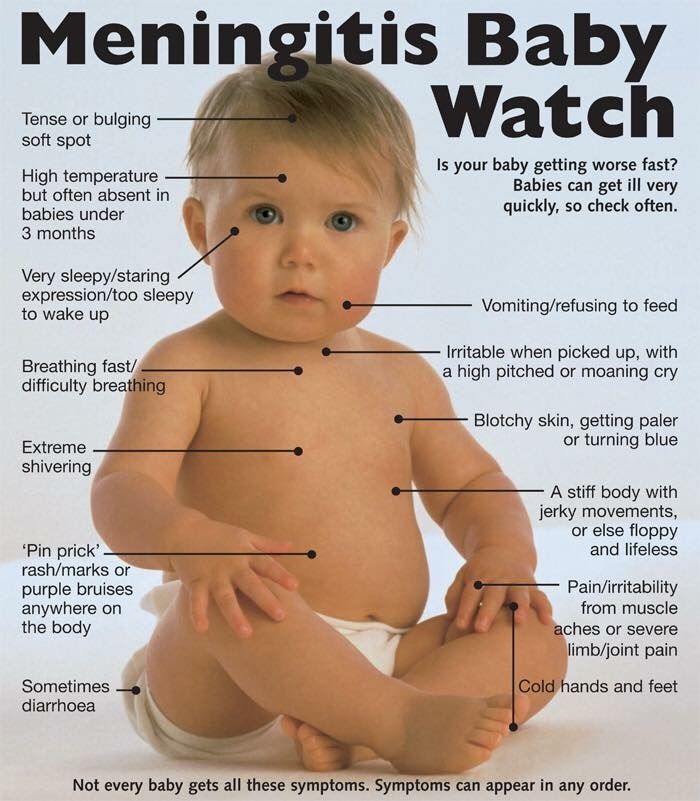
Meningitis rash chest
Meningitis Rash: Pictures, Symptoms, and More
Meningitis is a swelling of the membranes of the brain and spinal cord. It can be due to viral, fungal, or bacterial infection.
The most common cause of meningitis is a viral infection. But bacterial meningitis is one of the most dangerous forms of the disease.
Symptoms generally occur within 1 week after exposure and include:
- fever
- feeling ill
- headache
Not everyone develops every symptom. But they may develop a distinctive skin rash. In this article, we take a closer look at what that skin rash may look like, as well as other notable symptoms.
See a doctor if you think you or a loved one may have developed meningitis. This infection can be life threatening.
A meningitis skin rash is a distinct symptom of this serious illness. However, a skin rash doesn’t always appear in the early stages of meningitis, and when it does, it starts as small pinpricks on the skin before spreading into larger blotches.
Large, dark or purple rashes may indicate a related bloodstream infection called septicemia.
In these images, we show how an early meningitis skin rash begins and what it looks like as the illness progresses.
A meningitis rash may look similar to other skin rashes. However, what sets a meningitis-related rash apart from other skin symptoms is the presence of other symptoms, such as fever and stiff neck.
The glass test
One sign of meningococcal septicemia is that the rash doesn’t fade when you apply pressure to the skin. You can test this by pressing the side of a clear drinking glass against the skin.
If the rash looks like it fades, check periodically for changes. If you can still see the spots clearly through the glass, it may be a sign of septicemia, especially if you also have a fever.
The glass test is a good tool, but it’s not always accurate. Meningitis is a life threatening illness so it’s important to get medical attention if you have any symptoms.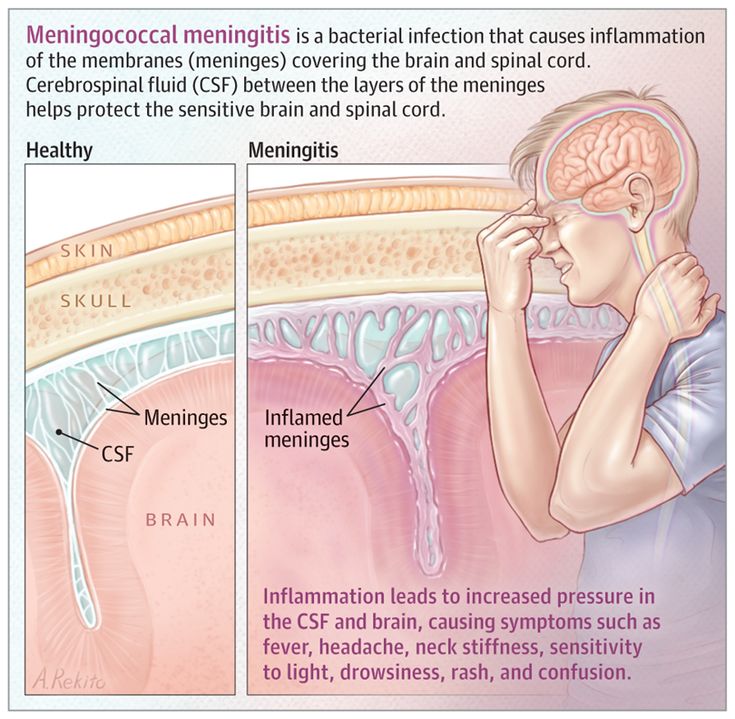
Other causes of skin rashes that appear like pinpricks or large, bruise-like blotches may include:
- Petechial rash. This leads to pinpoints in skin that look like tiny bruises. They’re typically less than 2 millimeters in size. Petechiae may develop on the skin or in mucous membranes from a variety of diseases, including meningitis, leukemia, and idiopathic thrombocytopenia (ITP).
- Vasculitis skin rashes. These rashes can cause petechiae or larger bruises. This rash may also cause itchy hives. Vasculitis is caused by an inflammation in the blood vessels and may also lead to other symptoms, such as fever, fatigue, and muscle pain.
- Purpura. These lesions may look like bruises but are larger than petechiae. Purpura rashes may be caused by a variety of conditions, such as vascular, platelet, and coagulation disorders.
- Hives (urticaria). These pale or dark and often itchy welts are common and may result from allergies, infections, and vascular diseases.

The symptoms of a meningitis infection in children are similar to those in adults. In addition to a possible rash, here’s what you might see during the early and later stages of this illness in children.
Early warning signs
Meningococcal bacteria reproduce in the bloodstream and release poisons (septicemia). As the infection progresses, blood vessels can become damaged.
This can cause a faint skin rash that looks like tiny pinpricks. The spots may be pink, red, or purple. In the early stages, these symptoms may be dismissed as a scratch or mild bruising. The skin may simply look blotchy and can appear anywhere on the body.
In addition to a meningitis rash, other symptoms of a meningococcal infection may include:
- fever
- a stiff neck
- nausea or vomiting
- confusion
- sensitivity to light (photophobia)
A worsening rash
As the infection spreads, the rash becomes more obvious. More bleeding under the skin may cause the spots to turn dark red or deep purple.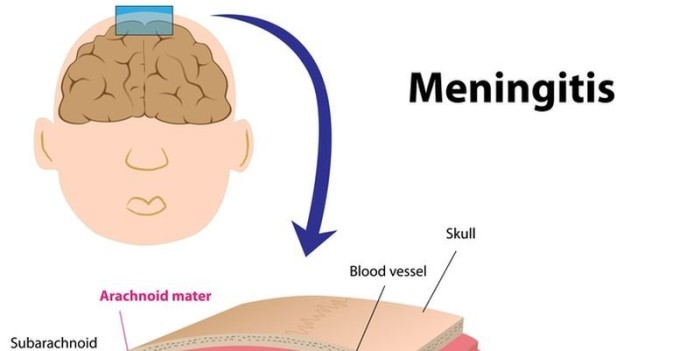 The rash may resemble large bruises.
The rash may resemble large bruises.
It’s harder to see the rash on darker skin. If you suspect meningitis, check lighter areas like the palms, eyelids, and inside the mouth.
Also, not everyone with meningitis develops a rash.
Tissue damage as the rash spreads
As the condition advances, the rash spreads and continues to darken. Blood vessel damage causes blood pressure and circulation to fall.
Because the limbs are at the far reaches of the circulatory system, a system-wide decrease in blood pressure leads to inadequate oxygen delivery, especially in the limbs. This can injure tissue and lead to permanent scarring.
Plastic surgery and skin grafting may be able to improve function after the illness passes. In severe cases, it becomes necessary to amputate fingers, toes, arms, or legs. Rehabilitative services may be helpful in those cases, but recovery could take years.
Anyone can get meningitis, but infants and children are at particular risk because they may not have fully developed immune systems, especially if they come in close contact with other children who have meningitis.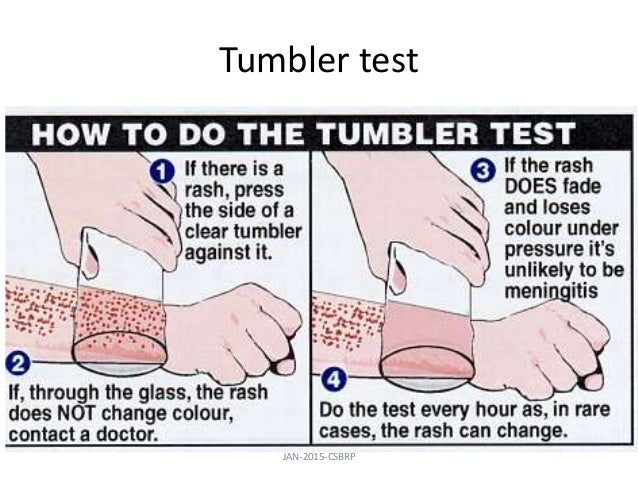
While the symptoms of meningitis are similar to those in adults, this infection may cause different symptoms in infants. Rather than causing the more classic symptoms, babies who have meningitis may display the following.
Abnormal arching in head, neck, and spine
Neck pain and stiffness are common symptoms of meningitis. It can sometimes cause the head, neck, and spine to become rigid and arch backward (opisthotonos). Infants may also exhibit widespread body stiffness and have jerky, or floppy movements.
Skin rash
Early in the course of infection, infants’ skin sometimes develops a yellow, blue, or pale tone. Like adults, they may also develop blotchy skin or a pinprick rash.
As the infection progresses, the rash grows and darkens. Lesions or blood blisters may form. The infection can spread quickly.
Seek medical attention if your infant has a fever with a rash.
Bulging fontanel
Another sign of meningitis concerns the soft spot on top of a baby’s head (fontanel).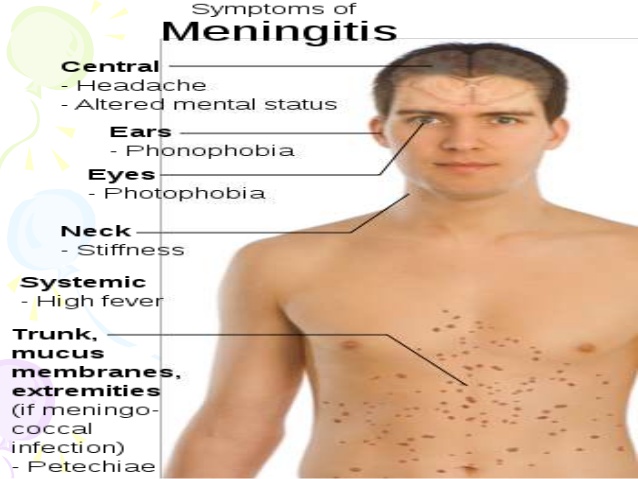 A soft spot that feels tight or forms a bulge could be a sign of swelling in the brain.
A soft spot that feels tight or forms a bulge could be a sign of swelling in the brain.
Always contact your doctor if you see bumps or bulges on your infant’s head. Meningitis can be a very serious illness even if your baby doesn’t develop septicemia.
Other symptoms in infants
In addition to the above symptoms, other signs of meningitis seen in infants may include:
- breathing difficulties
- rapid breathing
- extreme drowsiness
- diarrhea
- extreme shivering
- crying or irritability when being picked up due to pain
- cold hands and feet
- refusing to eat
- vomiting
If your baby exhibits any of these symptoms, it’s important to seek emergency medical help right away. A meningitis infection may spread quickly, and prompt treatment reduces the risk of complications.
Meningitis symptoms in adults are largely the same as those in children.
In addition to the most common symptoms of meningitis, you should look out for signs of septicemia.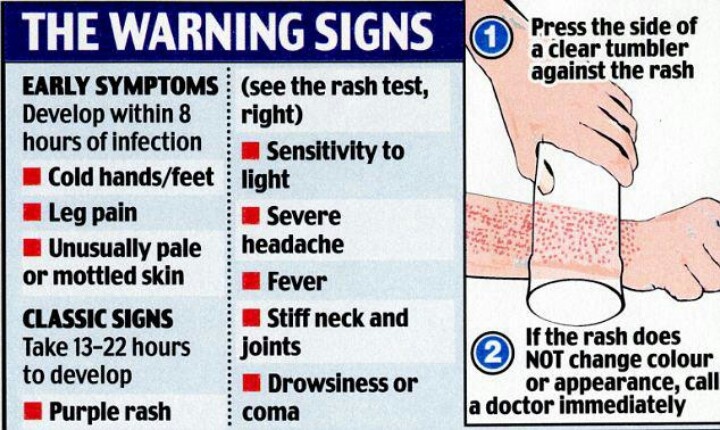 Seek emergency medical help if you also experience:
Seek emergency medical help if you also experience:
- rash that gets larger
- a fever accompanied by cold hands and feet
- severe muscle pain
- vomiting
- severe headache
- extreme drowsiness
- confusion and irritability
- severe stiff neck
- convulsions or seizures
Meningitis can happen at any age, but infants, children, and young adults are at a higher risk, as well as older adults. The disease is also more likely to spread in areas of close quarters, such as day care centers, nursing homes, and college dorms.
Additionally, having certain medical conditions like HIV may increase your risk of developing a meningitis infection, due to a weakened immune system. Chemotherapy treatments and immunosuppressants may also increase your risk.
Infants younger than 1 month old are also more likely to experience severe illness from an underdeveloped immune system.
Vaccines can help prevent some, but not all, types of meningitis. Early diagnosis and treatment can help you avoid complications and potential long-term effects.
Early diagnosis and treatment can help you avoid complications and potential long-term effects.
While early diagnosis and treatment can help you avoid complications and potential long-term effects, vaccination may also help prevent certain types of meningitis.
Currently, vaccines are available for bacterial meningococcal disease, the most serious type of meningitis. This is a two-dose series, typically administered around age 11 or 12, and then at the age of 16. These vaccines help prevent Neisseria meningitidis bacteria from causing meningitis.
There’s currently no vaccine to help prevent viral meningitis infections. However, the Centers for Disease Control and Prevention (CDC) outlines other types of routine vaccinations may offer some protection against viral meningitis, including those for chickenpox, influenza, and measles.
Besides vaccines, you can help prevent contracting the virus or bacteria that causes meningitis by washing your hands often, regularly disinfecting common surfaces, and avoiding others who may be sick.
It’s also important to prevent the spread of this illness to others. If you or your child are sick, stay home until your doctor says it’s OK to go back to work or school.
Vaccine recommendations
Children ages 11 or 12 should receive a meningococcal vaccine (MenACWY) vaccine, followed by a booster dose at age 16.
Vaccination is also recommended for teens ages 13 to 18 who did not receive this vaccine when they were younger. Talk with your child’s pediatrician about their recommendations for your child. Children who are at increased risk due to certain medical conditions may need additional boosters.
If you’re unsure whether you received a meningococcal vaccine as a child, talk with your doctor. You may still be able to get vaccinated as an adult to protect yourself against this serious illness.
A meningitis rash is a serious sign that a meningitis infection has developed and possibly spread. This distinct rash may start as small pinpricks but rapidly develop into larger blotches over your entire body.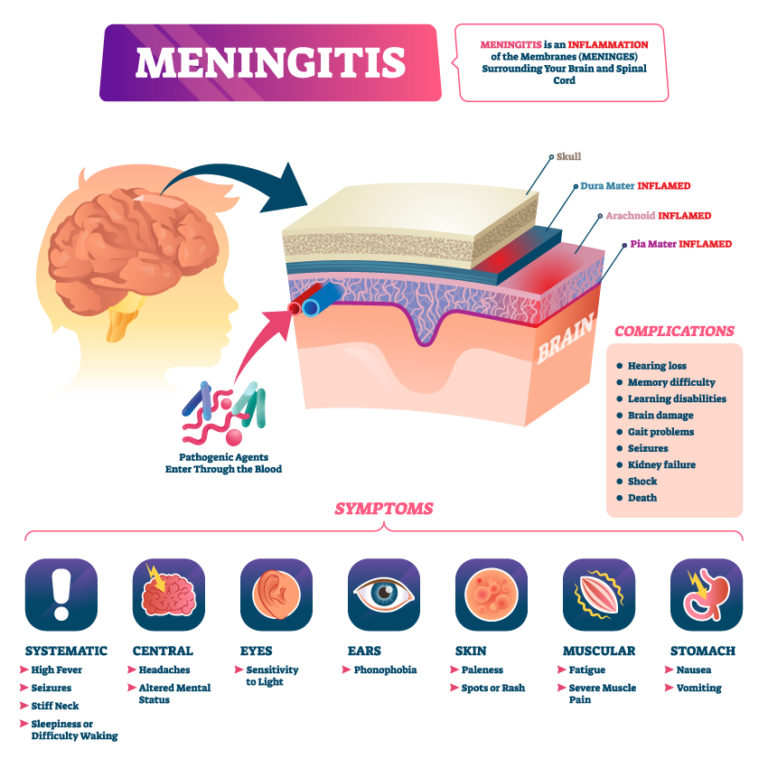 The appearance of the rash is similar across all age groups.
The appearance of the rash is similar across all age groups.
However, not everyone with meningitis experiences a rash. This is why it’s important to pay attention to other possible symptoms of meningitis, such as fever, headache, stiff neck, and photosensitivity.
Infants may also have bulging soft spots on their heads, along with unexplained fussiness and floppy movements.
If you suspect that you or your child has meningitis, seek emergency medical care right away.
Pictures, symptoms, and similar rashes
Meningitis causes a characteristic rash on the skin. Learning to spot this and other symptoms can help a person receive the right treatment fast.
Meningitis is an infectious disease caused by certain viruses, bacteria, or fungi. It causes swelling of the meninges, the protective coverings of the brain and spinal cord. The most serious type of meningitis is caused by a bacterium called Meningococcus.
The disease can be life-threatening, and it requires immediate medical attention.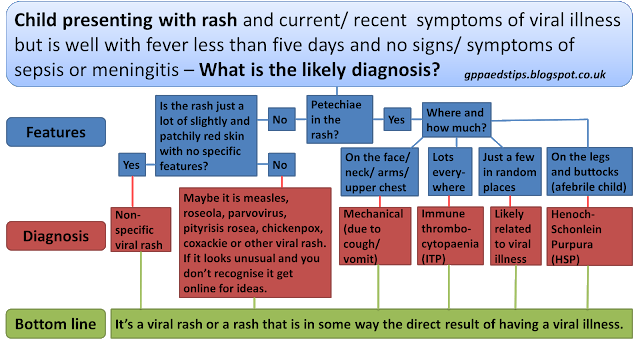
In this article, we describe how to spot a meningitis rash. We provide a picture guide, explore other meningitis symptoms, and discuss similar conditions.
Meningitis causes a variety of symptoms, including a distinctive rash. This is not a traditional rash, caused by irritation or inflammation. Instead, it results from bleeding under the skin.
The bleeding develops after the disease has progressed to cause blood poisoning. The medical term for this is meningococcal septicemia. It leads to broken blood vessels, giving the appearance of a rash.
A doctor may refer to this as a meningitis rash or a “petechial” rash.
A rash caused by bacterial meningitis may have these characteristics, regardless of the person’s age:
- tiny red, pink, brown, or purple “pinprick marks,” called petechiae, on the skin
- purple bruise-like marks
- blotchy areas of skin
- pale or mottled areas of skin
The meningitis rash may be less apparent on darker skin tones.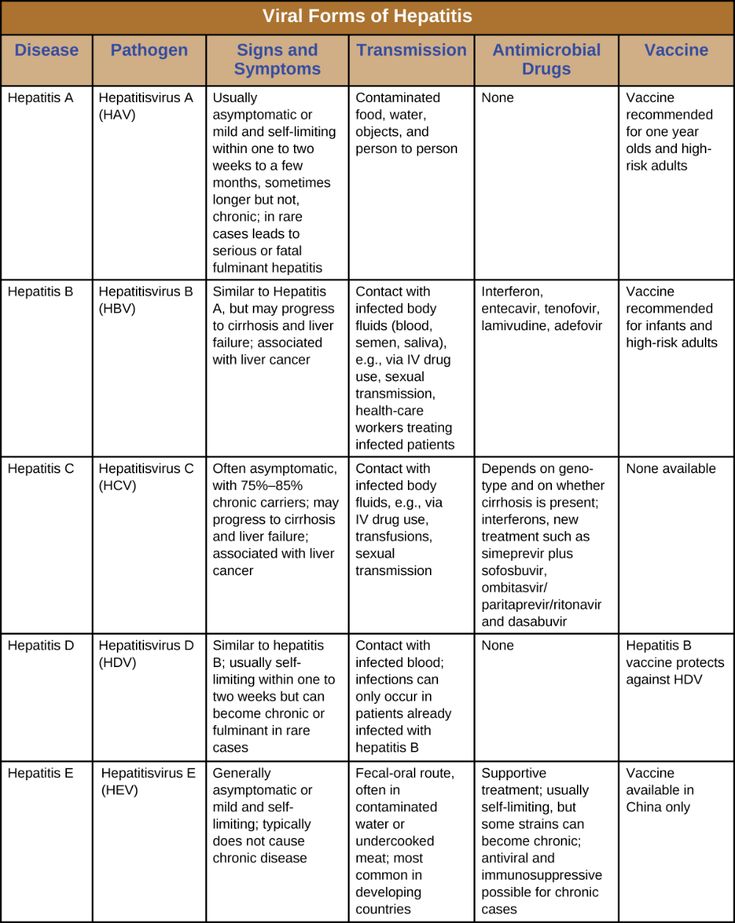
The rash can appear anywhere on the body, and it may be easier to see on paler parts of the body, such as the palms of the hands or the soles of the feet.
Usually, the rash is not raised, so the skin is unlikely to feel rough or bumpy.
At first, the rash may be subtle, but it can spread to larger areas of skin. The rash may also become darker over time, as the body reabsorbs blood cells.
The rash usually occurs in the later stages of meningitis, when the disease is more serious.
It is crucial to seek medical care for any symptoms of meningitis, even if no rash is present. Receiving quick treatment greatly increases the chances of recovery.
Other types of meningitis produce other rashes. If a person has any rash and any symptoms of meningitis, they should receive medical care right away.
The glass test can help a person tell whether their rash may result from meningitis.
While it is not a reliable way to diagnose any disease, this test can help a person decide whether to go to the emergency room.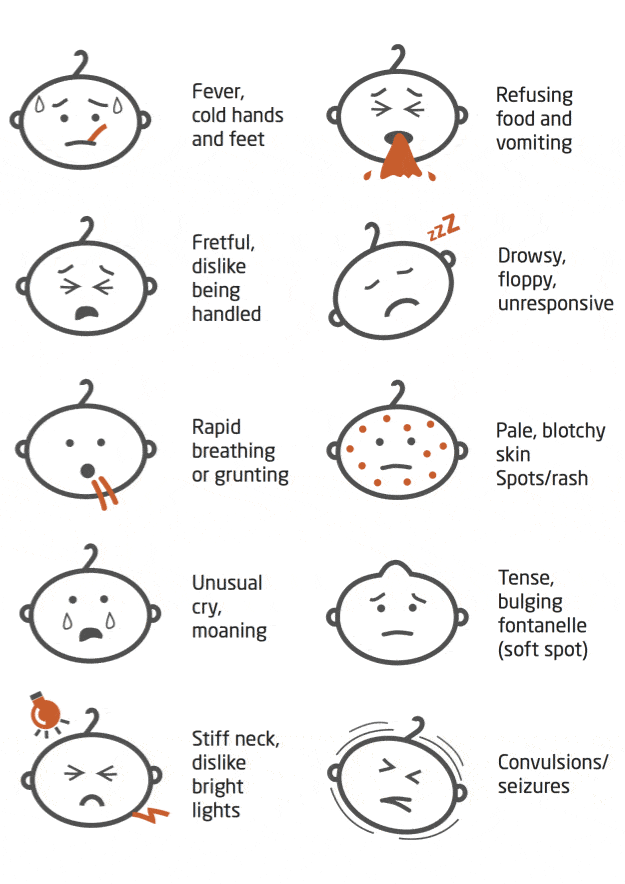
Press a clear drinking glass against the rash. If the marks are still visible, even with pressure, seek medical care immediately.
This is a sign that the rash is petechial, meaning that it results from meningitis or other serious illnesses that cause bleeding.
A meningitis rash can be difficult to see, especially on darker skin tones. Try the glass test on areas of rash that are easier to reach, such as the trunk or limbs, and lighter areas, such as the palms of the hands and the bottoms of the feet.
This test is not a surefire method of determining who needs medical care. Anyone with any meningitis symptoms should receive medical attention right away, even if their rash fades with pressure under the glass.
Anyone can get meningitis. In the United States, rates are highest in infants younger than 1 year, according to the Centers for Disease Control and Prevention (CDC).
Infants with meningitis can have a variety of symptoms, including:
- a fever
- shivering
- a stiff neck
- arching of the back
- cold hands and feet
- turning away from light
- excessive irritability, such as a dislike of being picked up
- intense lethargy, an inability to wake up, or both
- a bulging fontanel, which is the soft spot on the head
- a refusal to eat
- vomiting or diarrhea
The symptoms do not appear in any order.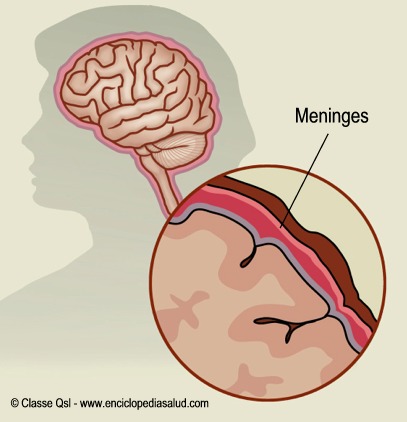 If a baby, or anyone, has any meningitis symptoms, they need medical attention.
If a baby, or anyone, has any meningitis symptoms, they need medical attention.
If meningitis progresses to septicemia, a rash or unusual skin coloration may develop. This can happen within hours, as meningitis often progresses quickly.
Share on PinterestImage credit: Stephen Kelly, 2019
Teens and young adults have a higher risk of meningitis than middle-aged or older adults. The National Meningitis Association reports that 21% of all cases develop between the ages of 11 and 24.
Symptoms of meningitis in teens and adults include:
- a severe headache
- sensitivity to light
- a stiff neck that is painful to move
- abdominal pain
- aches or muscle pain
- a fever
- double vision
- mental changes, including confusion
- vomiting
- seizures
Share on PinterestImage credit: Stephen Kelly, 2019
Doctors can diagnose meningitis by performing one or more medical tests, such as:
- a physical exam to check the symptoms
- blood tests
- urine tests
- a test of spinal fluid, which surrounds and protects the brain and spinal cord
- a CT scan
- an MRI scan
If a person tests positive for bacterial meningitis, the doctor will prescribe antibiotics.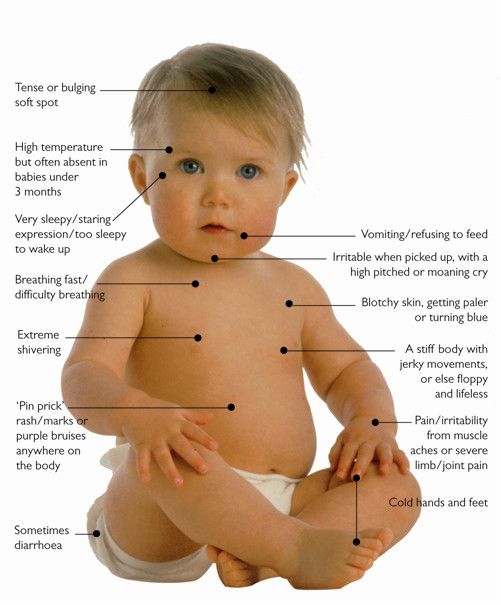
Typically, a doctor takes a sample of spinal fluid to identify the type of pathogen that is causing the infection. But they may prescribe antibiotics right away, as a precaution, because bacterial meningitis tends to be more serious than viral meningitis.
Milder cases of viral meningitis may go away on their own in 7–10 days. More severe cases require hospital care. A doctor may prescribe antiviral medications.
Doctors may treat fungal meningitis with antifungal medicines.
A person with meningitis may also need medications to prevent seizures, as well as steroids to reduce brain inflammation.
People who may have a higher risk of meningitis include:
- infants under 1 year of age
- people who live in close communities such as college dorms or adult care facilities
- anyone with a weakened immune system
- people with certain medical conditions
Meningitis can be life-threatening, and it can get worse quickly.
Many people recover from meningitis with prompt medical care.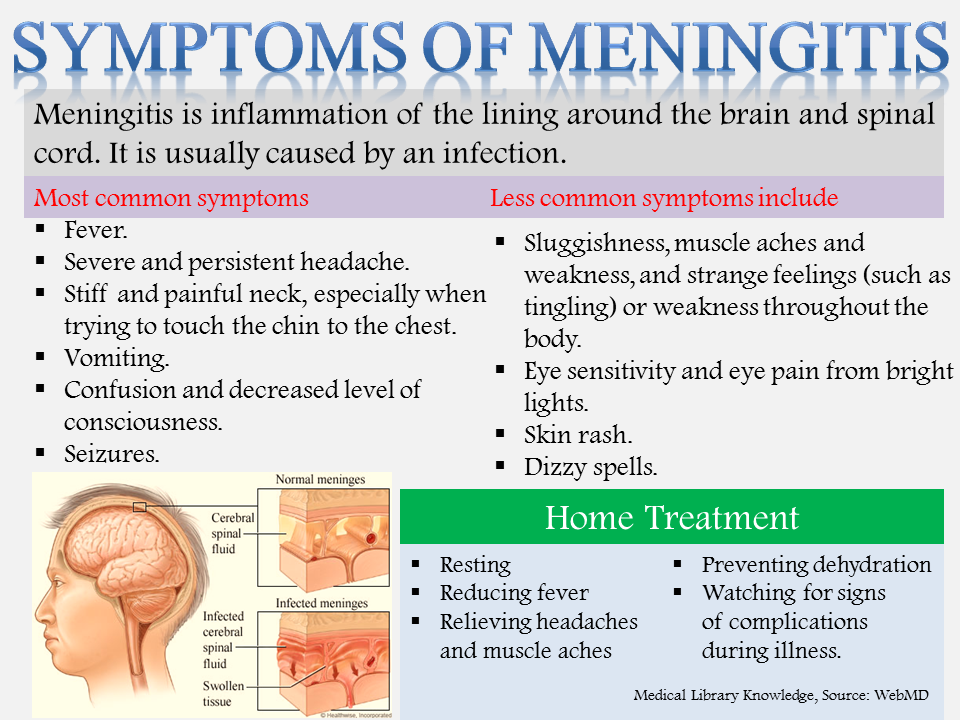 However, long-term complications can include:
However, long-term complications can include:
- headaches
- learning problems
- memory loss
- hearing problems
- speech problems
- vision problems
- weakness or paralysis
- seizures
- kidney damage
Some types of meningitis can pass from person to person. Strategies for avoiding meningitis include:
- not sharing foods, drinks, utensils, or personal items
- washing the hands properly and often with soap and running water, especially before eating and after using the bathroom.
- coughing and sneezing into the crook of the elbow, rather than the hands
- staying home when ill and keeping sick children from attending day care or school
One of the best ways to prevent many types of meningitis is to get vaccinated. The CDC recommend meningococcal vaccines for everyone at 11–12 years of age, with a booster dose at age 16.
Vaccination may be especially crucial for children and adults with a higher risk.
A petechial rash, which stems from bleeding under the skin, does not necessarily result from meningitis.
Some medications and many health issues — including injuries and viral infections — can cause rashes that may appear similar. This is why it is so important to check for other meningitis symptoms.
Noticing other changes in a person’s well-being can help them receive the necessary medical care swiftly.
The outlook for meningitis depends on many factors, including whether the disease is bacterial, fungal, or viral, and the person’s general health.
Seek emergency medical care if a person has any symptoms of meningitis. Prompt treatment can greatly increase the chance of survival and reduce the risk of long-term complications.
Meningococcal infection and its prevention
Meningococcal infection occupies an important place in infectious pathology and continues to be relevant for the Republic of Belarus
Meningococcal infection affects only people.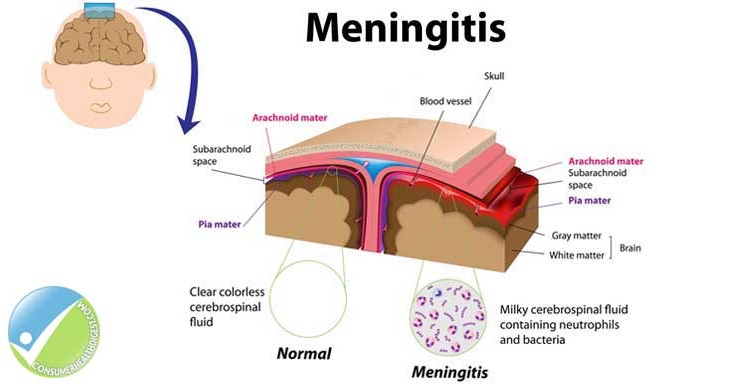 The causative agent - meningococcus - is transmitted by airborne droplets, as well as, for example, with the flu. This microbe lives in the nasal cavity and can be transmitted from person to person by sneezing, coughing and even talking. This is a very serious disease that can develop among full health in a matter of hours and minutes. Children are more often ill, and generalized forms of the disease in 80% of cases occur in children under 2 years of age. Sometimes it is not possible to save a sick child.
The causative agent - meningococcus - is transmitted by airborne droplets, as well as, for example, with the flu. This microbe lives in the nasal cavity and can be transmitted from person to person by sneezing, coughing and even talking. This is a very serious disease that can develop among full health in a matter of hours and minutes. Children are more often ill, and generalized forms of the disease in 80% of cases occur in children under 2 years of age. Sometimes it is not possible to save a sick child.
The incubation period (the period from the moment meningococcus enters the body until the first signs of the disease appear) can last from several hours to 10 days. It all depends on the age and immune status of the patient.
The microbe itself is relatively unstable in the external environment. Outside of a person, he dies within 30 minutes. Fresh air, direct sunlight, ultraviolet radiation and disinfectants are especially detrimental to meningococcus.
This disease is characterized by a very acute onset, one might say in the midst of full health or after a slight runny nose.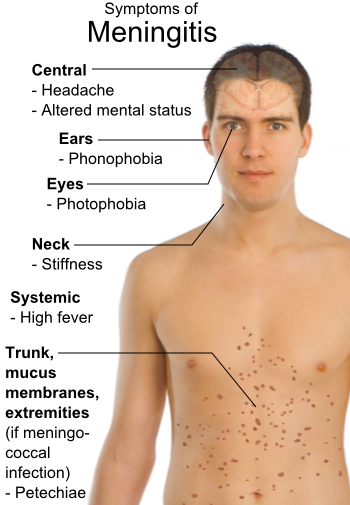 The temperature rises sharply to very high numbers, the child complains of a severe headache, at first a single, and then indomitable vomiting appears. Young children, who cannot yet complain, may have regurgitation, lethargy, refusal of the breast.
The temperature rises sharply to very high numbers, the child complains of a severe headache, at first a single, and then indomitable vomiting appears. Young children, who cannot yet complain, may have regurgitation, lethargy, refusal of the breast.
The main symptom of the fulminant form and the appearance of an infectious agent in the blood (meningococcemia) is a rash on the child's skin. Rash with meningitis in children is one of the most characteristic symptoms. Initially, it may be morbilliform in nature - in the form of small red spots and papules. After some time, such a rash disappears and a hemorrhagic rash characteristic of meningococcal infection appears. Pinpoint hemorrhages appear first in the feet and legs of the child, and then spread higher to the trunk and other parts of the body. On pale skin, they resemble a picture of a starry sky.
- Note that meningococcal rash does not go away with pressure. If a rash appears on the face, eyelids, oral mucosa, auricles, or at the very beginning of the disease, this is an unfavorable factor and is typical for severe forms of the disease.
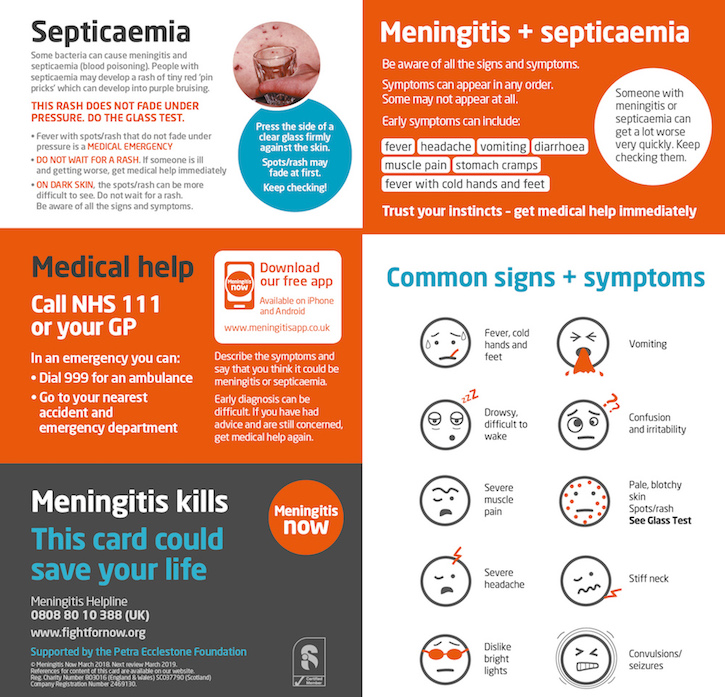 The rash will increase. And it is precisely in the presence of it that it is necessary to re-call the doctor, since the primary diagnosis before the rash can be set as an acute respiratory disease.
The rash will increase. And it is precisely in the presence of it that it is necessary to re-call the doctor, since the primary diagnosis before the rash can be set as an acute respiratory disease.
This form of meningitis is dangerous because toxic-septic shock can develop due to hemorrhage in vital organs and, above all, in the adrenal glands. This shock causes death in 5-10 percent of patients. Therefore, the sooner parents seek medical help, and the sooner an appropriate diagnosis is made, the greater the chance of saving the patient. But in any case, hospitalization will be required and parents do not need to refuse it.
- What are the preventive measures for meningococcal disease?
You just need to carefully monitor the child's condition and, if warning signs appear, immediately seek medical help.
Oddly enough, the best prevention of meningitis is to strengthen the immune system - walks in the fresh air, rational nutrition and hardening. Equally important is personal hygiene. Thorough hand washing is very important to avoid infection. Teach your children to wash their hands frequently, especially before eating, after being in a public place, and after they have touched animals.
Equally important is personal hygiene. Thorough hand washing is very important to avoid infection. Teach your children to wash their hands frequently, especially before eating, after being in a public place, and after they have touched animals.
And most importantly, do not try to treat the baby yourself. In many ways, the results of the treatment of meningitis depend on the time that has passed since the onset of the first symptoms and the start of therapy. Only a specialist is able to correctly assess the situation and select treatment tactics.
Prevention of meningitis in children is primarily the prevention of airborne infection of the child. For children aged 1 to 3 years, the main danger is adults, and first of all, relatives. The most dangerous age for meningitis is up to 5 years, and in many respects the health of the child depends on his parents. If one of the older family members has a cough, runny nose, nasal congestion, think about the child - do not approach him, or put on a four-layer gauze bandage, covering both the nose and mouth.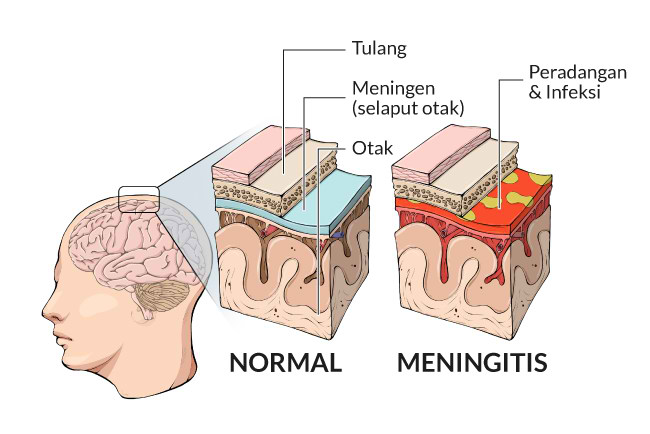
- Meningococcus is one of the weakest microbes, it dies very quickly outside the human body, especially from the action of ultraviolet rays of sunlight. Regular ventilation of the premises and sufficient sunlight can quickly get rid of these microbes in the air. Thus, you need to take care of good lighting in your child's room. The nursery should always be ventilated and washed clean.
Among other preventive measures, it is recommended to have fewer contacts during the period of the seasonal rise in the incidence of influenza and ARVI, to attend social events less frequently. All festive events (christenings) associated with the birth of a child must be carried out outside the apartment where he is.
And most importantly, don't try to treat yourself. The results of treatment of meningococcal infection largely depend on the time interval between the onset of the first symptoms and the start of therapy. Only a specialist can correctly assess the situation and choose the tactics of treatment.
If hospitalization is suggested by a health worker, do not refuse it, your child's life may depend on it.
A complete and balanced diet enriched with vitamins and microelements, playing sports, hardening the body also contribute to the body's resistance to infection.
The bacterium N. meningitidis is transmitted from person to person through droplets of secretions from the respiratory tract or throat of the carrier. Smoking, as well as close and prolonged contact, such as kissing, sneezing or coughing towards another person, or living in close proximity with an infected carrier person, contributes to the spread of the disease. Mass events also facilitate the transmission of the bacterium.
The risk group includes children under 5 years of age. The peculiarity of the infection is that due to the presence of a protective capsule in meningococcus, small children (1-5 years old) are unable to effectively develop immunity against a natural infection.
The incidence of meningococcal infection is recorded throughout the year, but most cases occur during the seasonal rise - from February to April.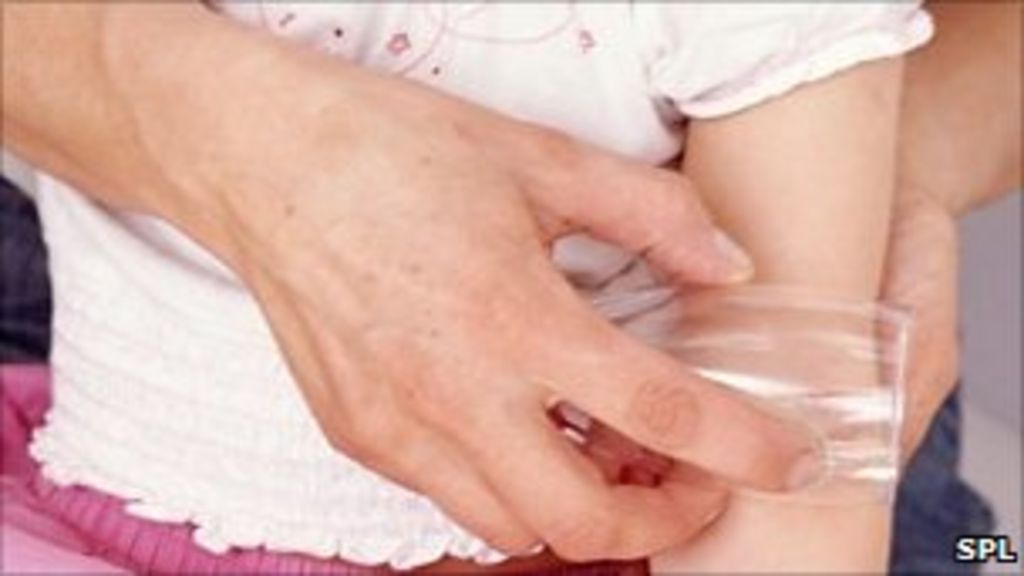
The usual incubation period is 4 days, but can vary from 2 to 10 days.
When meningococcus enters a healthy person, there are three possible scenarios:
First: meningococcus lives on the mucous membrane (up to a maximum of 6 weeks) and then disappears. The person was and remains healthy, only spreads the bacteria further. It's called carrier. Most children and almost all healthy adults react this way.
Second: after infection, a local inflammatory reaction develops at the site of introduction of the bacterium - meningococcal nasopharyngitis (inflammation of the nose and pharynx). The clinic is like a common cold. Temperature, cough, runny nose, red throat. In this case, a meningococcal infection can be suspected only when everyone in the area knows about the rise in the incidence of this infection. In other cases, it will be regarded as a common ARVI and, like a common ARVI, will pass safely and without treatment on its own in 5-7 days.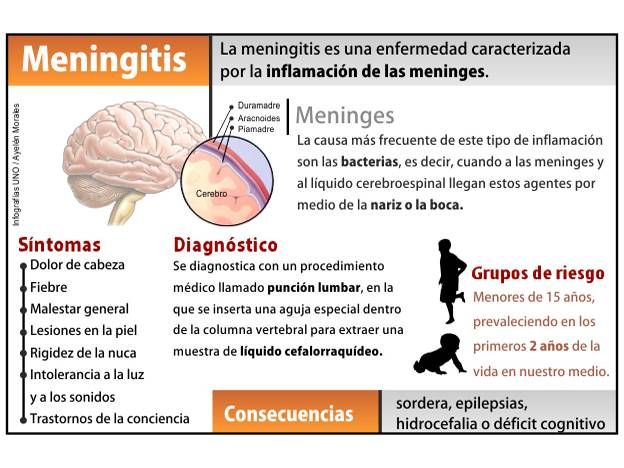
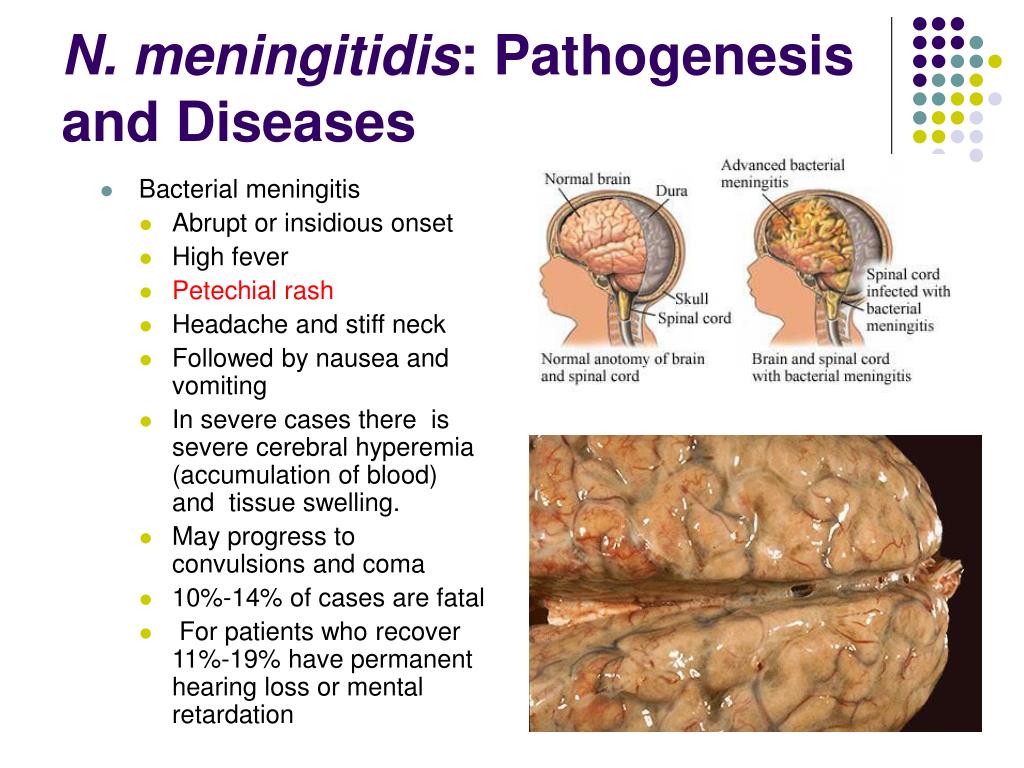
Third: in 1% of cases when the body is weakened, meningococcus breaks through the protection of the mucous membranes and enters the blood, spreads with its current throughout the body. This is how generalized forms of meningococcal infection develop: meningitis, meningococcemia, meningoencephalitis, mixed forms . This is an emergency. The bacterium is easy to destroy, it lends itself well to antibiotics, but it can be difficult to cope with the consequences of its stay in the body. Until now, even with timely treatment, up to 10% of children with severe forms of meningococcal infection die.
Meningitis usually begins acutely, with severe chills and fever up to 38-40°C.
The disease is also characterized by:
- severe general weakness
- pain in the eyeballs, especially when moving
- headache in the frontotemporal, less often in the occipital regions. The headache grows rapidly, becomes diffuse, excruciating, pressing or bursting.

- loss of appetite
- nausea, vomiting that does not bring relief.
- hypersensitivity to all kinds of external stimuli (eg photophobia),
- lethargy, lethargy, sleep disturbance.
- in severe forms of meningitis, impaired consciousness is characteristic.
After 12-14 hours from the onset of the disease, objective symptoms of irritation of the meninges appear (it is impossible to tilt the head forward; in the supine position, when the chin approaches the chest, the legs involuntarily bend).
In newborns and children under 2 years of age, meningitis usually does not present with typical symptoms. In this age group, meningitis is more likely to present with the following symptoms:
- high fever
- constant monotonous crying
- excessive drowsiness, or vice versa - excessive irritability
- passivity or slowness
- refusal to eat
- Bulging fontanelles on the head
- stiffness in the child's body, especially in the neck.
One of the most severe forms of meningococcal infection is meningococcemia. The key symptom of this form is a hemorrhagic rash: in the form of small bruises; starts as small pink or blue star-shaped spots and rapidly increases in number and diameter, becoming purplish in color. Most often, the rash occurs on the buttocks, legs, arms.
This is an extremely dangerous disease that threatens human life. If you suddenly find such a rash against the background of a high temperature, especially if new elements of the rash appear one by one in a matter of minutes - URGENTLY call an ambulance .
Prevention
( Immediate prophylactic administration of antibiotics to close contacts reduces the risk of transmission).
3. Non-Specific Prevention (Wash your hands thoroughly; do not share drinks, foods, straws, cutlery, lip balms, or toothbrushes; maintain your immune system through reasonable work, adequate rest, regular exercise, and a healthy diet with plenty of fresh fruits, vegetables, and whole grains; walk more outdoors, avoid public transportation, stay away from crowded indoor areas for extended periods of time).