How long until my milk comes in
Breastfeeding FAQs: Getting Started (for Parents)
Breastfeeding is natural, but it takes practice to get it right. Here's what you need to know about getting started.
When Will My Milk Come In?
For the first few days after your baby's birth, your body will make colostrum, a nutrient-rich "pre-milk." Colostrum (kuh-LOSS-trum) has many benefits, including nutrients that boost a baby's immune system and help fight infection.
For some women, colostrum is thick and yellowish. For others, it is thin and watery. The flow of colostrum is slow so that a baby can learn to nurse — a skill that requires a baby to suck, breathe, and swallow.
After 3–4 days of making colostrum, your breasts will start to feel firmer. This is a sign that your milk supply is increasing and changing from colostrum to mature milk. Your milk may become whiter and creamier, but this varies between women.
If your milk takes longer to come in, don't worry. This is normal and usually isn't a cause for concern, but let your doctor know. While babies don't need more than colostrum for the first few days, the doctor may need to make sure your baby's getting enough to eat. It can help to breastfeed often during this time to stimulate your milk production.
When Should I Begin Breastfeeding?
If possible, start nursing within an hour of your baby's birth. Babies tend to be alert in the first few hours of life, so breastfeeding right away takes advantage of this natural wakefulness. After this, newborns will sleep for most of the next 24 hours. At that point, it might be harder to get your baby to latch on.
When placed on your chest, your baby will naturally "root" (squirm toward the breast, turn the head toward it, and make sucking motions with the mouth). To breastfeed, babies latch onto the breast by forming a tight seal with the mouth around the nipple and areola (the dark part of skin around the nipple). Even if your baby doesn't latch on now and just "practices," it's still good for your baby (and you!) to get used to practicing breastfeeding.
In the first few days of life, your baby will want to feed on demand, usually about every 1–3 hours, day and night. As babies grow and their bellies can hold more milk, they may go longer between feedings.
How Can I Tell When My Baby's Ready to Nurse?
On-demand feeding means breastfeeding whenever your baby seems hungry. How can you tell? Hungry babies:
- move their head from side to side
- open their mouth
- stick out their tongue
- suck on their hands and fists
- pucker their lips as if to suck
- nuzzle against mom's breasts
- show the rooting reflex (when a baby moves their mouth in the direction of something that's stroking or touching their cheek)
Crying is a late sign of hunger. So try to nurse before your baby gets upset and harder to calm down.
To calm a crying or fussy baby before a feeding, try soothing "skin-to-skin" time. Dress your baby in only a diaper and place your little one onto your bare chest.
How Do I Get My Baby to Latch?
When you your baby shows hunger signs, follow these steps:
- Make a "nipple sandwich." Hold your breast with your hand, and compress it to make a "nipple sandwich." An easy way to remember how to hold your hand: Keep your thumb by your baby's nose and your fingers by the chin. (The thumb and fingers should be back far enough so that your baby has enough of the nipple and areola — the darker circle of skin around the nipple — to latch onto.) Compressing your breast this way lets your baby get a deep latch. Your baby's head should lean back slightly, so their chin is touching your breast.
- Get your baby to open wide. Touch or rub your nipple on the skin between your baby's nose and lips. When this happens, your baby should open wide (like a yawn) with the tongue down.
- Bring your baby to your breast. When your baby's mouth is open wide, quickly bring your baby to your breast (not your breast to your baby).
 Your baby should take as much of the areola into the mouth as possible. Your baby's nose should almost touch your breast (not press against it) and their lips should be turned out ("flanged").
Your baby should take as much of the areola into the mouth as possible. Your baby's nose should almost touch your breast (not press against it) and their lips should be turned out ("flanged").
When your baby is properly latched on, you may have a few moments of discomfort in the beginning. After that, it should feel like a tug when your baby is sucking.
To make sure you're doing it right, it's best to be observed by a lactation consultant, or someone else who knows about breastfeeding.
How Do I Know My Baby Is Getting Enough to Eat?
Your baby's diapers can help you tell if your little one is eating enough. The more your baby nurses, the more dirty diapers you'll see.
Pee
Because colostrum is concentrated, your baby may have only one or two wet diapers in the first 24 hours. After 3–4 days, look for:
- 6 or more wet diapers per day, with clear or very pale pee. Fewer wet diapers or darker pee may mean your baby's not getting enough to drink.
 If you see orange crystals in a wet diaper, call your baby's doctor. They're common in healthy, well-fed babies and usually not a cause for concern. But sometimes they're a sign that a baby isn't getting enough fluids.
If you see orange crystals in a wet diaper, call your baby's doctor. They're common in healthy, well-fed babies and usually not a cause for concern. But sometimes they're a sign that a baby isn't getting enough fluids.
Poop
A newborn's poop is thick and tarry at first, then more greenish-yellow as mom's milk comes in. After 3–4 days, look for:
- 4 or more yellow, seedy poops per day, usually one after each feeding. After about a month, babies poop less often and many may go a few days without pooping.
Your baby probably is getting enough milk if he or she:
- feeds 8–12 times a day
- seems satisfied and content after eating
- sleeps well
- is alert when awake
- is gaining weight
If you're worried that you baby isn't getting enough to eat, call your doctor.
I'm Having a Hard Time. What Can I Do?
Nursing takes time and practice. In fact, it can be one of the most challenging — and rewarding — things you do as a new mom.
While you're in the hospital, ask for help from a lactation consultant, the nursing staff, your baby's pediatrician, or your OB-GYN. When you get home, see if there's a lactation consultant in your area. You can search online at:
- United States Lactation Consultant Association
- International Lactation Consultant Association
The pediatrician will want to see your baby 24–48 hours after you leave the hospital. During this visit, the doctor will check your baby's weight and your feeding technique. If you have trouble or questions before then, call the doctor.
Whatever you do, don't let it get you down. With a little patience and some practice, breastfeeding is likely to get easier.
For more help or if you have questions, talk to a lactation consultant, your doctor, or someone who knows about breastfeeding.
When Does Breast Milk Come In & Signs It’s Coming
The look and feel of your colostrum, or early milk, is much different from your mature, later milk - which often comes in around 2 - 5 days after your baby's birth, though every mama’s timing is different.
Share this content
So, When Does Breast Milk Come In?
Though colostrum production begins as early as 16 weeks pregnant and should begin to be expressed right away after birth (with some moms even experiencing occasional leakage later in pregnancy), its look and composition differs significantly from your later breast milk. This is because colostrum, or your “first milk”, plays a much different role for your baby than your later breast milk, though both forms are incredibly important to your baby’s wellness and development. Though later breast milk may take some time to “come in” after delivery, your milk production has been in the works since early in your pregnancy, so don’t worry, mama – it’ll be here soon enough!
Moms shouldn’t expect to see large milk volumes in the first few days after birth, though most newborns lose weight during this time. Both of these things are normal and expected, and your colostrum is all your newborn needs until your later milk presents. With that in mind, your later milk – or the breast milk produced as your colostrum transitions to your mature milk – “comes in” about 2 – 5 days after your baby’s birth. “Coming in” refers to the significant increase in volume and changes in composition, though this popular term isn’t necessarily accurate. This is because your colostrum is breast milk and should be fed to your baby as soon as possible after birth. When your mature milk comes in later, however, it is accompanied by some very noticeable symptoms.
With that in mind, your later milk – or the breast milk produced as your colostrum transitions to your mature milk – “comes in” about 2 – 5 days after your baby’s birth. “Coming in” refers to the significant increase in volume and changes in composition, though this popular term isn’t necessarily accurate. This is because your colostrum is breast milk and should be fed to your baby as soon as possible after birth. When your mature milk comes in later, however, it is accompanied by some very noticeable symptoms.
Signs Milk Is Coming In
Many women, even first-time moms, know exactly when their breast milk has come in, mainly due to common indicators like:
- Breast engorgement, or the feeling of fullness, heaviness, and/or firmness.
- Swelling of the breasts.
- Breast milk leakage, particularly overnight.
- Flattened nipples and/or skin tightening or firmness around the areolas.
This initial engorgement – and the occasional discomfort that may accompany the first time your milk comes in – will dissipate as your body adjusts to a regular nursing and pumping routine. If your breasts are frequently engorged after your milk comes in, this is a sign that your body is working hard to produce milk and you may not be fully emptying your breasts after a nursing session – be sure to have a breast pump and breast milk storage bags on hand, so you can fully empty your breasts after and between breastfeeding your little one. Your pumped breast milk can be stored in the refrigerator or freezer, so you can start a stockpile for your little one – which can be especially helpful if your partner or another person, such as a babysitter, needs to feed the baby. Just be sure to read up on the latest breast milk storage guidelines and use a helpful feeding and pumping log to ensure none of your precious liquid gold goes to waste!
If your breasts are frequently engorged after your milk comes in, this is a sign that your body is working hard to produce milk and you may not be fully emptying your breasts after a nursing session – be sure to have a breast pump and breast milk storage bags on hand, so you can fully empty your breasts after and between breastfeeding your little one. Your pumped breast milk can be stored in the refrigerator or freezer, so you can start a stockpile for your little one – which can be especially helpful if your partner or another person, such as a babysitter, needs to feed the baby. Just be sure to read up on the latest breast milk storage guidelines and use a helpful feeding and pumping log to ensure none of your precious liquid gold goes to waste!
What Else Should I Know?
Though your body’s breast milk production is kicked into high gear within 30 – 40 hours after you deliver the placenta, your later milk coming in is dictated by the hormonal changes taking place in your body during this time. Because every woman – and every pregnancy – is different, there is a range of days during which breast milk may come in. With that in mind, there is evidence that skin to skin contact, initiating breastfeeding within 30 – 60 minutes after birth, and continuing to nurse early and often (or pumping or hand expressing your colostrum to feed your baby, if there are latching challenges) can positively impact your breast milk production.
Because every woman – and every pregnancy – is different, there is a range of days during which breast milk may come in. With that in mind, there is evidence that skin to skin contact, initiating breastfeeding within 30 – 60 minutes after birth, and continuing to nurse early and often (or pumping or hand expressing your colostrum to feed your baby, if there are latching challenges) can positively impact your breast milk production.
If your breasts are very engorged, it can be more difficult for your baby to latch properly. Try softening your breasts before a feeding, such as by taking a warm shower, applying a warm compress to each breast, and/or hand expressing a small volume of milk. You can also apply a cold compress – think a bag of frozen vegetables or an ice pack wrapped in a towel – to reduce swelling and discomfort. Prevent engorgement and reduce your risk of developing mastitis or encountering eventual breast milk supply issues by nursing or pumping frequently.
If you have questions about your breast milk coming in, concerns about supply, or are experiencing difficulties getting into a regular breast milk feeding routine, talk to a lactation consultant right away.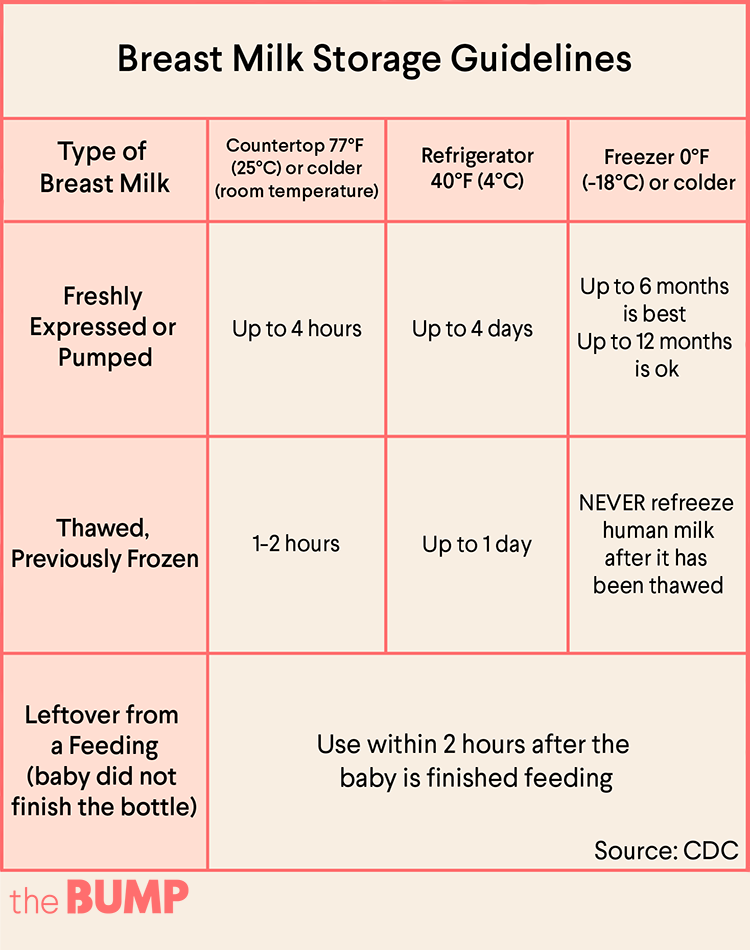 The sooner you can address any issues you may be facing, the easier it will be to minimize impact on your future breast milk production. Remember, mama, it’s common to encounter early breast milk feeding challenges – especially if you’re a first-time mom – and it may take some time for your body and hormones to adjust. After all, you just did an amazing thing by welcoming your little one into the world! The most important thing to remember is to persevere and continue finding ways to ensure your baby receives all that great liquid gold that your body is making – whether by pumping, nursing, or a combination of both. As your milk comes in and you adapt to life with a newborn, you and your baby will eventually get into a regular feeding routine. Congratulations on your new bundle of joy – and be sure to enjoy this unique bonding time together!
The sooner you can address any issues you may be facing, the easier it will be to minimize impact on your future breast milk production. Remember, mama, it’s common to encounter early breast milk feeding challenges – especially if you’re a first-time mom – and it may take some time for your body and hormones to adjust. After all, you just did an amazing thing by welcoming your little one into the world! The most important thing to remember is to persevere and continue finding ways to ensure your baby receives all that great liquid gold that your body is making – whether by pumping, nursing, or a combination of both. As your milk comes in and you adapt to life with a newborn, you and your baby will eventually get into a regular feeding routine. Congratulations on your new bundle of joy – and be sure to enjoy this unique bonding time together!
Breastfeeding a newborn | What to Expect in the First Week
The first week of a baby's life is a wonderful but hectic time, especially if you haven't breastfed before. Our breastfeeding tips will help you settle in as quickly as possible
Our breastfeeding tips will help you settle in as quickly as possible
Share this information
The first time after childbirth, mothers are often confused. The body is still recovering, and you are already starting to get to know your newborn baby. The emotional state during this period can be unstable, especially between the second and fifth day, when many women have milk 1 and at the same time postpartum depression begins 2 . In addition, people around often expect (and demand) that a woman come to her senses as soon as possible and become a “super mom”. But the best thing to do this first week is just to be with your baby and get breastfeeding going.
When should I start breastfeeding my newborn?
Try to breastfeed your baby within the first hour after birth. When the baby latch onto the breast and begins sucking rhythmically, it stimulates the mammary gland cells and starts milk production. 1 It is not for nothing that this time is called the “magic hour”!
1 It is not for nothing that this time is called the “magic hour”!
“Ideally, the baby should be placed on the mother's stomach immediately after birth so that it can immediately attach to the breast. He won't necessarily eat, but he should be able to,” explains Cathy Garbin, an internationally recognized expert on breastfeeding.
“Hold your baby and let him find the breast on his own and put the nipple in his mouth. This is called the breast-seeking reflex. On the Internet you can watch videos that show what this process looks like. If the baby does not latch onto the nipple on its own, the midwife will help to properly attach it to the breast. But for starters, it’s good to give the baby the opportunity to do it on their own. In this case, the optimal position for the mother is reclining. ”
Don't spend that special first hour of your baby's life weighing and swaddling—or at least wait until he's suckling for the first time. Enjoy hugs and close skin-to-skin contact. This promotes the production of oxytocin, the hormone of love, in you and your baby, and oxytocin plays a key role in the supply of the first breast milk - colostrum. 3
This promotes the production of oxytocin, the hormone of love, in you and your baby, and oxytocin plays a key role in the supply of the first breast milk - colostrum. 3
“As soon as the obstetricians were convinced that our son was healthy, the three of us — me, my husband and our baby — were left to give us the opportunity to get to know each other. It was a very special hour - an hour of awkwardness, turbulent emotions and bliss. During this time, I breastfed my son twice, ”recalls Ellie, a mother of two from the UK.
Did you know that breastfeeding helps to recover after childbirth? This is because oxytocin stimulates uterine contractions. In the first hours after childbirth, this contributes to the natural release of the placenta and reduces blood loss. 4
What if the birth did not go according to plan?
If you had a cesarean section or other complications during childbirth,
You can still make skin-to-skin contact with your baby and breastfeed him in the first hours after birth.
“If you can't hold your baby, have your partner do it for you and make skin-to-skin contact with the baby. This will give the baby a sense of security, care and warmth so that he can hold on until you recover, ”Katie advises.
If the baby is unable to breastfeed, it is advisable to start expressing milk as early as possible and do so as often as possible until the baby is able to feed on its own. “While breastfeeding in the first hours after birth lays an excellent foundation for the future, it is not so important,” Cathy reassures. “It is much more important to start lactation so that in the future, if necessary, you can start breastfeeding.”
To start milk production, you can express milk manually or use a breast pump that can be given to you at the hospital. 5 And with expressed precious colostrum, it will be possible to feed the child. This is especially important if the baby was born premature or weak, since breast milk is extremely healthy.
If a baby was born prematurely or has a medical condition and cannot be breastfed immediately, this is no reason not to continue breastfeeding. “I have worked with many new mothers who were unable to breastfeed their baby for the first six weeks due to preterm labor or other reasons. Nevertheless, all of them later successfully switched to breastfeeding,” says Kathy.
“I have worked with many new mothers who were unable to breastfeed their baby for the first six weeks due to preterm labor or other reasons. Nevertheless, all of them later successfully switched to breastfeeding,” says Kathy.
Does the baby latch on correctly?
Correct breastfeeding is essential for successful breastfeeding 6 , as it determines how effectively the baby will suckle milk and hence grow and develop. Latching on the breast incorrectly can cause sore or damaged nipples, so don't hesitate to ask your doctor to check that your baby is properly attached to the breast, even if you are told that everything is fine and you do not see obvious problems - especially while you are in the hospital.
“While I was in the hospital, I called the doctor at every feed and asked me to check if I was breastfeeding correctly,” says Emma, mother of two from Australia. - There were several cases when it seemed to me that everything seemed to be right, but it was painful to feed, and the doctor helped me take the baby off the breast and attach it correctly. By the time I was discharged, I had already learned to do it confidently.”
By the time I was discharged, I had already learned to do it confidently.”
When applying to the breast, point the nipple towards the palate. This will allow the baby to take the nipple and part of the areola under it into their mouth. It will be easier for him to suck if he has both the nipple and part of the areola around in his mouth. 6
“When a baby latch on properly, it doesn't cause discomfort and it causes a pulling sensation, not pain,” Cathy explains. - The baby's mouth is wide open, the lower lip may be slightly turned outward, and the upper one lies comfortably on the chest. The body language of the child indicates that he is comfortable. There isn't much milk at this early stage, so you probably won't notice your baby swallowing, but he will suckle a lot and nurse frequently."
How often should a newborn be fed?
The frequency and duration of breastfeeding in the first week can vary greatly. “The first 24 hours of life are completely different for different children. Someone sleeps a lot (after all, childbirth is tiring!), And someone often eats, says Katie. - Such a variety greatly confuses young mothers. Everyone gives different advice, so it's important to remember that every mother and child is different."
Someone sleeps a lot (after all, childbirth is tiring!), And someone often eats, says Katie. - Such a variety greatly confuses young mothers. Everyone gives different advice, so it's important to remember that every mother and child is different."
“Colostrum is thicker than mature breast milk and is produced in smaller amounts, but has many benefits. When the baby eats colostrum, he learns to suck, swallow and breathe until milk begins to flow in more volume, ”explains Cathy.
Milk usually arrives on the second or fourth day after birth. Until this time, the baby is applied to the breast 8-12 times a day (and sometimes more often!), including at night. 7 Feeding may last 10-15 minutes at this stage, or 45 minutes or even an hour, as the baby is just beginning to develop the muscles and coordination needed to suckle effectively.
“At first, the intensity of feeding is very high, often higher than many people realize, and this is shocking to most new mothers,” says Cathy. - Sometimes mom has no time to go to the toilet, take a shower and have a snack. It usually comes as a surprise."
Camille, a mother from Australia, experienced this. “The first week, Frankie ate every two hours, day and night, and each time it took half an hour to an hour to feed,” she recalls. “My husband and I were completely exhausted!”
Do I need to feed my newborn on a schedule?
The good news is that frequent feeding promotes lactation and stimulates milk production. 7 The more your baby eats, the more milk you will have. Therefore, forget about feeding your newborn on a schedule - this way he will have less chance of feeding. Try to feed your baby when he signals that he is hungry 8 :
- tossing and turning in her sleep;
- opens eyes;
- turns his head if he feels a touch on his cheek;
- sticks out tongue;
- groans;
- licks lips;
- sucks fingers;
- is naughty;
- whimpers;
- is crying.
Crying is the last sign of hunger, so when in doubt, just offer your baby the breast. If he bursts into tears, it will be more difficult to feed him, especially at first, when both of you are just learning how to do it. As your baby grows, he will likely eat less frequently and take less time to feed, so breastfeeding will seem more predictable.
Does breastfeeding hurt?
You may have heard that breastfeeding is not painful at all, but in fact, in the first days, many new mothers experience discomfort. And this is not at all surprising, given that the nipples are not used to such frequent and strong sucking.
“Breastfeeding can be uncomfortable for the first couple of days – your body and your baby are just getting used to it. If a baby eats for too long and does not latch well, the sensations are almost the same as from unworn new shoes, Cathy compares. Just as tight shoes can rub your feet, improper suckling can damage your nipples. Prevention is always better than cure, so if the pain persists after a few days of feeding, contact a lactation consultant or healthcare professional. ”
Maria, a mother from Canada, agrees: “Although my son seemed to latch onto the breast well, he damaged his nipples while feeding, and I was in pain. As it turned out, the reason was a shortened frenulum of the tongue. The breastfeeding specialists at our city clinic have been of great help in diagnosis and treatment.”
In addition, you may experience period cramps during the first few days after breastfeeding, especially if this is not your first baby. This is the so-called postpartum pain. The fact is that oxytocin, which is released during breastfeeding, contributes to further contraction of the uterus to restore its normal size. 4
When milk arrives, the breasts usually become fuller, firmer and larger than before delivery. In some women, the breasts swell, harden and become very sensitive - swelling of the mammary glands occurs. 10 Frequent breastfeeding relieves these symptoms. For more breast care tips, read our article What is Breast Swelling?
How often does the newborn urinate and defecate?
What goes into the body must go back out. Colostrum
has a laxative effect, helping to eliminate meconium - the original feces. It looks a little scary - black and sticky, like tar. 11 But don't worry, it won't always be like this. Breastfed babies usually have a slightly sweet smell of stool.
How many times a day you will need to change diapers and how the contents should look like, see below.
Day one
- Frequency: once or more.
- Colour: greenish black.
- Texture: sticky like tar.
Day two
- Frequency: twice or more.
- Colour: dark greenish brown.
- Texture: less sticky.
Day three
- Frequency: twice or more.
- Colour: greenish brown to brownish yellow.
- Texture: non-sticky.
Fourth day and then the entire first month
- Frequency: twice or more.
- Color: yellow (feces should turn yellow no later than by the end of the fourth day).
- Texture: grainy (like mustard with grains interspersed). Leaky and watery.
The baby's urine should be light yellow. On average, babies urinate once a day for the first two days. Starting around the third day, the number of wet diapers increases to three, and from the fifth day onwards, diapers have to be changed five times a day or more often. In addition, during the first few days, the weight of wet diapers increases. 11
Is the baby getting enough breast milk?
Since very little milk is produced at first,
You may feel that this is not enough for your baby. But if you feed your baby on demand, you will produce exactly as much milk as he needs. If you want to keep the process under control, be guided by the frequency of diaper changes above. If your baby soils less diapers, check with your doctor.
“For the first three or four weeks, most babies just eat and sleep. If the child is worried and constantly asks for a breast, you should consult with your doctor, ”Katie recommends.
Sometimes the baby may vomit after feeding. If the vomit is the color of milk, this is not a cause for concern. But if there are orange, red, green, brown or black blotches in it, or the child vomits with a "fountain", consult a doctor. You should also consult a doctor if the baby has a high temperature, the fontanel (soft spot on the head) has sunk, blood is found in the stool, and also if the weight recorded at birth has not recovered within two weeks. 11
But if there are no frightening symptoms and the baby is growing at a normal pace, it means that he has enough milk. Soon you will both get used to breastfeeding and establish a more stable routine.
For the next step in breastfeeding, see Breastfeeding in the First Month: What to Expect.
Literature
1 Pang WW, Hartmann PE. Initiation of human lactation: secretory differentiation and secretory activation. J Mammary Gland Biol Neoplasia 2007;12(4):211-221. - Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." G Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
- Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." G Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
2 Shashi R et al. Postpartum psychiatric disorders: Early diagnosis and management. Indian J Psychiatry . 2015; 57( Suppl 2): S 216– S 221. - Shashi R. et al., Postnatal mental disorders: early diagnosis and treatment. Indian J Saikiatri. 2015; 57(App 2):S216-S221.
3 Moberg KU, Prime DK. Oxytocin effects in mothers and infants during breastfeeding. Infant . 2013;9(6):201-206. - Moberg K, Prime DK, "The effects of oxytocin on mother and child during breastfeeding." Infant. 2013;9(6):201-206.
4 Sobhy SI, Mohame NA. The effect of early initiation of breast feeding on the amount of vaginal blood loss during the fourth stage of labor. J Egypt Public Health Assoc . 2004;79(1-2):1-12. - Sobhi SI, Moham NA, "Early initiation of breastfeeding and its effect on vaginal bleeding in the fourth stage of labor." G Egypt Public Health Assoc. 2004;79(1-2):1-2.
J Egypt Public Health Assoc . 2004;79(1-2):1-12. - Sobhi SI, Moham NA, "Early initiation of breastfeeding and its effect on vaginal bleeding in the fourth stage of labor." G Egypt Public Health Assoc. 2004;79(1-2):1-2.
5 Meier PP et al. Which breast pump for which mother: an evidence-based approach to individualizing breast pump technology. J Perinatol . 2016;36(7):493. - Meyer P.P. et al., Breastpump Selection: A Scientific Approach to Customizing Pumping Technology. J Perinatol (Journal of Perinatology). 2016;36(7):493-499.
6 Cadwell K. Latching - On and Suckling of the Healthy Term Neonate: Breastfeeding Assessment. J Midwifery & Women ’ s 2007;52(6):638-642. — Cadwell, K. , "Latching and sucking in healthy newborns: evaluation of breastfeeding." W Midwifery Women Health. 2007;52(6):638-642.
, "Latching and sucking in healthy newborns: evaluation of breastfeeding." W Midwifery Women Health. 2007;52(6):638-642.
7 Kent JC et al. Principles for maintaining or increasing breast milk production. 2012;41(1):114-121. - Kent J.S. et al., "Principles for Maintaining and Increasing Milk Production". J Obstet Ginecol Neoneutal Nurs. 2012;41(1):114-121.
8 Australian Breastfeeding Association [ Internet ]. Feeding cues ; 2017 Sep [ cited 2018 Feb ]. - Australian Breastfeeding Association [Internet], Feed Ready Signals; September 2017 [cited February 2018]
9 Jacobs A et al. S3-guidelines for the treatment of inflammatory breast disease during the lactation period. Geburtshilfe Frauenheilkd . 2013;73(12):1202-1208. - Jacobs A. et al., "Guidelines S -3 for the management of inflammatory breast disease during breastfeeding." Geburtskhilfe und Frauenheilkünde. 2013;73(12):1202-1208.
2013;73(12):1202-1208. - Jacobs A. et al., "Guidelines S -3 for the management of inflammatory breast disease during breastfeeding." Geburtskhilfe und Frauenheilkünde. 2013;73(12):1202-1208.
10 Lawrence RA, Lawrence RM. Breastfeeding: A guide for the medical profession. 7th ed. Maryland Heights MO, USA: Elsevier Mosby; 2010. 1128 p . - Lawrence R.A., Lawrence R.M., "Breastfeeding: A guide for healthcare professionals." Seventh edition. Publisher Maryland Heights , Missouri, USA: Elsevier Mosby; 2010. P. 1128.
Transitional milk | Stages of breast milk production
During the first couple of weeks after birth, the composition of breast milk changes dramatically. Learn about the amazing properties of this transitional milk.
Share this information
A newborn baby changes literally every day, and the same can be said about breast milk. With the advent of milk, the breast can increase to an impressive size, and changes occur not only on the outside, but also inside. During the first week, the milk-producing cells and the connections between them are rebuilt and prepare the breast for the upcoming feeding. 1 From now until about the end of the second week, they will produce what is called transitional milk. 2
With the advent of milk, the breast can increase to an impressive size, and changes occur not only on the outside, but also inside. During the first week, the milk-producing cells and the connections between them are rebuilt and prepare the breast for the upcoming feeding. 1 From now until about the end of the second week, they will produce what is called transitional milk. 2
“After the placenta is delivered, levels of progesterone, the pregnancy hormone, begin to decline rapidly,” explains Professor Peter Hartmann of the University of Western Australia, a leading authority on the composition of breast milk. “As progesterone levels decrease, milk synthesis increases and milk composition approaches to normal, although it takes another couple of weeks for the milk to fully mature.”
Breastmilk Stages: Intermediate Phase
If colostrum is your baby's very first food and mature milk is his main food for a long time, then transitional milk is a kind of bridge between them.
They should be considered as three different stages of milk production, not three types of milk. The main components remain unchanged throughout breastfeeding, only their quantity changes depending on the circumstances. During the transition period, the composition of milk undergoes the most significant changes, and this happens every day in accordance with the changing needs of the child.
Milk changes because it contains bioactive components, including cells, hormones and beneficial bacteria. The transition to mature milk does not happen all at once: the composition changes gradually and in strict accordance with the developmental needs of the baby. 3.4
“The amount of milk produced by the mother has a major influence on the composition of milk,” says Professor Hartman. “The composition of milk at low and higher levels of production is different.”
Transitional milk: increase in quantity
As the baby grows, it needs more food and a different ratio of nutrients. The amount of milk produced during this period also increases significantly. You can produce 600-700 ml per day, 5 which is a very impressive amount compared to the small amount of colostrum that was produced in the early days.
The amount of milk produced during this period also increases significantly. You can produce 600-700 ml per day, 5 which is a very impressive amount compared to the small amount of colostrum that was produced in the early days.
"The composition of milk in all mammals varies according to the needs of the young"
Your breasts are now in "boost" mode: your body is learning to produce the amount of milk your baby needs. The breast becomes more mature, as does the milk. Compared to colostrum, transitional milk contains more fat and lactose, a natural sugar that gives your baby energy. 2
“The level of lactose rises sharply in the first two or three days after birth,” says Prof. Hartmann, “Fat composition also changes: the content of medium-chain fatty acids C10 and C12 increases. They are an easily digestible source of energy and have antiviral properties. In addition, sodium and chloride levels are greatly reduced during this period, so that the milk has a very low salt content. ”
”
Protein: the right ratio
The protein content of breast milk does not stay the same either. There are two types of proteins in human milk: casein and whey. Under the influence of acid in the child's stomach, casein turns into a solid mass (cottage cheese) and gives a feeling of satiety for a longer time. It also has antimicrobial properties. Whey, on the other hand, is rich in antibodies and remains liquid, so it is easily absorbed, which is especially important for newborns. As the child's gastrointestinal tract strengthens, the ratio of casein to whey in milk gradually changes. If in colostrum it is about 90:10, then after a month it reaches 60:40, and after a year of breastfeeding, the balance is set at 50:50. 6
This ratio of proteins is ideal for humans, as our body grows relatively slowly and the brain is constantly growing and becoming more complex. In addition, it promotes the supply of all the essential amino acids that a child needs for the healthy development of the brain, eyes and other organs.
The amount of whey protein in human milk is significantly higher than that of other mammals. In cow's milk, the ratio of whey and casein is the opposite: 20:80 (therefore, it is not suitable for feeding children under one year old). 7
“Milk is designed to perform a specific task,” continues Professor Hartmann, “Some components are present in all milk, such as proteins and fats, but if you look at which proteins and which fats, it becomes clear which animal belongs to milk. The composition of milk in all mammals varies depending on the needs of the young.
Changing the protective properties of transitional milk
Although your baby is still very young, already in the first couple of weeks he begins to develop his own immune system, and now he needs your direct protection a little less.
The concentration of protective enzymes and antibodies in breast milk changes accordingly. The content of some substances, in particular lactoferrin (protective enzyme) and secretory immunoglobulin A (antibody), decreases, while other substances, such as the antibacterial enzyme lysozyme, on the contrary, increase. 8
8
“The protein content of milk decreases around the same time,” says Prof. Hartmann, “The synthesis of protective proteins occurs at the same rate, but they are more diluted due to increased milk production.”
The concentration of minerals such as zinc, copper and magnesium, which support the development of the child's immune system, also decreases as the immune system strengthens. 9
When breast milk becomes fully mature
During the transition period, the composition of breast milk changes significantly. By the end of the first month, it becomes fully mature. This means that the child will be able to eat them further as they grow. The composition of milk will no longer change much, no matter how long you continue breastfeeding - a few months, a year or more.
Would you like to know more? Read our free e-book Surprising Breast Milk Facts or article on mature milk.
Literature
1 Pang WW, Hartmann PE. 2 Ballard O, Morrow AL. Human milk composition: nutrients and bioactive factors. Pediatr Clin North Am 2013;60(1):49-74. - Ballard O., Morrow A.L., "Composition of breast milk: nutrients and biologically active factors." Pediatric Clean North Am. 2013;60(1):49-74. 3 Munblit D et al. Colostrum and mature human milk of women from London, Moscow, and Verona: determinants of immune composition. Nutrients. 2016; 8(11): 695. - Moonblit, D. et al., "Colostrum and mature breast milk from women in London, Moscow, and Verona: major factors in immune composition. 4 Pons SM et al. Triacylglycerol composition in colostrum, transitional and mature human milk. 9 Eur J Clin Nutr 2000;54(12):878-882. — Pons SM, "Triacylglycerol in colostrum, transitional and mature human milk". Yur J Klin Nutr. 2000;54(12):878-882. 5 Neville MC et al. Studies in human lactation: milk volumes in lactating women during the onset of lactation and full lactation. Am J Clin Nutr . 1988;48(6):1375-1386. - Neville M.S. et al., "Female Lactation Study: Milk Quantity in Lactating Women at the Beginning and Peak of Lactation." Am F Clean Nutr. 1988;48(6):1375-1386. 6 Kunz C, Lönnerdal B. Re-evaluation of the whey protein/casein ratio of human milk. 7 Martin CR et al. Review of infant feeding: key features of breast milk and infant formula. Nutrients. 2016;8(5). - Martin S.R. et al., Review of Infant Feeding Issues: Key Features of Breast Milk and Infant Formula. Nutrients. 2016;8(5). 8 Lönnerdal B et al. Longitudinal evolution of true protein, amino acids and bioactive proteins in breast milk: a developmental perspective. J Nutr Biochem. 2017;41:1-11. - Lönnerdahl B. et al., "Longitudinal evolution of true proteins, amino acids and biologically active proteins of human milk: a development perspective." G Nutr Biochem. Initiation of human lactation: secretory differentiation and secretory activation. J Mammary Gland Biol Neoplasia. 2007;12(4):211-221. - Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." F Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
Initiation of human lactation: secretory differentiation and secretory activation. J Mammary Gland Biol Neoplasia. 2007;12(4):211-221. - Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." F Mammary Gland Biol Neoplasia. 2007;12(4):211-221.  " Nutrients. 2016; 8(11): 695.
" Nutrients. 2016; 8(11): 695.  Acta Paediatr. 1992;81(2):107-112. Kunz S, Lonnerdal W. Act Pediatr.1992;81(2):107-112. - Kuntz S., Lönnerdahl B., "New Evaluation of Whey Protein/Casein in Breast Milk". Akta Pediatr. 1992;81(2):107-112.
Acta Paediatr. 1992;81(2):107-112. Kunz S, Lonnerdal W. Act Pediatr.1992;81(2):107-112. - Kuntz S., Lönnerdahl B., "New Evaluation of Whey Protein/Casein in Breast Milk". Akta Pediatr. 1992;81(2):107-112.