How give birth a baby
What happens to your body during childbirth
Childbirth is challenging and complications occur, but women's bodies are designed to give birth. The shape of the pelvis, hormones, powerful muscles and more all work together to help you bring your baby into the world - before, during and after childbirth.
How your body prepares for labour
Here are some of the ways your body will prepare both you and your baby for the birth ahead.
Braxton Hicks contractions
In the weeks or days before you start having proper contractions, you may experience Braxton Hicks contractions. This is your uterus tightening then relaxing. These contractions don't usually hurt and are thought to help your uterus and cervix get ready for labour.
Braxton Hicks contractions may become more regular as you get closer to the time of birth, but unlike labour contractions, they don't change the shape of the cervix and are sometimes referred to as 'false labour'. Your midwife can tell you if you're experiencing Braxton Hicks contractions or if you are in labour by doing a vaginal examination to look at your cervix.
Changes to the cervix
As labour gets closer, your cervix softens and becomes thinner, getting ready for the dilation (widening) that will allow the baby to enter the vagina. You may also see a 'show', which is a pinkish plug of mucus, stained with blood.
Engagement
Your baby may move further down your pelvis as the head engages, or sits in place over your cervix, ready for the birth. Some women feel they have more room to breathe after the baby has moved down. This is called 'lightening'.
Rupture of the membranes, or 'waters breaking'
Some women find the sac of amniotic fluid containing the baby breaks before labour, contractions start and the fluid runs (or gushes) out of the vagina. This is referred to as rupture of the membranes, or 'waters breaking'.
Let your maternity team know when your waters have broken and take notice of the colour of the fluid. It is usually light yellow. If it is green or red, tell your maternity team since this could mean the baby is having problems.
If your waters have broken but you have not started having regular contractions within 24 hours, you may need your labour to be induced because there is a risk of infection. Your midwife or doctor will talk to you about this.
How will you know when labour has started?
Movies often show women suddenly being struck by painful contractions and rushing to hospital. In real life, many women are not sure if they have actually started their labour.
You may feel restless, have back pain or period-like pain, or stomach disturbances such as diarrhoea.
Labour officially begins with contractions, which start working to open up the cervix. You should phone your midwife when your contractions start, although you probably won't be encouraged to come to the hospital or birthing centre until your contractions are closer together.
In preparation for labour, your baby may move further down your pelvis as the head engages, or sits in place over your cervix.How the pelvis is designed for childbirth
Your pelvis is located between your hip bones.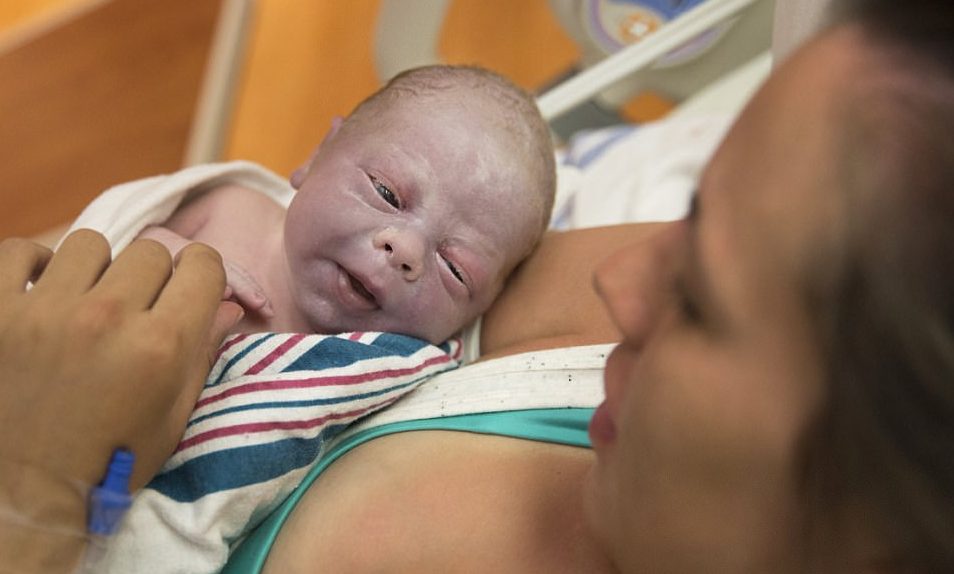 Women typically have wider, flatter pelvises than men, as well as a wider pelvic cavity (hole) to allow a baby to pass through.
Women typically have wider, flatter pelvises than men, as well as a wider pelvic cavity (hole) to allow a baby to pass through.
The organs sitting in a woman's pelvis include the uterus, cervix and vagina, which are held together by a group of muscles. During childbirth, the muscles at the top of your uterus press down on the baby's bottom. Your baby's head then presses on your cervix which, along with the release of the hormone oxytocin (see 'How hormones help you give birth', below), brings on contractions. Your cervix should dilate so your baby can pass through it.
Your pelvis has bones and ligaments that move or stretch as the baby travels into the vagina. Your baby also has spaces between the skull bones called 'sutures', and the gaps where the sutures meet on the skull are called fontanelles. This allows for the baby's head to mould as the skull bones meet or overlap, allowing it to fit more easily as it travels through your pelvis.
How hormones help you give birth
Your body produces hormones that trigger changes in your body before, during and after childbirth. Here's how they work to help you deliver your baby.
Here's how they work to help you deliver your baby.
- Prostaglandin Before childbirth, a higher level of prostaglandin will help open the cervix and make your body more receptive to another important hormone, oxytocin.
- Oxytocin This hormone causes contractions during labour, as well as the contractions that deliver the placenta after the baby is born. These post-birth contractions, including more that can occur during breastfeeding, help your uterus shrink back to its normal size. Oxytocin and prolactin are the two main hormones that produce and let down breast milk for your baby. Skin-to-skin contact between a mother and baby helps to release more of these hormones.
- Relaxin The hormone relaxin helps soften and stretch the cervix for birth, while helping your waters break and stretching the ligaments in your pelvis to allow the baby to come through.
- Beta-endorphins During childbirth, this type of endorphin helps with pain relief and can cause you to feel joyful or euphoric.

- 'Baby blues' After birth, your hormone balance can change again, and this is believed to cause the ‘baby blues’ in some women. You may feel teary, anxious and irritable and your mood can go up and down.
When childbirth doesn’t go to plan
Sometimes, complications can occur before or during childbirth that mean things don’t go as expected.
Sometimes, labour needs to be induced or started. There are a few ways to induce labour, including the mother being offered synthetic prostaglandin. This is inserted into the vagina to soften the cervix and start contractions.
If contractions slow down or stop during labour, the mother may be offered synthetic oxytocin from a drip to increase the contractions. In both these cases contractions can come on strongly and more pain relief may be needed. Your maternity team should explain the benefits and risks of this with you before you agree to it.
The baby could be in a posterior or breech position, not ideally placed above the cervix before the birth. Your maternity team may need to use forceps or a vacuum to help turn the baby or help the baby travel out of the vagina. Sometimes a caesarean is needed.
Your maternity team may need to use forceps or a vacuum to help turn the baby or help the baby travel out of the vagina. Sometimes a caesarean is needed.
In rare cases, a mother may experience cephalopelvic disproportion (CPD), which is when the baby’s head is too big to fit through the pelvis. A diagnosis of CPD is usually made when labour hasn’t progressed and synthetic oxytocin has not helped. A caesarean is usually the next step.
More information
If you have any questions about childbirth or pregnancy, you can call Pregnancy, Birth and Baby on 1800 882 436, 7 days a week, to speak to a maternal health nurse.
Learn more here about the development and quality assurance of healthdirect content.
Childbirth Options, Differences & Benefits
Overview
What are the types of delivery methods?
It’s hard to know exactly what will happen when you give birth. Most people have a plan in mind for how they hope their labor and delivery goes. When it comes to delivering your baby, it’s good to know there are many methods pregnancy care providers use. Types of delivery include:
Types of delivery include:
- Vaginal delivery.
- Assisted vaginal delivery (vacuum or forceps).
- C-section (Cesarean birth).
- VBAC (vaginal birth after cesarean).
What type of delivery is best?
A vaginal delivery is the safest and most common type of childbirth. Vaginal deliveries account for about 68% of all births in the United States. Most medical organizations and obstetricians recommend a vaginal delivery unless there is a medical reason for a C-section.
Vaginal delivery
What is a vaginal delivery?
In a vaginal birth, your baby is born through your vagina or birth canal. It’s the most preferred and most common way to deliver a baby because it carries the lowest risk (in most cases). A vaginal delivery occurs most often between weeks 37 and 42 of pregnancy. A vaginal delivery has three stages: labor, birth and delivering the placenta.
Some benefits of a vaginal delivery include:
- Faster recovery.

- Safest for the pregnant person and the baby.
- Lower rates of infection.
- Babies are at lower risk for respiratory problems and have a stronger immune system.
- Lactation and breastfeeding are usually easier.
A vaginal delivery can be spontaneous or induced:
- Spontaneous vaginal delivery: A vaginal delivery that happens on its own and without labor-inducing drugs. Going into labor naturally at 40 weeks of pregnancy is ideal.
- Induced vaginal delivery: Drugs or other techniques start labor and soften or open your cervix for delivery. Pregnancy care providers often recommend inducing labor when a pregnant person has a medical condition or is past due. Labor is usually induced with Pitocin®, a synthetic form of the drug oxytocin.
What happens if you don’t push during a vaginal delivery?
In most cases, once your cervix is fully dilated and your healthcare team is in place, your provider will ask you to push during a contraction.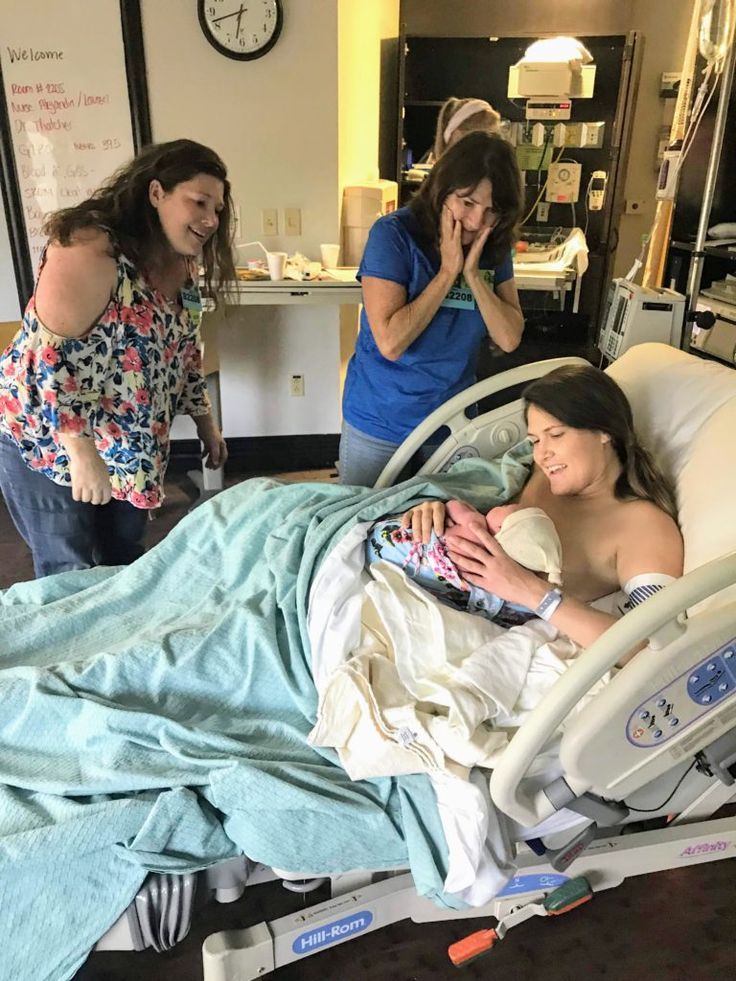 Pregnancy care providers have differing opinions on when to push, how long to push, delayed pushing or waiting until you feel the urge to push.
Pregnancy care providers have differing opinions on when to push, how long to push, delayed pushing or waiting until you feel the urge to push.
It’s hard to say what will happen if you don’t or can’t push during a vaginal delivery, because your birthing experience is so unique. However, studies show that resisting the urge to push or delaying pushing (laboring down) can cause complications like infection, bleeding or damage to your pelvis.
It’s best to discuss pushing with your pregnancy care provider ahead of time so you know what to expect during labor.
Assisted vaginal delivery
What is an assisted vaginal delivery?
An assisted vaginal delivery is when your obstetrician uses forceps or a vacuum device to get your baby out of your vagina. Assisted deliveries often happen when:
- You’ve been in labor a long time.
- Your labor isn’t progressing.
- You become too fatigued to continue pushing.
- You or your baby are showing signs of distress.

Assisted deliveries only occur when certain conditions are met.
What are examples of assisted deliveries?
The procedure your obstetrician recommends will depend on the conditions that arise while you’re in labor. Assisted delivery procedures can include the following:
- Forceps delivery: Forceps are a tong-like surgical tool obstetricians use to grasp your baby’s head in order to guide them out of the birth canal.
- Vacuum extraction delivery: In a vacuum extraction, your obstetrician places a small suction cup on your baby’s head. The cup is attached to a pump that pulls on your baby while you push.
Vacuum extraction and forceps delivery are similar in their advantages and disadvantages, and often the choice between them comes down to the experience of your obstetrician.
C-section
What is a C-section?
During a C-section birth, your obstetrician delivers your baby through surgical incisions made in your abdomen and uterus. A C-section delivery might be planned in advance if a medical reason calls for it, or it might be unplanned and take place during your labor if certain problems arise. There are about 1.2 million C-section deliveries in the United States each year.
A C-section delivery might be planned in advance if a medical reason calls for it, or it might be unplanned and take place during your labor if certain problems arise. There are about 1.2 million C-section deliveries in the United States each year.
Your provider may recommend a planned cesarean delivery if you:
- Had a previous C-section delivery.
- Are expecting multiples.
- Have placenta previa.
- Have a breech baby.
- Have a baby with fetal macrosomia or a large baby.
- Have a uterine fibroid or other obstruction.
Sometimes, your labor and delivery changes, and a cesarean birth becomes necessary for the health and safety of you or your baby. An unplanned C-section might be needed if any of the following conditions arise during your labor:
- Fetal distress (your baby isn’t tolerating labor).
- Labor isn’t progressing.
- Umbilical cord prolapse.
- Placental abruption.
- Hemorrhage or excessive bleeding.

Risks of C-section deliveries
Like any surgery, a cesarean birth involves some risks. In general, there is more risk associated with a C-section than with a vaginal delivery.
These might include:
- Infection.
- Loss of blood or need for a blood transfusion.
- A blood clot that may break off and enter the bloodstream (embolism).
- Injury to the bowel or bladder.
- Longer recovery and longer hospital stay.
- Abdominal adhesions.
Benefits of C-section deliveries
Some people prefer a C-section birth because it gives them more control on choosing a due date. This is called an elective C-section. Some providers may allow elective C-sections for nonmedical reasons, however, this is usually discouraged. In most cases, a C-section birth occurs because it’s medically necessary. The American Congress of Obstetrics and Gynecologists (ACOG) recommends that scheduled cesareans not be performed before 39 weeks gestation, unless medically indicated.
Some benefits of a C-section as compared to a vaginal delivery are:
- Lower risk of your baby having trauma from passing through your vagina.
- Less risk of your baby being oxygen-deprived during delivery.
- Possible lower risk of incontinence or sexual dysfunction.
VBAC (vaginal birth after cesarean)
What is a VBAC?
If you’ve already had a cesarean birth, you may be able to have your next baby vaginally. This is a VBAC, or vaginal birth after cesarean. Because a surgical cut results in a scar on your uterus, the concern is that the pressure of labor in a vaginal delivery could cause your uterus to open (rupture) along the previous C-section scar. For this reason, certain criteria must be met in order for your obstetrician to attempt a vaginal birth after C-section.
Can I have a baby vaginally after a C-section?
People who have had a cesarean delivery might be able to deliver vaginally in a future pregnancy. If you meet the following criteria, your chances of a successful vaginal birth after cesarean (VBAC) are high:
- Your obstetrician made a low transverse incision during your cesarean.
 This is the typical way to perform a C-section, unless they need to deliver your baby in a hurry.
This is the typical way to perform a C-section, unless they need to deliver your baby in a hurry. - You don’t have other uterine scars or abnormalities.
- You had a prior vaginal delivery.
- You haven’t had a previous uterine rupture.
What else should I know about delivery?
There are several other terms you should be familiar with in case your pregnancy care provider discusses them during labor and delivery.
Episiotomy
An episiotomy is a surgical incision that widens the opening of your vagina. This allows your baby’s head to pass through more easily. Most people will not need an episiotomy.
There are two types of episiotomy incisions: the midline, made directly back toward your anus, and the mediolateral, which slants away from your anus.
Amniotomy (breaking your bag of waters)
An amniotomy is the artificial rupture of the amniotic membranes, or sac, which contains the fluid surrounding your baby. Your pregnancy care provider may artificially rupture your membranes (AROM) to:
- Induce or progress labor.

- Place an internal monitor to assess your contractions.
- Place an internal monitor on your baby’s scalp to assess their well-being.
- Check for meconium (a greenish-brown substance, which is your baby’s first poop).
Your provider will use an amniohook, which looks like a crochet hook, to rupture the sac. Once the procedure is complete, delivery should take place within 24 hours to prevent infection.
Fetal monitoring
Fetal monitoring is the process of watching your baby’s heart rate during labor. This can be external or internal. Knowing how your baby is handling labor helps your pregnancy care provider decide if labor can continue or if delivery is necessary.
- In external fetal monitoring, an ultrasound device is placed on your abdomen to record information about your baby’s heart rate, and the frequency and duration of your contractions.
- Internal monitoring involves the use of a small electrode to record your baby’s heart rate.
 Your membranes must be ruptured before the electrodes can be attached to your baby’s scalp. A pressure sensor can also be placed near your baby to measure the strength of contractions.
Your membranes must be ruptured before the electrodes can be attached to your baby’s scalp. A pressure sensor can also be placed near your baby to measure the strength of contractions.
Frequently Asked Questions
Which type of delivery is most painful?
This may come down to personal opinion. There are many factors involved — for example, using pain medication, the type of pain medication or your pain tolerance. You should discuss pain relief with your pregnancy care provider before labor so you know the risks and benefits of each type.
There are two general options: no medication (drug-free or natural delivery) or using pain medications.
A drug-free delivery means you intend to give birth vaginally without any pain medication. You can’t have a C-section without medication.
Your options for pain relief during childbirth could consist of:
- Analgesics: Analgesics relieve pain without causing complete loss of feeling or muscle movement.
 The most common example of an analgesic used during childbirth is an epidural. You can receive an epidural for a vaginal or a cesarean delivery.
The most common example of an analgesic used during childbirth is an epidural. You can receive an epidural for a vaginal or a cesarean delivery. - Anesthetics: Anesthetics (or anesthesia) keep you from feeling pain by blocking signals from your brain. These drugs are given as a shot or through an intravenous (IV) line. During a C-section, you may receive general anesthesia, which puts you to sleep. Another option during childbirth could be local anesthesia, which involves a shot of medication in a specific area of your body, like the nerves in your vagina and vulva.
Another factor in deciding what type of delivery is most painful is the recovery. Generally, a vaginal delivery is easier to recover from than a C-section delivery.
A note from Cleveland Clinic
Your labor and delivery experience will be unique to you. During pregnancy, it’s a good idea to familiarize yourself with the different types of delivery and other terms associated with childbirth. Your pregnancy care provider will recommend the safest delivery method based on your medical history and pregnancy.
Your pregnancy care provider will recommend the safest delivery method based on your medical history and pregnancy.
How to Conceive and Give birth to a healthy child?
Acne is a problem that we most often try to hide from others. However, worries about this only worsen the condition of the skin. This conclusion was reached by Norwegian scientists. They found a relationship between stress and acne.
The age-old question of fathers and children will forever remain unresolved. But, despite all the misunderstandings between the older and younger generations, children want to see their parents happy and healthy, and moms and dads dream that their daughters and sons will never get sick. The health of the future generation, in addition to environmental factors, is strongly influenced by how the mother's pregnancy proceeded, how the parents felt, their chronic and hereditary diseases, the gene pool that adults pass on to their babies. Fortunately, many congenital diseases can be diagnosed at a very early stage and the child in this case will appear strong and healthy. Pregnancy and, what is important, preparation for it is a very crucial moment.
Pregnancy and, what is important, preparation for it is a very crucial moment.
A lot of negative factors fall on the body of a modern person: from stress to bad ecology. That is why family and children planning is better not to let it take its course. The human body is a smart system and looking for opportunities to survive even in the most difficult situations - nature arranged it that way, but no one can say for sure how these consequences will affect our children. We are often carriers of "hidden threats" and, in order not to transfer our diseases to the fragile children's shoulders, future parents should thoroughly prepare for the birth of their "cub".
Examination before pregnancy
Elimination of all kinds of deviations in the health of future parents and undesirable factors in the environment can increase the possibility of having a healthy child.
Examination before conception increases the confidence of parents, this is a manifestation of concern for the future person. Naturally, the main attention is paid to the mother, but the father should not stand aside either, because the health of both parents affects the baby.
Naturally, the main attention is paid to the mother, but the father should not stand aside either, because the health of both parents affects the baby.
Infections affecting the fetus
There are many hidden infections that both father and mother can carry. Future parents may look healthy, but an infection "dormant" in the body of one person inevitably affects the development of the fetus. Intrauterine infections are a common cause of the development of abnormalities and even death of the child.
Microorganisms in fetal tissues do not always lead to the development of a disorder - their presence only increases the risk of developing abnormalities. This makes it possible to have a healthy baby even if the woman suffered any infectious disease during pregnancy.
The main ways of transmission of infection from mother to child are through the placenta or through the infected genital tract of a pregnant woman.
Rubella
The rubella virus is considered the most dangerous.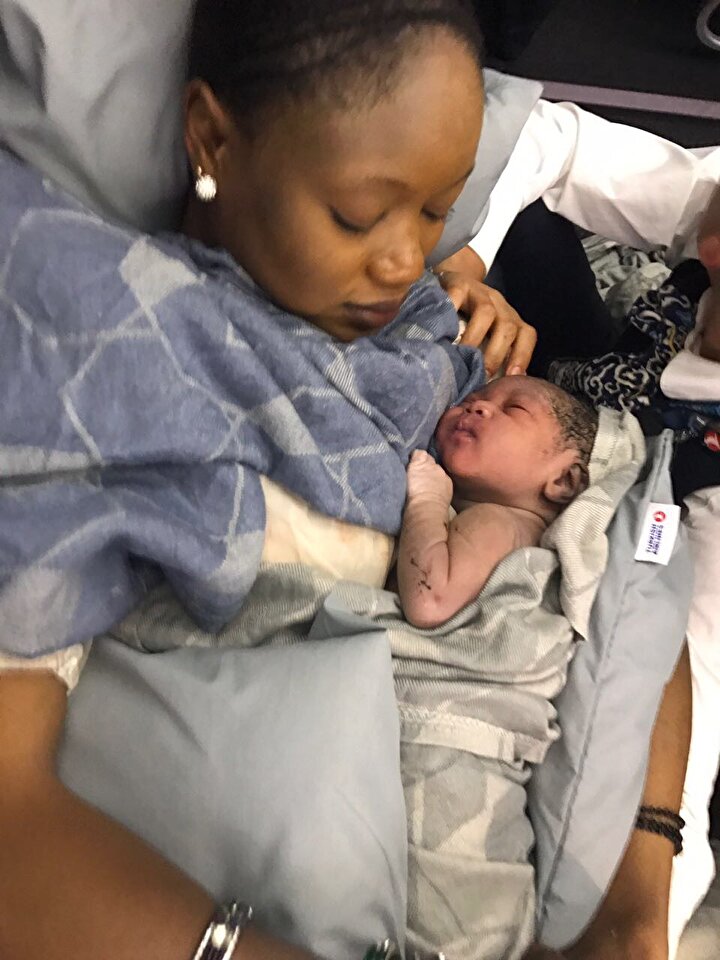 In most cases, it is transmitted to the fetus, which is the cause of many disorders. Deafness, heart disease and cataracts - in this combination, rubella affects the newborn. Sometimes there are violations of the blood, physical development.
In most cases, it is transmitted to the fetus, which is the cause of many disorders. Deafness, heart disease and cataracts - in this combination, rubella affects the newborn. Sometimes there are violations of the blood, physical development.
The transmission of the virus is carried out by airborne droplets, the source is most often sick children. Rubella can lead to stillbirth and miscarriage. The most dangerous period for infection is up to 5 weeks, it is at this time that the risk of developing congenital malformations is highest.
You can not worry about the health of the future person if the mother suffered this disease in childhood or was vaccinated against it. Otherwise, it is necessary to take a blood test for antibodies to rubella as soon as possible. With a planned pregnancy, it is worth getting vaccinated and taking tests a few months in advance.
Herpes
Herpes is the least dangerous for the fetus. But, in the case when genital herpes worsens in a woman after 32 weeks of pregnancy, the risk increases significantly.
To prevent the baby from becoming infected at birth, most often in such a situation, a caesarean section is prescribed. For peace of mind, the expectant mother can do a test to detect this virus.
Influenza
In this case, it is no longer the virus that is dangerous, but its consequences that affect the kidneys and the cardiovascular and immune systems. The threat of miscarriage and premature birth - that's what the flu can threaten. In the early stages of fetal development (up to about 12), the virus has the most serious consequences, since during this period the most important organs of the little man are laid and develop. To prevent this disease, mothers need to increase their immunity and avoid the possibility of infection.
Toxoplasmosis
Immunity from this disease after its transfer remains for life. But, in the case when a woman has not experienced toxoplasmosis, the risk associated with this bacterial infection is the most dangerous for the expectant mother and her child.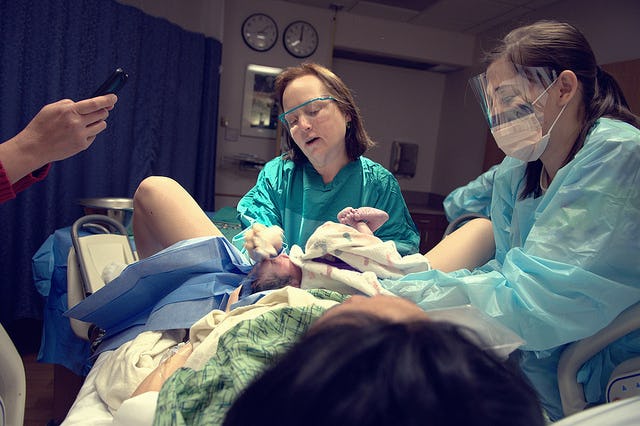 You can become infected through simple contact with a cat, or by eating an infected piece of meat.
You can become infected through simple contact with a cat, or by eating an infected piece of meat.
With the duration of pregnancy, the risk of toxoplasmosis increases. If a woman became infected in the first trimester, then this most likely will not lead to complications for the fetus. During the second trimester, the risk increases to 20%, in the third, the probability of the disease is 50-60%.
Other infections
Infectious diseases such as mycoplasmosis, thrush, gardenellosis, chlamydia, trichomoniasis, listeriosis can also adversely affect the health of the mother and child. But a timely diagnosis and proper treatment will help get rid of these diseases, leaving no memories of them.
Prevention of abnormalities in a child
In the event that a married couple already had deviations from a previous pregnancy, miscarriages, premature birth of a baby, the birth of sick children, then they need a thorough examination, medical advice and testing before conception.
Even if a woman is absolutely healthy, she must undergo research and visit doctors in order to determine the existing deviations and the possibility of their occurrence.
The expectant mother should also visit a dentist, therapist, otolaryngologist. At the onset of 10-12 weeks of pregnancy, a mandatory ultrasound is prescribed to exclude pronounced violations in the development of the unborn child.
If there is a suspicion of chromosomal abnormalities, especially for women over 35 years old, then a chorionic biopsy (genetic analysis) can be performed. This study in a short time makes it possible to exclude, with a high degree of probability, serious diseases and disorders in the development of a future person.
After 20-24 weeks, ultrasound can be used to monitor the intrauterine development of the child. At this time, the study shows all the organs, without difficulty, you can monitor the condition of the placenta, blood flow inside the vessels of the uterus and other important indicators.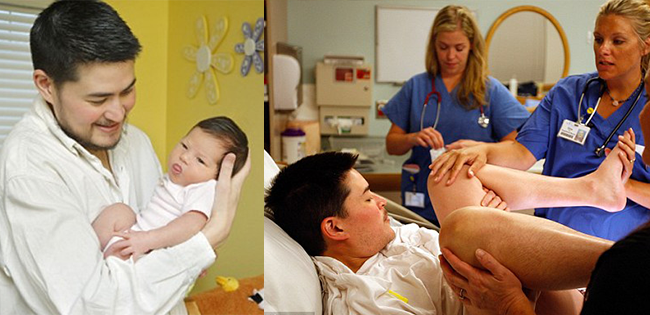
Pregnancy lifestyle
It is necessary, of course, to lead a healthy lifestyle all your life, but if some factors periodically interfere with this, then before pregnancy and even more so during it, they must be excluded. So, for future parents, both for mom and dad, the desire for the right lifestyle should begin as early as three months before conception!
It is very important to exclude the consumption of alcohol and, if not completely refuse, then minimize the number of cigarettes consumed as much as possible. Do not overheat and do not overcool, try to avoid seasonal diseases. An important factor will be to increase immunity and avoid stressful situations. In general, for this period, doctors advise to lead a more measured lifestyle: get enough sleep, fully eat right, be more happy.
You should increase the consumption of vegetables and fruits, try to eat more fish and meat, cottage cheese and a variety of dairy products. Vitamins and trace elements in them will help in the proper development of the fetus.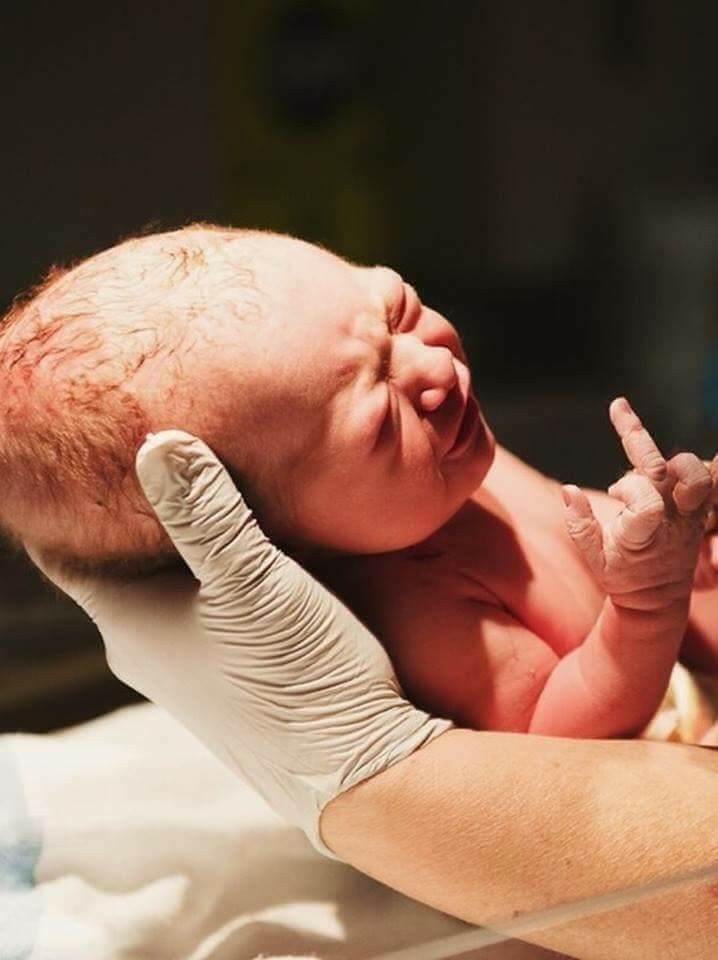 A big plus of proper nutrition is that in this case you do not have to take additional vitamins, unless, of course, a doctor prescribes them.
A big plus of proper nutrition is that in this case you do not have to take additional vitamins, unless, of course, a doctor prescribes them.
Flour and sweet foods should be limited. Extra pounds will interfere with the normal course of pregnancy. Salty foods, carbonated drinks, coffee and tea should also be limited. Why do you need an extra load on the body.
Don't sit still! Moderate physical activity, special exercises will only benefit you and your baby. Yoga for expectant mothers has been very popular lately, it will not only help prepare for childbirth and make it easier, but also bring a lot of positive emotions and relieve stress. A visit to the indoor pool will help strengthen the muscles of the back and pelvis, and lead the spine into a hole. But it is better to limit visits to open water bodies, the water in them can be infected with serious bacteria and viruses.
Compliance with the daily routine, rest and physical activity, healthy nutrition and positive emotions, timely visits to the doctor - all this together will help you endure and give birth to a healthy baby!
Articles
Return to the list
MEdel Multidisciplinary Clinic
We are waiting for you at the following addresses:
Kazan, st. Siberian tract, 34, bldg. 5
Siberian tract, 34, bldg. 5
Kazan, st. Adoratskogo, d. 17
Kazan, st. Julius Fucik, 91a
Mail: [email protected]
How to get to Kazan Clinics
Working hours:
from Mon to Fri 8:00 - 20:00
Saturday 8:00 - 17:00 Sunday
closed.
* Data processing policy
Review of the clinic Information search
How to bear and give birth to a healthy child
Dear parents, I would like to start my publication with these wonderful lines that carry a very deep meaning.
“When a man does not know which harbor he is on his way to, not a single wind will be favorable to him” (Seneca).
Have you ever thought about what your child's health depends on and what you have done to shape it.
Already from the moment you plan your pregnancy, you begin to lay brick by brick the foundation called "HEALTH" for your unborn child.
Every woman planning a pregnancy should be examined by a gynecologist, as well as other narrow specialists (depending on her diseases). Important at the stage of pregnancy planning is the refusal of a woman, and preferably both future parents, from bad habits. Many women who smoke do not even think about what their love for a cigarette can lead to. Smoking a woman before pregnancy, and subsequently during pregnancy, increases the risk of having a premature baby, the presence of congenital malformations, or even intrauterine death of the fetus. Such children often suffer from bronchial asthma in the future.
Important at the stage of pregnancy planning is the refusal of a woman, and preferably both future parents, from bad habits. Many women who smoke do not even think about what their love for a cigarette can lead to. Smoking a woman before pregnancy, and subsequently during pregnancy, increases the risk of having a premature baby, the presence of congenital malformations, or even intrauterine death of the fetus. Such children often suffer from bronchial asthma in the future.
I would like to say a few words about drug use at the planning stage and during pregnancy. Using drugs and having a healthy baby is next to impossible. Not many people know that drug use affects the activity of sex hormones and pregnancy may not occur at all. If pregnancy occurs, then the child may be born with signs of drug addiction, congenital malformations, low body weight, and in the worst case, may die in utero. These children are characterized by the presence of severe mental and neurological diseases, up to disability.
The second more important stage for you begins from the moment of fertilization, when a new life begins to develop in your body.
Arriving in this wonderful state of mind and body, you should not forget that right now the "HEALTH" of your child depends on you to a greater extent.
Be sure to eat well, walk in the fresh air. Avoid unreasonable use of medications, occupational hazards (especially in the first trimester of pregnancy).
Remember, even an uncomplicated pregnancy requires the supervision of an obstetrician-gynecologist. To do this, it is necessary to register for pregnancy no later than the 12th week of pregnancy.
From this moment begins the joint work of the doctor and the expectant mother on the formation of the health of the baby.
Throughout the pregnancy, a woman should be regularly observed by an obstetrician-gynecologist, control general tests, undergo an ultrasound scan of the fetus in a timely manner. A special examination for the presence of infections should also not be ignored, so as not to expose the fetus to the risk of intrauterine infection. Many infections are successfully treated if detected early.
Many infections are successfully treated if detected early.
Such well-coordinated work of an obstetrician-gynecologist and a pregnant woman makes it possible to prevent the development of various pathologies in the fetus and preserve the woman's health.
Unfortunately, quite often one hears that a pregnant woman was not registered for pregnancy, was not observed by an obstetrician-gynecologist, did not take tests, did not do an ultrasound of the fetus and was not at all aware of her interesting situation until the very birth.
But an even more irresponsible act on the part of a pregnant woman is the decision to conduct childbirth at home.
- Why does a woman refuse to provide her with qualified medical care in the digital age? - it's hard to say...
Perhaps the internet is to blame?
Now you can find a large number of forums where mothers enthusiastically share their experience, talk about the benefits of home birth in colors, describe everything: up to the step-by-step birth control.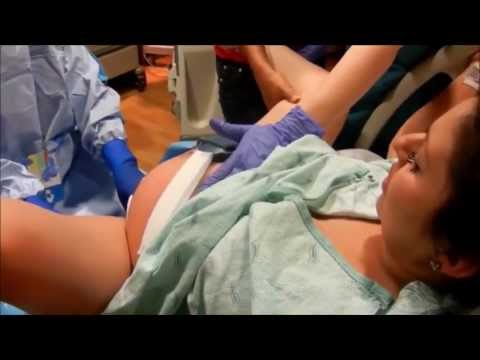 And it would seem: “Why a medical education?”, If you can give birth to a healthy child so easily with the help of GOOGLE!!!
And it would seem: “Why a medical education?”, If you can give birth to a healthy child so easily with the help of GOOGLE!!!
Recently, however, there have been frequent reports in the media about home births that resulted in the death of a child and even a woman in labor.
One such incident happened a few years ago.
A 29-year-old woman was admitted to the intensive care unit of one of the central district hospitals in the Minsk region. During the examination of the patient, doctors found traces of recent childbirth. Within hours, the woman dies. As it turned out, the woman was taken to the hospital forcibly. And at the place of residence in the bathroom were found two newborn girls with no signs of life. As it turned out, the woman was not registered for pregnancy, she was not examined by an obstetrician-gynecologist.
An equally horrific case of home birth occurred in Vitebsk in February 2017. As it turned out, our former compatriot from St. Petersburg in November 2016 turned to the antenatal clinic of the Vitebsk Regional Maternity Hospital and said that she was going to give birth in Vitebsk at home, as well as her first child.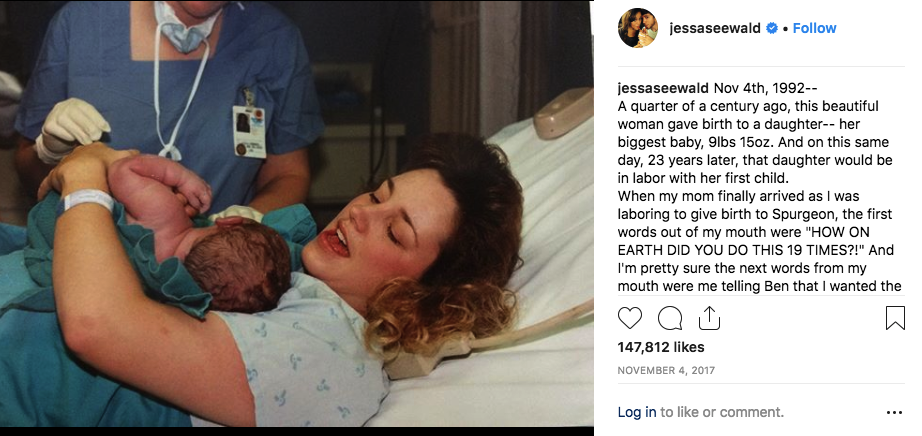 Doctors warned about the possible risks and consequences of childbirth at home, but the woman did not take this into account. In February 2017, an ambulance team delivered a newborn girl in serious condition to the Vitebsk City Clinical Emergency Hospital, who soon died. During the investigation, it was found that the death of the child was due to the aspiration of amniotic fluid during childbirth at home.
Doctors warned about the possible risks and consequences of childbirth at home, but the woman did not take this into account. In February 2017, an ambulance team delivered a newborn girl in serious condition to the Vitebsk City Clinical Emergency Hospital, who soon died. During the investigation, it was found that the death of the child was due to the aspiration of amniotic fluid during childbirth at home.
-Is it worth paying such a high price? - It's up to you, of course.
In our country, a lot of attention is paid to the issues of monitoring pregnancy, as well as issues of maternal and child health.
An incentive allowance has been introduced in the republic for pregnant women who are registered with the antenatal clinic before the 12th week of pregnancy and who fully comply with the recommendations of doctors.
Due to the high level of accessibility of medical care in our country, a pregnant woman can choose a doctor she would like to see in the antenatal clinic, as well as choose a medical facility for obstetric care.







:strip_icc():format(jpeg)/kly-media-production/medias/2785562/original/028627600_1556001360-shutterstock_1019963743.jpg)