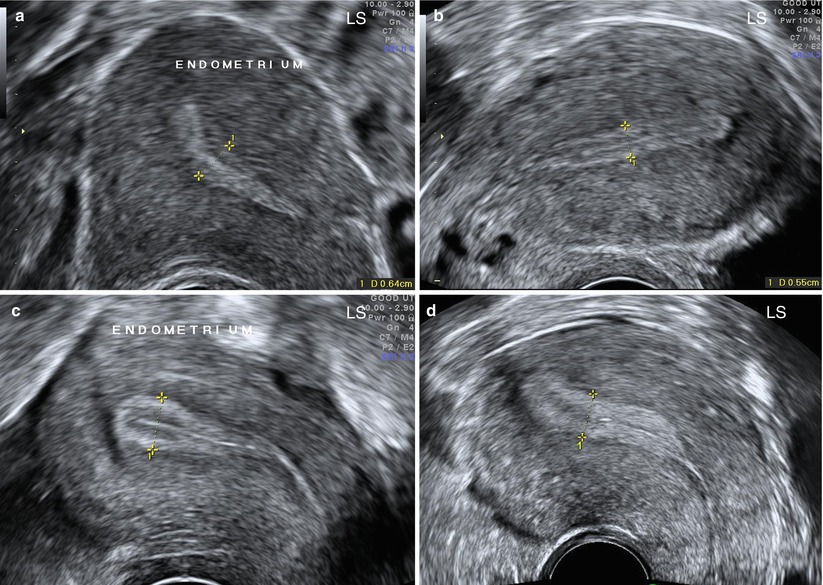 [15] Direct visualization is the mainstay for diagnosis. An appropriate diagnosis of ovarian torsion is made about 84% of the time.[19] The shortcomings of this modality should be known because ultrasound alone may not be sufficient to make a diagnosis.
[15] Direct visualization is the mainstay for diagnosis. An appropriate diagnosis of ovarian torsion is made about 84% of the time.[19] The shortcomings of this modality should be known because ultrasound alone may not be sufficient to make a diagnosis.
Enhancing Healthcare Team Outcomes
The proximity of the transvaginal ultrasound probe to the regions of interest allows for better image quality than its transabdominal counterpart.[4] It operates with a higher frequency transducer (5 to 7.5 MHz), resulting in less artifact. A higher frequency can only penetrate so much through tissue, making it ideal in the transvaginal route.[20] Additionally, there is marked difficulty in obtaining proper transabdominal sonographic images in an obese patient because of the amount of soft tissue the sound waves need to traverse; the transvaginal probe will bypass the pannus.[21]
The transabdominal counterpart operates at a lower frequency (around 3.5 MHz), allowing for deeper signal penetration (as is required) at the expense of poorer resolution.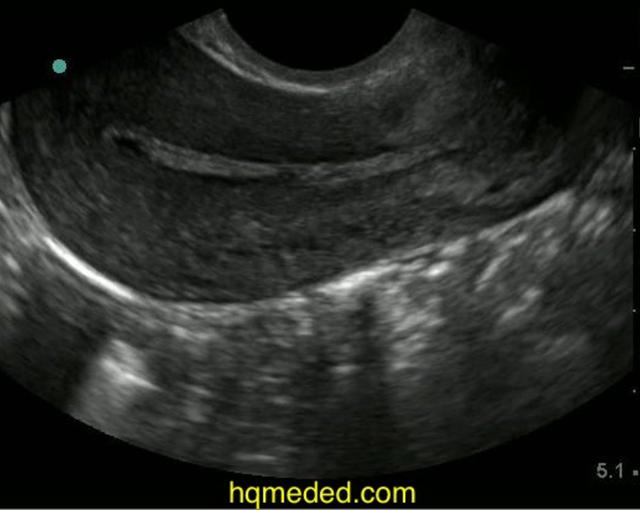 The transabdominal ultrasound also allows more flexibility to image a larger field of view, such as in the setting of the high-positioned adnexa because the probe may be moved anywhere across the abdomen.[22]
The transabdominal ultrasound also allows more flexibility to image a larger field of view, such as in the setting of the high-positioned adnexa because the probe may be moved anywhere across the abdomen.[22]
Each modality has its strength and shortcomings. Hence, the combination of the two methods provides more accurate evaluation and earlier detection of pathology.[23] [Level 2]
Review Questions
Access free multiple choice questions on this topic.
Comment on this article.
Figure
The semicircular region in the superior portion of the image indicates that this is a transvaginal ultrasound. This is a sagittal image (long axis) of the uterus with the cephalad portion on the left as indicated by the LOGIC label. This is a retroflexed (more...)
Figure
This is a sagittal image of the left ovary. Physiologic follicles are noted. Contributed by Suraya Nahlawi, DO
References
- 1.
Wildenberg JC, Yam BL, Langer JE, Jones LP.
 US of the Nongravid Cervix with Multimodality Imaging Correlation: Normal Appearance, Pathologic Conditions, and Diagnostic Pitfalls. Radiographics. 2016 Mar-Apr;36(2):596-617. [PubMed: 26963464]
US of the Nongravid Cervix with Multimodality Imaging Correlation: Normal Appearance, Pathologic Conditions, and Diagnostic Pitfalls. Radiographics. 2016 Mar-Apr;36(2):596-617. [PubMed: 26963464]- 2.
Saksouk FA, Johnson SC. Recognition of the ovaries and ovarian origin of pelvic masses with CT. Radiographics. 2004 Oct;24 Suppl 1:S133-46. [PubMed: 15486237]
- 3.
Dawood MT, Naik M, Bharwani N, Sudderuddin SA, Rockall AG, Stewart VR. Adnexal Torsion: Review of Radiologic Appearances. Radiographics. 2021 Mar-Apr;41(2):609-624. [PubMed: 33577417]
- 4.
Moorthy RS. TRANSVAGINAL SONOGRAPHY. Med J Armed Forces India. 2000 Jul;56(3):181-183. [PMC free article: PMC5532046] [PubMed: 28790701]
- 5.
Chang TS, Böhm-Vélez M, Mendelson EB. Nongynecologic applications of transvaginal sonography. AJR Am J Roentgenol. 1993 Jan;160(1):87-93. [PubMed: 8416655]
- 6.
Cohen C, McLean K, Barton S. Use of chaperones in general practice: chaperones protect both parties.
 BMJ. 2005 Apr 09;330(7495):846-7. [PMC free article: PMC556114] [PubMed: 15817559]
BMJ. 2005 Apr 09;330(7495):846-7. [PMC free article: PMC556114] [PubMed: 15817559]- 7.
Lyons EA, Gratton D, Harrington C. Transvaginal sonography of normal pelvic anatomy. Radiol Clin North Am. 1992 Jul;30(4):663-75. [PubMed: 1631275]
- 8.
AIUM Practice Parameter for the Performance of an Ultrasound Examination of the Female Pelvis. J Ultrasound Med. 2020 May;39(5):E17-E23. [PubMed: 32150295]
- 9.
Fleischer AC. Transvaginal sonography of endometrial disorders: an overview. Radiographics. 1998 Jul-Aug;18(4):923-30. [PubMed: 9672978]
- 10.
Mogavero G, Sheth S, Hamper UM. Endovaginal sonography of the nongravid uterus. Radiographics. 1993 Sep;13(5):969-81. [PubMed: 8210600]
- 11.
Allison SJ, Horrow MM, Kim HY, Lev-Toaff AS. saline-infused sonohysterography: tips for achieving greater success. Radiographics. 2011 Nov-Dec;31(7):1991-2004. [PubMed: 22084183]
- 12.
Pereira PP, Cabar FR, Gomez ÚT, Francisco RPV.
 Pregnancy of unknown location. Clinics (Sao Paulo). 2019;74:e1111. [PMC free article: PMC6784610] [PubMed: 31618321]
Pregnancy of unknown location. Clinics (Sao Paulo). 2019;74:e1111. [PMC free article: PMC6784610] [PubMed: 31618321]- 13.
Barnhart K, van Mello NM, Bourne T, Kirk E, Van Calster B, Bottomley C, Chung K, Condous G, Goldstein S, Hajenius PJ, Mol BW, Molinaro T, O'Flynn O'Brien KL, Husicka R, Sammel M, Timmerman D. Pregnancy of unknown location: a consensus statement of nomenclature, definitions, and outcome. Fertil Steril. 2011 Mar 01;95(3):857-66. [PMC free article: PMC3032825] [PubMed: 20947073]
- 14.
Histed SN, Deshmukh M, Masamed R, Jude CM, Mohammad S, Patel MK. Ectopic Pregnancy: A Trainee's Guide to Making the Right Call: Women's Imaging. Radiographics. 2016 Nov-Dec;36(7):2236-2237. [PubMed: 27831839]
- 15.
Guile SL, Mathai JK. StatPearls [Internet]. StatPearls Publishing; Treasure Island (FL): Jul 21, 2021. Ovarian Torsion. [PubMed: 32809510]
- 16.
Cunningham RK, Horrow MM, Smith RJ, Springer J.
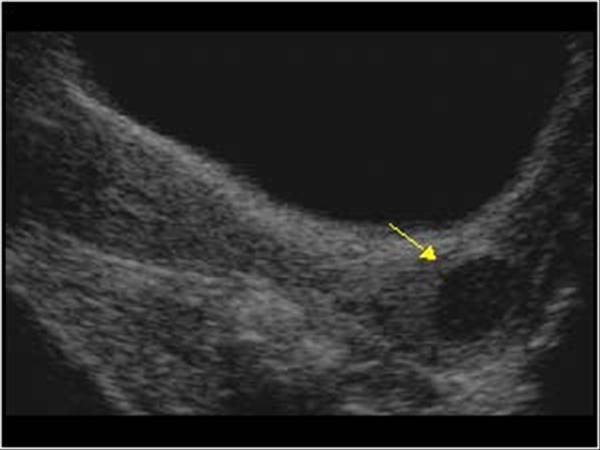
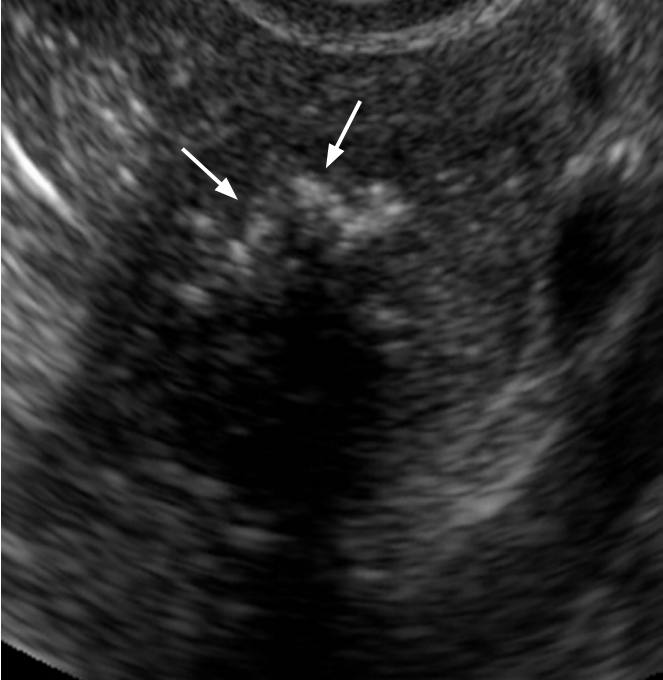 Adenomyosis: A Sonographic Diagnosis. Radiographics. 2018 Sep-Oct;38(5):1576-1589. [PubMed: 30207945]
Adenomyosis: A Sonographic Diagnosis. Radiographics. 2018 Sep-Oct;38(5):1576-1589. [PubMed: 30207945]- 17.
Abramowicz JS, Evans DH, Fowlkes JB, Maršal K, terHaar G., WFUMB Safety Committee. Guidelines for Cleaning Transvaginal Ultrasound Transducers Between Patients. Ultrasound Med Biol. 2017 May;43(5):1076-1079. [PubMed: 28190623]
- 18.
Valsky DV, Esh-Broder E, Cohen SM, Lipschuetz M, Yagel S. Added value of the gray-scale whirlpool sign in the diagnosis of adnexal torsion. Ultrasound Obstet Gynecol. 2010 Nov;36(5):630-4. [PubMed: 20586041]
- 19.
Bardin R, Perl N, Mashiach R, Ram E, Orbach-Zinger S, Shmueli A, Wiznitzer A, Hadar E. Prediction of Adnexal Torsion by Ultrasound in Women with Acute Abdominal Pain. Ultraschall Med. 2020 Dec;41(6):688-694. [PubMed: 31703238]
- 20.
Narayanan M, Tafti D, Cohen HL. StatPearls [Internet]. StatPearls Publishing; Treasure Island (FL): May 15, 2022. Pelvic Ultrasound.
 [PubMed: 29262064]
[PubMed: 29262064]- 21.
Glanc P, O'Hayon BE, Singh DK, Bokhari SA, Maxwell CV. Challenges of pelvic imaging in obese women. Radiographics. 2012 Oct;32(6):1839-62. [PubMed: 23065172]
- 22.
Mausner Geffen E, Slywotzky C, Bennett G. Pitfalls and tips in the diagnosis of ectopic pregnancy. Abdom Radiol (NY). 2017 May;42(5):1524-1542. [PubMed: 28144719]
- 23.
Li Y, Feng T, Sun J. Evaluation of clinical effect of transabdominal sonography and transvaginal sonography in early diagnosis of ectopic gestation. Pak J Med Sci. 2017 Jan-Feb;33(1):53-58. [PMC free article: PMC5368329] [PubMed: 28367172]
Ultrasound of the small pelvis, interpretation of results, preparation for ultrasound examination
Preparation for pelvic ultrasound, interpretation of the results of ultrasound.
Ultrasound is an informative and painless way to study the organs located in the small pelvis. Using this method, various disorders in the work of the genital organs of men and women are revealed.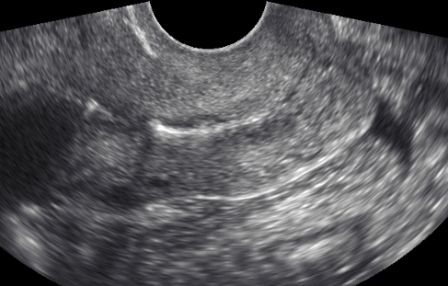 This study is suitable for almost all people.
This study is suitable for almost all people.
When is pelvic ultrasound indicated
During the ultrasound in women, you can see various pathologies in the reproductive organs. This study may be prescribed for:
- pain in the groin and lumbar region;
- pain when urinating;
- mucus and blood in urine;
- changes in the length of the menstrual cycle;
- inflammation of the organs of the reproductive system;
- inability to conceive;
- to confirm pregnancy;
- after difficult delivery or termination of pregnancy;
- installation of the Navy;
- possible ectopic pregnancy.
If pregnancy is confirmed, then ultrasound should be done 3 times - 1 time in each trimester. If necessary, the doctor will prescribe additional ultrasound to monitor the identified pathologies.
Ultrasound of the pelvic organs is prescribed for men with:
- inability to conceive a child;
- pain during urination;
- violation in the work of the prostate and bladder.
Adolescents may be prescribed an ultrasound if the genital organs are not properly developed, too early or, on the contrary, late puberty.
Ultrasound can be done by almost everyone, however, the vaginal method cannot be performed with bleeding, as well as girls who have not had sexual intercourse.
Rectal ultrasound can not be performed in cases where there is available:
- anal fissures;
- hemorrhoids;
- after surgery on the rectum.
Do not perform an ultrasound after an X-ray. This may skew the results. It is better to postpone the study for a few days.
How to prepare for an ultrasound
Preparation depends on which method the ultrasound is performed - transvaginally (performed through the vagina), transabdominally (through the abdominal wall) or transrectal (through the rectum). The uzist should tell you in advance how the procedure will be carried out, because only the vaginal method does not require preparation.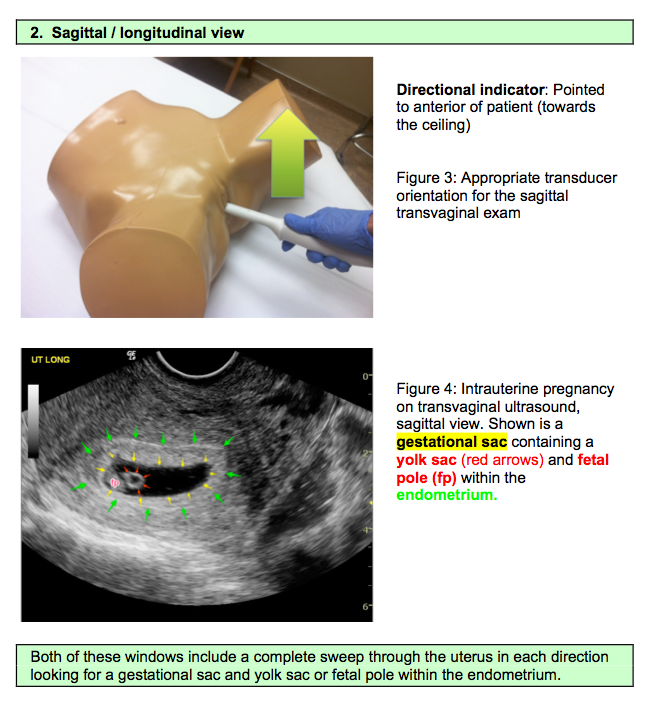
Preparation for transabdominal ultrasound:
- do not eat gas-producing foods It is better to eat cereals, steamed vegetables, low-fat fish and meat;
- If the diet did not bring results, then to get rid of gases, you can take activated charcoal a couple of days before the ultrasound;
- In the morning, on the day of the examination, breakfast is prohibited. It is allowed to have dinner the night before and also do an enema;
- an hour before the start of the ultrasound, the patient drinks 1.5-2 liters of water so that the bladder is full during the study.
Preparation for transrectal examination
Before a rectal examination (approximately 2-3 hours before) you need to do an enema. If a study of the work of the prostate is carried out, the search for the causes of erectile dysfunction and infertility of the bladder should be complete. To do this, one hour before the start of the ultrasound, you should drink 800-1000 ml of water.
Transvaginal examination method
With the vaginal method, the bladder does not need to be filled. The study can be performed on any day of the cycle (with the exception of the days of menstruation), but it will be more effective immediately after the end of the discharge. To assess the correct functioning of the ovaries, as well as to make sure that the follicles are maturing, ultrasound can be scheduled on different days of the cycle.
Features of different ultrasound methods
Each research method has its own characteristics:
- The transvaginal method is performed using a special transducer. The patient takes off his clothes below the waist, lies on his back, spreading his bent legs. The doctor must put a condom on the sensor, then lubricate it with a gel, thanks to which the organ under study will be better visible. When the probe is inserted into the vagina, the patient does not feel any pain. This method will most informatively tell about the state of the female genital organs.
- Transabdominal method. The patient lies on the couch, the specialist applies a special gel to the lower abdomen. With the help of this study, all organs located in the small pelvis are evaluated.
- Transrectal method. It is often used to study the condition of the male genital organs, as well as the bladder. The patient needs to undress below the waist, lie down in the fetal position. The ultrasound specialist applies a gel to the transducer for painless insertion into the rectum.
During the study, you can take material for a biopsy.
Ultrasound interpretation for women
The walls of the bladder in the normal state are of the same thickness, there are no stones in the cavity. In the presence of stones on ultrasound, dark areas with even and clear boundaries are visible.
The thickened walls of the bladder can indicate tumors, polyps, injuries with the formation of hematomas, cystitis.
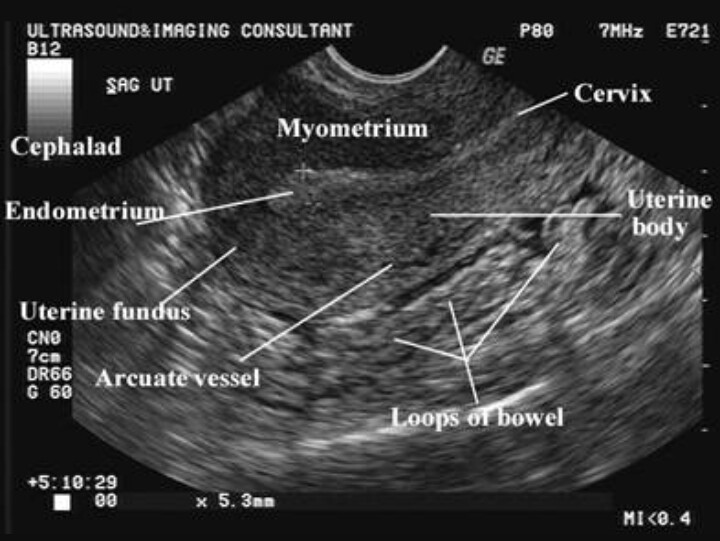
Normal indicators of the reproductive organs in women:
- The length of the uterus varies on average from 4 to 7.
 5 cm, and the width is 4.5 - 6 cm. The contours are clear and even, echogenicity is uniform.
5 cm, and the width is 4.5 - 6 cm. The contours are clear and even, echogenicity is uniform. - Endometrium can vary in thickness depending on cycle day
- The cervix is 2-3 cm in length and width in a healthy state. At the same time, the anterior-posterior size is about 1.5-2 cm. The ovaries have the same value.
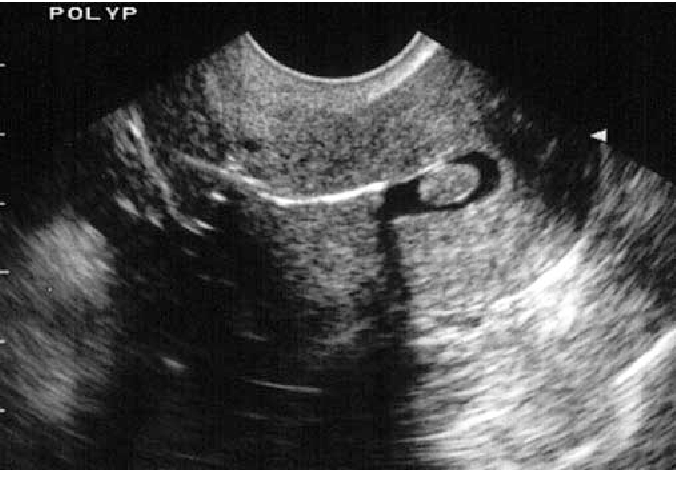
In the presence of an accumulation of benign tumors, echogenicity is reduced, and the size is increased. With endometriosis, the echogenicity of the muscular layer of the uterus is increased, retroversion of the uterus is often present.
If the ovaries are enlarged, and there are many small follicles in them, then the question of polycystic disease may arise.
Interpretation of ultrasound in men
In the study, the ultrasound doctor determines the shape, size, structure and genital organs, as well as the bladder.
The normal prostate is about 2.5 to 3.5 cm long, 2.5 to 4 cm wide, and about 0.2 cm thick.
Seminal vesicles no larger than 1 cm, without seals.
The size of the genital organs depends on the age of the patient. Normally, there are no cysts on the testicles, as well as fluid between them.
Ultrasound allows you to accurately and timely see various diseases of the pelvic organs for the appointment of the correct treatment.
| Ultrasound control of needle biopsy | 2000.00 | |
| Ultrasound imaging | 250.00 | |
| Ultrasound recording on video | 1000.00 | |
| Ultrasound in obstetrics and gynecology | ||
| Ultrasound of the pelvic organs in women (uterus, appendages) | 4000.00 | |
| Ultrasound of the pelvic organs in women (uterus, appendages) Dr. Fotina E.V. | 4000.00 | |
| Ultrasound of the pelvic organs (uterus, appendages) during pregnancy up to 10 weeks | 4000.00 | |
| Ultrasound of pregnant women (includes assessment of anatomical structures, including the fetal heart) | 5000. 00 00 | |
| Ultrasound of pregnant women (includes assessment of anatomical structures, including fetal heart) under contracts | 4500.00 | Dr. Alibegovich I.V. 5000.00 |
| Ultrasound of the pelvic organs in women (uterus, appendages) (expert) | 7000.00 | |
| Ultrasound of the pelvic organs during pregnancy up to 10 weeks (Professor Panina O.B.) | 7000.00 | |
| Ultrasound of pregnant women (includes assessment of anatomical structures, including fetal heart) (expert) | 7000.00 | |
| Fetal Doppler (under contracts) | 1400.00 | |
| Fetal Doppler | 1800.00 | |
| Dopplerometry in gynecology (uterine vessels) | 1700.00 | |
| Dopplerometry in gynecology (uterine vessels) II degree of complexity | 2200.00 | |
| Ultrasound folliculometry | 1700.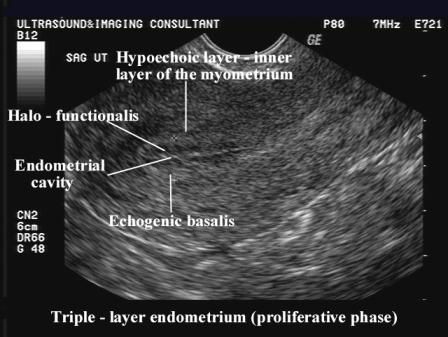 00 00 | |
| Ultrasound of the ovaries | 1400.00 | |
| Ultrasound of the location of the placenta | 1200.00 | |
| Ultrasound determination of the amount of amniotic fluid | 1400.00 | |
| Ultrasound determination of the fetal heartbeat | 1400.00 | |
| Ultrasound of the cervix | 1400.00 | |
| Uterine tone ultrasound | 1400.00 | |
| Ultrasound of the lower uterine segment | 1400.00 | |
| Endometrial ultrasound | 1400.00 | |
| Ultrasound control after IUD insertion | 1400.00 | |
| Vascular ultrasound | ||
| Duplex scanning of brachiocephalic arteries (neck vessels) | 3000.00 | |
| Duplex scanning of brachiocephalic arteries (neck vessels) Dr. Grigorieva M.A. | 3200.00 | |
| Upper limb duplex vein scanning | 2400.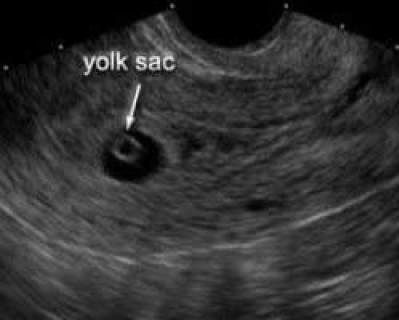 00 00 | |
| Duplex scanning of the veins of the upper extremities (Dr. Grigoryeva M.A.) | 2800.00 | |
| Upper limb duplex scanning | 2400.00 | |
| Duplex scanning of the arteries of the upper limbs (Dr. Grigorieva M.A.) | 2800.00 | |
| Duplex scanning of vessels of the upper extremities (veins and arteries) | 3800.00 | |
| Duplex scanning of vessels of the upper extremities (veins and arteries) Dr. Grigoryeva M.A. | 4600.00 | |
| Duplex scanning of the superficial and deep veins of the lower extremities | 3200.00 | |
| Duplex scanning of the superficial and deep veins of the lower extremities (Dr. Grigoryeva M.A.) | 3600.00 | |
| Duplex scanning of lower limb arteries | 3000.00 | |
| Duplex scanning of arteries of the lower extremities (Dr. Grigorieva M.A.) | 3200. 00 00 | |
| Duplex scanning of vessels of the lower extremities (veins and arteries) | 5200.00 | |
| Duplex scanning of vessels of the lower extremities (veins and arteries) Dr. Grigoryeva M.A. | 5800.00 | |
| Ultrasound Dopplerography of the veins of the lower extremities with mapping of perforating veins (duplex mode) in trophic ulcers (Mkrtchyan A.N.) | 3200.00 | |
| Doppler ultrasound of abdominal vessels | 2400.00 | |
| Doppler ultrasound of the abdominal aorta | 2200.00 | |
| Doppler ultrasound of renal vessels | 2200.00 | |
| Cardiac ultrasound | ||
| ECHO-KG | 3600.00 | |
| ECHO-KG (Dr. Serkina T.V., Filippova E.A.) | 4000.00 | |
| Ultrasound of small parts | ||
| Thyroid ultrasound | 2400.00 | |
| Breast ultrasound | 2400.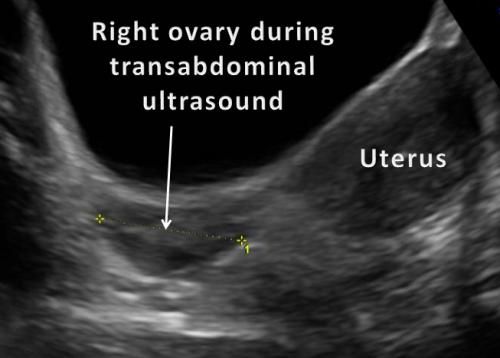 00 00 | |
| Ultrasound of one joint | 2400.00 | |
| Ultrasound of soft tissues (one anatomical zone) | 1800.00 | |
| Ultrasound of the pleural cavity | 1800.00 | |
| Ultrasound of the paranasal sinuses | 1800.00 | |
| Ultrasound of lymph nodes (anatomical area) | 1800.00 | |
| Ultrasound of the salivary glands | 1800.00 | |
| Abdominal ultrasound | ||
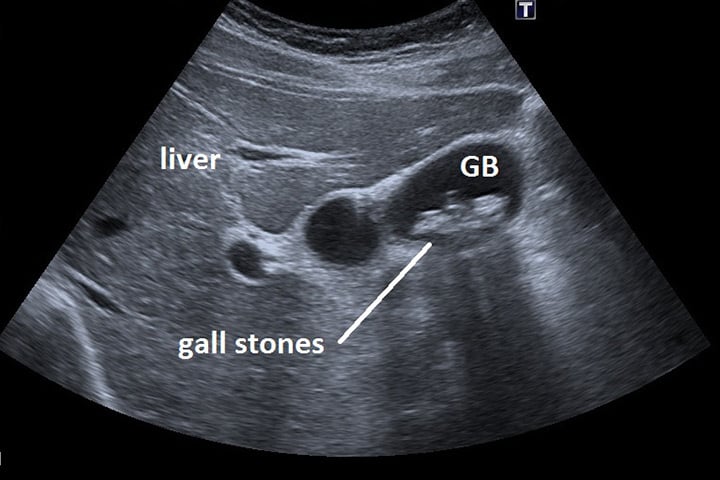
| Ultrasound of the abdominal organs (liver, gallbladder, pancreas, spleen) | 2900.00 | |
| Ultrasound of the gallbladder with a choleretic breakfast (assessment of the motor function of the gallbladder) (performed together with ultrasound of the abdominal cavity) | 3400.00 | |
| Ultrasound of the retroperitoneal space (adrenals, abdominal aorta, retroperitoneal lymph nodes) | 2400.00 | |
| Small bowel ultrasound | 1700.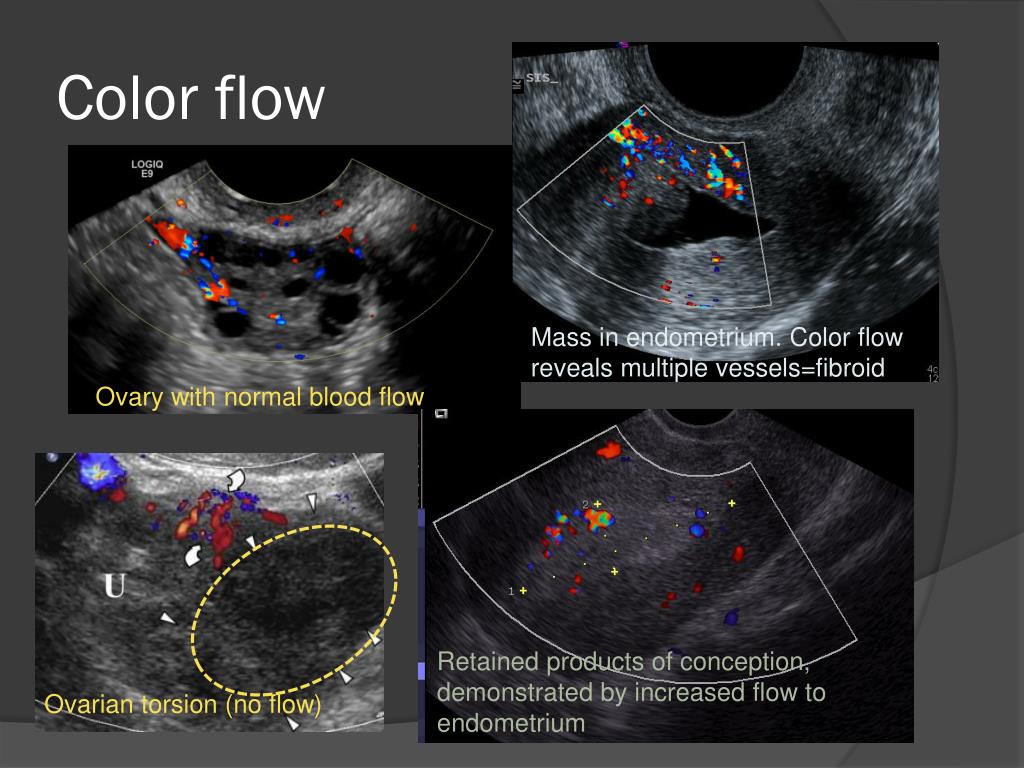 00 00 | |
| Colon ultrasound | 1700.00 | |
| Ultrasound in urology | ||
| Ultrasound of the urinary system (kidneys, ureters, bladder) | 2600.00 | |
| Ultrasound of the urinary system (kidneys, ureters, bladder) Dr. Sevostyanov V.I. | 2800.00 | |
| Ultrasound of the adrenal glands | 1400.00 | |
| Ultrasound of the adrenal glands (Dr. Sevostyanov V.I.) | 1800.00 | |
| Transabdominal ultrasound of the bladder and prostate (with determination of residual urine volume) | 2400.00 | |
| Transabdominal ultrasound of the bladder and prostate (with determination of residual urine volume) Dr. Sevostyanov V.I. | 2800.00 | |
| Transrectal ultrasound of the prostate (TRUS) | 2400.00 | |
| Transrectal ultrasonography of the prostate (TRUS) Dr. Sevostyanov V.I. | 2800.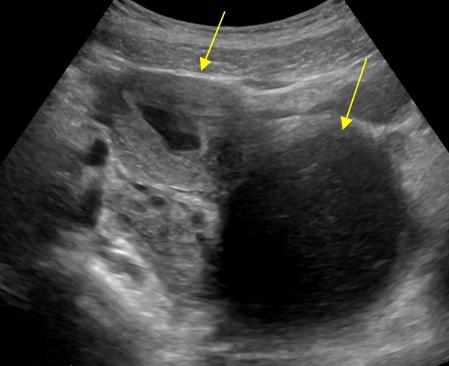 00 00 | |
| Prostate ultrasound | 2000.00 | |
| Ultrasound of the scrotum | 2400.00 | |
| Ultrasound of the scrotum (Dr. Sevostyanov V.I.) | 2800.00 | |
| Transabdominal ultrasound of the pelvic organs in men (prostate, testicles, bladder) | 2400.00 | |
| Ultrasound of the pelvic organs in men transabdominal (prostate, testicles, bladder) Dr. Sevostyanov V.I. | 3000.00 | |
| Duplex scanning of vessels of the scrotum | 2400.00 | |
| Duplex scanning of vessels of the scrotal organs (Dr. Sevostyanov V.I.) | 2800.00 | |
| Ultrasound (pediatrics) | ||
| Neurosonography (children) | 2200.00 | |
| Neurosonography with vascular dopplerography (children) | 3800.00 | |
| Ultrasound of the hip joints (children) | 2500.00 | |
| Reproductive ultrasound (children) | 2600.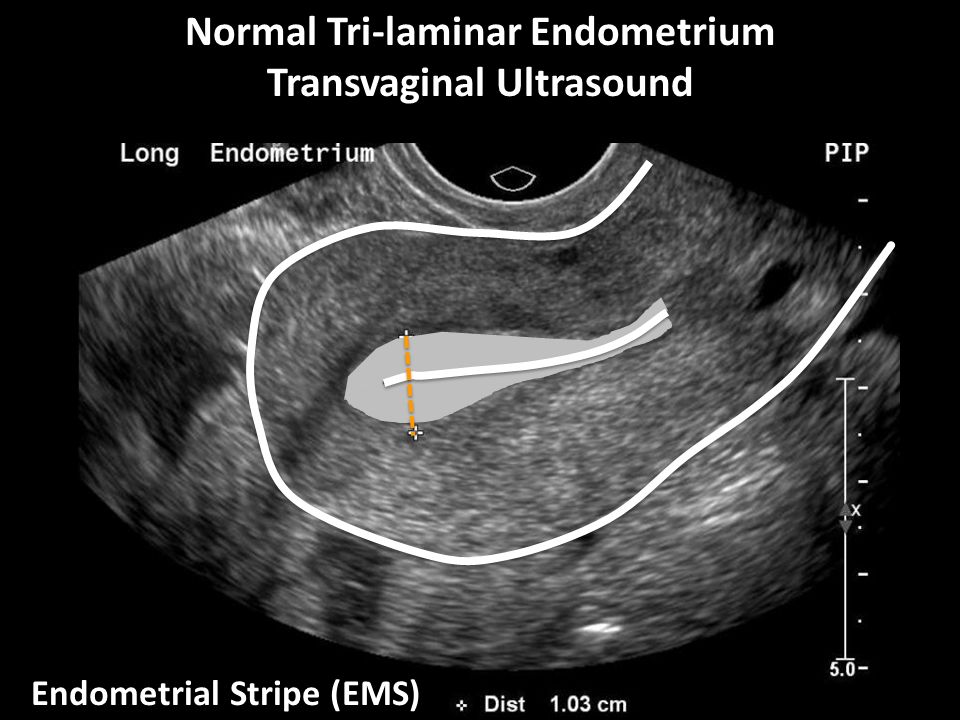 00 00 | |
| Ultrasound of the reproductive sphere (children) Ph.D. | 3400.00 | |
| Ultrasound of the thymus (thymus) | 2200.00 | |
| Ultrasound of hollow organs (children) | 2200.00 | |
| Ultrasound of the parotid glands (children) | 2200.00 | |
| Vascular Doppler (during neurosonography) | 1600.00 | |
| Ultrasound examination of the esophagus in a child | 1600.00 | |
| Ultrasound examination of the small intestine in a child | 1600.00 | |
| Ultrasound examination of the colon in a child | 1600.00 | |
| Child prostate ultrasound | 1800.00 | |
| Doppler ultrasound of the vessels of the spermatic cord in a child | 1600.00 | |
| Ultrasound examination of the adrenal glands in a child | 1200.00 | |
| Ultrasound examination of the child's brain | 2600. |