What does ivf stand for in medical terms
In vitro fertilization (IVF) - Mayo Clinic
Overview
In vitro fertilization
In vitro fertilization
During in vitro fertilization, eggs are removed from mature follicles within an ovary (A). An egg is fertilized by injecting a single sperm into the egg or mixing the egg with sperm in a petri dish (B). The fertilized egg (embryo) is transferred into the uterus (C).
In vitro fertilization (IVF) is a complex series of procedures used to help with fertility or prevent genetic problems and assist with the conception of a child.
During IVF, mature eggs are collected (retrieved) from ovaries and fertilized by sperm in a lab. Then the fertilized egg (embryo) or eggs (embryos) are transferred to a uterus. One full cycle of IVF takes about three weeks. Sometimes these steps are split into different parts and the process can take longer.
IVF is the most effective form of assisted reproductive technology. The procedure can be done using a couple's own eggs and sperm. Or IVF may involve eggs, sperm or embryos from a known or anonymous donor. In some cases, a gestational carrier — someone who has an embryo implanted in the uterus — might be used.
Your chances of having a healthy baby using IVF depend on many factors, such as your age and the cause of infertility. In addition, IVF can be time-consuming, expensive and invasive. If more than one embryo is transferred to the uterus, IVF can result in a pregnancy with more than one fetus (multiple pregnancy).
Your doctor can help you understand how IVF works, the potential risks and whether this method of treating infertility is right for you.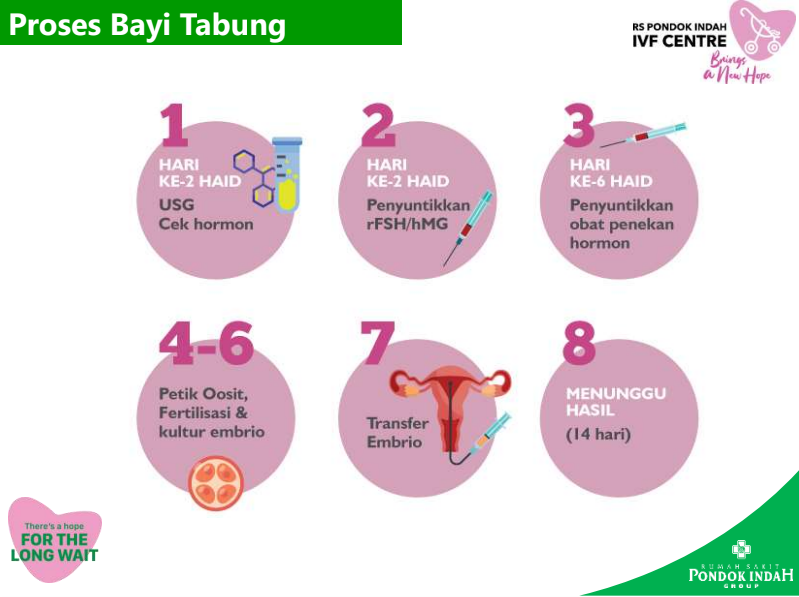
Products & Services
- Book: Mayo Clinic Family Health Book, 5th Edition
- Book: Mayo Clinic Guide to a Healthy Pregnancy
- Book: Mayo Clinic Guide to Fertility and Conception
- Newsletter: Mayo Clinic Health Letter — Digital Edition
Why it's done
In vitro fertilization (IVF) is a treatment for infertility or genetic problems. If IVF is performed to treat infertility, you and your partner might be able to try less-invasive treatment options before attempting IVF, including fertility drugs to increase production of eggs or intrauterine insemination — a procedure in which sperm are placed directly in the uterus near the time of ovulation.
Sometimes, IVF is offered as a primary treatment for infertility in women over age 40. IVF can also be done if you have certain health conditions. For example, IVF may be an option if you or your partner has:
For example, IVF may be an option if you or your partner has:
- Fallopian tube damage or blockage. Fallopian tube damage or blockage makes it difficult for an egg to be fertilized or for an embryo to travel to the uterus.
- Ovulation disorders. If ovulation is infrequent or absent, fewer eggs are available for fertilization.
- Endometriosis. Endometriosis occurs when tissue similar to the lining of the uterus implants and grows outside of the uterus — often affecting the function of the ovaries, uterus and fallopian tubes.
- Uterine fibroids. Fibroids are benign tumors in the uterus. They are common in women in their 30s and 40s. Fibroids can interfere with implantation of the fertilized egg.
- Previous tubal sterilization or removal. Tubal ligation is a type of sterilization in which the fallopian tubes are cut or blocked to permanently prevent pregnancy.
 If you wish to conceive after tubal ligation, IVF may be an alternative to tubal ligation reversal surgery.
If you wish to conceive after tubal ligation, IVF may be an alternative to tubal ligation reversal surgery. - Impaired sperm production or function. Below-average sperm concentration, weak movement of sperm (poor mobility), or abnormalities in sperm size and shape can make it difficult for sperm to fertilize an egg. If semen abnormalities are found, a visit to an infertility specialist might be needed to see if there are correctable problems or underlying health concerns.
- Unexplained infertility. Unexplained infertility means no cause of infertility has been found despite evaluation for common causes.
- A genetic disorder. If you or your partner is at risk of passing on a genetic disorder to your child, you may be candidates for preimplantation genetic testing — a procedure that involves IVF. After the eggs are harvested and fertilized, they're screened for certain genetic problems, although not all genetic problems can be found.
 Embryos that don't contain identified problems can be transferred to the uterus.
Embryos that don't contain identified problems can be transferred to the uterus. -
Fertility preservation for cancer or other health conditions. If you're about to start cancer treatment — such as radiation or chemotherapy — that could harm your fertility, IVF for fertility preservation may be an option. Women can have eggs harvested from their ovaries and frozen in an unfertilized state for later use. Or the eggs can be fertilized and frozen as embryos for future use.
Women who don't have a functional uterus or for whom pregnancy poses a serious health risk might choose IVF using another person to carry the pregnancy (gestational carrier). In this case, the woman's eggs are fertilized with sperm, but the resulting embryos are placed in the gestational carrier's uterus.
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Risks
Risks of IVF include:
- Multiple births.
 IVF increases the risk of multiple births if more than one embryo is transferred to your uterus. A pregnancy with multiple fetuses carries a higher risk of early labor and low birth weight than pregnancy with a single fetus does.
IVF increases the risk of multiple births if more than one embryo is transferred to your uterus. A pregnancy with multiple fetuses carries a higher risk of early labor and low birth weight than pregnancy with a single fetus does. - Premature delivery and low birth weight. Research suggests that IVF slightly increases the risk that the baby will be born early or with a low birth weight.
-
Ovarian hyperstimulation syndrome. Use of injectable fertility drugs, such as human chorionic gonadotropin (HCG), to induce ovulation can cause ovarian hyperstimulation syndrome, in which your ovaries become swollen and painful.
Symptoms typically last a week and include mild abdominal pain, bloating, nausea, vomiting and diarrhea. If you become pregnant, however, your symptoms might last several weeks. Rarely, it's possible to develop a more severe form of ovarian hyperstimulation syndrome that can also cause rapid weight gain and shortness of breath.

- Miscarriage. The rate of miscarriage for women who conceive using IVF with fresh embryos is similar to that of women who conceive naturally — about 15% to 25% — but the rate increases with maternal age.
- Egg-retrieval procedure complications. Use of an aspirating needle to collect eggs could possibly cause bleeding, infection or damage to the bowel, bladder or a blood vessel. Risks are also associated with sedation and general anesthesia, if used.
- Ectopic pregnancy. About 2% to 5% of women who use IVF will have an ectopic pregnancy — when the fertilized egg implants outside the uterus, usually in a fallopian tube. The fertilized egg can't survive outside the uterus, and there's no way to continue the pregnancy.
- Birth defects. The age of the mother is the primary risk factor in the development of birth defects, no matter how the child is conceived.
 More research is needed to determine whether babies conceived using IVF might be at increased risk of certain birth defects.
More research is needed to determine whether babies conceived using IVF might be at increased risk of certain birth defects. - Cancer. Although some early studies suggested there may be a link between certain medications used to stimulate egg growth and the development of a specific type of ovarian tumor, more-recent studies do not support these findings. There does not appear to be a significantly increased risk of breast, endometrial, cervical or ovarian cancer after IVF.
- Stress. Use of IVF can be financially, physically and emotionally draining. Support from counselors, family and friends can help you and your partner through the ups and downs of infertility treatment.
How you prepare
The Centers for Disease Control and Prevention and the Society for Assisted Reproductive Technology provide information online about U. S. clinics' individual pregnancy and live birth rates.
S. clinics' individual pregnancy and live birth rates.
A clinic's success rate depends on many factors. These include patients' ages and medical issues, as well as the clinic's treatment population and treatment approaches. Ask for detailed information about the costs associated with each step of the procedure.
Before beginning a cycle of IVF using your own eggs and sperm, you and your partner will likely need various screenings, including:
- Ovarian reserve testing. To determine the quantity and quality of your eggs, your doctor might test the concentration of follicle-stimulating hormone (FSH), estradiol (estrogen) and anti-mullerian hormone in your blood during the first few days of your menstrual cycle. Test results, often used together with an ultrasound of your ovaries, can help predict how your ovaries will respond to fertility medication.
- Semen analysis. If not done as part of your initial fertility evaluation, your doctor will conduct a semen analysis shortly before the start of an IVF treatment cycle.

- Infectious disease screening. You and your partner will both be screened for infectious diseases, including HIV.
- Practice (mock) embryo transfer. Your doctor might conduct a mock embryo transfer to determine the depth of your uterine cavity and the technique most likely to successfully place the embryos into your uterus.
- Uterine exam. Your doctor will examine the inside lining of the uterus before you start IVF. This might involve a sonohysterography — in which fluid is injected through the cervix into your uterus — and an ultrasound to create images of your uterine cavity. Or it might include a hysteroscopy — in which a thin, flexible, lighted telescope (hysteroscope) is inserted through your vagina and cervix into your uterus.
Before beginning a cycle of IVF, consider important questions, including:
-
How many embryos will be transferred? The number of embryos transferred is typically based on age and number of eggs retrieved.
 Since the rate of implantation is lower for older women, more embryos are usually transferred — except for women using donor eggs or genetically tested embryos.
Since the rate of implantation is lower for older women, more embryos are usually transferred — except for women using donor eggs or genetically tested embryos.Most doctors follow specific guidelines to prevent a higher order multiple pregnancy, such as triplets or more. In some countries, legislation limits the number of embryos that can be transferred. Make sure you and your doctor agree on the number of embryos that will be transferred before the transfer procedure.
-
What will you do with any extra embryos? Extra embryos can be frozen and stored for future use for several years. Not all embryos will survive the freezing and thawing process, although most will.
Having frozen embryos can make future cycles of IVF less expensive and less invasive. Or, you might be able to donate unused frozen embryos to another couple or a research facility. You might also choose to discard unused embryos.

- How will you handle a multiple pregnancy? If more than one embryo is transferred to your uterus, IVF can result in a multiple pregnancy — which poses health risks for you and your babies. In some cases, fetal reduction can be used to help a woman deliver fewer babies with lower health risks. Pursuing fetal reduction, however, is a major decision with ethical, emotional and psychological consequences.
- Have you considered the potential complications associated with using donor eggs, sperm or embryos, or a gestational carrier? A trained counselor with expertise in donor issues can help you understand the concerns, such as the legal rights of the donor. You may also need an attorney to file court papers to help you become legal parents of an implanted embryo.
What you can expect
IVF involves several steps — ovarian stimulation, egg retrieval, sperm retrieval, fertilization and embryo transfer. One cycle of IVF can take about two to three weeks. More than one cycle may be needed.
One cycle of IVF can take about two to three weeks. More than one cycle may be needed.
Ovulation induction
The start of an IVF cycle begins by using synthetic hormones to stimulate the ovaries to produce multiple eggs — rather than the single egg that typically develops each month. Multiple eggs are needed because some eggs won't fertilize or develop normally after fertilization.
Several different medications may be used, such as:
- Medications for ovarian stimulation. To stimulate your ovaries, you might receive an injectable medication containing a follicle-stimulating hormone (FSH), a luteinizing hormone (LH) or a combination of both. These medications stimulate more than one egg to develop at a time.
- Medications for oocyte maturation. When the follicles are ready for egg retrieval — generally after eight to 14 days — you will take human chorionic gonadotropin (HCG) or other medications to help the eggs mature.

- Medications to prevent premature ovulation. These medications prevent your body from releasing the developing eggs too soon.
- Medications to prepare the lining of your uterus. On the day of egg retrieval or at the time of embryo transfer, your doctor might recommend that you begin taking progesterone supplements to make the lining of your uterus more receptive to implantation.
Your doctor will work with you to determine which medications to use and when to use them.
Typically, you'll need one to two weeks of ovarian stimulation before your eggs are ready for retrieval. To determine when the eggs are ready for collection, you may have:
- Vaginal ultrasound, an imaging exam of your ovaries to monitor the development of follicles — fluid-filled ovarian sacs where eggs mature
- Blood tests, to measure your response to ovarian stimulation medications — estrogen levels typically increase as follicles develop, and progesterone levels remain low until after ovulation
Sometimes IVF cycles need to be canceled before egg retrieval for one of these reasons:
- Inadequate number of follicles developing
- Premature ovulation
- Too many follicles developing, creating a risk of ovarian hyperstimulation syndrome
- Other medical issues
If your cycle is canceled, your doctor might recommend changing medications or their doses to promote a better response during future IVF cycles.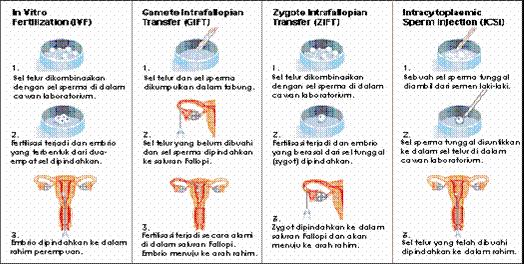 Or you may be advised that you need an egg donor.
Or you may be advised that you need an egg donor.
Egg retrieval
Egg retrieval can be done in your doctor's office or a clinic 34 to 36 hours after the final injection and before ovulation.
- During egg retrieval, you'll be sedated and given pain medication.
- Transvaginal ultrasound aspiration is the usual retrieval method. An ultrasound probe is inserted into your vagina to identify follicles. Then a thin needle is inserted into an ultrasound guide to go through the vagina and into the follicles to retrieve the eggs.
- If your ovaries aren't accessible through transvaginal ultrasound, an abdominal ultrasound may be used to guide the needle.
- The eggs are removed from the follicles through a needle connected to a suction device. Multiple eggs can be removed in about 20 minutes.
- After egg retrieval, you may experience cramping and feelings of fullness or pressure.
- Mature eggs are placed in a nutritive liquid (culture medium) and incubated.
 Eggs that appear healthy and mature will be mixed with sperm to attempt to create embryos. However, not all eggs may be successfully fertilized.
Eggs that appear healthy and mature will be mixed with sperm to attempt to create embryos. However, not all eggs may be successfully fertilized.
Sperm retrieval
If you're using your partner's sperm, a semen sample needs to be provided at your doctor's office or clinic the morning of egg retrieval. Typically, the semen sample is collected through masturbation. Other methods, such as testicular aspiration — the use of a needle or surgical procedure to extract sperm directly from the testicle — are sometimes required. Donor sperm also can be used. Sperm are separated from the semen fluid in the lab.
Fertilization
Fertilization can be attempted using two common methods:
- Conventional insemination. During conventional insemination, healthy sperm and mature eggs are mixed and incubated overnight.
- Intracytoplasmic sperm injection (ICSI). In ICSI, a single healthy sperm is injected directly into each mature egg.
 ICSI is often used when semen quality or number is a problem or if fertilization attempts during prior IVF cycles failed.
ICSI is often used when semen quality or number is a problem or if fertilization attempts during prior IVF cycles failed.
In certain situations, your doctor may recommend other procedures before embryo transfer.
- Assisted hatching. About five to six days after fertilization, an embryo "hatches" from its surrounding membrane (zona pellucida), allowing it to implant into the lining of the uterus. If you're an older woman, or if you have had multiple failed IVF attempts, your doctor might recommend assisted hatching — a technique in which a hole is made in the zona pellucida just before transfer to help the embryo hatch and implant. Assisted hatching is also useful for eggs or embryos that have been previously frozen as the process can harden the zona pellucida.
- Preimplantation genetic testing.
 Embryos are allowed to develop in the incubator until they reach a stage where a small sample can be removed and tested for specific genetic diseases or the correct number of chromosomes, typically after five to six days of development. Embryos that don't contain affected genes or chromosomes can be transferred to your uterus. While preimplantation genetic testing can reduce the likelihood that a parent will pass on a genetic problem, it can't eliminate the risk. Prenatal testing may still be recommended.
Embryos are allowed to develop in the incubator until they reach a stage where a small sample can be removed and tested for specific genetic diseases or the correct number of chromosomes, typically after five to six days of development. Embryos that don't contain affected genes or chromosomes can be transferred to your uterus. While preimplantation genetic testing can reduce the likelihood that a parent will pass on a genetic problem, it can't eliminate the risk. Prenatal testing may still be recommended.
Embryo transfer
Egg-retrieval technique
Egg-retrieval technique
Typically, transvaginal ultrasound aspiration is used to retrieve eggs. During this procedure, an ultrasound probe is inserted into your vagina to identify follicles, and a needle is guided through the vagina and into the follicles. The eggs are removed from the follicles through the needle, which is connected to a suction device.
ICSI
ICSI
In intracytoplasmic sperm injection (ICSI), a single healthy sperm is injected directly into each mature egg. ICSI is often used when semen quality or number is a problem or if fertilization attempts during prior in vitro fertilization cycles failed.
ICSI is often used when semen quality or number is a problem or if fertilization attempts during prior in vitro fertilization cycles failed.
Blastocyst
Blastocyst
Three days after fertilization, a normally developing embryo will contain about six to 10 cells. By the fifth or sixth day, the fertilized egg is known as a blastocyst — a rapidly dividing ball of cells. The inner group of cells will become the embryo. The outer group will become the cells that nourish and protect it.
Embryo transfer is done at your doctor's office or a clinic and usually takes place two to five days after egg retrieval.
- You might be given a mild sedative. The procedure is usually painless, although you might experience mild cramping.
- The doctor will insert a long, thin, flexible tube called a catheter into your vagina, through your cervix and into your uterus.
- A syringe containing one or more embryos suspended in a small amount of fluid is attached to the end of the catheter.

- Using the syringe, the doctor places the embryo or embryos into your uterus.
If successful, an embryo will implant in the lining of your uterus about six to 10 days after egg retrieval.
After the procedure
After the embryo transfer, you can resume your usual daily activities. However, your ovaries may still be enlarged. Consider avoiding vigorous activity, which could cause discomfort.
Typical side effects include:
- Passing a small amount of clear or bloody fluid shortly after the procedure — due to the swabbing of the cervix before the embryo transfer
- Breast tenderness due to high estrogen levels
- Mild bloating
- Mild cramping
- Constipation
If you develop moderate or severe pain after the embryo transfer, contact your doctor. He or she will evaluate you for complications such as infection, twisting of an ovary (ovarian torsion) and severe ovarian hyperstimulation syndrome.
Results
About 12 days to two weeks after egg retrieval, your doctor will test a sample of your blood to detect whether you're pregnant.
- If you're pregnant, your doctor will refer you to an obstetrician or other pregnancy specialist for prenatal care.
- If you're not pregnant, you'll stop taking progesterone and likely get your period within a week. If you don't get your period or you have unusual bleeding, contact your doctor. If you're interested in attempting another cycle of in vitro fertilization (IVF), your doctor might suggest steps you can take to improve your chances of getting pregnant through IVF.
The chances of giving birth to a healthy baby after using IVF depend on various factors, including:
- Maternal age. The younger you are, the more likely you are to get pregnant and give birth to a healthy baby using your own eggs during IVF.
Women age 41 and older are often counseled to consider using donor eggs during IVF to increase the chances of success.
- Embryo status. Transfer of embryos that are more developed is associated with higher pregnancy rates compared with less-developed embryos (day two or three). However, not all embryos survive the development process. Talk with your doctor or other care provider about your specific situation.
- Reproductive history. Women who've previously given birth are more likely to be able to get pregnant using IVF than are women who've never given birth. Success rates are lower for women who've previously used IVF multiple times but didn't get pregnant.
- Cause of infertility. Having a normal supply of eggs increases your chances of being able to get pregnant using IVF.
 Women who have severe endometriosis are less likely to be able to get pregnant using IVF than are women who have unexplained infertility.
Women who have severe endometriosis are less likely to be able to get pregnant using IVF than are women who have unexplained infertility. - Lifestyle factors. Women who smoke typically have fewer eggs retrieved during IVF and may miscarry more often. Smoking can lower a woman's chance of success using IVF by 50%. Obesity can decrease your chances of getting pregnant and having a baby. Use of alcohol, recreational drugs, excessive caffeine and certain medications also can be harmful.
Talk with your doctor about any factors that apply to you and how they may affect your chances of a successful pregnancy.
Clinical trials
Explore Mayo Clinic studies of tests and procedures to help prevent, detect, treat or manage conditions.
By Mayo Clinic Staff
Related
Products & Services
In vitro fertilization (IVF): MedlinePlus Medical Encyclopedia
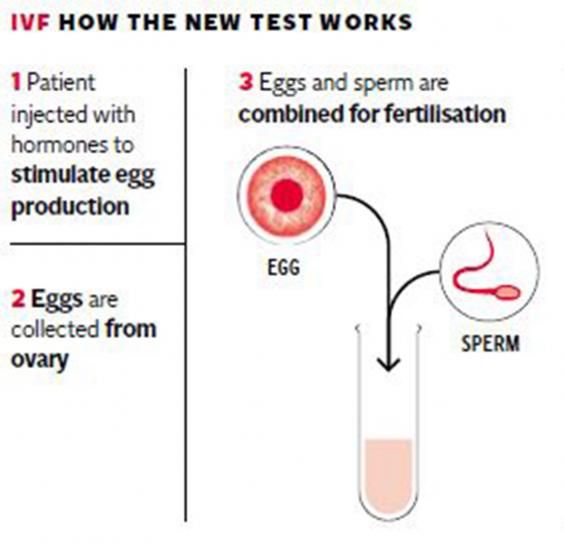
In vitro fertilization (IVF) is the joining of a woman's egg and a man's sperm in a laboratory dish. In vitro means outside the body. Fertilization means the sperm has attached to and entered the egg.
In vitro means outside the body. Fertilization means the sperm has attached to and entered the egg.
Normally, an egg and sperm are fertilized inside a woman's body. If the fertilized egg attaches to the lining of the womb and continues to grow, a baby is born about 9 months later. This process is called natural or unassisted conception.
IVF is a form of assisted reproductive technology (ART). This means special medical techniques are used to help a woman become pregnant. It is most often tried when other, less expensive fertility techniques have failed.
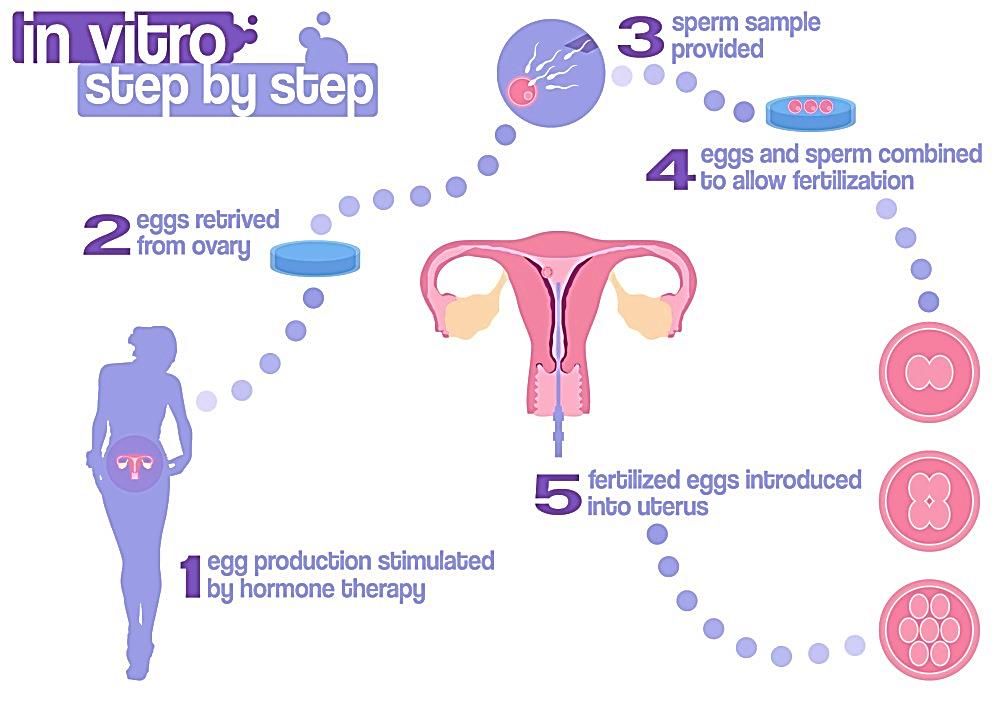
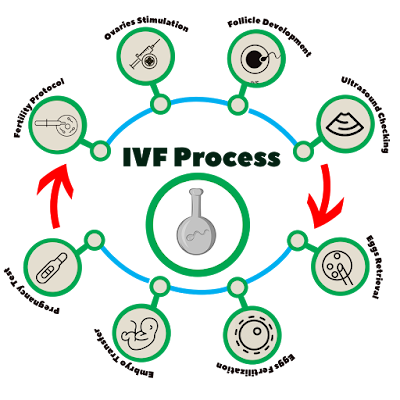
There are five basic steps to IVF:
Step 1: Stimulation, also called super ovulation
- Medicines, called fertility drugs, are given to the woman to boost egg production.
- Normally, a woman produces one egg per month. Fertility drugs tell the ovaries to produce several eggs.
- During this step, the woman will have regular transvaginal ultrasounds to examine the ovaries and blood tests to check hormone levels.
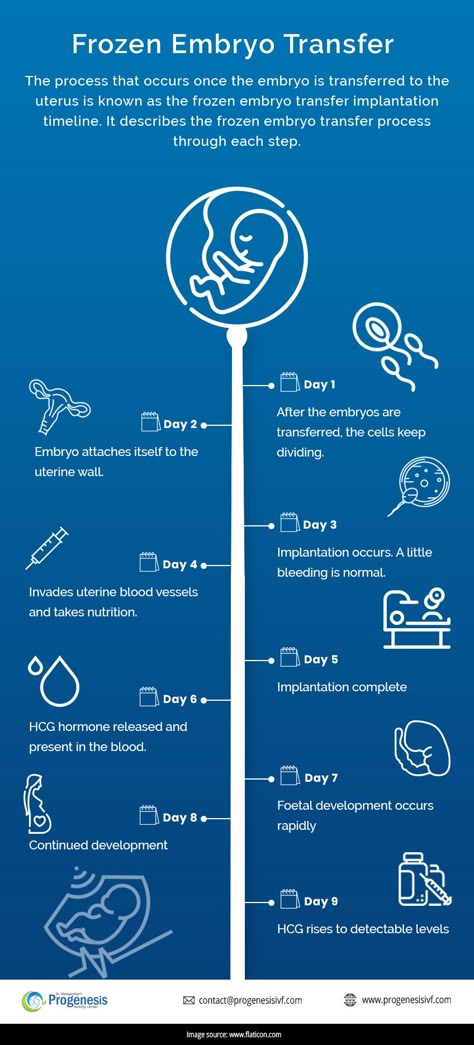
Step 2: Egg retrieval
- A minor surgery, called follicular aspiration, is done to remove the eggs from the woman's body.
- The surgery is done in the doctor's office most of the time. The woman will be given medicines so she does not feel pain during the procedure. Using ultrasound images as a guide, the health care provider inserts a thin needle through the vagina into the ovary and sacs (follicles) containing the eggs. The needle is connected to a suction device, which pulls the eggs and fluid out of each follicle, one at a time.
- The procedure is repeated for the other ovary. There may be some cramping after the procedure, but it will go away within a day.
- In rare cases, a pelvic laparoscopy may be needed to remove the eggs. If a woman does not or cannot produce any eggs, donated eggs may be used.
Step 3: Insemination and fertilization
- The man's sperm is placed together with the best quality eggs. The mixing of the sperm and egg is called insemination.
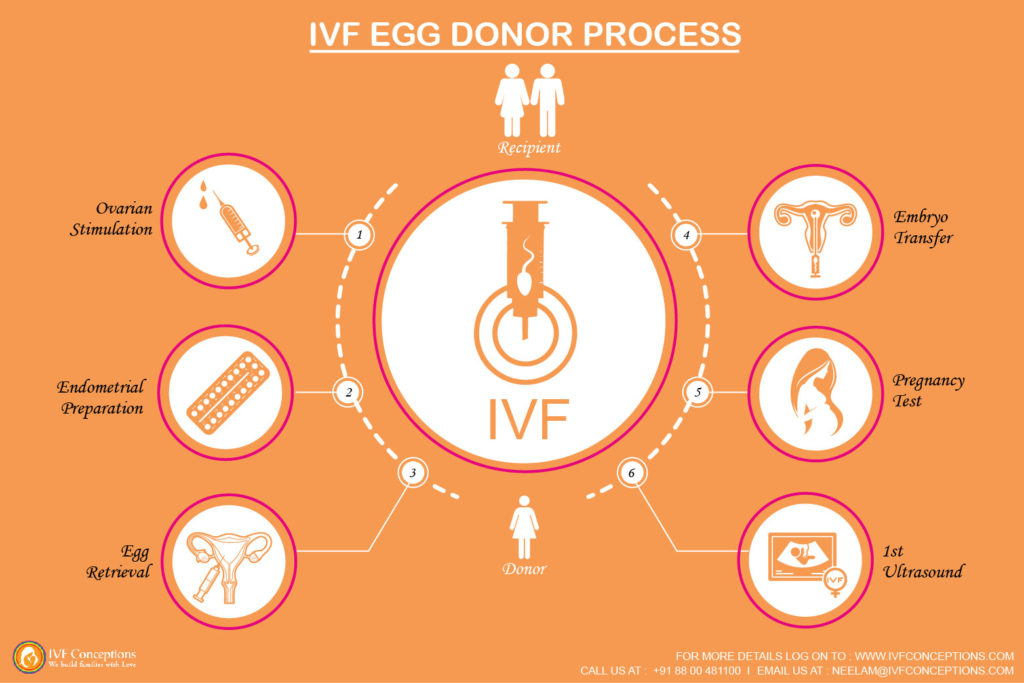
- Eggs and sperm are then stored in an environmentally controlled chamber. The sperm most often enters (fertilizes) an egg a few hours after insemination.
- If the doctor thinks the chance of fertilization is low, the sperm may be directly injected into the egg. This is called intracytoplasmic sperm injection (ICSI).
- Many fertility programs routinely do ICSI on some of the eggs, even if things appear normal.
Watch this video about:Intracytoplasmic sperm injection
Step 4: Embryo culture
- When the fertilized egg divides, it becomes an embryo. Laboratory staff will regularly check the embryo to make sure it is growing properly. Within about 5 days, a normal embryo has several cells that are actively dividing.
- Couples who have a high risk of passing a genetic (hereditary) disorder to a child may consider pre-implantation genetic diagnosis (PGD). The procedure is most often done 3 to 5 days after fertilization.
 Laboratory scientists remove a single cell or cells from each embryo and screen the material for specific genetic disorders.
Laboratory scientists remove a single cell or cells from each embryo and screen the material for specific genetic disorders. - According to the American Society for Reproductive Medicine, PGD can help parents decide which embryos to implant. This decreases the chance of passing a disorder onto a child. The technique is controversial and not offered at all centers.
Step 5: Embryo transfer
- Embryos are placed into the woman's womb 3 to 5 days after egg retrieval and fertilization.
- The procedure is done in the doctor's office while the woman is awake. The doctor inserts a thin tube (catheter) containing the embryos into the woman's vagina, through the cervix, and up into the womb. If an embryo sticks to (implants) in the lining of the womb and grows, pregnancy results.
- More than one embryo may be placed into the womb at the same time, which can lead to twins, triplets, or more. The exact number of embryos transferred is a complex issue that depends on many factors, especially the woman's age.

- Unused embryos may be frozen and implanted or donated at a later date.
IVF is done to help a woman become pregnant. It is used to treat many causes of infertility, including:
- Advanced age of the woman (advanced maternal age)
- Damaged or blocked fallopian tubes (can be caused by pelvic inflammatory disease or prior reproductive surgery)
- Endometriosis
- Male factor infertility, including decreased sperm count and blockage
- Unexplained infertility
IVF involves large amounts of physical and emotional energy, time, and money. Many couples dealing with infertility suffer stress and depression.
A woman taking fertility medicines may have bloating, abdominal pain, mood swings, headaches, and other side effects. Repeated IVF injections can cause bruising.
In rare cases, fertility drugs may cause ovarian hyperstimulation syndrome (OHSS). This condition causes a buildup of fluid in the abdomen and chest. Symptoms include abdominal pain, bloating, rapid weight gain (10 pounds or 4. 5 kilograms within 3 to 5 days), decreased urination despite drinking plenty of fluids, nausea, vomiting, and shortness of breath. Mild cases can be treated with bed rest. More severe cases require draining of the fluid with a needle and possibly hospitalization.
5 kilograms within 3 to 5 days), decreased urination despite drinking plenty of fluids, nausea, vomiting, and shortness of breath. Mild cases can be treated with bed rest. More severe cases require draining of the fluid with a needle and possibly hospitalization.
Medical studies have shown so far that fertility drugs are not linked to ovarian cancer.
Risks of egg retrieval include reactions to anesthesia, bleeding, infection, and damage to structures surrounding the ovaries, such as bowel and bladder.
There is a risk for multiple pregnancies when more than one embryo is placed into the womb. Carrying more than one baby at a time increases the risk for premature birth and low birth weight. (However, even a single baby born after IVF is at higher risk for prematurity and low birth weight.)
It is unclear whether IVF increases the risk for birth defects.
IVF is very costly. Some, but not all, states have laws that say health insurance companies must offer some type of coverage.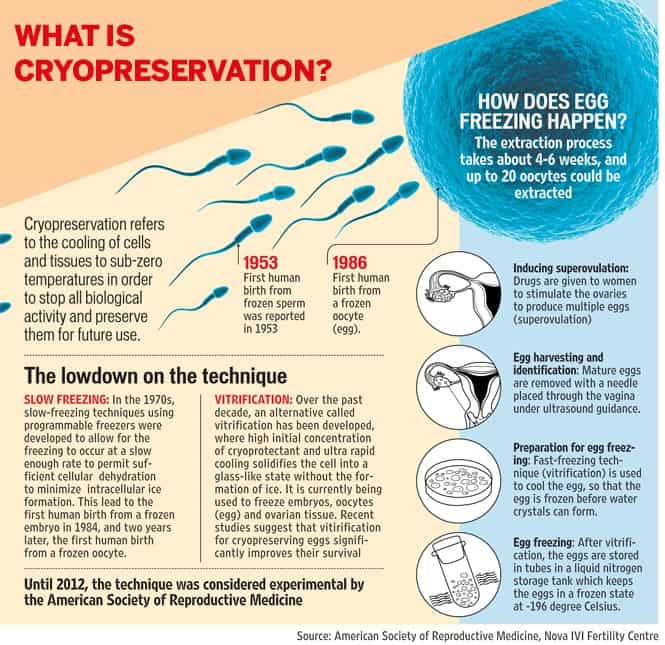 But, many insurance plans do not cover infertility treatment. Fees for a single IVF cycle include costs for medicines, surgery, anesthesia, ultrasounds, blood tests, processing the eggs and sperm, embryo storage, and embryo transfer. The exact total of a single IVF cycle varies, but may cost from approximately $12,000 to $17,000.
But, many insurance plans do not cover infertility treatment. Fees for a single IVF cycle include costs for medicines, surgery, anesthesia, ultrasounds, blood tests, processing the eggs and sperm, embryo storage, and embryo transfer. The exact total of a single IVF cycle varies, but may cost from approximately $12,000 to $17,000.
After embryo transfer, the woman may be told to rest for the remainder of the day. Complete bed rest is not necessary, unless there is an increased risk for OHSS. Most women return to normal activities the next day.
Women who undergo IVF must take daily shots or pills of the hormone progesterone for 8 to 10 weeks after the embryo transfer. Progesterone is a hormone produced naturally by the ovaries that prepares the lining of the uterus (womb) so that an embryo can attach. Progesterone also helps an implanted embryo grow and become established in the uterus. A woman may continue to take progesterone for 8 to 12 weeks after becoming pregnant. Too little progesterone during the early weeks of pregnancy may lead to miscarriage.
About 12 to 14 days after the embryo transfer, the woman will return to the clinic so that a pregnancy test can be done.
Contact your provider right away if you had IVF and have:
- A fever over 100.5°F (38°C)
- Pelvic pain
- Heavy bleeding from the vagina
- Blood in the urine
Statistics vary from one clinic to another and must be looked at carefully. However, patient populations are different in each clinic, so reported pregnancy rates cannot be used as an accurate indication of one clinic being preferable to another.
- Pregnancy rates reflect the number of women who became pregnant after IVF. But not all pregnancies result in a live birth.
- Live birth rates reflect the number of women who give birth to a living child.
Outlook of live birth rates depend on certain factors such as mother age, prior live birth, and single embryo transfer during IVF. Success rates have changed over the years in part due to the increasing use of single embryo transfers. IVF clinics have encouraged single embryo transfers to reduce the risk of twin pregnancies, which have higher risk for complications than singleton pregnancies. Embryos not transferred may be frozen and saved. The cycles in which those frozen embryos are thawed and transferred are called frozen embryo transfer cycles (FET).
IVF clinics have encouraged single embryo transfers to reduce the risk of twin pregnancies, which have higher risk for complications than singleton pregnancies. Embryos not transferred may be frozen and saved. The cycles in which those frozen embryos are thawed and transferred are called frozen embryo transfer cycles (FET).
IVF; Assisted reproductive technology; ART; Test-tube baby procedure; Infertility - in vitro
Catherino WH. Reproductive endocrinology and infertility. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 223.
Forman EJ, Lobo RA. In vitro fertilization. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 41.
Practice Committee of the American Society for Reproductive Medicine and the Practice Committee for the Society for Assisted Reproductive Technologies. Guidance on the limits to the number of embryos to transfer: a committee opinion. Fertil Steril. 2021;116(3):651-654. PMID: 34330423 pubmed.ncbi.nlm.nih.gov/34330423/.
Fertil Steril. 2021;116(3):651-654. PMID: 34330423 pubmed.ncbi.nlm.nih.gov/34330423/.
Tsen LC. In vitro fertilization and other assisted reproductive technology. In: Chestnut DH, Wong CA, Tsen LC, et al, eds. Chestnut's Obstetrics Anesthesia. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 15.
Updated by: John D. Jacobson, MD, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.
IVF – we study the issue from a professional point of view
ECO... Often, these letters hide tears and hope, attempts and firm faith, and, of course, the great, all-encompassing happiness of long-awaited parenthood.
Experts with many years of experience at the GMS IVF Family Planning House Clinic, GMS IVF Medical Director, gynecologist-reproductologist Anna Morozova and leading embryologist, embryological laboratory doctor Kirill Ilyin, will help us to look “behind the scenes” of IVF from a professional point of view.
Posta-Magazine: Anna Vladislavovna, first of all, tell us: why IVF? Still, this is probably the most “difficult” specialization for a gynecologist ...
Anna Morozova: IVF for me is not only a favorite and interesting job, but also a choice determined by personal factors. I grew up in a family of doctors, and at the same time, the problem of infertility, unfortunately, also affected my relatives. When I witnessed how, after many years of trying, a miracle called IVF happened to them, their joy and happiness struck me to the very heart. Therefore, already in graduate school, I began to deal with IVF problems, and then defended a dissertation on this topic.
In addition, IVF is a specialty that makes me constantly develop, think, study, go through a long and sometimes difficult path with each couple... And at the same time, my field of activity gives a huge charge of happiness, positive emotions and sometimes even tears of joy, when my patients receive a positive pregnancy test.
IVF is perhaps one of the most rapidly developing technologies. Do you try to offer patients all the new methods or do you advocate reasonable conservatism?
The IVF field is really developing by leaps and bounds. But as a doctor, I am primarily motivated for a successful result. This is a matter not only of reputation, but also of my moral satisfaction and pleasure from work. Trying to keep up with the times and always offering patients all possible ways to solve their problems, we use only proven and legally allowed methods in our work. For me, the main priority is the health of patients and their trust in me and in our team of specialists.
Kirill Alexandrovich, you also did internships and participated in educational programs at foreign universities and clinics. Are there any fundamental differences between the European and Russian approaches to IVF?
Kirill Ilyin: I think that there is practically no difference. It is possible that technological breakthroughs occur earlier and more often in the West, but in Russia there is no less extensive practice of maintaining IVF protocols. Our doctors and patients have more opportunities, for example, when conducting donor programs.
Our doctors and patients have more opportunities, for example, when conducting donor programs.
In addition, clinics and laboratories that are now opening in Russia (in particular, GMS IVF) are immediately equipped with the latest equipment and have the most modern technologies.
In general, our task is to ensure that everything goes as naturally as possible, carefully and safely for patients, and ends with the birth of a healthy baby.
A. Morozova: I would also like to add that there is also a difference in approaches to managing patients. In the West, a patient comes to the clinic and gets to the doctor on duty, who today is responsible for one or another stage of the protocol. Rarely does one doctor lead a pair of "from and to".
Our patients are much more fortunate in terms of an individual approach! We put our whole soul into them, all our skills and talent, we go all the way together with the patients. Of course, this approach implies the personal responsibility of the doctor for everything that happens, his readiness to constantly be in touch. It may be difficult for us at some points, but such involvement is an undeniable advantage for our patients.
It may be difficult for us at some points, but such involvement is an undeniable advantage for our patients.
To what extent is IVF a team effort? Is it important to you which team leads a pair with you?
A. Morozova: Absolutely! As I said, the most important thing for me is a successful result and a happy couple. Therefore, I must fully trust the specialists with whom I work: from an embryologist to a nurse. I believe that the teamwork of professionals who love patients and root for them wholeheartedly is in many ways the key to successful IVF.
It should not be forgotten that before starting the protocol, a couple must undergo a certain list of tests and examinations, enshrined in a special order of the Ministry of Health, and receive a "go-ahead" for IVF from several different doctors. In addition, in complex cases, additional consultations may be needed.
This is a huge plus for me to work in a multidisciplinary clinic: we have all the necessary specialists, from a geneticist to a family doctor. We not only help the couple save time and effort, but also get conclusions, the competence of which we can be sure.
We not only help the couple save time and effort, but also get conclusions, the competence of which we can be sure.
Why did you decide to work with GMS ECO?
K. Ilyin: For me, GMS ECO is not only a team of really high-class specialists whom I can fully trust. This is a rare opportunity for a specialist to create something of his own and use all the accumulated knowledge and practice in rare and non-standard clinical situations. After all, IVF, especially at the embryological stage, is a lot of important, seemingly unobvious little things that are important to take into account correctly. This only comes with experience.
A. Morozova: I have been working at the GMS clinic for a long time and I was infected with the combination of sincerity and professionalism that I met here. For me, our clinic has really become a family one.
A lot of patients go through me, and I realized that most of them need humanity. When the doctor does not just do his narrow part of the work, but helps the couple in the broadest sense of the word.
I really believe that with the help of various IVF programs, almost any couple can be helped. And I want to emphasize once again that we are primarily focused on the result! We will achieve it, we will strive to solve the problems of each individual couple. And to achieve this goal, we will keep up with the times, use the latest equipment, and invite highly qualified specialists.
That is why we decided to make not just a clinic, but a Family Planning House. Although we cannot guarantee a 100% result, we will do everything in any case to help our couples and make them happy!
Source: posta-magazine.ru
How does IVF work?
The two main stages of in vitro fertilization are the cultivation of the embryo and its transfer to the uterine cavity. Otherwise, the set of diagnostic and therapeutic manipulations may be different depending on the indications for the procedure and the patient's health status.
Our clinic implements all types of IVF programs, including those that use donor material, and also offers surrogate mother services.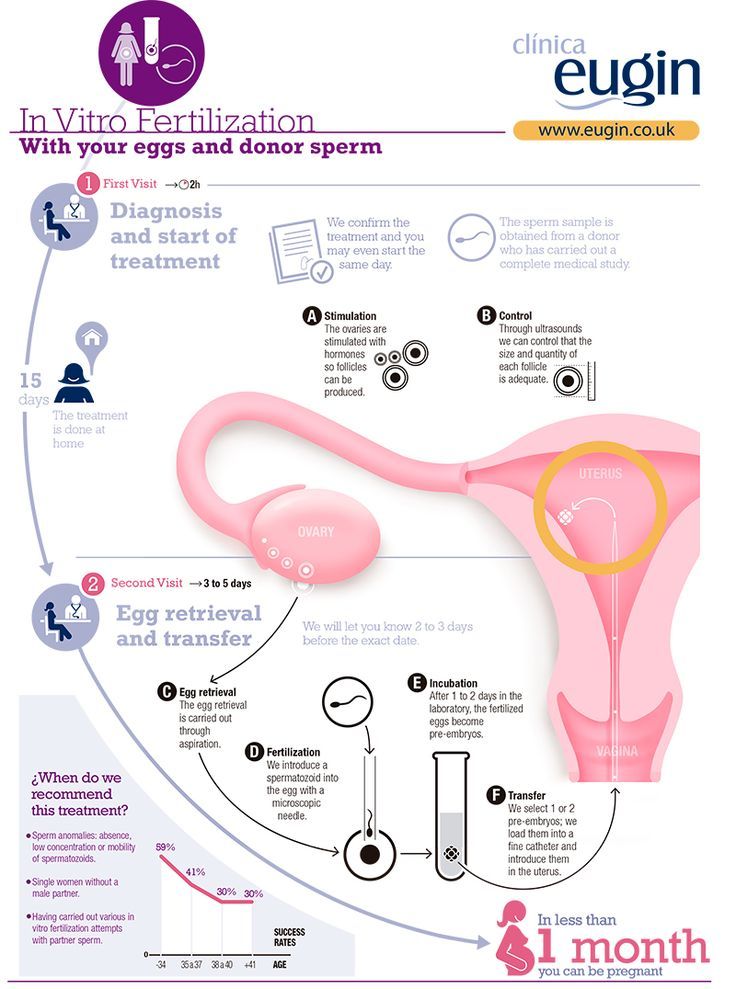
VIDEO TOUR TO THE CLINIC
Preparation for IVF
As a rule, IVF is recommended for couples who have an established diagnosis of "infertility" (with clarification of the factor or with an unclear genesis). For the first consultation with a reproductive specialist, it is recommended to bring all the results of the examinations with you.
Tests for a couple
Standard set of tests includes:
For both partners:
-
Tests for STIs (including HIV), viral hepatitis
-
Complete blood count, blood tests per group and Rh factor
3
-
Urinalysis
-
Fluorography
Additionally for a woman:
-
Pelvic ultrasound results
-
Ultrasound of the mammary glands (up to 35 years) or mammography (after 35 years)
-
Test for antibodies to the rubella virus, for TORCH infection
-
Hemostasiogram
-
estradiol, free T4, TSH (on the 2nd–3rd day of the cycle)
-
A smear for the flora from the urethra, vagina, cervical canal
-
The conclusion of the therapist that there are no contraindications to IVF and pregnancy
Additionally for men:
-
Spermogram (if necessary also MAP test), conclusion of an andrologist pipes, the opinion of the attending physician on chronic general diseases, etc.

0139
IVF has been performed all over the world for over 40 years. During this time, sufficient experience has been accumulated in order to be able to talk about contraindications on the part of women's health. But these contraindications do not apply to IVF as a whole, but only to individual stages. An obstacle to IVF can be:
- Oncological diseases (in case of remission, the decision to conduct IVF is made by the attending oncologist together with the reproductologist), severe cases of drug allergies: these conditions do not allow drug stimulation.
- Lack of a supply of eggs or the ovaries themselves (if they were removed) - in these cases, stimulation is also not carried out, since it does not make sense.
In the first case, an attempt to obtain an egg in a natural cycle is possible, in the second, a donor program is suitable.
- A number of common diseases in which the bearing and birth of a child is contraindicated (it does not matter if pregnancy occurs as a result of IVF or naturally).
 The inability to bear a child due to serious pathologies of the structure of the uterus or its absence.
The inability to bear a child due to serious pathologies of the structure of the uterus or its absence.
In this case, it is possible to conduct IVF together with the surrogacy program.
More about surrogacy
Recommendations for preparing for IVF
Main recommendations for the next month before IVF
reproductive physician.
First stage: consultation with a doctor and choice of protocol
At the first consultation, the reproductive specialist will see both future parents. Important information for the doctor is the duration of infertility, the presence of pregnancy attempts and IVF in the past, their outcome, and the results of examinations. These factors determine the choice of stimulation protocol, which is one of the most important conditions for obtaining high-quality eggs, and hence viable embryos.
Our specialists: obstetrician-gynecologists and reproductologists.
What option can the doctor offer based on the results of the appointment?
Additional procedures
According to the indications, the standard IVF program is supplemented with other procedures
Information about the cost of individual procedures and the formation of the full cost of the IVF program . The accumulated experience of working with embryos shows that more than 99% of them successfully tolerate conservation. The value of cryopreservation is that you can set the transfer date for any day in the following cycles, and not just when hormonal stimulation was performed. This allows you to choose the optimal moment in terms of the woman's well-being, as well as the condition of the endometrium. In case of failure, the next attempt does not require stimulation: it is enough to immediately go to the transfer stage, which is much easier physically for the woman and psychologically for both partners.

If, for example, 10 eggs are obtained during stimulation, 8 embryos are cultured and 6 are allowed for cryopreservation, this means that the transfer can be carried out 6 times in succession: this gives a very high chance of a successful pregnancy. In this case, the woman will have to undergo only one stimulation and one egg collection.
Preimplantation Diagnosis
Assisted Hatching
Sometimes unsuccessful IVF attempts can be due to the fact that the shell of the embryo becomes too dense. After the transfer, the embryo cannot break through it and gain a foothold in the uterine cavity, and after a few days it dies. The exact causes are unknown, but there is an assumption that the state of the embryonic membrane depends on the age of the mother.
To increase the chances of implanting the embryo in the uterine cavity, hatching is performed. Indications for it:
- Embryo transfer after cryopreservation.

- Mother's age over 38 years.
- Unsuccessful IVF attempts in the past.
Before transfer, the shell of the embryo is incised with a laser beam. A simple and quick procedure does not harm the embryo and increases the chances of a successful implantation.
Donor programs
Second stage: stimulation
The duration of drug stimulation depends on the selected protocol. The drugs are injected subcutaneously into the abdomen. As a rule, patients cope with this procedure at home. Injections can also be carried out in the treatment room free of charge if you purchase drugs in the pharmacy of our clinic.
Medications are generally well or satisfactorily tolerated. Before the start of stimulation, the doctor recommends a daily regimen and diet that contribute to good health and a favorable course of stimulation. In rare cases (approximately 1%), patients experience ovarian hyperstimulation syndrome (OHSS).
 This condition requires a visit to the attending physician. The doctor will also warn you about the symptoms that you need to pay attention to.
This condition requires a visit to the attending physician. The doctor will also warn you about the symptoms that you need to pay attention to. IVF sick leave
All patients are entitled to a sick leave for in vitro fertilization. The sick leave is opened on the first day of stimulation and is valid until the day of diagnosis of pregnancy (or until its exclusion in case of failure) - this is the 14th day after the embryo transfer.
Reason: Order of the Ministry of Health and Social Development of the Russian Federation dated June 29, 2011 No. 624n “On Approval of the Procedure for Issuing Certificates of Incapacity for Work”.
If desired, the patient can do without a sick leave if the work schedule allows her to visit the clinic. If you feel well, you can continue to work during stimulation and after the transfer, if the work is not associated with serious stress, stress.
The third stage: obtaining eggs and embryos
This is an important and responsible stage, which completes the stimulation.
 With the help of ultrasound, the process of maturation of the follicles is monitored. Based on the results of the ultrasound, the doctor prescribes the optimal day for egg collection. 36 hours before the planned puncture, an injection of hCG (human chorionic gonadotropin) is prescribed - this is necessary to complete the process of maturation of the follicles.
With the help of ultrasound, the process of maturation of the follicles is monitored. Based on the results of the ultrasound, the doctor prescribes the optimal day for egg collection. 36 hours before the planned puncture, an injection of hCG (human chorionic gonadotropin) is prescribed - this is necessary to complete the process of maturation of the follicles. 1
Puncture and collection of mature follicles
The procedure is performed under general anesthesia (medicated sleep) and lasts up to 30 minutes. In the evening before the operation, you should have dinner no later than 18 hours, after which you should refrain from eating (to reduce the risk of nausea and vomiting during anesthesia).
Egg retrieval is done with a needle inserted into the ovary through the vaginal wall (under ultrasound guidance). After completion of the procedure, the patient needs to spend about 2 hours in the ward under the supervision of a doctor. On the same day, the spouse undergoes a sperm donation procedure (if it has not been performed earlier). The reproductologist will report the results of the puncture (how many follicles were obtained), prescribe the estimated transfer time if it is planned to be carried out in the same cycle. After that, if the woman has no complaints about her well-being, the couple can go home.
The reproductologist will report the results of the puncture (how many follicles were obtained), prescribe the estimated transfer time if it is planned to be carried out in the same cycle. After that, if the woman has no complaints about her well-being, the couple can go home.
After the puncture, there may be slight pain in the abdomen, small bleeding, drowsiness. These symptoms do not cause concern and do not require a visit to a doctor. With an increase in temperature of more than 37 degrees, heavy bleeding, sharp pains in the abdomen, severe bloating, you should urgently contact your fertility doctor.2
Fertilization
The liquid medium obtained during the puncture (follicular liquid) is sent to the embryological laboratory, where the embryologist extracts mature follicles from it. For several hours, the follicles are in the incubator. Then the sperm is prepared (received on the same day or earlier and located in the cryostorage). If the male factor of infertility is absent (spermogram parameters are normal), then the follicles and prepared (purified) sperm are placed in a nutrient medium in conditions close to natural. Within 16–18 hours, fertilization and the formation of a zygote occur.
Within 16–18 hours, fertilization and the formation of a zygote occur. 3
ICSI
If male factor infertility has been established, the fertility specialist may recommend fertilization using the ICSI procedure. If for normal fertilization you need about 50 thousand mobile healthy spermatozoa per 1 egg, then only one is enough for ICSI. This method is used if spermatozoa are obtained by testicular puncture (for example, with impaired patency of the seminiferous tract). With the help of a microneedle under the control of a microscope, the spermatozoon is injected into the egg. After that, the process of maturation of the resulting zygote proceeds as usual.Cultivation, diagnosis and preservation of embryos
After fertilization
The day of puncture and fertilization is considered “zero”, the next day is the first. Embryos are grown for 3-5 days. After that, their condition is evaluated according to several criteria: “excellent”, “good”, “satisfactory”.

According to indications, preimplantation diagnostics of embryos is carried out. The procedure has two tasks:
- Detection of genetic and chromosomal diseases, which are considered the most common and can occur even in apparently healthy people.
- Diagnosis of those genetic diseases, the genes of which are reliably present in the parents.
Cryopreservation
Vitrification is a method of freezing living tissues. Its fundamental difference from simple cryopreservation is that a special gel-like medium is used, which has a structure different from water. This medium replaces water in tissue cells. After being placed in liquid nitrogen (temperature is -196 ° C), freezing takes place without the formation of water crystals, which means that the cells of the embryos are not damaged. Vitrification preserves the embryos so that approximately 99% of them successfully endure the thawing process. This method has helped improve the effectiveness of IVF programs.
 Therefore, in most cases, fertility doctors recommend cryopreservation and transfer in another cycle.
Therefore, in most cases, fertility doctors recommend cryopreservation and transfer in another cycle. Embryos are placed one or two on special straws. They are marked: indicate the full name of the patients and the number of the medical record. In parallel, records are kept in a special laboratory journal, which eliminates errors. After that, the straws are placed in a vessel with liquid nitrogen and sent to the clinic's cryostorage. The period of preservation of embryos is calculated in years (today there are known cases of the birth of children 20 or more years after the cultivation of the embryos).
Our cryobank
Embryo transfer
This is the final stage of IVF. Even at the first appointment, the reproductive specialist, together with the patients, decides whether to carry out the transfer in the same cycle or not. If there are no contraindications on the part of the health and well-being of the woman and the condition of the endometrium allows you to count on the successful attachment of the embryo, this is possible.
 Then the day of transfer is tied to the day of puncture (“zero”): embryos are transferred from 3 to 5 days old.
Then the day of transfer is tied to the day of puncture (“zero”): embryos are transferred from 3 to 5 days old. If the patient has had OHSS or complications after puncture, if the endometrium requires drug preparation, then it is preferable to transfer all received embryos to storage and set the day of transfer in another cycle. This will allow you to take a break from procedures and medication, restore good health.
Transfer one or more embryos?
15–20 years ago, the survival rate of embryos was much lower, and then the transfer of several embryos (up to 4–6) was practiced. In the event that more embryos took root than the couple was ready to bear, it was necessary to resort to the reduction procedure (one or more embryos were removed at an early stage). Such a procedure is not only fraught with complications for the embryos that need to be preserved, but also difficult from a psychological and ethical point of view.
Now the effectiveness of the programs is quite high, so the transfer of only one embryo has become optimal.
 Even if the couple is ready to carry twins, any multiple pregnancy is a risk to the health of the woman and children. Most multiple pregnancies end prematurely and often require inpatient care. In addition, there is always a risk that the embryo will divide into two in the first days after the transfer (this is a process similar to the natural conception of identical twins). When transferring two embryos, this option can lead to triplets. Therefore, now the main tactics of fertility doctors is as follows:
Even if the couple is ready to carry twins, any multiple pregnancy is a risk to the health of the woman and children. Most multiple pregnancies end prematurely and often require inpatient care. In addition, there is always a risk that the embryo will divide into two in the first days after the transfer (this is a process similar to the natural conception of identical twins). When transferring two embryos, this option can lead to triplets. Therefore, now the main tactics of fertility doctors is as follows: - In most cases, it is advised to transfer only one embryo.
- If the couple wishes and if there are no contraindications from the woman's health, transfer two embryos, but no more.
Preparing for transfer
How does the transfer work?
Recommendations after the transfer
Pregnancy diagnosis
Final step: On the 14th day after the transfer, a pregnancy test can be done at home.
 The doctor usually also prescribes a blood test for hCG and ultrasound. With a successful attachment of the embryo, as a rule, it is already possible to diagnose pregnancy.
The doctor usually also prescribes a blood test for hCG and ultrasound. With a successful attachment of the embryo, as a rule, it is already possible to diagnose pregnancy. In case of failure
If pregnancy does not occur, the procedure for the next IVF depends on whether the couple has embryos stored in the cryobank. If not, all stages are repeated from the beginning (from stimulation), if necessary, the couple undergoes additional examinations. If there are embryos, a new transfer can be scheduled in the next cycle or, if necessary, later.
Our prices
Own eggs and sperm programs
Treatment of a nonsense by VTR
Primary technique Genetics2.500 ₽
Repeat - 2.000 ₽
Classical program ECO140.800 ₽
Controlled stimulation of the ovaries, general anesthesia, follicles, fertilization, fertilization of embryos, embryo cultivation, and postponement of embryo into the uterine cavity
IVF+ICSI172.
 700 ₽
700 ₽ Controlled ovarian stimulation, general anesthesia, follicle puncture, ICSI fertilization, embryo cultivation, embryo transfer into the uterine cavity
Repeat IVF program120.800 ₽
Controlled ovarian stimulation, general anesthesia, follicle puncture, IVF fertilization, embryo culture, embryo transfer into the uterine cavity
IVF with ICSI in natural cycle97.800 ₽
900 in natural cycle, ICSI egg fertilization, embryo culture and transferIVF with minimal stimulation106.300 ₽
Controlled ovarian stimulation, general anesthesia, follicle puncture, ICSI egg fertilization, embryo culture and transfer
IVF with low AMH (embryo banking)99.500 ₽
General anesthesia, follicle puncture, fertilization of eggs in a natural cycle by ICSI, cultivation and vitrification of embryos, storage for six months in a cryobank
donor oocytes or fresh donors
IVF program with 6 donor eggs 217.800 ₽
Selection of a donor according to 70 parameters from the cryobank, 6 donor oocytes, IVF fertilization, embryo cultivation, embryo transfer
Oocyte donation program
(with 12 oocytes provided) donor oocytes and spermDonor embryo program99.