My body at 5 weeks pregnant
5 Weeks Pregnant | Pregnancy
When you're pregnant, you have lots of questions. Our week-by-week pregnancy guide is packed with lots of useful information. From what's happening inside your body, to how your baby is developing, and tips and advice on having a healthy pregnancy – this is your one-stop pregnancy guide!
- 1st trimester
- 2nd trimester
- 3rd trimester
Our week-by-week pregnancy guide is full of essential information. From early pregnancy symptoms to how your baby is growing and developing, you' ll find it all here.
- Week 4
- Week 5
- Week 6
- Week 7
- Week 8
- Week 9
- Week 10
- Week 11
- Week 12
To the outside world, you'll look much the same as usual – but on the inside, some amazing things are happening.
What's happening in my body?
Your baby's nervous system is developing, and the brain and spinal cord are taking shape. The tiny heart is starting to form and will beat for the first time around now.
Many women realise that they're pregnant around week 5. You might notice that your period is late, and you may feel a bit under the weather. If you're wondering when to take a pregnancy test, now is a good time as they are sensitive to changes in your urine from week 3 or 4 onwards.
Finding out that you are pregnant can be exciting, but it's normal to have worries too. More than 1 in 10 mums feel anxious during pregnancy. Try not to keep your worries to yourself – talk to your midwife or doctor. You could also try doing some relaxing breathing exercises.
Food cravings
Are you getting food cravings? Some people do, some don't. Pregnancy cravings are caused by hormonal changes affecting your senses of taste and smell. Try to eat a balanced healthy diet.
If you have any unusual cravings, like wanting to eat dirt, talk to your midwife or doctor, as you may have a condition called pica which is caused by a lack of iron.
Early pregnancy symptoms (at 5 weeks)
It's still early days, and many women won't know they're pregnant at 5 weeks. Not everyone has regular menstrual cycles, so you may not realise that your period is late. You might notice some light bleeding, and think it's your period, but it can also be a sign of implantation bleeding (when an embryo attaches to the lining of the womb).
In the 1st trimester, many women feel extreme tiredness. Other early signs of pregnancy can include:
- a metallic taste in your mouth
- sore breasts
- nausea - also known as "morning sickness", although you can experience it at any time (read about morning sickness in week 6)
- mood swings (week 8's page has information on mood swings)
- new food likes and dislikes
- a heightened sense of smell
- needing to pee more frequently
- a milky white pregnancy discharge from your vagina
- light spotting (see your doctor if you get bleeding in pregnancy)
- cramping, a bit like period pains
- darkened skin on your face or brown patches – this is known as chloasma faciei or the "mask of pregnancy"
- thicker and shinier hair
- bloating (read about bloating on week 16's page)
Read Tommy's guide to common pregnancy symptoms.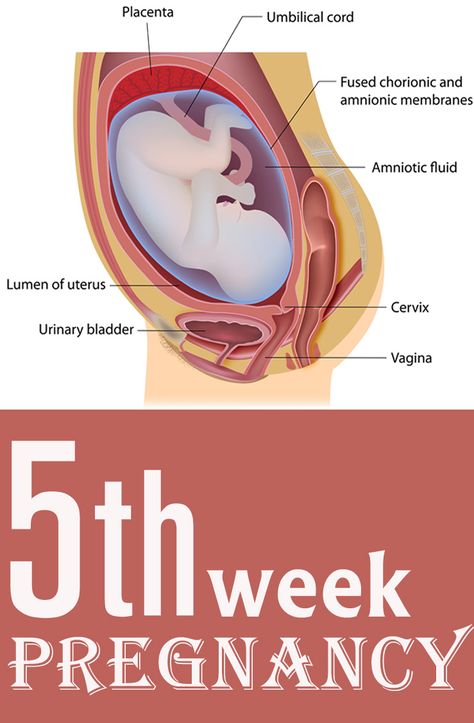
What does my baby look like?
Your baby, or embryo, is around 2mm long (about the size of a sesame seed). The face is starting to take shape, with a tiny nose and little eyes which stay closed until around 28 weeks. Your baby's brain and spinal cord are forming rapidly inside you.
Your baby already has some of its own blood vessels and a string of them will make up the umbilical cord. This cord delivers everything it needs from the placenta. The placenta, which is being created now, will give your baby nutrients and oxygen, while removing waste products.
Action stations
The advice for week 5 is the same as for week 4 - basically keep up the good work looking after yourself!
In particular:
Share the news with your GP or ask for an appointment with a midwife at your doctors' surgery. Alternatively you can refer yourself to your local hospital – look for contact details on their website.
You'll need to arrange a booking appointment. This usually takes place between weeks 8 and 12 and takes around an hour. You can talk about the options for your pregnancy and the birth. You will also be offered screening tests for infectious diseases and conditions such as Down's syndrome. Now is a good time to ask about the Maternity Transformation Programme and how it could benefit you.
This usually takes place between weeks 8 and 12 and takes around an hour. You can talk about the options for your pregnancy and the birth. You will also be offered screening tests for infectious diseases and conditions such as Down's syndrome. Now is a good time to ask about the Maternity Transformation Programme and how it could benefit you.
You will be offered your first dating scan at 8 to 14 weeks.
If it's your first pregnancy, you will probably have around 10 appointments and 2 scans in total.
Ask your midwife or doctor about online antenatal classes – they may be able to recommend one. The charity Tommy's has lots of useful information on antenatal classes and preparing you for birth.
Antenatal classes will give you the chance to meet other people and prepare you for parenthood. The NCT offers online antenatal classes with small groups of people that live locally to you.
Take prenatal vitamins. You're advised to take 400 micrograms of folic acid, every day, until at least week 12. This helps your baby's nervous system to form and offers some protection from conditions such as spina bifida.
This helps your baby's nervous system to form and offers some protection from conditions such as spina bifida.
To keep bones and muscles healthy, we need vitamin D. From late March/early April to the end of September, most people make enough vitamin D from sunlight on their skin. However, between October and early March, consider taking a daily vitamin D supplement because we cannot make enough from sunlight.
Some people should take a vitamin D supplement all year round, find out if this applies to you on the NHS website. You just need 10 micrograms (it's the same for grown-ups and kids). Check if you're entitled to free vitamins.
Do you think you or your partner could have a sexually transmitted infection (STI)? If so, get it checked out, as this could affect your baby's development. Talk to your midwife or GP, or visit a sexual health clinic.
It's recommended that you do 150 minutes of exercise a week while pregnant. You could start off with just 10 minutes of daily exercise - perhaps take a brisk walk outside.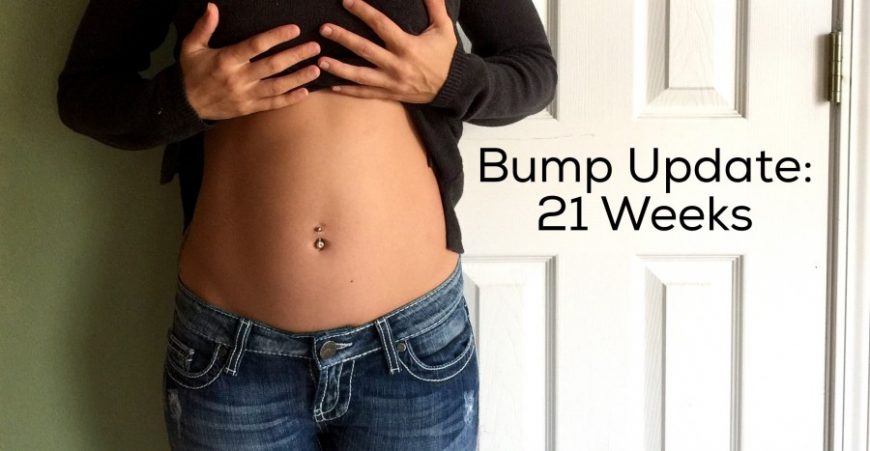 Check out Sport England's #StayInWorkOut online exercises (scroll to the pregnancy section). Listen to your body and do what feels right for you.
Check out Sport England's #StayInWorkOut online exercises (scroll to the pregnancy section). Listen to your body and do what feels right for you.
There's no need to eat for 2. If you pile on the pounds, you could put you and your baby at risk of health problems such as high blood pressure. Eat healthily, with plenty of fresh fruit and veg, and avoid processed, fatty and salty foods. You may be able to get free milk, fruit and veg through the Healthy Start scheme.
If you have a long-term health condition, then let your specialist or GP know that you're pregnant as soon as possible. Don't stop taking any regular medication without discussing it first with your doctor.
How are you today? If you're feeling anxious or low, then talk to your midwife or doctor who can point you in the right direction to get all the support that you need.
You could also discuss your worries with your partner, friends and family. You may be worried about your relationship, or money, or having somewhere permanent to live. Don't keep it to yourself. It's important to ask for help if you need it.
Don't keep it to yourself. It's important to ask for help if you need it.
You and your family should follow the government and NHS guidance on coronavirus (COVID-19):
To find out about about COVID-19 and pregnancy, childbirth and breastfeeding, have a look at advice on the:
Go back to week 4
Go to week 6
5 Weeks Pregnant: Symptoms and Baby Development
5 Weeks Pregnant: Your Baby's Development
Even though you’re just five weeks pregnant, lots of changes are taking place. The placenta and the beginnings of the umbilical cord are developing in order to channel essential nutrients and oxygen from your body to the embryo.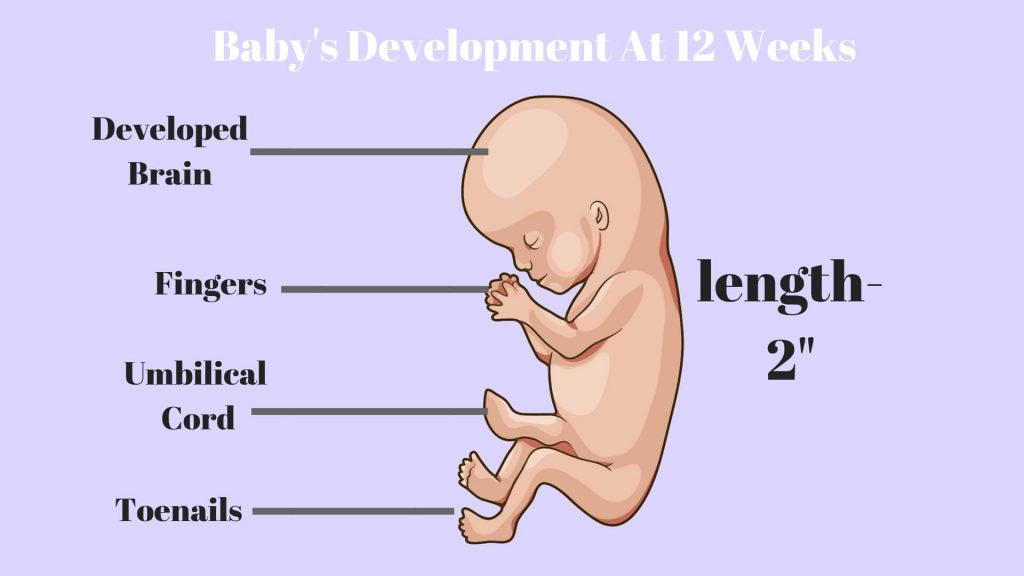 These nutrients, like calcium, folic acid, and other vitamins, all play a vital role in healthy development.
This week, the neural tube continues to develop; it will eventually become the spinal column and the brain. At this point, taking at least 400 micrograms of folic acid every day is a great way to support your baby’s healthy growth and development and reduce the risk of neural tube disorders.
Your baby's heart will develop from what is now just a bulge in the middle of the embryo, and the heartbeat itself may be detected as early as the sixth week of pregnancy.
These nutrients, like calcium, folic acid, and other vitamins, all play a vital role in healthy development.
This week, the neural tube continues to develop; it will eventually become the spinal column and the brain. At this point, taking at least 400 micrograms of folic acid every day is a great way to support your baby’s healthy growth and development and reduce the risk of neural tube disorders.
Your baby's heart will develop from what is now just a bulge in the middle of the embryo, and the heartbeat itself may be detected as early as the sixth week of pregnancy.
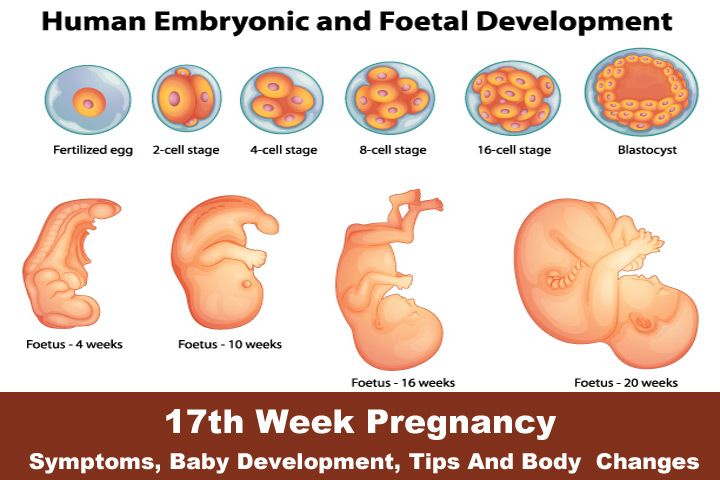
The Size of the Embryo at 5 Weeks Pregnant
At five weeks the embryo is still very small but growing quickly! Picture a small orange seed or a grain of rice. At this stage, your little one could be between 0.05 and 0.10 inches long, with a shape similar to that of a tiny tadpole.
Take a look at this visual for an idea of all the things that are happening to make your uterus a comfortable home for your baby during your pregnancy.
Mom's Body at 5 Weeks Pregnant
How do you feel knowing that you’re pregnant? If you’ve been trying to conceive for a while, you’re probably ecstatic. Whether you’ve been planning for this, it’s come as a beautiful surprise, or it’s all a bit of a shock, it’s natural to feel a range of other emotions like nervousness, happiness, hope, and wonder.
You may also find yourself wondering about all the changes in store and when you may be able to meet your little one. Try our Due Date Calculator to find out!
Some symptoms you may notice at five weeks pregnant include fatigue, nausea, and tender breasts, and they're all quite common.
You might like to read up on the pregnancy hormone hCG as it plays an important role in pregnancy.
Treat your hard-working body to a break by soaking in a warm bath, listening to some soothing music, or taking a nap.
You can also give yourself a boost and get your little one off to a great start by adopting healthier habits, starting with quitting smoking and eliminating alcoholic beverages. Talk to your healthcare provider about how to include moderate exercise in your pregnancy, and keep taking any prenatal vitamins your healthcare provider recommends or prescribes.
Talk to your healthcare provider about how to include moderate exercise in your pregnancy, and keep taking any prenatal vitamins your healthcare provider recommends or prescribes.
5 Weeks Pregnant: Your Symptoms
Although every mom-to-be is unique, these are some of the symptoms you may be experiencing at five weeks pregnant:
Morning sickness. Some women start to experience morning sickness at five weeks pregnant. Unpleasant, nauseous feelings can happen in the morning, evening, or all day long, and many women will also throw up. To deal with morning sickness, drink enough fluids to prevent dehydration and avoid any greasy, spicy, or fatty foods that may trigger your bouts of nausea. Many women with morning sickness benefit from eating small meals and snacks frequently.
Light bleeding or spotting. It’s common to see some spotting at five weeks pregnant, but there should be no more than a few drops of blood — not even enough to cover a small pantyliner.
 This is likely just implantation bleeding, but you’ll want to mention it to your doctor so that he or she can rule out complications. If you see a lot of blood, if the spotting lasts longer than two days, or you have any concerns, see your doctor right away.
This is likely just implantation bleeding, but you’ll want to mention it to your doctor so that he or she can rule out complications. If you see a lot of blood, if the spotting lasts longer than two days, or you have any concerns, see your doctor right away.
Breast tenderness. Around five weeks pregnant, a surge of hormones might cause your breasts to ache as they continue to stretch and grow in preparation for breastfeeding.
Frequent urination. The urgent need to pee can strike any time, especially as your kidneys are starting to have extra fluid to process, thanks to the increasing volume of blood in your body. Although this symptom can be annoying, it’s also completely normal.
Fatigue. Don’t be surprised if you feel completely wiped out. Your body is dealing with an increase in levels of progesterone, which can leave you feeling more tired than usual. Avoiding caffeine and vigorous activity before bed can help you sleep better at night.
 Try to keep your daily schedule regular, but also try not to overschedule yourself. It's important to find a healthy balance between your daily activities and rest time. And don't feel guilty about taking time to rest or nap when you need it. You'll be doing yourself and your little one a big favor by getting as much rest as you can now.
Try to keep your daily schedule regular, but also try not to overschedule yourself. It's important to find a healthy balance between your daily activities and rest time. And don't feel guilty about taking time to rest or nap when you need it. You'll be doing yourself and your little one a big favor by getting as much rest as you can now.
Mood swings. Happy one moment, crying the next? Mood swings are common when you're pregnant, and for some women they feel like PMS at its worst. It may help to find some ways to distract yourself when an unpleasant mood interferes with your normal routine. Try going for a walk or listening to music, for example.
Acne. Hormonal changes may be to blame for any pregnancy-related acne you are experiencing. Read up on how you can combat some of those spots and blemishes in our article on pregnancy acne, and remember that it’s just one of those pesky pregnancy that should clear once your baby is born.
Mild or no symptoms.
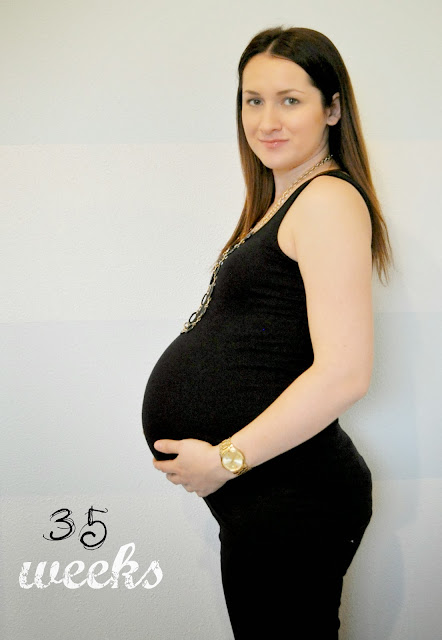 What if, at five weeks pregnant, you are symptom-free? It’s not unusual for women to feel and look completely normal at this stage, or for certain symptoms to come and go. As for that five weeks pregnant belly, it may appear unchanged, or it may be looking and feeling bloated. If you’ve got severe morning sickness, you may even lose a little bit of weight during the first trimester. Be sure to talk to your healthcare provider if you have questions about the changes that are taking place, or if the lack of any symptoms has you feeling uneasy.
What if, at five weeks pregnant, you are symptom-free? It’s not unusual for women to feel and look completely normal at this stage, or for certain symptoms to come and go. As for that five weeks pregnant belly, it may appear unchanged, or it may be looking and feeling bloated. If you’ve got severe morning sickness, you may even lose a little bit of weight during the first trimester. Be sure to talk to your healthcare provider if you have questions about the changes that are taking place, or if the lack of any symptoms has you feeling uneasy.
If this is not your first pregnancy, read up on how the symptoms of this second (or subsequent) pregnancy may be different to your first.
5 Weeks Pregnant: Things to Consider
If you haven’t yet told your partner you’re pregnant yet, and you’re looking for fun ways to surprise him, check out these cute and creative ways to tell your partner he’s about to become a parent.

Give some thought to what you're eating, making sure that you're consuming a variety of healthy foods. Avoid fish that could contain high levels of mercury — like shark, swordfish, and mackerel — and skip any food that’s uncooked or unpasteurized. You'll also want to avoid things like sushi made with raw fish and oysters, as well as soft cheeses like Brie and feta. These items can cause food-borne illnesses that can affect you and your little one. Read up on all the foods to avoid eating when pregnant.
Curious about other early signs and symptoms of pregnancy? Try our Early Signs of Pregnancy quiz to learn more.
Think about whether to share the news that you’re five weeks along with family and friends. Some people prefer to wait until the end of the first trimester when the risk of miscarriage drops significantly. Others tell at least a select few the moment they’ve got a positive pregnancy test in hand.
Have a cat? Now is the time to get someone else to take care of the litter box so that you can stay clear of toxoplasmosis, an infection that can harm unborn babies.

Download our Pregnancy Guide to learn more about what to look forward to over the coming weeks and months. Our guide covers everything from nutrition and weight gain to all the questions you'll want to ask your healthcare provider.
If this is your first pregnancy you might like to read up on the trimesters of pregnancy so that you know more about what’s to come in the coming months.
Start a journal. It’s normal to feel a range of different emotions as you adjust to the idea that you are pregnant. Whether it’s something you’ve been hoping for for a long time, or come as a bit of a surprise, your feelings about it may be different to what you had expected. And, they may even change from one day to the next! Writing in a journal is one way to get your inner-most thoughts and feelings out of your system and journaling can help you navigate the emotional highs and lows of early pregnancy.
Although you won’t be showing just yet, you may want to start a month-by-month baby bump photoshoot using our free downloadable bump to baby monthly milestone cards.
 You can either save the photos as a private keepsake or share the images on social media (once you’re ready to share news of your pregnancy). In the years to come, you’ll love to look back on how your bump grew during your pregnancy, and your little one will also love to see his first “home.”
You can either save the photos as a private keepsake or share the images on social media (once you’re ready to share news of your pregnancy). In the years to come, you’ll love to look back on how your bump grew during your pregnancy, and your little one will also love to see his first “home.”
5 Weeks Pregnant: Ask Your Doctor
Your prenatal visits are usually scheduled about once a month until the last two months of your pregnancy, when they will become more frequent. These regular checkups give you the perfect opportunity to ask questions and bring up concerns.
Are there any possible risks for your pregnancy based on your health, age, or family history?
What should you do if you notice slight bleeding at this stage of pregnancy?
What is normal pregnancy discharge?
How often should you see your healthcare provider during your pregnancy?
How far along are you and when is your due date?
5 Weeks Pregnant: Your Checklist
Read up on how to choose a prenatal care provider– that is unless you already have one.

Schedule your first prenatal appointment. Your healthcare provider will be able to fill you on the specifics of your care, but you can read up on prenatal care to get a general idea of what’s coming.
Find out who to call if your healthcare provider is unavailable or if it’s after hours and you have a medical concern.
Save your provider’s number to your phone and have emergency contact numbers stuck on your fridge and saved to your contact list, too.
Be ready to feel anxious or excited, worried or ecstatic — all normal reactions to becoming pregnant.
Soothe any cramps and backaches with a warm bath or a nap.
Cut out smoking and alcohol, if you haven't already.
Although rare, it’s a good idea to read up on the signs and symptoms of an ectopic pregnancy just in case.
Sign up for even more weekly pregnancy tips:
Critical stages of pregnancy - why are they dangerous?
Services
Virtual tour.
 Clinic "ARNIKA"
Clinic "ARNIKA"
The wonderful period of waiting for a baby for almost every woman is far from serene: how many anxieties, worries and doubts arise in expectant mothers at this time - they simply cannot be counted. In most cases, all fears are in vain - the baby develops and grows safely. However, it must be remembered that there are also so-called critical periods of pregnancy, when inattention to oneself and one's body can lead to a disastrous result - its spontaneous termination.
First trimester
The beginning of a new life in a woman's body, or 2-3 weeks of pregnancy, is considered the first critical period. This is due to the fact that the egg can be fertilized, but due to changes as a result of inflammation, hormonal imbalances, the presence of nodes, scars, fibroids or synechia on the inner mucous membrane of the uterus, implantation does not occur, the embryo dies and is removed from the mother's body during menses. However, even if implantation has occurred, the embryo may stop developing and early miscarriage , and the main reason for this course of events is chromosomal abnormalities.
The second critical period of the first trimester begins at 8 and ends at 12 weeks of gestation. At this time, the main cause of interruption is considered to be hormonal deficiency, which disrupts the process of placental formation. This condition may be associated with reduced work of the corpus luteum of the ovaries, excessive production of androgens by the adrenal glands - male sex hormones, as well as malfunctions of the pituitary gland or thyroid gland. The threat of abortion can be eliminated with the help of properly selected and timely prescribed hormonal treatment, which will allow the baby to safely reach the due date.
In addition, throughout the first trimester of pregnancy, the fetus may stop developing due to the following adverse environmental factors:
- harmful working conditions
- bad habits
- physical effects - radiation, vibration, intense sports training, etc.
- acute infectious diseases (influenza, cytomegalovirus, herpes, rubella and others)
- severe stressful situations
And even if the fetus develops further, the negative impact of most of these factors may appear after a few months of pregnancy or even after the baby is born: these may be anatomical disorders or severe malformations. Therefore, the entire first trimester of the development of a new life can be considered "critical".
Therefore, the entire first trimester of the development of a new life can be considered "critical".
Second trimester
The third critical period of pregnancy occurs at 18-24 weeks of gestation and is largely associated with the active growth of the uterus. At this time, spontaneous interruption most often occurs due to isthmic-cervical insufficiency (ICI), as a result of which the fetal egg descends under the influence of gravity, loses its integrity and triggers the mechanism of labor activity. However, shortening and expansion of the cervical canal, detected in time, allows suturing the cervix or installing an obstetric pessary and safely prolonging the pregnancy. Here we should also remember about infectious diseases, including intrauterine infection, which can disrupt the functions of the placenta, lead to the outflow of water from the fetal bladder and late miscarriage.
Another common reason for interrupting the process of bearing a fetus at this time is placenta previa or its low location: for various reasons, it can exfoliate, cause severe bleeding and death of the fetus. In addition, at this time, pregnancy may stop developing due to violations in the development of the brain and the most important functional systems of the baby, caused by the harmful effects of various negative factors on them in the first trimester.
In addition, at this time, pregnancy may stop developing due to violations in the development of the brain and the most important functional systems of the baby, caused by the harmful effects of various negative factors on them in the first trimester.
Third trimester
In this trimester - at 28-32 weeks - the fourth critical period takes place. The threat of premature birth may occur due to insufficiency of the placenta, its premature detachment, severe forms of late toxicosis of pregnant women, ICI and various hormonal disorders. In addition, due to the overdistension of the uterus, most multiple pregnancies end at this time. Children born during this period are already viable, but they need long-term qualified medical care.
In addition to all the periods listed above, the critical periods for women who have had reproductive losses in the past are the days of planned menstruation, miscarriages or "fading" pregnancies. Doctors believe that during these periods the body can “remember” the need for hormonal changes, so they carefully monitor the condition of the expectant mother and baby and prescribe treatment in a timely manner if any threat arises.
In order to safely overcome the dangerous periods of pregnancy , it is necessary to avoid any physical exertion, stress, and, if necessary, visit a doctor when these dates are approaching. In addition, if you experience pain, bleeding or other warning signs, you should also seek medical attention as soon as possible. Only an attentive attitude to oneself will help to safely endure a healthy baby and give birth to him at the time set by nature.
Take care of yourself and your baby!
Save at all costs: reasons for abortion
January 17, 2017 Articles on gynecology
According to Wikipedia, 15-20% of clinically diagnosed pregnancies end in spontaneous abortion. These numbers are a lower estimate, as many miscarriages occur in the early stages, before the woman knows she is pregnant. After all, often the clinical signs of a miscarriage are mistaken for heavy periods or for their delay.
What are the reasons for termination of pregnancy at different terms? How to prepare for pregnancy after a bad experience that ended in a miscarriage? These questions were answered by an obstetrician-gynecologist of the highest category at Bullfinch Medical Center ALEXANDER GIL.
- Alexander Vadimovich, most miscarriages happen at the beginning of pregnancy, and many women are perplexed: why could this happen?
- The main cause of miscarriages before 6 weeks is natural selection. There is a laying of pregnancy with congenital malformations of the embryo, which is no longer viable - thus, natural selection is carried out, in which we cannot interfere.
You will never know the exact cause of a miscarriage at this time, even if after abrasion (curettage of the uterine mucosa), the contents are sent for research. As a rule, the answer comes: “short-term pregnancy” and nothing more.
There is another reason for termination of pregnancy, especially if it is not the first one - Rh-conflict (when a woman has Rh-negative blood, and men - Rh-positive). But in our country, effective prevention of the Rh conflict is used, so that troubles can be avoided at the stage of pregnancy planning.
But in our country, effective prevention of the Rh conflict is used, so that troubles can be avoided at the stage of pregnancy planning.
In the structure of early termination of pregnancy, no one excludes infections and problems associated with hormones. At a period of 6-8 weeks, promising pregnancies are often interrupted due to a lack of hormones. During normal pregnancy, a woman has a so-called corpus luteum in one of the ovaries, which produces endogenous progesterone.
Unfortunately, the functioning of the corpus luteum ends by about 7 weeks of pregnancy, and if initially there was not enough endogenous progesterone, the pregnancy stops developing: the fetal egg detaches and the so-called missed pregnancy occurs.
In some cases, with detachment of the fetal egg, pregnancy can be saved, the main thing is to contact a specialist in time. If, based on the results of ultrasound studies, the doctor sees that the embryo is still alive, pregnant women are prescribed exogenous progesterone in tablets or suppositories. This hormone also exists in the form of injections - it is used to saturate the body faster and prevent miscarriage.
This hormone also exists in the form of injections - it is used to saturate the body faster and prevent miscarriage.
- Agree, when a woman becomes pregnant, she cannot suspect that she does not have enough progesterone in her body. What should be her concern? What signs indicate this?
- Any discharge from scanty dark brown to more profuse bloody is a bad sign. You should not hesitate to contact a gynecologist.
In the event of spotting spotting, an ultrasound examination is indicated, a blood test for progesterone.
I want to say that lack of progesterone can cause miscarriage up to 15 weeks. At 15-16 weeks, the placenta is finally formed, which will secrete (produce) this hormone.
— Alexander Vadimovich, what problems can arise with the placenta during pregnancy?
- In the early stages, the chorion (unformed placenta) can block the internal os, maybe its marginal location - this is a big risk of abortion. In this case, the woman is admitted to the hospital and observed for up to 16 weeks - by this time, the chorion, as a rule, rises. But there remains a percentage of pregnant women in whom the placenta overlaps the cervix of the uterus - this is called the "central location of the placenta." To maintain pregnancy, such women, as a rule, must be in the clinic and under observation all the time.
In this case, the woman is admitted to the hospital and observed for up to 16 weeks - by this time, the chorion, as a rule, rises. But there remains a percentage of pregnant women in whom the placenta overlaps the cervix of the uterus - this is called the "central location of the placenta." To maintain pregnancy, such women, as a rule, must be in the clinic and under observation all the time.
— What is the treatment for infections that appear during pregnancy?
- Infections can occur even in women who were carefully examined before pregnancy. Often this problem occurs due to spotting - this is a favorable environment for the development of infections.
Ectopia (erosion) of the cervix is also an infection that is a clear threat to pregnancy. Therefore, it is so important to undergo a colposcopy before conception and be treated for ectopia, if it is detected.
Infection by ascending route can penetrate in utero and adversely affect the health of the fetus. There is such a complication as intrauterine fetal pneumonia, which is treated very poorly and occupies a large percentage in the structure of infant mortality.
There is such a complication as intrauterine fetal pneumonia, which is treated very poorly and occupies a large percentage in the structure of infant mortality.
And we treat infections whenever possible in any way that is prescribed in the protocol. There is such a tactic, which is to take antibiotics. There is no need to be afraid of them, as the doctor will prescribe only medicines approved for pregnant women. Sometimes you have to use those drugs, the benefits of which are greater than the risk of adverse reactions.
— What threats can affect a mid-term pregnancy?
— Among the many causes that lead to spontaneous miscarriages is isthmic-cervical insufficiency. This is a condition in which the isthmus and cervix cannot cope with the increasing load (growing fetus, amniotic fluid), begin to open - and the baby is born prematurely.
There are indications for the prevention of this condition - the imposition of a circular submucosal suture on the cervix. The best time is 16-17 weeks. You can do this procedure after 20 weeks, but the effect will be less.
The best time is 16-17 weeks. You can do this procedure after 20 weeks, but the effect will be less.
In the middle of pregnancy, a placental abruption can occur in a woman. In some cases, pregnancy can be saved with the help of drugs that affect blood clotting. But often doctors are forced to resort to a small caesarean section. As a rule, childbirth before 22 weeks ends in the death of the fetus, and here we are already talking about saving the life of the mother.
I encourage pregnant women to refrain from flying. In my medical practice, there have been several cases where placental abruption in patients occurred during a flight. Who will provide you with qualified assistance in this case? I advise you not to take risks.
In Belarus, as in other European countries, labor begins at 22 weeks, but it is considered premature. Doctors are doing everything possible to save a promising pregnancy by any means. The main thing is to always be under the supervision of a specialist and follow all his recommendations.
- Alexander Vadimovich, unauthorized termination of a desired pregnancy is always a great psychological trauma for a woman. No one wants to experience this again. What are the features of preparing for the next pregnancy after a miscarriage?
— Before thinking about a second pregnancy, it is advisable for women who experience mental anguish to undergo a course of psychotherapy. This is very important, because mental problems can be very serious, especially in women after unsuccessful in vitro fertilization (IVF).
The main rule: do not get pregnant after a miscarriage for 6 months. It is best to protect yourself at this time with oral contraceptives, which the doctor will prescribe. This is necessary in order to restore normal reproductive function.
A set of examinations for women who have had a miscarriage is ordered individually. But the general recommendations are:
1. Diagnosis of sexually transmitted infections: mycoplasmosis, ureaplasmosis, chlamydia, herpes simplex virus, human papillomavirus (HPV).
You should also be screened for infections that may have caused a miscarriage in a previous pregnancy.
2. Test for sex hormones - if prescribed by a doctor.
3. Thyroid hormones (TSH, T4 free, ATPO), ultrasound of the thyroid gland, consultation with an endocrinologist.
4. If necessary, consultation of a therapist and other specialists, a blood test for sugar, syphilis, HIV.
5. Ultrasound of the abdomen and kidneys. During pregnancy, many chronic diseases are exacerbated, incl. and kidney disease. You need to be treated before conception.
6. Colposcopy (examination of the cervix under a microscope).
7. Analysis of the spermogram of the partner.
An examination by a geneticist is indicated if, when planning a pregnancy, a woman is 36 years old, and a man is 45 years old and over. Also, this doctor should be visited by a couple who had two non-developing early pregnancies in a row.
Another tip from practice. Many women, having barely become pregnant, rush to confirm this on an ultrasound. Of course, there is no direct evidence that such research is harmful to the fetus, but there is also no evidence to the contrary that it is absolutely harmless. Since you so desire this pregnancy, it’s not worth the risk, and a competent doctor will definitely warn a woman against doing an early ultrasound without any special indications.
Of course, there is no direct evidence that such research is harmful to the fetus, but there is also no evidence to the contrary that it is absolutely harmless. Since you so desire this pregnancy, it’s not worth the risk, and a competent doctor will definitely warn a woman against doing an early ultrasound without any special indications.
Pregnancy and its prospects can be determined using a blood test for hCG (human chorionic gonadotropin), or, more simply, the pregnancy hormone. It is absolutely harmless for pregnancy. It is advisable to donate blood at the beginning of the delay, a week later - again. If the increase in hCG is normal, then the pregnancy is promising, not ectopic - and there are no indications for ultrasound.
For the first time, a woman should come for ultrasound diagnostics at 11-12 weeks of pregnancy. Oleksandr Gil
March 29, 2022 Articles on gynecology
Frequency of examinations by a gynecologist
July 20, 2020 Articles on gynecology
MVS in elderly patients
Population aging is one of the global problems.