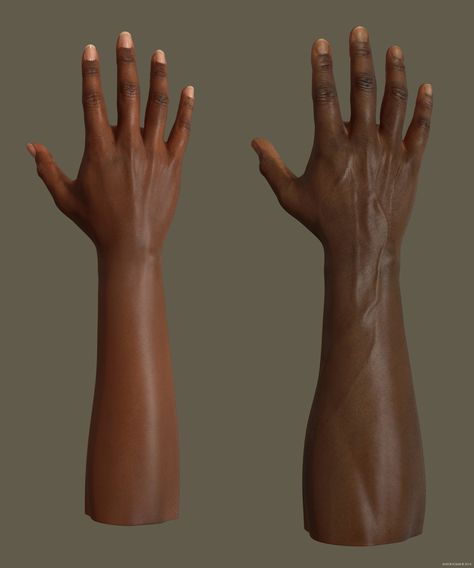
Rash torso and arms
22 Common Skin Rashes, Pictures, Causes & Treatment
A rash is any area of irritated or swollen skin on your body. Rashes are often itchy and painful and can appear differently on different skin tones. While they are often described as red, on darker skin tones they may be purple, gray, or white.
There are many different causes of rashes. Here’s a list of 22 potential causes with pictures.
Warning: graphic images ahead.
Fleabites
Share on PinterestFlea bites of the lower leg causing red bumps and scabbing. Angela Hampton Picture Library / Alamy Stock Photo- usually located in clusters on the lower legs and feet
- itchy, small red bumps on lighter skin tones, and more plum-like in color on darker skin tones
- symptoms begin immediately after being bitten
Read the full article on fleabites.
Fifth disease
Share on PinterestFifth disease is a viral illness caused by parvovirus, which can cause a ‘slapped cheek’ rash.- symptoms include headache, fatigue, low fever, sore throat, runny nose, diarrhea, and nausea
- children are more likely than adults to experience a rash
- round, bright red rash on the cheeks, but it may be less noticeable on darker skin tones
- usually after the face rash, a lacy-patterned rash may appear on the arms, legs, and upper body and might be more visible after a hot shower or bath
Read the full article on fifth disease.
Rosacea
Share on PinterestWeinkle, A. P., Doktor, V., & Emer, J. (2015). Update on the management of rosacea. Clinical, cosmetic and investigational dermatology, 8, 159177. https://doi.org/10.2147/CCID.S58940- chronic (long-term) skin disease that goes through cycles of fading and relapse
- relapses may be triggered by spicy foods, alcoholic beverages, sunlight, stress, and the intestinal bacteria Helicobacter pylori
- the four subtypes of rosacea encompass a wide variety of symptoms
- common symptoms include facial flushing, raised red bumps, facial redness, skin dryness, and skin sensitivity
- on darker skin tones, brown or yellowish-brown bumps may appear, and the rash can have a dusky coloration
Read the full article on rosacea.
Impetigo
Share on PinterestThis image also depicts impetigo on dark skin. Photography courtesy of Grook Da Oger/Wikimedia- most common in children 2 to 5 years old, but can happen at any age
- often located in the area around the mouth, chin, and nose
- irritating rash and fluid-filled blisters that pop easily and form a honey-colored crust
- can also appear brown, purple, or gray on darker skin tones
Read the full article on impetigo.
Ringworm
Share on PinterestRingworm on the face of a child. BSIP SA / Alamy Stock Photo- itchy, circular scaly patches with raised borders
- on lighter skin tones, the patches can appear pink or red
- on darker skin tones, the patches can appear gray or brown
- skin in the middle of the ring appears clearer, and the edges of the ring may spread outward
Read the full article on ringworm.
Contact dermatitis
- appears hours to days after contact with an allergen
- has visible borders and typically appears where your skin touched the irritating substance
- on lighter skin tones, it can appear red
- on darker skin tones, it may be less noticeable
- may have blisters that weep, ooze, or become crusty
- typically itchy, scaly, or raw
Read the full article on contact dermatitis.
Allergic eczema
- may resemble a burn
- often found on hands and forearms
- skin is itchy, scaly, or raw
- may have blisters that weep, ooze, or become crusty
- on lighter skin tones, it can appear red
- on darker skin tones, it can cause darker brown, purple, or gray patches
Read the full article on allergic eczema.
Hand, foot, and mouth disease
Share on PinterestHand-foot-and-mouth disease MidgleyDJ at en.wikipedia, CC BY-SA 3.0, via Wikimedia Commons- usually affects children under age 5
- painful, red blisters in the mouth and on the tongue and gums
- flat or raised red spots located on the palms of the hands and soles of the feet
- on darker skin tones, it can be skin-colored or grayish-brown
- spots may also appear on the buttocks or genital area
Read the full article on hand, foot, and mouth disease.
Diaper rash
- located on areas that have contact with a diaper
- skin looks red, wet, and slightly lighter or darker than typical skin color
- may be warm to the touch
Read the full article on diaper rash.
Eczema
- dry, rough, flaky, inflamed, and irritated skin
- affected areas may be red and itchy
- hair loss may occur in the area with the rash
- on darker skin tones, it can appear as darker brown or gray patches
Read the full article on eczema.
Psoriasis
Share on PinterestPsoriasis is an inflammatory skin condition that causes dry, scaly plaques on the skin. It is immune system mediated, and genetics likely also play a role. Vitek2808/Shutterstock- scaly, silvery, sharply defined skin patches
- on darker skin tones, it may look darker than the surrounding skin or it might appear purple
- commonly located on the scalp, elbows, knees, and lower back
- may be itchy or asymptomatic
Read the full article on psoriasis.
Chickenpox
Share on PinterestChild with chickenpox Grook da oger, CC BY-SA 4.0, via Wikimedia Commons- clusters of itchy, red, fluid-filled blisters in various stages of healing all over the body
- on darker skin tones, it can be red, the same as the natural skin tone, or a little darker; scabs can appear gray
- rash is accompanied by fever, body aches, sore throat, and loss of appetite
- remains contagious until all blisters have crusted over
Read the full article on chickenpox.
Systemic lupus erythematosus (SLE)
- an autoimmune disease that displays a wide variety of symptoms and affects many body systems and organs
- a wide array of skin and mucous membrane symptoms that range from rashes to ulcers
- classic butterfly-shaped face rash that crosses from cheek to cheek over the nose
- can appear bright red on lighter skin tones
- on darker skin tones, it may appear red, brown, or darker than the original skin color
- rashes may appear or get worse with sun exposure
Read the full article on systemic lupus erythematosus (SLE).
Share on Pinterestchatuphot/Shutterstock
- painful rash that may burn, tingle, or itch, even if there are no blisters present
- clusters of fluid-filled blisters that break easily and weep fluid
- rash emerges in a band-like pattern that appears most commonly on the torso, but may occur on other parts of the body, including the face
- may be accompanied by low fever, chills, headache, or fatigue
Read the full article on shingles.
Cellulitis
Share on PinterestCellulitis of the lower legs. TisforThan/Shutterstock
This condition is considered a medical emergency. Urgent care is required.
- caused by bacteria or fungi entering through a crack or cut in the skin
- tends to be red or pink
- it may appear less obvious on darker skin tones and can also look brown, gray, or purple
- painful, swollen skin with or without oozing that spreads quickly
- hot and tender to the touch
- might be a sign of serious infection requiring medical attention
Read the full article on cellulitis.
Drug allergy
Share on Pinterest
This condition is considered a medical emergency. Urgent care is required.
- mild to severe itchy, red rash may occur days to weeks after taking a drug
- severe drug allergies can be life threatening, and symptoms include rash, blisters, hives, racing heart, swelling, itching, and difficulty breathing
- other symptoms include fever, stomach upset, and tiny purple or red dots on the skin
Read the full article on drug allergies.
Scabies
Share on PinterestScabies is an itchy skin infestation with mites. Public domain, via Wikimedia Commons
- symptoms may take 2 to 5 weeks to appear
- extremely itchy rash with small bumps that may be scaly
- raised, white, or flesh-toned lines
Read the full article on scabies.
Measles
Share on PinterestMeasles on the torso of a child phichet chaiyabin/Shutterstock
- symptoms include fever, sore throat, red watery eyes, loss of appetite, cough, and runny nose
- depending on skin tone, the rash may be red, skin-colored, or darker than the natural skin color
- the rash spreads from the face down the body 3 to 5 days after first symptoms appear
- tiny white spots with bluish-white centers on a red background can appear inside the mouth
Read the full article on measles.
Tick bite
Share on PinterestAitor Diago/Getty Images
- painless and causes only minor signs and symptoms, such as a change in skin color, swelling, or a sore on the skin
- rash, burning sensation, or blisters
- difficulty breathing, which requires immediate medical attention
- the tick often remains attached to the skin for a long time
- bites rarely appear in groups
- may look like a target, circular, expanding — 70 to 80 percent of people with Lyme disease will have this rash
Read the full article on tick bites.
Seborrheic eczema
Share on PinterestZay Nyi Nyi/Shutterstock
- yellow or white scaly patches that flake off
- affected areas may be red — though they may appear faint on darker skin tones —, itchy, greasy, yellowish or white patches
- hair loss may occur in the rash area
Read the full article on seborrheic eczema.
Scarlet fever
Share on PinterestChild with scarlet fever rash and rosy cheeks badobadop, CC BY-SA 3.0, via Wikimedia Commons
- occurs at the same time as or right after a strep throat infection
- rash is made up of tiny bumps that make it feel like “sandpaper”
- bright red tongue
- people with lighter skin tones can have a bright red rash all over the body (but not on the palms of your hands and soles of your feet)
- on people with darker skin tones, it may be more difficult to see the rash, but their skin will have a sandpaper-like texture
Read the full article on scarlet fever.
Kawasaki disease
Share on Pinterest
This condition is considered a medical emergency. Urgent care is required.
- usually affects children under age 5
- red cracked lips, swollen tongue (strawberry tongue), high fever, swollen red palms and soles of the feet, swollen lymph nodes, bloodshot eyes
- can be harder to recognize on darker skin tones
- may cause severe heart problems
Read the full article on Kawasaki disease.
Contact dermatitis
Contact dermatitis is one of the most common causes of rashes. This type of rash occurs when the skin comes into direct contact with a foreign substance that causes an adverse reaction, leading to a rash. The resulting rash may be itchy, red, or inflamed.
Possible causes of contact dermatitis include:
- beauty products
- soaps
- laundry detergent
- dyes in clothing
- chemicals in rubber, elastic, or latex
- poisonous plants, such as poison oak, poison ivy, or poison sumac
Medications
Taking medications may also cause rashes. They can form as a result of:
They can form as a result of:
- an allergic reaction to the medication
- a side effect of the medication
- photosensitivity from the medication
Other causes
Other possible causes of rashes include the following:
- A rash can sometimes develop in the area of a bug bite, such as a fleabite. Tick bites are of particular concern because they can transmit disease.
- Atopic dermatitis, the most common form of eczema, is a rash that may be more common in people with asthma or allergies. The rash is often reddish, though it can be skin-colored or darker on people with darker skin tones. It can be itchy with a scaly texture.
- Psoriasis is a common skin condition that can cause a scaly, itchy, red, or purplish rash to form along the scalp, elbows, and joints.
- Seborrheic eczema is a type of eczema that most often affects the scalp and causes redness, scaly patches, and dandruff. It can also occur on the ears, brows, or nose. When babies have it, it’s known as cradle cap.
- Systemic lupus erythematosus is an autoimmune disease that can trigger a rash on the cheeks and nose. This rash is known as a “butterfly,” or malar, rash.
- Rosacea is a chronic skin condition of unknown cause. There are several types of rosacea, but all are characterized by redness and rash on the face.
- Ringworm is a fungal infection that causes a distinctive ring-shaped rash. The same fungus that causes ringworm on the body and the scalp also causes jock itch and athlete’s foot.
- Diaper rash is a common skin irritation in infants and toddlers. It can be associated with prolonged exposure to a wet diaper.
- Scabies is an infestation by tiny mites that live on and burrow into your skin. It causes a bumpy, itchy rash.
- Cellulitis is a bacterial infection of the skin. It usually appears as a red, swollen area that is painful and tender to the touch. If left untreated, the infection causing the cellulitis can spread and become life threatening.
Causes of rashes in children
Children are particularly prone to rashes that develop as a result of illnesses:
- Chickenpox is caused by a virus, and the rash is characterized by small itchy bumps and blisters that form all over the body.

- Measles is a viral respiratory infection that causes a widespread rash consisting of itchy, red bumps.
- Scarlet fever is an infection due to group A Streptococcus bacteria that produces a toxin, causing a bright red or skin-tone-colored, sandpaper-like rash.
- Hand, foot, and mouth disease is a viral infection that can cause red lesions on the mouth and a rash on the hands and feet.
- Fifth disease is a viral infection that causes a red, flat rash on the torso, arms, and legs.
- Kawasaki disease is a rare but serious illness that triggers a rash and fever in the early stages and can lead to heart complications.
- Impetigo is a contagious bacterial infection that causes an itchy, crusty rash and yellow, fluid-filled sores on the affected area, such as the face, neck, or hands.
You can treat most contact rashes, but it depends on the cause. Follow these guidelines to help ease discomfort and speed up the healing process:
- Use mild, gentle cleansers instead of scented bar soaps.
- Use warm water instead of hot water for washing your skin and hair.
- Pat the rash dry instead of rubbing it.
- Let the rash breathe. If it’s possible, avoid covering it with clothing.
- Stop using new cosmetics or lotions that may have triggered the rash.
- Apply unscented moisturizing lotion to areas affected by eczema.
- Avoid scratching the rash because doing so can make it worse and could lead to infection.
- Apply an over-the-counter (OTC) hydrocortisone cream to the affected area if the rash is very itchy and causing discomfort. Calamine lotion can also help relieve rashes from chickenpox, poison ivy, or poison oak.
- Take an oatmeal bath. This can soothe the itchiness associated with rashes from eczema or psoriasis. Here’s how to make an oatmeal bath.
- Wash your hair and scalp regularly with dandruff shampoo if you have dandruff along with a rash. Medicated dandruff shampoo is commonly available at drugstores, but your doctor can prescribe stronger types if you need them.
Over-the-counter (OTC) medications
Talk with a healthcare professional, who may recommend OTC medication like ibuprofen or acetaminophen to treat mild pain associated with the rash.
Avoid taking these medications for an extended period because they can have side effects. Ask a healthcare professional how long it’s safe for you to take them. You may not be able to take them if you have liver or kidney disease or a history of stomach ulcers.
Call a healthcare professional if the rash doesn’t go away with home remedies. You should also contact them if you’re experiencing other symptoms in addition to your rash and you suspect you have an illness.
If you don’t already have a physician, you can use the Healthline FindCare tool to find a professional near you.
Go to the hospital immediately if you experience a rash along with any of the following symptoms:
- increasing pain or discoloration in the rash area
- tightness or itchiness in the throat
- difficulty breathing
- swelling of the face or limbs
- fever of 100.
 4°F (38°C) or higher
4°F (38°C) or higher - confusion
- dizziness
- severe head or neck pain
- repeated vomiting or diarrhea
Contact a healthcare professional if you have a rash as well as other systemic symptoms, including:
- joint pain
- a sore throat
- red streaks or tender areas near the rash
- a recent tick bite or animal bite
Your healthcare professional will perform a physical exam and inspect your rash. Expect to answer questions about your:
- rash
- medical history
- diet
- recent use of products or medications
- hygiene
Your healthcare professional may also:
- take your temperature
- order tests, such as an allergy test or complete blood count
- perform a skin biopsy, which involves taking a small sample of skin tissue for analysis
- refer you to a specialist, such as a dermatologist, for further evaluation
Your healthcare professional may also prescribe medication or medicated lotion to relieve your rash. Most people can treat their rashes effectively with medical treatments and home care.
Most people can treat their rashes effectively with medical treatments and home care.
Follow these tips if you have a rash:
- Use home remedies to soothe mild contact rashes.
- Identify potential triggers for the rash and avoid them as much as possible.
- Call a healthcare professional if the rash doesn’t go away with home treatments. You should also contact them if you’re experiencing other symptoms in addition to your rash and you suspect you have an illness.
- Carefully follow any treatments your doctor prescribes. Speak with a healthcare professional if your rash persists or gets worse despite treatment.
Healthline and our partners may receive a portion of revenues if you make a purchase using a link above.
Read the article in Spanish.
Rash on Hands and Feet: Common Causes and Treatment
Rashes are earmarked by a change in the color and texture of your skin. They may have blisters, and they may itch or hurt. Rashes that break out on your hands and feet have a wide range of underlying causes.
We’ll explore some of the common conditions that cause rashes to occur on the hands and feet. We’ll also look at treatment options you can try at home, or under a doctor’s care.
| Common causes of rashes on the hands and feet | Overview |
| hand, foot, and mouth disease | contagious infection caused by several viruses, including the coxsackie virus |
| granuloma annulare | chronic, degenerative skin condition with an unknown cause |
| dyshidrotic eczema (dyshidrosis, pompholyx) | itchy, common form of eczema |
| impetigo | contagious, bacterial skin infection |
| hand-foot syndrome (acral erythema or palmar-plantar erythrodysesthesia) | side effect of certain chemotherapy drugs |
| athlete’s foot | contagious fungal infection |
Rashes on the hands and feet can be caused by environmental factors, such as irritants or allergens. They may also be the result of medical conditions or infections.
They may also be the result of medical conditions or infections.
Some common causes of rashes on hands and feet include:
Hand, foot, and mouth diseas
eHand, foot, and mouth disease is a contagious infection caused by several viruses, including the coxsackie virus. Anyone can get hand, foot, and mouth disease, although it most commonly occurs in babies and children.
This condition causes a rash on the hands and feet, as well as sores in the mouth and on the tongue. You may experience fever and a sore throat with this condition.
The hand and foot rash caused by this condition sometimes causes blistering to occur, and may be painful, but not itchy. In some instances, it may appear on the buttocks, as well.
Granuloma annulareGranuloma annulare is a chronic, degenerative skin condition with an unknown cause. There are five recognized types:
- localized granuloma annulare
- generalized or disseminated granuloma annulare
- subcutaneous granuloma annulare
- perforating granuloma annulare
- linear granuloma
The most common type, localized granuloma annulare, causes rings of flesh-toned, red, or yellow nodules to form on the feet, hands and fingers.
These nodules are small and hard, but do not typically itch. The rings usually clear up on their own without treatment, within a few months to two years. They may, however, come back.
Granuloma annulare is more common in women than in men, and tends to occur during young adulthood.
Dyshidrotic eczema (dyshidrosis, pompholyx)
This very itchy, common form of eczema causes deep-set blisters on the palms of hands, edges of fingers, soles and sides of feet, and toes. The blisters can become large and painful, and may last for several weeks.
Dyshidrotic eczema outbreaks often coincide with seasonal allergies, during spring and summer. It’s more common in women than in men. This condition is not curable, but its symptoms can be successfully treated. It’s not contagious.
Impetigo
This very contagious, bacterial skin infection begins with an oozing rash of red sores around the mouth and nose that can be spread to the hands and feet via touch. When the sores burst, they develop brownish-yellow crusts.
The rash can be itchy, and painful. Impetigo most commonly occurs in infants and children. Itching and soreness are other symptoms.
Hand-foot syndrome (acral erythema or palmar-plantar erythrodysesthesia)
This condition is a side effect of certain chemotherapy drugs used for cancer treatment. It’s earmarked by pain, swelling, and redness in either or both the palms of the hands and soles of the feet. It can also cause tingling, burning, and blisters. In severe cases, deeply cracked skin and extreme pain may occur.
Athlete’s foot
Athlete’s foot is caused by a contagious fungal infection. It usually starts between the toes, and spreads to the entire foot. This condition is earmarked by a scaly, red rash that itches.
In some instances, athlete’s foot can spread to the hands. This is more likely to happen if you pick at or scratch the rash on your feet.
Athlete’s foot is caused by keeping very sweaty feet trapped in shoes. It can also be transmitted on locker room and shower floors.
Many hand and foot rashes can be treated at home, but some require medical treatment, based on their underlying cause and severity.
There are a number of over-the-counter and at-home rash treatments that may help alleviate itching and pain, plus reduce the appearance of the rash. You may have the best success by combining several.
Home treatments include:
- topical application of over-the-counter hydrocortisone cream
- topical application of anti-itch medications containing pramoxine
- topical application of lidocaine, or other types of pain medication
- cold compresses
- oral antihistamines
- oral pain medication, such as acetaminophen or ibuprofen
- cool oatmeal baths
- applying unscented moisturizing cream
- avoiding triggers, such as pollen
If you have dyshidrotic eczema: Avoid cobalt and nickel in food and in everyday items. Foods that contain cobalt include clams, fish, and leafy green vegetables. Foods that contain nickel include chocolate, soy beans, and oatmeal.
Foods that contain nickel include chocolate, soy beans, and oatmeal.
If you have impetigo: Cleaning and soaking the blisters and removing the crusts every few days may help. Cover the area with an antibiotic cream and loose dressing after treating.
If your rash does not clear up, your doctor may recommend the following:
- corticosteroid injections
- liquid nitrogen, applied directly to the rash to freeze the area and remove lesions
- oral medication to reduce immune system reactions
- light therapy using a laser
- blister draining
- antibiotics, if infection occurs
Any rash that’s painful, accompanied by fever, or looks infected should be seen by a doctor. You should also seek medical attention for a rash that doesn’t clear up easily with treatments you use at home.
Your doctor may be able to diagnose the rash visually after taking an oral history. In some instances, you may also expect diagnostic tests, such as:
- skin culture
- allergy tests
- skin lesion biopsy
If your child has a rash that does not clear up within one or two days, they should be seen by their pediatrician. This will help determine the cause of the rash, and provide relief for their symptoms.
This will help determine the cause of the rash, and provide relief for their symptoms.
If your child has sores in their mouth or throat that prohibit them from drinking, they should also be seen by their doctor, to avoid complications such as dehydration.
Since conditions such as hand, foot, and mouth disease and impetigo are contagious, make sure to wash your hands after caring for your child.
If you’re a cancer patient experiencing hand-foot syndrome, let your doctor know. Your doctor may be able to change the dosage or type of medication you’re taking.
Rashes on the hands and feet can be caused by a wide range of conditions. These types of rashes sometimes clear up on their own, or they are treated easily at home.
Depending on their underlying conditions, some rashes will respond better to treatments performed or prescribed by a doctor. See your healthcare provider for any rash that’s accompanied by fever or pain.
Rash COVID-19 | A rash can be a symptom of coronavirus
The onset of COVID-19 can be associated with the appearance of various types of skin lesions. They resemble papules, nodules, vesicles, excoriations (abrasions), scales, ulcers, some are in the form of spots, indurations or nets. The rash can occur in people who are asymptomatic with COVID-19. In 21% of patients, dermatosis was the only symptom of SARS-CoV-2 infection. At the same time, 17% of patients reported skin rash as the first manifestation of the disease.
They resemble papules, nodules, vesicles, excoriations (abrasions), scales, ulcers, some are in the form of spots, indurations or nets. The rash can occur in people who are asymptomatic with COVID-19. In 21% of patients, dermatosis was the only symptom of SARS-CoV-2 infection. At the same time, 17% of patients reported skin rash as the first manifestation of the disease.
The incidence of skin symptoms of COVID-19 is difficult to determine. There is also no known relationship between some skin symptoms and disease severity. In addition, it cannot be ruled out that in some patients, skin lesions may be a manifestation of a reaction to multiple treatments for COVID-19.
Contents:
1. Covid-19 rash - where does it appear?
2. What does a COVID-19 rash look like?
coronavirus - when does it occur and how long does it last?
5. Rash as a manifestation of childhood inflammatory multisystem syndrome (PIMS) after COVID-19 in children
6. "Coronavirus fingers"
"Coronavirus fingers"
7. COVID-19 and chickenpox - how is the rash different?
8. Treating COVID-19 rash
Covid-19 rash - where does it appear?
Skin lesions are often the body's response to viral infections. However, in the case of COVID-19, doctors are surprised by the variety of skin rashes, the time of their appearance and location.
Skin lesions associated with COVID-19 occur on various parts of the body, such as around the mouth, trunk, limbs, legs and arms. They are not always accompanied by itching.
What does the rash of COVID-19 look like?
The rashes associated with Covid-19 are varied and similar to skin lesions associated with other viral diseases, according to a study conducted by specialists in Spain. They noted that skin changes did not correlate with the severity of the infection: some were accompanied by asymptomatic COVID-19, others - severe forms of infection.
Five types of rash were noted:
• Irregular frostbite-like patches on the arms and legs, sometimes accompanied by soreness and itching. Mostly encountered in young patients with a mild course of the disease, appeared in the later stages and lasted about 12 days. Registered in 19% of cases.
Mostly encountered in young patients with a mild course of the disease, appeared in the later stages and lasted about 12 days. Registered in 19% of cases.
• Focal eruption in the form of small vesicles, which can cause itching, located on the body and upper and lower limbs. Occurs at the time of the onset of any other symptoms and occurs at 9% of cases in middle-aged patients; kept for 10 days.
• Urticaria-like patchy eruption, white or pink, often itchy. They were noted in 19% of cases, mainly on the body, but also happened on the palms.
• Maculopapular eruptions in the form of small flat or bulging vesicles, which were observed in 47% of cases. These rashes persisted for about a week and appeared simultaneously with other symptoms, but most often accompanied by a severe course of the disease.
• The appearance of a vascular red-blue network or signs of skin necrosis on the skin was observed in 6% of patients, mostly elderly with a severe course of the disease.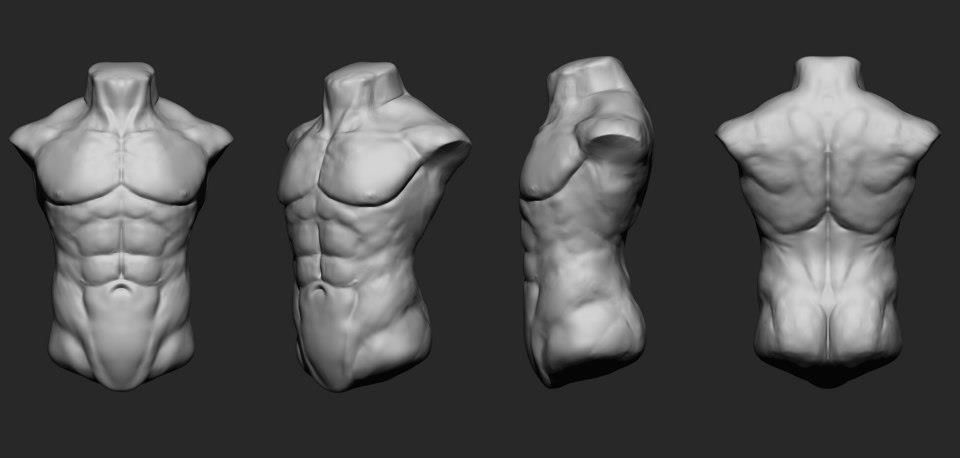
At the same time, experts note that the rash can have a different origin, and it is difficult to classify it without having the appropriate experience and knowledge.
In case of any skin symptoms, Medicover dermatologists with many years of experience and extensive experience in diagnosing various skin lesions are always ready to help you!
Skin lesions and diagnosis of COVID-19
Diagnosis of dermatological changes caused by COVID-19 consists primarily in the exclusion of other possible causes of rashes, such as allergies.
This may require a series of studies to determine if the rash is related to SARS-CoV-2 infection, or if it is a reaction of the body to certain medications, or if the infection is caused by other pathogens.
If finger pressure on purple-red skin lesions does not cause them to disappear, this is an alarm that indicates the need to seek medical attention in order to rule out infection with the SARS-CoV-2 virus.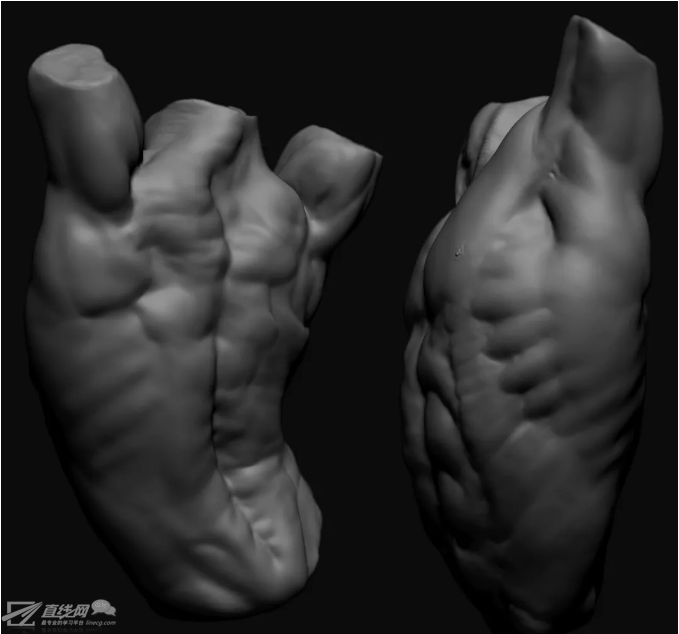
In Medicover clinics, you can get professional advice from a dermatologist and undergo all the necessary examinations to establish an accurate diagnosis, as well as get advice on effective treatment in accordance with modern international clinical guidelines.
Coronavirus rash - when does it occur and how long does it last?
The first symptoms of COVID-19 can occur approximately 5-6 days after infection, sometimes this period is extended up to 14 days. However, a rash can be both the first symptom and the only sign of COVID-19..
Depending on the type of skin lesions and their severity, they last from several days to several weeks.
Skin rash may be accompanied by other systemic symptoms associated with COVID-19. These include:
• fever
• Permanent cough
• shortness of breath, breathing problems,
• Fatigue
• Ground
• Dizziness
• Loss of smell and taste.
rash as a manifestation of children inflammatory multisystem syndrome (PIMS) after COVID-19in children
Viral diseases are a common cause of skin lesions in children.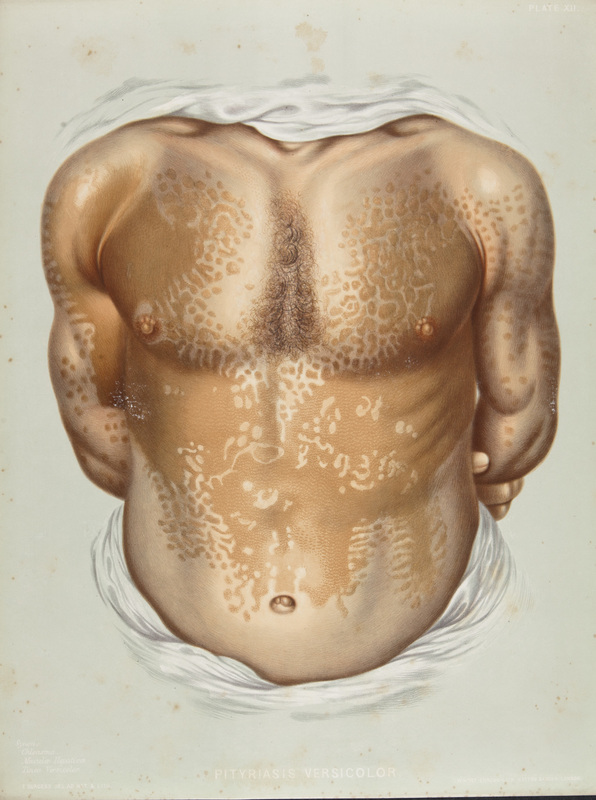 A rash caused by SARS-Cov-2 may appear on a child's skin up to 2-4 weeks after infection and indicate the development of childhood inflammatory multisystem syndrome associated with SARS-CoV-2.
A rash caused by SARS-Cov-2 may appear on a child's skin up to 2-4 weeks after infection and indicate the development of childhood inflammatory multisystem syndrome associated with SARS-CoV-2.
PIMS with multiform inflammatory syndrome in children sometimes occurs after COVID-19 infection, sometimes even after asymptomatic infection. PIMS most commonly occurs in schoolchildren around the age of 9years.
In the case of children, skin lesions caused by SARS-CoV-2 infection may appear as reddish papules, resembling other viral exanthems. Papules may appear on the face and back, and within 3-5 days they disappear spontaneously.
Any rash in children should be consulted with a pediatrician. Until an accurate diagnosis is established and the connection with COVID-19 is excluded, children should not come into contact with other people, especially the elderly, who are prone to a severe course of coronavirus infection up to death.
"Coronavirus fingers"
Skin lesions in the form of so-called "coronavirus fingers" are more often diagnosed in young people, adolescents and children.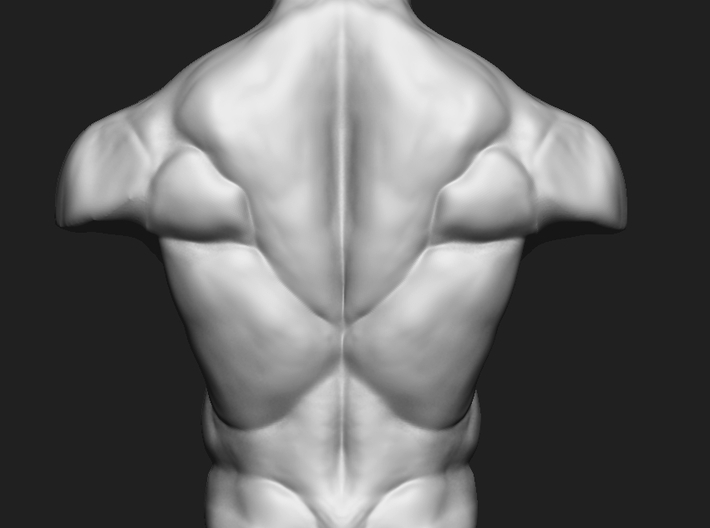 They take the form of red spots, vesicles and even ulcers, accompanied by swelling of the skin of the fingers and interdigital spaces.
They take the form of red spots, vesicles and even ulcers, accompanied by swelling of the skin of the fingers and interdigital spaces.
COVID-19 and chickenpox - how is the rash different?
Papulo-vesicular eruptions in COVID-19 and chickenpox are very similar to each other. They differ in the age of patients and localization of skin lesions.
In SARS-CoV-2 infection, skin lesions are more common in adults with a mean age of 60 years. However, one of the main clinical features is the localization of lesions in the trunk area, the elements are diffuse in nature, they are characterized by the absence of itching.
The rash appears 3 days after the onset of symptoms of COVID-19 and spontaneously disappears after 8 days without leaving marks, while with chickenpox the rash can be biphasic and last up to 2 weeks.
Treatment of rash due to COVID-19
Rash due to SARS-CoV-2 infection does not require specific medical procedures. Clinical data show that it is enough to simply observe its course and apply symptomatic treatment if necessary. Useful antihistamines that relieve itching and swelling of the skin. Mild patients can use them at home.
Clinical data show that it is enough to simply observe its course and apply symptomatic treatment if necessary. Useful antihistamines that relieve itching and swelling of the skin. Mild patients can use them at home.
In case of serious and significant skin lesions, systemic treatment with corticosteroids under medical supervision is recommended.
Where does the rash on the body come from and what to do about it
Share
0A rash on the body is a common occurrence. Most often, it does not harm Rash 101 in adults: When to seek medical treatment health: small red spots, pimples, blisters spoil the appearance, itch, but quickly disappear by themselves.
However, sometimes rashes can be symptoms of serious and even life-threatening disorders.
When to seek medical treatment as soon as possible
Go to a GP, dermatologist, nearest emergency room as soon as possible, or call an ambulance if Rash 101 in adults: When to seek medical treatment:
- The rash has spread all over the body .
- Rash accompanied by fever. A temperature above 38.3 °C indicates an acute inflammatory process.
- The rash on the body appeared suddenly and is getting thicker. This may be a sign of a powerful allergic reaction that risks developing into Quincke's edema or even anaphylactic shock. Be especially careful if the rash appears on the face and neck. If you notice that it is becoming difficult to breathe, immediately dial 103 or 112.
- The rash is blistering. That is, in place of numerous red spots, bubbles filled with liquid begin to appear.
- The rash is painful to touch.
- The rash on the body is very itchy and you easily scratch it until it bleeds. In this case, there is a risk of introducing an infection into the wounds and getting blood poisoning.
If there are no threatening symptoms, exhale. Most likely, nothing bad is happening to you.
Now reading 🔥
- What to do if the temperature persists at 37 °C
Causes of a rash on the body
It is often difficult to immediately determine where the rashes come from. Here are some of the most common variations of What is causing my rash?.
Here are some of the most common variations of What is causing my rash?.
Insect bites
View image
Close
The bite of a mosquito or, say, a bee is easy to identify: in its place there is a rounded dense swelling that itches or hurts. You can’t confuse such damage to the skin with a rash. But there are insects whose bites look like rashes. These are, for example, fleas - bed or sandy.
If you find itchy red dots on your skin in the morning or after the beach, you may have been bitten.
Photoallergy
Open image
Close
AKA allergic reaction Sun Allergy to ultraviolet ("sun poisoning"). The rash may be different:
- small itchy redness;
- flesh-coloured pimples that feel like sandpaper;
- blisters;
- patches of distinct red color tending to merge into a single whole.
Most often, an allergy to the sun occurs due to the fact that during tanning, some harmful substance was present on the skin - cream, lotion, medicine, plant juice - and ultraviolet turned it into an allergen. Alternatively, you may be taking medication that has made your skin sensitive to the sun.
Alternatively, you may be taking medication that has made your skin sensitive to the sun.
Contact dermatitis
View image
Close
Occurs when some toxic substance (allergen) comes into contact with the skin and the epidermis reacts with irritation and rashes in response. Allergens are often:
- The sap or pollen of some plants, such as poison ivy or nettle. A skin reaction to nettle pollen is so common that the characteristic skin rash is called hives.
- Latex.
- Certain metals that may be found in jewelry, hair clips, key rings. Most often, allergies occur on nickel, cobalt, chromium, copper.
- Various cosmetic products, from creams to eau de toilette.
- Dyes in cheap clothes.
Drug Allergy
View Image
Close
Rash and itching can be side effects of certain medications, such as antibiotics. If you have recently started taking a new medicine, check the package leaflet. At the same time, check if there is any mention that the drug has a photosensitizing (that is, increasing sensitivity to sunlight) effect.
At the same time, check if there is any mention that the drug has a photosensitizing (that is, increasing sensitivity to sunlight) effect.
Pollinosis
Open image
Close
Also known as pollen allergy. This variant can be suspected if the rash appeared against the background of other signs of an allergic reaction:
- runny nose;
- watery eyes;
- compulsive coughing or sneezing.
Food Allergy
View Image
Close
May manifest itself as hives that appear on different parts of the body, and scarlet rashes on the cheeks (this symptom is more common in young children).
The most common food allergens are Food Allergies:
- eggs;
- milk;
- peanuts and tree nuts;
- fish and crustaceans;
- wheat;
- soy.
Skin infections
Rash may appear due to bacteria, fungi, viruses attacking the epidermis.
For example, with ringworm, round, itchy patches with a bright border appear. This fungal infection, contrary to stereotypes, can attack not only the scalp, but also any other part of the skin.
This fungal infection, contrary to stereotypes, can attack not only the scalp, but also any other part of the skin.
Open image
Close
An example of a viral infection is molluscum contagiosum. This disease makes itself felt by raised reddish-brown and, importantly, hard bumps with a diameter of 1-5 mm, which can appear on any part of the body. Despite the name, no shellfish lives under the skin. This is the skin's reaction to the virus.
View image
Close
What to do if you have a rash on your body
The symptoms that require you to see a doctor as soon as possible are described above. If you do not have them, you can try to cope with the rash at home What is causing my rash?.
- Keep your skin clean. In the morning, evening, and as it gets dirty, gently wash it with warm water and a mild, unscented soap. Until the rash goes away, stop using hard washcloths and brushes.
- Wear soft, breathable clothing.