How many centimeters dilated when water breaks
Stages of Labor Explained - Kernodle Clinic
If you’re pregnant with your first baby, or if it’s been a while since your last pregnancy, learning about the stages of labor before your due date can help you know what to expect. First and foremost, it’s important to understand that every woman’s labor is different and it may be different each time you have a baby. However, there are patterns of labor that will hold true for most women. To help you feel ready for your baby’s birth, here is a brief explanation of the three stages of labor and what happens during each:
Stage 1: LaborThe first stage of labor is defined as the time of the onset of true labor until the cervix is completely dilated to 10 cm. This stage is also the longest and involves three phases.
- Early labor begins when you go into labor until the cervix is dilated 3 cm.
- Active labor occurs as the cervix continues to dilate from 3 cm to 7 cm.
- Transition is the final phase of the first stage when the cervix continues to dilate fully to 10 cm.
According to the American Pregnancy Association, early labor typically lasts 8-12 hours with contractions lasting about 30-45 seconds anywhere from 5 to 30 minutes apart. Contractions generally start out mild and may be irregular, but during this phase will become progressively stronger and more frequent. It is also during this phase that your water might break.
On average, the active labor phase will last 3-5 hours with contractions lasting about 45-60 seconds roughly 3-5 minutes apart. If you didn’t already head to the hospital when your water broke in the first phase, this is usually the time to head to the hospital.
Although it is the shortest phase, the transition phase is the most challenging. Transition typically lasts 30 minutes to 2 hours as your cervix fully dilates from 8 cm to 10 cm. Contractions will last roughly 60-90 seconds with only 30 seconds to 2 minutes between.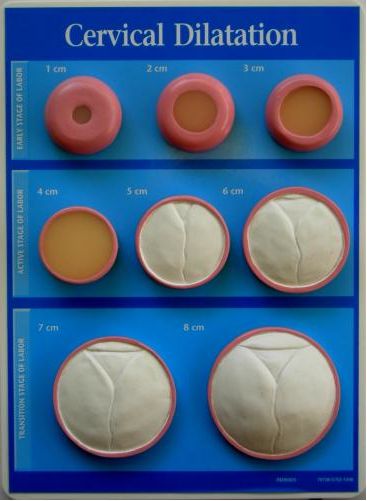 Due to the length and intensity of contractions, women may experience hot flashes, chills, nausea or vomiting. You may also feel a lot of pressure in your lower back and rectum, but if you start feeling the need to push, be sure to tell your provider.
Due to the length and intensity of contractions, women may experience hot flashes, chills, nausea or vomiting. You may also feel a lot of pressure in your lower back and rectum, but if you start feeling the need to push, be sure to tell your provider.
The second stage of labor begins once you are fully dilated to 10 cm. Your provider will let you know that it is time to start pushing your baby out. This stage can be as short as 20 minutes or as long as a few hours. Here are some important things to know about the second stage of labor:
- Your contractions may slow down to come every 2 to 5 minutes apart. They last about 60 to 90 seconds.
- Push during contractions and rest between them. Push when you feel the urge or when your provider tells you.
- If you’re uncomfortable or pushing has stopped, try a new position until you find one that is comfortable for you. You can squat, sit, kneel or lie back.
- You may get an episiotomy, a small cut made at the opening of the vagina to help let the baby out.
 Most women don’t need an episiotomy but may tear naturally.
Most women don’t need an episiotomy but may tear naturally. - Your provider will help guide your baby out of the birth canal. Special tools, like forceps or suction, may be needed to help your baby out.
- Your baby is born, the umbilical cord will need to be cut. Considering adding instructions in your birth plan about who you would like to cut the umbilical.
What some women may not realize is that after you deliver your baby, you still have to deliver the placenta–the organ that developed in your uterus and supplied food and oxygen to your baby throughout your pregnancy through the umbilical cord. This is the short stage of labor and for most women, it typically lasts fewer than 20 minutes. If you had an episiotomy or natural tearing, it will be repaired during this time. If you’ve elected to store your umbilical cord blood, this is also the time your provider will collect it.
You may still experience mild contractions before and even after the placenta is delivered as your uterus begins to start contracting back to its normal size. But, as your provider is helping to deliver the placenta and make any repairs you can enjoy the first few moments with your baby with skin-to-skin contact. You can also start breastfeeding right away, as most women are able to start breastfeeding within 1 hour of their baby’s birth.
But, as your provider is helping to deliver the placenta and make any repairs you can enjoy the first few moments with your baby with skin-to-skin contact. You can also start breastfeeding right away, as most women are able to start breastfeeding within 1 hour of their baby’s birth.
—
After you’ve successfully navigated through all three stages of labor, relish in the amazing feat that your body just accomplished. And, remember to be kind to yourself in the hours, days and months ahead. Your care team at Kernodle OB/GYN is here for you every step of the way from pre-conception, throughout your pregnancy and postpartum. You can call us at (336) 538-2367 or use our patient portal, Duke MyChart, to send a secure message to your care team about any non-urgent medical questions or needs that you may have.
Cervix Dilation Chart: Stages of Labor
The cervix, which is the lowest portion of the uterus, opens when a woman has a baby, through a process called cervical dilation. The process of the cervix opening (dilating) is one way that healthcare staff track how a woman’s labor is progressing.
The process of the cervix opening (dilating) is one way that healthcare staff track how a woman’s labor is progressing.
During labor, the cervix opens to accommodate the passage of baby’s head into the vagina, which is around 10 centimeters (cm) dilated for most term babies.
If your cervix is dilated with regular, painful contractions, you’re in active labor and getting closer to delivering your baby.
The first stage of labor is divided into two parts: the latent and active phases.
Latent phase of laborThe latent phase of labor is the first stage of labor. It can be thought of more as the “waiting game” stage of labor. For first-time moms, it can take a while to move through the latent phase of labor.
In this stage, contractions aren’t yet strong or regular. The cervix is essentially “warming up,” softening, and shortening as it prepares for the main event.
You might consider picturing the uterus as a balloon. Think of the cervix as the neck and opening of the balloon. As you fill that balloon up, the neck of the balloon draws up with the pressure of the air behind it, similar to the cervix.
As you fill that balloon up, the neck of the balloon draws up with the pressure of the air behind it, similar to the cervix.
The cervix is simply the bottom opening of the uterus drawing up and opening wider to make room for the baby.
Active stage of laborA woman is considered to be in the active stage of labor once the cervix dilates to around 5 to 6 cm and contractions begin to get longer, stronger, and closer together.
The active stage of labor is characterized more by the rate of regular cervical dilation per hour. Your doctor will expect to see your cervix opening at a more regular rate during this stage.
How long does stage 1 of labor last?There’s no scientific hard and fast rule for how long the latent and active phases last in women. The active stage of labor can range from a woman dilating anywhere from 0.5 cm per hour up to 0.7 cm per hour.
How fast your cervix dilates will also depend on if it’s your first baby or not. Mothers who have delivered a baby before tend to move more quickly through labor.
Mothers who have delivered a baby before tend to move more quickly through labor.
Some women will simply progress more quickly than others. Some women may “stall” at a certain stage, and then dilate very quickly.
In general, once the active stage of labor kicks in, it’s a safe bet to expect a steady cervical dilation every hour. Many women don’t start really dilating more regularly until closer to around 6 cm.
The first stage of labor ends when a woman’s cervix is fully dilated to 10 cm and fully effaced (thinned out).
The second stage of labor begins when a woman’s cervix is fully dilated to 10 centimeters. Even though a woman is fully dilated, it doesn’t mean that the baby is necessarily going to be delivered immediately.
A woman may reach full cervical dilation, but the baby may still need time to move down the birth canal fully to be ready for birth. Once the baby is in prime position, it’s time to push. The second stage ends after the baby is delivered.
In this stage, there’s again a wide range for how long it can take for the baby to come out. It can last anywhere from minutes to hours. Women may deliver with only a few hard pushes, or push for an hour or more.
Pushing occurs only with contractions, and the mother is encouraged to rest between them. At this point, the ideal frequency of contractions will be about 2 to 3 minutes apart, lasting 60 to 90 seconds.
In general, pushing takes longer for first-time pregnant people and for women who have had epidurals. Epidurals can reduce the woman’s urge to push and interfere with her ability to push. How long a woman is allowed to push depends on:
- the hospital’s policy
- the doctor’s discretion
- the health of the mom
- the health of the baby
The mother should be encouraged to change positions, squat with support, and rest between contractions. Forceps, vacuum, or cesarean delivery is considered if the baby isn’t progressing or the mother is becoming exhausted.
Again, every woman and baby is different. There’s no universally accepted “cut-off time” for pushing.
The second stage ends with the birth of the baby.
The third stage of labor is perhaps the most forgotten phase. Even though the “main event” of birth has occurred with the birth of the baby, a woman’s body still has important work to do. In this stage, she’s delivering the placenta.
A woman’s body actually grows an entirely new and separate organ with the placenta. Once the baby is born, the placenta no longer has a function, so her body must expel it.
The placenta is delivered the same way as the baby, through contractions. They may not feel as strong as the contractions that are needed to expel the baby. The doctor directs the mother to push and the delivery of the placenta is typically over with one push.
How long does stage 3 of labor last?The third stage of labor can last anywhere from 5 to 30 minutes. Putting the baby on the breast for breastfeeding will hasten this process.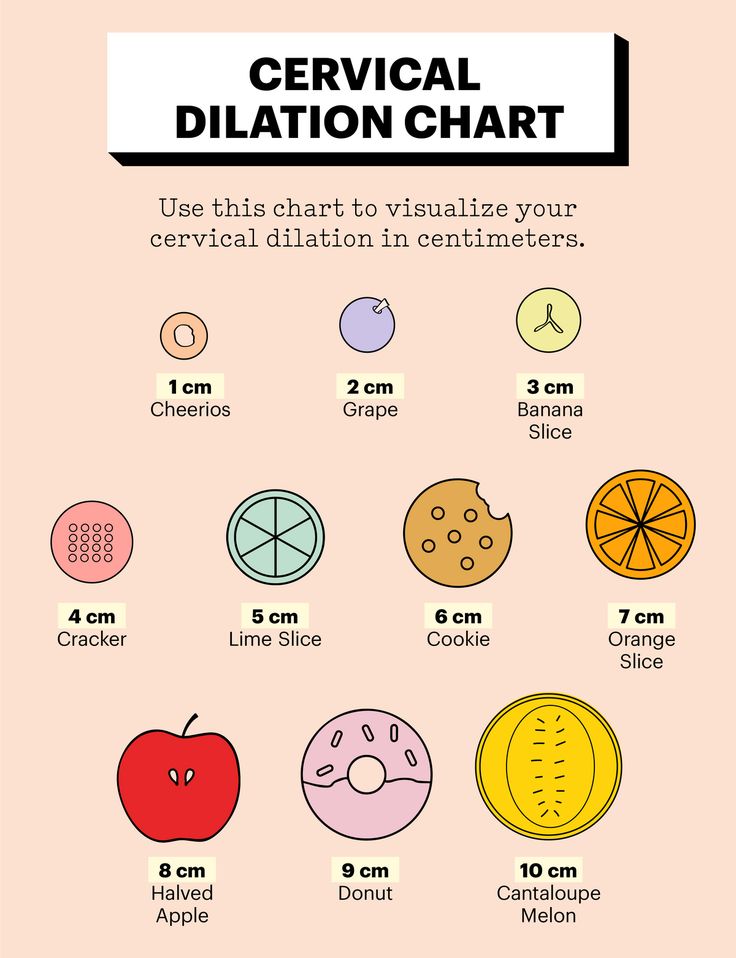
Postpartum recovery
Once the baby is born and the placenta has been delivered, the uterus contracts and the body recovers. This is often referred to as the fourth stage of labor.
After the hard work of moving through the stages of labor is finished, a woman’s body will need time to return to its nonpregnant state. On average, it takes about 6 weeks for the uterus to return to its nonpregnant size and for the cervix to return to its prepregnancy state.
Leakage of amniotic fluid | Symptoms of water leakage during pregnancy
Amniotic fluid is the first cradle of the baby, a comfortable environment for him to live before birth. Let's find out why it is so important for the development of the child? When and how do the waters leave? And what to do in difficult situations?
Tuesday, May 7th, 2019
- Seal
- Share
Why amniotic fluid is needed?
Amniotic fluid (also amniotic or fetal fluid) fills the fetal bladder (amnion) and creates favorable conditions for the development of the fetus. Liquid for 97% consists of water, which contains various nutrients, mineral salts, enzymes, hormones and vitamins.
Liquid for 97% consists of water, which contains various nutrients, mineral salts, enzymes, hormones and vitamins.
What are the important functions of the amniotic fluid?
- A harmonious environment for development. The waters provide a stable temperature of 37 ° C, contain immunoglobulins that neutralize viruses, microbes and some harmful substances.
- Baby protection. The liquid dampens shocks and shocks, reduces pressure from the outside and the volume of sounds. In addition, due to the tightness of the fetal bladder and the presence of a mucous plug in the cervical canal, nothing dangerous will get to the child.
- Development of body functions. When the baby swallows water, the kidneys begin to work, and if he draws in his nose, the lungs exercise.
- Facilitate childbirth. The bladder-filling liquid makes the pressure of the baby's head on the cervix softer, so that the cervix dilates smoothly. And after the waters break, they wash the birth canal, helping the child move forward.

How much liquid should I have?
The volume of amniotic fluid varies depending on the gestational age:
- at 10 weeks approximately 30 ml;
- in 20 - 450 ml;
- to 38-40 - 1000-1500 ml.
If the fluid is less or more, you need regular monitoring by a doctor, and if the condition of the pregnant woman and the fetus worsens, inpatient treatment. Since both polyhydramnios and oligohydramnios can negatively affect the developing body of the baby and the health of the expectant mother.
When and how does the water break?
In an ideal pregnancy, the amniotic fluid is drained after or with the mucus plug in the first stage of labour.
In the active phase of the first period, contractions become more frequent and the lumen in the cervix increases from 4 to 8 cm. If the fetal sac remains intact, then the doctor opens it.
More often in the first period, only the anterior waters come out, that is, located in front of the baby's head.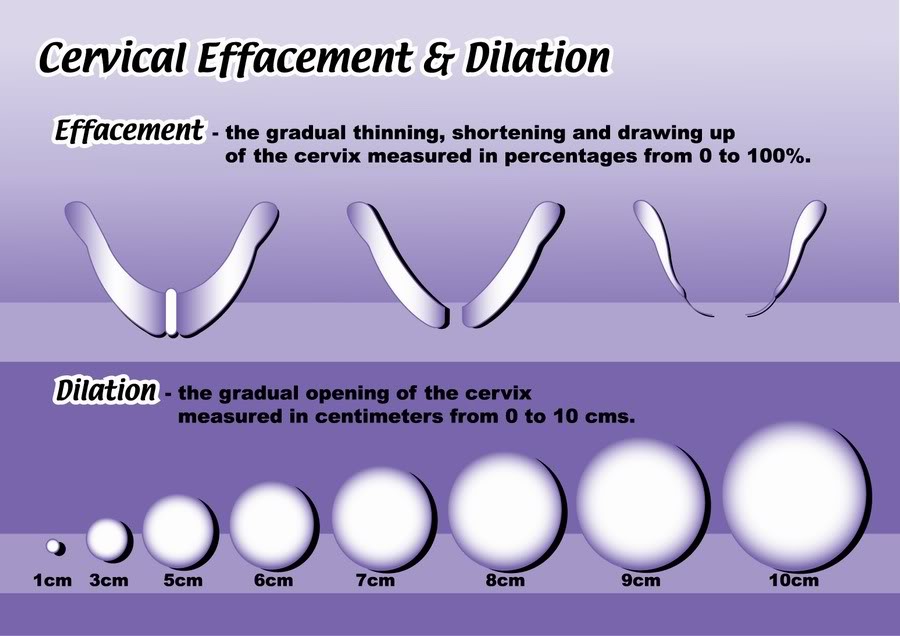 The posterior ones are poured out after the baby is born.
The posterior ones are poured out after the baby is born.
Isolation of amniotic fluid before delivery
According to statistics, 20% of women lose some of their amniotic fluid before the full rupture of the amniotic sac during labor. Let's take a closer look: when and how this happens, and what consequences it can entail.
If the waters have broken, but there are still no contractions, then the outpouring has occurred prematurely. If contractions have already begun, but the cervix is not open, such a departure is called early. Both options can lead to a protracted course and weakness of labor, hypoxia and injury to the fetus, as well as inflammatory processes in the woman in labor.
A third option is also possible - leakage of amniotic fluid. In this case, the fetal bladder only bursts and the fluid leaves little by little, sometimes imperceptibly for a pregnant woman.
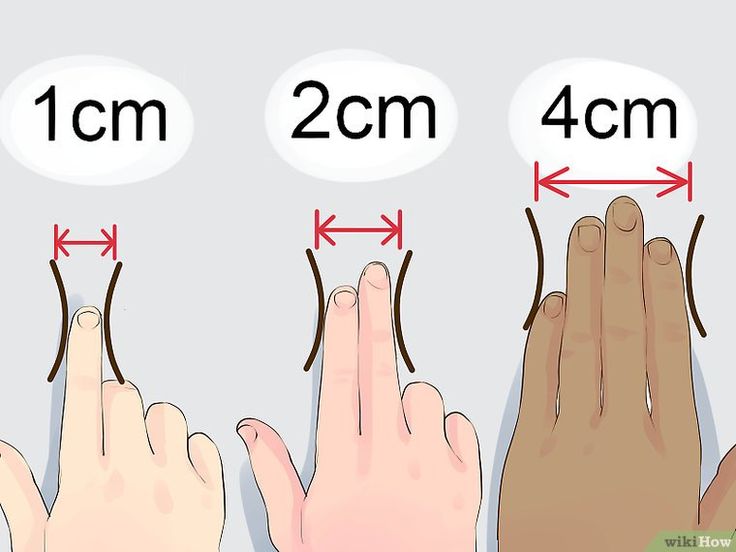
How can you tell if your waters have broken? In order not to confuse the fetal fluid with the mucous plug, pay attention to a number of differences:
- color: water is transparent, sometimes pinkish or greenish; the cork is beige-brown, sometimes with streaks of blood;
- consistency: water is more liquid, cork is slimy;
- frequency: water leaks constantly, the cork comes out in portions (about 1 tablespoon).
In case of leakage, due to the loss of tightness of the fetal bladder, the path to the baby is opened for bacteria and viruses. If damage occurs before 34 weeks, doctors protect the fetus with antibiotics and prolong the pregnancy. In the event of an infection, the woman is immediately prepared for childbirth.
What to do when the water breaks?
If a pregnant woman notices a leak of amniotic fluid, see a doctor as soon as possible. The specialist will take a smear from the cervix and, after conducting tests, will be able to decide what to do next.
When the water breaks abruptly, you must immediately go to the hospital, regardless of the presence and intensity of contractions. Note the time the fetal sac ruptured and note the color and smell of the fluid. If the waters are odorless, clear or slightly pinkish, then everything is normal. But a greenish, dark brown or black tint of the liquid is a signal that the baby has oxygen starvation and needs emergency help.