Blanched nipples after breastfeeding
Extremely Sore Nipples? Nipples Changing Colour After Breastfeeding? Could it Be Vasospasm?
Most people will not have heard of the term vasospasm. It is a rather cool sounding name, but, unfortunately, it often brings a lot of pain with it...
Share this content
Vasospasm is not exceedingly common but this definitely happens to a few women. In this blog, we will discuss nipple blanching and vasospasm as they are separate issues, which can often be mistaken for the same thing.
What is Nipple Blanching?
Nipple Blanching happens when the nipple comes out from your baby’s mouth whitened and misshapen. The most frequent reason for this is due to your baby compressing your nipple during a breastfeed.
When you notice your nipple is white after breastfeeding, you may see that the end of the nipple is also flattened, creased or pointed; imagine the shape of a new lipstick – that’s a misshapen nipple!
Your nipple should always come out of baby’s mouth the same shape it went in, but, maybe a little elongated.
You may find that pain in your nipple increases several seconds to a few minutes after the feed.
Nipple blanching can be due to:
- Incorrect attachment at your breast
- Your baby clamping down on your nipple in order to slow down your fast flow of milk
- Your baby may have a tongue-tie (your lactation consultant will be able to assess for this)
- There may be certain oral palate variations (your lactation consultant will be able to assess for this)
It is really important to seek help with breastfeeding from a lactation consultant or your maternal child health nurse to enable you and bub to find a way to solve this for you. This way you will be able to go on enjoying your feeding time together.
What is Vasospasm?
A condition known as Raynaud’s phenomenon, where your fingers turn white when they are cold can also affect the nipples.
Pain can occur during, immediately after, or even between breastfeeds. You may notice that your nipple turns white. Then, you will often see the nipple change colour again; from white to blue to red as the blood flow returns to the nipple.
You may notice that your nipple turns white. Then, you will often see the nipple change colour again; from white to blue to red as the blood flow returns to the nipple.
Vasospasm due to Raynaud’s is more likely to occur on both nipples.
Vasospasm tends to last for longer periods of time than nipple blanching and does not go away even with good attachment at the breast during feeds.
Cold is usually the trigger for vasospasm. This happens when your baby stops breastfeeding and pulls off the breast exposing your nipple to the cooler air.
The pain from vasospasm can be mild or severe, and may be in the form of sharp or burning pains and throbbing.
Vasospasm is often mistaken for thrush of the nipple because of the similarities in how women describe the pain. But the colour change in the nipple tends to make it clearer when it is vasospasm rather than thrush.
What Can You Do if You Think You May Be Suffering from Vasospasm?
First, seek help from a lactation consultant to check your breastfeeding attachment and suggest nipple vasospasm treatment. Your lactation consultant can also check for any nipple damage, infections or thrush of the nipple.
Your lactation consultant can also check for any nipple damage, infections or thrush of the nipple.
Try and keep your nipples warm. Here are a few options that may help:
- Using a warm heat pack on your nipples straight after feeding
- Placing a pair of clean warm socks in your bra
- Purchasing some Breast Warmers which reflect your own body heat through the reflective material in the Breast Warmers
- Wearing an extra layer of clothes
- Avoiding exposing your nipples to “air” them
Massaging your nipple with olive oil when you are feeling pain is helpful for some women.
Avoid caffeine, nicotine, diet pills and cold medications containing pseudoephedrine or phenylephrine, beta blockers, and other vasoconstrictive drugs. These can all make your symptoms worse.
Oral contraceptives containing estrogen have also been associated with vasospasm, so, it is important to discuss this further with your GP or Gynaecologist.
There are some supplements which have been shown to help vasospasm and may be appropriate to look further into if the above recommendations are not working:
- Magnesium tablets help to relax the blood vessels.
 It is advisable to speak to a naturopath to discuss the best dose. This can be done in the health store.
It is advisable to speak to a naturopath to discuss the best dose. This can be done in the health store. - Fish oil capsules or evening primrose oil may also improve blood vessel relaxation.
- Dietary supplementation with a vitamin B complex that includes B6 and niacin may help.
- Ibuprofen for may be helpful for pain management.
Some women may need to discuss this further with their GP or lactation consultant. If none of the above is helping they may need to take a prescription medicine of low dose oral nifedipine to relieve the vasospasm.
The good news is that vasospasm can be treated and you will be able to go on breastfeeding, pain free.
Please reach out to health professionals qualified in breastfeeding support to gain the best information and support for vasospasm and nipple blanching.
If you have suffered with vasospasm or nipple blanching share your thoughts and comments with us on our Medela Australia Facebook page.
Why do my nipples turn white when I breastfeed?
Have you been finding breastfeeding painful and noticing that your nipples are turning white? You could be experiencing nipple blanching.
Do your nipples turn white—and maybe even hurt—during breastfeeding? This is called nipple blanching and can be caused by a few different things. It’s usually a result of blood flow to your nipple being restricted, often because your baby is compressing your nipples because the latch is too shallow, your baby is tongue-tied, or your milk lets down so quickly that she clamps down in an attempt to slow the flow. With this type of blanching, your nipple might also look flattened, creased or pointed when your baby comes off the breast. And for some moms, it can be quite painful.
Nipple blanching can also be caused by vasospasms, a tightening of the blood vessels due to lack of blood flow and oxygen that usually occurs during and right after breastfeeding, when the baby comes off the breast. This is typically caused by latch issues, and it can be extremely painful, often searing at first, then throbbing. “Vasospasms could be your body’s reaction to the fact that your nipples were damaged early on by latch issues or, in some cases, even thrush,” says Pam Davey, a certified doula and registered lactation consultant. They will eventually go away, but you’ll need to seek professional help to correct the problem causing it, and it can take a long time for the nipple damage to heal.
This is typically caused by latch issues, and it can be extremely painful, often searing at first, then throbbing. “Vasospasms could be your body’s reaction to the fact that your nipples were damaged early on by latch issues or, in some cases, even thrush,” says Pam Davey, a certified doula and registered lactation consultant. They will eventually go away, but you’ll need to seek professional help to correct the problem causing it, and it can take a long time for the nipple damage to heal.
Often, the key to both preventing and stopping nipple blanching from compression or vasospasm is as simple as improving the latch, says Nathalie Pambrun, vice-president of the Canadian Association of Midwives, who recommends getting help from a lactation consultant. “In the case of vasospasm, you can relieve the symptoms by keeping your body warm to avoid blood vessel constriction during nursing, and applying a hot washcloth or dry heat with a blow dryer set on low to your breasts afterwards.”
“In the case of vasospasm, you can relieve the symptoms by keeping your body warm to avoid blood vessel constriction during nursing, and applying a hot washcloth or dry heat with a blow dryer set on low to your breasts afterwards.”
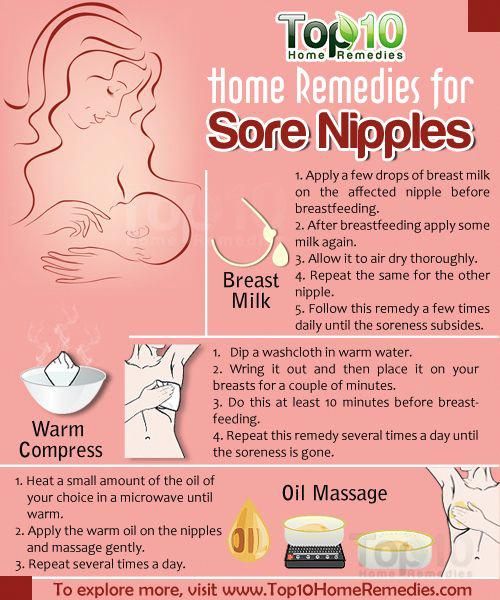
10 ways to prevent and treat sore nipples
Another, although less common, cause of nipple blanching is Raynaud’s disease. This condition affects both men and women and isn’t related to being pregnant or breastfeeding. In addition to white nipples after nursing, you might have cold fingers, toes, lips or ears, changes in skin colour in response to cold or stress, and a tingling or throbbing feeling when circulation returns after a few minutes or a few hours. Blanching in this case comes with severe and searing pain, which are also symptoms of thrush and so it is often misdiagnosed. A doctor can do a blood test for the disease and, in more severe cases, may prescribe a medication to widen your blood vessels and increase circulation. To relieve symptoms of Raynaud’s, breastfeed in warm environments and wearing warm clothing, prevent a temperature change by covering your breasts with your shirt or your hand as soon as your baby has finished nursing, apply dry heat with a blow dryer set on low, or massage your nipples with olive oil to help return blood flow and soothe any lingering pain or discomfort.
To relieve symptoms of Raynaud’s, breastfeed in warm environments and wearing warm clothing, prevent a temperature change by covering your breasts with your shirt or your hand as soon as your baby has finished nursing, apply dry heat with a blow dryer set on low, or massage your nipples with olive oil to help return blood flow and soothe any lingering pain or discomfort.
Don’t hesitate to contact a lactation consultant or your doctor if you’re experiencing blanching or pain while nursing.
Read more:
How to handle oversupply and overactive letdown
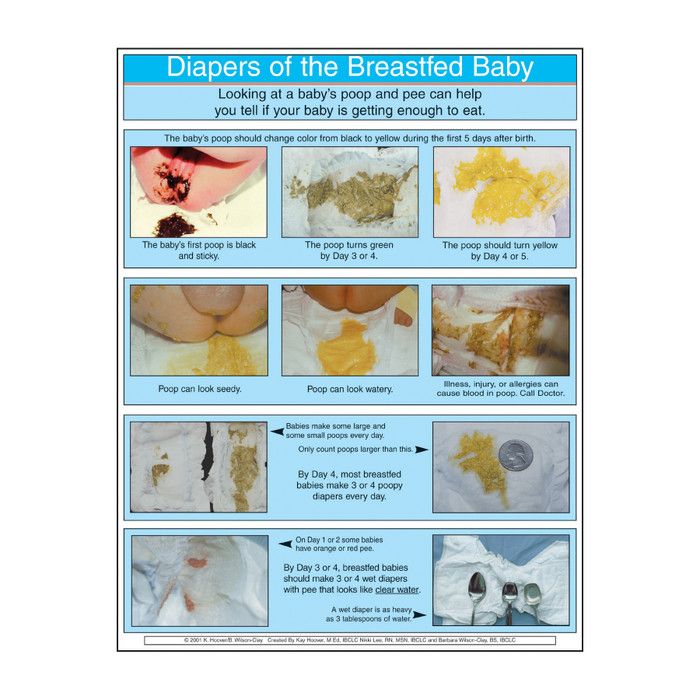
How do I know my baby’s getting enough breast milk?
Stay in touch
Subscribe to Today's Parent's daily newsletter for our best parenting news, tips, essays and recipes.- Email*
- CAPTCHA
- Consent*
Yes, I would like to receive Today's Parent's newsletter. I understand I can unsubscribe at any time.
 **
**
FILED UNDER: Breastfeeding breastfeeding problems Maternal health sore nipples
Breastfeeding Vasospasm - Milk Fairies
Some breastfeeding moms experience nipple discomfort during and after feeding their baby. Discomfort and pain can occur for various reasons, and one of them is vasospasm .
Vasospasm of the nipples is often correlated with Raynaud's syndrome - a disease characterized by a disorder of arterial circulation mainly in the vessels of the extremities (feet and hands) under the influence of cold or emotional excitement.
Vasospasm of the nipple occurs when the vessels in the upper part of the nipple spasm so much that all the blood drains from its tip, as a result of which the nipple turns white (as an option - successively turns white - blue - purple), and then, when the spasm passes , and the blood rushes back, turns pink again. Vasospasm can occur on one or both breasts at once and last from a few minutes to an hour or more. Soreness can be of a different nature.
Vasospasm can occur on one or both breasts at once and last from a few minutes to an hour or more. Soreness can be of a different nature.
The mother may feel burning, throbbing, stabbing or burning pain; moreover, pain and external manifestations of vasospasm can occur both immediately after feeding and between them [5]. Some moms feel Shooting pain that starts from the nipple and radiates deep into the chest, so vasospasm is often misdiagnosed as a yeast infection.
Vasospasm can occur on its own or as a result of infections or injuries to the nipple - this is how the nipple signals a problem. Often, a mother notices that it has become painful to feed, and after the feeding is completed, she finds that the nipple has become white. Usually injuries and damage to the nipples during lactation are associated with features breastfeeding the baby - in order to prevent or alleviate the symptoms of vasospasm, you must first make sure that the baby is properly attached to the breast and does not injure it when sucking.
In addition, vasospasm may occur in women who have had breast or nipple surgery in the past, possibly due to tissue and nerve damage. Also, some drugs (eg, fluconazole and oral contraceptives [3]) and some substances, including nicotine and caffeine, can contribute to vasospasm [9].].
How to help yourself during vasospasm?
During the vasospasm itself, to stop the pain, you can try to restore blood flow to the tip of the nipple by gently squeezing the nipple at its base. [8] Gentle massage with light squeezing movements (you can lubricate your fingers with cosmetic or vegetable oil) will help to quickly restore blood supply to the nipple and reduce pain until it disappears completely.
In the case of prolonged and severe pain, you can take (on consultation with your doctor!) an anesthetic that is compatible with breastfeeding, such as Ibuprofen or Paracetamol. [1
How to prevent vasospasm?
To avoid or reduce the intensity of vasospasms, in the first place - do not overcool ! [2] Put on a warm vest or carry your baby in your arms for a while after feeding. Some mothers find it helpful to put a warm diaper on the nipple as soon as the baby releases the breast. Some people use a hair dryer on warm air, blowing it on their breasts. Similarly, any warm dry and wet compresses help or even your own warm hand covering the nipple immediately after breastfeeding.
Some mothers find it helpful to put a warm diaper on the nipple as soon as the baby releases the breast. Some people use a hair dryer on warm air, blowing it on their breasts. Similarly, any warm dry and wet compresses help or even your own warm hand covering the nipple immediately after breastfeeding.
If painful vasospasm continues despite non-traumatic breastfeeding and heat application after feedings, then medication prevention and treatment of vasospasm (only prescribed by your physician!) may be an option. For example, you can ask the doctor to prescribe vitamin B6, calcium and magnesium as a preventive measure and relieve vasospasm .
Some doctors recommend applying a moderate amount of nitroglycerin ointment or 2% spray to the nipples after each feed for the first 24 hours and then whenever symptoms of vasospasm begin [6]. However, its use can cause a side effect in the form of headaches, and only about half of the patients confirm the effectiveness of such an ointment for vasospasm.
One tablet Nifedipine long-acting tablets per day for two weeks may also help. Nifedipine is a calcium channel blocker commonly used to treat hypertension and is not excreted in breast milk. [7] Nifedipine therapy has been shown to be effective in vasospasm and has no side effects in the baby [4]. 9
 & Pitman, T. The Ultimate Breastfeeding Book of Answers. Roseville, California: Prima 2000
& Pitman, T. The Ultimate Breastfeeding Book of Answers. Roseville, California: Prima 2000 Alena Korotkova,
Clinical psychologist, breastfeeding consultant
Alena Lukyanchuk, 9000 Correction 9,0004,000 4000 4000 4000 4000 4000 4000 4000 4000 4000 4000 4000 9000 moms | Breast care Breastfeeding is good for you and your baby, but it can be a real challenge for the nipples. Check out our tips and tricks to help reduce the pain.
Share this information
Sioned Hilton, health visitor, neonatal nurse and lactation consultant:
A mother of three, Sioned Hilton has been supporting families with newborns and young children for over 30 years. She provides advice on breastfeeding and pumping, both in clinics and at home. In addition, Schoned writes articles for parenting magazines, attends conferences, and conducts seminars for attending physicians.
New mothers often hear: "Breastfeeding doesn't have to be painful." However, in the early days, many are faced with the opposite.
During pregnancy, most women's nipples enlarge and become more sensitive. When a newborn baby begins to suckle, it creates a certain pressure, and this is a completely new and unfamiliar sensation for a woman (at least for a first-time mother).
Feedings can be prolonged for a long time, sometimes up to an hour, and the child may ask to be breastfed up to 13 times a day. 1 This sucking, pressure and saliva of the baby can cause sore nipples.
1 This sucking, pressure and saliva of the baby can cause sore nipples.
Remember how your lips crack in the wind and sun. The more often you lick them, the more they will dry and become inflamed. Therefore, lips require good hydration to soften, protect and speed up the healing of cracks. The same thing happens with nipples.
However, sore nipples usually don't last more than a couple of weeks and go away as your baby and your breasts get used to breastfeeding. It is important to start nipple care as early as possible to prevent the situation from worsening. Therefore, if your nipples become very inflamed, crack or bleed, contact your doctor as soon as possible. 2
Prevention is better than cure, so check out our tips.
Check your baby's latch-on
Correct latch is the key to pain-free breastfeeding. When putting the baby to the breast, point the nipple towards his palate. This will allow him to grab the nipple and the part of the areola (the darker skin around the nipple) underneath. When the nipple and part of the breast is in the baby's mouth, feeding is taking place correctly. 3
When the nipple and part of the breast is in the baby's mouth, feeding is taking place correctly. 3
For the first few days, see a lactation consultant or specialist to check for proper latch. He will be able to give you advice on how to solve problems and recommend other feeding positions that will make it less painful for you to feed your baby.
Check tongue tie
Tongue tie (ankyloglossia) occurs in 4-11% of
newborns. 4 At the same time, the strip of skin that attaches the tongue to the bottom of the mouth - the so-called frenulum - is too short. A child with a shortened frenulum will not be able to open his mouth wide enough to latch onto the breast well, and his tongue will not cover the lower gum when sucking. As a result, the baby will be nervous, and your nipples may become inflamed.
The child's doctor or lactation consultant must examine the child to make this diagnosis. The problem of a shortened bridle is solved by a simple undercutting procedure. It is performed by a doctor, and is usually done without blood and does not require anesthesia. Cutting the bridle allows you to restore the normal feeding mechanism almost instantly. 5
It is performed by a doctor, and is usually done without blood and does not require anesthesia. Cutting the bridle allows you to restore the normal feeding mechanism almost instantly. 5
Less common in children is a short frenulum of the upper lip. In this case, it is necessary to dissect the skin that connects the upper lip to the gum. A shortened frenum of the tongue or upper lip in a newborn is not always detected during the examination conducted immediately after birth, so if you think that this is what is causing your nipples pain, seek medical advice as soon as possible. 4
Breastfeeding Nipple Tips
- Wash your breasts with water only when you shower or bathe. Small bumps on the areola (Montgomery's glands) secrete oil that moisturizes and protects your nipples. Soaps and shower gels can strip away this natural defense, causing dryness and irritation. 6
- Pat the nipples gently with a soft towel or simply let them air dry.
 In the past, women were often advised to rub their nipples to make them stiffer, but thankfully, such advice is a thing of the past!
In the past, women were often advised to rub their nipples to make them stiffer, but thankfully, such advice is a thing of the past! - Do not wash breasts or nipples before feeding. The bacteria found on the surface of the breast actually help the baby's intestinal microflora to develop. 7
- Fresh breast milk helps to heal cracked nipples, 8 so rub a few drops of milk into them before and after feeding.
- Change your bra pads often if they get wet. This will reduce the risk of bacterial and fungal infections, including thrush. 6
- It is not necessary to increase the intervals between feedings to give the nipples a "rest". For a baby to be healthy and grow well, it needs to be fed on demand. Remember, frequent feeding stimulates and maintains milk production, so keep feeding despite the pain. 9
Healthy teat care products
- Pure lanolin teat cleaner, a natural product derived from sheep's wool.
 It moisturizes and promotes healing of the nipples. This cream is safe for the baby, so it does not need to be washed off before feeding.
It moisturizes and promotes healing of the nipples. This cream is safe for the baby, so it does not need to be washed off before feeding. - Hydrogel Pads* can be applied to sore nipples to relieve pain while feeding and help promote healing. They can even be stored in the refrigerator to enhance the soothing cooling effect.
- Breast pads* fit inside the bra. They help prevent nipple irritation from clothing and have air holes to help nipples heal.
- Nursing bras** are made from breathable material such as cotton or a special fabric that dries quickly and wicks moisture away from sore nipples.
- Nursing pads* are special silicone pads that fit over the nipples. They have small holes through which milk flows when you are breastfeeding. The pads help to protect the skin underneath and help the baby to better latch on to the nipple by making the nipple stiffer. Do not use nursing pads for a long time. If you have problems or pain, contact your healthcare professional or lactation consultant.

When to Seek Medical Care
The soreness should go away as your nipples and baby get used to breastfeeding. It is worth repeating that the main cause of sore nipples is improper grip. If your lactation consultant has not been able to resolve your pain while feeding, see another specialist and a third if necessary.
If nipple pain persists or if you notice unusual symptoms, talk to your doctor. The appearance of white spots or flakes on the nipples may be a sign of thrush, whitish or bluish nipples may indicate a circulation disorder such as Raynaud's disease (vasospasm), and pus and redness indicate an infection. 2
Literature
1 Kent JC et al. Volume and frequency of breastfeedings and fat content of breast milk throughout the day. Pediatrics. 2006;117(3): e 387-395. - Kent J.S. et al., "Amount and frequency of breastfeeding and fat content of breast milk during the day." Pediatrix (Pediatrics). 2006;117(3):e387-95.
2006;117(3):e387-95.
2 Berens P et al. Academy of Breastfeeding Medicine. ABM Clinical Protocol#26: Persistent pain with breastfeeding. Breastfeeding Medicine. 2016;11(2):46-53. - Behrens, P. et al., Academy of Breastfeeding Medicine, AVM Clinical Protocol #26: Persistence of Breastfeeding Pain. Brestfeed Med (Breastfeeding Medicine). 2016;11(2):46-53.
3 Cadwell K. Latching - On and Suckling of the Healthy Term Neonate: Breastfeeding Assessment. J Midwifery & Women's Health. 2007;52(6):638-42. — Cadwell, K., "Latching and sucking in healthy newborns: evaluation of breastfeeding." F Midwifery Women Health. 2007;52(6):638-642.
4 Segal LM et al. Prevalence, diagnosis, and treatment of ankyloglossia: methodological review. Canadian Family Physician. 2007;53(6):1027-1033. - Segal L.M. et al., Incidence, Diagnosis, and Treatment of Ankyloglossia: A Methodological Review. Canadian Family Physic. 2007;53(6):1027-1033.
Canadian Family Physic. 2007;53(6):1027-1033.
5 O'Shea JE et al. Frenotomy for tongue - tie in newborn infants. The Cochrane Library. 2017. - O'Shea J.I. et al., "Dissection of the frenulum in the newborn", The Cochrane Labrery (Cochrane Library), 2017.
6 Jacobs A et al. S3-guidelines for the treatment of inflammatory breast disease during the lactation period. Geburtshilfe und Frauenheilkunde. 2013;73(12):1202-1208. - Jacobs A. et al., "Recommendations S -3 for the treatment of inflammatory diseases of the breast during breastfeeding. Geburtskhilfe und Frauenheilkünde. milk bacterial communities and establishment and development of the infant gut microbiome JAMA pediatrics 2017;171(7):647-654 - P. S. Pannaraj et al., "Bacterial communities in breast milk and their association with the occurrence and development of the neonatal gut microbiome.




/cdn.vox-cdn.com/uploads/chorus_asset/file/9892303/tpc5.png)






