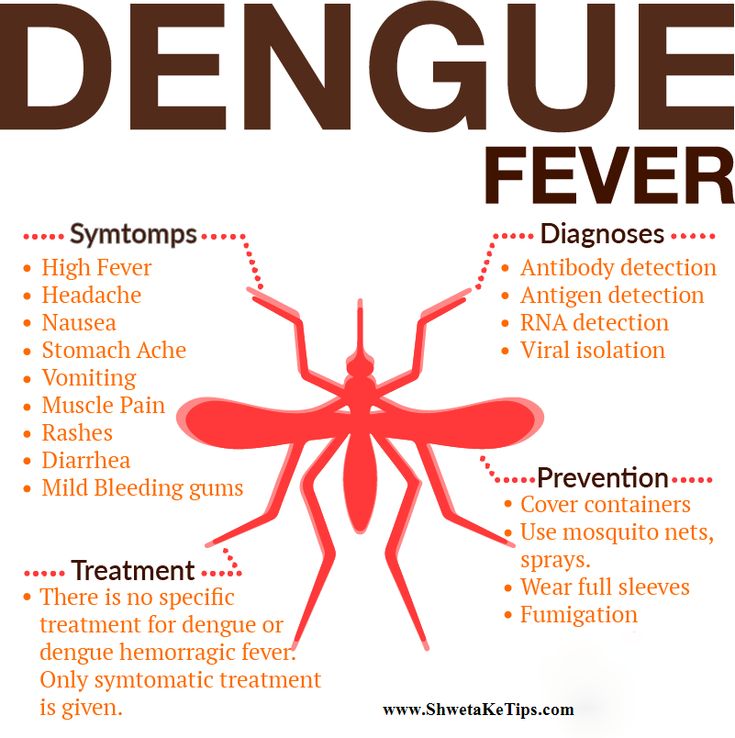
Beta blood test for pregnancy
HCG blood test - quantitative Information | Mount Sinai
Serial beta HCG; Repeat quantitative beta HCG; Human chorionic gonadotropin blood test - quantitative; Beta-HCG blood test - quantitative; Pregnancy test - blood - quantitative
A quantitative human chorionic gonadotropin (HCG) test measures the specific level of HCG in the blood. HCG is a hormone produced in the body during pregnancy.
Other HCG tests include:
- HCG urine test
- HCG blood test -- qualitative
Blood is drawn from a vein (venipuncture), usually from the inside of the elbow or the back of the hand. A needle is inserted into the vein, and the blood is collected in an air-tight vial or a syringe. Preparation may vary depending on the specific test.
How the Test is Performed
A blood sample is needed. This is most often taken from a vein. The procedure is called a venipuncture.
How to Prepare for the Test
No special preparation is needed.
How the Test will Feel
When the needle is inserted to draw blood, some people feel moderate pain. Others feel only a prick or stinging sensation. Afterward, there may be some throbbing.
Why the Test is Performed
HCG appears in the blood and urine of pregnant women as early as 10 days after conception. Quantitative HCG measurement helps determine the exact age of the fetus. It can also assist in the diagnosis of abnormal pregnancies, such as ectopic pregnancies, molar pregnancies, and possible miscarriages. It is also used as part of a screening test for Down syndrome.
Quantitative HCG measurement helps determine the exact age of the fetus. It can also assist in the diagnosis of abnormal pregnancies, such as ectopic pregnancies, molar pregnancies, and possible miscarriages. It is also used as part of a screening test for Down syndrome.
This test is also done to diagnose abnormal conditions not related to pregnancy that can raise HCG level.
Normal Results
Results are given in milli-international units per milliliter (mUI/mL).
Normal levels are found in:
- Non-pregnant women: less than 5 mIU/mL
- Healthy men: less than 2 mIU/mL
In pregnancy, HCG level rises rapidly during the first trimester and then declines slightly. The expected HCG ranges in pregnant women are based on the length of the pregnancy.
The expected HCG ranges in pregnant women are based on the length of the pregnancy.
- 3 weeks: 5 - 72 mIU/mL
- 4 weeks: 10 -708 mIU/mL
- 5 weeks: 217 - 8,245 mIU/mL
- 6 weeks: 152 - 32,177 mIU/mL
- 7 weeks: 4,059 - 153,767 mIU/mL
- 8 weeks: 31,366 - 149,094 mIU/mL
- 9 weeks: 59,109 - 135,901 mIU/mL
- 10 weeks: 44,186 - 170,409 mIU/mL
- 12 weeks: 27,107 - 201,165 mIU/mL
- 14 weeks: 24,302 - 93,646 mIU/mL
- 15 weeks: 12,540 - 69,747 mIU/mL
- 16 weeks: 8,904 - 55,332 mIU/mL
- 17 weeks: 8,240 - 51,793 mIU/mL
- 18 weeks: 9,649 - 55,271 mIU/mL
Normal value ranges may vary slightly among different laboratories. Talk to your provider about the meaning of your specific test result.
What Abnormal Results Mean
Higher than normal level may indicate:
- More than one fetus, for example, twins or triplets
- Choriocarcinoma of the uterus
- Hydatidiform mole of the uterus
- Ovarian cancer
- Testicular cancer (in men)
During pregnancy, lower than normal levels based on the gestational age may indicate:
- Fetal death
- Incomplete miscarriage
- Threatened spontaneous abortion (miscarriage)
- Ectopic pregnancy
Risks
Risks of having blood drawn are slight, but may include:
- Excessive bleeding
- Fainting or feeling lightheaded
- Blood accumulating under the skin (hematoma)
- Infection (a slight risk any time the skin is broken)
Jain S, Pincus MR, Bluth MH, McPherson RA, Bowne WB, Lee P. Diagnosis and management of cancer using serological and other body fluid markers. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 23rd ed. St Louis, MO: Elsevier; 2017:chap 74.
Diagnosis and management of cancer using serological and other body fluid markers. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 23rd ed. St Louis, MO: Elsevier; 2017:chap 74.
Jeelani R, Bluth MH. Reproductive function and pregnancy. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 23rd ed. St Louis, MO: Elsevier; 2017:chap 25.
University of Iowa Diagnostic Laboratories. Test directory: HCG - serum, quantitative. www.healthcare.uiowa.edu/path_handbook/rhandbook/test446.html. Updated February 10, 2022. Accessed March 11, 2022.
Yarbrough ML, Stout M, Gronowski AM. Pregnancy and its disorders. In: Rifai N, ed. Tietz Textbook of Clinical Chemistry and Molecular Diagnostics. 6th ed. St Louis, MO: Elsevier; 2018:chap 69.
Last reviewed on: 12/3/2020
Reviewed by: LaQuita Martinez, MD, Department of Obstetrics and Gynecology, Emory Johns Creek Hospital, Alpharetta, GA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. Editorial update 03/11/2022.
Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. Editorial update 03/11/2022.
hCG Levels | The American Pregnancy Association
HCG (Human Chorionic Gonadotropin) is often called the pregnancy hormone because it is made by cells formed in the placenta, which nourishes the egg after it has been fertilized and becomes attached to the uterine wall. Levels can first be detected by a blood test about 11 days after conception and about 12-14 days after conception by a urine test.
Typically, the hCG levels will double every 72 hours. The level will reach its peak in the first 8-11 weeks of pregnancy and then will decline and level off for the remainder of the pregnancy.
- As you get further along in pregnancy and the hCG level gets higher, the time it takes to double can increase to about every 96 hours.
- Caution must be used in making too much of hCG numbers. A normal pregnancy may have low hCG levels and result in a perfectly healthy baby. The results from an ultrasound after 5 -6 weeks gestation are much more accurate than using hCG numbers.
- An hCG level of less than 5 mIU/mL is considered negative for pregnancy, and anything above 25 mIU/mL is considered positive for pregnancy.
- An hCG level between 6 and 24 mIU/mL is considered a grey area, and you’ll likely need to be retested to see if your levels rise to confirm a pregnancy.
- The hCG hormone is measured in milli-international units per milliliter (mIU/mL).
- A transvaginal ultrasound should be able to show at least a gestational sac once the hCG levels have reached between 1,000 – 2,000 mIU/mL. Because levels can differentiate so much and conception dating can be wrong, a diagnosis should not be made by ultrasound findings until the hCG level has reached at least 2,000 mIU/mL.
- A single reading is not enough information for most diagnoses. When there is a question regarding the health of the pregnancy, multiple testings of hCG done a couple of days apart give a more accurate assessment of the situation.
- The hCG levels should not be used to date a pregnancy since these numbers can vary so widely.
- There are two common types of hCG tests. A qualitative test detects if hCG is present in the blood. A quantitative test (or beta) measures the amount of hCG actually present in the blood.
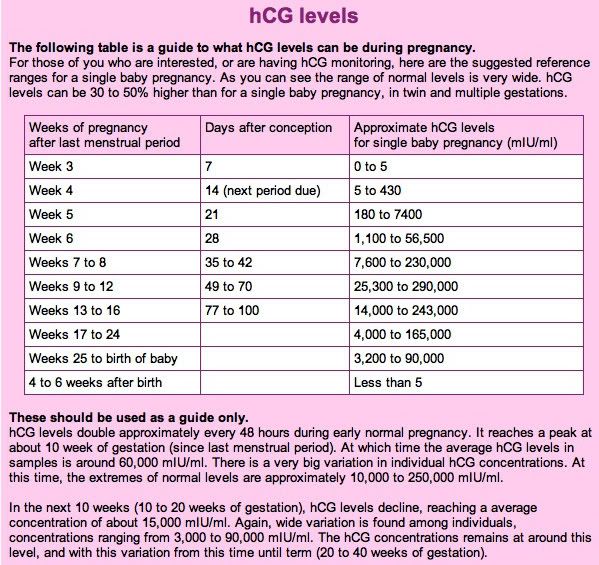
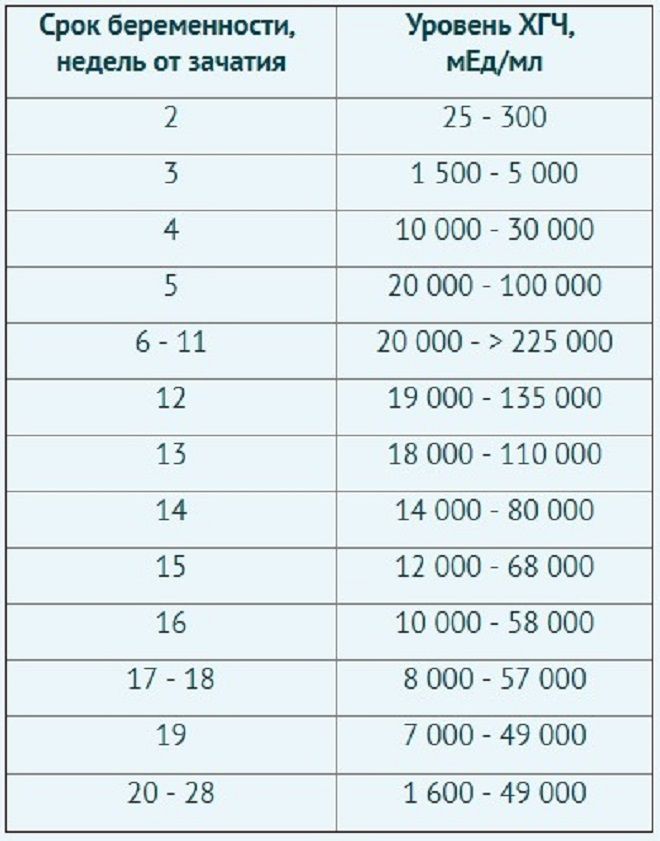
Guideline to hCG levels in weeks during pregnancy
* These numbers are just a guideline – every woman’s level of hCG can rise differently. It is not necessarily the level that matters, but rather the change in the level.
What Does a Low hCG Level Mean?
A low hCG level can mean any number of things and should be rechecked within 48-72 hours to see how the level is changing.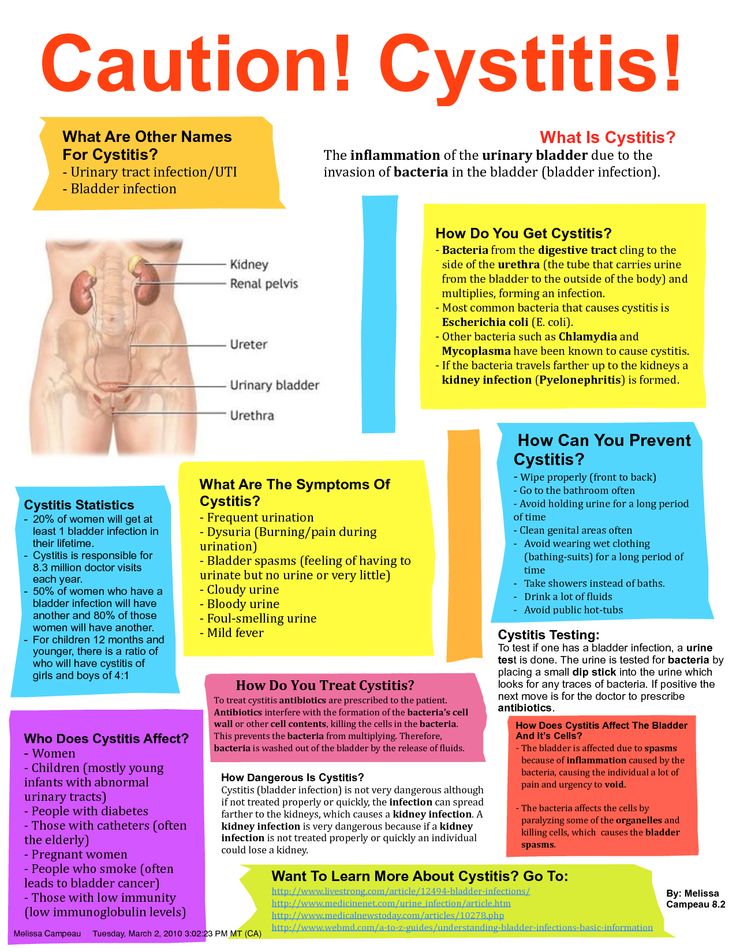 A low level can indicate:
A low level can indicate:
- Miscalculation of pregnancy dating
- Possible miscarriage or blighted ovum
- Ectopic pregnancy
Is a High hCG Level a Bad Thing?
A high level of hCG can also mean a number of things and should be rechecked within 48-72 hours to evaluate changes in the level. A high level can indicate:
- Miscalculation of pregnancy dating
- Molar pregnancy
- Multiple pregnancies
Should I Check My hCG level Regularly?
It’s not common for doctors to routinely check your hCG levels unless you are showing signs of a potential problem.
A health care provider may recheck your levels if you are bleeding, experiencing severe cramping, or have a history of miscarriage.
What Can I Expect After a Pregnancy Loss?
Most women can expect their levels to return to a non-pregnant range about 4 – 6 weeks after a pregnancy loss has occurred.
This can differentiate by how the loss occurred (spontaneous miscarriage, D & C procedure, abortion, natural delivery) and how high the levels were at the time of the loss.
Healthcare providers usually will continue to test hCG levels after a pregnancy loss to ensure they return back to <5.0.
What Can Interfere With My hCG Levels?
If you get a positive test result, you are most likely pregnant. False positives are extremely rare. However, there are some conditions that may cause a false positive, such as certain types of cancer and early miscarriage. Some antibodies may also interfere with test results.
Medications that contain hCG may interfere with hCG levels, as well.
These medications are often used infertility treatments, and your health care provider should advise you on how they may affect a test.
All other medications such as antibiotics, pain relievers, contraception or other hormone medications should not have any effect on a test that measures hCG.
Want to Know More?
- Pregnancy Calculator
- Calculating Gestation Age
- Concerns Regarding Early Fetal Development
Compiled using information from the following sources:
1. U.S. Food and Drug Administration
U.S. Food and Drug Administration
www.fda.gov
2. Bashir, I; Ihenetu, K; Miller, J.J.; Gim, M.; Lippmann, S. A Positive Pregnancy Test in the Post-Menopausal Psychiatric Patient — What to Think? Psychiatry (Edgemont). Feb. 2006.
Beta-subunit of human chorionic gonadotropin (beta-hCG)
Beta-subunit of human chorionic gonadotropin is one of the subunits of a specific hormone molecule - chorionic gonadotropin, which is formed in the shell of the human embryo. The analysis is carried out for the purpose of early diagnosis of pregnancy, detection of its complications and diagnosis of diseases associated with impaired hCG secretion.
Synonyms Russian
Beta subunit of hCG.
Synonyms English
Human Chorionic Gonadotropin, hCG, b-HCG, Quantitative hCG; Beta hCG, Total hCG, Total beta hCG.
Test method
Electrochemiluminescent immunoassay (ECLIA).
Detection range: 0. 1 - 1,000,000 IU/l.
1 - 1,000,000 IU/l.
Units
IU/l (international unit per litre).
What biomaterial can be used for research?
Venous blood.
How to properly prepare for an examination?
- Do not smoke for 30 minutes before the test.
Study Overview
Human chorionic gonadotropin (hCG) is a hormone produced in the fetal membrane of the human embryo. It is an important indicator of the development of pregnancy and its deviations. It is produced by the cells of the chorion (the shell of the embryo) immediately after it is attached to the wall of the uterus (this happens only a few days after fertilization). The embryo at this stage of pregnancy is a microscopic vesicle filled with fluid, the walls of which are made up of rapidly multiplying cells. From one part of these cells, the unborn child (embryoblast) develops, while from the cells outside the embryo, a trophoblast is formed - that part of the fetal egg, with which it is attached to the wall of the uterus. Later, the chorion is formed from the trophoblast.
Later, the chorion is formed from the trophoblast.
Chorion performs the function of nourishing the embryo, being an intermediary between the body of the mother and the child. In addition, it produces chorionic gonadotropin, which, on the one hand, affects the formation of the child, on the other hand, it specifically affects the mother's body, ensuring a successful pregnancy. The appearance of this hormone in the body of a future mother at the initial stage of pregnancy explains the importance of the test for early diagnosis of pregnancy.
Chorionic gonadotropin stimulates the secretory function of the corpus luteum of the ovaries, which should produce the hormone progesterone, which maintains the normal state of the inner lining of the uterine wall - the endometrium. The endometrium provides reliable attachment of the fetal egg to the mother's body and its nutrition with all the necessary substances.
Due to a sufficient amount of human chorionic gonadotropin, the corpus luteum, which normally exists for only about 2 weeks during each menstrual cycle, does not undergo resorption after successful conception and remains functionally active throughout the entire period of pregnancy.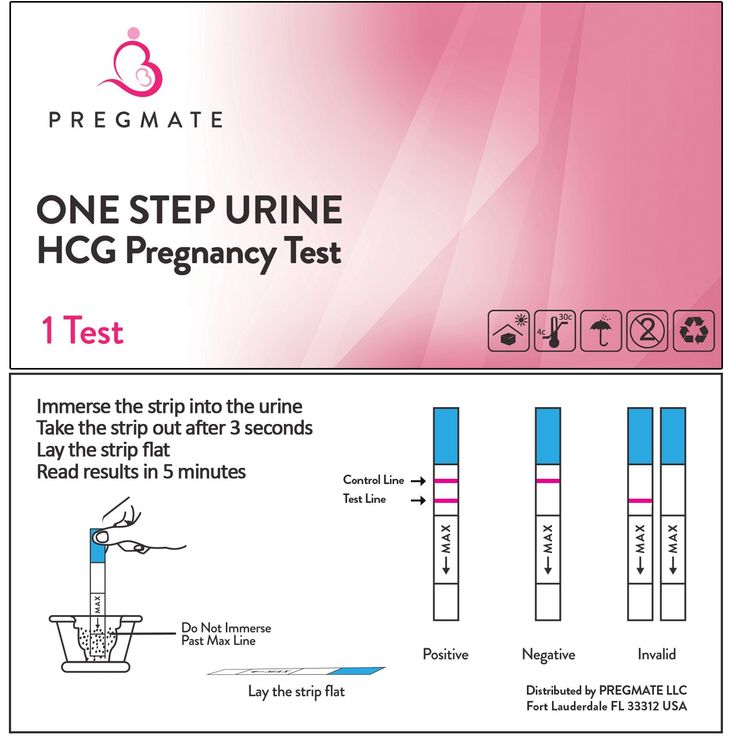 Moreover, it is in pregnant women under the influence of chorionic gonadotropin that it produces very large amounts of progesterone. In addition, CG stimulates the production of estrogens and weak androgens by ovarian cells and promotes the development of the functional activity of the chorion itself, and later the placenta, which is formed as a result of the maturation and growth of the chorionic tissue, improving its own nutrition and increasing the number of chorionic villi.
Moreover, it is in pregnant women under the influence of chorionic gonadotropin that it produces very large amounts of progesterone. In addition, CG stimulates the production of estrogens and weak androgens by ovarian cells and promotes the development of the functional activity of the chorion itself, and later the placenta, which is formed as a result of the maturation and growth of the chorionic tissue, improving its own nutrition and increasing the number of chorionic villi.
Thus, the role of human chorionic gonadotropin lies in the specific and multifaceted effect on the body of a woman and the fetus in order to ensure a successful pregnancy. Based on the analysis for chorionic gonadotropin, the presence of chorionic tissue in the woman's body is determined, and hence pregnancy.
According to its chemical structure, chorionic gonadotropin is a combination of protein and complex carbohydrates, consisting of two parts (subunits): alpha and beta. The alpha subunit of chorionic gonadotropin is completely identical to the alpha subunits of the luteinizing, follicle-stimulating and thyroid-stimulating hormones of the pituitary gland, which perform functions that are largely similar to the function of chorionic gonadotropin, but not during pregnancy. The beta subunit of chorionic gonadotropin is unique, which, on the one hand, determines the specificity of its action, and, on the other hand, allows it to be identified in biological media. In this regard, this test is called "beta-subunit of human chorionic gonadotropin (beta-hCG)".
The beta subunit of chorionic gonadotropin is unique, which, on the one hand, determines the specificity of its action, and, on the other hand, allows it to be identified in biological media. In this regard, this test is called "beta-subunit of human chorionic gonadotropin (beta-hCG)".
Knowing the level of beta-hCG in the blood, it is possible to diagnose pregnancy already on the 6-8th day after conception (in the urine, the concentration of beta-hCG reaches the diagnostic level 1-2 days later). Normally, during pregnancy between the 2nd and 5th weeks, the amount of beta-hCG doubles every 1.5 days. With multiple pregnancy, it increases in proportion to the number of fetuses. The maximum level of hCG reaches the 10-11th week, and then gradually decreases. This is due to the fact that from the beginning of the 2nd third of pregnancy, the placenta is able to independently produce enough estrogens and progesterone, with the participation of which the endometrium functions normally, regardless of the secretion of hormones in the ovarian corpus luteum.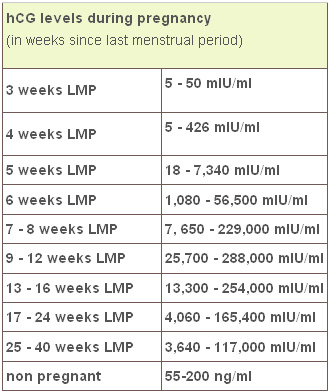 At the same time, the concentration of CG in the blood of a pregnant woman gradually decreases, and the corpus luteum can function without the effects of CG. During this period, the role of the hormone is to stimulate the production of testosterone in the fetus, which is necessary for the normal development of the external genital organs of the embryo.
At the same time, the concentration of CG in the blood of a pregnant woman gradually decreases, and the corpus luteum can function without the effects of CG. During this period, the role of the hormone is to stimulate the production of testosterone in the fetus, which is necessary for the normal development of the external genital organs of the embryo.
Thus, during pregnancy, the level of beta-hCG in the blood first increases and then decreases. According to this indicator, one can judge the successful course of pregnancy and identify violations of the development of the fetus. The test for hCG in the blood is the most reliable method for determining pregnancy in the early stages. HCG appears in the body of a woman from 6-8 days after fertilization. A common rapid pregnancy test that every woman can use at home is also based on measuring hCG in the urine.
Below normal hormone levels at various stages of fetal development suggest ectopic pregnancy, fetal growth retardation, threatened miscarriage, non-progressive pregnancy, or placental insufficiency. The reason for the increased content of beta-hCG may be toxicosis, diabetes mellitus, or an incorrectly set gestational age. A high level of the hormone after a mini-abortion indicates a progressing pregnancy.
The reason for the increased content of beta-hCG may be toxicosis, diabetes mellitus, or an incorrectly set gestational age. A high level of the hormone after a mini-abortion indicates a progressing pregnancy.
Determining the level of hCG is included in the triple test study, the results of which can be used to judge some anomalies in the development of the fetus, but an accurate diagnosis cannot be made. The study only allows you to classify a woman as a risk group for this pathology. In this case, further investigation is necessary. In non-pregnant women, CG is normally absent, but it can be secreted by some abnormal chorion-derived tissues (hydatidiform mole, chorionepithelioma) and some other tumors.
What is research used for?
- For the diagnosis of pregnancy, including multiple, ectopic and non-developing.
- To monitor the progress of pregnancy.
- To detect fetal growth retardation, threatened miscarriage, placental insufficiency.
- For the diagnosis of amenorrhea.
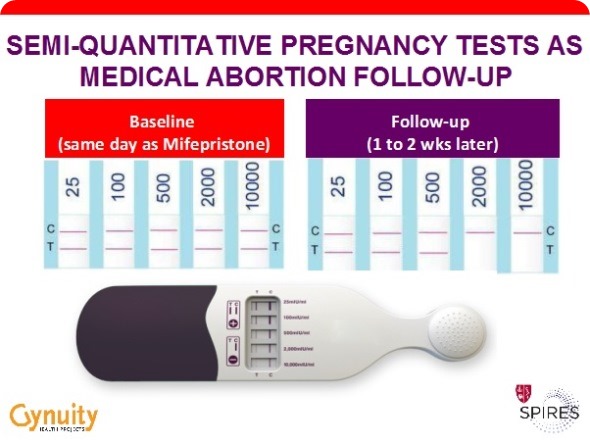
- To monitor the effectiveness of induced abortion.
- As part of a comprehensive examination to identify fetal malformations.
- For the diagnosis of CG-producing tumors.
When is the test ordered?
- If pregnancy is suspected, in particular multiple pregnancy.
- When monitoring the progress of pregnancy.
- When there is an assumption about a complication during pregnancy: fetal growth retardation, the threat of spontaneous abortion, non-developing or ectopic pregnancy, chronic placental insufficiency.
- Confirm successful induced abortion if necessary.
- With a comprehensive examination to identify fetal malformations.
- When finding out the reason for the absence of menstruation (amenorrhea).
- When is the diagnosis of tumors producing hCG.
What do the results mean?
Reference values
| Floor | Week of pregnancy (from conception) | Reference values |
|
Female | Not pregnant | Less than 5 IU/L |
| 3 weeks | 5. | |
| 4 weeks | 9.5 - 750 IU/L | |
| 5 weeks | 217 - 7138 IU/L | |
| 6 weeks | 158 - 31795 IU/l | |
| 7 weeks | 3697 - 163563 IU/L | |
| 8 weeks | 32065 - 149571 IU/l | |
| 9 weeks | 63803 - 151410 IU/L | |
| 10 weeks | 46509 - 186977 IU/L | |
| 11-12 weeks | 27832 - 210612 IU/L | |
| 13-14 weeks | 13950 - 62530 IU/L | |
| 15 weeks | 12039 - 70971 IU/L | |
| 16 weeks | 9040 - 56451 IU/L | |
| 17 weeks | 8175 - 55868 IU/L | |
| 18 weeks | 8099 - 58176 IU/L | |
| Male |
| Less than 5 IU/L |
Causes of high beta-hCG levels
In the absence of pregnancy, the result of the beta-hCG test should be negative.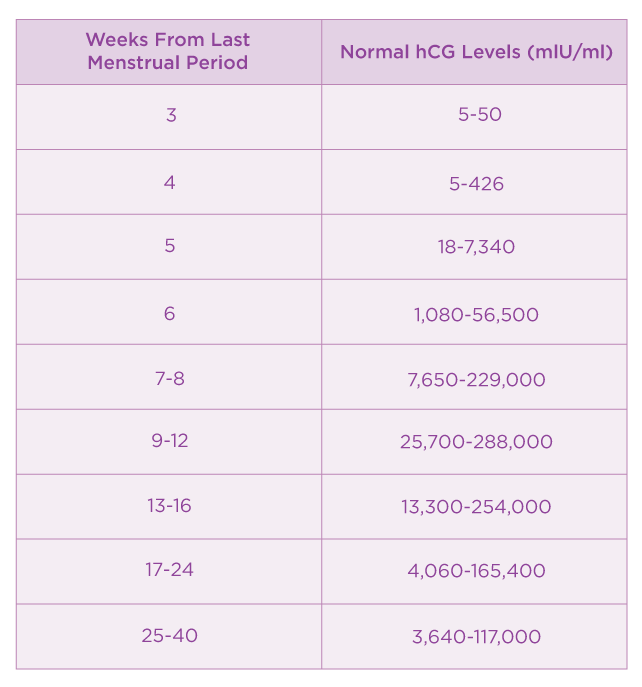 The detection of beta-hCG suggests that at least 5-6 days have passed since fertilization. Between the 2nd and 5th weeks of pregnancy, during its normal course, the level of beta-hCG doubles every 1.5 days and soon reaches its maximum. Then it starts to slowly decline. The results of the analysis are compared with the normal values for each gestational age. For a correct interpretation of the results, it is necessary to know exactly when the conception occurred.
The detection of beta-hCG suggests that at least 5-6 days have passed since fertilization. Between the 2nd and 5th weeks of pregnancy, during its normal course, the level of beta-hCG doubles every 1.5 days and soon reaches its maximum. Then it starts to slowly decline. The results of the analysis are compared with the normal values for each gestational age. For a correct interpretation of the results, it is necessary to know exactly when the conception occurred.
In pregnant women:
- multiple pregnancies (the rate increases in proportion to the number of fetuses),
- toxicosis,
- prolonged pregnancy,
- maternal diabetes mellitus,
- fetal malformations,
- taking synthetic hormones.
Not pregnant:
- hCG-producing tumors,
- surgical abortion (first 4-5 days after the procedure),
- taking hCG preparations.
Causes of low beta-hCG levels (during pregnancy):
- ectopic or non-developing pregnancy,
- fetal growth retardation,
- threatened miscarriage,
- chronic placental insufficiency,
- fetal death (in the 2nd-3rd trimester of pregnancy).
What can influence the result?
- When diagnosing pregnancy, taking the test too early - when less than 5 days have passed since conception - can lead to a false negative result.
Also recommended
- Alpha-fetoprotein (alpha-FP)
- Antiphospholipid antibodies IgG
- Antiphospholipid antibodies IgM
- Placental lactogen
- Free estriol
- Pregnancy - Prenatal screening for trisomies of the first trimester of pregnancy (Down syndrome), PRISCA
- Plasma pregnancy-associated protein A (PAPP-A)
- Pregnancy - Prenatal screening for trisomies of the second trimester of pregnancy, PRISCA
- Antibodies to steroid-producing cells of the placenta
Who orders the examination?
General practitioner, obstetrician-gynecologist, oncologist.
Literature
- Handbook of Clinical Laboratory Testing During Pregnancy, edited by Ann M.
 Gronowski. Springer-Verlag LLC, New York, 2004
Gronowski. Springer-Verlag LLC, New York, 2004 - Prenatal Diagnosis in Obstetric Practice. M. J. J. Whittle, Blackwell Publishers 1995
- Endocrinology of Pregnancy. Fuller W. Bazer, Humana Press 1998
- Blood Biochemistry. N J Russell, G M Powell, J G Jones, P J, Winterburn and J M Basford, Croom Helm, London and Canberra, 1982
- Blood Chemistry and CBC analysis-Clinical Laboratory Testing from a Functional Perspective. Rychard Weatherby N.D and Scott Fergusson, N.D., Bear Mounting Publishing, 2002.
- Tietz Clinical Guide to Laboratory Tests. Alan H. B. Wu, Saunders/Elsevier, 2006
- Laboratory and Diagnostic Tests. Joyce LeFever Kee - Pearson, Prentice Hall, 8th Edition 2010
- District Laboratory Practice in Tropical Countries. Monica Cheesbrough, Cambridge University Press, second edition, 2005.
- Clinical Chemistry. A Laboratory Perspective. Wendy L. Arneson, Jean M. Brickell, F.A. Davis Company, 2007
- Clinical Chemistry.
 Michael L. Bishop, Edward P. Fody, Larry E. Schoef, Lippincott Williams & Wilkins, 2005
Michael L. Bishop, Edward P. Fody, Larry E. Schoef, Lippincott Williams & Wilkins, 2005
Blood test for hCG (beta-hCG)
Benefit from the knowledge of our specialists
- Home page
- Knowledge
Return to the list of articles
21 janvāris 2022 | 3.5 minutes of reading
Beta-hCG (human chorionic gonadotropin) is one of the most important hormones in a woman's body, as it is responsible for regulating hormonal processes during gestation. It is produced by the tissue of the chorion (embryo membrane) after implantation and maintains the existence of the corpus luteum until the fetus-placenta complex is formed. It also ensures the synthesis of another important hormone, progesterone. An analysis for beta-hCG not only determines pregnancy, but also allows you to identify complications.
How to test for beta hCG?
HCG enters the bloodstream and is then excreted in the urine, so pregnancy can be diagnosed by a high level of hCG in the woman's blood or urine.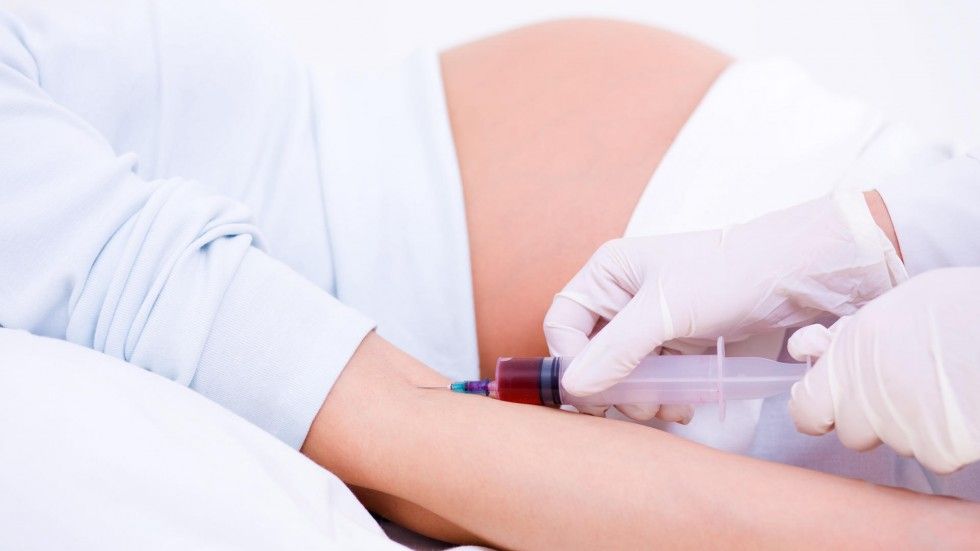 Most women use the fastest method - a urinalysis. This can be done as early as two weeks after conception, but the test is not the most accurate. The result of the home test must later be confirmed in the laboratory and a blood sample taken for analysis. A blood test for beta-hCG during pregnancy, such as one done at a fertility clinic, is by far the more sensitive method with almost 100% certainty.
Most women use the fastest method - a urinalysis. This can be done as early as two weeks after conception, but the test is not the most accurate. The result of the home test must later be confirmed in the laboratory and a blood sample taken for analysis. A blood test for beta-hCG during pregnancy, such as one done at a fertility clinic, is by far the more sensitive method with almost 100% certainty.
Do you have questions? Contact us!
When should I test for beta hCG?
Many women ask when to test for beta-hCG in order to get a reliable result. The analysis should be done no earlier than the expected date of menstruation and preferably 10-14 days after the expected time, then it gives the most reliable result.
How to determine the gestational age?
Pregnancy after in vitro fertilization and natural conception is counted from the first day of the last menstruation. As a result of hormonal stimulation used prior to embryo transfer, changes in the menstrual cycle are possible, in which case the day of ovarian puncture and fertilization is considered the day of ovulation. From this point, 14 days must be subtracted to obtain the theoretical start of the cycle, from which the gestational age after in vitro fertilization is calculated.
From this point, 14 days must be subtracted to obtain the theoretical start of the cycle, from which the gestational age after in vitro fertilization is calculated.
How should hCG levels rise? Standards and Interpretation of Results
Beta-hCG levels typically double every 2 days (48 hours). The highest level of beta-hCG in the blood for a period of 10-12 weeks, after which it begins to gradually decline. This is a natural condition and is not associated with a risk of pregnancy loss, unless the hormone level is below 5 mU / ml.
Beta-hCG level by week of pregnancy (single fetus):
| 3 weeks of pregnancy | 5.8 - 71.2 Med/ml | |
|---|---|---|
| 4 weeks Breeding weeks | 158 - 31 795 honey/ml | |
| 7 weeks of pregnancy | 3 697 - 163 563 honey/ml | |
| 8 weeks of pregnancy | 32 065 - 149 571 honey/ml honey/ml of honey/ml of honey/ml of honey/ml of honey/ml of honey/ml weeks of pregnancy | 63 803-151 410 Med/ml |
| 10 weeks of pregnancy | 46 509-186 977 Med/ml |
Analysis for beta-HCH and detection of anomalies
Beto-HSE level, MASE BETHERS, MASE TREATIONS, MASE OF THE PROBLEMENTION, MASE OF THE PROBLEMENTIONS.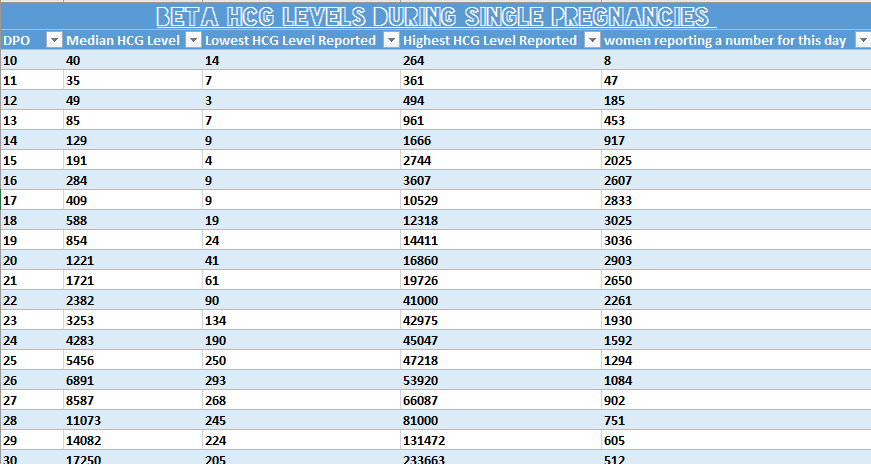
 8 - 71.2 IU/L
8 - 71.2 IU/L