Pictures of women with chlamydia
Herpes, Genital Warts, Gonorrhea, STD Symptoms, & Testing
Medically Reviewed by Traci C. Johnson, MD on August 16, 2021
You don't have to have sex to get an STD. Skin-to-skin contact is enough to spread HPV, the virus family that causes genital warts. Some types cause warts and are usually harmless, but others may lead to cervical or anal cancer. Vaccines can protect against some of the most dangerous types.
Signs: Pink or flesh-colored warts that are raised, flat, or shaped like cauliflower. Often there are no symptoms.
"Crabs" is the common term for lice that set up shop in pubic hair. The term comes from the shape of the tiny parasites, which look very different from head or body lice. The creatures crawl from one person to another during close contact. Pubic lice can be killed with over-the-counter lotions.
Symptoms: Intense itching, tiny eggs attached to pubic hair, or crawling lice.
Scabies is an itchy infestation caused by a tiny mite that burrows into human skin to lay eggs. It is not always an STD, as it can spread through any skin-to-skin contact. But among young adults, the mites are often acquired during sex. Scabies is treated with prescription creams.
Symptoms: Intense itching especially at night and a pimple-like rash. It may take 2-6 weeks for symptoms to appear.
Gonorrhea spreads easily and can lead to infertility in both men and women, if untreated. Antibiotics stop the infection.
Symptoms: Common symptoms are burning during urination and discharge, but often there are no early symptoms. Later, the infection may cause skin rashes or spread to the joints and blood.
In Men: Discharge from the penis, swollen testicles.
In Women: Vaginal discharge, pelvic pain, spotting. Symptoms may be mild and are easily confused with a urinary tract or vaginal infection.
Most people don't notice the early symptoms of syphilis. Without treatment, it can lead to paralysis, blindness, and death. Syphilis can be cured with antibiotics.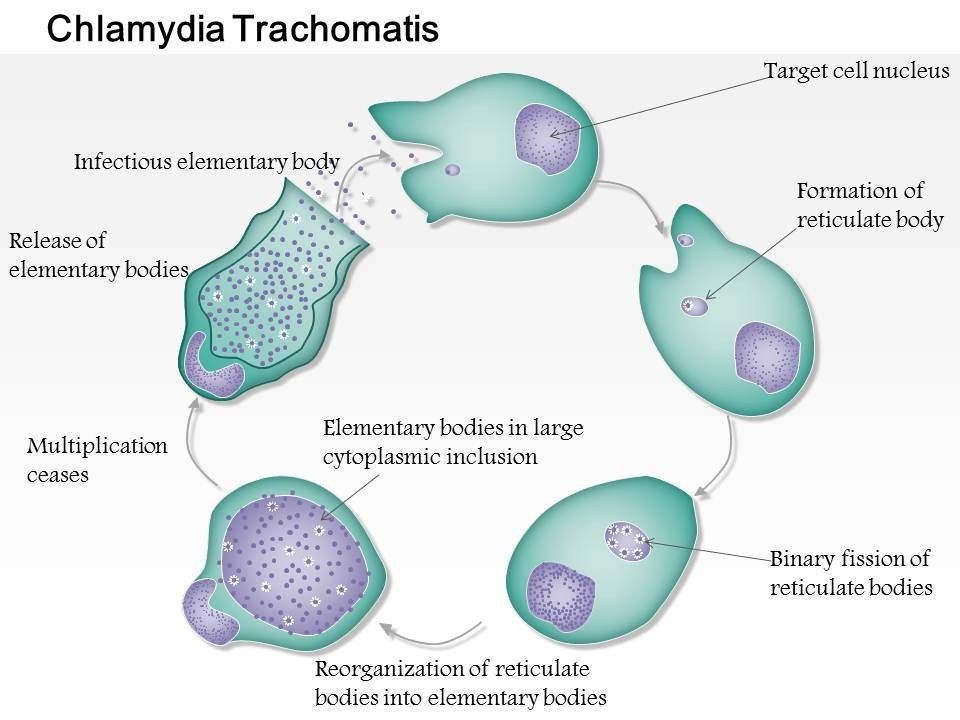
Signs and Symptoms: The first sign is usually a firm, round, painless sore on the genitals or anus. The disease spreads through direct contact with this sore. Later there may be a rash on the soles, palms, or other parts of the body (seen here), as well as swollen glands, fever, hair loss, or fatigue. In the late stage, symptoms come from damage to organs such as the heart, brain, liver, nerves, and eyes.
Chlamydia is a common STD that can lead to infertility if left untreated. It clears up quickly with antibiotics. But it often goes unnoticed because symptoms are vague or absent. Chlamydia can also infect the rectum and throat.
Symptoms in Men: Burning and itching at the tip of the penis, discharge, painful urination.
Symptoms in Women: Vaginal itching, discharge that may have an odor, pain during sex, painful urination.
That painful cold sore you get on your lip every now and then? It's probably caused by a type of herpes virus called HSV-1.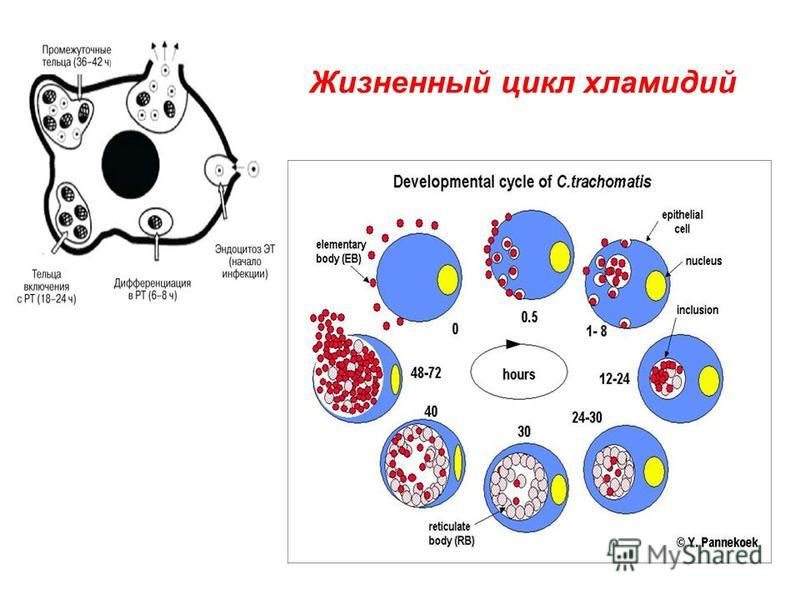 This virus is usually not an STD; it spreads easily among household members or through kissing. But it can be spread to the genitals through oral or genital contact with an infected person. Though there is no cure, drugs can shorten or prevent outbreaks.
This virus is usually not an STD; it spreads easily among household members or through kissing. But it can be spread to the genitals through oral or genital contact with an infected person. Though there is no cure, drugs can shorten or prevent outbreaks.
Signs and Symptoms: Occasional cold sores or "fever blisters" on the lips. Small blister or sores on the genitals are also possible.
Most cases of genital herpes are caused by a virus called HSV-2. It's highly contagious and can spread through intercourse or direct contact with a herpes sore. As with HSV-1, there is no cure. But antiviral drugs can make outbreaks less frequent and help clear up symptoms more quickly.
Symptoms: Fluid-filled blisters that form painful, crusted sores on the genitals, anus, thighs, or buttocks. Can spread to the lips through oral contact.
Hepatitis B is a stealthy virus that can cause severe liver damage. It spreads through contact with blood and other body fluids. People can be infected through sex, needle sharing, and at birth, as well as by sharing razors and toothbrushes. There is no cure, but drugs can keep the virus in check. There's also an effective vaccine to prevent hepatitis B.
People can be infected through sex, needle sharing, and at birth, as well as by sharing razors and toothbrushes. There is no cure, but drugs can keep the virus in check. There's also an effective vaccine to prevent hepatitis B.
Symptoms: People may develop nausea, belly pain, dark urine, fatigue, and a yellowing of the skin or eyes with acute infection. Chronic infection can lead to liver cirrhosis and liver cancer. Many people have no symptoms for years.
The HIV virus weakens the body's defense against infections. HIV spreads through unprotected sex, needle sharing, or being born to an infected mother. It may cause no symptoms for years, so a blood test is the best way to learn your status. Timely treatment is important to help prevent serious illnesses.
Early symptoms of HIV Infection: Many have no symptoms, but some people get temporary flu-like symptoms one to two months after infection: swollen glands (seen here), a fever, headaches, and fatigue. Canker sores in the mouth can occur, too.
Reliable HIV tests can be done in a clinic or at home with the FDA-approved Home Access brand test kit. Anonymous tests use only a number to identify you. One limitation is the "window period" of up to six months after exposure to HIV when these antibody tests sometimes do not find the virus. You can pass HIV to others during that time.
If You Suspect HIV/AIDS: If you've been exposed to HIV, starting medications immediately can help prevent infection. If you have the virus, treatments can help prevent HIV from turning into AIDS.
While there is no cure for HIV, there are medications that can suppress the amount of virus multiplying inside the body. People take a combination of antiviral drugs in hopes of preventing the infection from advancing to AIDS. Additional treatments can help prevent or fight off serious infections, if the immune system has weakened.
Trichomoniasis is caused by a parasite that spreads during sexual contact. It can be cured with prescription drugs.
Signs and Symptoms in Men: Most men have no obvious symptoms. Some develop a mild discharge or slight burning during urination.
Signs and Symptoms in Women: Women may develop a yellow-green discharge with a strong odor, vaginal itching, or pain during sex or urination. Symptoms usually begin five to 28 days after acquiring the parasite.
Chancroid is a bacterial STD that is common in Africa and Asia but rare in the U.S. It causes genital sores that can spread the bacteria from one person to another. Antibiotics can cure the infection.
Symptoms in Men: Painful bumps on the penis that may develop into pus-filled open sores, pain in the genitals and groin.
Symptoms in Women: Painful bumps in the genital area that can develop into open sores, swollen lymph nodes in the groin.
LGV is caused by a type of chlamydia that is usually rare in the U.S. But it's becoming more common in men who have sex with men. Like other forms of chlamydia, it can be cured with antibiotics.
Symptoms: Open sores on the genitals or anus, headache, fever, fatigue, and swollen lymph glands in the groin (seen here). If acquired through anal sex, LGV may cause rectal bleeding or discharge.
Not an STD itself, pelvic inflammatory disease (PID) is a serious complication of untreated STDs, especially chlamydia and gonorrhea. It happens when bacteria spread to infect the uterus and other female reproductive organs. Prompt treatment is essential to prevent damage to a woman's fertility.
Signs and Symptoms: Lower abdominal pain, fever, unusual discharge, painful intercourse, painful urination, and spotting. However, there are often no warning signs.
Anyone who is sexually active is at risk for an STD, regardless of gender, race, social class, or sexual orientation. That said, teenagers and young adults acquire STDs more easily than older people. By age 25, half of sexually active adults get an STD. Having multiple sex partners also raises the risk.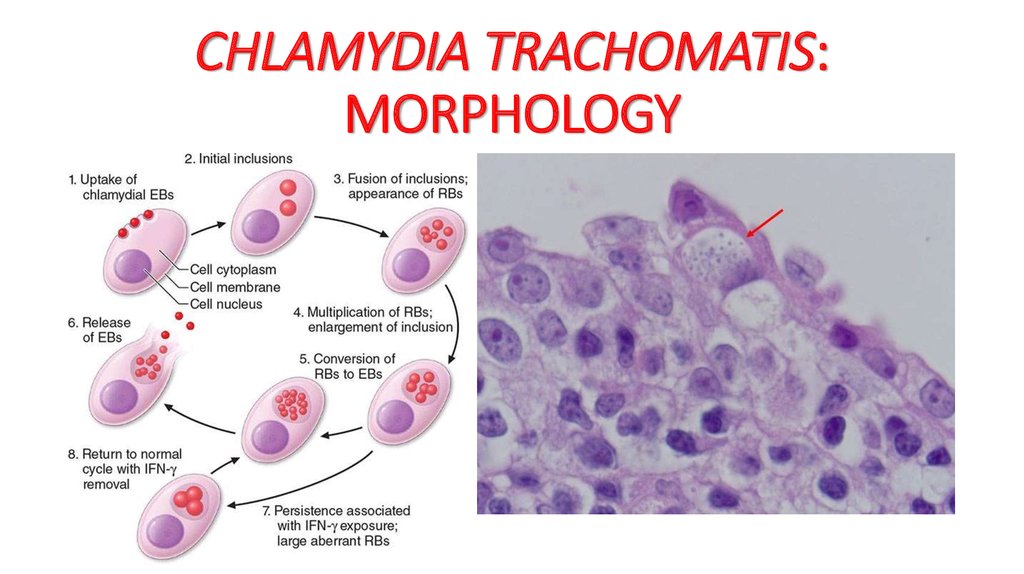 The CDC has noted that some STDs are on the rise in men who have sex with men, including syphilis and LGV.
The CDC has noted that some STDs are on the rise in men who have sex with men, including syphilis and LGV.
Yes, they can. Many STDs spread through any type of sexual activity, including skin-to-skin contact and oral sex. This is especially true of STDs that produce genital lesions or sores.
The best ways to avoid getting an STD are to abstain from any sexual contact and be in a monogamous, long-term relationship with an uninfected partner. To reduce the odds of getting STDs:
- Ask your partner if they have an STD.
- Ask partners to be tested before sexual activity.
- Use condoms.
- Avoid sexual activity if your partner has signs of an STD.
- Be aware of symptoms and get regular checkups with your health care provider.
While condoms are effective in preventing the spread of some STDs, they are not perfect. Condoms are better at protecting against gonorrhea, chlamydia, HIV, and trichomoniasis. But they offer less protection against herpes, syphilis, and genital warts. These infections can spread through contact with skin lesions that are not covered by a condom. Finally, condoms offer virtually no protection against crabs and scabies.
These infections can spread through contact with skin lesions that are not covered by a condom. Finally, condoms offer virtually no protection against crabs and scabies.
If you think you have an STD, tell your partner(s) as soon as possible. You may be able to spread the infection even if you have already begun treatment or are using condoms. With some STDs, doctors recommend treating both partners at the same time. This may be a difficult conversation. Some people find it helpful to write a script ahead of time. Be sure to let your partner ask questions and express their feelings.
It is important for pregnant women to be checked for STDs. They can cause women to go into labor too early and may complicate delivery. Many STDs can be passed from mother to baby during pregnancy, childbirth, or after the baby is born. STDs' effects on babies can include stillbirth, low birth weight, neurologic problems, blindness, liver disease, and serious infection. But there are treatments to minimize these risks. Treatment during pregnancy can cure some STDs and lower the risk of passing the infection to your baby.
Treatment during pregnancy can cure some STDs and lower the risk of passing the infection to your baby.
Most STD treatments do not protect you from getting the same infection again. A course of drugs may cure gonorrhea, syphilis, chlamydia or trichomoniasis, but a new exposure can start a new infection. If your partner is not treated, you can continue to pass infections back and forth. And if you're not taking the right precautions to protect yourself, you can be re-infected quickly or even pick up a second STD.
IMAGES PROVIDED BY:
1) Science Source, Dr P. Marazzi, Dr. Harout Tanielian, Biophoto Associates / Photo Researchers Inc.
2) London Scientific Films
3) Dr. P. Marazzi / Photo Researchers, Inc.
4) Juergen Berger / Photo Researchers, Interactive Medical Media LLC , Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatology
5) Science Source/Photo Researchers, Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatology
6) BSIP/Photo Researchers Inc
7) Interactive Medical Media LLC
8) Interactive Medical Media LLC, Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatology, Dr. Harold Fisher/Visuals Unlimited
Harold Fisher/Visuals Unlimited
9) Eye of Science/Photo Researchers Inc
10) Dr. M.A. Ansary / Photo Researchers, Inc., Science Source, Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatology
11) Bildagentur RM/Tips Italia
12) Bruce Forester/Photographer's Choice
13) IMA / Photo Researchers Inc
14) Dr. M.A. Ansary / Photo Researchers, Inc., David M. Phillips / Photo Researchers, Inc, Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatolog
15) Dr. M.A. Ansary / Photo Researchers, Inc.
16) Judith Glick / Phototake
17) Clarissa Leahy/Photographer's Choice
18) Christoph Martin/Lifesize
19) George Diebold/Photographer's Choice
20) Michael Winokur/Workbook Stock
21) John Lamb/Stone
22) UHB Trust/Stone
23) Alan Powdrill/Stone
REFERENCES:
American Social Health Association.
American Social Health Association's National Herpes Resource Center.
Centers for Disease Control and Prevention web site.
FDA web site.
Fleming, et al. The New England Journal of Medicine, Oct. 16, 1997.
March of Dimes web site.
Merck Manual, 17th edition.
National HIV Testing Resources.
National Institute of Allergy and Infectious Diseases.
National Institutes of Health.
The Nemours Foundation's Kids Health web site.
U.S. Dept. of Health and Human Services.
© 2021 WebMD, LLC. All rights reserved. View privacy policy and trust info
Pictures, Symptoms, Treatment, and More
Medically Reviewed by Nivin Todd, MD on December 17, 2020
You may feel itchy or tingly around your genitals. This is usually followed by painful, small blisters that pop and leave sores that ooze or bleed. Most people notice symptoms within a few weeks after they catch the virus from someone else. The first time it happens, you may also have a fever, headache, or other flu-like feelings. Some people have few or no symptoms.
You get herpes by having any kind of sex -- vaginal, oral, or anal -- with someone who’s infected. It’s so common in the U.S. that 1 in every 5 adults has it. Herpes can be spread during oral sex if you or your partner has a cold sore. Because the virus can't live long outside your body, you can't catch it from something like a toilet seat or towel.
It’s so common in the U.S. that 1 in every 5 adults has it. Herpes can be spread during oral sex if you or your partner has a cold sore. Because the virus can't live long outside your body, you can't catch it from something like a toilet seat or towel.
Sometimes people mistake a pimple or ingrown hair for herpes. Your doctor can take a small sample from sores by using a swab test. If you don’t have symptoms but think you might have herpes, your doctor can do a blood test. It may take a few days to get your results.
Genital herpes usually comes from the virus called herpes simplex-2 (HSV-2). Its cousin, HSV-1, is what gives you cold sores. You can get HSV-2 from someone whether they have symptoms or not.
Your doctor will prescribe an antiviral medicine. These pills can help you feel better and shorten an outbreak. In the meantime, don’t kiss or have any kind of sex with other people. Even if you don’t have symptoms, you can still spread the disease.
Some people only take their medications if they feel the itching and tingling that means an outbreak is coming on -- or when sores show up -- to stop it from getting worse. Your doctor may suggest you take an antiviral every day if you:
Your doctor may suggest you take an antiviral every day if you:
- Have lots of outbreaks
- Want to prevent more outbreaks
- Want to lower the risk of spreading it to your partner
You can treat herpes, but once you get it, you’ll always have it. When symptoms show up, it’s called having an outbreak. The first is usually the worst. Most people have them on and off for several years, but they get milder and happen less often over time.
As long as you're sexually active, there's a chance you could get herpes. You'll make it a lot less likely if you use a latex or polyurethane condom or dental dam every time, for every activity. The dam or condom only protects the area it covers. If you don’t have herpes, you and your partner should get tested for STDs before sex. If you’re both disease-free and aren’t having sex with other people, you should be safe.
- Wear loose-fitting clothes and cotton underwear.
- Avoid sun or heat that could cause more blisters.
- Take a warm, soothing bath.
- Don't use perfumed soaps or douches near your blisters.
The herpes virus stays in your body forever, even if you have no symptoms. You may have an outbreak when you're sick, after you’ve been out in the sun, or when you’re stressed out or tired. If you’re a woman, you could get one when you start your period.
You still can have sex if you have genital herpes, but you must tell your partner you have the virus. They need to know so they can get tested. Wear a condom any time you have sex. Never have sex during an outbreak.
People often don’t have serious problems from herpes, but there's a chance of them. Wash your hands often, especially during an outbreak. If you touch a blister and rub your eyes, the infection can spread to your eyes. If your eyes are red, swollen, hurt, or are sensitive to light, see your doctor. Treating it can help prevent serious vision problems.
If you’re pregnant and have herpes, your doctor may suggest that you have your baby by C-section if you are experiencing an outbreak. Why? During vaginal birth, the herpes virus could spread to your baby, especially if your first outbreak happens around the delivery time. The virus could give your baby rashes, eye problems, or more serious issues. A C-section makes that less likely. Your doctor may also have you take anti-viral medicine starting at about 34 weeks to avoid an outbreak around your due date.
Why? During vaginal birth, the herpes virus could spread to your baby, especially if your first outbreak happens around the delivery time. The virus could give your baby rashes, eye problems, or more serious issues. A C-section makes that less likely. Your doctor may also have you take anti-viral medicine starting at about 34 weeks to avoid an outbreak around your due date.
Getting ready to talk to your partner about herpes? These tips can help you prepare for the conversation. The American Sexual Health Association recommends you pick a time when you won't be interrupted, plan what you want to say ahead of time, and practice what you'll say so you feel confident.
IMAGES PROVIDED BY:
(1) Interactive Medical Media LLC, Fitzpatrick's Color Atlas & Synopsis of Clinical Dermatology, Dr. Harold Fisher
(2) Blend Images
(3) iStock
(4) The Image Bank
(5) Moment Open
(6) Stockbyte
(7) iStock
(8) Photo Alto
(9) Digital Vision
(10) Taxi
(11) Iconica
(12) Photo Researchers / Getty
(13) Monkey Business
(14) Photonica
SOURCES:
American Sexual Health Association
Brown University Health Education: "Genital Herpes. "
"
CDC: "Genital Herpes - CDC Fact Sheet."
Kimberlin, D. Human Herpes Viruses, 2007.
TeensHealth: "Genital Herpes."
University of Rochester Medical Center: "What You Need to Know About STDs."
UpToDate.com: "Patient information: Genital herpes (Beyond the Basics)."
WomensHealth.gov: "Genital herpes fact sheet."
© 2020 WebMD, LLC. All rights reserved. View privacy policy and trust info
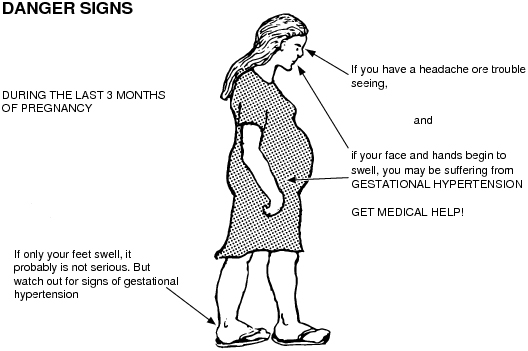
Signs of chlamydia in women.
According to the World Health Organization, urogenital chlamydia is one of the most common sexually transmitted diseases. And this means that no woman is immune from this disease, especially if she is not protected by barrier contraceptives. How is chlamydia diagnosed in women? By what signs can one suspect this disease in oneself in order to proceed with the prompt treatment?
What is chlamydia
Chlamydia is a sexually transmitted disease caused by a specific bacteria called chlamydia. They affect the genitals and urinary system and begin their vigorous activity there. According to various sources, from 6% to 8% of the adult population of the planet suffer from chlamydia.
They affect the genitals and urinary system and begin their vigorous activity there. According to various sources, from 6% to 8% of the adult population of the planet suffer from chlamydia.
The insidiousness of chlamydia lies in the variety of their types, which often complicates the treatment process. And you also need to keep in mind that this intracellular parasite very often becomes the culprit of infertility and miscarriage during pregnancy. That's why to recognize chlamydia in time is extremely important for the health of a woman and her future offspring.
Manifestation of chlamydia in women
The first 2-3 weeks after infection with chlamydia are the incubation period. At this time, chlamydia are embedded in the cells of their new host and multiply. After that, the first signs of an acute stage may appear, or the opposite may happen - the disease will not manifest itself in any way and for the time being will proceed in a latent form with no visible symptoms. nine0003
nine0003
- The most striking sign is chlamydia discharge. In women, it is a yellowish mucous discharge from the vagina with an unpleasant odor.
- Another manifestation of chlamydia in women is discomfort during urination: itching, burning.
- General symptoms: fever, weakness.
Often, after the acute stage of the disease passes, all unpleasant manifestations disappear, which, of course, does not mean a cure. Chlamydia does not disappear, on the contrary, it becomes chronic. Such an asymptomatic course of the disease becomes the reason that chlamydia is diagnosed late, usually by accident, when a woman comes for a routine examination to a gynecologist. Late diagnosis of this sexually transmitted disease requires a longer and more complex treatment. In addition, chronic chlamydia often leads to complications. nine0003
Complications of chlamydia in women
In the process of childbirth in a mother with chlamydia, infection of the child is possible. Chlamydia easily affects the internal organs, joints and eyes of the baby. That is why pregnancy should be planned: visit a gynecologist in advance, undergo an examination, do all the necessary research and take tests.
Chlamydia easily affects the internal organs, joints and eyes of the baby. That is why pregnancy should be planned: visit a gynecologist in advance, undergo an examination, do all the necessary research and take tests.
In addition, chlamydia can cause inflammation in the fallopian tubes and abdominal cavity, which contributes to the formation of adhesions, which leads to problems with conception. Chlamydia can also enter the bladder, causing cystitis. nine0003
The human body is so arranged that many pathological processes proceed asymptomatically in it, especially in the early stages. We invite you to the International Medical Center ON CLINIC! Find time for yourself! Get your checkups done by our experts.
Chlamydia - KVD №2
What is chlamydia?
Chlamydia is a common sexually transmitted infection (STI). The disease is caused by the bacterium Chlamydia trachomatis (Chlamydia trachomatis), which affects the female genital area and is the cause of non-gonococcal urethritis in men. Manifestations of chlamydia are usually minor or absent, but serious complications develop. Complications can cause irreparable damage to the body, including infertility - all this proceeds very secretly. nine0003
Manifestations of chlamydia are usually minor or absent, but serious complications develop. Complications can cause irreparable damage to the body, including infertility - all this proceeds very secretly. nine0003
Chlamydia also causes penile discharge in infected men.
Chlamydia transmission routes
Chlamydia can be transmitted through:
- vaginal or anal contact with an infected partner;
- less common with oral sex;
- use of sex toys with an infected partner;
- infection of a newborn during childbirth from a sick mother.
Absolutely all sexually active people can get chlamydia. The greater the number of sexual partners, the greater the risk of infection. The risk of infection is especially high in girls, because their cervix is not fully formed. About 75% of new cases occur in women under 25 years of age. By the age of 30, approximately 50% of sexually active women have had chlamydia. In sexually active men, the risk of infection is highest between the ages of 20 and 24. nine0003
nine0003
You cannot get chlamydia through kisses, hugs, dishes, baths, towels.
Manifestations of chlamydia
Chlamydia is very secretive. About 75% of infected women and 50% of infected men are asymptomatic. If manifestations of the disease develop, then this occurs approximately 1 to 3 weeks after infection.
In women, chlamydia first affects the cervix and urethra (urinary canal).
Manifestations:
- unusual vaginal discharge; nine0020
- pain or discomfort when urinating;
If the infection penetrates to the appendages, manifestations are possible:
- pain in the lower abdomen;
- pain in the lumbar region;
- nausea;
- slight increase in temperature;
- pain during intercourse or bleeding after it;
- bleeding between periods.
Symptoms in men:
- clear or cloudy discharge from the penis; nine0020
- pain or discomfort when urinating;
- there may be burning and itching in the area of the outlet of the urethra;
- rarely pain and/or swelling of the testicles.

Men or women who have anal sex with an infected partner can infect the rectum, resulting in inflammation, pain, discharge, or bleeding from the rectum.
Chlamydia can cause sore throat (pharyngitis) in men and women who have oral contact with an infected partner. nine0003
What complications can develop if chlamydia is not treated?
If the disease is not treated, serious short-term and persistent complications develop. Like the disease itself, complications often occur insidiously.
In women with untreated chlamydia, the infection can spread from the urethra to the fallopian tubes (the tubes that carry the egg from the ovaries to the uterus) - this causes (in 40% of cases) the development of pelvic inflammatory disease (PID). PID causes permanent damage to the fallopian tubes, uterus, and surrounding tissues. Chronic pelvic pain, infertility and ectopic pregnancy are the result of PID. nine0003
Women with chlamydia are more susceptible to HIV infection, the risk increases by almost 5 times.
To prevent serious consequences of chlamydia, an annual chlamydia screening is required for all sexually active women 25 years of age and younger. An annual examination is necessary for women over 25 who are at risk (new sexual partner, multiple sexual partners). All pregnant women should be screened for chlamydia. nine0003
Complications of chlamydia are rare in men. The infection sometimes extends to the epididymis and causes pain, fever, and, rarely, male infertility (sterility).
Rarely, chlamydial infection can cause inflammation of the joints in combination with skin lesions, inflammation of the eyes and urinary tract - this is the so-called Reiter's syndrome.
The effect of chlamydia on a pregnant woman and her child
Chlamydia in pregnant women increases the risk of miscarriage, premature detachment of the placenta. Newborns from infected mothers can get eye and lung infections. A lung infection (pneumonia) can be fatal to a newborn. nine0003
Diagnosis of chlamydia
Diagnosis includes observation of the patient's clinical symptoms, testing for chlamydia smears from the cervix, scraping from the urinary canal, the first morning portion of urine.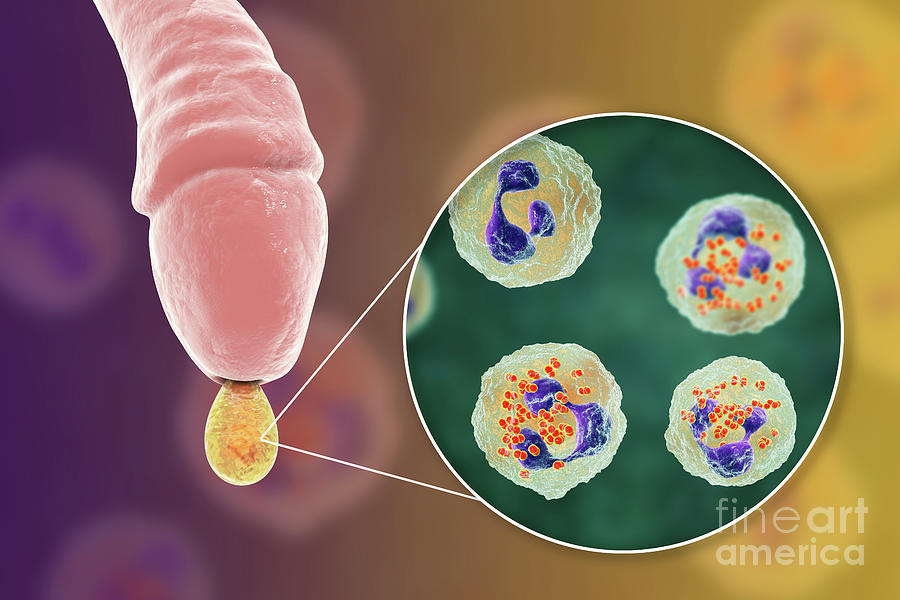 Most often, the study is carried out by PCR (polymerase chain reaction). Swabs and scrapings may cause minor discomfort.
Most often, the study is carried out by PCR (polymerase chain reaction). Swabs and scrapings may cause minor discomfort.
In addition, a blood test is performed by ELISA (enzyme-linked immunosorbent assay) for the presence of immunity to chlamydia, this auxiliary test often helps to establish an accurate diagnosis. nine0003
Chlamydia treatment
Chlamydia treatment is with oral antibiotics. To prevent re-infection, all sexual partners must be found, examined and treated. Patients with chlamydia should refrain from unprotected sex during treatment, otherwise it is possible to re-infect the sexual partner. Unfortunately, after successful treatment, re-infection with chlamydia is possible, since a strong immunity to this microorganism does not develop. Repeated infection of women with chlamydia leads to a significant increase in the risk of serious complications, including infertility. A re-examination is carried out 4 weeks after treatment. nine0003
Chlamydia prevention
The best way to prevent sexually transmitted infections is through long-term sexual contact with one healthy sexual partner.