Belly band for diastasis recti
Diastasis Recti Splint | Abdominal Binder Post Pregnancy Stomach Wrap
SKU: 08W0101XS
Why You Need This Abdominal Binder & Compression Belly Band
There are a number of situations where an abdominal wrap is an effective garment. A binder brace for the stomach applies compression to your low back as well as your upper and lower abdomen. The compression and support provided have a number of benefits that make this belly band great for treating a variety of things, including:
-
Diastasis recti (stomach muscle separation)
- Early stage abdominal hernias or post hernia surgery
-
Pregnancy-related discomfort or pain
-
Abdominal muscle strain or cramping
-
Weak abdominal muscles
-
Post-surgical incisions
-
Back pain
-
Bladder problems
Some examples of post-surgical care include after liposuction, hysterectomy or tummy tuck surgery, postnatal (after your baby is born), especially if you had a C-section or multiple birth delivery, or following hernia surgery (see more hernia supports).
But remember, it’s important to consult with your doctor or physical therapist about using abdominal supports after surgery, as splinting isn’t right for everyone.
Diastasis Recti Splint for Abdominal Support During & After Pregnancy
Pregnancy puts a lot of extra pressure on your belly, which occasionally causes the muscles in your abdominal wall to lose their shape, pull apart, and separate, also known as diastasis recti. When your stomach muscles separate, your abdominal organs only have a thin band of connective tissue in front to hold them in place. In some rare, extreme cases this thin tissue may tear, and your organs may poke out of the opening, which is called a hernia.
The muscle opening often shrinks after giving birth, but research shows some women with diastasis recti experience symptoms even up to a year postnatal. Combined with exercise, this elastic bandage provides great diastasis recti prevention and lightweight support for expecting mothers.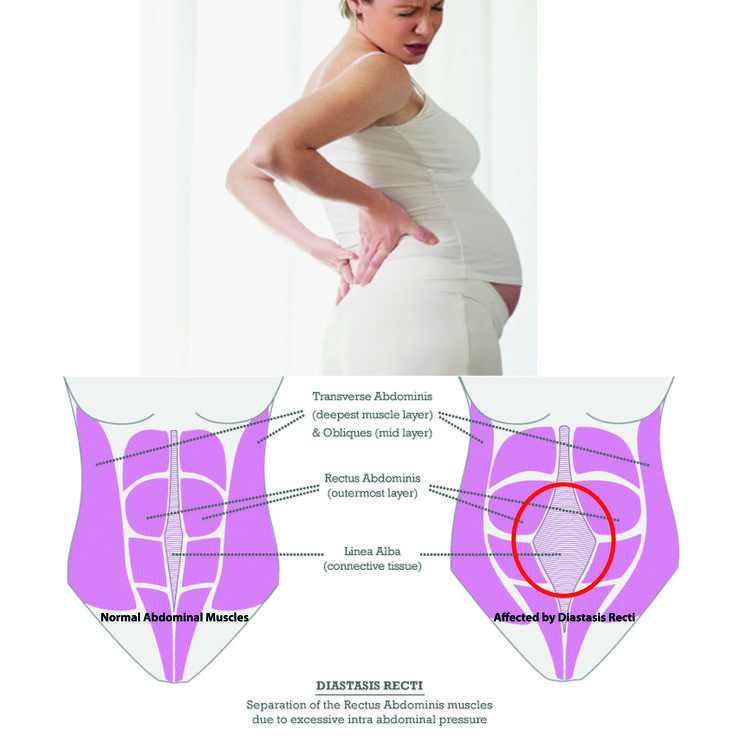
Looking for heavy-duty support during pregnancy? Check out BraceAbility’s full line of maternity braces.
How Do I Know If I Have Diastasis Recti?
There will likely be a bulge or “pooch” in the middle of your belly. You might only notice it while your abdominal muscles are tense, such as during coughing.
Diastasis recti can also occur among middle-aged and older men with abdominal obesity, as well as men who yo-yo diet, do sit-ups wrong, or weight lift incorrectly. (Use our quick and easy BMI calculator to find out if you’re overweight or obese!)
What Is an Abdominal Hernia? (Do I Have One?)
An abdominal hernia refers to a protrusion of your intestine through an opening or weak area of the abdominal wall. While this does cause a noticeable bulge, it does not typically cause a lot of pain.
A hernia can occur in a number of places on your body, with the hernia’s classification depending upon where—one that develops around your belly button is known as an umbilical hernia, while an inguinal hernia might appear in the groin area, for example. Learn the difference between an abdominal strain and a hernia.
Learn the difference between an abdominal strain and a hernia.
Thanks to the versatility of this abdominal hernia brace, it can help whether you are in need of an abdominal binder for an umbilical hernia or a femoral hernia in the leg.
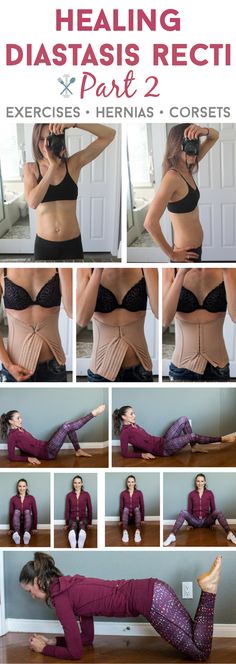
4 Reasons Why People Love This Postpartum Abdominal Support Band
This stomach tightening girdle has several transformative features that make it stand out from other abdominal support braces. Following we list the top 4 reasons why people love this compression truss belt.
-
Entire Binder is Fastener Compatible for Adjustable Compression
With just one fastener closure, this recovery wrap is a breeze to apply. Without fraying the fabric the medical-grade, fastener strip can be applied anywhere on this belt for custom support and compression. Many users describe the flexible fit as being so comfortable you forget you’re even wearing an abdominal wrap. It also helps hold in excess or hanging stomach fat like a girdle, providing a slight slimming effect to your belly.

-
Made of Non-Slip, Moisture-Wicking Material
Perhaps the best feature of this tummy separation repair splint is the non-slip, moisture-wicking, and lightweight foam material it’s specially engineered out of. The foam-like interior is smooth and soft against your skin for optimal comfort.
This belly binder is hypoallergenic, neoprene, and latex-free, which is perfect if you suffer from allergies. The same medical-grade nylon / spandex fabric is also used for BraceAbility’s non-slip knee wrap.
How Does the Moisture-Wicking Material Work?
The sweat-resistant material is specially designed to release moisture and heat, making this tummy splint a cool and comfortable abdominal brace for a variety of athletes.
-
Exercise Friendly
This body bandage is perfect if you’re looking to maintain an active lifestyle but need extra support around your core while walking, running, or working out.
The moisture-wicking, non-slip fabric keeps your athletic abdominal support in place even after you break a sweat.
-
Helps Diminish Back Pain
In addition to speeding up your recovery process, the compression also helps transfer stress away from your lumbar spine, diminishing lower back pain and protecting against further damage. The back support sleeve also promotes better posture, which in and of itself can help ease pain.
Frequently Asked Questions About This Non-Slip Stomach Wrap for Diastasis Recti
-
Who can wear it? With sizes ranging from XS to Large, anyone from petite to plus size females and males can wear this abdominal binder.
-
How do I know what size to get? Using a fabric tape measure, stand up and measure the circumference of your waist at its smallest point. To get the most accurate measurements, we recommend having a close family member or friend assist you. Refer to our sizing graphic in the photos above to choose the right size. (Click here to see BraceAbility’s full line of plus-size bariatric supports!)
-
What conditions does this abdominal support brace treat? This abdominal trainer helps fix and provide support for rectus diastasis (stomach separation), lumbar pain, and abdominal muscle strain / injury.
 The splint also promotes healing following childbirth, hysterectomy, gastroplasty, liposuction, abdominoplasty, and coolsculpting.
The splint also promotes healing following childbirth, hysterectomy, gastroplasty, liposuction, abdominoplasty, and coolsculpting. -
How do I put it on? While standing, simply wrap the belly band around your core and secure with fasteners once you’ve reached a nice, snug fit.
-
Can I wear this stomach wrap over my shirt? Yes. It can fit comfortably under or over shirts.
-
How tall is this support? XS 8” tall, S 8" tall, M 9" tall, and L 10".
-
What material is this binder made of? The material is a proprietary hydrophilic, open cell foam joined to quality, specially engineered, medical grade nylon / spandex fabrics. It is hypoallergenic, latex-free, and neoprene-free.
-
When should I wear this? This tummy binder can be comfortably worn all day while sitting, standing, and during physical activity. However, you should consult with your doctor before wearing any abdominal support for extended periods of time, such as sleeping.

-
Washing Instructions: We recommend hand washing this diastasis recti splint in warm water with mild soap. Allow the binder to air dry completely before reapplying.
-
Other features:
- Color: Black.
Diastasis Recti (Abdominal Separation): Symptoms & Treatment
Overview
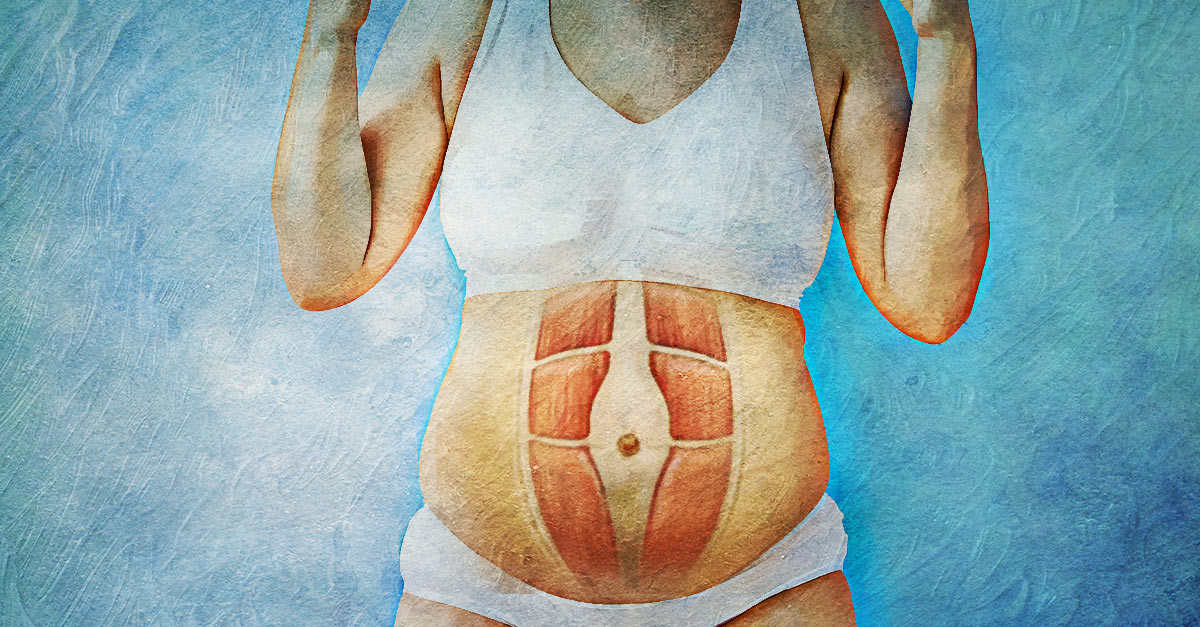
Diastasis recti happens when a person's abdomen stretches during pregnancy and creates a gap in the abdominal muscles.What is diastasis recti?
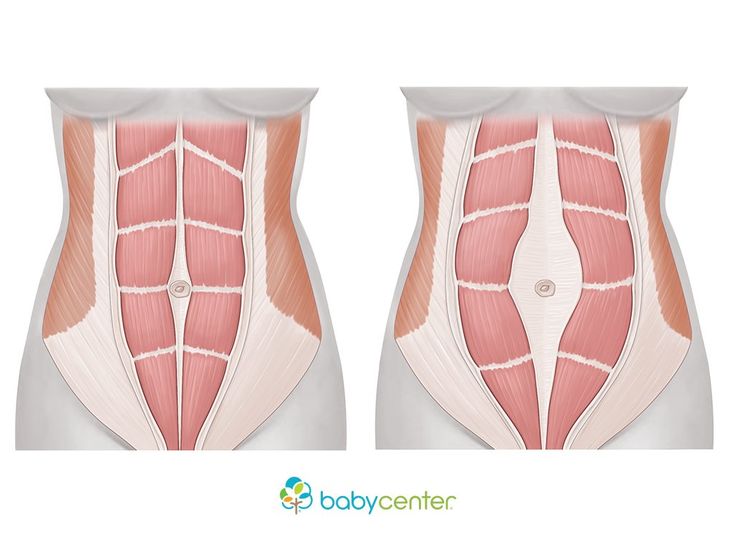
Diastasis recti (diastasis rectus abdominis or diastasis) is the separation of the rectus abdominis muscles during and after pregnancy. The rectus abdominis runs vertically along the front of your stomach. It's frequently referred to as someone's "six-pack abs." It's divided into left and right sides by a band of tissue called the linea alba that runs down the middle. As your uterus expands during pregnancy, the abdominals are stretched and the linea alba thins and pulls apart. This band of tissue gets wider as it's pushed outward.
This band of tissue gets wider as it's pushed outward.
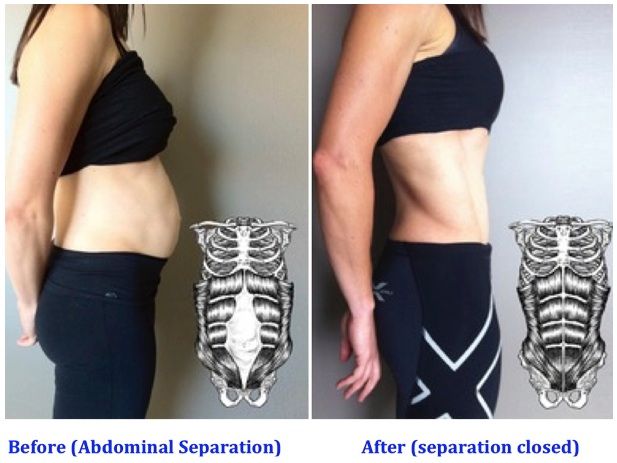
Once you deliver your baby, the linea alba can heal and come back together. It's highly elastic and retracts backs (like a rubber band). When the tissue loses its elasticity from being overstretched, the gap in the abdominals will not close as much as it should. This is diastasis recti.
If you have diastasis, your belly may appear to stick out just above or below the belly button, making you appear pregnant months or years after giving birth.
Why does diastasis recti happen?
Pregnancy puts a lot of pressure on your abdomen (abs). The abdomen is made up of left and right ab muscles and a thin band of connective tissue (linea alba) in between. They are pushed outward and stretched to make room for the growing baby. Diastasis recti occurs when the linea alba is overstretched and doesn't come back together. The left and right sides of the abdominals stay separated. It's also referred to as an "ab gap" or abdominal separation.
Who gets diastasis recti?
Diastasis recti is most common in pregnant and postpartum women (it can also be seen in men and infants). Diastasis recti usually develops in the third trimester. There is increased pressure on the abdominal wall because the baby is growing quickly during this time. Most people don't notice diastasis recti until the postpartum period.
How common is diastasis recti?
Diastasis recti is extremely common in those who are pregnant and during the postpartum period. It affects 60% of people. It usually resolves itself within eight weeks of delivery. About 40% of those who have diastasis recti still have it by six months postpartum.
Symptoms and Causes
What are the symptoms of diastasis recti?
Most people don't notice signs of diastasis recti until they are postpartum. You can have diastasis recti during pregnancy, but it's hard to distinguish because your abdomen is stretched.
Common signs of diastasis recti during the postpartum period are:
- A visible bulge or "pooch" that protrudes just above or below the belly button.

- Softness or jelly-like feeling around your belly button.
- Coning or doming when you contract your ab muscles.
- Difficulty lifting objects, walking or performing everyday tasks.
- Pain during sex.
- Pelvic or hip pain.
- Low back pain.
- Poor posture.
- Urine leaking when you sneeze or cough.
- Constipation.
- Feeling weak in your abdominals.
What does diastasis recti feel like?
Diastasis recti is not painful. You may feel pain associated with some of the side effects of diastasis, but the ab separation itself doesn't hurt. You may feel weakness in your core when doing once easy tasks, like lifting a laundry basket. Some people feel a jelly-like texture in the space between the left and right abdominals when contracting the ab muscles.
How do I know if I have diastasis recti?
There are some common signs that can signal you have diastasis recti. One of the most common signs of diastasis recti is a bulge in your midsection that doesn't go away, even after exercising or losing weight gained during pregnancy. Another sign is that your belly cones or domes when you lean back on a chair or get up out of bed. You can check for diastasis recti on your own, but it is always a good idea to speak with your healthcare provider about your symptoms.
Another sign is that your belly cones or domes when you lean back on a chair or get up out of bed. You can check for diastasis recti on your own, but it is always a good idea to speak with your healthcare provider about your symptoms.
What are the risk factors for developing diastasis recti?
Several factors can increase your risk for developing diastasis recti:
- Having multiple pregnancies (especially back-to-back).
- Being over 35 years old.
- Having multiples (such as twins or triplets).
- Having a heavy or big baby.
- Being extremely petite.
- Vaginal delivery. Pushing can increase abdominal pressure.
Diagnosis and Tests
How is diastasis recti diagnosed?
Your healthcare provider will evaluate if diastasis is present, where it's located and how severe it is. Diastasis recti can occur above the belly button, below the belly button and at the belly button.
Your provider will use their hands and fingers to feel the abdominal area for gaps and muscle tone. Some providers may use ultrasound, measuring tape or a tool called a caliper for a more accurate measurement. This exam typically occurs at your postpartum appointment before being cleared for exercise.
Some providers may use ultrasound, measuring tape or a tool called a caliper for a more accurate measurement. This exam typically occurs at your postpartum appointment before being cleared for exercise.
An abdominal gap wider than 2 centimeters is considered diastasis recti. Diastasis recti is also measured in finger widths, for example, two or three fingers' separation.
Your healthcare provider may recommend movements for diastasis recti or they may refer you to a specialist for additional treatment.
How do I test myself for diastasis recti?
You can test yourself for diastasis recti:
- Lie on your back with your knees bent and feet flat on the floor.
- Lift your shoulders slightly off the ground, keeping one hand behind your head for support. Almost like you are doing a sit-up. Look down at your belly.
- Move your other hand above your belly button area, palms down and fingers towards your toes.
- Use your fingers to feel for a gap between the abs.
 See how many fingers can fit in the gap between your right and left abdominals.
See how many fingers can fit in the gap between your right and left abdominals.
If you feel a gap of two or more finger widths, discuss your concerns with your healthcare provider. They should confirm diastasis recti with a proper diagnosis and recommend appropriate care.
Management and Treatment
How can I fix diastasis recti?
To fix diastasis recti, you'll need to perform gentle movements that engage the abdominal muscles. Before starting an exercise program, be sure it's safe for diastasis recti. Work with a fitness professional or physical therapist who has experience with diastasis recti. They can create a treatment plan to make sure you are performing the movements correctly and progressing to more challenging movements at the right time.
Certain movements will make abdominal separation worse. During the postpartum period, there are some modifications you should make:
- Avoid lifting anything heavier than your baby.
- Roll onto your side when getting out of bed or sitting up.
 Use your arms to push yourself up.
Use your arms to push yourself up. - Skip activities and movements that push your abdominals outward (like crunches and sit-ups).
Some people use binding devices (elastic belly bands) to help hold their belly in and support the lower back. Wearing binders can't heal diastasis recti and will not strengthen your core muscles. It can be a good reminder of your diastasis recti and promote good posture.
Can you fix diastasis recti without surgery?
Yes, it's possible to fix diastasis recti without surgery. Surgery is rarely performed to fix diastasis recti. Healthcare providers will recommend physical therapy or at-home exercises to help heal diastasis before surgical methods. Surgery is performed in cases of hernia (when an organ pushes through the linea alba) or if a woman wants diastasis recti surgery (a tummy tuck).
What are the best exercises for diastasis recti?
The best exercises for diastasis recti are those that engage the deep abdominals. Most diastasis recti exercises involve deep breathing and slow, controlled movements. Unfortunately, many of the most common ab exercises (like crunches) can worsen your diastasis. Before starting abdominal exercises, ask your healthcare provider to check you for diastasis recti.
Most diastasis recti exercises involve deep breathing and slow, controlled movements. Unfortunately, many of the most common ab exercises (like crunches) can worsen your diastasis. Before starting abdominal exercises, ask your healthcare provider to check you for diastasis recti.
What movements make diastasis recti worse?
Any movement that bulges the abdominal wall forward can cause more damage to your diastasis recti. Everyday movements like getting out of bed or up off a chair can worsen diastasis. Try to be mindful about how you are using your abdominals as you go about your day.
These exercise movements should be avoided if you have diastasis recti:
- Crunches or sit-ups of any kind.
- Planks or push-ups (unless using modifications).
- Downward dog, boat pose and other yoga poses.
- Double leg lifts, scissors and other Pilates moves.
- Any exercise that causes your abdominals to bulge, cone or dome.
Prevention
How do I prevent diastasis recti?
Some abdominal separation is normal and expected with pregnancy.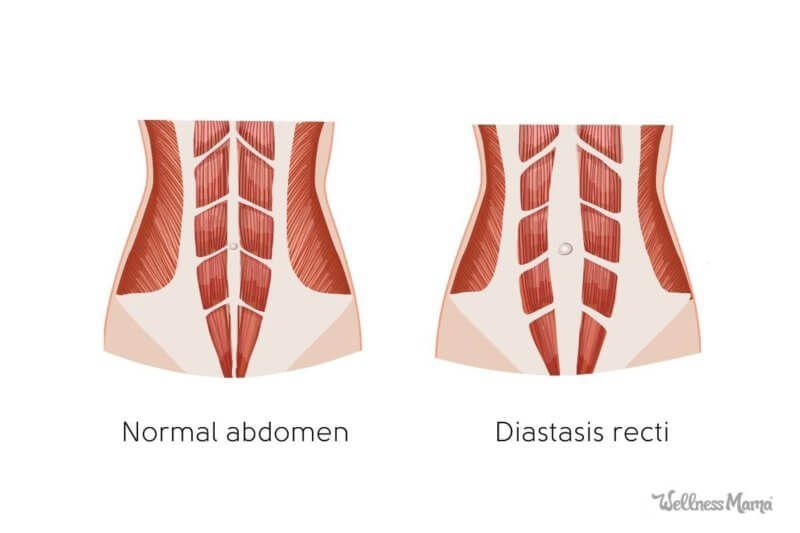 There are some things you can do to lower your risk for developing diastasis recti:
There are some things you can do to lower your risk for developing diastasis recti:
- Healthy weight gain during pregnancy: Exercising and eating healthy foods to keep weight gain within a healthy range.
- Proper posture and deep breathing: Stand up straight with your shoulders back. Take deep breaths that allow your ribs to expand and not just your belly.
- Safe core exercises: Avoid exercises like sit-ups and crunches that put pressure on your abdominals after 12 weeks of pregnancy and postpartum.
- Don't strain while lifting: Certain day-to-day activities like lifting grocery bags or your children can put undue strain on your abdominals.
- Log roll when getting out of bed: If you're pregnant or postpartum, roll to one side and use your arms to push up out of bed.
Outlook / Prognosis
How long will it take to heal my diastasis recti?
The amount of time it takes to heal diastasis recti depends on the amount of ab separation and how consistent you are with strengthening exercises. After several weeks postpartum, this gap will start to close as your muscles regain strength. If you're making modifications to your lifestyle and performing exercises with good form, you're more likely to notice progress.
After several weeks postpartum, this gap will start to close as your muscles regain strength. If you're making modifications to your lifestyle and performing exercises with good form, you're more likely to notice progress.
Can I get diastasis recti again?
Yes, you can heal your diastasis recti and get it again. Your risk for diastasis recti increases the more times you are pregnant. Think of the linea alba as a rubber band that is continuously stretched. Over time, the rubber band will lose its elasticity. The linea alba may not regain its original shape or form after being stretched through multiple pregnancies.
Is it too late to fix my diastasis recti?
It's never too late to repair your diastasis recti. With the proper exercises, you can fix your ab separation years after you've delivered your last baby.
Are there complications from diastasis recti?
If left untreated or in severe cases of diastasis recti, complications can include:
- Umbilical hernia.

- Increase in back pain.
- Pain during sex.
- Urinary incontinence.
- Pelvic and hip pain.
Living With
When should I see my healthcare provider?
Diastasis recti is a common and easily treated condition. If you have more than a two-finger gap between your abdominals or are experiencing pain, contact your healthcare provider for a diagnosis. They may want you to see a physical therapist or pelvic floor specialist to help strengthen your abdominal muscles.
A note from Cleveland Clinic:
Diastasis recti can make you appear pregnant years after your last baby. Discuss your concerns with your healthcare provider so they can diagnose and treat you. Getting treatment can help you feel more confident in your body and correct any pain you are experiencing.
Benefits and harms of a corset for diastasis of the abdominal muscles
Almost every woman faces complications after childbirth, regardless of the initial level of physical fitness and age. Often diastasis of the rectus abdominis muscles develops.
Often diastasis of the rectus abdominis muscles develops.
The pathology is characterized by stretching of the anterior abdominal wall due to increased intra-abdominal pressure during the period of active growth of the fetus. Also, the disease occurs not only in pregnant women, but also in children, men. Many are interested in the question - will a bandage help with diastasis and how to wear it correctly.
Article content
- 1. How diastasis occurs
- 2. What is the danger
- 3. The role of the bandage
- 3.1. Benefits of
- 3.2. When it is contraindicated
- 3.3. How to choose bandage
- 3.4. Where to buy a quality product
- 4. Reviews of wearing a bandage for diastasis
- 5. Conclusion
How diastasis occurs
With prolonged and frequent tension of the abdominal muscles, intra-abdominal pressure increases. With the weakening of the aponeurosis (the white line dividing the abdominal muscles into the right and left segments), the abdominal wall weakens. Most often, the disease occurs in such cases:
Most often, the disease occurs in such cases:
- During pregnancy. Under the action of the hormones relaxin and progesterone, the abdominal wall and ligamentous apparatus become pliable to stretching. This is necessary to create space for the rapidly growing uterus with the fetus. As a result, there is a strong internal pressure, which strenuously stretches the aponeurosis. After pregnancy, muscle tone returns, but the ligaments may remain loose, creating a visible bulging belly. The least susceptible to diastasis are women involved in sports and those who have gained no more than 10 kg during pregnancy.
- Sudden weight loss or weight gain. In particular, this problem concerns those who are prone to male-type obesity (adipose tissue accumulates mainly in the abdomen). More often the problem occurs with a sharp weight gain. Due to the rapidly growing amount of adipose tissue, the ligaments and muscles do not have time to adapt, which leads to a divergence of the aponeurosis.
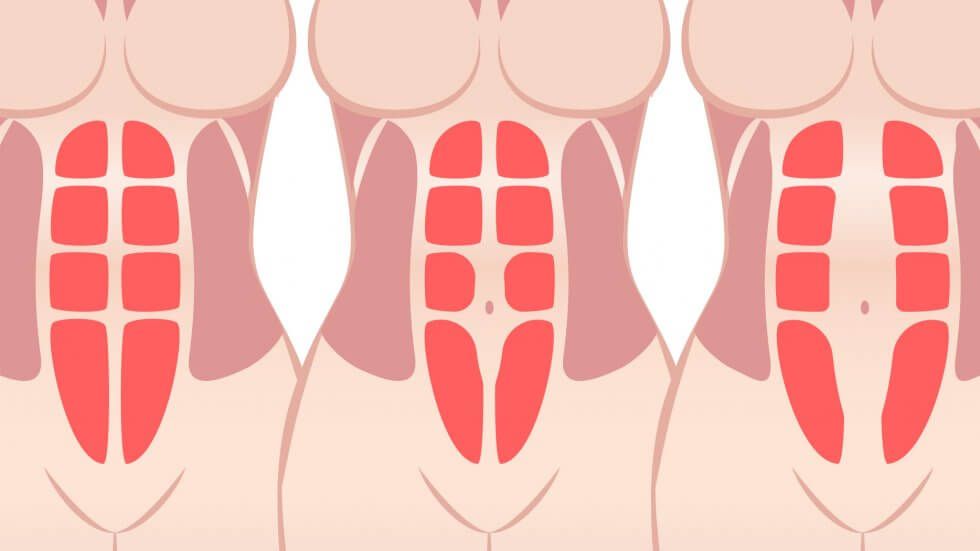
- Strengthened physical activity. Athletes in weightlifting sports often develop diastasis due to heavy lifting, which creates strong intra-abdominal pressure. If the connective tissue is not strong enough, then stretching of the aponeurosis of the white line develops.
- Frequent constipation or hacking cough. If there are problems with the stool during defecation, a strong overstrain occurs, which is fraught with diastasis. A similar mechanism occurs with increased coughing.
- If there is a history of connective tissue dysplasia (congenital weakness), diastasis may occur without treatment.
Outwardly, the disease is manifested by a strong protrusion of the abdomen after eating. There are also associated symptoms - flatulence, stool disorders, abdominal pain.
There are several effective therapies to get rid of the problem. With uncomplicated mild diastasis, experts recommend choosing a set of exercises aimed at restoring the normal muscle tone of the press. They also strengthen the anterior abdominal wall. When the connective tissue becomes stronger, the normal distance between the muscle segments is restored.
They also strengthen the anterior abdominal wall. When the connective tissue becomes stronger, the normal distance between the muscle segments is restored.
"Wearing a slimming belt in combination with physical education helps to restore the tone of the abdominal muscles as soon as possible. In advanced cases, conservative methods of therapy will not help.
In the presence of the third stage of the protrusion, it is necessary to perform an abdominoplasty operation and suture the separated muscle tissues. This is followed by a long recovery period.
What is the danger
When a disease is detected, it is necessary to take measures to eliminate the stretching of the aponeurosis. If the problem is ignored, complications may occur. The danger depends on the degree of divergence of the abdominal wall:
- stage 1 - the distance between muscle segments does not exceed 5 - 7 cm;
- stage 2 - diastasis distance no more than 7 - 10 cm;
- Grade 3 - the stretching width is from 10 cm.

The first degree is not dangerous, in most cases it goes away on its own if special recovery exercises are used during training. The second and third degrees of discrepancy are associated with risks of complications. Most common:
- lumbar-pelvic pain;
- instability of the muscles of the core;
- back pain;
- digestive problems;
- the most serious complication is umbilical hernia (more typical for stage 3 diastasis).
In very rare cases, muscle rupture may occur. The condition occurs due to uncontrolled and neglected stretching. During pregnancy, rupture may occur if there are aggravating factors:
- congenital poor elasticity of ligaments and muscles;
- polyhydramnios or multiple pregnancy;
- poor muscle tone before conception due to physical inactivity;
- large weight gain, severe obesity that arose during the period of bearing a child;
- rapid growth of the abdomen of enormous size (over 110 cm in girth), which occurs in rare cases without the presence of other pathologies.

There is also a rupture of the anterior abdominal wall with excessive loads. If there is an increased contraction of the muscles with their insufficient elasticity, then this increases the risk of tearing off the muscle group. A more rare case is the divergence of the aponeurosis due to injury or a fall. If in parallel there is a displacement of internal organs, then a diagnosis is made - a hernia.
The role of the bandage
In the postpartum period, diastasis of the rectus abdominis can be improved by using a special bandage. Doctors recommend periodic wearing of the device even during pregnancy, when increased abdominal growth begins (in the 2nd or 3rd trimesters). It is also useful to use it in the postpartum period to recover faster. The corset, when used correctly, keeps the stomach in a comfortable state without squeezing. It is especially useful to wear it to women with weakened abdominal muscles.
"You should not purchase a postpartum corset yourself if the doctor has not authorized the use. There are cases when the corset can harm, which will further aggravate the situation with diastasis. There are 3 groups of supporting corsets:
- orthopedic;
- antiradiculitis;
- for pregnant women.
Orthopedic belts are fixing and corrective. Corsets for pregnant women are divided into prenatal and postnatal.
Bandages for women are of the following types:
- Belt. This is an elastic and wide tape with Velcro. The width is adjustable. The belt does not press on the uterus and creates good support from above. It must be worn over clothing.
- Briefs with special support inserts. Compression shorts are the most comfortable to wear, but they need to be washed more often. The disadvantage of this type of corset is the fixed width at the waist. As the belly grows, you will have to buy a larger corset.
- Combination bandage - universal option.
It looks like a ribbon with different widths. During pregnancy, the narrow part is worn under the stomach, and the wide part is worn on the lower back. After pregnancy, the position of the elastic belt changes and is worn with the wide part in front and the narrow part at the back.
The second and third options are most suitable for use in the postpartum period. The bandage accelerates the recovery of muscle tone, tightens the stomach, improves blood circulation and relieves stress from the back, if used correctly.
Benefits
Benefits of wearing a bandage during pregnancy and after childbirth include:
- Elimination of fatigue and pain in the back, legs, lower back.
- Protection against stretch marks, muscle divergence (does not give a 100% guarantee).
- Prevention of scoliosis.
- Reduced risk of miscarriage.
- Promotes the correct position of the fetus in the uterus.
- Prevents premature prolapse of the abdomen.

- Supports the abdomen with weakened muscle tone.
- Facilitates pregnancy.
- Acceleration of uterine retraction after the birth of a baby.
Despite the above positive properties, not all doctors speak highly of bandages. It has been proven that with too frequent or prolonged wear, muscle atrophy of the extensors of the lower back and the press develops.
When it is contraindicated
Strict contraindications to postpartum bandage include:
- Presence of stitches in the perineal area (if during labor there were tears or cuts were made, then it is impossible to wear a corset). The presence of unhealed wounds is fraught with increased inflammation. The bandage can cut off blood circulation in the abdominal area, which will slow down recovery.
- Presence of kidney disease. Squeezing the peritoneum is fraught with a violation of the outflow of fluid, which provokes swelling, congestion and exacerbation of chronic diseases.

- Problems with the gastrointestinal tract, including ulcers, gastritis, or difficulty passing stools. Pulling the abdomen can provoke an attack of the disease.
- Skin diseases including eczema, dermatitis, wounds. A tight fit of the fabric to the body will interfere with the healing of skin lesions.
- Allergic reaction to corset material.
In other cases, you can wear a supporting corset. It is not recommended to walk in it all the time, so as not to cause complete atrophy of the muscles of the back and abdomen. The device well removes the load from these parts of the body. To keep the muscles in good shape, the bandage should be removed every 2-3 hours.
How to choose a brace
There are several rules for choosing a corset for muscle support:
- Made from natural fabric. The ideal option is cotton. Synthetic fabrics float, cause diaper rash and irritation. In a cotton corset, the skin will breathe, so the risk of irritation is minimal.
Such a product is more expensive, but it is better not to save on health.
- You should not choose a corset on the advice of friends. It is recommended to consult a doctor. The specialist knows better what kind of product is suitable in a particular case, taking into account the individual characteristics of a woman.
- Antenatal bandage should not be attempted after the baby is born. This is due to the fact that no one predicts what changes in the body will await the young mother. She may lose or gain weight drastically, making a prenatal brace no longer suitable. It is also important to consider whether a caesarean section was performed, how many ruptures there were, how badly the soft tissues were damaged. Based on these parameters, it is better to acquire a diastasis corset after pregnancy.
- Try on the corset while lying down. In this position, the abdominal muscles relax, which allows you to firmly fix the product.
Where to buy a quality product
It is recommended to choose support corsets in specialized stores that sell orthopedic products.
Choose a store based on ratings and reviews. The best option is on the recommendation of a doctor or friends who bought the product and were satisfied with the quality. A prerequisite is the ability to try on a corset before buying, so online stores are not the best option.
Do not order a bandage from an online maternity store. The sellers of such Internet resources are not narrowly focused specialists who understand supporting bandages. As a result, you can buy a low-quality item.
Reviews about wearing a bandage for diastasis
In most cases, the reviews are positive. Many note that the stomach is drawn in faster with a corset than without it. In particular, the difference is visible when the birth is not the first. Also, women indicate that the drag belt is effective only in the first stage of the divergence of the abdominal muscles. With severe diastasis, the corset did not help. Deterioration and pain in the back were observed in those who wore the belt without removing it for a long time.
This condition develops due to muscle weakness. If the recommendations of a specialist were followed, problems usually did not arise.
Conclusion
Postpartum diastasis bandage is one of the aids to solve the problem. In combination with exercises, the abdomen will retract quickly if the gap is minimal. Belts are recommended to buy only on the advice of a specialist.
Diastasis rectus abdominis and pubic diastasis. Solvable problems of pregnancy. Interview with Doctor of Medical Sciences, Professor M.A. Chechnevoy
— What is muscle diastasis and what is pubic symphysis diastasis?
— Pregnancy is an amazing and wonderful time, but it is also a period of additional loads, which undoubtedly becomes a test of strength for the female body.
The previously existing everyday point of view that pregnancy rejuvenates and gives strength is not confirmed by anything. During the bearing of a child, significant additional loads are placed on the mother's body, which often lead to the manifestation of problems that were invisible before pregnancy.

Diastasis of the rectus abdominis muscles is a divergence of the inner edges of the muscles along the white line of the abdomen (connective tissue structure) at a distance of more than 27 mm. Pubic diastasis is one of the manifestations of pregnancy-associated pelvic girdle pain. This pathology affects the entire pelvic ring, sacroiliac joints and symphysis. And they certainly have common causes for the appearance.
The formation of such problems is facilitated by a decrease in the strength of connective tissue collagen. One of the reasons is an innate predisposition, the so-called connective tissue dysplasia, when the tissues are very elastic, extensible. During pregnancy, the body of a woman increases the production of the hormone relaxin, which reduces the synthesis of collagen and enhances its breakdown. This is provided by nature to create maximum elasticity of the birth canal. However, other structures, such as the anterior abdominal wall and the pubic symphysis, also fall under the action of relaxin.
— How does diastasis of the muscles and diastasis of the pubis affect pregnancy and childbirth?
— Divergence of the rectus abdominis occurs in about 40% of pregnant women. During pregnancy, it does not give serious complications that threaten the life of the mother or the condition of the fetus. However, the inferiority of the work of the rectus abdominis muscles forces the redistribution of the load on the back muscles, which can lead to lumbar-pelvic pain and, accordingly, discomfort in the back. During childbirth, the abdominal muscles are involved in attempts, and the violation of their anatomy and function can affect the birth act.
With diastasis of the pubis, things are more complicated. As already mentioned, this is only one of the manifestations of a violation of the structure and function of the pubic joint (symphysiopathy) during pregnancy. It occurs in about 50% of pregnant women in varying degrees of severity: in 25% of cases it leads to restriction of the mobility of the pregnant woman, in 8% - to severe disorders up to disability.
With symphysiopathy, the ligaments of the pubic articulation and cartilage that connect the pubic bones suffer. All this leads to severe pain in the pubic joint, pelvic bones, lower back, as well as to a violation of gait and the inability to stand up or lie down without outside help. Women with pelvic girdle pain syndrome experience significant levels of discomfort, disability, and depression, with associated social and economic problems. These include impaired sexual activity during pregnancy, chronic pain syndrome, risk of venous thromboembolism due to prolonged immobility, and even seeking early induction of labor or caesarean section to stop pain.
During childbirth, such a patient may have a rupture of the pubic symphysis, may require surgery to restore it.
— How to prevent the development of muscle and pelvic diastasis during pregnancy and childbirth? What factors increase the likelihood of its development?
- There is no recipe that will be one hundred percent.
There is a wonderful term in the medical literature called "lifestyle modification". Whatever diseases we study, be it symphysiopathy, diabetes mellitus or preeclampsia, the risk group for pathology is always overweight women. You need to prepare for pregnancy, you need to be in good physical shape. During pregnancy, weight gain should be monitored. The recommendation to "eat for two" is not just wrong, but extremely harmful. Pregnant women should maintain reasonable physical activity. Weak and flabby abdominal muscles, combined with the large size of the fetus, undoubtedly increase the risk of diastasis.
The risk factors for symphysiopathy in numerous studies are hard physical labor and previous injuries of the pelvic bones. Factors such as time elapsed from previous pregnancies, smoking, use of hormonal contraception, epidural anesthesia, mother's ethnicity, number of previous pregnancies, bone density, weight and gestational age of the fetus (post-term fetus) are not associated with an increased risk of symphysiopathy.
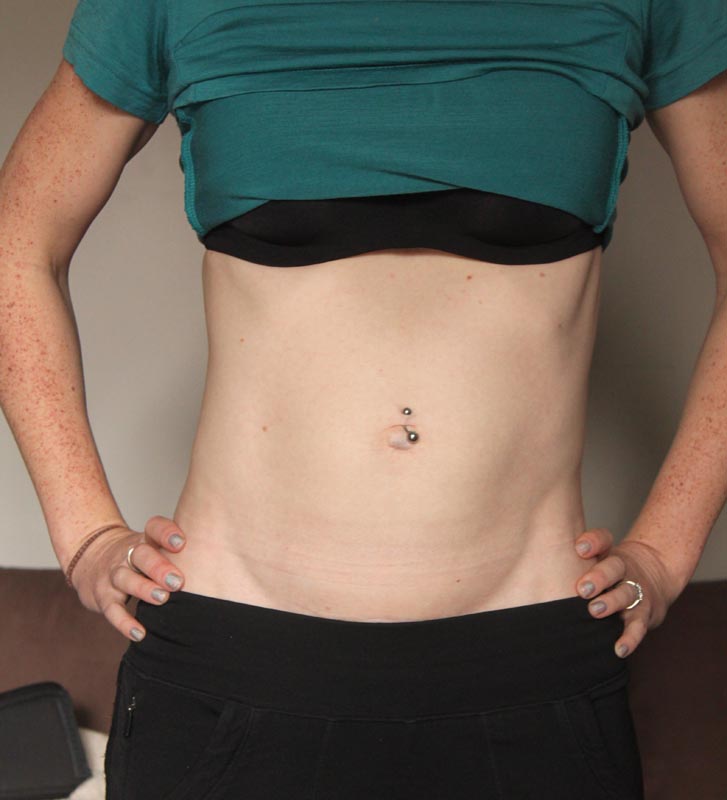
- How to diagnose diastasis of the rectus muscles and diastasis of the pubic symphysis?
— In most cases, diastasis rectus abdominis can be diagnosed clinically. It happens that inspection, palpation and simple measurements are enough.
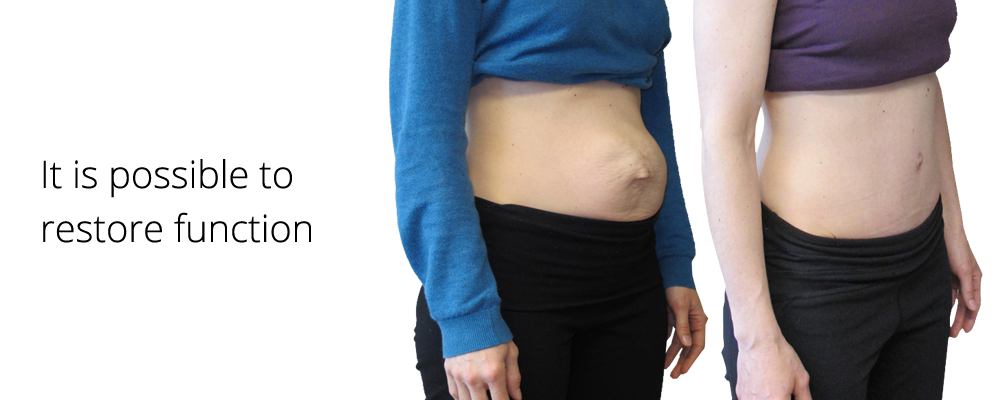
In the standing position, you can see the divergence of the muscles when the woman does not have subcutaneous fat. In this case, diastasis is defined as a vertical defect between the rectus muscles.
With tension of the abdominal press, a longitudinal protrusion is observed in the diastasis zone. Such a protrusion is especially noticeable if the patient in the supine position is asked to raise her head and legs. If necessary, you can measure the width of the defect simply with a ruler.
Ultrasound may be the most accurate diagnostic method. With ultrasound, the inner edges of the rectus muscles are clearly visible and the distance between them at different levels can be measured.
Computed tomography is used in the diagnosis of diastasis extremely rarely, mainly in scientific research.
For the diagnosis of symphysiopathy and diastasis pubis there is no one test as a "gold standard".
The first place, of course, is the questioning and examination of the patient. We pay attention to the gait of the pregnant woman, to how she sits down, lies down and how she gets up. Symphysiopathy is characterized by a “duck gait”, when a pregnant woman rolls from foot to foot. On palpation in the area of the womb, pain and swelling are noted. The so-called pain provocative tests are used, for example, a mat-test (pulling up an imaginary rug, mat with your foot towards you).
The following questionnaires are used to assess quality of life, pain and disability: Health-Related Quality of Life (HRQL), Oswestry Disability Index (ODI), Disability Rating Index (DRI), Edinburgh Postpartum Depression Scale (EPDS), Pregnancy Mobility Index (PMI), and Pelvic Ring Score (PGQ).
Of the instrumental methods, ultrasound is the most widely used, less often computed or magnetic resonance imaging.
Ultrasound allows you to assess the condition of the ligaments of the pubic joint and the interpubic disc, the severity of the changes and the risk of natural childbirth.
— What is the treatment for diastasis recti or pubis?
— Primary prevention: when planning and during pregnancy, it is necessary to strengthen all muscle groups of the pelvic girdle, as well as the pelvic diaphragm.
More often, diastasis of the rectus muscles disappears on its own during the first months after childbirth. Special physical exercises to correct the work of muscles, to tone them and restore their basic functions should be performed under the guidance of a competent instructor. There are types of physical exercises that can, on the contrary, worsen the situation with diastasis of the rectus abdominis muscles. In some cases, when there is no effect from physiotherapy exercises, it is necessary to resort to surgical correction of the defect. Currently, both endoscopic and open surgery are practiced.
The choice of method depends on the size and localization of the defect.
In case of symphysiopathy, therapeutic exercises reduce back and pelvic pain. Acupuncture and wearing a pelvic bandage have a positive effect on symphysiopathy.
Initial treatment for pubic symphysis should be conservative even if symptoms are severe. Treatment includes bed rest and the use of a pelvic brace or corset that tightens the pelvis. Early appointment of physiotherapy with dosed therapeutic exercises will help to avoid complications associated with prolonged immobilization. Walking should be done with assistive devices such as walkers.
In most cases (up to 93%), the symptoms of dysfunction of the pelvic ring, including the pubic joint, progressively subside and completely disappear six months after birth. In other cases, it persists, becoming chronic. However, if the diastasis exceeds 40 mm, then surgical treatment may be required. Most studies recommend surgery only after failure of conservative treatment, inadequate enlargement of diastasis, or its recurrence.