How does chlamydia affect pregnancy
Chlamydia and pregnancy | Pregnancy Birth and Baby
Chlamydia and pregnancy | Pregnancy Birth and Baby beginning of content3-minute read
Listen
Chlamydia is a bacterial sexually transmitted infection (STI) that affects both men and women. Chlamydia can also cause a number of issues during pregnancy.
Most people with chlamydia are unaware that they have the infection. Left untreated, chlamydia can cause serious complications including infertility and chronic pain. Chlamydia is fairly easy to treat if you know you have it — one course of antibiotics is usually enough.
Causes of chlamydia
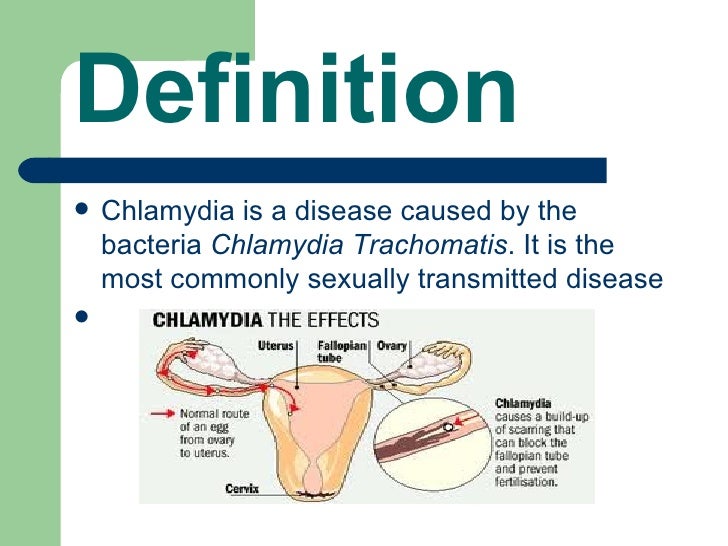
Chlamydia is caused by an infection with the bacterium Chlamydia trachomatis. It is spread by unprotected (unsafe) vaginal or anal sex with an infected person.
Chlamydia is the most commonly reported STI in Australia.
What are the symptoms of chlamydia?
Most men and women with chlamydia have no signs or symptoms, which makes it very easy to spread. Some people have the infection for many months or years without knowing it.
Women who get symptoms may have:
- vaginal discharge
- bleeding between periods or after sex
- burning or pain when urinating
- abdominal or pelvic pain
- pain during sex
Men who get symptoms may have some clear discharge from the penis or pain during urination.
In rare cases, people with chlamydia have sore joints (arthritis) or inflammation of the eye (uveitis).
Diagnosing chlamydia
Chlamydia is easily diagnosed. Your doctor may take a sample from the vagina, cervix, anus or penis, and may ask for a urine test. These are sent to a laboratory for testing.
If you think you or your partner have chlamydia, see your doctor or sexual health clinic so you can both be tested.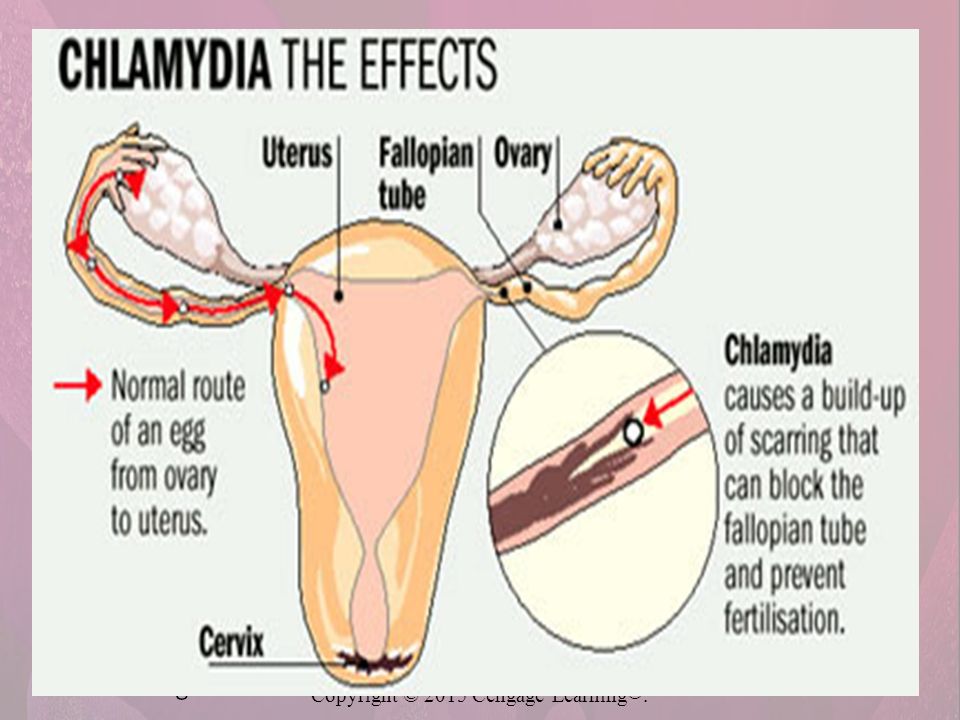 It is important that any sexual partners of people with chlamydia are tested, even if they don’t have symptoms.
It is important that any sexual partners of people with chlamydia are tested, even if they don’t have symptoms.
Treating chlamydia
Treatment for chlamydia is a course of antibiotics. It is important to avoid sex until the full course of treatment is finished, and for at least a week following. You should have another test 3 months after you are treated.
If you have chlamydia, all of your sexual partners should be informed, tested and treated, as they may be infected and can infect you, and others, again after treatment.
If your partner has had a positive test for chlamydia, you should be treated even if you have had a negative test result. As chlamydia infection increases the possibility of contracting other infections, it is important to be tested for other STIs such as gonorrhoea, hepatitis, HIV and syphilis. Using latex condoms and a water-based lubricant is the most effective way to prevent STIs. People who have chlamydia for long periods without treatment risk becoming infertile or developing arthritis. Women can get pelvic inflammatory disease, and men can get epididymitis (a painful infection near the testicle).
Women can get pelvic inflammatory disease, and men can get epididymitis (a painful infection near the testicle).
Chlamydia complications
If chlamydia isn't treated properly, it can cause serious complications. People who have chlamydia for long periods without treatment risk becoming infertile or developing arthritis.
For women, chlamydia can spread into the uterus and fallopian tubes, causing pelvic inflammatory disease. Pelvic inflammatory disease can lead to ectopic pregnancies, chronic pelvic pain and infertility.
In men, chlamydia can cause epididymitis (a painful infection near the testicle) or spread to the prostate gland, and the tubes that carry sperm, which may result in chronic pain and/or fertility problems.
Both men and women can develop arthritis, eye inflammation and inflammation of the rectum.
Chlamydia and pregnancy
Because of this, doctors recommend that pregnant women under the age of 30 should be screened for chlamydia.
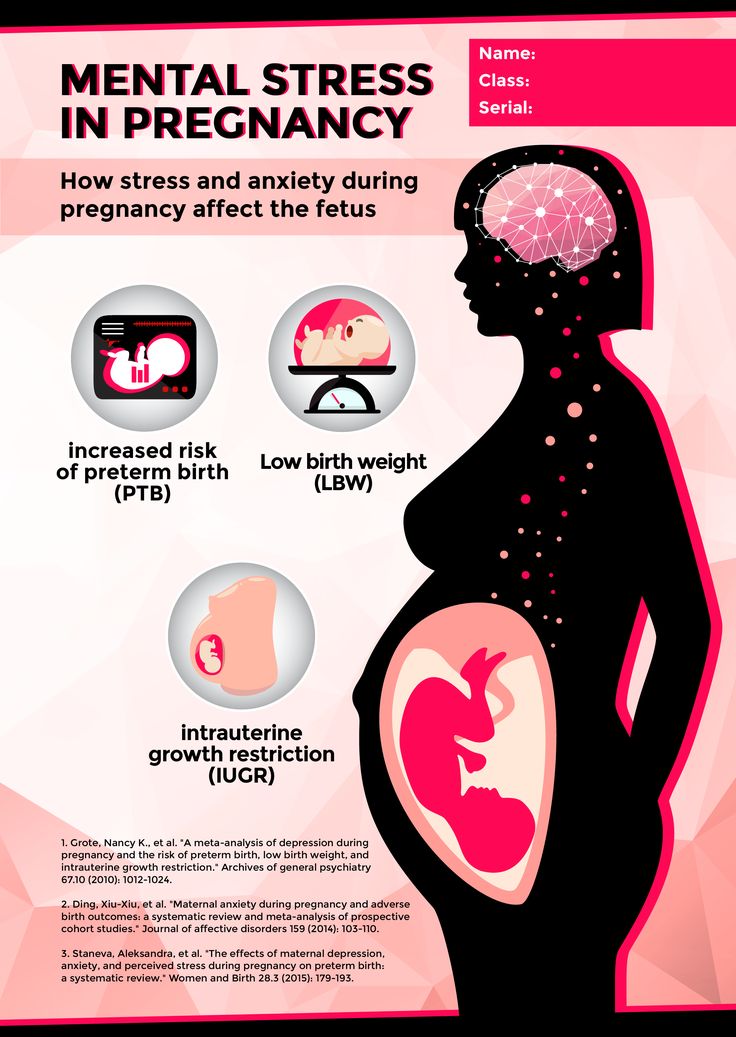
Pregnant women who are infected with chlamydia have an increased risk of their waters breaking prematurely, causing the baby to be born early.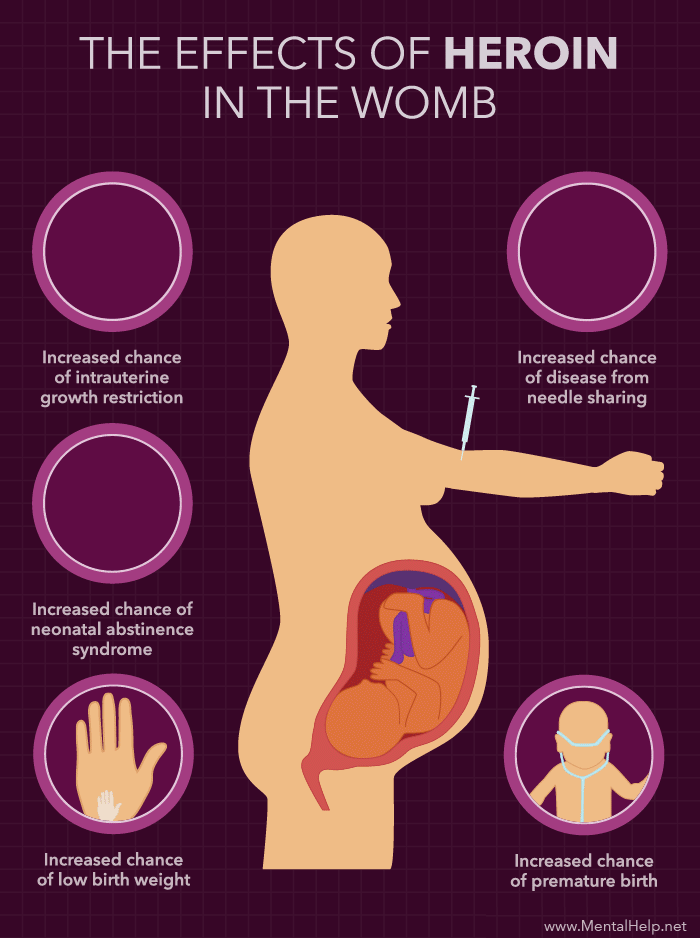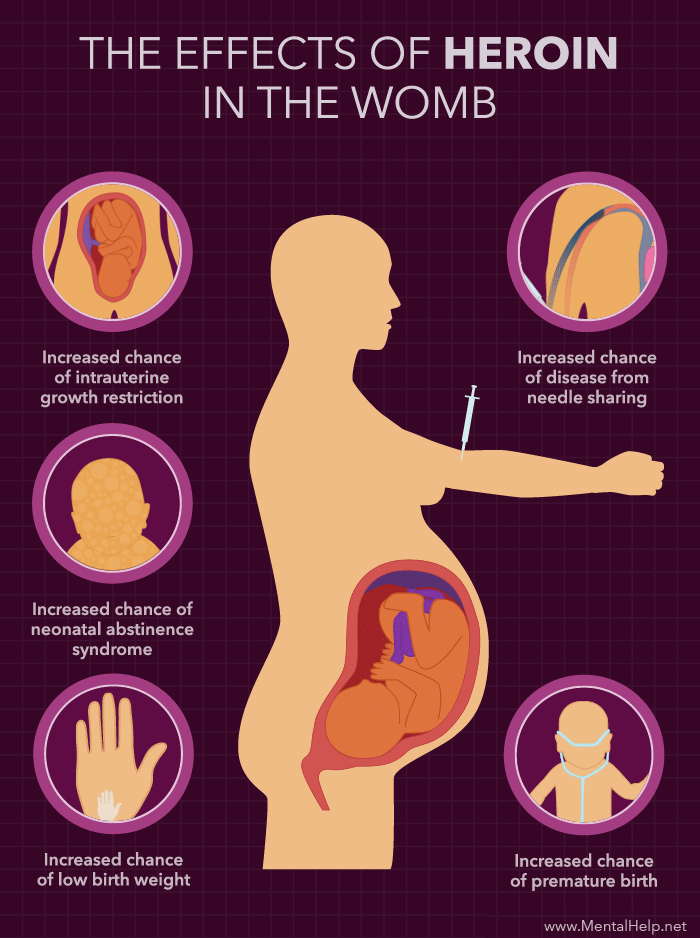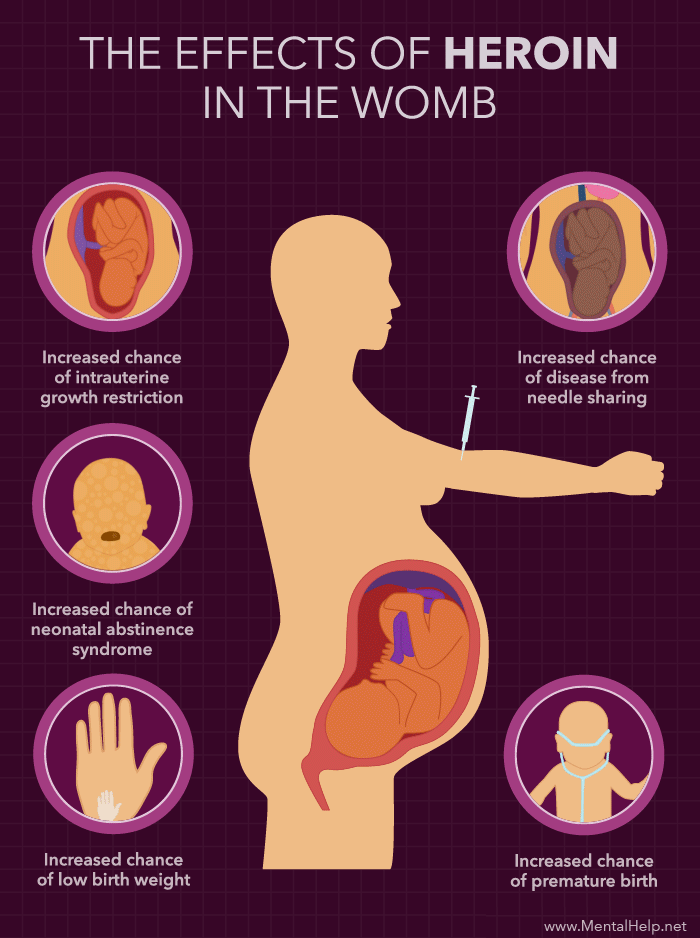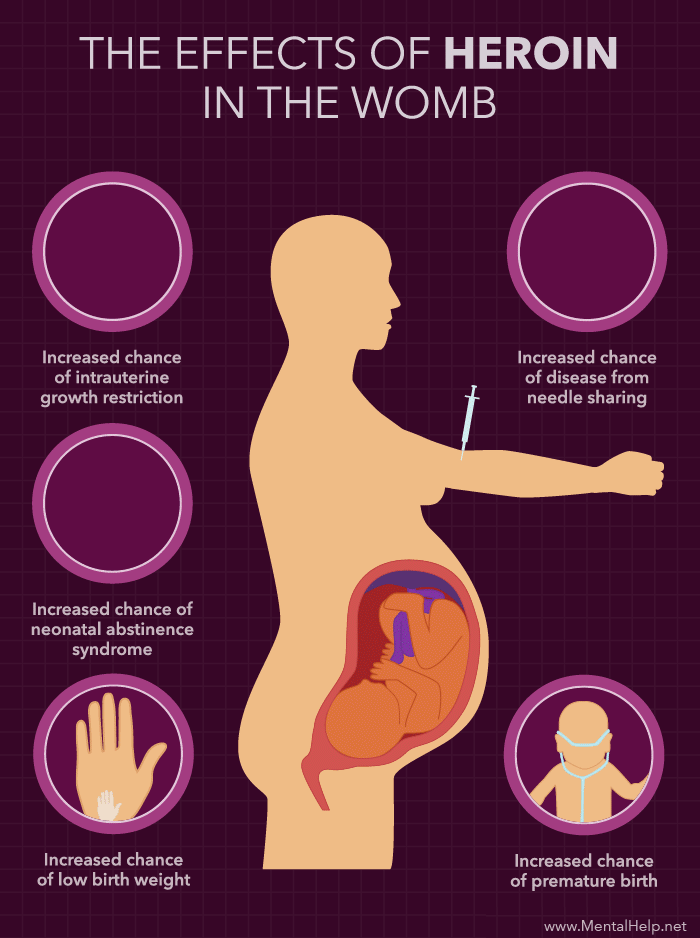
If a woman has chlamydia when giving birth, the baby might become infected during delivery. These babies can develop an eye infection (conjunctivitis) or pneumonia, and might need antibiotics. Chlamydia has also been associated with low birthweight.
The antibiotics used to treat chlamydia are safe in pregnancy and are used in pregnant women for many other types of infections.
Sources:
Australian Sexual Health Alliance (STI Management Guidelines for use in primary care; Chlamydia), King Edward Memorial Hospital Women and Newborn Health Service (Chlamydia clinical practice guideline), Lab Tests Online AU (Chlamydia), Melbourne Sexual Health Centre (National Management Guidelines for Sexually Transmissible Infections - Chlamydia), NSW Health (Chlamydia fact sheet)Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: November 2020
Back To Top
Related pages
- Routine antenatal tests
- Antenatal care during your pregnancy
Need more information?
Chlamydia - MyDr.com.au
Chlamydia is a sexually transmitted infection (STI). It affects both men and women, and it's spread by having sex with a person who has the infection.
Read more on myDr website
Chlamydia - Better Health Channel
Chlamydia is often called the 'silent infection' because most people do not realise they have it.
Read more on Better Health Channel website
Chlamydia fact sheet - Fact sheets
Chlamydia is a sexually transmissible infection.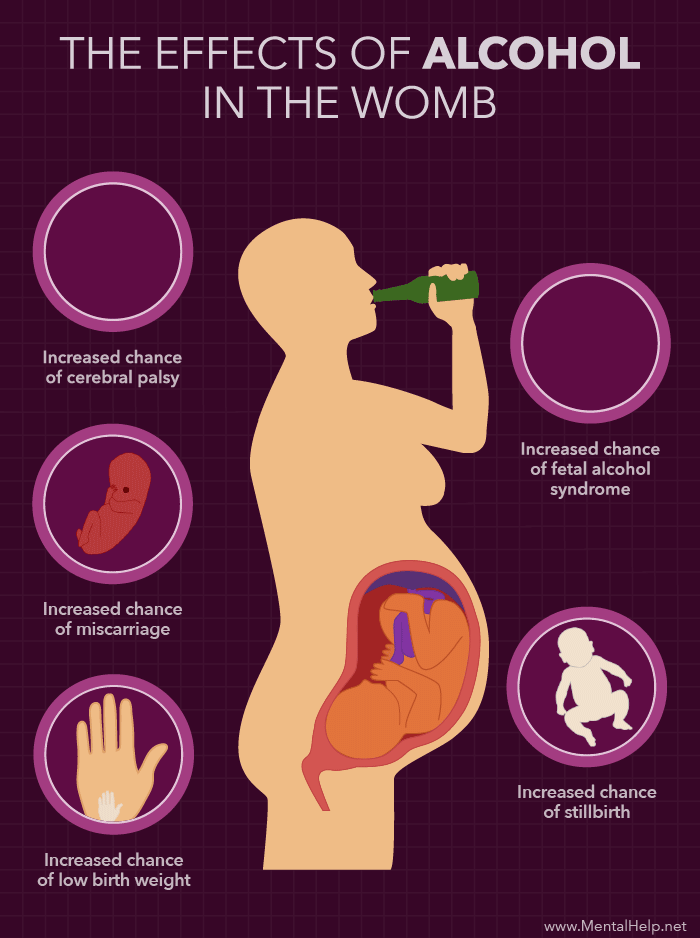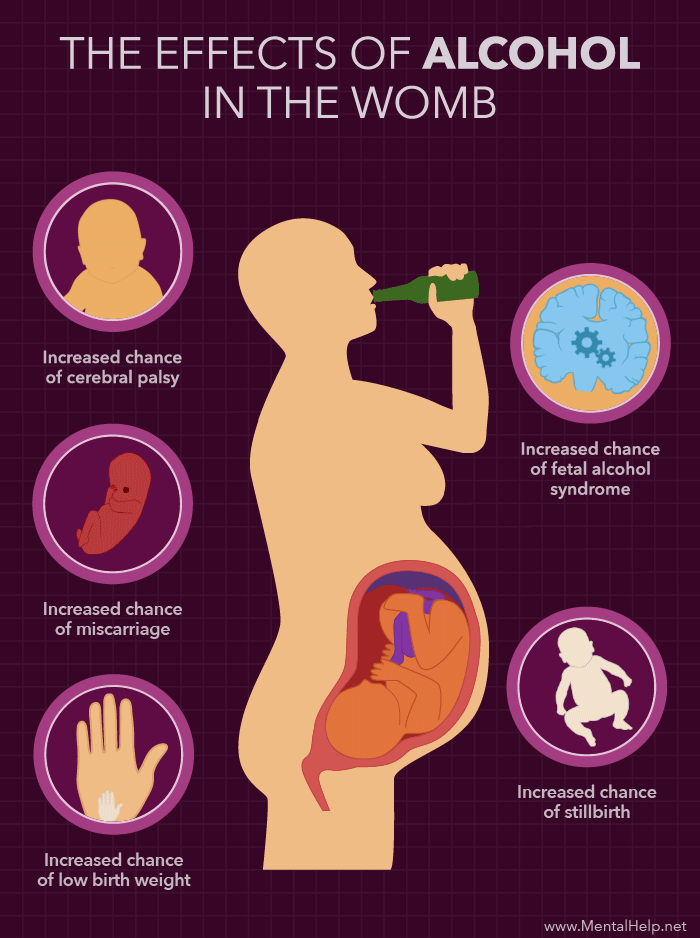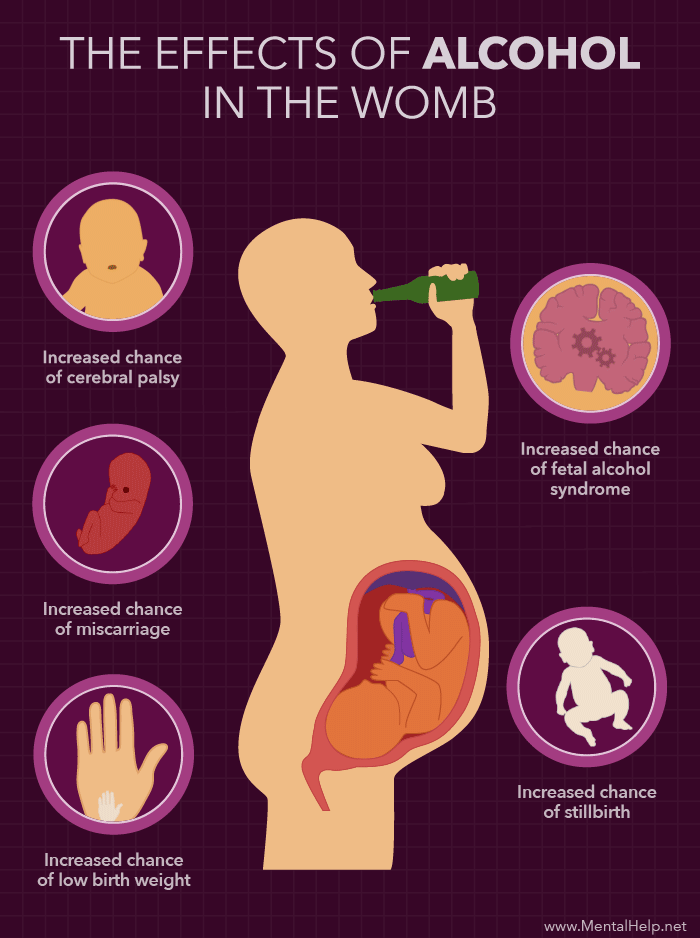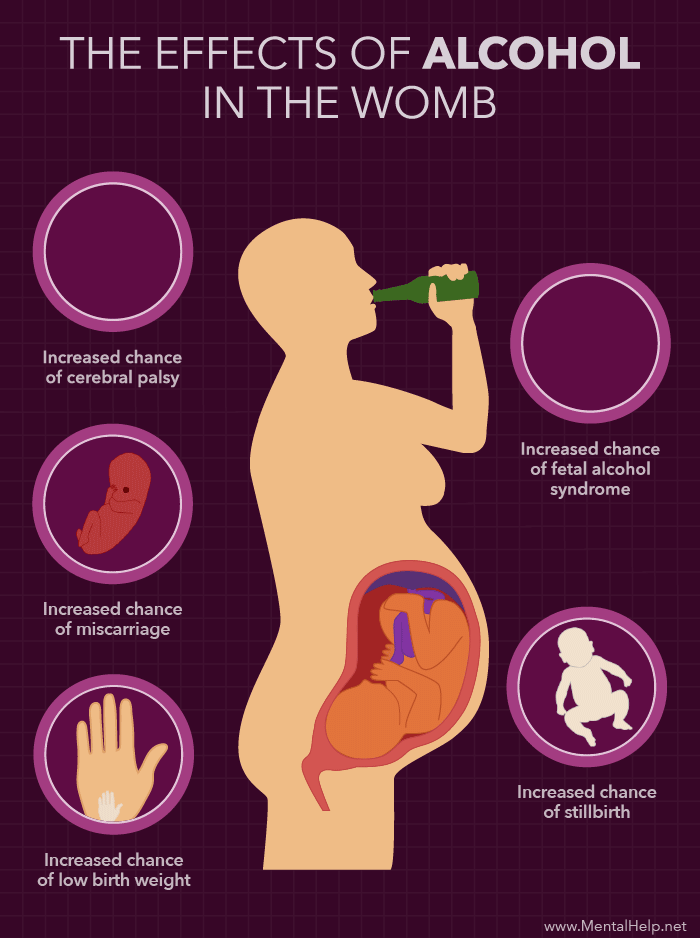 Many people who are infected do not have symptoms of infection but can still spread the disease. Chlamydia can lead to infertility, and other complications if not treated.
Many people who are infected do not have symptoms of infection but can still spread the disease. Chlamydia can lead to infertility, and other complications if not treated.
Read more on NSW Health website
Chlamydia | Family Planning NSW
Chlamydia is a common sexually transmitted infection (STI) caused by a bacteria. It affects both men and women. Most people with chlamydia do not have symptoms. This means you can pass the infection to a partner without knowing it. Having a regular sexual health check-up can help you find out if you have chlamydia.
Read more on Family Planning NSW website
Chlamydia treatment for your partner - Play Safe
Did you know it’s possible for your partner to get treated for Chlamydia without ever having to see a GP or go to a sexual health clinic? This is known as Patient Delivered Partner Therapy (PDPT)
Read more on NSW Health website
The facts about Chlamydia, what it is, how to prevent it, and how to treat it
Chlamydia is on the rise in Australia and it’s the most important thing for young people to test for.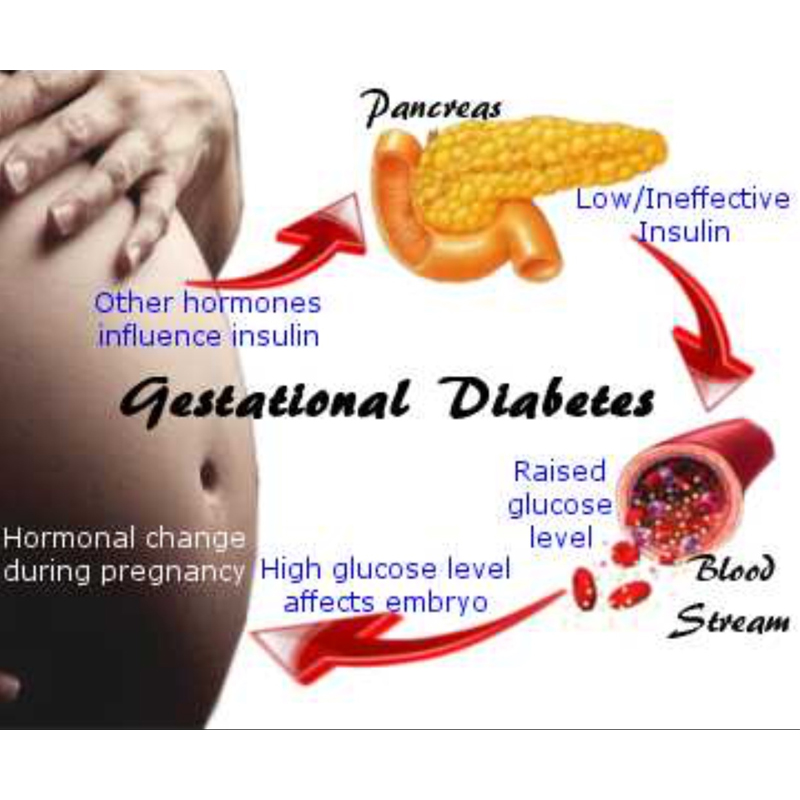 It often doesn’t have any symptoms which means that it’s easy to miss without regular STI testing.
It often doesn’t have any symptoms which means that it’s easy to miss without regular STI testing.
Read more on NSW Health website
Trachoma - Eye Infection
Trachoma is a preventable eye condition caused by repeated infections with eye strains of the bacterium Chlamydia trachomatis that lead to a roughening of the inner surface of the eyelid.
Read more on Queensland Health website
Gonorrhoea | Family Planning NSW
Gonorrhoea is a bacterial sexually transmitted infection (STI). It is spread through vaginal, anal or oral sex, or by the fingers and hands from the genitals to the eyes. It is less common in the general community than other STIs such as chlamydia.
Read more on Family Planning NSW website
Sexually transmitted infections (STIs) | Healthy Male
A sexually transmitted infection (STI) is an infection you get or give during sexual activity.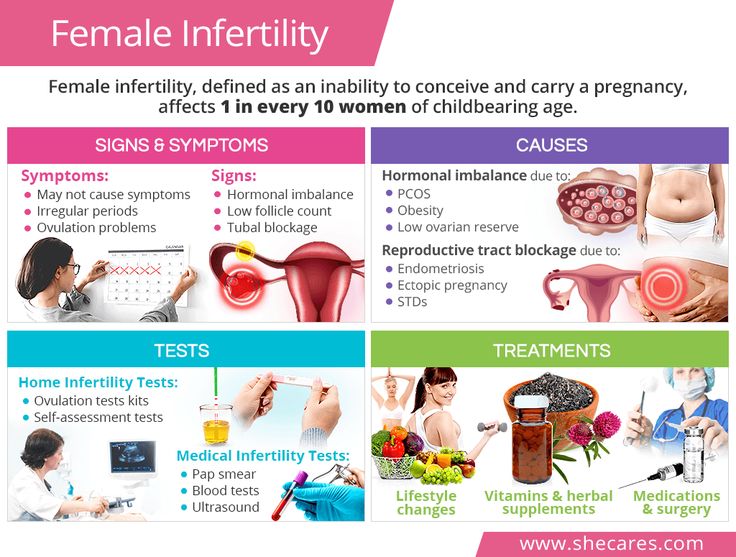 STIs can be caused by viruses (e.g., human immunodeficiency virus, herpes), bacteria (e.g., gonorrhea, syphilis), or parasites (e.g., pubic lice).
STIs can be caused by viruses (e.g., human immunodeficiency virus, herpes), bacteria (e.g., gonorrhea, syphilis), or parasites (e.g., pubic lice).
Read more on Healthy Male - Andrology Australia website
STIs and pregnancy
Sexually transmitted infections (STIs), if left untreated, can cause serious problems for both mother and child.
Read more on Pregnancy, Birth & Baby website
Disclaimer
Pregnancy, Birth and Baby is not responsible for the content and advertising on the external website you are now entering.
OKNeed further advice or guidance from our maternal child health nurses?
1800 882 436
Video call
- Contact us
- About us
- A-Z topics
- Symptom Checker
- Service Finder
- Linking to us
- Information partners
- Terms of use
- Privacy
Pregnancy, Birth and Baby is funded by the Australian Government and operated by Healthdirect Australia.
Pregnancy, Birth and Baby is provided on behalf of the Department of Health
Pregnancy, Birth and Baby’s information and advice are developed and managed within a rigorous clinical governance framework. This website is certified by the Health On The Net (HON) foundation, the standard for trustworthy health information.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
This information is for your general information and use only and is not intended to be used as medical advice and should not be used to diagnose, treat, cure or prevent any medical condition, nor should it be used for therapeutic purposes.
The information is not a substitute for independent professional advice and should not be used as an alternative to professional health care. If you have a particular medical problem, please consult a healthcare professional.
Except as permitted under the Copyright Act 1968, this publication or any part of it may not be reproduced, altered, adapted, stored and/or distributed in any form or by any means without the prior written permission of Healthdirect Australia.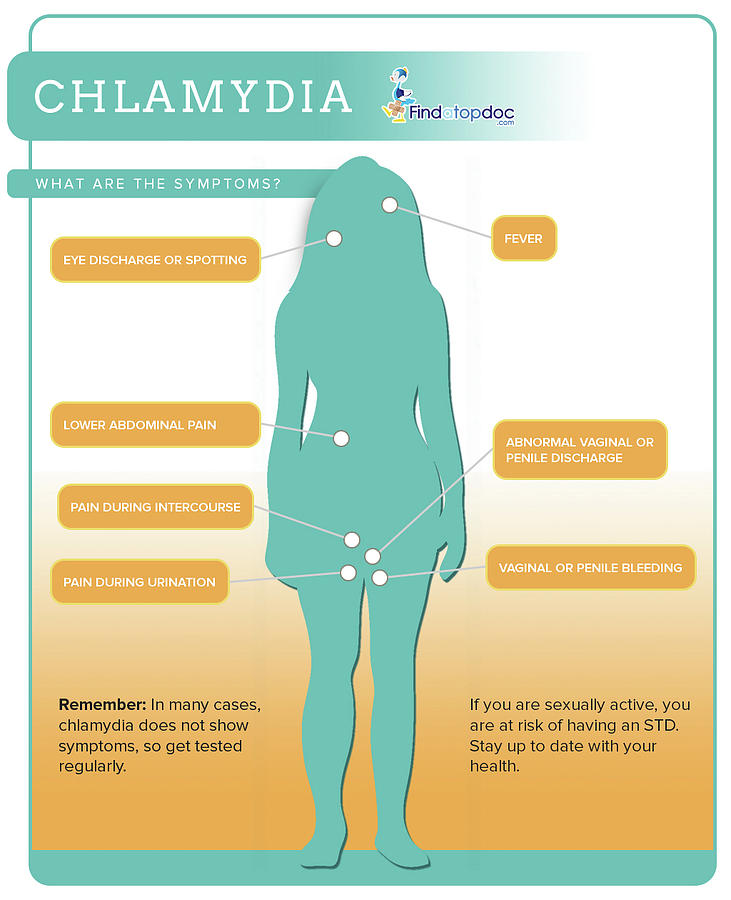
Support this browser is being discontinued for Pregnancy, Birth and Baby
Support for this browser is being discontinued for this site
- Internet Explorer 11 and lower
We currently support Microsoft Edge, Chrome, Firefox and Safari. For more information, please visit the links below:
- Chrome by Google
- Firefox by Mozilla
- Microsoft Edge
- Safari by Apple
You are welcome to continue browsing this site with this browser. Some features, tools or interaction may not work correctly.
Chlamydia During Pregnancy - American Pregnancy Association
Navigating pregnancy is difficult enough, but the addition of having a sexually transmitted infection (STI) like chlamydia during pregnancy can add more stress. If you think you may have an STI during your pregnancy, it is crucial that you talk to your healthcare provider and get tested right away. If you think you may have (or have already been diagnosed with chlamydia during your pregnancy), you probably have a lot of questions about how the infection could affect your baby and your prenatal care. Answers to all these questions are presented below!
If you think you may have (or have already been diagnosed with chlamydia during your pregnancy), you probably have a lot of questions about how the infection could affect your baby and your prenatal care. Answers to all these questions are presented below!
Chlamydia is a bacterial infection and is the most commonly reported bacterial STI. It is often symptomless, making it difficult to diagnose without running tests. The Centers for Disease Control (CDC) suggests that all pregnant women be screened at their first prenatal visit, and additionally if any symptoms appear or if risk factors are present.
The CDC estimates that there are 2.86 million infections each year in the USA, with some individuals accounting for multiple cases.
What are the symptoms of chlamydia during pregnancy?
In most cases, there are no symptoms. Some women may experience vaginal discharge and/or pelvic or abdominal pain.
Males usually have pain while urinating and may have a discharge from the penis. If you are pregnant and you notice your partner is experiencing these symptoms, you should both be screened for STIs like chlamydia.
If you are pregnant and you notice your partner is experiencing these symptoms, you should both be screened for STIs like chlamydia.
Am I at risk for contracting chlamydia during my pregnancy?
Anyone who is sexually active (outside of a monogamous relationship where you both have not had previous sexual partners) is at risk for contracting chlamydia via vaginal, anal, or oral sex.
You have the highest risk of contracting chlamydia during your pregnancy if you are sexually active and:
- Have multiple sexual partners,
- Have sex without a condom,
- Have had a previous or current STI, and/or
- Have a partner with an STI.
How will chlamydia affect my pregnancy?
The largest risk to the fetus is if the infection goes untreated. The CDC suggests that all pregnant women be tested at the first prenatal appointment.
If you are at a higher risk for contracting STIs during your pregnancy (i.e. have a new sexual partner or multiple partners), an additional test should be done in the third trimester so that treatment can be started before delivery.
If you have an active or untreated chlamydia infection during delivery, the baby has a chance of contracting the infection that will affect the baby in one of two ways: chlamydial conjunctivitis (18-44% of cases) or chlamydial pneumonia (3-16%).
The CDC also states that an active chlamydia infection during pregnancy increases the risk of preterm delivery.
Can my baby get chlamydia from me?
Yes, chlamydia may be spread from mother to child during birth (perinatal transmission).
The best way to prevent passing chlamydia to your baby during birth is to clear the infection before you are due. This is why first and third trimester screenings are so important, as well as reporting any new symptoms to your doctor.
How is chlamydia diagnosed?
Chlamydia may be diagnosed by your healthcare provider using a lab test to assess the secretions from the infected area which may include the cervix, urethra, anus, or throat. The lab may also use a urine sample for testing.
How is chlamydia treated during pregnancy?
Chlamydia may be treated and cured with antibiotics administered orally. This may be either a single dose or a 7-day course. The antibiotics used are typically safe during pregnancy.
If you continue seeing symptoms after a few days into the antibiotic treatment, you should return to your doctor for another evaluation. The CDC suggests that pregnant women who are treated for chlamydia infection should be retested at 3 weeks and 3 months post-treatment since reinfection is somewhat common.
How can I prevent getting chlamydia during pregnancy?
There are only two 100% effective ways to prevent chlamydia. The first is to refrain from sexual contact of any kind. The second is to be in a long-term monogamous relationship such as marriage in which both of you test negative for STIs.
According to the Sexuality Information and Education Council of the United States (SIECUS), the consistent and correct use of condoms can decrease the risk of contracting chlamydia during vaginal, oral, or anal intercourse by only 60%.
Compiled using information from the following sources:
1. Centers for Disease Control and Prevention (CDC)
https://www.cdc.gov/std/chlamydia/stdfact-chlamydia-detailed.htm
2. Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/chlamydia-trachomatis/symptoms-causes/dxc-20315310
3. Sexuality Information and Education Council of the United States (SIECUS)
Chlamydia and pregnancy
Their favorite habitat is the cervix (more precisely, the mucous membrane of the cervical canal). It is there that they are located in colonies, i.e. are not found throughout. Such frequent cases are associated with this fact, when one doctor takes a smear from the cervical canal and chlamydia is found in it, and the other one also takes a smear a day later, but chlamydia is not found again. That is why the diagnostic value of swabs for chlamydia is quite low - about 30%.
How chlamydia manifests itself
During an exacerbation of the infectious process, women's complaints may be different, depending on the level of chlamydia spread.
When chlamydia is found in the cervix, there may be slight discharge from the vagina, accompanied by moderate pulling pains in the lower abdomen, which is typical with local exacerbation of the process (there are practically no complaints in the chronic form). If the infection spreads higher (uterine cavity, tubes), then the complaints are more pronounced, because, for example, inflammation of the appendages may begin.
Exacerbation of chlamydial infection is especially dangerous during pregnancy, as it can lead to various complications.
Possible complications:
- early miscarriages are possible,
- late term premature amniotic fluid and preterm labor,
- in childbirth, there is a high probability of infection of the fetus (conjunctivitis, pharyngitis, otitis and even pneumonia).
Chlamydia diagnostics
The most informative method is a blood test for antibodies (immunoglobulins) to chlamydia. If a small concentration of these antibodies is detected, then they speak of a chronic carriage of chlamydia. If the concentration is high, there is an exacerbation of chlamydial infection.
If a small concentration of these antibodies is detected, then they speak of a chronic carriage of chlamydia. If the concentration is high, there is an exacerbation of chlamydial infection.
The diagnosis of "chlamydia" is legitimate when it is confirmed by two fundamentally different diagnostic methods: smear (microscopy) and blood for antibodies to chlamydia (biochemical method). Only when the titer (concentration) of antibodies is high and / or in the presence of complaints specific to this infection, a course of treatment is indicated.
Digits must be multiples, i.e. more or less than twice, from the previous one (IgA 1:40 and IgG 1:80). Titers of 1:5 and less are doubtful and negative. Elevated IgG numbers indicate that the process is chronic. In this case, treatment is indicated if there are certain complaints, or if before that, the person has never been treated for this infection. High numbers of IgA are mainly found in an acute process (primary infection) or during an exacerbation of a chronic one that needs treatment.
What to do if the test is positive?
It must be remembered that today there are almost no 100% reliable methods, including the ELISA method (enzymatic immunoassay) is no exception. Quite often there are “false positive” results - you have to do either repeated tests or use other, fundamentally different methods.
These can be:
- taking smears for the PIF method (examination with a luminescent microscope) - where there may also be “false positive” answers,
- PCR blood test (based on the principle of genetic engineering, the study of DNA or its fragments) - today, its reliability is very high.
In the search for the truth of the diagnosis, quite often, everything can rest either on the financial capabilities of patients, or on the insufficient equipment of a particular laboratory. The better the body's defenses, the less likely it is to contract chlamydia. In which case, only “carriage” threatens you, it is not dangerous for you (only IgG, in low titers, will be determined in the blood test).
It is considered optimal if the whole family is examined at the same time (all interested persons, including children), because in this case, it is possible to identify who is at what stage and monitor the effectiveness of treatment.
In most cases, the pathogens of ureplasmosis and mycoplasmosis do not manifest themselves (hidden bacteriocarrier), and only when the process is exacerbated, they cause pregnancy complications similar to chlamydia and infection of the fetus. Therefore, when examining women who have had the above problems in the past, swabs and blood are taken at least immediately for these three pathogens. By the way, studies have shown that taking hormonal birth control pills reduces the risk of chlamydia infection, this effect is associated with an increase in the protective properties of cervical mucus (its permeability to bacteria decreases). As mentioned above, chlamydia is dangerous for pregnant women.
What to do?
But what to do if, after all, doctors found chlamydia in the acute stage in the expectant mother?
The placenta can be thought of as a mesh filter through which large molecules cannot pass (they remain in the mother's body). Therefore, in the treatment of a pregnant woman, antibiotics are used that are harmless to the fetus (i.e. those that do not pass through the placenta). These include drugs whose molecular weight is greater than the "capacity" of the capillaries. However, when taking these drugs, the effect on the fetus is still possible. The antibiotic acts primarily on the mother's body, however, during the period of treatment, it changes the metabolism in the body, which in turn affects the metabolism of the fetus. Antibiotics are always prescribed in short courses so that the effects are minimal.
Therefore, in the treatment of a pregnant woman, antibiotics are used that are harmless to the fetus (i.e. those that do not pass through the placenta). These include drugs whose molecular weight is greater than the "capacity" of the capillaries. However, when taking these drugs, the effect on the fetus is still possible. The antibiotic acts primarily on the mother's body, however, during the period of treatment, it changes the metabolism in the body, which in turn affects the metabolism of the fetus. Antibiotics are always prescribed in short courses so that the effects are minimal.
References
- Zofkie AC., Fomina YY., Roberts SW., McIntire DD., Nelson DB., Adhikari EH. Effectiveness of Chlamydia Trachomatis expedited partner therapy in pregnancy. // Am J Obstet Gynecol - 2021 - Vol - NNULL - p.; PMID:33894150
- Zofkie AC., Fomina YY., Roberts SW., McIntire DD., Nelson DB., Adhikari EH. Effectiveness of Chlamydia Trachomatis expedited partner therapy in pregnancy.
 // Am J Obstet Gynecol - 2021 - Vol - NNULL - p.; PMID:33894147
// Am J Obstet Gynecol - 2021 - Vol - NNULL - p.; PMID:33894147 - Shilling HS., Garland SM., Costa AM., Marceglia A., Fethers K., Danielewski J., Murray G., Bradshaw C., Vodstrcil L., Hocking JS., Kaldor J., Guy R., Machalek D.A. Chlamydia trachomatis and Mycoplasma genitalium prevalence and associated factors among women presenting to a pregnancy termination and contraception clinic, 2009-2019. // Sex Transm Infect - 2021 - Vol - NNULL - p.; PMID:33782146
- Vercruysse J., Mekasha S., Stropp LM., Moroney J., He X., Liang Y., Vragovic O., Valle E., Ballard J., Pudney J., Kuohung W., Ingalls RR. Chlamydia trachomatis Infection, when Treated during Pregnancy, Is Not Associated with Preterm Birth in an Urban Safety-Net Hospital. // Infect Dis Obstet Gynecol - 2020 - Vol2020 - NNULL - p.8890619; PMID:33082702
- Olaleye AO., Babah OA., Osuagwu CS., Ogunsola FT., Afolabi BB. Sexually transmitted infections in pregnancy - An update on Chlamydia trachomatis and Neisseria gonorrhoeae.
 // Eur J Obstet Gynecol Reprod Biol - 2020 - Vol255 - NNULL - p.1-12; PMID:33059307
// Eur J Obstet Gynecol Reprod Biol - 2020 - Vol255 - NNULL - p.1-12; PMID:33059307 - Hoenderboom BM., van Bergen JEAM., Dukers-Muijrers NHTM., Götz HM., Hoebe CJPA., de Vries HJC., van den Broek IVF., de Vries F., Land JA., van der Sande MAB., Morré SA., van Benthem BHB. Pregnancies and Time to Pregnancy in Women With and Without a Previous Chlamydia trachomatis Infection. // Sex Transm Dis - 2020 - Vol47 - N11 - p.739-747; PMID:32701764
- He W., Jin Y., Zhu H., Zheng Y., Qian J. Effect of Chlamydia trachomatis on adverse pregnancy outcomes: a meta-analysis. // Arch Gynecol Obstet - 2020 - Vol302 - N3 - p.553-567; PMID:32643040
- Freeman J., Pettit J., Howe C. Chlamydia test-of-cure in pregnancy. // Can Fam Physician - 2020 - Vol66 - N6 - p.427-428; PMID:32532724
- Rajabpour M., Emamie AD., Pourmand MR., Goodarzi NN., Asbagh FA., Whiley DM. Chlamydia trachomatis, Neisseria gonorrhoeae, and Trichomonas vaginalis among women with genitourinary infection and pregnancy-related complications in Tehran: A cross-sectional study.
 // Int J STD AIDS - 2020 - Vol31 - N8 - p.773-780; PMID:32517577
// Int J STD AIDS - 2020 - Vol31 - N8 - p.773-780; PMID:32517577 - Goggins ER., Chamberlain AT., Kim TG., Young MR., Jamieson DJ., Haddad LB. Patterns of Screening, Infection, and Treatment of Chlamydia trachomatis and Neisseria gonorrhea in Pregnancy. // Obstet Gynecol - 2020 - Vol135 - N4 - p.799-807; PMID:32168225
Reproductive Health Education Center Reproductive Health Education Center
Pregnancy is a happy period in every woman's life. Everyone knows how important it is to take care of your health during this period, because during pregnancy any infection is dangerous not only for the mother, but also for the health of the unborn baby. In pregnant women, immunity is always slightly reduced: a change in the immune status is a physiological response to pregnancy. Reduced immunity is necessary for the expectant mother so that her body does not reject the fetus, perceiving it as a foreign object. That is why the body of the expectant mother during pregnancy becomes extremely vulnerable to infections that lie in wait for a woman at every turn. Unfortunately, no one is immune from various diseases during this period. Venereal diseases are no exception. In particular, chlamydia is quite common during pregnancy.
Unfortunately, no one is immune from various diseases during this period. Venereal diseases are no exception. In particular, chlamydia is quite common during pregnancy.
The effect of chlamydia on pregnancy can be extremely detrimental, which is why it is very important to know what are the symptoms of the disease, what are the dangers of chlamydia for the unborn child, how to treat the infection so as not to harm the fetus.
The danger of chlamydia in pregnant women lies in the fact that very often it occurs in a latent form. After a rather long incubation period, mild signs of the disease may appear, which are easy to mistake for a common ailment, but they may be absent altogether if the woman does not suffer from serious diseases and immunodeficiency. If chlamydia is not recognized in time in the blood of a pregnant patient, they can cause premature miscarriage or intrauterine infection of the fetus, which often leads to serious malformations and disorders in the formation of the body of the unborn baby.
What is Chlamydia trachomatis?
The nature of the pathogen easily explains why chlamydia is so difficult to recognize and treat. Chlamydia are intracellular parasites. They combine the features of bacteria and viruses at the same time. They are much larger than bacteria, but do not reach the usual size of viruses. Getting into the external environment, chlamydia quickly die, so the disease is not transmitted by contact-household method. Once in the human body, the pathogen begins to feed on energy from the cells, affecting the genitourinary system. Chlamydia during pregnancy affects not only the vulva, cervix, fallopian tubes and ovaries, but also the fetal membranes. This is especially dangerous for the health and life of the unborn child.
Causes of disease
The source of the disease is an infected sexual partner. Chlamydia is transmitted exclusively through sexual intercourse, if barrier contraception was not used during sexual intercourse. A woman's sexual partner may be a carrier of chlamydia, but due to the latent course of the disease, he may not be aware of its existence. That is why it is so important during pregnancy to undergo a comprehensive examination for the presence of a variety of diseases, which includes PCR for chlamydia. Timely detected chlamydia is treated quite successfully (see a detailed article about the treatment of chlamydia during pregnancy). Pregnancy after treatment and during it proceeds in most cases favorably if the doctor recognizes the infection in time and takes all measures to eliminate it safely and effectively.
A woman's sexual partner may be a carrier of chlamydia, but due to the latent course of the disease, he may not be aware of its existence. That is why it is so important during pregnancy to undergo a comprehensive examination for the presence of a variety of diseases, which includes PCR for chlamydia. Timely detected chlamydia is treated quite successfully (see a detailed article about the treatment of chlamydia during pregnancy). Pregnancy after treatment and during it proceeds in most cases favorably if the doctor recognizes the infection in time and takes all measures to eliminate it safely and effectively.
The cause of intrauterine infection of the fetus is the penetration of chlamydia into the fluid surrounding the fetus. After infection of the fetal membrane, the infection of the fetus itself also occurs, since the child, while in the womb, regularly swallows a small amount of amniotic fluid.
Why are chlamydia dangerous during pregnancy?
In addition to its usual complications, chlamydia in pregnant women can lead to the following adverse effects:
- Complicated pregnancy, threatened miscarriage
- Early and late miscarriages
- Intolerable toxicosis
- Inflammatory processes in the endometrium, inflammation of the mucous membranes of the uterus and vagina
- Inflammation of the amniotic membrane, negatively affecting the development of the child, since the amniotic membrane is involved in the supply of nutrients to the fetus
- Increased risk of preterm birth
- Development of intrauterine diseases in a child (anemia, pneumonia, conjunctivitis).
 Chlamydia affects the mucous membrane of the child's eyes, as well as the upper respiratory tract and lungs.
Chlamydia affects the mucous membrane of the child's eyes, as well as the upper respiratory tract and lungs. - It is very common for pregnant women with chlamydia to have premature babies.
How does chlamydia appear during pregnancy?
Symptoms of the disease are identical to normal chlamydia. Usually the signs are quite weak and resemble urethritis or cystitis. A woman experiences discomfort and burning during urination, scanty and cloudy discharge from the urethra is observed. The discharge may contain pus. Pain in the lower abdomen and pain when urinating often cause the initial stage of chlamydia to be mistaken for cystitis.
In some cases, chlamydia in pregnant women can occur without inflammation in the urinary tract. The infection immediately affects the inner lining of the uterus, as well as the mucous membrane of the cervix. There is swelling of the cervix, its epithelium begins to collapse, erosion of varying severity develops.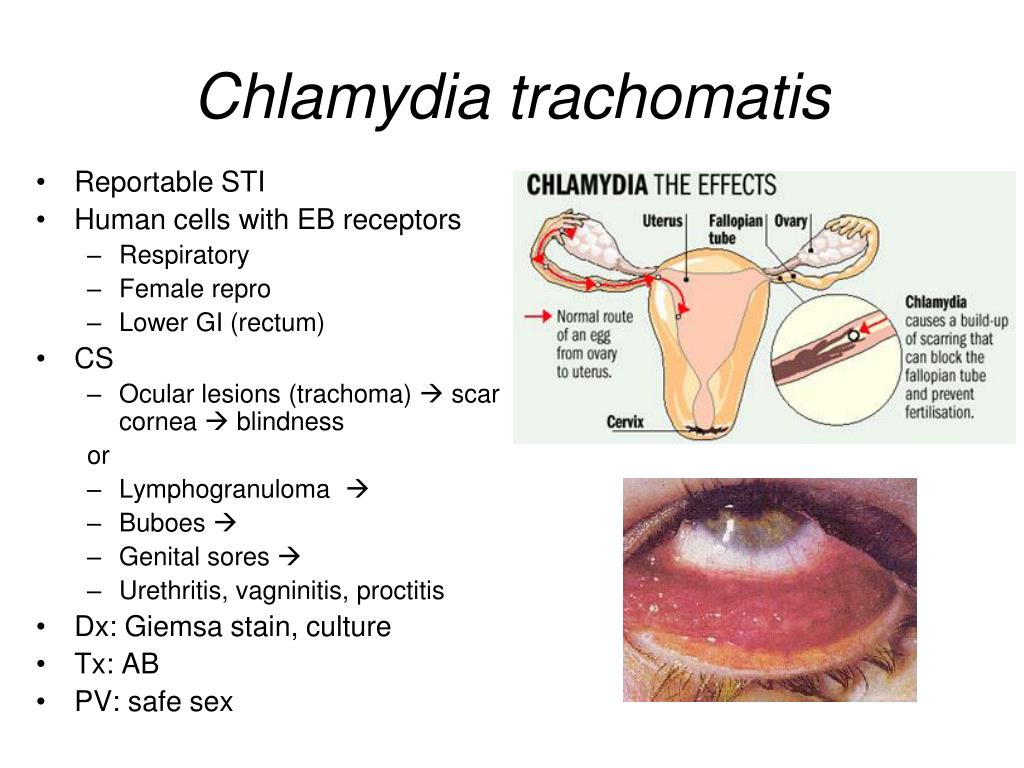
Due to hormonal changes, a pregnant woman may also develop chlamydial colpitis (inflammation of the vagina), which is not typical for ordinary patients.
How to treat chlamydia in pregnant women?
As mentioned above, the most important stage from which treatment begins is the recognition of infection, for which serious examinations are prescribed. As for the treatment itself, not all antibacterial drugs are suitable for pregnant women. The task for the doctor in this case is complicated, since he will not only have to draw up an individual treatment regimen, but also choose antibiotics that will be as safe as possible and will not have contraindications. Most often, antibiotics of the tetracycline group are used to treat chlamydia, but they are highly undesirable for use during pregnancy. In this regard, doctors use antibiotics from the pharmacological group of macrolides to treat expectant mothers. Drugs are also prescribed to eliminate dysbacteriosis and restore the normal microflora of the vagina, as well as drugs that stimulate and strengthen the immune system.