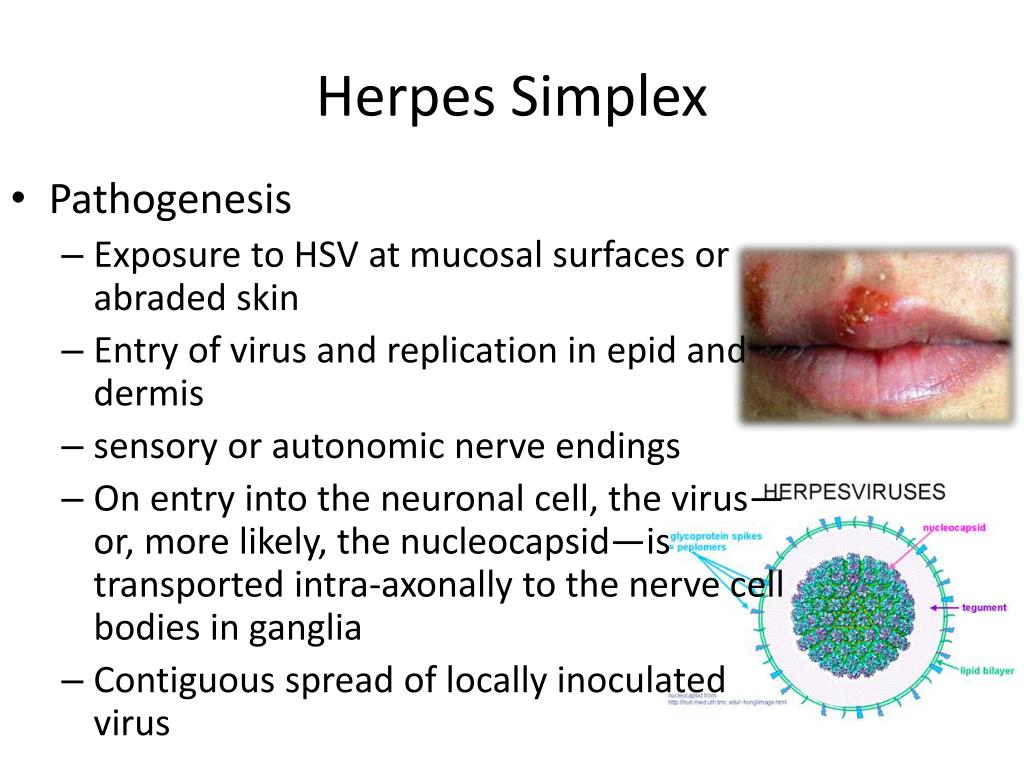
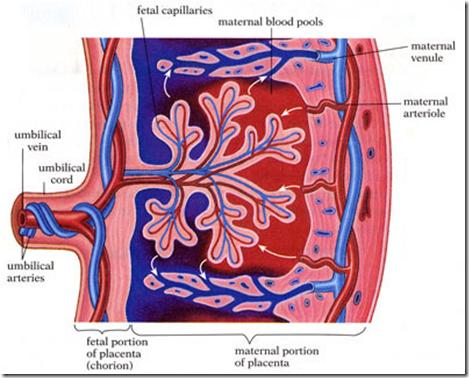
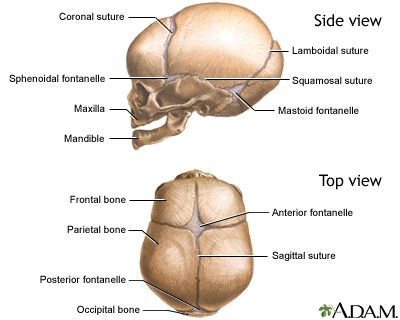
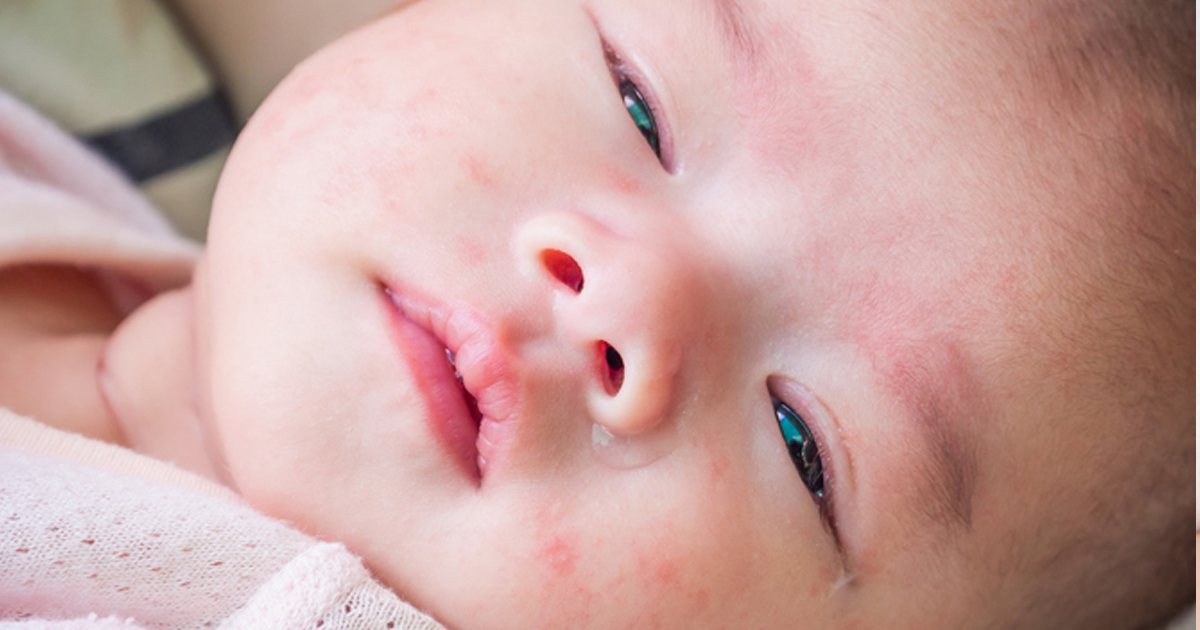
Pimple like rash on children
What are those bumps on my child's skin?
Diseases & conditions
- Coronavirus Resource Center
- Acne
- Eczema
- Hair loss
- Psoriasis
- Rosacea
- Skin cancer
- A to Z diseases
- A to Z videos
- DIY acne treatment
- How dermatologists treat
- Skin care: Acne-prone skin
- Causes
- Is it really acne?
- Types & treatments
- Childhood eczema
- Adult eczema
- Insider secrets
- Types of hair loss
- Treatment for hair loss
- Causes of hair loss
- Hair care matters
- Insider secrets
- What is psoriasis
- Diagnosis & treatment
- Skin, hair & nail care
- Triggers
- Insider secrets
- What is rosacea
- Treatment
- Skin care & triggers
- Insider secrets
- Types and treatment
- Find skin cancer
- Prevent skin cancer
- Raise awareness
- Español
Featured
Monkeypox: What you need to knowMonkeypox is a contagious disease that causes a rash. A board-certified dermatologist explains what the rash looks like and when to seek medical care.
This contagious skin disease will usually clear on its own, but sometimes dermatologists recommend treating it. Find out when.
Everyday care
- Skin care basics
- Skin care secrets
- Injured skin
- Itchy skin
- Sun protection
- Hair & scalp care
- Nail care secrets
- Basic skin care
- Dry, oily skin
- Hair removal
- Tattoos and piercings
- Anti-aging skin care
- For your face
- For your skin routine
- Preventing skin problems
- Bites & stings
- Burns, cuts, & other wounds
- Itch relief
- Poison ivy, oak & sumac
- Rashes
- Shade, clothing, and sunscreen
- Sun damage and your skin
- Aprenda a proteger su piel del sol
- Your hair
- Your scalp
- Nail care basics
- Manicures & pedicures
Featured
Practice Safe SunEveryone's at risk for skin cancer. These dermatologists' tips tell you how to protect your skin.
These dermatologists' tips tell you how to protect your skin.
Find out what may be causing the itch and what can bring relief.
Darker Skin Tones
- Skin care secrets
- Hair care
- Hair loss
- Diseases & Conditions
- Acne
- Dark spots
- Dry skin
- Light spots
- Razor bumps
- Caring for Black hair
- Scalp psoriasis
- Weaves & extensions
- Central centrifugal cicatricial alopecia
- Frontal fibrosing alopecia
- Hairstyles that pull can cause hair loss
- Acanthosis nigricans
- Acne keloidalis nuchae
- Hidradenitis suppurativa
- Keloid scars
- Lupus and your skin
- Sarcoidosis and your skin
- Skin cancer
- Vitiligo
- More diseases & conditions
Featured
Fade dark spotsFind out why dark spots appear and what can fade them.
If you have what feels like razor bumps or acne on the back of your neck or scalp, you may have acne keloidalis nuchae. Find out what can help.
Cosmetic treatments
- Your safety
- Age spots & dark marks
- Cellulite & fat removal
- Hair removal
- Scars & stretch marks
- Wrinkles
- Younger-looking skin
Featured
Laser hair removalYou can expect permanent results in all but one area. Do you know which one?
Do you know which one?
If you want to diminish a noticeable scar, know these 10 things before having laser treatment.
BotoxIt can smooth out deep wrinkles and lines, but the results aren’t permanent. Here’s how long botox tends to last.
Public health programs
- Skin cancer awareness
- Free skin cancer screenings
- Kids' camp
- Good Skin Knowledge
- Shade Structure grants
- Skin Cancer, Take a Hike!™
- Awareness campaigns
- Flyers & posters
- Get involved
- Lesson plans and activities
- Community grants
Featured
Free materials to help raise skin cancer awarenessUse these professionally produced online infographics, posters, and videos to help others find and prevent skin cancer.
Free to everyone, these materials teach young people about common skin conditions, which can prevent misunderstanding and bullying.
Find a dermatologist
- Find a dermatologist
- What is a dermatologist?
- FAAD: What it means
- How to select a dermatologist
- Telemedicine appointments
- Prior authorization
- Dermatologists team up to improve patient care
Featured
Find a DermatologistYou can search by location, condition, and procedure to find the dermatologist that’s right for you.
A dermatologist is a medical doctor who specializes in treating the skin, hair, and nails. Dermatologists care for people of all ages.
12 Common Summertime Skin Rashes in Children
Sunny days and starlit evenings spent playing, splashing, and exploring can leave kids with more than warm summertime memories. Balmy weather also can lead to itchy, irritated skin.
Check out the list from the American Academy of Pediatrics (AAP) to see how you can help prevent, identify, and soothe these common summertime skin rashes.
1. Heat Rash
Heat rash (also known as prickly heat or miliaria) is seen most often in babies and young children when sweat gland pores become blocked and perspiration can't escape. The rash looks like patches of small pink or red bumps or blisters under clothing or spots where skin tends to fold—on the neck, elbows, armpits, or thighs—although heat rash can occur on other covered areas.
What parents can do:
Keep kids cool. Dress your child in clothing that keeps the skin cool and dry. If possible, use fans and air conditioning to avoid overheating.
Pay attention to hot spots. Wash areas of the skin that stay wet with sweat, urine, or drool with cool water. Pat them dry.
Keep skin bare. Leave areas open to air without clothing. Do not apply skin ointments.
2. Poison Ivy & Other Plant Rashes
Many children get a burning, intensely itchy rash where their skin touches plants—such as poison ivy, poison oak, sumac—containing a sticky oil called urushiol. An allergic skin reaction causes redness, swelling and blisters. Other plants—such as wild parsnip, giant hogweed, and citrus—contain chemicals that make skin hypersensitive to sunlight and cause a phytophotodermatitis rash.
What parents can do:
Prevent exposure.
 Teach your child what these plants look like and how to avoid them. Both poison ivy and poison oak have shiny green leaves that grow three to a stem, so you might share the rhyme: "Leaves of three, let them be." The sumac shrub has stems that contain 7-13 leaves arranged in pairs, while wild parsnip and giant hogweed have clusters of small, flat-topped yellow and white flowers. If you have younger children, inspect the parks they play in and have rash-causing plants removed.
Teach your child what these plants look like and how to avoid them. Both poison ivy and poison oak have shiny green leaves that grow three to a stem, so you might share the rhyme: "Leaves of three, let them be." The sumac shrub has stems that contain 7-13 leaves arranged in pairs, while wild parsnip and giant hogweed have clusters of small, flat-topped yellow and white flowers. If you have younger children, inspect the parks they play in and have rash-causing plants removed.Wash and trim. If your child comes into contact with these plants, wash all of his or her clothes and shoes in soap and water. Also, wash the area of the skin that was exposed with soap and water for at least 10 minutes after the plant or the oil is touched. To discourage scratching and further damage to the skin, keep your child's fingernails trimmed. This will also prevent the rash from spreading if there is still a small amount of oil under the fingernails.
Soothing salves.
 If the rash is mild, apply calamine lotion to cut down on the itching. Avoid ointments containing anesthetics or antihistamines—they can cause allergic reactions themselves. Another good option to reduce skin inflammation is 1% hydrocortisone cream.
If the rash is mild, apply calamine lotion to cut down on the itching. Avoid ointments containing anesthetics or antihistamines—they can cause allergic reactions themselves. Another good option to reduce skin inflammation is 1% hydrocortisone cream.Talk with your pediatrician. While mild cases can be treated at home, talk with your pediatrician if your child is especially uncomfortable, the rash is severe and/or isn't going away, if the rash is on your child's face or groin area, or if you notice signs of infection (i.e., fever, redness, swelling beyond the poison ivy or oak lesions).
3. Eczema
Eczema (also called atopic dermatitis or AD) is a chronic condition common in children that causes patches of dry, scaly red skin and tends to flare up during colder months when there's less moisture in the air. But dryness caused by air conditioning and pressurized planes during summer travel can cause problems, too.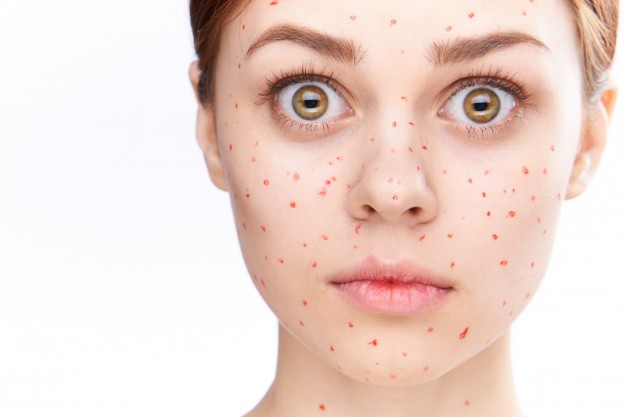 Overheating, sweating and chlorine in swimming pools also can trigger eczema.
Overheating, sweating and chlorine in swimming pools also can trigger eczema.
What parents can do:
Moisturize. Apply fragrance-free creams or ointments at least once a day or more often if needed. After a bath or swimming, gently pat your child's skin with a towel and then apply moisturizer to his or her damp skin.
Dress wisely. Choose clothing made of soft, breathable fabrics like cotton when possible. Wash clothes in a detergent free of irritants such as perfumes and dyes.
Don't scratch. Keep your child's fingernails short and smooth, and remind him or her not to scratch. Scratching can make the rash worse and lead to infection.
Talk with your pediatrician. Ask your child's pediatrician if allergies, sometimes triggered by trees and plants that bloom during summer, could be a cause of the eczema. Your child's pediatrician may recommend medicines to help your child feel better and to keep the symptoms of eczema under control.

4. Insect Bites & Stings
Insects such as bees, wasps, mosquitos, fire ants, and ticks can cause itching and minor discomfort where they prick the skin. For some children, insect bites and stings can cause a severe allergic reaction called anaphylaxis—which includes a rash or hives and life-threatening symptoms such as airway swelling. (For children with a known allergy to insect bites and stings, it is important to have anaphylaxis emergency care plan in place). Other times, diseases spread by insects such as Lyme Disease, Rocky Mountain Spotted Fever, and Zika Virus can cause rashes and other health problems.
What parents can do:
Avoidance. When spending time outdoors, avoid scented soaps and shampoos and brightly colored clothing—they can attract insects. If possible, steer clear of areas where insects nest and gather (i.e., stagnant pools of water, uncovered food, and blooming flowers).
Use insect repellent. Products with DEET can be used on the skin, but look for family-friendly products that contain concentrations of no more than 30% DEET. Wash the insect repellent off with soap and water when your child returns indoors.
Cover up. When in wooded areas or in or near tall grass, stay on cleared trails as much as possible. Have your child wear a long-sleeved shirt, pants, and hat. Avoid wearing sandals in an area where ticks may live.
Look closely. Wear light-colored clothing to make it easier to spot ticks. After coming indoors, check for ticks on your child's skin—they often hide behind the ears or along the hairline.
Remove stingers and ticks. To remove a visible stinger from skin, gently scrape it off horizontally with a credit card or your fingernail. If you find a tick, gently grasp it with fine-tipped tweezers as close to the skin as possible.
 Without squeezing the tick's body, slowly pull it away from the skin. See How To Remove A Tick for more information.
Without squeezing the tick's body, slowly pull it away from the skin. See How To Remove A Tick for more information. Clean the skin. After the stinger or tick is out, clean the bitten area with rubbing alcohol or other first aid ointment.
Treat swelling. Apply a cold compress or an ice pack to any swelling for at least 10 minutes.
Help relieve the itch. Applying ice, along with calamine lotion or 1% hydrocortisone cream, can also help relieve itching.
5. Impetigo
Impetigo is a bacterial skin infection that's more common during hot, humid weather. It causes a rash that may have fluid-filled blisters or an oozing rash covered by crusted yellow scabs. Impetigo is more likely to develop where there is a break in the skin, like around insect bites.
What parents can do:
Clean and cover. Clean the infected area with soap and water.
 Cover the infected area loosely to help prevent contact that would spread the infection to others or to other parts of the body. Wash your own hands well after treating your child's sores.
Cover the infected area loosely to help prevent contact that would spread the infection to others or to other parts of the body. Wash your own hands well after treating your child's sores. Avoid scratching. Trim your child's fingernails and discourage scratching. A child can spread the infection to other parts of his or her body by scratching. You can cover the rash loosely with a bandage to discourage your child from touching the rash, but make sure air can flow through so the skin can heal.
Talk with your pediatrician. While mild cases may respond to over-the-counter antibiotics such as bacitracin or bacitracin-polymyxin, impetigo is usually treated with prescription antibiotics—either a skin cream or oral medication. Your pediatrician may order a skin culture (test of your child's skin) to determine which bacteria are causing the rash.
6. Swimmer's Itch
Swimmer's itch (also called clam digger's itch or cercarial dermatitis) may appear after playing in lakes, oceans, and other bodies of water. The rash is caused by microscopic parasites found in shallow, warmer water near the shoreline where children tend to stay. The parasites burrow into skin, and cause tiny reddish, raised spots on skin not covered by the swimsuit to appear. Welts and blisters may also form.
What parents can do:
Be aware. Don't swim near or wade in marshy areas where snails are commonly found. Try not to attract birds (by feeding them, for example) where your family swims. Birds may eat the snails and spread the parasites in the water.
Shower or towel dry. Shower or briskly rub the skin with a towel immediately after getting out of the water. The parasites start to burrow when the water on skin begins evaporating. If your skin child's skin stings with rubbing—and the rash appears under the swimsuit—he or she may instead have Seabather's Eruption from stinging larvae of sea critters such as jellyfish or sea anemone. Stop rubbing and shower instead.

Don't scratch. Trim your child's fingernails and discourage scratching. Home treatments such cool compresses on the affected areas, Epsom salt or oatmeal baths, or baking soda paste may help to relieve the discomfort. If itching is severe, talk with your child's pediatrician. He or she may suggest prescription-strength lotions or creams to reduce your child's symptoms.
7. Cutaneous Larva Migrans (Sandworms)
Sandworms may be present in sand contaminated with feces from pets or stray animals. When a child stands or sits in contaminated sand on a beach or in a sandbox, the worms may burrow under the skin, usually around the feet or buttocks. Lines of itchy, reddish rash known as a creeping eruption appear as the worms move under the skin, up to a few centimeters a day. The condition is more common subtropical and tropical areas such as the Caribbean, as well as parts of the southwestern United States.
What parents can do:
Keep shoes on.
 Don't let your child play on beaches where people walk their dogs. If your family goes on an outing to a designated pet-friendly beach, make sure your child keeps shoes on and doesn't sit in the sand without a blanket or towel.
Don't let your child play on beaches where people walk their dogs. If your family goes on an outing to a designated pet-friendly beach, make sure your child keeps shoes on and doesn't sit in the sand without a blanket or towel.Talk with your pediatrician. Your pediatrician can prescribe anti-parasitic medications such as albendazole or ivermectin to treat the rash. Without treatment, the larvae usually will die off in 5 to 6 weeks. Your pediatrician may suggest a cream to help relieve itching.
8. Folliculitis (Hot Tub Rash)
Folliculitis (hot tub rash) is an itchy, pimply rash that occurs when bacteria in unclean pools and hot tubs gets into hair follicles on the skin. The area where hairs grow from the skin becomes infected and inflamed, sometimes forming small, pus-filled blisters. A similar rash may come from wearing a damp swimsuit that wasn't washed and dried well after previous use. Hot rub rash typically starts 12-48 hours after being in a hot tub.
What parents can do:
Avoid dirty pools. If you're unsure whether the acid and chlorine levels are properly controlled in a heated pool, don't allow your child to go in.
Don't allow young children in spas or hot tubs. In addition to the risk for drowning and overheating, young children are also at higher risk of bacterial skin infection because they tend to spend more time in the water than teens or adults.
Talk with your pediatrician. Hot tub rash usually clears up without medical treatment. In the meantime, warm compresses and an over-the-counter anti-itch cream recommended by your pediatrician can help your child be more comfortable. If your child's rash lasts more than a few days, talk with your pediatrician.
9. Molluscum Virus
Molluscum contagiosum is a viral infection that causes pearly bumps on the skin on a child's chest, back, arms or legs. The dome-shaped bumps, also known as "water warts," may have a dimple in the center. The poxvirus that causes the bumps is more common in hot, humid climates. Some studies suggest the infection may spread in contaminated swimming pools.
The poxvirus that causes the bumps is more common in hot, humid climates. Some studies suggest the infection may spread in contaminated swimming pools.
What parents can do:
Wait it out. In most cases, molluscum contagiosum does not need treatment. The bumps usually will go away in 6 to 12 months.
Stop the spread. A child with molluscum contagiosum should not share towels, bedding, or clothing with others to avoid spreading the virus. The bumps are contagious as long as they are present.
Avoid scratching. Scratching the bumps can spread the virus and cause a second, bacterial infection where the skin is open.
10. Juvenile Plantar Dermatosis (Sweaty Sock Syndrome)
A smooth, reddened rash on your child's feet, sometimes with peeling, cracking skin or scaly skin, could be from a condition called Juvenile Plantar Dermatosis (Sweaty Sock Syndrome). It happens when feet get wet and then dry quickly, again and again—like when shoes are taken on and off coming in and out of the house during summer.
What parents can do:
Breathable footwear. Reduce how often the feet go from wet to dry quickly by having your child wear open or more breathable footwear made of materials like mesh or cotton (i.e., water shoes) and/or thicker more absorbent socks.
Apply ointment. Applying moisturizing ointment or an over-the-counter steroid cream to the affected areas of your child's foot immediately after taking shoes off or getting out of water can help. If the condition does not improve, or if you notice any sign of infection where your child's skin is cracking, talk to your pediatrician.
11. Tinea (Ringworm)
Despite having "worm" in its misleading name, tinea (ringworm) is an infection caused by a fungus that thrives in warm, damp conditions. It is similar to athlete's foot and jock itch and can appear on a child's scalp or other parts of the body. It's called ringworm because the rash from the infection tends to form round or oval spots that become smooth in the center as they grow while the border remains red and scaly. The fungus can spread quickly among student athletes, especially during sweaty, summertime practices and games, when they share sports equipment and locker rooms.
The fungus can spread quickly among student athletes, especially during sweaty, summertime practices and games, when they share sports equipment and locker rooms.
What parents can do:
Stop the spread. Check and treat any pets that may have the fungus—look for scaling, itchy, hairless areas on their fur. Family members, playmates, or schoolmates who show symptoms also should be treated. Do not allow your child to share combs, brushes, hair clips, barrettes, or hats. Make sure mats used in sports like wrestling and gymnastics are properly disinfected after use.
Talk with your pediatrician. A single ringworm patch on the body can be treated with an over-the-counter cream recommended by your pediatrician. If there are any patches on the scalp or more than one on the body, or if the rash is getting worse while being treated, your pediatrician may prescribe a stronger medication and special shampoo.
12.
 Hand, Foot & Mouth Disease
Hand, Foot & Mouth DiseaseMany parents assume virus season winds down after winter. But some viral illnesses, such as hand, foot, and mouth disease, are more common during summer and early fall. Outbreaks are most common in younger children and can spread in child care centers, preschools, and summer camps. Caused by Enterovirus coxsackie, the illness starts with a fever, sore throat, and runny nose—much like the common cold—but then a rash with tiny blisters may appear on any or all the following places on the body:
In the mouth (inner cheeks, gums, sides of the tongue or back of the mouth)
Fingers or palms of hands
Soles of feet
Buttocks
Symptoms are the worst in the first few days, but they are usually gone within a week. Peeling skin on the fingers, toes, and nails may begin after a week or two, but it is harmless. Parents of children with a history of atopic dermatitis or eczema should be aware that their children may be prone to a more severe outbreak.
What parents can do:
Monitor symptoms. Be sure to call your pediatrician if your child's fever lasts more than 3 days or if he or she is not drinking fluids. If symptoms are severe, your pediatrician may collect samples from your child's throat for lab testing.
Ease the pain. For fever and pain, the pediatrician may also recommend acetaminophen or ibuprofen. Liquid mouth-soothing remedies may be useful to alleviate mouth ulcer pain. Do not use regular mouthwashes, because they sting.
Avoid dehydration: Children with hand, foot, and mouth disease need to drink plenty of fluids. Call your pediatrician or go to the ER if you suspect your child is dehydrated. See Signs of Dehydration in Infants & Children for more information.
Inform others. Tell child care providers and playmates' parents to watch for symptoms of the illness.
Children with hand, foot, and mouth disease may spread the virus through the respiratory tract (nose, mouth and lungs) for 1-3 weeks, and in the stool for weeks to months after the infection starts. Once a child's fever has gone away and he or she is feeling better, there is no need to keep him or her home unless there are still open and oozing blisters. See When to Keep Your Child Home from Child Care for more information.
Remember…
Protecting your child's skin is a year-round concern, but it's especially important in the summer months when so much skin is exposed and vulnerable. Fortunately, many summertime rashes clear up quickly on their own. Be sure to talk with your pediatrician about any rash that you're unsure about—especially if you don't know what caused it, if it is making your child feel miserable or doesn't clear up quickly, or if it shows signs of infection or is accompanied by any shortness of breath.
Additional Information:
- Summer Safety Tips: Staying Safe Outdoors
- Antibiotic Prescriptions for Children: 10 Common Questions Answered
- American Academy of Dermatology
- American College of Allergy, Asthma & Immunology
- Society for Pediatric Dermatology
The information contained on this Web site should not be used as a substitute for the medical care and advice of your pediatrician. There may be variations in treatment that your pediatrician may recommend based on individual facts and circumstances.
There may be variations in treatment that your pediatrician may recommend based on individual facts and circumstances.
Rash in a child on the body, legs, back
We treat children according to the principles of evidence-based medicine: we choose only those diagnostic and treatment methods that have proven their effectiveness. We will never prescribe unnecessary examinations and medicines!
Make an appointment via WhatsApp
Prices Doctors
The first children's clinic of evidence-based medicine in Moscow
No unnecessary examinations and medicines! We will prescribe only what has proven effective and will help your child.
Treatment according to world standards
We treat children with the same quality as in the best medical centers in the world.
The best team of doctors in Fantasy!
Pediatricians and subspecialists Fantasy - highly experienced doctors, members of professional societies. Doctors constantly improve their qualifications, undergo internships abroad.
Doctors constantly improve their qualifications, undergo internships abroad.
Ultimate treatment safety
We made pediatric medicine safe! All our staff work according to the most stringent international standards JCI
We have fun, like visiting best friends
Game room, cheerful animator, gifts after the reception. We try to make friends with the child and do everything to make the little patient feel comfortable with us.
You can make an appointment by calling or by filling out the form on the website
Other Pediatric services
- Pediatrician's consultation
- Child Health Management Program
Frequent calls
- Acute bronchiolitis in children: diagnosis and treatment
- SARS
- Angina streptococcal tonsillitis
- Frequently ill child
- Intestinal infections
- Pneumonia (pneumonia) in children
- Colic
- Feeding problems
- Prolonged cough in a child: diagnosis and treatment
- Acute bronchitis in children: diagnosis and treatment
- Pneumonia (pneumonia) in children: diagnosis and treatment
- False croup in a child
- Coxsackie virus in a child
- The child was bitten by a tick! What to do?
Online payment
Documents online
Online services
Rashes on the child's body
Many parents have noticed suspicious rashes on the body of their children. This symptom indicates the presence of any disease of the body or simply its painful condition. In any case, a rash on a child's body can be very dangerous. Therefore, if you notice a rash on the skin, you should immediately make an appointment with the child's pediatrician.
This symptom indicates the presence of any disease of the body or simply its painful condition. In any case, a rash on a child's body can be very dangerous. Therefore, if you notice a rash on the skin, you should immediately make an appointment with the child's pediatrician.
Rash help
Make an appointment with a doctor
Online appointment
Phones:
+7 (812) 30-888-03
+7 (812) 242-53-50 Clinic address: 900 900 50 Petersburg, Vyborgsky district, st. Asafiev, 9, building 2, lit. A (metro station Ozerki, metro station Prosveshcheniya)
Causes of rashes
A rash in children can appear for various reasons. The most “safe” case is when rashes appear due to poor hygiene. In addition, the cause of the rash is allergies, blood diseases, cardiovascular diseases, as well as infections and microbes. In the case of an infection, a rash is not the only symptom: fever, runny nose, sore throat, severe cough, chills, etc. are added to it. Often infections are accompanied by indigestion and vomiting. The rash in such cases does not occur immediately, but appears after a few days.
Often infections are accompanied by indigestion and vomiting. The rash in such cases does not occur immediately, but appears after a few days.
Rash most often occurs as a symptom of diseases that are commonly referred to as "children's". We are talking about chicken pox, rubella, measles, scarlet fever and some other infections that people get sick, mainly in childhood. Moreover, depending on the disease, the nature of the rash changes, so that doctors can diagnose only one type of rash. The most dangerous rash, which refers to the symptoms of meningitis.
Diseases causing rashes on the skin of children
Let's analyze the types of rash in a child in more detail, depending on the disease.
- Chicken pox. Perhaps the most famous disease that is accompanied by a rash. With chickenpox, reddish spots appear on the entire surface of the body, which grow and become bubbles filled with a clear liquid. The growth of the bubbles is accompanied by itching, but over time they dry out and fall off, sometimes leaving characteristic “pockmarks”.
 Chicken pox often causes fever, and doctors recommend treating blisters of the rash with brilliant green.
Chicken pox often causes fever, and doctors recommend treating blisters of the rash with brilliant green. - Measles. Initially, a rash in the form of large red spots appears on the face, but literally within 2-3 days it spreads “from top to bottom” along the body to the very legs. In addition, the child begins to have a sore throat, runny nose and cough, and the temperature rises. The largest spots merge into large inflamed areas.
- Meningococcal infection. The most dangerous infection, as it causes meningitis. It is very important to recognize the disease in time, as it develops very quickly. The rash is expressed in the form of large spots resembling bruises. If you see a doctor as soon as possible, the chances of a cure are very high.
- Rubella. The rash is accompanied by fever and inflammation of the lymph nodes. A rash on the body of a child in the form of small red spots appears mainly on the buttocks and in the places where the limbs are bent.
 After a few days, the rash disappears without leaving any consequences.
After a few days, the rash disappears without leaving any consequences. - Scarlet fever. With scarlet fever, a rash in the form of small pimples appears on the second day all over the body, but their highest concentration is noted in the groin, in the places of the folds of the arms and legs and in the lower abdomen. After a few days, the rash disappears, and the skin in these places begins to peel off strongly. Also during the peak of the disease, swelling, rash and redness of the entire skin are noted.
- Enteroviral infection. Redness and rash appear on the third day after infection and last for about two to three days. Their other symptoms, doctors note vomiting, diarrhea, fever and general weakness of the body.
- Parasites. In this case, the rash is not caused by infections, but by scabies mites or other parasites that live on the human body. The scabies mite "drills" holes in the skin, leaving entrances and exits in the form of dots. The most “attractive” parts of the body for a tick are places with thin skin: groin, wrists, areas between fingers, etc.
 Since the tick can be transmitted from one person to another, urgent treatment is necessary after the detection of this pathology.
Since the tick can be transmitted from one person to another, urgent treatment is necessary after the detection of this pathology. - Cardiovascular diseases. As a rule, these diseases are not typical for children, although they occur in them. Vascular disease can be recognized by small hemorrhages under the skin. Larger areas form bruises.
Other causes of rashes
Sometimes, even with all the rules of hygiene and the absence of diseases, a rash on the body of a child appears with enviable regularity. In this case, it is most likely an allergic reaction of the body to various substances. If this is true, then allergies can be recognized by other symptoms that will inevitably appear along with the rash: a runny nose, cough, tears, and itching. Also, a rash on the body of a child may appear from burns by plants or insect bites. Even a simple mosquito bite often causes a severe rash in children, which is accompanied by itching.
And, of course, very often a rash appears due to poor hygiene. Unlike adults, children's skin is much thinner and more delicate, so even a short-term lack of care for it can lead to a rash. Children, especially the smallest, should be washed and washed regularly. But wearing a lot of clothes on him or leaving him in wet diapers is not worth it - this can lead to diaper rash, irritation, and a rash.
Unlike adults, children's skin is much thinner and more delicate, so even a short-term lack of care for it can lead to a rash. Children, especially the smallest, should be washed and washed regularly. But wearing a lot of clothes on him or leaving him in wet diapers is not worth it - this can lead to diaper rash, irritation, and a rash.
Rash Help
If you find a rash on your child's body, you should see a doctor as soon as possible. You can make an appointment at our Poem Health clinic. In addition, you can call a doctor at home if the child is in a serious condition. Moreover, sometimes a doctor's house call is mandatory, since many diseases with symptoms in the form of a rash are easily transmitted to such children. You need to be especially careful with rubella, as it seriously affects the health of pregnant women. And if you suspect meningitis, you need to call not just a doctor, but an ambulance team.
Do not try to get rid of the rash on your own before seeing a doctor. Firstly, it will make it difficult for a doctor to determine the diagnosis. Secondly, it can lead to even more rashes in the child. It is best to wait for the examination of the doctor and listen to his recommendations for further treatment of the rash. Bacterial rashes are treated with antibiotics, scabies - with special means against ticks, allergies - with appropriate drugs with isolation from the source of allergies, etc. More complex treatment is needed for cardiovascular diseases, but, in the end, a rash on the body of a child is always treated successfully.
Firstly, it will make it difficult for a doctor to determine the diagnosis. Secondly, it can lead to even more rashes in the child. It is best to wait for the examination of the doctor and listen to his recommendations for further treatment of the rash. Bacterial rashes are treated with antibiotics, scabies - with special means against ticks, allergies - with appropriate drugs with isolation from the source of allergies, etc. More complex treatment is needed for cardiovascular diseases, but, in the end, a rash on the body of a child is always treated successfully.
Rash Prevention
To avoid a rash on the body, you need to take steps to prevent it. First of all, we are talking about the basic rules of personal hygiene. At the earliest age, parents should take care of this, later they should teach this to their child as early as possible. Compliance with hygiene helps to get rid of not only rashes, sweating and dirt, but also prevents many infectious diseases.
In addition, infections can be prevented by vaccination.