Rash like measles
Roseola vs. measles rash: What is the difference?
Roseola and measles are two different diseases that present with a high fever and a rash. They are both most commonly seen in childhood, although measles can affect people of any age, and roseola in adults is very rare.
While both diseases share similarities, there are distinguishing factors, such as how the symptoms present and the disease progression.
Read on to find out the difference between roseola and measles rashes.
Roseola, also known as roseola infantum, sixth disease, or exanthema subitum, is a viral infection that typically affects children. The human herpesvirus 6 (HHV-6) or human herpesvirus 7 (HHV-7) causes roseola.
The disease is spread through tiny respiratory droplets that people either breathe in or pick up from surfaces they touch.
This disease usually presents in children between the ages of 6–12 months. Children who have this disease experience a high fever, followed by a pink or red rash.
Roseola is a self-limiting viral illness, meaning it will typically go away without any medical attention. Doctors advise treating roseola at home unless the child has seizures or persistent high fever.
Measles is a very infectious disease that killed more than 140,000 people in 2018 globally. A majority of these were children under 5 years old.
The measles virus is a part of the Paramyxoviridae family, and the Morbillivirus genus and people can spread this through direct contact and the air.
People who have measles often experience a high fever and a rash. Measles carries a higher risk of complications in children under 5 years old, or adults over 30 years.
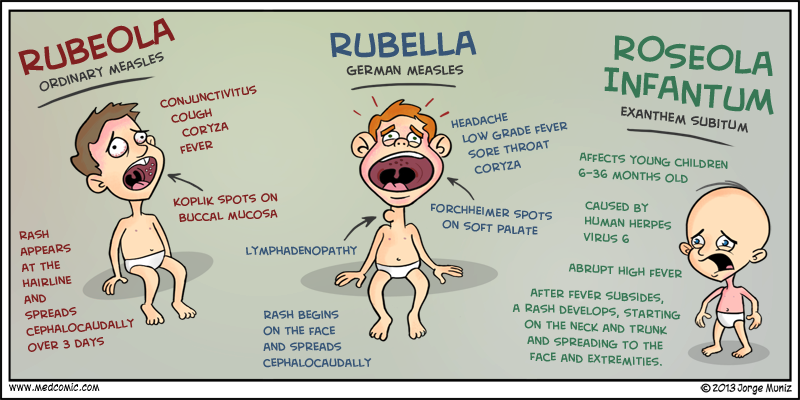
Both roseola and measles may look similar in appearance as they usually present with a maculopapular rash. However, roseola rash is usually more pink-red, while measles rash is more red-brown.
While it may be easy to confuse the two, other features help to differentiate between roseola and measles.
The rash from roseola begins in the torso and spreads out, while the measles rash starts on the face and moves downwards.
Additionally, children with roseola usually appear well, while those with measles typically look and behave as if they are unwell.
Roseola
Roseola shows a unique disease progression in that the rash appears shortly after the fever ends.
The fever will last roughly 3–5 days, and, as it subsides, children will experience small pink-red bumps and rashes, approximately only 2–5 millimeters across. Sometimes, a pale halo will appear around these areas.
The rash usually starts on the torso and spreads to the neck, face, legs, and arms within 24 hours.
The rash is usually not itchy and turns white under pressure. The rash usually disappears after 1–2 days.
Measles
Similarly to roseola, the measles rash appears roughly 3–5 days after symptoms begin.
In the case of measles, however, the fever symptoms do not subside and instead accompany the rash.
While the measles rash is also not usually itchy, it consists of distinct red spots that start along the hairline and then spread downwards to the neck, torso, limbs, and feet.
Some people may have small, raised bumps, and these may merge as the rash spreads.
A defining characteristic of measles is that the fever disappears when the rash stops spreading.
In addition to fever and rash, both diseases may also include other symptoms, as follows:
Roseola
Children with roseola may also experience:
- a high fever that may be above 104oF,
- conjunctivitis
- swelling around the eyes
- malaise
- irritability
- loss of appetite
- diarrhea
- cough
- Nagayama spots, bumps in the mouth between the soft palate and uvula
- swelling of the inner ear
- swelling of the lymph nodes
Roseola does not tend to have many complications. However, around 15% of children with roseola experience seizures due to the high fever. The symptoms of a seizure include:
The symptoms of a seizure include:
- fainting
- twitching or jerky movements
- a potty trained child soiling themselves
- irritability
Measles
People with measles will also experience a cough, conjunctivitis, and a runny nose along with the rash and fever.
Some children will experience Koplik spots 2–3 days after symptoms begin. Koplik spots are tiny white spots that appear in the mouth.
Measles can be fatal in some cases. Most people who die from measles complications are children under 5 years old, or adults over 30 years old.
Some serious complications include:
- blindness
- brain swelling
- severe diarrhea and dehydration
- ear infections
- pneumonia
Roseola resolves relatively quickly. The fever lasts 3–5 days, followed by the rash. The rash lasts around 2 days.
Measles symptoms can last up to 2 weeks after a person is infected. People who do not experience any complications usually recover a week after the appearance of the rash.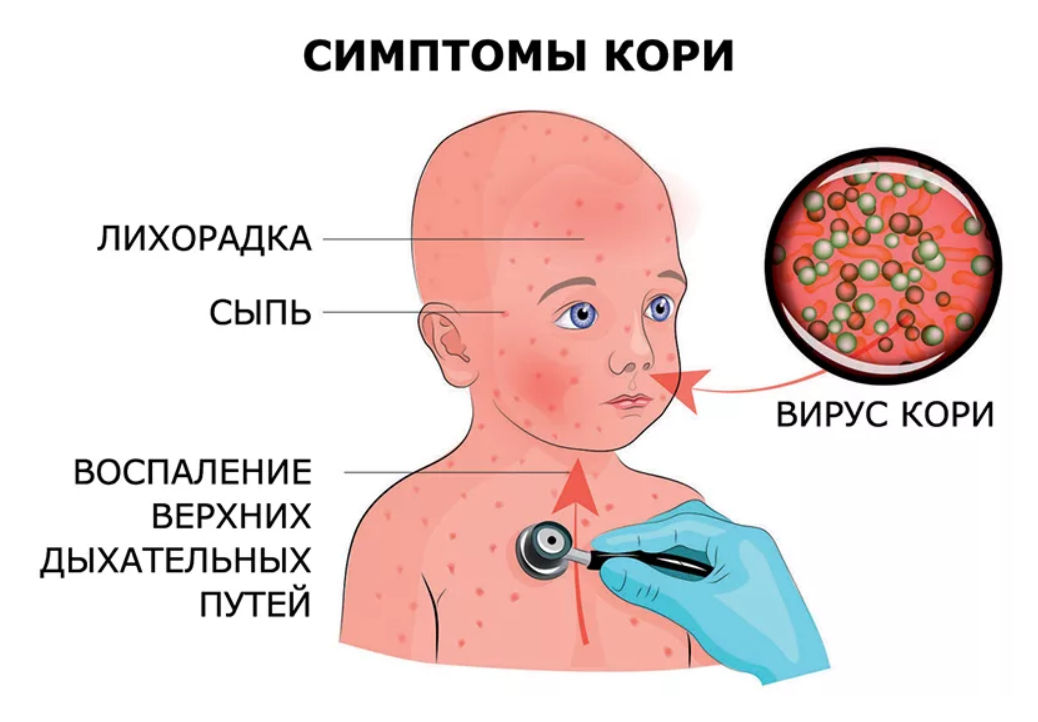
People may be able to treat both diseases in a similar way. Some treatment options include:
Roseola
Doctors do not have a specific treatment for roseola. They recommend rest and fluids, with painkillers such as acetaminophen, or anti-inflammatories such as ibuprofen to control the fever. However, unless a doctor advises, carers must not give aspirin to a child with fever due to the risk of Reye’s syndrome.
Measles
As with roseola, there is no specific treatment for measles. People can use painkillers and anti-inflammatories to control the fever and drink lots of fluid to prevent dehydration.
The World Health Organization (WHO) recommend daily doses of vitamin A for 2 days for those who are malnourished or immunocompromised.
Measles is a preventable disease as there is a safe, inexpensive, and effective vaccine.
While it may be possible to treat symptoms of both diseases at home with rest, painkillers, and fluid, seeing a doctor as soon as anyone starts showing symptoms of measles is important.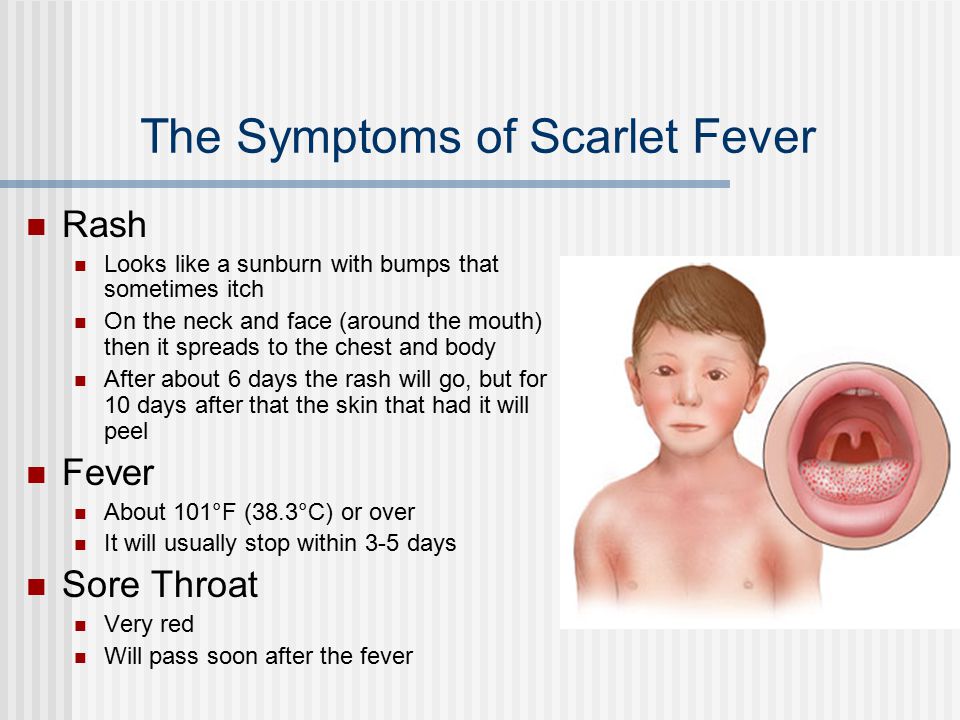
If a person displays persistent high fever or rash, it is advisable to seek medical attention. Emergency medical care is necessary if a child has a febrile seizure.
Both roseola and measles are illnesses that commonly affect children. Both of these diseases present with a rash and fever, however, their disease progression is different.
The rashes of both diseases vary in color, and roseola rash starts in the torso and spreads out, while measles rash begins in the face and spreads downwards.
Neither of these diseases has a specific treatment. Doctors instead advise that people treat the fever with anti-inflammatories and painkillers, and drink lots of fluids.
It is essential to seek medical attention if a very high fever occurs, or if there are any signs of complications.
Rubella (german measles) - NHS
Rubella (german measles) is a rare illness that causes a spotty rash. It usually gets better in about a week, but it can be serious if you get it when you're pregnant.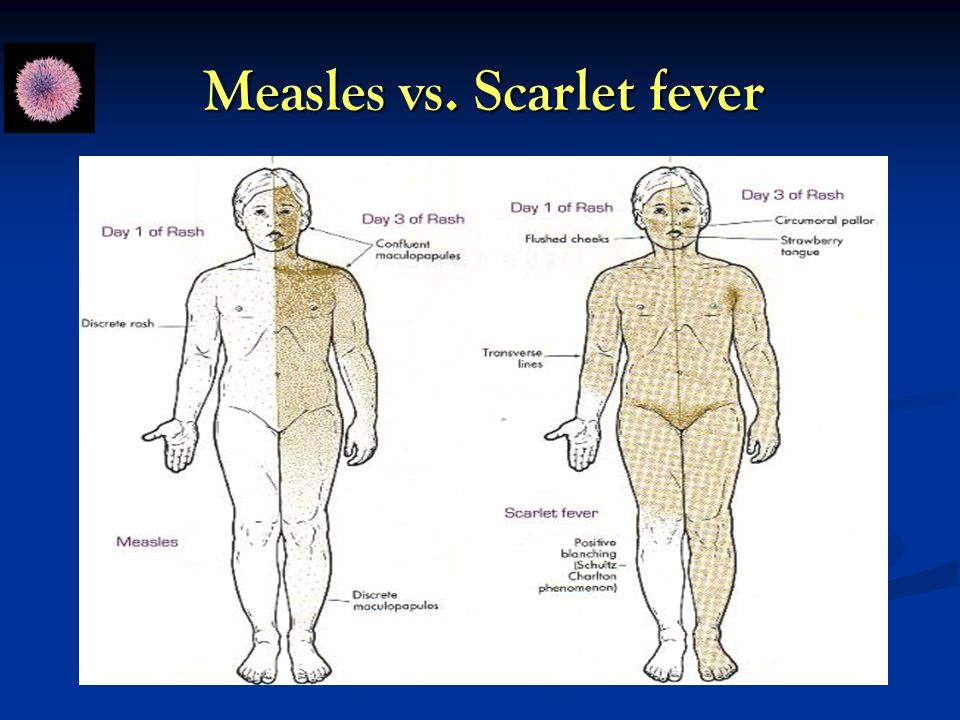
Check if you or your child have rubella
The main symptom of rubella is a spotty rash that starts on the face or behind the ears and spreads to the neck and body.
The rash takes 2 to 3 weeks to appear after getting rubella.
The rash looks red or pink on white skin.Credit:
PR. PH. FRANCESCHINI/CNRI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259748/view
It can be harder to see on brown or black skin, but might feel rough or bumpy.Credit:
DR P. MARAZZI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259492/view
You might also have lumps (swollen glands) in your neck or behind your ears.Credit:
DR P. MARAZZI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259236/view
MARAZZI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259236/view
Rubella can also cause:
- aching fingers, wrists or knees
- a high temperature
- coughs
- sneezing and a runny nose
- headaches
- a sore throat
- sore, red eyes
Information:
It's very unlikely to be rubella if you have had both doses of the MMR vaccine or had rubella before.
See other rashes in children and babies
Non-urgent advice: Call a GP if:
- you or your child have symptoms of rubella
Rubella can spread to others. It's best to call before you go in. The GP may suggest talking over the phone.
The GP may suggest talking over the phone.
How to look after yourself or your child
Rubella usually gets better in about a week.
After getting advice from a GP, you or your child should:
- get plenty of rest
- drink lots of fluids, like water or squash
- take paracetamol or ibuprofen if you're uncomfortable – do not give aspirin to children under 16
How to avoid spreading rubella
Rubella spreads in coughs and sneezes.
It’s infectious from 1 week before the symptoms start and for 5 days after the rash first appears.
It can be serious for some people, so you should try to avoid spreading it to others.
Do
-
stay off nursery, school, or work for 5 days after the rash appears
-
try to avoid close contact with anyone who is pregnant
-
wash your hands often with soap and warm water
-
use tissues when you cough or sneeze
-
throw used tissues in the bin
Don’t
-
do not share cutlery, cups, towels, clothes, or bedding
Rubella in pregnancy
Rubella is very rare in pregnancy. But if you get it when you're pregnant, rubella could harm your baby.
But if you get it when you're pregnant, rubella could harm your baby.
It can cause:
- loss of the baby (miscarriage)
- serious problems after the baby is born – such as problems with their sight, hearing, heart, or brain
The risk is highest if you get rubella early in pregnancy.
There's not thought to be a risk to your baby if you get rubella after week 20 of your pregnancy.
Urgent advice: Call your midwife, maternity unit, or GP immediately if:
You're pregnant and either:
- you have a new rash
- you’ve been in close contact with someone who has rubella
Get vaccinated against rubella
The MMR vaccine can prevent rubella. It also protects you from measles and mumps.
It also protects you from measles and mumps.
The MMR vaccine is offered to all children in the UK. 2 doses can give lifelong protection against measles, mumps, and rubella.
Ask at your GP surgery if you're not sure you or your child have had the vaccine. They can give it for free on the NHS.
Find out more about the MMR vaccine
Page last reviewed: 23 May 2022
Next review due: 23 May 2025
Measles - signs, symptoms, treatment of measles in children - Murmansk City Children's Clinic No. 1
By smaweb Healthy child
Measles is an acute infectious disease, the distinguishing features of which are a typical rash, as well as damage to the conjunctiva of the eyes and mucous membranes of the upper respiratory tract.
Nature, development and spread of infection
Measles is a viral infection spread by airborne droplets. The measles virus enters the body through the mucous membrane of the upper respiratory tract, from where it spreads through the blood throughout the body. The virus selectively damages the cells of the skin, mucous membranes of the eyes, respiratory tract and oral cavity, which causes typical manifestations of the disease.
The measles virus enters the body through the mucous membrane of the upper respiratory tract, from where it spreads through the blood throughout the body. The virus selectively damages the cells of the skin, mucous membranes of the eyes, respiratory tract and oral cavity, which causes typical manifestations of the disease.
The source of measles infection is only a sick person capable of shedding the virus into the external environment from the last two days of the incubation period to the fourth day after the onset of the rash. People who have not received prophylactic measles vaccination and have not had measles throughout their lives remain susceptible to infection, so the disease can develop at any age.
Before the introduction of measles vaccine, 95% of cases were in children under 16 years of age. After the widespread vaccination of children, a significant decrease in the incidence of measles was noted, but individual cases and limited outbreaks were noted constantly, and now there is a tendency for them to increase.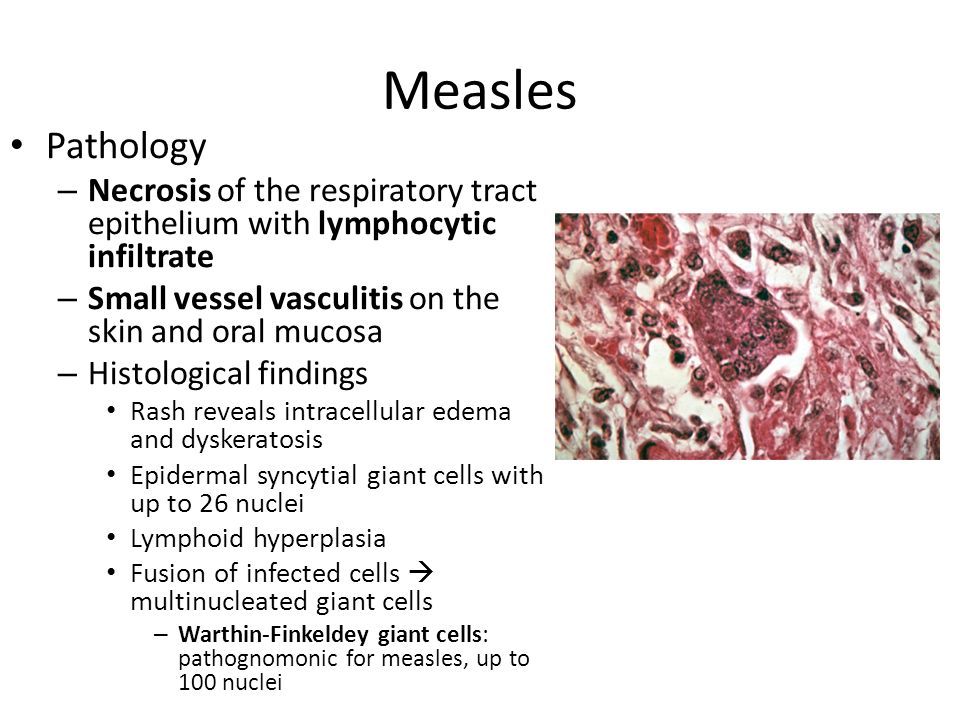 Complete protection against measles requires immunization 94-97% of children under 15 months of age. However, this level of vaccination is practically unfeasible even for developed countries.
Complete protection against measles requires immunization 94-97% of children under 15 months of age. However, this level of vaccination is practically unfeasible even for developed countries.
Measles outbreaks can also occur among vaccinated individuals (67-70% of all outbreaks). As a rule, they are typical for older age groups (children of school age, teenagers, military personnel, students, etc.). The nature of such cases of the disease is associated with a drop in the intensity of immunity after a long period (10-15 years) after vaccination.
Signs and course of the disease
The duration of the latent period of infection is 9-11 days. The introduction of immunoglobulin for prophylactic purposes can contribute to its lengthening up to 15-21 days (sometimes more). From the second half of the latent period, the initial symptoms of the disease may be noted (weight loss in a child under one year old, evening subfebrile condition, slight cough and runny nose, swelling of the lower eyelid, redness of the conjunctiva).
The initial non-specific period begins with an increase in body temperature to 38-39°C, weakness, lethargy, loss of appetite are noted. Cough acquires a rough "barking" character, runny nose and redness of the conjunctiva intensify. During this period, the doctor can identify a specific sign of measles - small whitish spots on the mucous membrane of the cheeks, soft and hard palate, similar to semolina or bran (Filatov-Koplik spots).
On the 3rd-4th day, the fever decreases somewhat, but from the moment the rash appears, it increases again. The same applies to signs of damage to the respiratory system. The period of the rash is characterized by a strict staging. First, the elements appear on the face and neck, on the 2nd day - on the trunk, thighs, arms, on the 3rd day, the elements of the rash appear on the feet and legs, and on the face they already turn pale. As a rule, the maximum number of elements of the rash is localized on the face, upper chest and neck.
The rash is represented by irregularly shaped patches, slightly elevated in the center above the surface of the skin. The spot diameter usually does not exceed 10 mm, the spots show a tendency to merge. The fading of the rashes begins on the 3-4th day after their appearance, they leave behind a brownish pigmentation, later peeling occurs on the face and trunk in these places.
The spot diameter usually does not exceed 10 mm, the spots show a tendency to merge. The fading of the rashes begins on the 3-4th day after their appearance, they leave behind a brownish pigmentation, later peeling occurs on the face and trunk in these places.
A typical sign of measles is conjunctivitis, which in most cases is purulent. Often there is gluing of eyelashes in the morning (when waking up) with purulent discharge. The layering of a purulent infection can cause the development of pneumonia. A severe complication is damage to the central nervous system, which is quite rare.
what kind of disease? Symptoms, treatment, consequences
Measles, what kind of disease? How to recognize in time, what are its consequences, how is it treated? We will talk about everything in this article. Measles is a viral disease that is transmitted by airborne droplets directly from an infected person.
A bit of history.
When did measles appear? The history of the disease will help us to understand that issue.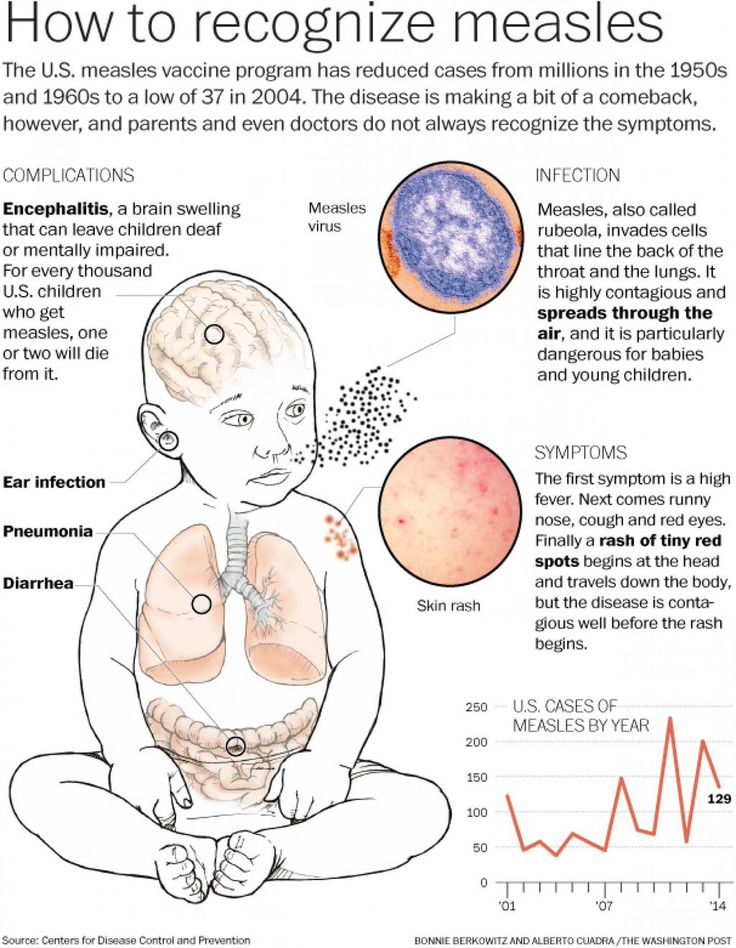 The first case that was recorded occurred at 9century, and was described by an Arab physician, Rhazes. The doctor mistakenly thought that the patient had a mild form of smallpox. Therefore, at first measles had the name "small disease" (morbilli), and smallpox - morbus, which means "great disease". What kind of disease is measles? What symptoms does it have and how does it proceed? This was established only in the 17th century, thanks to Sydenhom (England) and Morton (France). But these doctors could not establish the cause of the disease, and only in 1911 experiments were carried out on monkeys, and it was possible to establish that measles is an acute viral disease that is transmitted by airborne droplets. The causative agent of the disease was identified only in 1954 year. Measles is a disease that everyone should be aware of. From the middle of the 19th century to the beginning of the 20th century, measles was the most dangerous childhood disease, which often ended in death. It was only after the development of a vaccine that the epidemic of the disease was reduced.
The first case that was recorded occurred at 9century, and was described by an Arab physician, Rhazes. The doctor mistakenly thought that the patient had a mild form of smallpox. Therefore, at first measles had the name "small disease" (morbilli), and smallpox - morbus, which means "great disease". What kind of disease is measles? What symptoms does it have and how does it proceed? This was established only in the 17th century, thanks to Sydenhom (England) and Morton (France). But these doctors could not establish the cause of the disease, and only in 1911 experiments were carried out on monkeys, and it was possible to establish that measles is an acute viral disease that is transmitted by airborne droplets. The causative agent of the disease was identified only in 1954 year. Measles is a disease that everyone should be aware of. From the middle of the 19th century to the beginning of the 20th century, measles was the most dangerous childhood disease, which often ended in death. It was only after the development of a vaccine that the epidemic of the disease was reduced. Mandatory vaccination has been able to reduce the activity of the disease, and in some countries even eliminate it altogether. However, cases of the disease are recorded and today, annually, according to WHO statistics, about 30 thousand people die.
Mandatory vaccination has been able to reduce the activity of the disease, and in some countries even eliminate it altogether. However, cases of the disease are recorded and today, annually, according to WHO statistics, about 30 thousand people die.
Symptoms in children.
First of all, it is worth noting that children aged from one to 7 years are most susceptible to infection, cases of infection of children older than 7 years and adults are less often recorded.
Important to know: measles begins to manifest itself after 7-14 days. What kind of disease is measles? How to diagnose it? In order to start treatment on time, you need to be able to recognize the disease.
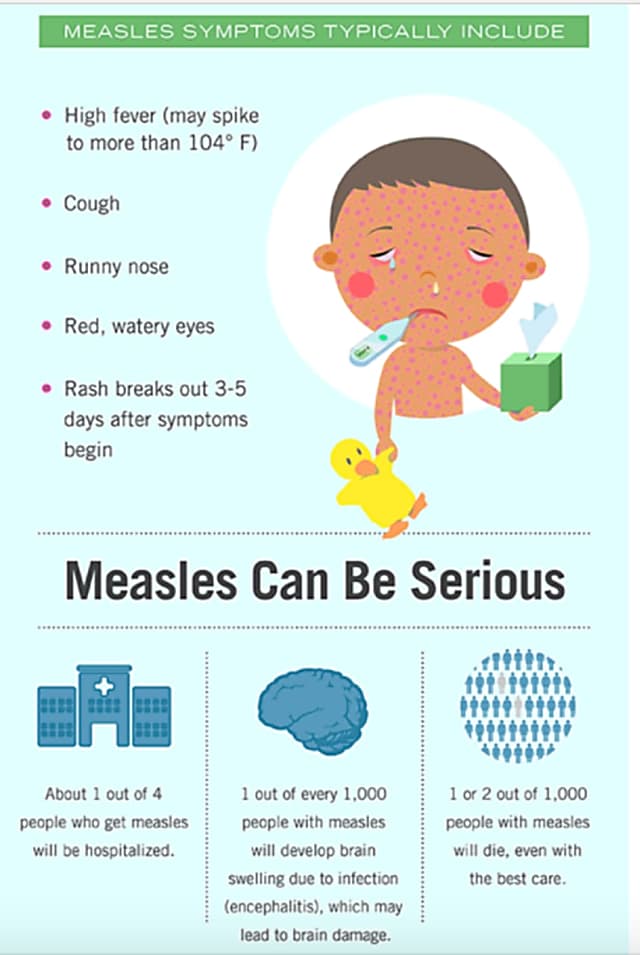
Measles disease in children has the following symptoms:
- Feeling unwell.
- Sleep disturbance.
- Lethargy.
- Fatigue.
- Headache.
- Poor appetite, or its complete absence.
- Temperature increase.

The catarrhal stage lasts from 3 to 5 days. The symptoms are as follows:
- Sore throat.
- Cough appears.
Further worse. The disease begins to affect the vessels, small capillaries in the eyes and skin begin to burst. A runny nose with purulent discharge begins. Puffiness appears on the face, the eyes become swollen. An infected child develops a fear of light, from which he constantly squints his eyes. The temperature rises to 40 degrees, gradually the cough becomes stronger, vomiting may occur.
It is only after the child shows the main symptoms of measles that an accurate diagnosis is made.
To make a diagnosis, the doctor must prescribe:
- Complete blood count.
- Urinalysis.
- Virus isolation test in blood.
- Chest x-ray.
- In some cases, electroencephalography.
Main symptoms of the disease: measles in children
- Small, grain-sized rashes on the inside of the lips and cheeks.
 In the presence of such symptoms, the child must be isolated.
In the presence of such symptoms, the child must be isolated. - Unlike other childhood diseases, measles rash does not appear in a chaotic manner, but in stages. First of all, pink spots appear on the scalp and behind the ears. Then they move to the bridge of the nose, and gradually spread over the entire face. On the second day, the rash begins to spread over the upper body (arms, chest). Third day - legs.
- From the moment the rash appears, the body temperature rises sharply to 40 degrees.
- Loose period lasts from 4 to 7 days.
Symptoms of measles in adults.
Although measles is commonly considered a childhood disease, adults are still not immune from infection. How does the disease progress in adults, what symptoms indicate the disease? We will consider the main signs of the disease. Measles is something that cannot be ignored!
- First of all, the state of health deteriorates sharply, appetite disappears, terrible headaches and insomnia appear.
 The sick person feels like with a cold, his throat tickles, a runny nose appears, the temperature rises sharply, and the lymph nodes increase.
The sick person feels like with a cold, his throat tickles, a runny nose appears, the temperature rises sharply, and the lymph nodes increase. - After 2 - 5 days all symptoms disappear, strength and cheerfulness appear.
- A day after the improvement, the disease comes with renewed vigor. All symptoms return, but more acutely and painfully.
- The next stage is a rash. Many spots appear, which subsequently combine and turn into one continuous spot. The rash appears in a certain sequence: behind the ears, head, upper body, lower body.
Therapy
Measles is a very insidious disease. Treatment must begin immediately. How should it happen in children? After the doctor has prescribed tests, and the diagnosis is confirmed, treatment is prescribed. Unfortunately, to date, a single cure for measles has not been developed, so all efforts are directed to treating the symptoms.
Ibufen and paracetamol antipyretics are prescribed for children.
High fever and vomiting lead to dehydration, so it is imperative to observe the drinking regimen.
- Since the child develops a fear of light, the windows in the room where he is staying should be covered with dark thick curtains. Use a night light in the evening.
- Antihistamines are used to relieve swelling and itching from rashes.
- The doctor prescribes expectorants to help ease the coughing spells.
- Drops were put into the nose (vasoconstrictor) and into the eyes (for conjunctivitis).
- The throat and oral cavity are treated with chamomile.
- Antibiotics are being taken.
- Chapped lips from high temperatures should be lubricated with a damp handkerchief.
An infected child should not come into contact with other children, he is prescribed bed rest and complete rest. In addition to medicines, it is imperative to ventilate the room, do wet cleaning 2 times a day, and humidify the air. A prerequisite for treatment is diet. All the food that the child eats should be high-calorie, since the body needs a lot of strength to fight the virus. But at the same time, food should be easily digestible, natural. Hospitalization for measles is rare, only in cases where the symptoms of the disease are very acute. Basically, patients stay at home and follow all the instructions of the doctor.
A prerequisite for treatment is diet. All the food that the child eats should be high-calorie, since the body needs a lot of strength to fight the virus. But at the same time, food should be easily digestible, natural. Hospitalization for measles is rare, only in cases where the symptoms of the disease are very acute. Basically, patients stay at home and follow all the instructions of the doctor.
Treatment of measles in adults
The first thing to do is to alleviate the patient's condition. Antibiotics are used to fight inflammation. If the disease is mild, then there is no need for hospitalization. In order to make up for the loss of fluid in the body, you need to drink plenty of water, syrups, tea, compotes. –
Since the mucous membranes of the mouth become inflamed during measles, special attention must be paid to hygiene. The throat must be gargled with infusion of chamomile and a water-salt solution. Also, treatment necessarily includes cough medicines with an expectorant effect, prednisone, and antipyretics.
Complications of measles
- The most dangerous and common complications that measles can cause:
- Pneumonia is an infectious inflammation of the lungs.
- Visual impairment, rarely total blindness.
- Otitis is an inflammatory process in the ear.
- Laryngitis is an inflammatory process in the mucous membranes of the larynx.
- Encephalitis - inflammation of the brain.
- Stomatitis - inflammation of the oral mucosa.
- Polyneuritis - multiple lesions of nerve fibers.
- Bronchopneumonia is an acute inflammation of the bronchi.
Complications in adults
In most cases, measles does not leave any consequences, but still, although rarely, the disease does not make itself forgotten even after treatment. So why is measles dangerous?
Consequences of the disease in adults may be as follows:
- Bronchiolitis is an acute inflammation of the bronchioles, transmitted by airborne droplets.

- Croup - inflammation of the respiratory tract. Bronchitis.
- Mild myocarditis - damage to the heart muscle.
- Sometimes the disease leaves an imprint on vision, can lead to complete blindness.
Prophylaxis
There are two types of prophylaxis: emergency and planned. Emergency prophylaxis is carried out if the fact of contact with an infected person is precisely established. But at the same time, it must be reliably known that the child has not previously had measles and has not been vaccinated. In such cases, immunoglobulin is administered. The drug must be administered within 5 days from the date of contact. Routine prevention is nothing more than vaccination. What is a vaccination? This is an artificial introduction of a virus so that the body can develop immunity. According to the vaccination schedule, the child receives the first routine measles vaccination at 1 year, the second - at 6 years.
After a routine vaccination, every mother is warned about the possible consequences and reactions of the child's body. Therefore, the mother must carefully monitor the condition of the child after vaccination. There are symptoms, upon the appearance of which parents should immediately respond and seek medical help. Among them:
Therefore, the mother must carefully monitor the condition of the child after vaccination. There are symptoms, upon the appearance of which parents should immediately respond and seek medical help. Among them:
- Runny nose.
- Conjunctivitis.
- Temperature increase.
- Cough.
Particular vigilance must be exercised from 5 to 20 days after the introduction of the virus. Any rash on the body is a reason to go to the doctor. After all, it is better to make sure once again than to risk the health of the child. Any mother should know that each vaccination is given only to a healthy child. From the moment of the last illness should pass from 1 to 6 weeks. Anyone can get a measles vaccine, for this you need to contact the clinic at the place of residence. You must have a card with records of previous vaccinations with you. An unpleasant disease is measles. The photos clearly demonstrate this. The patient's body itches and itches.
Rubella, chickenpox, and measles are infectious diseases most common in children.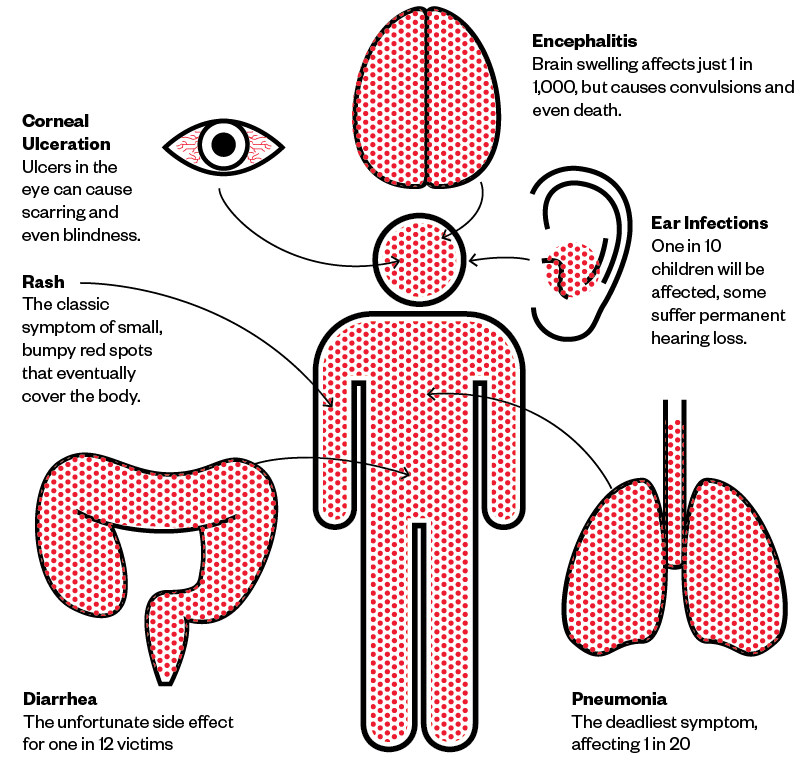 However, an adult can also get sick with them. Measles is much more difficult to tolerate in this case. Photos of infected adults are not much different from images of the manifestation of the disease in children, but the child's well-being is an order of magnitude better during the entire period of the disease.
However, an adult can also get sick with them. Measles is much more difficult to tolerate in this case. Photos of infected adults are not much different from images of the manifestation of the disease in children, but the child's well-being is an order of magnitude better during the entire period of the disease.
Quarantine
It is very important to isolate the patient from healthy people, especially children. But as we know, infected patients are admitted to the hospital only in special cases, so it is necessary to allocate a separate room at home. If this is not possible, then healthy children should be taken to relatives for a while. In the room where the patient is located, wet cleaning and ventilation must be done. All windows must be covered with thick curtains so that the room is twilight. It is very important to allocate separate cutlery to a sick family member: plates, mugs, spoons. It is important to wear a gauze bandage, both for the sick and those who care for him.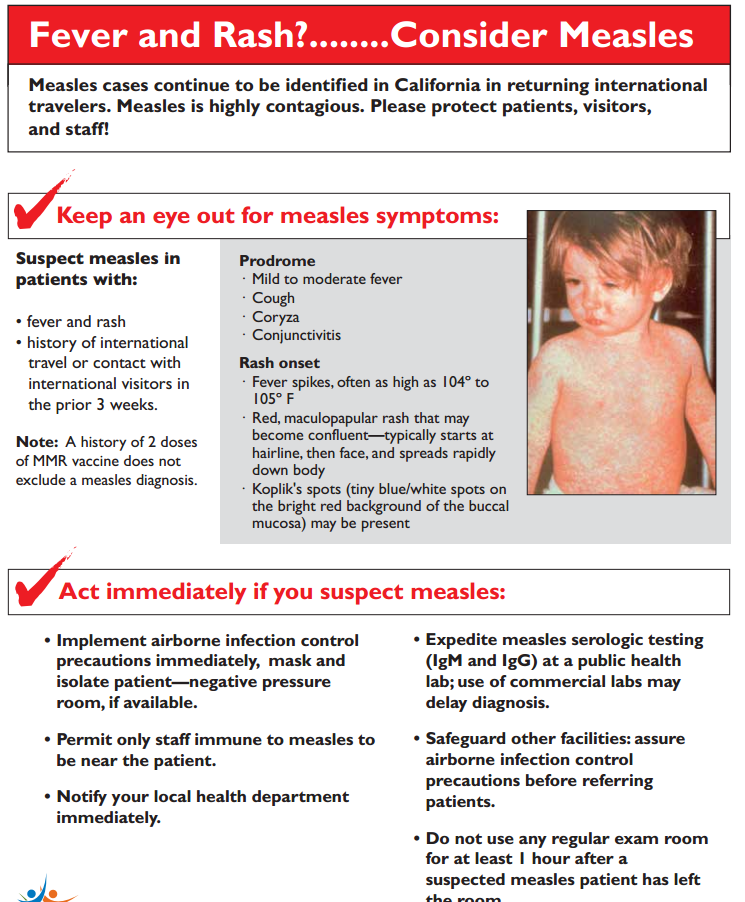 An adult who has been vaccinated or has been ill with measles should care for a sick child. Be sure to remember that childhood measles is highly contagious.
An adult who has been vaccinated or has been ill with measles should care for a sick child. Be sure to remember that childhood measles is highly contagious.
Measles during pregnancy
What if a pregnant woman gets measles? How dangerous is the disease for the baby and the expectant mother? Any viral diseases (measles, chickenpox or rubella) are extremely dangerous during pregnancy. As for measles, if a woman becomes infected with the virus at an early stage of pregnancy, then this is fraught with a variety of malformations in the development of the fetus. And despite all the modern diagnostic methods, doctors have no way to establish how much the disease managed to affect the brain of a child. It can only be revealed after birth. If a pregnant woman becomes ill with measles at a later date, the probability of infecting the child is very high. And it means only that the child will be born with a virus. This is fraught with the fact that a child's, still fragile body, most likely, will not be able to endure the disease.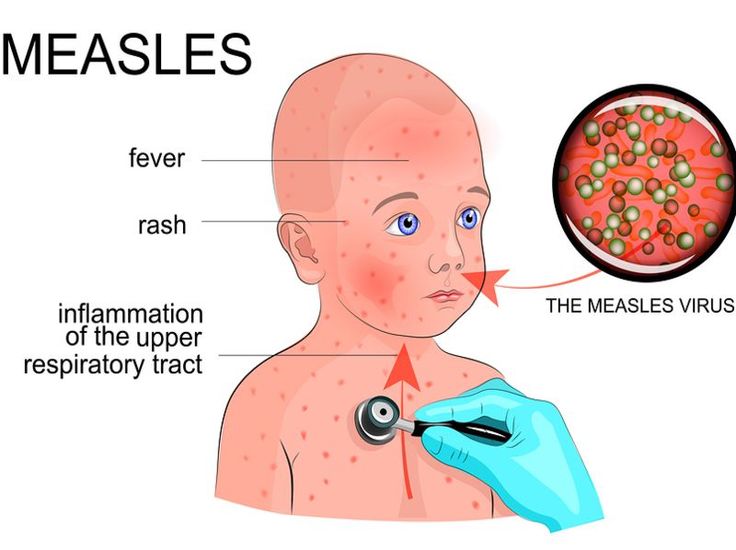 Despite all the danger, measles is not an indication for abortion, for example, as is the case with rubella. But still, if a woman falls ill with measles at an early date, the doctor must warn the expectant mother about possible irreversible consequences. But the choice always remains with the woman. Naturally, any future mother does not want her child to have any diseases. Therefore, during pregnancy, a woman should not only eat right and take all the necessary vitamins, but also carefully monitor her health.
Despite all the danger, measles is not an indication for abortion, for example, as is the case with rubella. But still, if a woman falls ill with measles at an early date, the doctor must warn the expectant mother about possible irreversible consequences. But the choice always remains with the woman. Naturally, any future mother does not want her child to have any diseases. Therefore, during pregnancy, a woman should not only eat right and take all the necessary vitamins, but also carefully monitor her health.
Summary of the above
Measles what kind of disease? This is a dangerous disease that spreads by airborne droplets, has an acute course. The disease is quite ancient, however, there is no cure for measles. Only the symptoms of the disease are treated. Fortunately, the signs of children's diseases (measles) are pronounced, it will not be possible to miss them.
Children of preschool and primary school age most often suffer from measles, but this does not mean that adults are protected from infection.