Pregnancy at 23 weeks movements
23 Weeks Pregnant: Symptoms and Baby Development
23 Weeks Pregnant: Your Baby's Development
You might be surprised to know that your baby can hear your voice, thanks to recent ear development. Give her a daily treat by reading, talking, or singing to her. Your partner can also do the same!
When you’re 23 weeks pregnant your baby is probably getting plenty of shut-eye. Most of her snooze time — about 80 percent of it, actually — will be spent in what’s called rapid eye movement sleep, or REM sleep. During REM sleep your baby’s eyes move and her brain is very active.
You might not have given too much thought to the fluid that surrounds your baby in the amniotic sac, but it actually plays a very important role: It creates the perfect environment for your baby to grow into a healthy newborn. The fluid helps keeps her warm, and cushions her as she grows.
Experts recommend drinking lots of water during pregnancy not only to benefit your overall health but also because the water you drink actually helps form the amniotic fluid.
If you’re 23 weeks pregnant with twins, take a look at our twin pregnancy week-by-week guide to find out more about what your babies are up to!
The Size of the Fetus at 23 Weeks Pregnant
At 23 weeks, your fetus is about the size of an eggplant.
To get an understanding of how your little one is developing inside your uterus, check out the illustration below:
Mom's Body at 23 Weeks Pregnant
By the time you’re 23 weeks pregnant, you may have gained about 10 to 15 pounds of weight. It’s always a good idea to check in with your healthcare provider periodically to make sure that your pregnancy weight gain is healthy.
You can also read up on pregnancy weight gain facts and advice.
If your provider determines that you're gaining too much weight or not enough weight, he or she can offer advice to help you stay on track. For example, if you’re gaining too much, your provider may recommend adjusting your diet and exercising more.
Gaining a healthy amount of weight during pregnancy will make it easier to slowly lose those extra pounds after you’ve given birth. For additional help, try using our Pregnancy Weight Gain Calculator.
At 23 weeks pregnant, you can probably feel your baby’s movement, although some moms-to-be may need to wait a little while longer.
At some point in the next few months, your healthcare provider may ask you to monitor your baby’s movements by doing a set of “kick counts” each day. To do this, you would choose a time of day when your baby is usually active, and keep track of how long it takes to count 10 movements that your baby makes.
Give your provider a call if it takes more than 2 hours to feel these 10 movements, or if you detect any overall changes in your baby’s movement. You may find this downloadable fetal movement tracker helps you do the tracking.
If you are wondering how many months pregnant you are at 23 weeks, here's your answer: you are about six months pregnant! Just one more month and you’ll be in the home stretch, the third trimester. You’ve got this!
You’ve got this!
23 Weeks Pregnant: Your Symptoms
At 23 weeks pregnant, here are some of the symptoms you may be experiencing:
Aches and pains. As your belly grows and you gain weight, it’s normal to feel some aches and pains, both as you move around and when you try to rest. At around 23 weeks pregnant, you might have sore muscles or have a mild headache from time to time. To help relieve muscle aches and pains, try things like taking a warm bath, massaging the affected area, or applying a heating pad to the sore spot. For headaches, lie down and apply a cool pack to your head. For severe pains, and for headaches that don't go away, always contact your healthcare provider. You should also check with your provider before taking any over-the-counter pain relief medications, even for ones you used to take before you were pregnant.
Leg cramps. You might be experiencing this symptom if you’re 23 weeks pregnant, because it’s quite common in the second and third trimesters.
 What you can try is to massage your calves in long downward strokes, and to flex your foot up and down — this stretch might help resolve the cramp right away.
What you can try is to massage your calves in long downward strokes, and to flex your foot up and down — this stretch might help resolve the cramp right away.
23 Weeks Pregnant: Things to Consider
Take a look at how much salt is in your diet, and make sure you’re eating salty foods in moderation. Experts recommend consuming no more than one teaspoon of salt per day, so avoid high-sodium foods like processed meats and canned soups.
It’s important to do what you can to avoid food poisoning, and to recognize the signs of it early, as getting this kind of illness can be dangerous for your baby. The signs of food poisoning typically include vomiting, diarrhea, fever, chills, aches, and abdominal cramps. If you think you have food poisoning, contact your healthcare provider right away for treatment. Of course, your best strategy is to avoid getting food poisoning; here are some tips on how to do this: o Don’t eat raw or undercooked seafood and eggs o Wash raw fruits and vegetables before eating them o Wash your hands well with hot, soapy water, particularly after preparing a meal o Wash kitchen surfaces after cooking o Unless they are cooked until steaming hot, avoid cold cuts, deli meats, and smoked or pickled fish o Read up on what you should not eat while pregnant.
 This article doesn’t just explore food poisoning risks, but gives you lots of other great advice too.
This article doesn’t just explore food poisoning risks, but gives you lots of other great advice too. If your blood pressure is too high, your doctor may keep an eye out for preeclampsia, a complication of pregnancy characterized by high blood pressure, edema (swelling), and protein in the urine. Though this condition is more common in the third trimester, it can occur any time after 20 weeks, and catching it early is crucial. Your healthcare provider will be able to diagnose preeclampsia by checking your blood pressure and by testing your urine for protein levels. If you notice any of the symptoms of preeclampsia, including vision problems such as seeing spots, a persistent headache, sudden swelling in your feet and hands, feeling nauseous, sudden weight gain, or having trouble breathing, call your healthcare provider immediately. If left untreated, preeclampsia can cause decreased blood flow to your placenta, and can affect your kidney, liver, brain, and eyes.
Get to know the signs of preterm labor, just in case! Preterm labor is when labor starts before the end of the 37th week of pregnancy.
 If your healthcare provider recognizes soon enough that you’ve gone into labor, he or she may be able to postpone the birth, giving your baby precious extra time in the womb to grow and develop. That’s why you should keep an eye out for the signs of labor and tell your provider right away if you think you’re experiencing them. Signs include a constant lower backache; vaginal discharge that is watery, mucus-like, or bloody; pressure in your pelvis; abdominal cramps; diarrhea; regular contractions; and your water breaking.
If your healthcare provider recognizes soon enough that you’ve gone into labor, he or she may be able to postpone the birth, giving your baby precious extra time in the womb to grow and develop. That’s why you should keep an eye out for the signs of labor and tell your provider right away if you think you’re experiencing them. Signs include a constant lower backache; vaginal discharge that is watery, mucus-like, or bloody; pressure in your pelvis; abdominal cramps; diarrhea; regular contractions; and your water breaking. Do you have older children? If yes, now could be a good time to start preparing them for the arrival of their baby brother or sister. They may have lots of questions about where babies come from, so be prepared for unexpected reactions! With younger children, it may be best to tell them that you’re expecting when they ask questions about your changing body. If you’re feeling unsure about the best way to navigate this area or broach the topic, ask your healthcare provider for advice.
Would you consider giving your child a name based on a specific theme? Perhaps something fit for a prince or princess? Or a name inspired by your favorite flower? Or perhaps a name that sound strong and powerful, inspired by mythology? Check out these lists of baby names, curated by theme: o Floral names o Royal names o Mythological names o Biblical names
23 Weeks Pregnant: Ask Your Doctor
Does loud noise affect your baby’s hearing development?
How can you tell if you’re doing Kegels correctly?
What are the benefits of reading or playing music to your baby?
What is the heaviest amount you can safely pick up at this point in your pregnancy? What is the safest way to lift an object?
23 Weeks Pregnant: Your Checklist
You’ll love looking back on this time, so create lasting memories by organizing a maternity photoshoot while you still have the energy.
 You could hire a professional photographer, or ask a friend who you know takes lovely pictures. You could create a love-heart shape with your hands and place them over your bump, or place mini mittens over your belly. You could do the photoshoot in a beautiful outdoors spot, or in the nursery, if it’s ready. Plus, you could have some individual shots, and then have some shots with your partner or loved ones. For some extra inspiration, take our quiz to discover your maternity photoshoot style.
You could hire a professional photographer, or ask a friend who you know takes lovely pictures. You could create a love-heart shape with your hands and place them over your bump, or place mini mittens over your belly. You could do the photoshoot in a beautiful outdoors spot, or in the nursery, if it’s ready. Plus, you could have some individual shots, and then have some shots with your partner or loved ones. For some extra inspiration, take our quiz to discover your maternity photoshoot style.If you have time this week, read this article on pregnancy warning signs you should not ignore. It's always wise to prepared and to know what to look out for.
Wondering how prepared you are for your baby’s arrival? Take this baby arrival quiz to find out! No matter the result – don’t worry – you still have time to get everything as prepared as it needs to be.
Have a little extra energy and feel like doing something creative? Why not download these pregnancy milestone cards, and get creative with documenting each month of pregnancy.
 For example, you could create your baby’s first photo album and add photos of your growing belly alongside a printout of these milestone cards. This is a lovely memento that you can then share with your baby in the years to come. You can also print these cards and use them to share your pregnancy journey with your loved ones on social media.
For example, you could create your baby’s first photo album and add photos of your growing belly alongside a printout of these milestone cards. This is a lovely memento that you can then share with your baby in the years to come. You can also print these cards and use them to share your pregnancy journey with your loved ones on social media.Sign up for even more weekly pregnancy tips.
How will my baby's movements feel, week by week?
In this article
- 16 weeks to 19 weeks
- 20 weeks to 23 weeks
- 24 weeks to 28 weeks
- 29 weeks to 31 weeks
- 32 weeks to 35 weeks
- 36 weeks to 40 weeks
Every pregnancy is different, so it’s hard to say exactly what you’ll feel and when. If this is your first baby, you may not be able to feel much until after 20 weeks of pregnancy. However, some women can feel flutterings from as early as 16 weeks, especially if this is their second pregnancy. Here’s an idea of what to expect from your baby’s movements during your second trimester and third trimester.
Here’s an idea of what to expect from your baby’s movements during your second trimester and third trimester.
16 weeks to 19 weeks
You’ll probably experience some faint and fluttery feelings (quickening) in your tummy at around 18 weeks. They may feel like gentle puffs or bubbles of air being released, or you may notice a soft swirling or rolling sensation in your belly. If this is your first pregnancy, it may take a bit longer before you realise that those gentle little jolts and knocks are actually your baby moving about!
Not everyone enjoys those first little flutters, however. Some women find them unpleasant at first, but they quickly get used to the sensations.
20 weeks to 23 weeks
You may notice gentle kicks, or repetitive jerking movements when your baby gets hiccups now. As the weeks go by, your baby's activity will gradually increase and become stronger.
You may find that your baby becomes more lively as the day goes on, kicking, squirming and somersaulting the most in the evening as you relax. Another top time for movements is just before or at mealtimes. As your pregnancy progresses, you'll come to recognise your baby's pattern of activity.
24 weeks to 28 weeks
At this point in your pregnancy your baby still has plenty of space to move around freely. You’re likely to notice frequent movements and feel that your baby is very active. Limb movements may feel punchy, while whole-body movements may be smoother. You may even notice your little one jumping at loud, sudden noises!
29 weeks to 31 weeks
Your baby is likely to be making sharper, more definite movements now, such as strong kicks and pushes. Over the coming weeks, you may feel as if they’re fighting for space, as they run out of wriggle room in your womb (uterus). It may even be possible to see ripples of movement across your belly as your baby turns.
It may even be possible to see ripples of movement across your belly as your baby turns.
32 weeks to 35 weeks
This may be the most exciting time for feeling your baby move, as at 32 weeks your baby's movements will be at their peak. Afterwards, the frequency of your baby's movements will stay roughly the same until you go into labour. As your baby grows and has less room to move, you may notice that the type of movement you feel changes. But you should still feel them moving as often as before. Your baby’s movements may start to feel more sustained or slower due to lack of space but they should still feel hard, strong and powerful in the weeks leading up to the birth.
You should still be able to feel your baby wriggling around in there, though! If their thumb pops out of their mouth, you may feel their head darting from side to side as they try to find it again. You may also notice that your baby develops a regular time of the day when they’re most active.
36 weeks to 40 weeks
If this is your first baby, they will probably take up their final head-down position at around 36 weeks, if they haven't already. The firm muscles of your womb and tummy will help to keep them in place. It may feel as if there's a melon pressing on your pelvic floor!
Is my baby head-down?
Nearing your due date? Learn how to tell if your baby's in the optimum head-down position. More pregnancy videos
If you've had a baby before, your tummy muscles are likely to be weaker, so your baby may keep changing their position right up to your due date.
As you approach your due date, your baby will be getting larger, and won't be rolling over as often. Instead, you may notice strong but less frequent kicks underneath your ribs on one side or the other, and more squirming movements. Their movements may feel slower, but also harder and stronger. Jabs and kicks from those little arms and legs may feel sharp, uncomfortable and even painful. You may even spot a tiny, fleeting handprint or footprint on the surface of your bump.
You may even spot a tiny, fleeting handprint or footprint on the surface of your bump.
It's normal to notice a change in the types of movement you feel in late pregnancy. But you should still be feeling your baby move as often as before, right up until, and even during labour itself.
Rather than counting your baby’s kicks, it’s better to pay attention to your baby’s pattern of movements so that you know what’s normal. If you’ve noticed that your baby is moving less than usual, or you are at all worried about your baby, call your midwife straight away, even if it’s the middle of the night. They can listen to your baby's heartbeat to check that all is well.
In the meantime, there will be times when your baby is sleeping, and times when they’re awake and active. They may liven up in the evenings or when you're lying in bed trying to get to sleep. Find out more about your baby’s movements in pregnancy.
More on baby movements:
- Can I predict my baby's sleeping routine from their movement in the womb?
- Does it take longer to feel my baby kicking if I’m overweight?
- Can my baby’s movements predict if I’m having a boy or a girl?
References
Bradford B, Maude R. 2014. Fetal response to maternal hunger and satiation - novel finding from a qualitative descriptive study of maternal perception of fetal movements. BMC Pregnancy Childbirth 14:288. www.biomedcentral.com [Accessed May 2021]
2014. Fetal response to maternal hunger and satiation - novel finding from a qualitative descriptive study of maternal perception of fetal movements. BMC Pregnancy Childbirth 14:288. www.biomedcentral.com [Accessed May 2021]
CDC. 2019. Reproductive health and the workplace. Centers for Disease Control and Prevention. www.cdc.gov [Accessed May 2021]
Fretts, RC. 2020. Decreased fetal movement: Diagnosis, evaluation, and management. UpToDate. www.uptodate.com [Accessed May 2021]
Jakes AD, Whybrow R, Spencer C, et al. 2018. Reduced fetal movements. BMJ. 360:k570. www.bmj.com [Accessed May 2021]
Kicks Count. nd. Your baby’s movements. Kicks Count. www.kickscount.org.uk [Accessed May 2021]
Nawadike, VR. 2020. Have Your Baby’s Movements Changed? Here’s When to Worry. Healthline. www.healthline.com [Accessed May 2021]
NHS. 2018. Your baby’s movements. NHS. www.nhs.uk [Accessed May 2021]
Raynes-Greenow CH, Gordon A, Li Q, et al.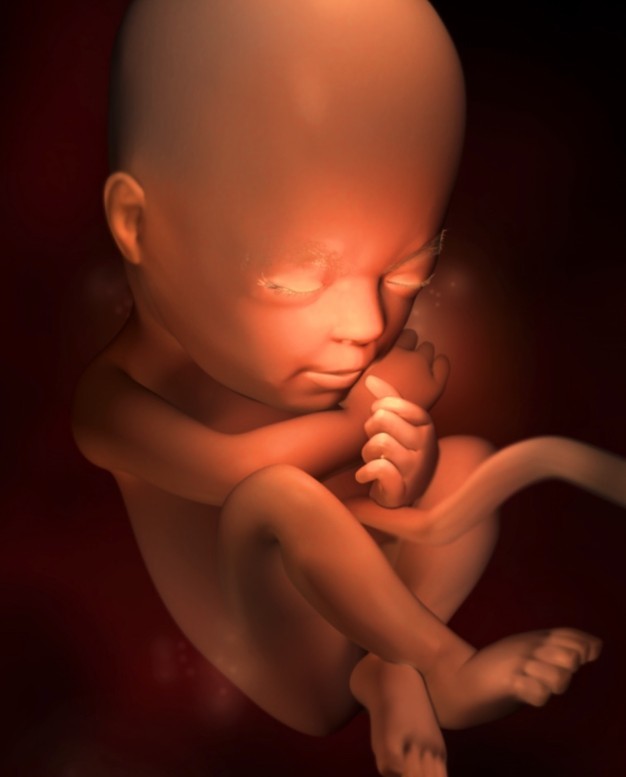 2013. A cross-sectional study of maternal perception of fetal movements and antenatal advice in a general pregnant population, using a qualitative framework. BMC Pregnancy Childbirth 13:32. www.biomedcentral.com [Accessed May 2021]
2013. A cross-sectional study of maternal perception of fetal movements and antenatal advice in a general pregnant population, using a qualitative framework. BMC Pregnancy Childbirth 13:32. www.biomedcentral.com [Accessed May 2021]
RCOG. 2011. Reduced fetal movements. Royal College of Obstetricians and Gynaecologists, Green-top guideline, 57. London: RCOG press. www.rcog.org.uk [Accessed May 2021]
RCOG. 2012. Information for you: your baby's movements in pregnancy. Royal College of Obstetricians and Gynaecologists. www.rcog.org.uk [Accessed May 2021]
Smith, V, Muldoon, K, et al. 2021. Assessing fetal movements in pregnancy: A qualitative evidence synthesis of women’s views, perspectives and experiences. BMC Pregnancy Childbirth 21: 197. www.biomedcentral.com [Accessed May 2021]
Show references Hide references
how the fetus develops, feeling of stirring in the abdomen, the size and weight of the child is normal, ultrasound
Published: 06/02/2017
Reading time: 5 min.
Number of reads: 23286
The twenty-third fetal week is the twenty-fifth obstetric and the end of the sixth month of pregnancy. The embryonic period is calculated from the expected date of conception. There are still fifteen weeks ahead, but most of the pregnancy is over. Toxicosis no longer torments, the stomach has not yet grown very much to interfere with movement, so mommy can safely enjoy her position.
Feelings
So, what does a woman feel during this period? Of course, a lot depends on the size of the tummy. The baby is constantly growing, and it becomes harder for mommy to walk. Often a pregnant woman is worried about back pain caused by excessive muscle tension. In this case, doctors recommend wearing a bandage that will support the stomach and reduce the load on the spine. Also, loads can provoke varicose veins (if the woman's body is prone to it). Then you need to wear tight stockings. They help reduce the risk of thrombosis. Mommy may also feel a slight discomfort in the lower abdomen, which is caused by stretching of the muscles of the uterus. Such feelings are considered normal. But if the pain is palpable and cramping in nature, you should immediately call an ambulance. A decrease in metabolism can provoke fluid retention in the body and, as a result, swelling of the legs and arms. Some mothers complain of heartburn, because the baby puts pressure on the digestive organs. How to deal with it, each woman chooses for herself individually.
Such feelings are considered normal. But if the pain is palpable and cramping in nature, you should immediately call an ambulance. A decrease in metabolism can provoke fluid retention in the body and, as a result, swelling of the legs and arms. Some mothers complain of heartburn, because the baby puts pressure on the digestive organs. How to deal with it, each woman chooses for herself individually.
What happens to the fetus
By the 23rd week, the baby weighs about 700 g and is about 20–35 cm tall. It is about the size of a spaghetti squash. The baby in the womb looks like a real little man. From that moment on, his appearance will hardly change. On ultrasound, you can already see, with a successful location of the crumbs, who he looks like.
So, what is important happens to the baby at the 23rd week of intrauterine life?
• The child's face is fully formed. All features are in place.
• The baby is rounded. The 23rd week is the period when the development of the fetus is not in its growth, but in weight gain and the accumulation of subcutaneous fat.
• The formation of the bone marrow is completed. Now it is in it that hematopoiesis occurs.
• The bone tissue of the baby is actively formed. At this time, it is very important that the mother consumes enough foods rich in calcium.
• The lungs produce surfactant, which helps the baby's lungs expand and breathe on their own after birth.
• The sexual organs are finally formed. In girls, a vagina appears; in boys, the testicles descend into the scrotum.
• The baby develops taste preferences. He already distinguishes what mom eats, what he likes and what not.
• The baby is sensitive to mommy's mood swings. Therefore, during this period, you need to carefully monitor your well-being, avoid unrest and try to maintain a positive attitude.
Changes in mother's body
Stomach. By the 23rd week of pregnancy, the tummy rises and rounds. Many mothers notice that it is growing rapidly. On average, the stomach adds 1 cm per week. Due to active growth, digestive problems are possible. If you have any problems with this, you should consult your doctor. The skin is stretched, which can cause it to itch. During this period, stretch marks often appear, which are quite difficult to deal with after childbirth. Therefore, it is preferable to try to prevent their occurrence. Today, in pharmacies and specialized stores, you can find creams that allow you to make the skin more elastic and prevent the occurrence of stretch marks.
If you have any problems with this, you should consult your doctor. The skin is stretched, which can cause it to itch. During this period, stretch marks often appear, which are quite difficult to deal with after childbirth. Therefore, it is preferable to try to prevent their occurrence. Today, in pharmacies and specialized stores, you can find creams that allow you to make the skin more elastic and prevent the occurrence of stretch marks.
Uterus. Most of the sensations that a woman experiences in the 23rd week are due to the active growth of the uterus. By this time, it reaches the size of a soccer ball. Its bottom is located at a height of 25–27 cm from the pubis. The indicator is important, and the gynecologist measures it at each visit by the mother of the antenatal clinic. If the indicators diverge from the norm, the doctor begins to look for the cause of the violation. These causes include polyhydramnios or placental insufficiency. At the same time, some women may experience false contractions. They are not too painful and irregular. However, if the contractions are accompanied by pain, they occur at regular intervals, and the stomach hardens, you must immediately call an ambulance and go to the hospital. This state of the body may indicate the onset of premature birth.
Weight. On average, by the 23rd week, a woman adds about 8–9 kg. The value is considered optimal, but deviations from it are allowed. This is primarily due to the constitution of the woman and the course of pregnancy in the first trimester. So, a small weight gain is typical for thin girls. If the body is prone to fullness, then the increase will be more than the average value. Weight should be kept under control. It is recommended to make it a habit to weigh yourself on an empty stomach in the morning.
Allocations. Women regularly experience discharge during pregnancy. How to determine if they are safe for the health of the fetus or should you see a doctor? So, if the discharge is brown, brown or rusty with streaks of blood, then you should immediately go to the gynecologist. A grey, green, or yellowish secretion with an unpleasant odor indicates an infection in the vagina. In such cases, swabs are taken for pathogenic flora. Curdled discharge is characteristic of thrush, which is treated in a few days with the help of special suppositories that are safe for a pregnant woman. However, in no case should you go to the pharmacy and independently purchase funds for thrush. Not all of them are allowed and safe for the child. Before starting treatment, you should consult with a specialist. Watery discharge usually indicates amniotic fluid leakage. And in this case, you should also consult a doctor.
A grey, green, or yellowish secretion with an unpleasant odor indicates an infection in the vagina. In such cases, swabs are taken for pathogenic flora. Curdled discharge is characteristic of thrush, which is treated in a few days with the help of special suppositories that are safe for a pregnant woman. However, in no case should you go to the pharmacy and independently purchase funds for thrush. Not all of them are allowed and safe for the child. Before starting treatment, you should consult with a specialist. Watery discharge usually indicates amniotic fluid leakage. And in this case, you should also consult a doctor.
Pain. Under the weight of the tummy, mommy may begin to have pain in the lower back and spine. The pressure of the uterus can cause aches in the pelvic region. The constant stress also affects the legs. The muscles in them also begin to hurt. Doctors recommend in such cases to rest as much as possible, wear exceptionally comfortable flat shoes, try to sit on soft surfaces and always with a back that you can lean on. Relief can bring special gymnastics for pregnant women.
Relief can bring special gymnastics for pregnant women.
Movements
At the 23rd week, the gynecologist already offers the woman to monitor the number of movements of the baby and note them in a special journal. Mom needs to fix the tremors of the crumbs for a certain period of time. Normally, the baby should move 4 times per hour or 10-15 times per day. The lack of movement of the crumbs for 12 hours is not considered a cause for concern, since the child can simply sleep. However, if a mother does not hear her baby for more than 12 hours or even more than a day, you should immediately consult a doctor.
Examinations and tests
Ultrasound
At the 23rd week of pregnancy, ultrasound is rarely prescribed: a routine examination of a woman takes place three weeks earlier. However, if any abnormalities are suspected, an ultrasound examination is ordered. On ultrasound, they look at the size of the child, measure the heartbeat. The uzist also notes the condition of the uterus, the thickness of its walls, the amount of amniotic fluid. All these data allow us to judge the state of health of the baby and the normal course of pregnancy.
All these data allow us to judge the state of health of the baby and the normal course of pregnancy.
Tests
At a scheduled examination in the antenatal clinic, the gynecologist prescribes an OAM and a UAC. The results of these tests show whether everything is fine in the mother's body, whether there are any inflammatory processes, anemia and other abnormalities. If necessary, if there are doubts about absolute health, the doctor may prescribe additional examinations (blood for sugar, smear for flora pathology, etc.).
Intimacy
At 23 weeks, sex is considered safe for the baby. Moreover, doctors even recommend doing it. Regular intimate life promotes relaxation, stress relief, which has a beneficial effect on the mood of a woman. It is important to choose comfortable positions, because the stomach is already reaching a large size, and pressure on it is prohibited.
Recommendations for expectant mothers
Sleep. On the 23rd week, a lot of time should be devoted to sleep.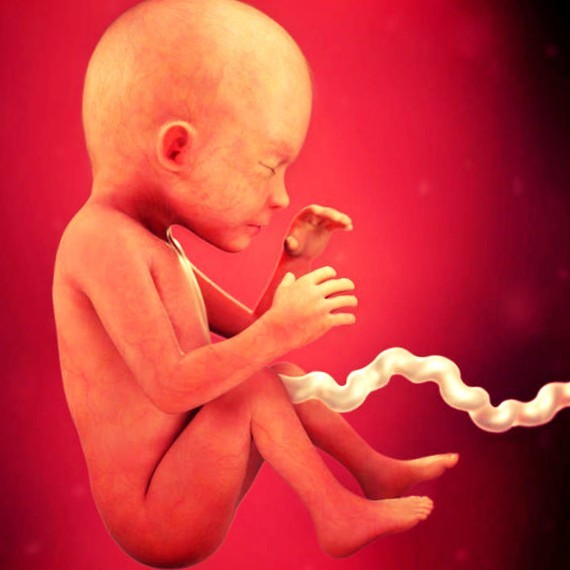 Fatigue in mothers increases, constant drowsiness appears. If a woman sleeps little, then she becomes irritated, her mood begins to deteriorate, which can adversely affect the child's nervous system. If you are concerned about lack of sleep, then it is recommended to adjust the regimen and devote more time to sleep.
Fatigue in mothers increases, constant drowsiness appears. If a woman sleeps little, then she becomes irritated, her mood begins to deteriorate, which can adversely affect the child's nervous system. If you are concerned about lack of sleep, then it is recommended to adjust the regimen and devote more time to sleep.
Nutrition. The baby is actively growing, so the daily diet must be approached carefully and responsibly. Proper nutrition is one of the keys to the well-being of the mother and the healthy development of the baby. The menu at the 23rd week of pregnancy is no different from what the woman had in previous months. The diet should include sour-milk and dairy products, cereals, fruits, herbs, vegetables, fish, seafood. It is not recommended to eat a lot of salt, as it retains water in the body, which ultimately leads to edema. Also, do not eat anything that can cause allergies (honey, chocolate, citrus fruits, etc.). Eat foods high in calcium and iron.
Vitamins.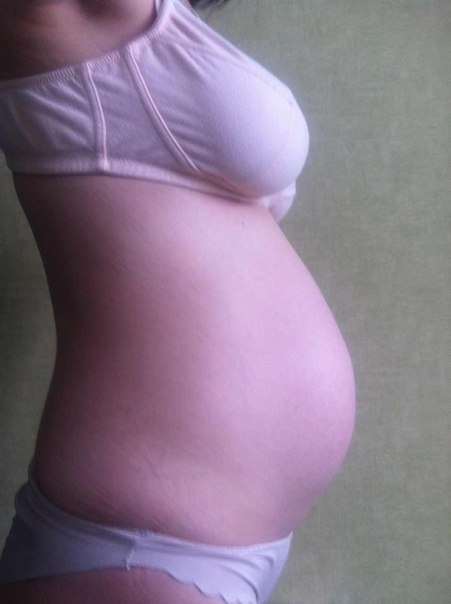 During this period, doctors often prescribe vitamins for mothers. The baby needs more and more nutrients and trace elements, and a woman does not always receive them in the proper amount from food. Vitamins help to provide the child with everything necessary and actively grow.
During this period, doctors often prescribe vitamins for mothers. The baby needs more and more nutrients and trace elements, and a woman does not always receive them in the proper amount from food. Vitamins help to provide the child with everything necessary and actively grow.
Health. The female body during pregnancy is weakened, so you need to be careful about your health. At the slightest hint of a disease, you should consult a doctor and in no case self-medicate. It is recommended to walk a lot and do special exercises for pregnant women.
Mood. Since the baby shares your mood, try not to worry, not to allow negative emotions. Pregnancy is a wonderful time, enjoy it and share your happiness with your baby.
Rate article
(Number of votes: 9, average 4.3)
Go back
Fetal movement - how and when does it occur
- At what time does fetal movement begin
- Fetal movement rate
- Methods for assessing the "sufficiency" of fetal movements
- Changes in fetal activity
- Determining the condition of the fetus
“Dear patients, we are glad to welcome you to the website of the Fetal Medicine Center – a medical center of expert level in the field of modern prenatal medicine.
We see our mission in making the expectation of a child and its birth a happy, calm and most comfortable period for every woman. By providing professional medical support, we help couples plan pregnancy, control its harmonious course, conduct expert-level prenatal diagnostics, providing comprehensive care for the health of the expectant mother and baby.”
Roza Saidovna Bataeva
Head of the Fetal Medicine Center in Moscow
From the very beginning of pregnancy, every expectant mother begins to listen anxiously to the sensations inside the growing tummy. Can't wait to feel your baby move. When does the fetus begin to move? At what time can a pregnant woman begin to listen carefully to herself, waiting for the first movements of her child? Should I be worried if they are not felt or the baby suddenly calmed down? And can movements carry any other information, besides communicating with mom?
At what time does the fetal movement begin
The first movements of the future baby begin early - already at 7-8 weeks of pregnancy . It was at this time that the first muscles and the rudiments of the nervous system of the fetus are formed. Naturally, at this time, the movements of the embryo are still very primitive - these are muscle contractions in response to nerve impulses.
It was at this time that the first muscles and the rudiments of the nervous system of the fetus are formed. Naturally, at this time, the movements of the embryo are still very primitive - these are muscle contractions in response to nerve impulses.
Approximately from 10 weeks of pregnancy the fetus begins to move more actively in the uterus, and, encountering an obstacle on its way (walls of the uterus), change the trajectory of movements. However, the baby is still very small and the impacts on the uterine wall are very weak, the expectant mother cannot yet feel them. At 11-12 weeks of intrauterine life, a little man already knows how to clench his fists, grimace, frown, by 16 weeks of pregnancy he begins to react to loud, sharp sounds with increased motor activity, at 17 weeks the first facial expressions appear, and at 18 weeks he covers his face with his hands and plays with the umbilical cord, clenching and unclenching the fingers.
Gradually, with increasing gestational age, movements become more coordinated and more like conscious. When the baby grows up, the pregnant woman begins to feel his movements.
When the baby grows up, the pregnant woman begins to feel his movements.
When does the fetal movement begin during the first and subsequent pregnancies
It is generally accepted that during the first pregnancy, the expectant mother feels the first fetal movements at 20 weeks of pregnancy, with repeated pregnancies - at 18 weeks. This is not entirely true. A mother who is expecting her first child, indeed, most often begins to feel the movements of the fetus a little later than a multiparous woman. This is due to the fact that "experienced" mothers know how the movements of the crumbs are felt at first and what they should feel. Some primigravidas perceive the first movements of the fetus as an increase in intestinal peristalsis, “gaziki”. Many women describe the first movements of the fetus as a feeling of fluid transfusion in the abdomen, "fluttering butterflies" or "swimming fish."
The first movements are usually rare and irregular. The time of the first sensations of fetal movements naturally depends on the individual sensitivity of the woman. Some future mothers feel the first movements as early as 15-16 weeks, and someone only after 20. Slender women, as a rule, begin to feel movements earlier than full ones. Women who lead an active lifestyle, work hard, usually feel the movements of the fetus later.
Some future mothers feel the first movements as early as 15-16 weeks, and someone only after 20. Slender women, as a rule, begin to feel movements earlier than full ones. Women who lead an active lifestyle, work hard, usually feel the movements of the fetus later.
By 20 weeks, due to the formation of the spinal cord and brain, as well as the accumulation of a certain amount of muscle mass in the fetus, movements become more regular and noticeable .
From 24 weeks of pregnancy, the movements of the fetus are already reminiscent of the movements of a newborn - the expectant mother feels how the fetus changes position, moves its arms and legs. The motor activity of the fetus increases gradually and its peak falls on the period from the 24th to the 32nd week of pregnancy. At this time, the activity of the baby's movements becomes one of the indicators of its normal development. After 24 weeks, the child begins to "communicate" with the mother with the help of movements, respond to the sounds of voice, music, and the emotional state of the mother. With an increase in the gestational age of more than 32 weeks, the motor activity of the fetus gradually decreases due to the fact that the baby is growing up and he simply does not have enough space for active movements. This becomes especially noticeable at the time of childbirth. By the end of the third trimester of pregnancy, the number of fetal movements may decrease somewhat, but their intensity and strength remain the same or increase.
With an increase in the gestational age of more than 32 weeks, the motor activity of the fetus gradually decreases due to the fact that the baby is growing up and he simply does not have enough space for active movements. This becomes especially noticeable at the time of childbirth. By the end of the third trimester of pregnancy, the number of fetal movements may decrease somewhat, but their intensity and strength remain the same or increase.
Fetal movement rate
The baby in the mother's belly moves almost constantly. At the 20th week of pregnancy, the fetus makes about 200 movements per day, and between the 28th and 32nd weeks, the number of movements reaches 600 per day. Naturally, a pregnant woman does not feel all the movements of the fetus, but only a small part of them. So, after 28 weeks, the frequency of fetal movement, according to the sensations of a woman, is usually 4 to 8 times per hour, with the exception of periods of fetal sleep (3-4 hours in a row).
In the third trimester, a pregnant woman may notice that her baby has regular sleep and wake cycles. Children are usually most active from 19:00 to 4:00 in the morning, and the period of "rest" occurs more often from 4 to 9:00 in the morning. Of course, the movements of the fetus depend on the mood of the mother, if the mother is worried or happy, the baby can move more actively, or vice versa, calm down. The fact is that when a mother rejoices, her body significantly increases the amount of hormones of joy - endorphins, which regulate the work of the heart and blood vessels, including the vessels of the placenta. During stress or pronounced negative emotions, biologically active substances are also produced - stress hormones, they also affect the work of the heart and blood vessels. It is thanks to this biological interaction between the organisms of mother and baby that the fetus feels the state of the mother. When the expectant mother is resting, the baby usually becomes more active, if the pregnant woman is active, busy with some kind of work, the child most often calms down. The movements also change depending on the satiety of the expectant mother.
Children are usually most active from 19:00 to 4:00 in the morning, and the period of "rest" occurs more often from 4 to 9:00 in the morning. Of course, the movements of the fetus depend on the mood of the mother, if the mother is worried or happy, the baby can move more actively, or vice versa, calm down. The fact is that when a mother rejoices, her body significantly increases the amount of hormones of joy - endorphins, which regulate the work of the heart and blood vessels, including the vessels of the placenta. During stress or pronounced negative emotions, biologically active substances are also produced - stress hormones, they also affect the work of the heart and blood vessels. It is thanks to this biological interaction between the organisms of mother and baby that the fetus feels the state of the mother. When the expectant mother is resting, the baby usually becomes more active, if the pregnant woman is active, busy with some kind of work, the child most often calms down. The movements also change depending on the satiety of the expectant mother. Usually the baby begins to move actively after the mother eats, especially something sweet. At the same time, the level of glucose in the blood increases sharply, which causes the fetus to be more active.
Usually the baby begins to move actively after the mother eats, especially something sweet. At the same time, the level of glucose in the blood increases sharply, which causes the fetus to be more active.
Fetal movements are the language in which the unborn child speaks to the mother. Naturally, a pregnant woman should listen to the movements, because in some cases, changes in the movements of the fetus may indicate a violation of its intrauterine state and a not entirely successful pregnancy.
If, after 20 weeks of pregnancy, the expectant mother does not feel the movement of the fetus, it may be worthwhile to see a doctor and make sure that everything is in order with the baby.
Methods for assessing the "sufficiency" of fetal movements
Counting the number of movements
The easiest way to assess fetal movements is to count the number of movements of the pregnant woman herself. Self-assessment methods are very easy to use, do not require additional equipment, the presence of a doctor and are easily reproducible by any woman. Their disadvantages are that each woman has different thresholds of susceptibility.
Their disadvantages are that each woman has different thresholds of susceptibility.
"Count to ten"
The most common method for assessing fetal movements is called "count to ten" . It can be performed after 28 weeks of pregnancy, when the fetus is mature enough to move actively. Its essence lies in the fact that the expectant mother counts the movements of the fetus for a 12-hour time interval, for example, from 9 am to 9 pm. The time when a pregnant woman catches the tenth movement is recorded on a tablet. If the fetus makes less than 10 movements in 12 hours, this is a reason to consult a doctor for an additional examination.
Sadowski method
In the evening after dinner (approximately between 19until 11 p.m.), the woman lies on her left side and counts the movements of the fetus. At the same time, everything is considered, even the smallest movements. If 10 or more movements are noted within an hour, this indicates that the baby is moving quite actively and feels good. If the fetus moved less than 10 times in an hour, then the movements are counted for the next hour. Evening time for this assessment method was not chosen by chance. It is in the evening hours, especially after dinner and the associated increase in glucose, that the greatest activity of the fetus is noted. If the number of fetal movements during this test is less than 10 per two hours, this should be considered as a sign of a violation of his condition and additional studies should be carried out.
If the fetus moved less than 10 times in an hour, then the movements are counted for the next hour. Evening time for this assessment method was not chosen by chance. It is in the evening hours, especially after dinner and the associated increase in glucose, that the greatest activity of the fetus is noted. If the number of fetal movements during this test is less than 10 per two hours, this should be considered as a sign of a violation of his condition and additional studies should be carried out.
For an obstetrician-gynecologist, fetal movements are also an important diagnostic criterion for some deviations in the course of pregnancy from the norm. Too active, violent, painful fetal movement or weak, rare movements may indicate its unfavorable condition.
Changes in fetal activity
Changes in fetal activity may be associated with external influences. For example, if a pregnant woman lies on her back for a long time, then the enlarged uterus compresses a large vessel - the inferior vena cava, the blood flow to the fetus is disrupted, which immediately causes its violent reaction - active movements. The same changes in the activity of the baby can occur in any other uncomfortable position of the mother - if she leans forward, squeezing her stomach, sits with her legs crossed, the child forces her mother to change her position with her activity. A similar situation occurs if the baby himself squeezes or presses the loops of the umbilical cord, limiting the flow of blood through it. He begins to move more actively, changes his position and relieves pressure on the umbilical cord. However, in some cases, an increase or vice versa, a subsidence of fetal movements can be a sign of a serious pathology.
The same changes in the activity of the baby can occur in any other uncomfortable position of the mother - if she leans forward, squeezing her stomach, sits with her legs crossed, the child forces her mother to change her position with her activity. A similar situation occurs if the baby himself squeezes or presses the loops of the umbilical cord, limiting the flow of blood through it. He begins to move more actively, changes his position and relieves pressure on the umbilical cord. However, in some cases, an increase or vice versa, a subsidence of fetal movements can be a sign of a serious pathology.
After 28 weeks of pregnancy, if your baby does not let you know for 3-4 hours, he may just be sleeping. In this case, the expectant mother needs to eat something sweet and lie down on her left side for half an hour. If these simple manipulations do not lead to a result, it is worth repeating them again after 2-3 hours. If this time the baby does not make itself felt, this is an occasion to consult a doctor. Rare and weak movements can also indicate a fetal problem, most often a lack of oxygen for the baby, that is, fetal hypoxia.
Rare and weak movements can also indicate a fetal problem, most often a lack of oxygen for the baby, that is, fetal hypoxia.
Determining the condition of the fetus
To determine the condition of the fetus, the doctor conducts a series of examinations:
Auscultation (listening)
The simplest is auscultation (listening) using a special wooden tube (obstetric stethoscope) or a special device that captures the heartbeat of the fetus, doctor listens to the baby's heartbeat. Normally, it is about 120-160 beats per minute. A decrease in heart rate less than 120 or an increase of more than 160 indicates intrauterine suffering of the child.
Ultrasound and dopplerometry
During ultrasound, the doctor visually assesses the size of the fetus, the correspondence of the development of the fetus to the gestational age, because with oxygen starvation, the growth rate of the fetus slows down and its size lags behind the norm for each period of pregnancy. Also important is the structure of the placenta, the presence of signs of aging in it, as a result of which the function of transferring blood, oxygen and nutrients to the fetus usually worsens. During ultrasound, the amount and type of amniotic fluid is assessed, which can also change with intrauterine fetal suffering. Dopplerometry of the vessels of the placenta and umbilical cord is a method for studying blood flow velocities in these vessels. With a decrease in the speed of blood flow in any vessel, one can speak of fetal malnutrition of varying severity.
Also important is the structure of the placenta, the presence of signs of aging in it, as a result of which the function of transferring blood, oxygen and nutrients to the fetus usually worsens. During ultrasound, the amount and type of amniotic fluid is assessed, which can also change with intrauterine fetal suffering. Dopplerometry of the vessels of the placenta and umbilical cord is a method for studying blood flow velocities in these vessels. With a decrease in the speed of blood flow in any vessel, one can speak of fetal malnutrition of varying severity.
Cardiotocography (CTG)
This is an important method for assessing the condition of the fetus. CTG is performed at a gestational age of 33 weeks or more, since only in this period of intrauterine development of the baby is a full-fledged regulation of the activity of the cardiovascular system of the fetus by the centers of the spinal cord and brain. Recording of fetal heartbeats is carried out for at least 40 minutes, and if necessary, the study can be extended up to one and a half hours. The device registers and records the baby's heart rate. For example, with a decrease in the concentration of oxygen in the blood of the fetus, the supply of oxygen to the cells of the nervous system decreases, which in turn affects the heart rate, especially during the period of wakefulness of the child. The obstetrician-gynecologist evaluates the heartbeat recording curve, episodes of slowing down and a sharp increase in the fetal heart rate, and based on these data, makes a conclusion about how comfortable the baby feels in the mother's stomach.
The device registers and records the baby's heart rate. For example, with a decrease in the concentration of oxygen in the blood of the fetus, the supply of oxygen to the cells of the nervous system decreases, which in turn affects the heart rate, especially during the period of wakefulness of the child. The obstetrician-gynecologist evaluates the heartbeat recording curve, episodes of slowing down and a sharp increase in the fetal heart rate, and based on these data, makes a conclusion about how comfortable the baby feels in the mother's stomach.
If during additional methods for assessing the condition of the fetus, initial disturbances in the supply of oxygen to the baby are detected, drug treatment is carried out aimed at increasing the access of blood and oxygen through the placenta and mandatory control examinations against the background of ongoing therapy. If the changes are profound and the baby experiences a pronounced deficiency of oxygen and nutrients, his condition suffers, an emergency delivery of such a patient is performed.
Fetal movements are not only an indicator of his condition, it is a way of communication between the baby and parents. The movements of the crumbs in the mother's tummy are unforgettable sensations that a woman can experience only in this short, but such a happy period of her life.
Center for Fetal Medicine in Moscow:
The main activities of our center are the early detection of congenital malformations in the fetus, prenatal screening for the detection of chromosomal abnormalities in the fetus, as well as pregnancy complications such as preeclampsia, fetal growth retardation and threatened abortion.
Our center is organized in such a way that the whole range of services is concentrated in one place, where a woman receives the results of various types of examinations, including ultrasound, biochemical, and specialist consultation within 1-1.5 hours. In the presence of a high risk for chromosomal diseases in the fetus, invasive diagnostics and genetics consultation are carried out here in the center.
Fetal echocardiography is given special attention in our center, since congenital heart defects in the fetus are increasingly common today, but, unfortunately, are often missed during ultrasound during pregnancy.
In view of the ever-increasing number of multiple pregnancies, which requires more time and a special approach, the observation of women with multiple pregnancies has been allocated to us in a separate clinic for multiple pregnancies.
All examinations in the center are carried out according to the international standards FMF (Fetal Medicine Foundation) and ISUOG (International Society for Ultrasound in Obstetrics and Gynecology). In complex clinical cases, we can consult with specialists from King's College Hospital, King's College Hospital (London, UK).
The team is a special pride of the center. Our doctors are not only one of the leading specialists, professors, doctors and candidates of medical sciences, doctors of the highest categories, they are also a team of like-minded people and real enthusiasts in their field.