Baby hip click
When to Worry About Your Child’s Hip Click
When to Worry About Your Child’s Hip Click | Health Hive Bone and Joint Sometimes parents notice a clicking or popping sound with the movement of their baby’s legs. We spoke to a pediatric orthopaedic surgeon for advice on what to do if this is the case.Jan. 27, 2022 • 4 min read
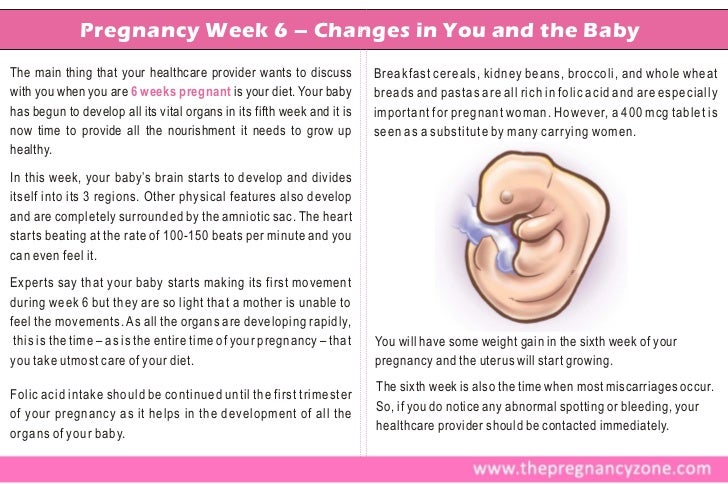
The hip is a ball-and-socket joint, meaning that the femoral head (the top of the femur) is shaped like a ball and sits within the cup-like socket in the pelvis. In some cases, parents may notice abnormalities when an infant or young child’s legs are moved, such as a clicking sound or the feeling of looseness or displacement of the hip.
James Engels, MD, a pediatric orthopaedic surgeon with Rochester Regional Health, advises parents on what to do if their child has a hip click and provides need-to-know information on hip dysplasia.
What is a hip click?
A “hip click” refers to an audible clicking or popping sound that occurs when a baby’s hips are being examined or moved around. Most clicks are not problematic.
There are tendons or ligaments associated with an infant’s hip joint that can make a snapping or popping sound for a variety of reasons. A hip click could be a sign of abnormalities in hip development, but further examination and possible testing are required to reach a diagnosis. More importantly, instability or displacement of the hip is a significant concern for hip dysplasia.
“A child that has a hip click or hip instability should be monitored for hip dysplasia or other developmental abnormalities. This is something that is usually caught early on by physicians during well-child visits. ”
”
Should my newborn receive a hip exam?
After a child is born at the hospital, pediatric specialists perform a newborn examination. During this thorough physical exam, a specialist will check the baby's hips and legs for abnormalities to assess for hip dysplasia. They do this by gently pushing and pulling the baby’s thigh bones to see how they move in the hip socket.
“If we notice an abnormality in a newborn’s hips, we may order an ultrasound to get a more in-depth look. Once we perform further examinations and testing, we can determine the best way to treat the problem,” said Dr. Engels.
Are there risk factors for hip dysplasia?Some factors may lead to a greater likelihood that a child will have hip dysplasia, such as:
- if a primary relative of the child had hip dysplasia (a parent or sibling)
- if there was an extended breech position while the baby was in the womb
- a specialist detects laxity during the newborn hip screening exam
If any of the above are present, the patient should receive further testing to check for hip dysplasia.
Should my child see a doctor for their hip click?
Parents may notice clicking or popping sounds when their child walks or moves their hips or legs. In this case, they should schedule an appointment with their child’s pediatrician for an examination. After the exam, the pediatrician can determine whether further evaluation from a pediatric orthopaedic surgeon is necessary.
Children should have routine well-child visits from the moment they are born up through age 21. For children under 2, these exams occur 2-3 months. At these early visits, a physician will check their hips and legs for signs of hip dysplasia or other abnormalities.
If there is no detection of hip dysplasia or other abnormalities and your child is experiencing a hip click after three or more years of age, schedule an exam with their pediatrician to check for any undetected orthopaedic abnormalities.
“Abnormalities or signs of problems in the hip joints can often be identified at the child’s routine well-exams, especially during the first few years of life. However, if a parent notices clicking, popping, abnormal walking pattern, they should schedule an additional exam with their pediatrician.”
However, if a parent notices clicking, popping, abnormal walking pattern, they should schedule an additional exam with their pediatrician.”
What is hip dysplasia?
Hip dysplasia is a condition in which the hip socket does not fully cover the ball of the upper thighbone, allowing the hip joint to become partially or completely dislocated.
Hip dysplasia can damage the cartilage lining in the hip joint, and in some cases, can lead to loss of the soft cartilage that lines the socket portion of the hip joint, resulting in a painful arthritic hip. That’s why early detection and treatment of hip dysplasia is so important.
Hip dysplasia symptoms
Signs and symptoms of hip dysplasia vary based on age and severity. A hip click may be a sign of hip dysplasia, but it does not guarantee the condition.
Symptoms of hip dysplasia may include:
- Pain in the hip
- Loose or unstable hip joint
- Limping or abnormal walking patterns
- Unequal leg lengths
- Loss of motion
“Many of the signs of hip dysplasia go unnoticed in everyday life, which is why it’s so important for infants to have routine well-child exams that include hip screen examination right from the moment they’re born. This way, we are more likely to detect any abnormalities early on and begin treatment as needed,” said Dr. Engels.
This way, we are more likely to detect any abnormalities early on and begin treatment as needed,” said Dr. Engels.
Hip dysplasia treatments
Pavlik harness
The most common treatment for hip dysplasia in infants is a Pavlik harness. The Pavlik harness is a soft splint that helps keep the infant’s hips and knees bent and the thighs apart. An infant treated with a Pavlik harness stays in the harness at all times of day and night.
In most cases, the infant will wear the harness for 3-4 months and will be monitored as they grow.
“The Pavlik harness is very comfortable for baby. It’s soft and easy to clean. Most importantly, it is extremely effective in treating and curing hip dysplasia,” said Dr. Engels.
Semi-rigid orthosis
If an infant’s hips do not stabilize with the Pavlik harness, or if hip dysplasia is diagnosed later than 6-8 months of age, an orthopaedic physician may prescribe a semi-rigid orthosis.
Instead of a harness, this is more like a brace that keeps the infant’s legs and hips in a more stable and secure position.
Surgery
In severe cases, an infant may need surgery to correct the development of their hips. There are two types of surgical options: closed reduction surgery and open reduction surgery.
Closed reduction surgery occurs under general anesthesia and the infant's hip is placed back into the socket. To help with this process, a tendon in the groin is usually lengthened through a small incision. The infant is then put into a body cast, bracing the pelvis area to hold their hips in position.
In open reduction surgery, under general anesthesia, an incision is made to put the hip back into place. This option is for severe cases in which bones may also need to be cut to help keep the hip in place.
“After any surgical option, we follow-up with the patient routinely until they’re at least 5-7 years of age. We continue to check on their development to ensure everything is healthy."
NEXT STEPS Personalized Bone & Joint Care
At any age, orthopedic conditions can keep us from the basic tasks that mean so much. Using advanced and proven techniques, and drawing on the resources and talents of our full regional network, our team will provide you with personalized care – and the freedom of a happy, active life.
Using advanced and proven techniques, and drawing on the resources and talents of our full regional network, our team will provide you with personalized care – and the freedom of a happy, active life.
Learn More
Recent ArticlesDevelopmental Dysplasia of the Hip (for Parents)
What Is Developmental Dysplasia of the Hip?
Developmental dysplasia of the hip (DDH) is a problem with the way a baby's hip joint forms. Sometimes the condition starts before the baby is born, and sometimes it happens after birth, as the child grows. It can affect one hip or both.
Most infants treated for DDH develop into active, healthy kids and have no hip problems.
What Happens in a Hip With Developmental Dysplasia?
The hip joint is a ball and socket joint. The top part of the thighbone (the ball part of the hip) sits inside a socket that's part of the pelvic bone. The ball moves around in different directions, but always stays inside the socket. This lets us move our hips front, back, and side to side. It also supports our body weight for walking and running.
The ball moves around in different directions, but always stays inside the socket. This lets us move our hips front, back, and side to side. It also supports our body weight for walking and running.
In DDH, the hip does not form well. The ball part of the joint may be completely, or partly, out of the socket. Sometimes the ball part may slide in and out of the socket. Often, the socket is shallow. If this is not fixed, the hip joint will not grow well. This can lead to pain with walking and hip arthritis at a young age.
What Are the Signs & Symptoms of Developmental Dysplasia of the Hip?
Developmental dysplasia of the hip doesn't cause pain in babies, so can be hard to notice. Doctors check the hips of all newborns and babies during well-child exams to look for signs of DDH.
Parents could notice:
- The baby's hips make a popping or clicking that is heard or felt.
- The baby's legs are not the same length.
- One hip or leg doesn't move the same as the other side.

- The skin folds under the buttocks or on the thighs don't line up.
- The child has a limp when starting to walk.
Babies with any of these signs should see a doctor to have their hips checked. Finding and treating DDH early usually means there's a better chance for a baby's hips to develop normally.
What Is Hip Laxity?
Many babies are born with hips that feel loose when moved around. This is called neonatal hip laxity. It happens because the bands of tissue that connect one bone to another, called ligaments, are extra stretchy. Neonatal hip laxity usually gets better on its own by 4–6 weeks of age and is not considered true DDH.
A baby's whose hip ligaments are still loose after 6 weeks might need treatment. So follow-up doctor visits for babies with hip laxity are important.
Who Gets Developmental Dysplasia of the Hip?
Any baby can have DDH. But there's a higher chance of being born with it in babies who:
- are girls
- are first-born
- were breech babies (in the womb buttocks-down instead of head-down), especially during the third trimester of pregnancy
- have a family member with the condition, such as parent or sibling
Rarely, a baby isn't born with DDH, but develops it after birth. To prevent DDH in babies who aren't born with it, don't swaddle a newborn's hips or legs tightly together. Always make sure a baby's legs have plenty of wiggle room.
To prevent DDH in babies who aren't born with it, don't swaddle a newborn's hips or legs tightly together. Always make sure a baby's legs have plenty of wiggle room.
How Is Developmental Dysplasia of the Hip Diagnosed?
Doctors find most cases of DDH during well-child exams. If a baby has signs of DDH or has a higher risk for it, the doctor will order tests.
Two tests help doctors check for DDH:
- An ultrasound uses sound waves to make pictures of the baby's hip joint. This works best with babies under 6 months of age. That's because most of a baby's hip joint is still soft cartilage, which won't show up on an X-ray.
- An X-ray works best in babies older than 4–6 months. At that age, their bones have formed enough to see them on an X-ray.
How Is Developmental Dysplasia of the Hip Treated?
A pediatric orthopedic surgeon (a specialist in children's bone conditions) cares for babies and kids with DDH. The goal of care is to get the ball of the hip in the socket and keep it there, so the joint can grow normally.
The goal of care is to get the ball of the hip in the socket and keep it there, so the joint can grow normally.
The orthopedic surgeon chooses the treatment based on the child's age. Options include:
- bracing
- a closed reduction and casting
- an open reduction (surgery) and casting
A brace or cast will hold the hip in place and will be on both sides, even if only one hip is affected.
Bracing
Treatment for babies younger than 6 months old usually is a brace. The brace used most often is a Pavlik harness. It has a shoulder harness that attaches to foot stirrups. It puts the baby's legs into a position that guides the ball of the hip joint into the socket.
Treatment with the Pavlik harness often lasts about 6–12 weeks. While wearing the harness, the baby has a checkup every 1–3 weeks with hip ultrasounds and exams. During the visit, the medical team can adjust the harness if needed.
The harness (brace) usually works well to keep the hips in position. Most babies won't need other treatment.
Most babies won't need other treatment.
Rarely, the harness isn't able to keep the ball of the hip in the socket. Then, doctors might do either:
- a closed reduction (manually moving the ball back into the socket) and casting
- an open reduction (surgery) and casting
Closed Reduction and Casting
A child might need a closed reduction if:
- The harness was not successful at keeping the ball of the hip in the socket.
- A baby starts care after age 6 months.
For a closed reduction, the baby gets medicine (general anesthesia) to sleep through the procedure and not feel pain. The surgeon:
- Injects contrast dye into the joint to see the cartilagepart of the ball.
- Moves the baby's thighbone so that the ball of the joint goes back into place in the socket.
- Puts on a hip spica cast to hold the hip in place. The baby wears the cast for 2–4 months.
Sometimes, the orthopedic surgeon also loosens the tight muscle in the groin during the closed reduction.
Open Reduction (Surgery) and Casting
A child might need surgery (an open reduction) if:
- The closed reduction was not successful at keeping the ball of the hip in the socket.
- The child is older than 18 months when starting treatment.
During an open reduction, the child is asleep under anesthesia. The surgeon:
- Makes a cut through the skin.
- Moves muscles out of the way to see the hip joint directly.
- Puts the ball back into place.
- Closes the surgical cut with stitches placed under the skin. These won't need to be removed.
- Puts on a hip spica cast to hold the hip in place. The child wears the cast for 6–12 weeks.
Sometimes, the orthopedic surgeon also does a surgery on the pelvic bone to deepen a very shallow hip socket, especially for a child older than 18 months.
What Else Should I Know?
Kids will have regular checkups with their orthopedic specialist until they're 16–18 years old and done growing. These help make sure the hip develops well.
These help make sure the hip develops well.
Snapping hip syndrome: treatment, causes, symptoms
Snapping hip syndrome: treatment, causes, symptomsAbout Portal
BUT BUT BUT
- Diseases
- sports injuries
- Video
- Good to know
- News
- I'm worried about
- Preparations
- First aid
- About the portal
- Contacts
What is it
Main types and causes of occurrence
Symptoms
Examination and diagnosis
Treatment
Exercise
Prognosis
Snapping Hip Syndrome or Coxa Saltans is a condition where a person feels clicks or hears characteristic sounds in the hip joint.
The syndrome occurs in people who are engaged in professional sports, choreography, gymnastics and other active physical activities. Some patients feel weakness or pain when extending or flexing the hip. Sometimes there is a feeling of dislocation of the hip. This affects activity and the overall quality of life.
The main types and causes of occurrence
External
The cause of pain is constant contact of the ilio-tibial tract with the trochanter. The outdoor type is considered the most common.
People have clicks when running or climbing stairs. Often there is pain on the outside of the thigh. During the night period, pain intensifies if a person lies on the problem side. Symptoms are most often accompanied by trochanteritis - inflammation of the upper point of the femur.
Special tests
- Aubert's test: the patient lies on his side with the injured thigh up. The upper leg is straight, the lower leg is bent at the knee.
 The doctor bends the upper leg at a right angle. After unbends and abducts the thigh, slowly lowering the limb. If the leg falls below the horizontal line without pain, the test is negative.
The doctor bends the upper leg at a right angle. After unbends and abducts the thigh, slowly lowering the limb. If the leg falls below the horizontal line without pain, the test is negative. - Feeling the area of the greater trochanter during flexion, external and internal rotation of the thigh and checking the condition with circular rotations.
- FABER test: check for clicks during passive hip flexion.
Internal (in front of the thigh)
In this case, the problems are related to the tendon of the muscle. The click occurs when the thigh muscles slide over the protruding bony structures of the joint, or the quadriceps moves over the ball and socket. Symptoms come on gradually, worsen over time: crackling while running, pain in the groin area, when bending the hip.
Special tests
- Stanchfield test: the person lies on his back, hip flexion 30°. The doctor asks to bend the thigh completely, at the same time resisting it.
 If there is pain in the groin, the test is positive.
If there is pain in the groin, the test is positive. - Thomas test: carried out in the supine position. The patient bends and grasps the knees so that the lower back touches the surface. After lowering one leg, keeping the hip and knee in a bent state. The test result is negative if the lower back does not come off the surface.
The intra-articular type is caused by impact injuries to the joint. For example, during a fall on a large skewer. The head of the femur strongly collides with the bottom of the acetabulum - as a result, the articular cartilage dies. With this type of syndrome, pain appears during movements: flexion, rotation of the extended hip.
Intra-articular type
Syndrome occurs due to problems within the joint or cartilage damage. There is a change in the inner part of the capsules: ruptures of the acetabular lip and free joint muscles, osteoarthritis, chondromatosis of the hip joint.
Main symptoms
The condition is accompanied by a characteristic click in the inner or outer part of the hip joint. In addition to clicking, other symptoms occur.
In addition to clicking, other symptoms occur.
- pain and swelling;
- inflammatory processes;
- weakness in the legs when trying to lift a limb;
- problems with physical activity;
- Sensation as if thigh were failing.
Examination and diagnostics
During the examination, the doctor analyzes the patient's condition, collects an anamnesis: the location of the click, the period of onset of symptoms, the duration of symptoms, the presence of pain, the effect of clicks on physical activity.
The specialist uses a visual analogue scale to measure the intensity of pain. Clinical examination, in addition to palpation, includes special tests. To make an accurate diagnosis, the patient is sent for an ultrasound or MRI.
Treatment
Most often, snapping hip syndrome does not require intervention to recover. Only when a person is in pain or there are problems in movements, the doctor develops a therapeutic program.
Conservative treatment and physiotherapy
Therapy is based on the exclusion of movements that cause unpleasant symptoms and on simple methods: taking anti-inflammatory drugs, rest, pain injections. For example, the Elox-SOLOpharm drug has analgesic, anti-inflammatory and antipyretic effects: it will help to cope with pain. Additionally, the patient is referred to a physiotherapist. Exercises to strengthen the muscles around the hip joint and stretching are recommended.
Surgical treatment
Surgical intervention is rarely used when there are no results from conservative therapy. The goal of treatment is to relieve tension in the iliopsoas tendon. The type of operation depends on the reason for the click. For example, arthroscopy is used to remove or repair fragments of a torn upper lip. The surgeon inserts a small camera into the hip joint that displays a real picture to control the instruments.
Snapping Hip Syndrome
Try our set of exercises, developed in collaboration with specialists: this is a workout that takes into account the specifics of sports injuries.
Attention! If you've recently been injured, check with your doctor before you start exercising to see if it's right for your body.
Watch video
Exercises
PBT (Iliotibial Tract) Stretch
- Stand with the right side against the wall and cross the lower limbs, placing the right foot behind the left.
- Drive the hips towards the support until there is tension on the outside of the right leg.
- Hold the position for thirty seconds and repeat the exercise on the left side.
- Do 4 reps in 2-3 sets.
Piriformis Stretch
- Lie on your back with knees bent and feet flat on the floor.
- Place the right foot on the knee of the left, grasp the left thigh with the hands.
- Pull the thigh towards you until tension appears in the buttocks and thighs.
- Hold the position for thirty seconds, then repeat with opposite legs.

- Perform 4 reps on each side for 2-3 sets.
Prognosis
Conservative treatment usually helps to reduce pain and eliminate clicking. Proper exercise leads to rapid recovery of the joints. After 7-28 days, athletes return to training again. If the condition does not improve, epidural injections of glucocorticoids are prescribed. After 7-14 days, most often clicks and pains disappear.
When symptoms of the syndrome appear, monitor the level of exercise and eliminate movements that provoke complications. Getting rid of snapping hip syndrome is more difficult if the situation is running. Consult a doctor as soon as discomfort appears to find methods for restoring the body.
Cervical spine distortion
Ankle sprain
Dislocation of the foot
Broken arm
Shoulder dislocation
Anterior shoulder dislocation
Collateral ligament tear
Fractured nose
Top
THE INFORMATION PROVIDED ON THE SITE DOES NOT REPRESENT AND DOES NOT REPLACE THE CONSULTATION OF A SPECIALIST
Hip dysplasia - clinic "Family Doctor".

“Your child has hip dysplasia” - very often this phrase from the mouth of an orthopedic doctor causes a state close to emotional shock in the parents of the baby. But is everything so gloomy and scary, and what kind of pathology is this?
Dysplasia - this term means a violation of the formation of any organ or body system. In this material we will talk about hip dysplasia.
Hip dysplasia is understood as a violation of the formation of the hip joint, which captures all the elements that make up the joint: the bone and cartilage base, the ligamentous-capsular apparatus and the muscle component. This definition is quite broad and includes the physiological immaturity of the hip joint, preluxation, subluxation and dislocation of the hip.
Physiological immaturity consists in the incomplete formation of the joint components without violating the congruence (correct matching) of the articular surfaces of the bones and, as a rule, requires minimal treatment or only dynamic observation, and it is this form of hip joint pathology that is mainly assigned the diagnosis of "dysplasia", although this is not entirely correct. terminologically. With pronounced immaturity of the hip joint, treatment is necessary to create favorable conditions for the proper maturation of the joint components.
terminologically. With pronounced immaturity of the hip joint, treatment is necessary to create favorable conditions for the proper maturation of the joint components.
Predislocation of the hip is already a pathology of the joint associated with the lack of stability of the femoral head in another component of the hip joint - the acetabulum and already requires close attention. In the absence of adequate treatment, hip predislocation can lead to the development of joint deformity (arthrosis), which leads to pain and impaired joint mobility, and can also lead to hip dislocation after the start of walking.
Dislocation of the hip is the most severe form of the pathology of the development of the hip joint, which consists in the almost complete discrepancy between the articular surfaces of the femoral head and the acetabulum. Such a malformation of the joint requires maximum efforts for a thorough diagnosis and active and prompt treatment. Late diagnosis or inadequate treatment leads to gross impairment of the hip joint mobility and, ultimately, leads to disability.
Now we understand why so much attention is paid to hip dysplasia by pediatricians and orthopedists. Why is it the hip joint that is most susceptible to these misfortunes?
The fact is that the hip joint, due to its anatomical and physiological characteristics, is the most loaded joint in our body, and a failure in one of its constituent components leads to dysfunction of the joint and, ultimately, to a deterioration in the quality of life of the patient. That is why the diagnosis of hip dysplasia can so often be heard from the lips of an orthopedist, although one cannot but recognize the fact of some overdiagnosis of this pathology, but given the severity of the consequences in the absence of treatment, this is still justified.
According to statistics, the incidence of hip dysplasia is 4-6 cases per 1000 newborns, in girls it occurs 6-7 times more often. Unilateral lesion predominates over bilateral (more often the left hip joint is affected). There is inheritance from mother to daughter. Quite a lot of factors leading to impaired intrauterine joint formation have been noted, among them are breech presentation of the fetus, narrowness of the uterus, oligohydramnios, toxic and biological (primarily viral diseases of the mother during pregnancy) factors and much more.
There is inheritance from mother to daughter. Quite a lot of factors leading to impaired intrauterine joint formation have been noted, among them are breech presentation of the fetus, narrowness of the uterus, oligohydramnios, toxic and biological (primarily viral diseases of the mother during pregnancy) factors and much more.
When and by what methods can and should hip dysplasia be diagnosed? Can a mother herself suspect the presence of hip dysplasia in a child and, if so, with what methods? The answer to this question depends on the severity of the joint injury. Let's try to answer this question by tying the timing and methods of diagnosis to the age of the baby.
When conducting ultrasound diagnostics during pregnancy, it is possible to diagnose only gross violations - subluxation and dislocation of the hip, that is, those changes in which the articular surface of the femoral head does not correspond to the surface of the acetabulum of the child's pelvis.
In the first 7-10 days of a child's life, an examination can reveal a “click symptom” or “slipping symptom” - dislocation and reduction of the hip in the joint. These symptoms are revealed in a child as follows: in the supine position, the legs are bent at the knee and hip joints at an angle of 90 degrees. The thumbs are located on the inner surface of the child's thighs, the index and middle fingers on the outer. With careful abduction and traction of the hips, the femoral head is set into the acetabulum with a characteristic click.
These symptoms are revealed in a child as follows: in the supine position, the legs are bent at the knee and hip joints at an angle of 90 degrees. The thumbs are located on the inner surface of the child's thighs, the index and middle fingers on the outer. With careful abduction and traction of the hips, the femoral head is set into the acetabulum with a characteristic click.
After the 2nd - 3rd week of a child's life, limitation of hip abduction comes to the fore in the diagnosis of hip dysplasia. To identify it, the legs of the child bent at the knee and hip joints in the supine position are bred without violence. Normally, it is possible to spread the hips to an angle of 85-90 degrees to the surface. With increased muscle tone and spasm of the muscles adducting the thigh, abduction can be limited to an angle of about 70 degrees, but such a restriction of hip abduction can also be caused by impaired joint formation. Limitation of hip abduction on one side in most cases is a sign of pathology from the hip joint.
In favor of the pathology of the hip joint, symptoms such as shortening of one limb, turn of the foot on the side of the lesion outward from the middle position (external rotation of the foot) also speak.
The most widely known in parents (so to speak, "mommy symptom") - the asymmetry of the subgluteal folds - is not absolute and can be caused by many factors, but its importance in the diagnosis of hip dysplasia should not be underestimated, since this is the most common question that is addressed to orthopedic doctor.
To confirm the diagnosis of hip dysplasia and control the dynamics of treatment, ultrasound diagnostics are currently widely used. The positive aspects of this method of examination include painlessness, non-invasiveness, relative safety and a sharp increase in recent availability. Also, with the help of an ultrasound examination of the joint, minimal changes in the structure of the hip joint can be detected. But, unfortunately, this examination method does not always give accurate results (its reliability is about 85-90%. Nevertheless, to date, ultrasound diagnostics is the main method of screening for the diagnosis of hip dysplasia.
Nevertheless, to date, ultrasound diagnostics is the main method of screening for the diagnosis of hip dysplasia.
In the case when the clinical picture differs from the data of the ultrasound examination or in case of late diagnosis of the pathology of the hip joint, the X-ray method is used. With a correctly performed radiograph, the picture of the structure of the joint and the position of the femoral head in the joint become completely clear. But due to the rather large radiation exposure during radiography, this examination method is used as rarely as possible.
In children older than a year, the main symptom is lameness on the affected side when walking or a "duck" gait with a bilateral process. Diagnosis at this age is belated. The clinical picture in this case almost always requires confirmation by x-ray, since it is necessary to accurately determine the relative position of the joint components.
And so, the child was diagnosed with hip dysplasia, what to do next and how to help the baby?
Treatment of hip dysplasia should be started as early as possible. The goal of the treatment is to center the femoral head in the joint and create conditions for the formation of the entire acetabulum. Early, most gentle, but systematic treatment allows you to completely restore the anatomy and function of the underdeveloped hip joint.
The goal of the treatment is to center the femoral head in the joint and create conditions for the formation of the entire acetabulum. Early, most gentle, but systematic treatment allows you to completely restore the anatomy and function of the underdeveloped hip joint.
The centering of the hip in the joint in the early stages of treatment is achieved by wide swaddling - two diapers are placed between the divorced hips of the child and fixed with a third. In severe degrees of hip dysplasia, special splints are used to center the femoral head (Pavlik's stirrups, Freik's pillow, etc.). When using these tires, parents may have questions and difficulties in caring for their baby, here are some tips to help you and your baby adjust during this period:
1. Only a baby diaper (disposable or gauze) should be under the stirrups or pillow. If you prefer to use gauze diapers, wear oilcloth panties that have zippers on the sides.
2. When changing a diaper, do not lift the child by the legs, but put your hand under the buttocks.
3. The vests can be changed without removing the stirrups: unfasten the shoulder straps from the chest strap and remove the vest over your head.
Over the tires you can wear loose pants, suits, dresses.
4. During the splint period, bathing the child is less frequent, so it is necessary to examine the skin under the straps, under the knees and around the neck 2-3 times a day to make sure there are no signs of inflammation (redness) of the skin. During this period, it is necessary to wipe the baby's skin with a soft cloth soaked in warm water. When carrying out water procedures, you can unfasten one foot part of the stirrup, but do not remove it, and keep the leg in a bent and retracted position.
5. It is also necessary to monitor the hygienic condition of the tire itself, it must always remain dry, avoid getting powders and lotions under the belts, this can cause inflammation on the baby's skin.
6. When feeding, be especially careful to ensure that the baby's hips do not come together.
The wearing of these devices (orthoses) is long-term - from 3 months to a year, and it is extremely important for the parents of a child who has been diagnosed with hip dysplasia to be patient and not be cowardly during the treatment period and meticulously follow the doctor's prescriptions.
After centering the femoral head, they begin massage and therapeutic exercises aimed at creating the correct ratio of the articular surfaces. We can recommend some exercises that are easy to do at home.
1. In the position of the child lying on his back, we bend the child's legs at the knee and hip joints as much as possible, and then fully straighten them.
2. In the previous starting position, we bend the child's legs at the knee and hip joints at a right angle, moderately spread the hips and, giving a moderate load along the axis of the hips, perform rotational movements with the hips.
3. In the position of the child lying on his back, we breed the legs of the child bent at the knee and hip joints as much as possible to the surface of the table.
All exercises are performed 8-10 times 3-4 times a day.
Also during this period, physiotherapy (paraffin baths, electrophoresis with calcium and phosphorus preparations) is used to improve the nutrition of the joint components and complex orthopedic massage.
In cases of late diagnosis of hip dysplasia or in the absence of adequate treatment in the early stages, treatment is carried out by long-term staged plastering, as well as surgical treatment, but in these cases there are no standard treatment regimens and patient care tactics are developed individually.
After treatment of hip dysplasia, the child should be kept in the dispensary with an orthopedist for a long time - from 3 to 5 years until the end of growth. If necessary, control radiographs are performed once every 2 years to monitor the correct development of the joint. Also, restrictions on the load on the joint are often imposed. For children treated for hip dysplasia, it is desirable to visit specialized orthopedic groups in preschool institutions.
In severe degrees of hip dysplasia, functional disorders are, as a rule, lifelong in nature, even with timely and properly conducted treatment.
So what do the parents of the baby need to do in order to recognize hip dysplasia in time and, if this diagnosis was made to the child, to prevent serious complications?
First of all, it is necessary to show the child to the orthopedist in time. The recommended terms of examination by an orthopedist are 1 month, 3 months, 6 months and 1 year.
If the orthopedist nevertheless made a diagnosis of hip dysplasia, then the effectiveness of treatment by 50 percent depends on the correct and timely fulfillment by the child's parents of the doctor's prescriptions. It is important to remember that the sooner treatment is started, the better the results and the less chance of severe complications. With early diagnosis of hip dysplasia and correct and timely treatment, a positive result is achieved in 96-98% of cases.