What are the symptoms of dairy allergy
Milk allergy - Symptoms and causes
Overview
Milk allergy is an atypical immune system response to milk and products containing milk. It's one of the most common food allergies in children. Cow's milk is the usual cause of milk allergy, but milk from sheep, goats, buffalo and other mammals also can cause a reaction.
An allergic reaction usually occurs soon after you or your child consumes milk. Signs and symptoms of milk allergy range from mild to severe and can include wheezing, vomiting, hives and digestive problems. Milk allergy can also cause anaphylaxis — a severe, life-threatening reaction.
Avoiding milk and milk products is the primary treatment for milk allergy. Fortunately, most children outgrow milk allergy. Those who don't outgrow it may need to continue to avoid milk products.
Products & Services
- Book: Mayo Clinic Family Health Book, 5th Edition
- Newsletter: Mayo Clinic Health Letter — Digital Edition
- Product for Nursing from Mayo Clinic Store
Symptoms
Milk allergy symptoms, which differ from person to person, occur a few minutes to a few hours after you or your child drinks milk or eats milk products.
Immediate signs and symptoms of milk allergy might include:
- Hives
- Wheezing
- Itching or tingling feeling around the lips or mouth
- Swelling of the lips, tongue or throat
- Coughing or shortness of breath
- Vomiting
Signs and symptoms that may take more time to develop include:
- Loose stools or diarrhea, which may contain blood
- Abdominal cramps
- Runny nose
- Watery eyes
- Colic, in babies
Milk allergy or milk intolerance?
A true milk allergy differs from milk protein intolerance and lactose intolerance. Unlike milk allergy, intolerance doesn't involve the immune system. Milk intolerance requires different treatment from true milk allergy.
Common signs and symptoms of milk protein intolerance or lactose intolerance include digestive problems, such as bloating, gas or diarrhea, after consuming milk or products containing milk.
Anaphylaxis
Milk allergy can cause anaphylaxis, a life-threatening reaction that narrows the airways and can block breathing. Milk is the third most common food — after peanuts and tree nuts — to cause anaphylaxis.
If you or your child has a reaction to milk, tell your health care provider, no matter how mild the reaction. Tests can help confirm milk allergy, so you can avoid future and potentially worse reactions.
Anaphylaxis is a medical emergency and requires treatment with an epinephrine (adrenaline) shot (EpiPen, Adrenaclick, others) and a trip to the emergency room. Signs and symptoms start soon after milk consumption and can include:
- Constriction of airways, including a swollen throat that makes it difficult to breathe
- Facial flushing
- Itching
- Shock, with a marked drop in blood pressure
When to see a doctor
See your provider or an allergist if you or your child experiences milk allergy symptoms shortly after consuming milk. If possible, see your provider during the allergic reaction to help make a diagnosis. Seek emergency treatment if you or your child develops signs or symptoms of anaphylaxis.
If possible, see your provider during the allergic reaction to help make a diagnosis. Seek emergency treatment if you or your child develops signs or symptoms of anaphylaxis.
Request an Appointment at Mayo Clinic
From Mayo Clinic to your inbox
Sign up for free, and stay up to date on research advancements, health tips and current health topics, like COVID-19, plus expertise on managing health.
To provide you with the most relevant and helpful information, and understand which
information is beneficial, we may combine your email and website usage information with
other information we have about you. If you are a Mayo Clinic patient, this could
include protected health information. If we combine this information with your protected
health information, we will treat all of that information as protected health
information and will only use or disclose that information as set forth in our notice of
privacy practices.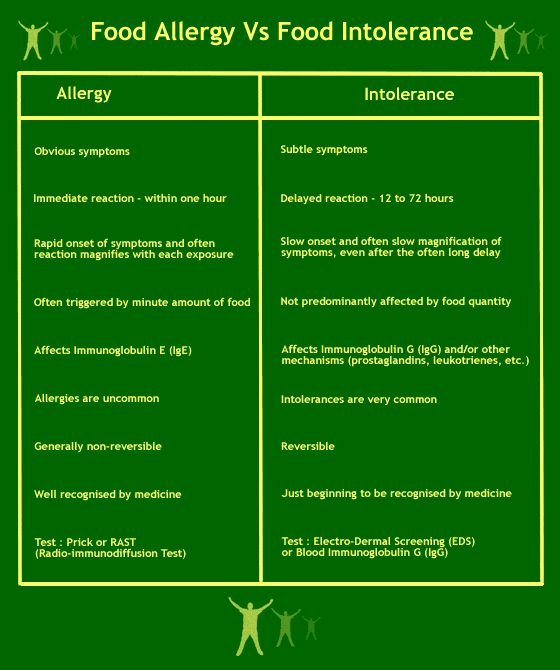 You may opt-out of email communications at any time by clicking on
the unsubscribe link in the e-mail.
You may opt-out of email communications at any time by clicking on
the unsubscribe link in the e-mail.
Causes
All true food allergies are caused by an immune system malfunction. If you have milk allergy, your immune system identifies certain milk proteins as harmful, triggering the production of immunoglobulin E (IgE) antibodies to neutralize the protein (allergen). The next time you come in contact with these proteins, IgE antibodies recognize them and signal your immune system to release histamine and other chemicals, causing a range of allergic signs and symptoms.
There are two main proteins in cow's milk that can cause an allergic reaction:
- Casein, found in the solid part (curd) of milk that curdles
- Whey, found in the liquid part of milk that remains after milk curdles
You or your child may be allergic to only one milk protein or to both. These proteins may be hard to avoid because they're also in some processed foods. And most people who react to cow's milk will react to sheep, goat and buffalo milk.
These proteins may be hard to avoid because they're also in some processed foods. And most people who react to cow's milk will react to sheep, goat and buffalo milk.
Food protein-induced enterocolitis syndrome (FPIES)
A food allergen can also cause what's sometimes called a delayed food allergy. Although any food can be a trigger, milk is one of the most common. The reaction, commonly vomiting and diarrhea, usually occurs within hours after eating the trigger rather than within minutes.
Unlike some food allergies, FPIES usually resolves over time. As with milk allergy, preventing an FPIES reaction involves avoiding milk and milk products.
Risk factors
Certain factors may increase the risk of developing milk allergy:
- Other allergies. Many children who are allergic to milk also have other allergies.
 Milk allergy may develop before other allergies.
Milk allergy may develop before other allergies. - Atopic dermatitis. Children who have atopic dermatitis — a common, chronic inflammation of the skin — are much more likely to develop a food allergy.
- Family history. A person's risk of a food allergy increases if one or both parents have a food allergy or another type of allergy or allergic disease — such as hay fever, asthma, hives or eczema.
- Age. Milk allergy is more common in children. As they age, their digestive systems mature, and their bodies are less likely to react to milk.
Complications
Children who are allergic to milk are more likely to develop certain other health problems, including:
- Nutritional deficiencies. Because of dietary restrictions and feeding challenges, children with milk allergy may have slowed growth as well as vitamin and mineral deficiencies.
- Reduced quality of life.
 Many common, and sometimes unexpected, foods contain milk, including some salad dressings or even hot dogs. If you or your child is severely allergic, avoiding milk exposure may increase stress or anxiety levels when it comes to making food choices.
Many common, and sometimes unexpected, foods contain milk, including some salad dressings or even hot dogs. If you or your child is severely allergic, avoiding milk exposure may increase stress or anxiety levels when it comes to making food choices.
Prevention
There's no sure way to prevent a food allergy, but you can prevent reactions by avoiding the food that causes them. If you know you or your child is allergic to milk, avoid milk and milk products.
Read food labels carefully. Look for casein, a milk derivative, which can be found in some unexpected places, such as in some canned tuna, sausage or nondairy products. Question ingredients when ordering in restaurants.
Sources of milk
Obvious sources of allergy-causing milk proteins are found in dairy products, including:
- Whole milk, low-fat milk, skim milk, buttermilk
- Butter
- Yogurt
- Ice cream, gelato
- Cheese and anything that contains cheese
- Half-and-half
Milk can be harder to identify when it's used as an ingredient in processed foods, including baked goods and processed meats.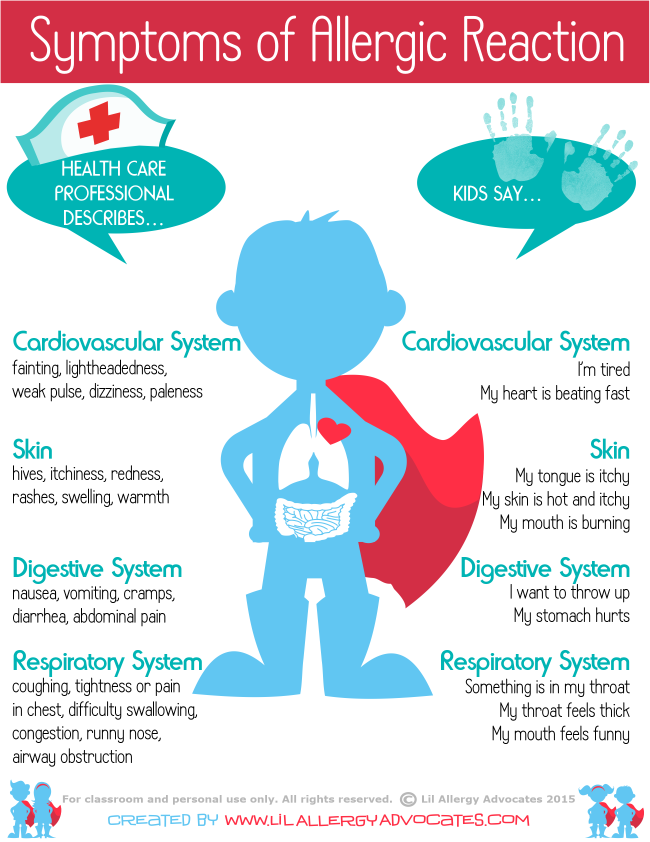 Hidden sources of milk include:
Hidden sources of milk include:
- Whey
- Casein
- Ingredients spelled with the prefix "lact" — such as lactose and lactate
- Candies, such as chocolate, nougat and caramel
- Protein powders
- Artificial butter flavor
- Artificial cheese flavor
- Hydrolysates
Even if a food is labeled "milk-free" or "nondairy," it may contain allergy-causing milk proteins — so you have to read the label carefully. When in doubt, contact the manufacturer to be sure a product doesn't contain milk ingredients.
When eating out, ask how foods have been prepared. Does your steak have melted butter on it? Was your seafood dipped in milk before cooking?
If you're at risk of a serious allergic reaction, talk with your health care provider about carrying and using emergency epinephrine (adrenaline). If you have already had a severe reaction, wear a medical alert bracelet or necklace that lets others know you have a food allergy.
Milk alternatives for infants
In children who are allergic to milk, breastfeeding and the use of hypoallergenic formula can prevent allergic reactions.
- Breastfeeding is the best source of nutrition for your infant. Breastfeeding for as long as possible is recommended, especially if your infant is at high risk of developing milk allergy.
-
Hypoallergenic formulas are produced by using enzymes to break down (hydrolyze) milk proteins, such as casein or whey. Further processing can include heat and filtering. Depending on their level of processing, products are classified as either partially or extensively hydrolyzed. Or they may also be called elemental formulas.
Some hypoallergenic formulas aren't milk based, but instead contain amino acids. Besides extensively hydrolyzed products, amino-acid-based formulas are the least likely to cause an allergic reaction.
- Soy-based formulas are based on soy protein instead of milk.
 Soy formulas are fortified to be nutritionally complete — but, unfortunately, some children with a milk allergy also develop an allergy to soy.
Soy formulas are fortified to be nutritionally complete — but, unfortunately, some children with a milk allergy also develop an allergy to soy.
If you're breastfeeding and your child is allergic to milk, cow's milk proteins passed through your breast milk may cause an allergic reaction. You may need to exclude from your diet all products that contain milk. Talk to your health care provider if you know — or suspect — that your child has milk allergy and develops allergy signs and symptoms after breastfeeding.
If you or your child is on a milk-free diet, your health care provider or dietitian can help you plan nutritionally balanced meals. You or your child may need to take supplements to replace calcium and nutrients found in milk, such as vitamin D and riboflavin.
By Mayo Clinic Staff
Related
Associated Procedures
Products & Services
Lactose intolerance - Symptoms and causes
Overview
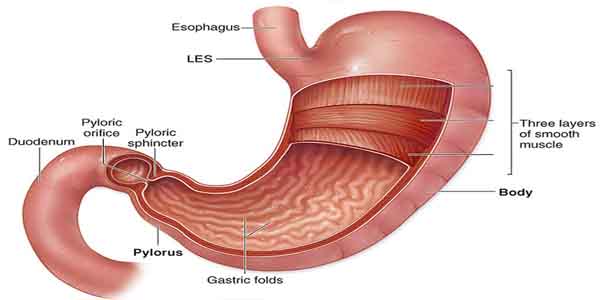
Small intestine
Small intestine
The small intestine is a hollow tube that runs from the stomach to the large intestine (colon).
People with lactose intolerance are unable to fully digest the sugar (lactose) in milk. As a result, they have diarrhea, gas and bloating after eating or drinking dairy products. The condition, which is also called lactose malabsorption, is usually harmless, but its symptoms can be uncomfortable.
Too little of an enzyme produced in your small intestine (lactase) is usually responsible for lactose intolerance. You can have low levels of lactase and still be able to digest milk products. But if your levels are too low you become lactose intolerant, leading to symptoms after you eat or drink dairy.
Most people with lactose intolerance can manage the condition without having to give up all dairy foods.
Products & Services
- Book: Mayo Clinic Book of Home Remedies
- Book: Mayo Clinic Family Health Book, 5th Edition
- Newsletter: Mayo Clinic Health Letter — Digital Edition
Symptoms
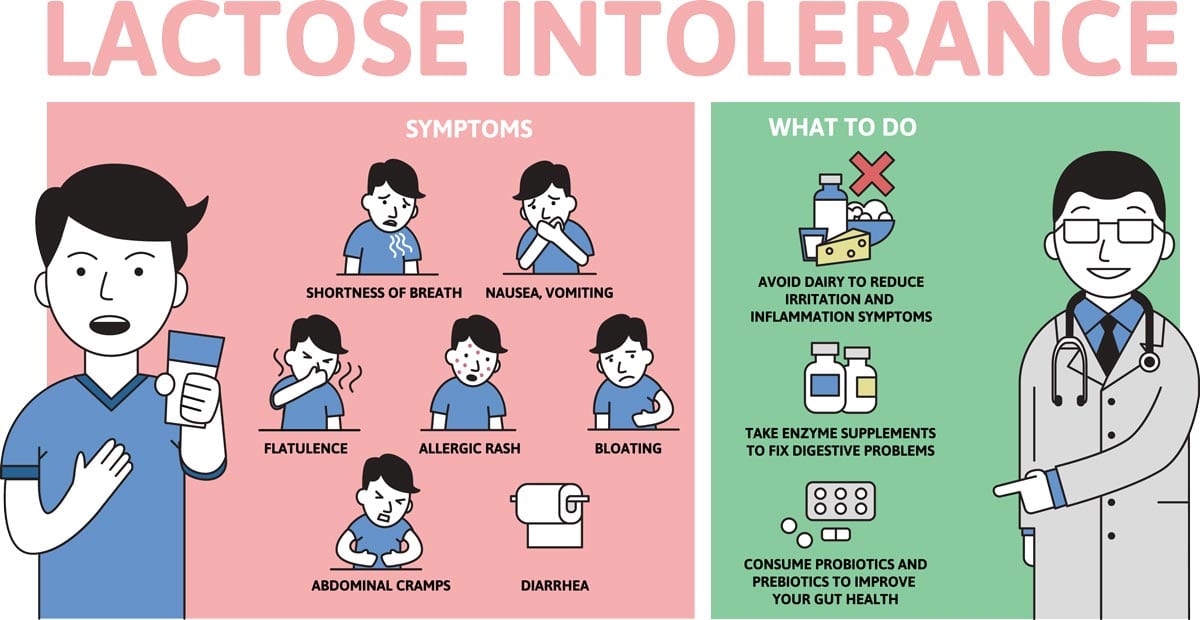
The signs and symptoms of lactose intolerance usually begin from 30 minutes to two hours after eating or drinking foods that contain lactose. Common signs and symptoms include:
Common signs and symptoms include:
- Diarrhea
- Nausea, and sometimes, vomiting
- Stomach cramps
- Bloating
- Gas
When to see a doctor
Make an appointment with your doctor if you frequently have symptoms of lactose intolerance after eating dairy foods, particularly if you're worried about getting enough calcium.
Request an Appointment at Mayo Clinic
Get the latest health information from Mayo Clinic delivered to your inbox.
Subscribe for free and receive your in-depth guide to digestive health, plus the latest on health innovations and news. You can unsubscribe at any time.
Email address
To provide you with the most relevant and helpful information, and understand which information is beneficial, we may combine your email and website usage information with other information we have about you. If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
If you are a Mayo Clinic patient, this could include protected health information. If we combine this information with your protected health information, we will treat all of that information as protected health information and will only use or disclose that information as set forth in our notice of privacy practices. You may opt-out of email communications at any time by clicking on the unsubscribe link in the e-mail.
Causes
Lactose intolerance occurs when your small intestine doesn't produce enough of an enzyme (lactase) to digest milk sugar (lactose).
Normally, lactase turns milk sugar into two simple sugars — glucose and galactose — which are absorbed into the bloodstream through the intestinal lining.
If you're lactase deficient, lactose in your food moves into the colon instead of being processed and absorbed. In the colon, normal bacteria interact with undigested lactose, causing the signs and symptoms of lactose intolerance.
In the colon, normal bacteria interact with undigested lactose, causing the signs and symptoms of lactose intolerance.
There are three types of lactose intolerance. Different factors cause the lactase deficiency underlying each type.
Primary lactose intolerance
People who develop primary lactose intolerance — the most common type — start life producing enough lactase. Infants, who get all their nutrition from milk, need lactase.
As children replace milk with other foods, the amount of lactase they produce normally drops, but usually remains high enough to digest the amount of dairy in a typical adult diet. In primary lactose intolerance, lactase production falls off sharply by adulthood, making milk products difficult to digest.
Secondary lactose intolerance
This form of lactose intolerance occurs when your small intestine decreases lactase production after an illness, injury or surgery involving your small intestine. Diseases associated with secondary lactose intolerance include intestinal infection, celiac disease, bacterial overgrowth and Crohn's disease.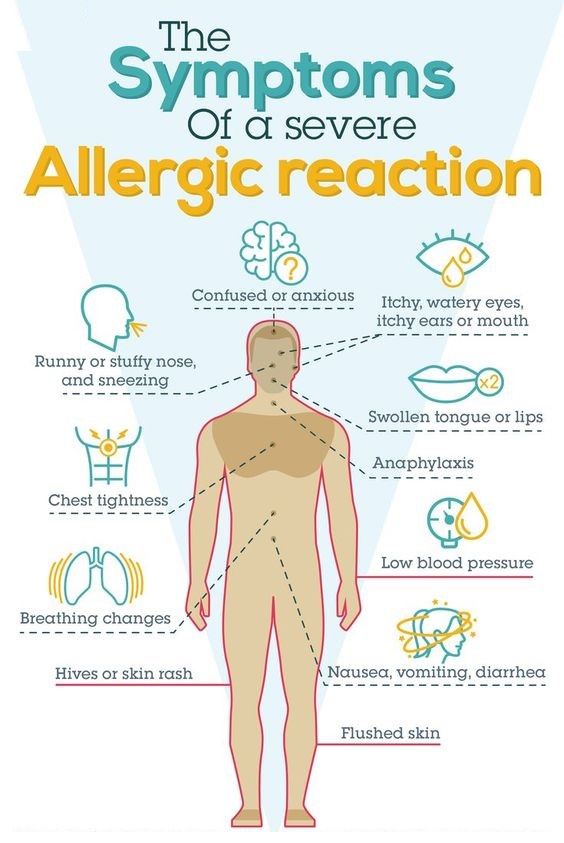
Treatment of the underlying disorder might restore lactase levels and improve signs and symptoms, though it can take time.
Congenital or developmental lactose intolerance
It's possible, but rare, for babies to be born with lactose intolerance caused by a lack of lactase. This disorder is passed from generation to generation in a pattern of inheritance called autosomal recessive, meaning that both the mother and the father must pass on the same gene variant for a child to be affected. Premature infants can also have lactose intolerance because of an insufficient lactase level.
Risk factors
Factors that can make you or your child more prone to lactose intolerance include:
- Increasing age. Lactose intolerance usually appears in adulthood. The condition is uncommon in babies and young children.
- Ethnicity. Lactose intolerance is most common in people of African, Asian, Hispanic and American Indian descent.

- Premature birth. Infants born prematurely might have reduced levels of lactase because the small intestine doesn't develop lactase-producing cells until late in the third trimester.
- Diseases affecting the small intestine. Small intestine problems that can cause lactose intolerance include bacterial overgrowth, celiac disease and Crohn's disease.
- Certain cancer treatments. If you've had radiation therapy for cancer in your stomach or you have intestinal complications from chemotherapy, your risk of developing lactose intolerance increases.
By Mayo Clinic Staff
Related
Products & Services
Good to know about MILK ALLERGY (melk)
MILK ALLERGY
Useful information about milk allergy – Information sheet of the Norwegian Asthma and Allergy Association
What is milk allergy?
When allergic to cow's milk protein, a strong reaction of the body's immune system may be the production of antibodies (IgE), or the activation of inflammatory cells.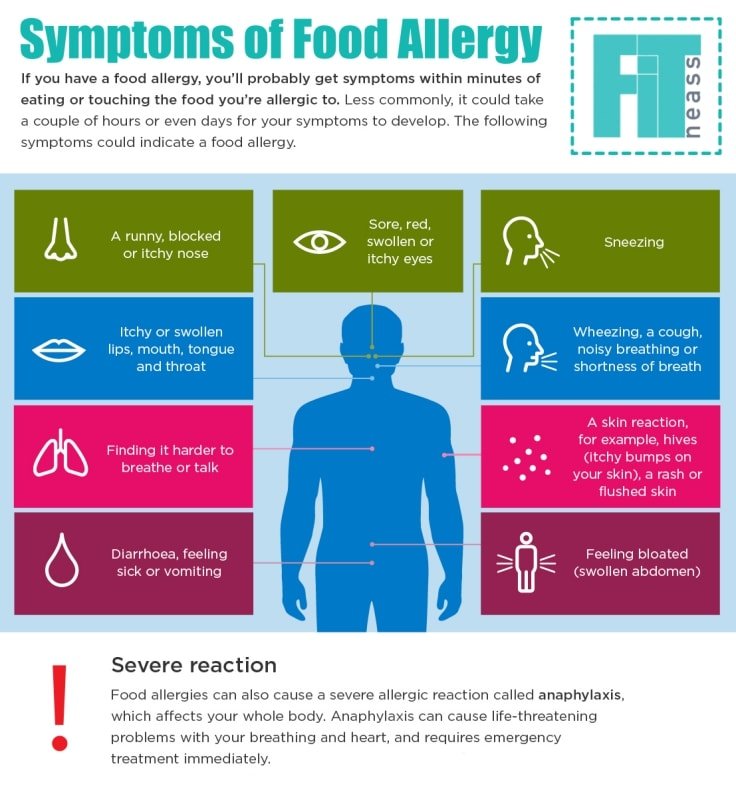 With every meal containing milk proteins, an allergic reaction of the immune system is observed in the form of the production of mediators, such as histamine, or a T-cell inflammatory reaction. Histamine is produced in several places in the body and leads to symptoms such as diarrhea, nausea, abdominal pain, or skin lesions (urticaria, eczema).
With every meal containing milk proteins, an allergic reaction of the immune system is observed in the form of the production of mediators, such as histamine, or a T-cell inflammatory reaction. Histamine is produced in several places in the body and leads to symptoms such as diarrhea, nausea, abdominal pain, or skin lesions (urticaria, eczema).
Cow's milk contains over 25 different proteins that can cause a reaction in "milk" allergies. For most people, an allergic reaction can be caused by more than one type of protein. The milk of other artiodactyls such as goat, horse and buffalo contains many of the same proteins. Therefore, allergy sufferers should not consume artiodactyl milk at all.
If a breastfeeding mother consumes cow's milk herself, some proteins may be transferred with breast milk to the baby's body and lead to negative consequences. Therefore, a breastfeeding mother should follow a dairy-free diet.
Cow's milk allergy is not the same as lactose intolerance.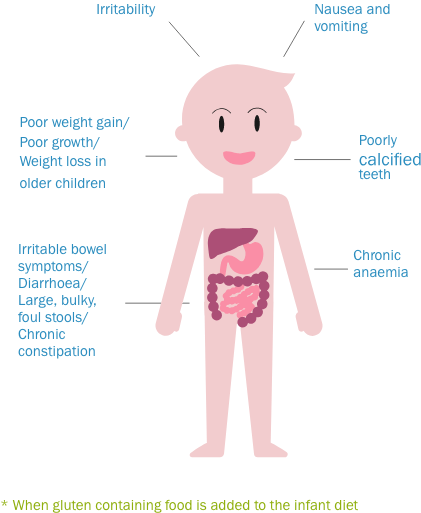 The latter occurs due to the reduced ability of the body to digest milk sugar (lactose). Lactose intolerance leads to stomach pain and diarrhea as a consequence of eating large amounts of dairy products with high levels of lactose (sweet milk, brown (goat) cheese, ice cream and cream).
The latter occurs due to the reduced ability of the body to digest milk sugar (lactose). Lactose intolerance leads to stomach pain and diarrhea as a consequence of eating large amounts of dairy products with high levels of lactose (sweet milk, brown (goat) cheese, ice cream and cream).
Symptoms
The symptoms of a milk allergy are very individual. For some, they are minor and harmless, while for others, a severe allergic reaction can occur, even when drinking a small amount of milk. Gastrointestinal tract disorder is common. Not so often there is itching in the mouth and throat, swelling of the mucous membrane and breathing problems, which is especially true for young children. It is also common for them to develop eczema and hives on the skin.
Who is affected?
Milk allergy is the most common type of allergy in young children, which is explained by the early introduction of cow's milk into the diet of infants (eg cereals or mother's milk substitute).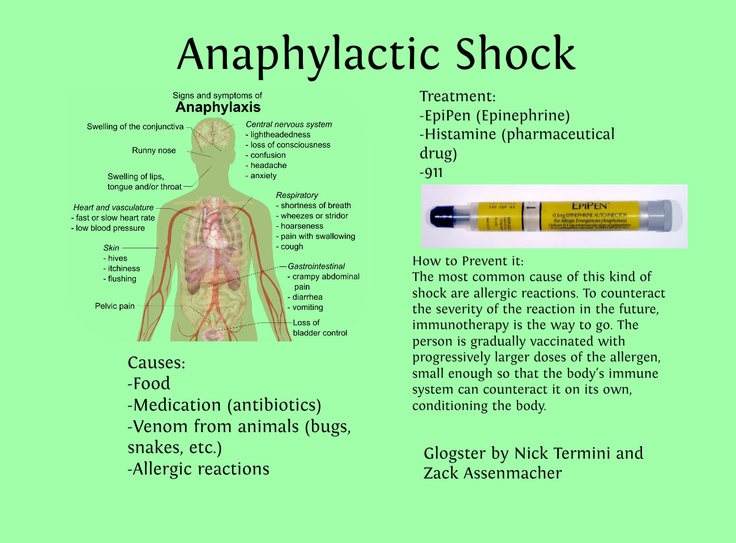 About 2-5% of Norwegian babies (0-3 years old) suffer from this type of allergy.
About 2-5% of Norwegian babies (0-3 years old) suffer from this type of allergy.
Diagnosis
In order to determine the presence of milk allergy, the doctor must read the patient's medical history, as well as take a blood test for allergic antibodies and a Pirquet test. Not all milk allergy sufferers will show positive results from these tests. This is especially true for infants with symptoms such as vomiting, diarrhea, or blood in the stool. The only reliable way to find out if milk causes these symptoms is to eliminate milk from the diet for a period of time. When in doubt, reintroduce it back into the diet and see if symptoms return. For children who have not received milk for some time due to allergies, a control test using cow's milk should be performed to ensure that there is no allergic reaction.
Predictions
Generally, cow's milk allergy has a fairly good prognosis. Most of the children get rid of it before reaching school age. Babies who have had negative test results are often allowed to resume milk intake after half a year or a year. It is not known how many adults suffer from milk allergy, but it is estimated that this number does not exceed one percent of the population.
Babies who have had negative test results are often allowed to resume milk intake after half a year or a year. It is not known how many adults suffer from milk allergy, but it is estimated that this number does not exceed one percent of the population.
Where is milk protein found?
Milk is found in many processed and prepared industrial foods. Therefore, when buying a product, it is important to familiarize yourself with the list of substances contained in it. The goods declaration must list all ingredients containing milk. A certain group of words used in such lists indicates the content of milk protein in the product: butter, yogurt, yogurt powder.
Cocoa butter, lactic acids and group E substances do not contain milk protein.
Diet
Milk is an important source of nutrients in the Norwegian diet. 25% of the protein given to children, 70% of the iodine and about 70% of the calcium are obtained from dairy products. That is why, in cases of exclusion of dairy products from the diet, these products should be replaced with others that will provide the intake of the above nutrients. Alternatively, specially formulated additives can be used.
What can replace milk?
- Drinks: For small children, a hypoallergenic milk substitute is recommended, available from a pharmacy. These products can be purchased at a pharmacy or obtained from a blue prescription (prescription prescription). Because older children can be difficult to accustom to these milk substitutes due to their taste, it is recommended to start using substitutes as early as possible, for example during breastfeeding. Youth and adults can consume milk substitutes such as rice milk, oat milk, etc. The amount of calcium contained in these products corresponds to the calcium content in cow's milk, however, these drinks often contain less protein and nutrients.
- Cooking: Pharmaceutical-purchased milk substitutes can be used in most meals. Depending on what you are cooking, you can use soy, rice or coconut milk.
- Other substitutes: The following products are available in a dairy-free version - margarine, sour cream, yogurt, ice cream and cream substitutes based on soy, rice or oats.
Allergist Section
Section for a practicing allergist | Remedium.ruPopular
- Russia and Turkey discussed the prospects for cooperation in the field of medicine and pharmaceuticals
- The Ministry of Health published a form for obtaining a prescription drug through online sale
- Innovative drugs in Russia: reality and prospects
- RAAS will take the initiative to limit the number of pharmacies in the country
- Unite to help millions of people
The section is only for specialists in the field of medicine, pharmacy and healthcare!
Item not found!
Latest Articles
10/19/2022
Anticoagulant therapy with direct oral anticoagulants in polypharmacy: a course towards safety
10/18/2022
Inosine pranobex in the treatment of mild cervical intraepithelial neoplasia (clinical experience)
10/17/2022
Efficacy of an esophagoprotector in the treatment of patients with gastroesophageal reflux disease: a systematic review
10/14/2022
Dental anomalies: classification, causes and treatment
10/13/2022
Painful sexual disorder
10/11/2022
Diagnosis of disorders in the coagulation system, assessment of the risk of hemorrhagic complications in severe cirrhosis/liver diseases according to global screening tests of the hemostasis system and principles for their correction: guidelines
| Login: | |
| Password: | |
| Remember me | |
| Registration | |
| Forgot your password? | |
Subscription Online
Books Magazines
News
October 19, 2022
Innovative drugs in Russia: reality and prospects
Clinical research cannot be canceled - where to put a comma?
More
October 19, 2022
It is planned to transfer 14 high-cost nosologies to the Circle of Kindness Foundation
October 19, 2022
Name of academician Chazov immortalized in Moscow and Nizhny Novgorod
/doctor/allergology/allergiya-na-moloko-proyavlenie-diagnostika-trechenie/%231
Doctors
October 19, 2022
Anticoagulant therapy with direct oral anticoagulants in polypharmacy: a course towards safety
I.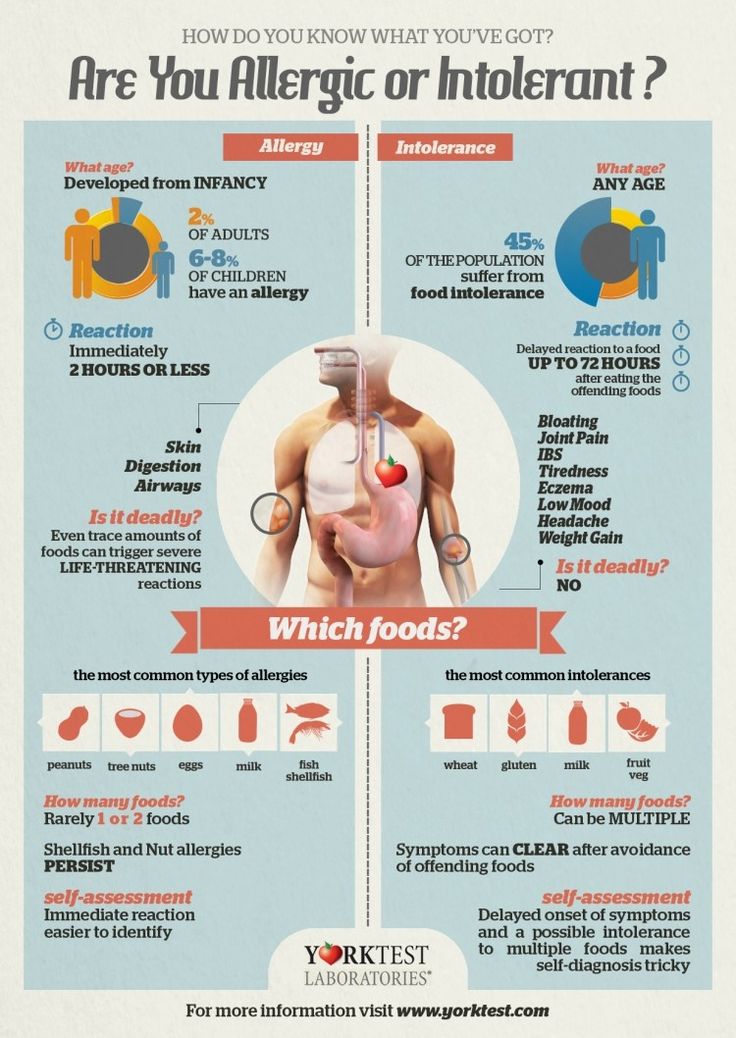 N. Sychev 1.2 L.V. Fedina 1.2 , D.A. Gabrielyan 1 , etc. Rastvorova 1 , E.V. Strigunkova 1 , K.B...
N. Sychev 1.2 L.V. Fedina 1.2 , D.A. Gabrielyan 1 , etc. Rastvorova 1 , E.V. Strigunkova 1 , K.B...
More
October 18, 2022
Inosine pranobex in the treatment of mild cervical intraepithelial neoplasia (clinical experience)
October 17, 2022
Efficacy of an esophagoprotector in the treatment of patients with gastroesophageal reflux disease: a systematic review
Pharmacists
August 30, 2022
Release of a large number of packages of an OTC drug at once
A customer asked for 20 packs of OTC, but the man following her.