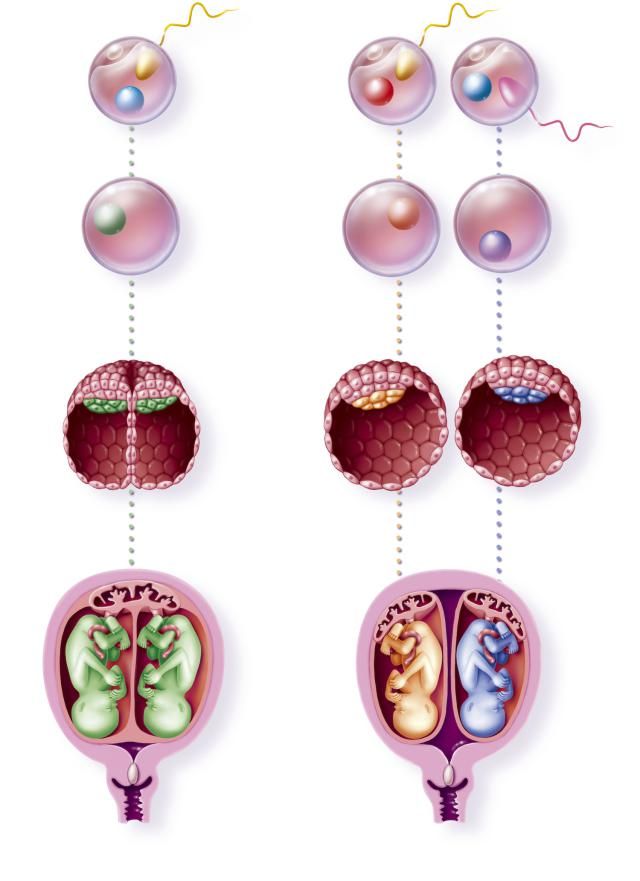
Types of identical twins pregnancy
Multiple Pregnancy | ACOG
-
A pregnancy with more than one fetus is called a multiple pregnancy.
-
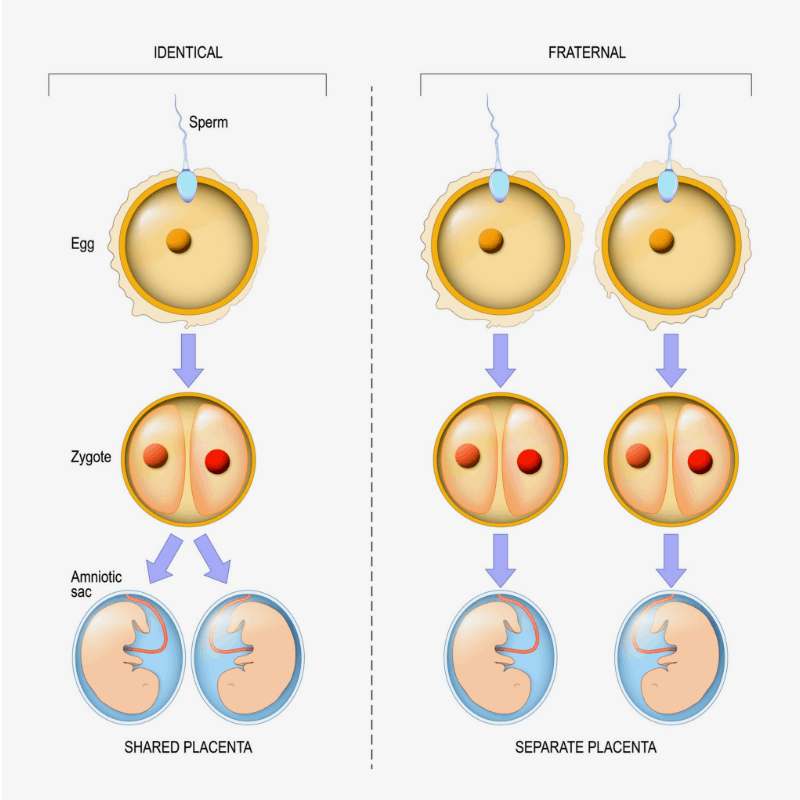
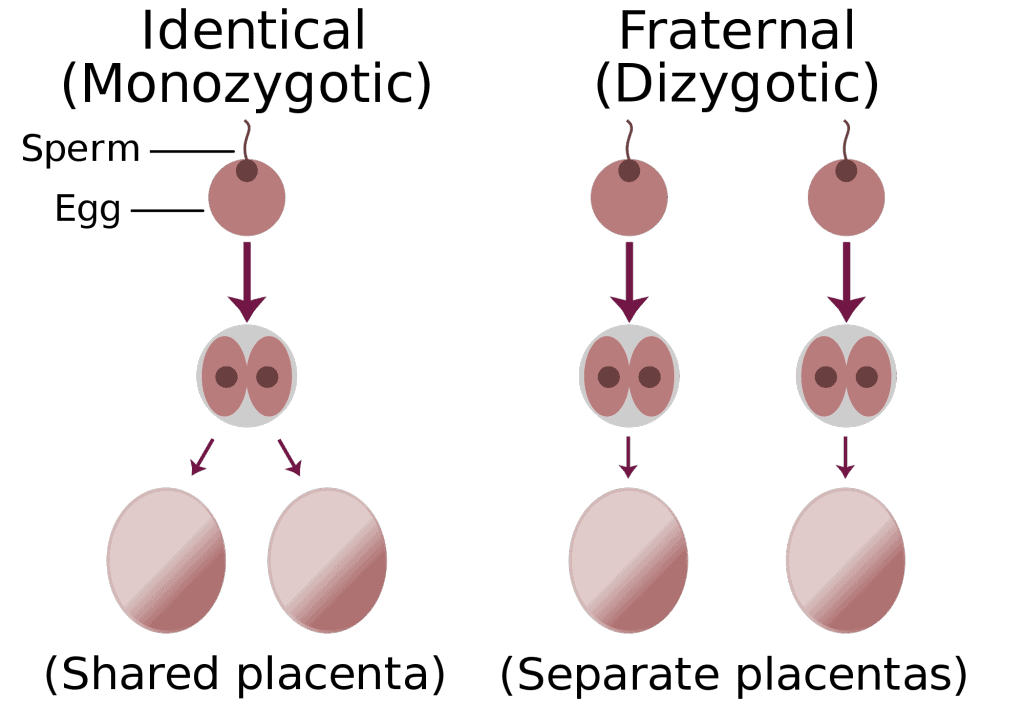
If more than one egg is released during the menstrual cycle and each egg is fertilized by a sperm, more than one embryo may implant and grow in the uterus. This type of pregnancy results in fraternal twins (or more). When a single fertilized egg splits, it results in multiple identical embryos. This type of pregnancy results in identical twins (or more). Fraternal twins are more common than identical twins.
-
The use of fertility drugs to induce ovulation often causes more than one egg to be released from the ovaries and can result in twins, triplets, or more.
In vitro fertilization (IVF) can lead to a multiple pregnancy if more than one embryo is transferred to the uterus.
Identical multiples also may result if the fertilized egg splits after transfer.
Women older than age 35 are more likely to release two or more eggs during a single menstrual cycle than younger women. So older women are more likely than younger women to become pregnant with multiples.
-
Women who are pregnant with multiples may have more severe morning sickness or breast tenderness than women who are pregnant with a single fetus. They also may gain weight more quickly. Most multiple pregnancies are discovered during an ultrasound exam.
-
Most women who are pregnant with multiples need to gain more weight than women who are pregnant with one fetus. An extra 300 calories a day is needed for each fetus. For example, if you are pregnant with twins, you need an extra 600 calories a day.
 For triplets and more, talk with your obstetrician–gynecologist (ob-gyn) about the right amount of weight gain for your pregnancy.
For triplets and more, talk with your obstetrician–gynecologist (ob-gyn) about the right amount of weight gain for your pregnancy. -
Staying active during multiple pregnancy is important for your health, but you may need to avoid strenuous exercise. Try low-impact exercise, such as swimming, prenatal yoga, and walking. You should aim for 30 minutes of exercise a day. If problems arise during your pregnancy, your ob-gyn may recommend that you avoid exercise.
-
You likely will have more frequent prenatal care visits with your ob-gyn. Starting in your second trimester, you may have ultrasound exams every 4 to 6 weeks. If a problem is suspected, you may have special tests or more frequent ultrasound exams.
-
The most common complication of multiple pregnancy is preterm birth.
 More than one half of all twins are born preterm. Triplets and more are almost always born preterm.
More than one half of all twins are born preterm. Triplets and more are almost always born preterm. -
Babies born before 37 weeks of pregnancy may have an increased risk of short-term and long-term health problems, including problems with breathing, eating, and staying warm. Other problems, such as learning and behavioral disabilities, may appear later in childhood or even in adulthood. Very preterm babies (those who are born before 32 weeks of pregnancy) can die or have severe health problems, even with the best of care.
Preterm multiples also have a greater risk of serious complications that can lead to cerebral palsy. Children born with problems related to being preterm may need lifelong medical care.
-
Early in a multiple pregnancy, an ultrasound exam is done to find out whether each fetus has its own chorion (chorionicity) and amniotic sac (amnionicity).
 There are three types of twins:
There are three types of twins:-
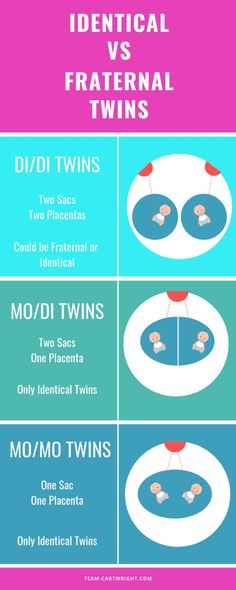
Dichorionic–diamniotic—Twins who have their own chorions and amniotic sacs. They typically do not share a placenta and can be fraternal or identical.
-
Monochorionic–diamniotic—Twins who share a chorion but have separate amniotic sacs. They share a placenta and are identical.
-
Monochorionic–monoamniotic—Twins who share one chorion and one amniotic sac. They share a placenta and are identical.
-
-
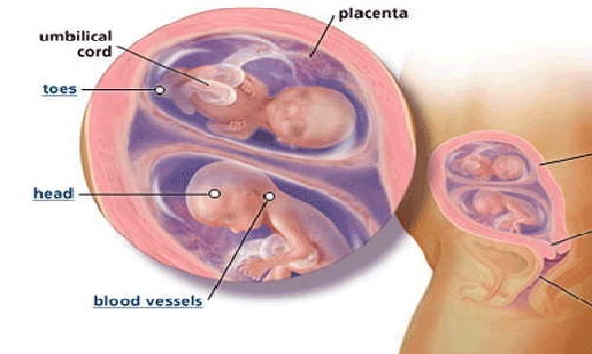
Monochorionic twins have a higher risk of complications than those with separate placentas. One problem that can occur in monochorionic–diamniotic babies is twin–twin transfusion syndrome (TTTS). In TTTS, the blood flow between the twins becomes unbalanced. One twin donates blood to the other twin. The donor twin has too little blood, and the recipient twin has too much blood.
 The earlier TTTS occurs in the pregnancy, the more serious the outcomes for one or both babies.
The earlier TTTS occurs in the pregnancy, the more serious the outcomes for one or both babies.Although monochorionic–monoamniotic babies are rare, this type of pregnancy is very risky. The most common problem is an umbilical cord complication. Women with this type of pregnancy are monitored more frequently and are likely to have a cesarean birth.
-
Preeclampsia is a blood pressure disorder that usually starts after 20 weeks of pregnancy or after childbirth. It occurs more often in multiple pregnancies than in singleton pregnancies. It also tends to occur earlier and is more severe in multiple pregnancies.
Preeclampsia can damage many organs in your body, most commonly your kidneys, liver, brain, and eyes. Preeclampsia that worsens and causes seizures is called eclampsia. When preeclampsia occurs during pregnancy, the babies may need to be delivered right away, even if they are not fully grown.

-
Women carrying multiples have a high risk of gestational diabetes. This condition can increase the risk of preeclampsia and of developing diabetes mellitus later in life. Newborns may have breathing problems or low blood sugar levels. Diet, exercise, and sometimes medication can reduce the risk of these complications.
-
Multiples are more likely to have growth problems than single babies. Multiples are called discordant if one fetus is much smaller than the others.
Discordant growth is common with multiples. It does not always signal a problem. Sometimes, though, a fetus’s restricted growth may be caused by an infection, TTTS, or a problem with the placenta or umbilical cord. If growth restriction is suspected in one or both fetuses, frequent ultrasound exams may be done to track how the fetuses are growing.

-
Screening tests for genetic disorders that use a sample of a woman's blood are not as sensitive in multiple pregnancy. It is possible to have a positive screening test result when no problem is present in either fetus.
-
Diagnostic tests for birth defects include chorionic villus sampling (CVS) and amniocentesis. These tests are harder to perform in multiples because each fetus must be tested. There also is a small risk of loss of one or all of the fetuses. Results of these tests may show that one fetus has a disorder, while the others do not.
-
The chance of cesarean birth is higher with multiples. In some cases, twins can be delivered by vaginal birth. How your babies are born depends on
-
the number of babies and the position, weight, and health of each baby
-
your health and how your labor is going
-
the experience of your ob-gyn
-
-
Having multiples might increase your risk of postpartum depression.
 If you have intense feelings of sadness, anxiety, or despair that keep you from being able to do your daily tasks, talk with your ob-gyn or other member of your health care team.
If you have intense feelings of sadness, anxiety, or despair that keep you from being able to do your daily tasks, talk with your ob-gyn or other member of your health care team. -
Yes, but it may take some practice. Your milk supply will increase to the right amount. You will need to eat healthy foods and drink plenty of liquids. Lactation specialists are available at many hospitals and in your community to help you work out any problems you may have.
[See How to Prepare for Breastfeeding in the Month Before Birth]
-
Amniocentesis: A procedure in which amniotic fluid and cells are taken from the uterus for testing. The procedure uses a needle to withdraw fluid and cells from the sac that holds the fetus.
Amnionicity: The number of amniotic (inner) membranes that surround fetuses in a multiple pregnancy.
 When multiple fetuses have only one amnion, they share an amniotic sac.
When multiple fetuses have only one amnion, they share an amniotic sac.Amniotic Sac: Fluid-filled sac in a woman’s uterus. The fetus develops in this sac.
Birth Defects: Physical problems that are present at birth.
Cerebral Palsy: A disorder of the nervous system that affects movement, posture, and coordination. This disorder is present at birth.
Cesarean Birth: Birth of a fetus from the uterus through an incision made in the woman’s abdomen.
Chorion: The outer membrane that surrounds the fetus.
Chorionic Villus Sampling (CVS): A procedure in which a small sample of cells is taken from the placenta and tested.
Chorionicity: The number of chorionic (outer) membranes that surround the fetuses in a multiple pregnancy.
Complication: A disease or condition that happens as a result of another disease or condition.
 An example is pneumonia that occurs as a result of the flu. A complication also can occur as a result of a condition, such as pregnancy. An example of a pregnancy complication is preterm labor.
An example is pneumonia that occurs as a result of the flu. A complication also can occur as a result of a condition, such as pregnancy. An example of a pregnancy complication is preterm labor.Diabetes Mellitus: A condition in which the levels of sugar in the blood are too high.
Diagnostic Tests: Tests that look for a disease or cause of a disease.
Discordant: A large difference in the size of fetuses in a multiple pregnancy.
Eclampsia: Seizures occurring in pregnancy or after pregnancy that are linked to high blood pressure.
Egg: The female reproductive cell made in and released from the ovaries. Also called the ovum.
Embryo: The stage of development that starts at fertilization (joining of an egg and sperm) and lasts up to 8 weeks.
Fetus: The stage of human development beyond 8 completed weeks after fertilization.
Fraternal Twins: Twins that have developed from two different fertilized eggs.
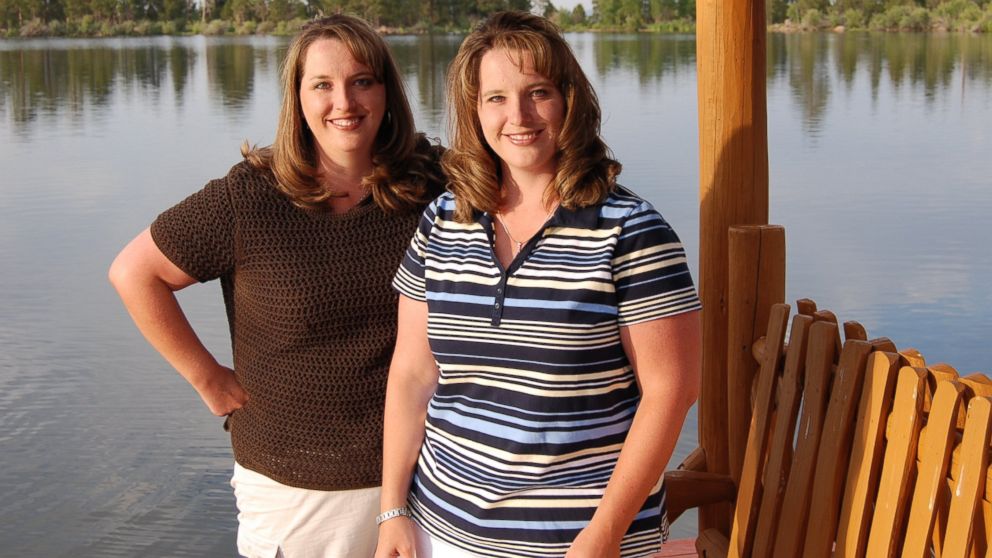
Genetic Disorders: Disorders caused by a change in genes or chromosomes.
Gestational Diabetes: Diabetes that starts during pregnancy.
Identical Twins: Twins that have developed from a single fertilized egg that are usually genetically identical.
In Vitro Fertilization (IVF): A procedure in which an egg is removed from a woman’s ovary, fertilized in a laboratory with the man’s sperm, and then transferred to the woman’s uterus to achieve a pregnancy.
Menstrual Cycle: The monthly process of changes that occur to prepare a woman’s body for possible pregnancy. A menstrual cycle is defined as the first day of menstrual bleeding of one cycle to the first day of menstrual bleeding of the next cycle.
Multiple Pregnancy: A pregnancy where there are two or more fetuses.
Obstetrician–Gynecologist (Ob-Gyn): A doctor with special training and education in women’s health.

Ovaries: Organs in women that contain the eggs necessary to get pregnant and make important hormones, such as estrogen, progesterone, and testosterone.
Ovulation: The time when an ovary releases an egg.
Placenta: An organ that provides nutrients to and takes waste away from the fetus.
Postpartum Depression: A type of depressive mood disorder that develops in the first year after the birth of a child. This type of depression can affect a woman’s ability to take care of her child.
Preeclampsia: A disorder that can occur during pregnancy or after childbirth in which there is high blood pressure and other signs of organ injury. These signs include an abnormal amount of protein in the urine, a low number of platelets, abnormal kidney or liver function, pain over the upper abdomen, fluid in the lungs, or a severe headache or changes in vision.
Prenatal Care: A program of care for a pregnant woman before the birth of her baby.

Preterm: Less than 37 weeks of pregnancy.
Screening Tests: Tests that look for possible signs of disease in people who do not have signs or symptoms.
Sperm: A cell made in the male testicles that can fertilize a female egg.
Twin–Twin Transfusion Syndrome (TTTS): A condition of identical twins in which one twin gets more blood than the other during pregnancy.
Ultrasound Exam: A test in which sound waves are used to examine inner parts of the body. During pregnancy, ultrasound can be used to check the fetus.
Umbilical Cord: A cord-like structure containing blood vessels. It connects the fetus to the placenta.
Uterus: A muscular organ in the female pelvis. During pregnancy, this organ holds and nourishes the fetus. Also called the womb.
Don't have an ob-gyn? Search for doctors near you.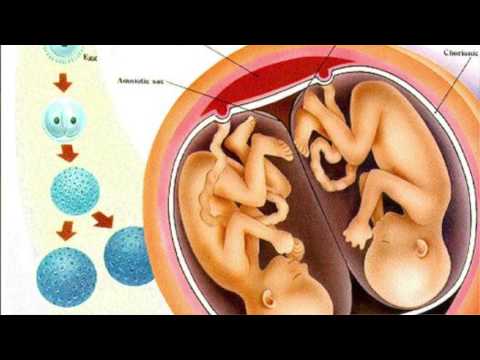
FAQ188
Last updated: February 2021
Last reviewed: June 2020
Copyright 2022 by the American College of Obstetricians and Gynecologists. All rights reserved. Read copyright and permissions information.
This information is designed as an educational aid for the public. It offers current information and opinions related to women's health. It is not intended as a statement of the standard of care. It does not explain all of the proper treatments or methods of care. It is not a substitute for the advice of a physician. Read ACOG’s complete disclaimer.
Twins - identical and fraternal
Multiple births are more common than they were in the past, due to the advancing average age of mothers and the associated rise in assisted reproductive techniques, in particular the use of fertility drugs. Twins account for over 90 per cent of multiple births. There are two types of twins – identical (monozygotic) and fraternal (dizygotic).
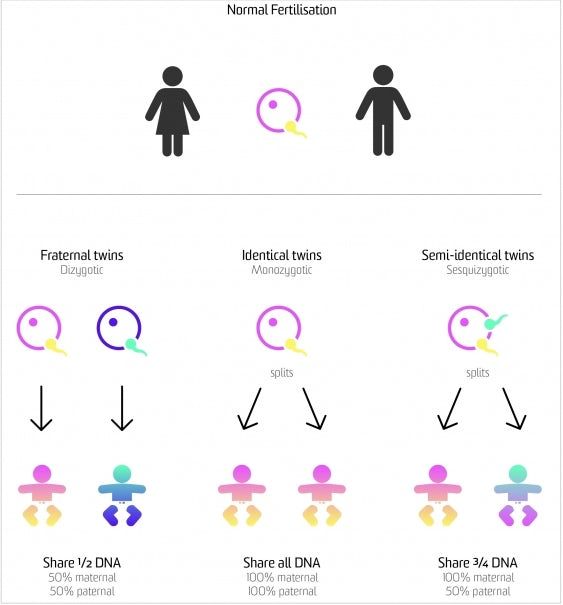
To form identical twins, one fertilised egg (ovum) splits and develops two babies with exactly the same genetic information. This differs from fraternal twins, where two eggs (ova) are fertilised by two sperm and produce two genetically unique children, who are no more alike than individual siblings born at different times. Twins are more or less equally likely to be female or male. Contrary to popular belief, the incidence of twins doesn’t skip generations.
This differs from fraternal twins, where two eggs (ova) are fertilised by two sperm and produce two genetically unique children, who are no more alike than individual siblings born at different times. Twins are more or less equally likely to be female or male. Contrary to popular belief, the incidence of twins doesn’t skip generations.
Factors that increase the odds of having twins
Some women are more likely than others to give birth to twins. The factors that increase the odds include:
- Advancing age of the mother – women in their 30s and 40s have higher levels of the sex hormone oestrogen than younger women, which means that their ovaries are stimulated to produce more than one egg at a time.
- Number of previous pregnancies – the greater the number of pregnancies a woman has already had, the higher her odds of conceiving twins.
- Heredity – a woman is more likely to conceive fraternal twins if she is a fraternal twin, has already had fraternal twins, or has siblings who are fraternal twins.
- Race – Black African women have the highest incidence of twins, while Asian women have the lowest.
- Assisted reproductive techniques – many procedures rely on stimulating the ovaries with fertility drugs to produce eggs and, often, several eggs are released per ovulation.
Fertilisation
Hormones secreted by the ovaries, and a small gland in the brain called the pituitary, control the menstrual cycle. The average cycle is around 28 days. After a menstrual period, rising levels of the hormone oestrogen help to thicken the lining of the womb (the endometrium) and release an egg from one of the ovaries (ovulation).
If the egg is fertilised on its journey down the fallopian tube, it lodges in the thickened womb lining, starts dividing and evolves into an embryo.
Identical or ‘monozygotic’ twins
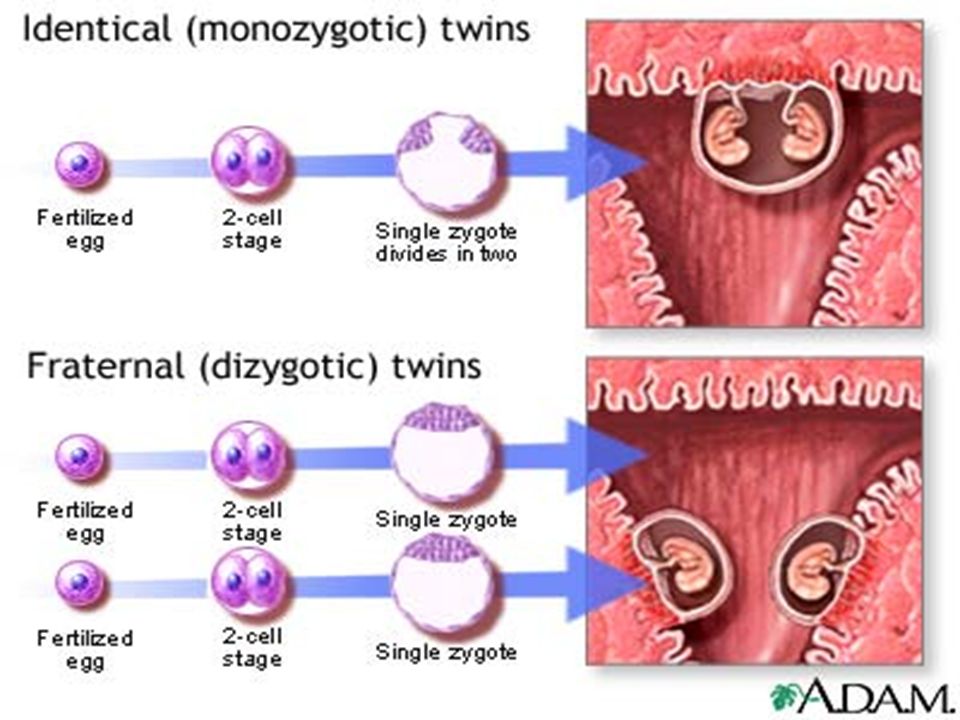
Around one in three sets of twins is identical.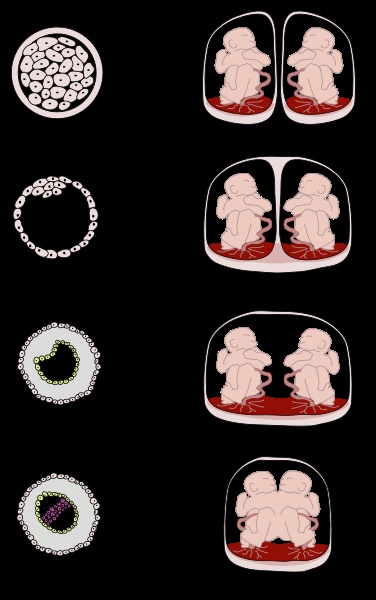 This occurs because the fertilised egg divides in two while it is still a tiny collection of cells. The self-contained halves then develop into two babies, with exactly the same genetic information.
This occurs because the fertilised egg divides in two while it is still a tiny collection of cells. The self-contained halves then develop into two babies, with exactly the same genetic information.
Twins conceived from one egg and one sperm are called identical or ‘monozygotic’ (one-cell) twins. The biological mechanisms that prompt the single fertilised egg to split in two remain a mystery.
Approximately one quarter of identical twins are mirror images of each other, which means the right side of one child matches the left side of their twin.
Fraternal or ‘dizygotic’ twins
Around two in three sets of twins are fraternal. Two separate eggs (ova) are fertilised by two separate sperm, resulting in fraternal or ‘dizygotic’ (two-cell) twins. These babies will be no more alike than siblings born at separate times. The babies can be either the same sex or different sexes, with the odds roughly equal for each.
The proposed ‘third-twin type’
Some researchers believe there may be a third type of twin, although medical opinion is still divided. It is proposed that the egg splits in two, and each half is then fertilised by a different sperm. This theory is an attempt to explain why some fraternal twins look identical.
The normal length of gestation for a single baby is around 40 weeks. However, gestation for twins, either identical or fraternal, is usually around 38 weeks. This shorter time is due to the increased demands on the mother’s body, and the inability of the babies to receive all the nutrients they need in utero.
Since twins are usually premature, they are more likely to have lower birth weights. Prematurity is associated with increased risk of a number of disorders, including jaundice.
Giving birth to twins
Childbirth can give rise to complications when just one baby is present, so twins present extra potential for difficulties. It is advised that women carrying twins give birth in hospital, rather than at home. The babies can be delivered vaginally, but caesarean section delivery may be considered a better alternative in some circumstances.
Zygosity testing
It is difficult to tell if twins are identical or fraternal at birth. Some identical twins may be born with individual sets of membranes, which may lead to the mistaken assumption that the babies are fraternal.
One way to tell the difference is to have the twins DNA-tested. Identical twins share the same genetic information, while fraternal twins share around half. The test can be done with a sample of cheek cells, collected painlessly. Other tests include blood group examinations.
Where to get help
- Your doctor
- Paediatrician
- Maternity hospital
Things to remember
- Twins account for over 90 per cent of multiple births.
- To form identical or monozygotic twins, one fertilised egg (ovum) splits and develops into two babies with exactly the same genetic information.
- To form fraternal or dizygotic twins, two eggs (ova) are fertilised by two sperm and produce two genetically unique children.
Multiple pregnancy
Author: Mikheeva Natalia Grigoryevna, Malyshok magazine
A multiple pregnancy is a pregnancy in which two or more fetuses develop simultaneously in the uterus. Multiple pregnancy occurs in 0.4 - 1.6% of all pregnancies. Recently, there has been an obvious trend towards an increase in the incidence of such pregnancies due to the active use of assisted reproduction technologies, including in vitro fertilization (IVF).
Types of multiple pregnancies
Children born in multiple pregnancies are called TWINS. There are two main types of twins: monozygotic (identical, homologous, identical, similar) and dizygotic (fraternal, heterologous, different). African countries have the highest twin birth rate, Europe and the USA have an average rate, and Asian countries have a low rate.
Dizygotic (fraternal) twins are more common (in 66-75% of all twins). The birth rate of dizygotic twins varies from 4 to 50 per 1000 births. Dizygotic twins occur when two separate eggs are fertilized. The maturation of two or more eggs can occur both in one ovary and in two. The predisposition to develop dizygotic twins may be maternally inherited. Dizygotic twins can be either same-sex or opposite-sex, they look like each other like ordinary brothers and sisters. With fraternal twins, two placentas are always formed, which can be very close, even touching, but they can always be separated. Two fruit spaces (i.e., fetal bladders or two “houses”) are separated from each other by a septum consisting of two chorionic and two amniotic membranes. Such twins are called dizygotic dichorionic diamniotic twins.
Dizygotic twins occur when two separate eggs are fertilized. The maturation of two or more eggs can occur both in one ovary and in two. The predisposition to develop dizygotic twins may be maternally inherited. Dizygotic twins can be either same-sex or opposite-sex, they look like each other like ordinary brothers and sisters. With fraternal twins, two placentas are always formed, which can be very close, even touching, but they can always be separated. Two fruit spaces (i.e., fetal bladders or two “houses”) are separated from each other by a septum consisting of two chorionic and two amniotic membranes. Such twins are called dizygotic dichorionic diamniotic twins.
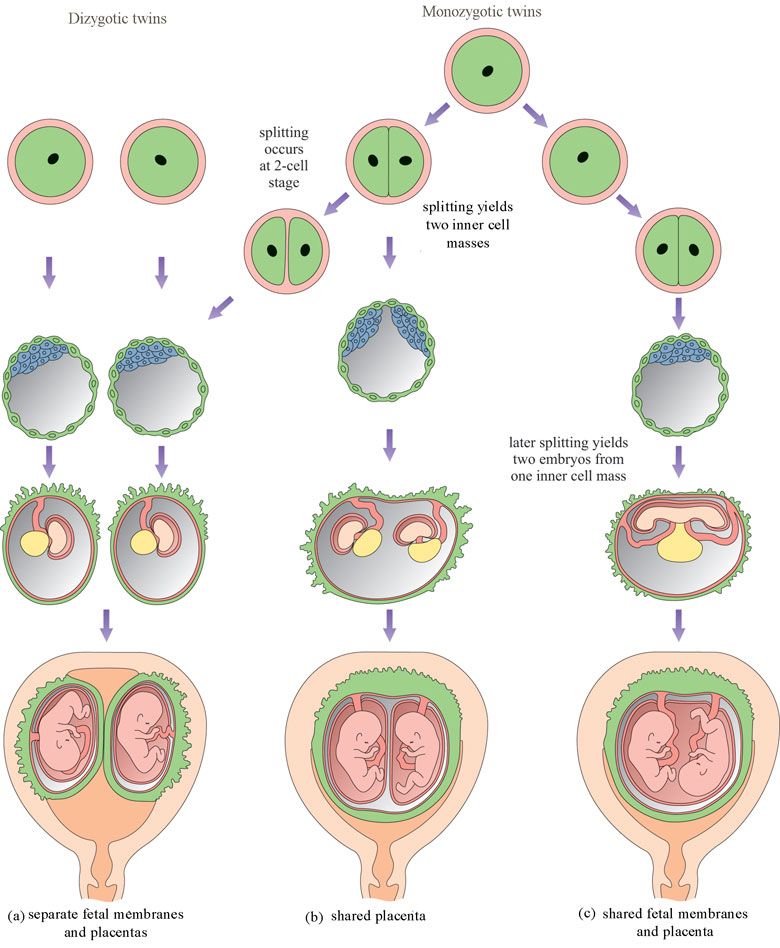
Monozygotic (identical) twins are formed as a result of the separation of one fetal egg at various stages of its development. The frequency of birth of monozygotic twins is 3-5 per 1000 births. The division of a fertilized egg into two equal parts can occur as a result of a delay in implantation (immersion of the embryo in the uterine mucosa) and oxygen deficiency, as well as due to a violation of the acidity and ionic composition of the medium, exposure to toxic and other factors. The emergence of monozygotic twins is also associated with the fertilization of an egg that had two or more nuclei. If the separation of the fetal egg occurs in the first 3 days after fertilization, then monozygotic twins have two placentas and two amniotic cavities, and are called monozygotic diamniotic dichoriones (Fig. A). If the division of the ovum occurs between 4 - 8 days after fertilization, then two embryos will form, each in a separate amniotic sac. Two amniotic sacs will be surrounded by a common chorionic membrane with one placenta for two. Such twins are called monozygotic diamniotic monochorionic twins (Fig. B). If division occurs by 9- 10th day after fertilization, then two embryos are formed with a common amniotic sac and placenta. Such twins are called monozygotic monoamniotic monochorionic (Fig. B) If the egg is separated at a later date on the 13th - 15th day after conception, the separation will be incomplete, which will lead to the appearance of conjoined (undivided, Siamese) twins.
The emergence of monozygotic twins is also associated with the fertilization of an egg that had two or more nuclei. If the separation of the fetal egg occurs in the first 3 days after fertilization, then monozygotic twins have two placentas and two amniotic cavities, and are called monozygotic diamniotic dichoriones (Fig. A). If the division of the ovum occurs between 4 - 8 days after fertilization, then two embryos will form, each in a separate amniotic sac. Two amniotic sacs will be surrounded by a common chorionic membrane with one placenta for two. Such twins are called monozygotic diamniotic monochorionic twins (Fig. B). If division occurs by 9- 10th day after fertilization, then two embryos are formed with a common amniotic sac and placenta. Such twins are called monozygotic monoamniotic monochorionic (Fig. B) If the egg is separated at a later date on the 13th - 15th day after conception, the separation will be incomplete, which will lead to the appearance of conjoined (undivided, Siamese) twins. This type is quite rare, approximately 1 observation in 1500 multiple pregnancies or 1: 50,000 - 100,000 newborns. Monozygotic twins are always the same sex, have the same blood type, have the same eye color, hair, skin texture of the fingers, and are very similar to each other.
This type is quite rare, approximately 1 observation in 1500 multiple pregnancies or 1: 50,000 - 100,000 newborns. Monozygotic twins are always the same sex, have the same blood type, have the same eye color, hair, skin texture of the fingers, and are very similar to each other.
Twin births occur once in 87 births, triplets - once in 87 2 (6400) twins, quadruples - once in 87 3 (51200) triplets, etc. (according to the Gallin formula). The origin of triplets, quadruplets, and more twins varies. So, triplets can be formed from three separate eggs, from two or one egg. They can be monozygotic and heterozygous. Quadruples can also be identical and fraternal.
Features of the course of multiple pregnancy
In case of multiple pregnancies, the woman's body is subject to increased requirements. All organs and systems function with great tension. In connection with the displacement of the diaphragm by the enlarged uterus, the activity of the heart becomes difficult, shortness of breath, fatigue occur.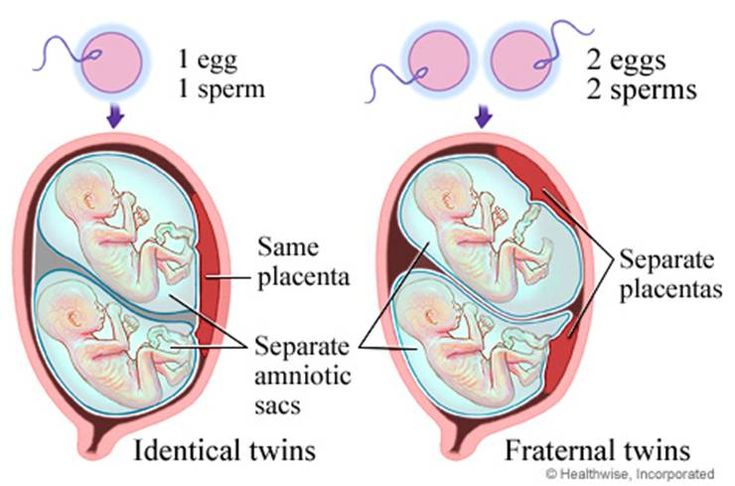 Enlargement of the uterus, especially towards the end of pregnancy, leads to compression of the internal organs, which is manifested by impaired bowel function, frequent urination, and heartburn. Almost 4-5 times more often there is the development of preeclampsia, which is characterized by an earlier onset, a protracted and more severe clinical course, often combined with acute pyelonephritis of pregnant women. Due to the increased need and consumption of iron, iron deficiency anemia often develops in pregnant women. Significantly more often than with a singleton pregnancy, complications such as bleeding during pregnancy and childbirth, anomalies in labor, and a low location of the placenta are observed. Often, with multiple pregnancies, abnormal positions of the fetus occur. One of the most common complications in multiple pregnancy is its premature termination. Preterm birth is observed in 25-50% of cases of such pregnancies.
Enlargement of the uterus, especially towards the end of pregnancy, leads to compression of the internal organs, which is manifested by impaired bowel function, frequent urination, and heartburn. Almost 4-5 times more often there is the development of preeclampsia, which is characterized by an earlier onset, a protracted and more severe clinical course, often combined with acute pyelonephritis of pregnant women. Due to the increased need and consumption of iron, iron deficiency anemia often develops in pregnant women. Significantly more often than with a singleton pregnancy, complications such as bleeding during pregnancy and childbirth, anomalies in labor, and a low location of the placenta are observed. Often, with multiple pregnancies, abnormal positions of the fetus occur. One of the most common complications in multiple pregnancy is its premature termination. Preterm birth is observed in 25-50% of cases of such pregnancies.
The development of term twins is normal in most cases.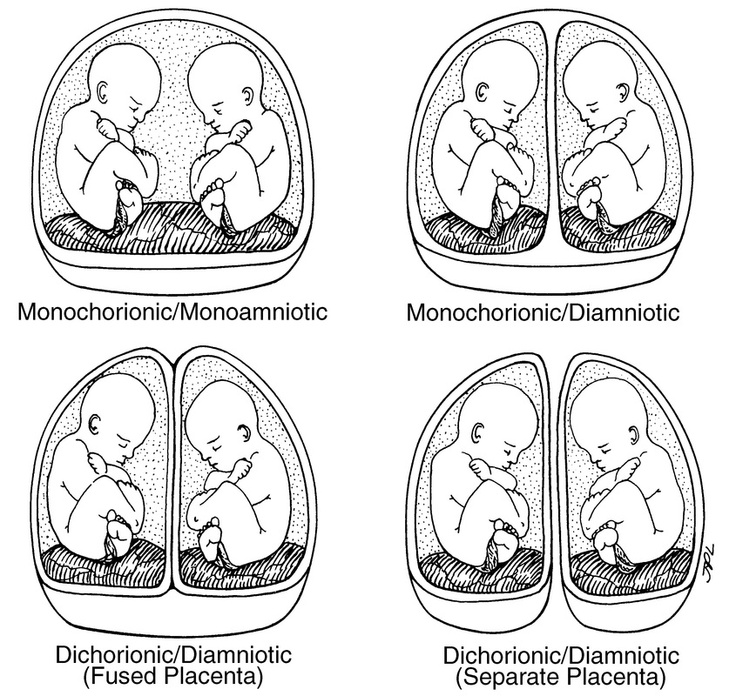 However, their body weight is usually less (by 10% or more) than in singleton pregnancies. With twins, the weight of children at birth less than 2500 g is observed in 40-60%. The low weight of twins is most often due to insufficiency of the uteroplacental system, which is not able to adequately provide several fetuses with nutrients, trace elements and oxygen. The consequence of this is a delay in the development of the fetus, which is a common occurrence in multiple pregnancies. The mass of twins, respectively, decreases in proportion to their number (triplets, quadruplets, etc.).
However, their body weight is usually less (by 10% or more) than in singleton pregnancies. With twins, the weight of children at birth less than 2500 g is observed in 40-60%. The low weight of twins is most often due to insufficiency of the uteroplacental system, which is not able to adequately provide several fetuses with nutrients, trace elements and oxygen. The consequence of this is a delay in the development of the fetus, which is a common occurrence in multiple pregnancies. The mass of twins, respectively, decreases in proportion to their number (triplets, quadruplets, etc.).
With monochorionic twins in the placenta, anastomoses are often formed between the vascular systems of the fetus, which can lead to a serious complication - the syndrome of feto-fetal transfusion. In this case, there is a redistribution of blood from one fetus to another, the so-called "stealing". The severity of feto-fetal transfusion (mild, moderate, severe) depends on the degree of redistribution of blood through the anastomoses, which vary in size, number and direction.
Diagnosis in multiple pregnancy
The most reliable method for diagnosing multiple pregnancies is ultrasound, which allows not only early diagnosis of multiple pregnancies, but also to determine the position and presentation of fetuses, localization, structure and number of placentas, the number of amniotic cavities, the volume of amniotic fluid, congenital malformations and antenatal fetal death, the state of the fetus from a functional point of view, the nature of the uteroplacental and fetal-placental blood flow.
In multiple pregnancies, due to the higher risk of complications, ultrasound monitoring is performed more frequently than in singleton pregnancies. With dizygotic twins, about once every 3-4 weeks, with monozygotic twins - once every 2 weeks.
In addition, examinations and control of clinical tests are carried out with great care, and CTG is regularly recorded from 28 weeks of pregnancy.
Birth management
Indications for caesarean section associated with multiple pregnancies are triplets (quadruple), the transverse position of both or one of the fetuses, breech presentation of both fetuses or the first of them, and not associated with multiple pregnancy - fetal hypoxia, anomalies labor activity, prolapse of the umbilical cord, extragenital pathology of the mother, severe gestosis, placenta previa and abruption, etc.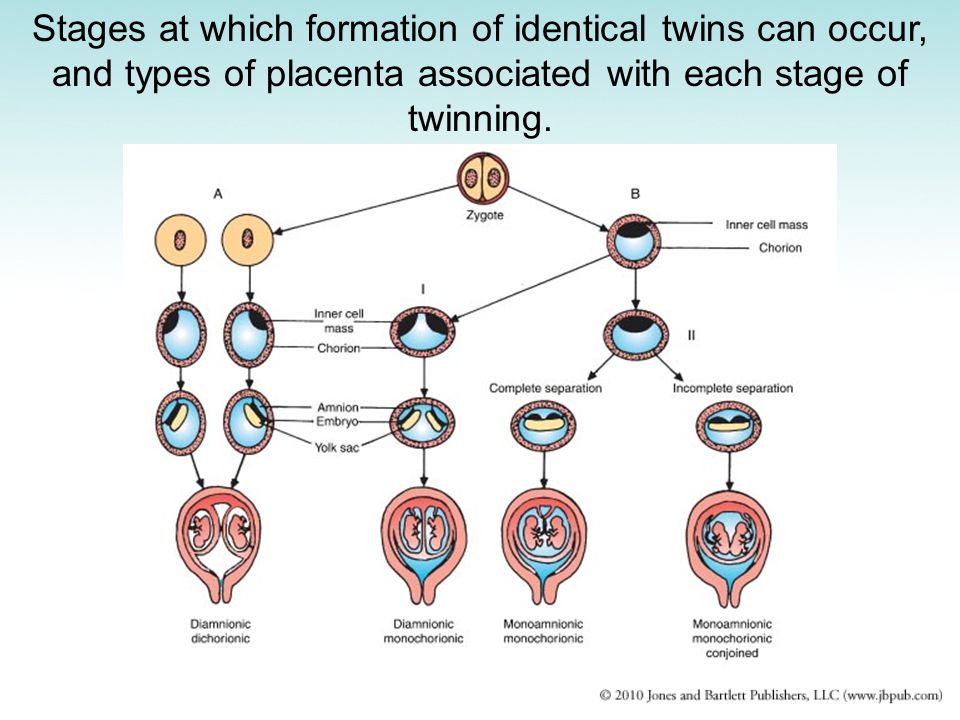
-
ECO
In the department of assisted reproductive technologies of the Maternity Hospital No. 2
, IVF is performed at the expense of the Republican budget for couples
who have received a positive decision from the Minsk city or regional commissions to provide one free IVF attempt.
No drug supply problem. There is no waiting list. -
Farewoman
-
Individual care for patients
-
Ultrasound diagnostics
- Pregnant women often complain of fatigue and shortness of breath, which increases towards the end of pregnancy. The cause of shortness of breath is a difficulty in the activity of the heart due to a significant displacement of the diaphragm by the bottom of the uterus, the size of which is larger in multiple pregnancy than in singleton.
- Often there is a dilation of the veins of the lower extremities. By the end of pregnancy, there is often an increase in the urge to urinate due to the pressure of a large fetus on the bladder.
- Pregnant women often complain of heartburn and constipation.
- In multiple pregnancies, toxicosis occurs more often than in singleton pregnancies: vomiting, salivation, edema, nephropathy, eclampsia.
- With twins, polyhydramnios of one of the fetuses is often found, which leads to a sharp increase and overstretching of the uterus, shortness of breath, tachycardia and other disorders. Polyhydramnios is more common in one of the identical twins. In some cases, the polyhydramnios of one twin is accompanied by an oligohydramnios of the other fetus.
- Premature termination of multiple pregnancies often occurs.
- With twins, preterm birth is observed in at least 25% of women.
- Triplets are more likely to miscarry than twins. The greater the number of gestated fetuses, the more often preterm births are observed.
- Development of term twins is normal in most cases. However, their body weight is usually less than that of single fetuses.
 Often there is a difference in body weight of twins by 200-300 g, and sometimes more.
Often there is a difference in body weight of twins by 200-300 g, and sometimes more. - Uneven development of twins is associated with unequal intake of nutrients from a single placental circulation.
- Often there is a difference not only in weight, but also in the length of the body of the twins. In connection with this, the theory of supergenesis (superfoetatio) was put forward. Proponents of this hypothesis believe that fertilization of eggs of different ovulation periods is possible, i.e., the onset of a new pregnancy in the presence of an already existing, previously occurring, pregnancy.
- Due to the uneven delivery of nutrients and oxygen, a significant developmental disorder and even death of one of the twins can occur. This is more commonly seen in identical twins. The dead fetus is squeezed by the second, well-growing fetus, the amniotic fluid is absorbed, the placenta undergoes regression. The compressed mummified fetus ("paper fetus") is released from the uterus along with the placenta after the birth of a live twin.
 Polyhydramnios of one fetus, which occurs during multiple pregnancies, often also prevents the other twin from developing correctly. With pronounced polyhydramnios, certain anomalies in the development of the fetus, which grows with an excess of amniotic fluid, are often observed. Rarely, fused twins are born (fusion can be in the head, chest, abdomen, pelvis) and twins with other malformations.
Polyhydramnios of one fetus, which occurs during multiple pregnancies, often also prevents the other twin from developing correctly. With pronounced polyhydramnios, certain anomalies in the development of the fetus, which grows with an excess of amniotic fluid, are often observed. Rarely, fused twins are born (fusion can be in the head, chest, abdomen, pelvis) and twins with other malformations. - The position of the fetuses in the uterine cavity in most cases (about 90%) is normal. In the longitudinal position, different presentation options are observed: both fetuses are presented with the head, both with the pelvic end, one with the head, and the other with the pelvic end. With longitudinal presentation, one fetus may be behind the other, which makes diagnosis difficult. Less commonly observed is the longitudinal position of one fetus and the transverse position of the other. The most rare is the transverse position of both twins.
- The position of the twins in the uterus, both fetuses are presented with the head, one fetus is presented with the head, the second - with the pelvic end, both fetuses are in the transverse position
- In case of multiple pregnancies, women are taken into special account and carefully monitored.
 When the earliest signs of complications appear, the pregnant woman is sent to the pregnancy pathology department of the maternity hospital. Given the frequent occurrence of preterm birth, it is recommended that a pregnant woman with twins be sent to the maternity hospital 2 to 3 weeks before delivery, even in the absence of complications.
When the earliest signs of complications appear, the pregnant woman is sent to the pregnancy pathology department of the maternity hospital. Given the frequent occurrence of preterm birth, it is recommended that a pregnant woman with twins be sent to the maternity hospital 2 to 3 weeks before delivery, even in the absence of complications. - The enlargement of the uterus in multiple pregnancies occurs faster than in pregnancy with one fetus, so the size of the uterus does not correspond to the gestational age.
 The bottom of the uterus is usually high, especially at the end of pregnancy, the circumference of the abdomen during this period reaches 100-110 cm or more.
The bottom of the uterus is usually high, especially at the end of pregnancy, the circumference of the abdomen during this period reaches 100-110 cm or more. - The following signs are unstable and not sufficiently reliable: a) deepening of the uterine fundus (saddle uterus), the formation of which is associated with protrusion of the corners of the uterus with large parts of the fetus; b) the presence of a longitudinal depression on the anterior wall of the uterus, which is formed as a result of the fruits that are in a longitudinal position adjacent to each other; c) the presence of a horizontal groove on the anterior wall of the uterus with the transverse position of the fetus.
- The small size of the presenting head with a significant volume of the pregnant uterus and the high standing of its bottom also make it possible to suspect a multiple pregnancy. The presence of this sign is explained by the fact that the study determines the head of one and the pelvic end (in the bottom of the uterus) of another fetus, which lies slightly higher.

- Feeling the movement of the fetus in different places and probing parts of the fetus in different parts of the abdomen (both on the right and on the left) also indicate multiple pregnancies.
Curious facts are
0
, how many are the Geminis? up to 80 million pairs of twins.
The number of twins born in relation to the total number of newborns in different countries and on different continents is different, but in general the trend is such that it continues to grow. Compared with the 60s, the percentage of twins has increased from 1.18 to 2. 78, that is, almost 2.5 times.
78, that is, almost 2.5 times.
The largest number of children
The largest number of children born to one mother, according to official data, is 69. According to reports made in 1782, between 1725 and 1765. The wife of a Russian peasant Fyodor Vasiliev gave birth 27 times, giving birth to twins 16 times, triplets 7 times and 4 twins 4 times. Of these, only 2 children died in infancy.
The most prolific mother of our contemporaries is considered to be Leontina Albina (or Alvina) of San Antonio, Chile, who at 1943-81 years gave birth to 55 children. As a result of the first 5 pregnancies, she gave birth to triplets, and exclusively male.
Most birthed
The record 38 births are said to be Elizabeth Greenhillies Abbots-Langley, c. Hertfordshire, UK. She had 39 children - 32 daughters and 7 sons.
The largest number of multiple births in one family
Maddalena Pomegranate from Italy (b. 1839) had triplets born 15 times.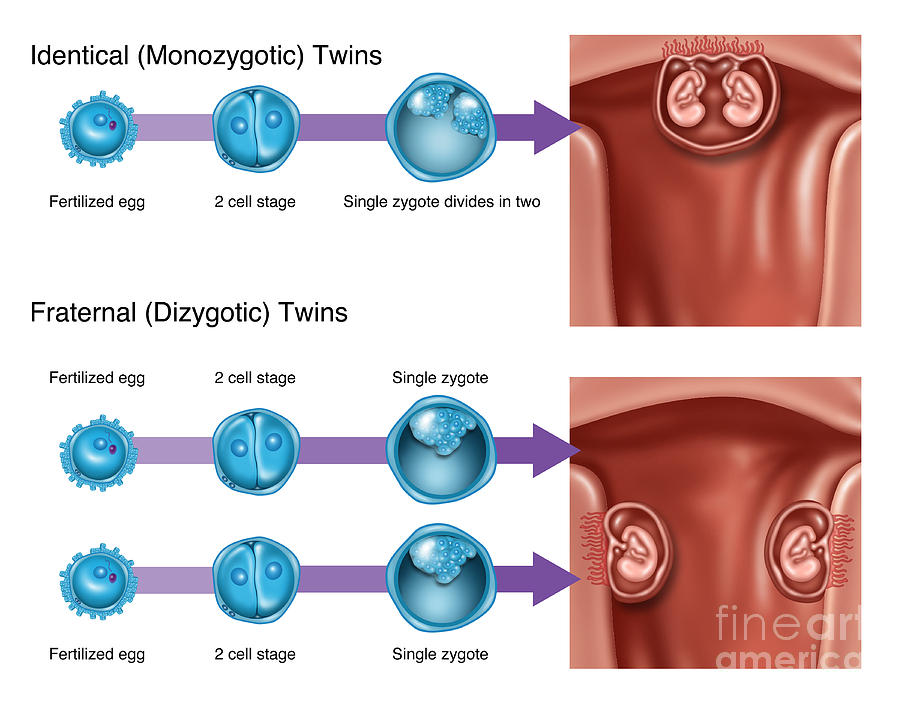
There is also information about the birth on May 29, 1971 in Philadelphia, Pennsylvania, USA, and in May 1977 in Bagarhat, Bangladesh, 11 twins. In both cases, no child survived.
Most fertile pregnancies
Dr. Gennaro Montanino, Rome, Italy, claimed to have removed, in July 1971, the embryos of 10 girls and 5 boys from the uterus of a 35-year-old woman who was 4 months pregnant. This unique case of 15-fertility was the result of infertility pills.
9 children - the largest number in one pregnancy - were born on June 13, 1971 by Geraldine Broadrick in Sydney, Australia. 5 boys and 4 girls were born: 2 boys were stillborn, and none of the rest survived more than 6 days.
The birth of 10 twins (2 boys and 8 girls) is known from reports from Spain (1924), China (1936) and Brazil (April 1946).
The father with many children
The largest father in the history of Russia is Yakov Kirillov, a peasant from the village of Vvedensky, who in 1755 was presented to the court in connection with this (he was then 60 years old). The first wife of a peasant gave birth to 57 children: 4 times four, 7 times three, 9once twice and 2 times once. The second wife gave birth to 15 children. Thus, Yakov Kirillov had 72 children from two wives.
The first wife of a peasant gave birth to 57 children: 4 times four, 7 times three, 9once twice and 2 times once. The second wife gave birth to 15 children. Thus, Yakov Kirillov had 72 children from two wives.
Longest Birth Intervals for Multiple Pregnancies
Peggy Lynn of Huntington Pennsylvania, USA, gave birth to a girl, Hanna, on November 11, 1995, and the second of the twins, Erika, only 84 days later (February 2, 1996).
Siamese twins
United twins became known as "Siamese" after Chang and Eng Bunkers were born fused in the area of the sternum on May 11, 1811 in the Maeklong region of Siam (Thailand). They married Sarah and Adelaide Yates of pc. North Carolina, USA, and had 10 and 12 children, respectively. They died in 1874, and with a difference of 3 hours.
The science of twins - gemellology.
"Secret language"
Twins often talk to each other in a language that others do not understand.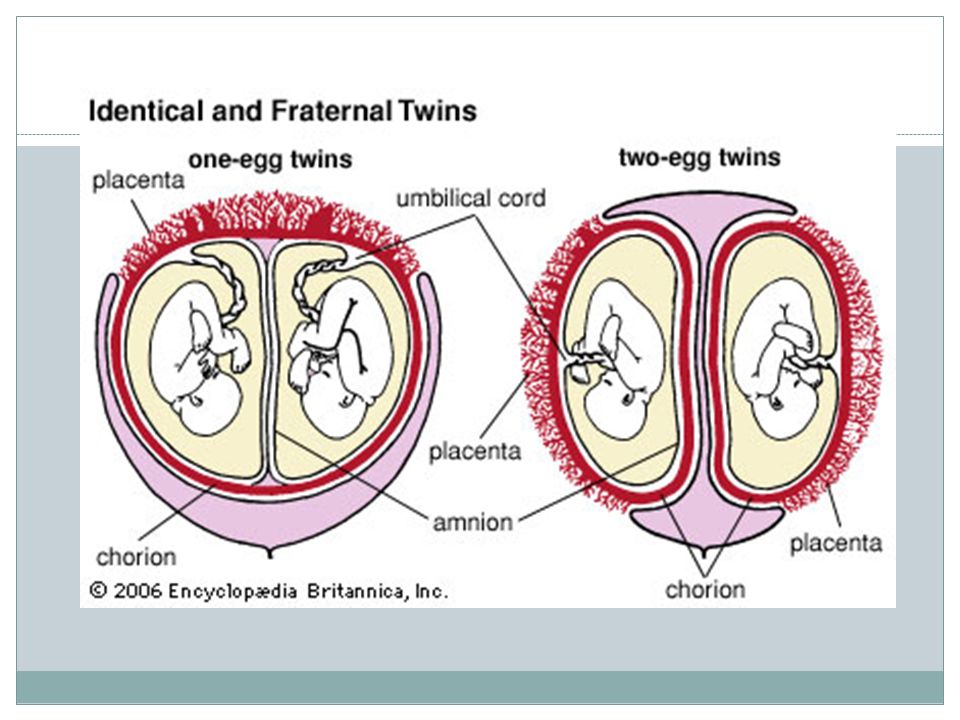 This phenomenon is called cryptophasia.
This phenomenon is called cryptophasia.
Left-handed twins
18-22% of left-handed twins (for non-twins this percentage is 10).
articles from specialists of the clinic "Mother and Child"
Arifullina Claudia Viktorovna
Gastroenterologist
Clinical Hospital "AVICENNA" GC "Mother and Child"
There is data on the frequency of twins in case of anomalies in the development of the uterus, characterized by its bifurcation (bicornuate uterus, having a septum in the cavity, etc.). The cause of polyembryony may be the separation of blastomeres (in the early stages of crushing), resulting from hypoxia, cooling, acidity and ionic composition of the medium, exposure to toxic and other factors. Multiple pregnancy can occur: as a result of the fertilization of two or more simultaneously mature eggs, as well as the development of two or more embryos from one fertilized egg.
Twins formed from two (three, etc. ) eggs are called dizygotic (polyzygotic), those arising from one are called identical. The origin of fraternal twins (polyzygotic twins): the simultaneous maturation (and ovulation) of two or more follicles in one ovary is possible. There may be maturation of two or more follicles and ovulation in both ovaries.
) eggs are called dizygotic (polyzygotic), those arising from one are called identical. The origin of fraternal twins (polyzygotic twins): the simultaneous maturation (and ovulation) of two or more follicles in one ovary is possible. There may be maturation of two or more follicles and ovulation in both ovaries.
A third way of the origin of fraternal (multi-ovular) twins is possible - the fertilization of two or more eggs that have matured in one follicle. The origin of identical twins: most often, the occurrence of identical twins is associated with the fertilization of an egg that has two or more nuclei. a single embryonic germ in the stage of crushing is divided into two parts; from each part an embryo (fruit) is formed. Twin twin. Fertilized eggs develop on their own. After penetration into the mucous membrane, each embryo develops its own aqueous and fleecy membranes; in the future, each twin forms its own placenta with an independent network of vessels, each fetal egg, except for the chorion and amnion, has an independent capsular membrane (decidua capsularis). In some cases, anastomoses are formed between the vessels of independent placentas. Twins can be same-sex (both boys or both girls) or different-sex (boy and girl). Their blood type can be the same or different. Identical twin. Identical twins have a common capsular and fleecy membrane and a common placenta; the vessels (both arterial and venous) of both twins in the placenta communicate with the help of numerous anastomoses. The water membrane of each twin is separate, the septum between the fetal sacs consists of two water membranes (biamniotic twins).
In some cases, anastomoses are formed between the vessels of independent placentas. Twins can be same-sex (both boys or both girls) or different-sex (boy and girl). Their blood type can be the same or different. Identical twin. Identical twins have a common capsular and fleecy membrane and a common placenta; the vessels (both arterial and venous) of both twins in the placenta communicate with the help of numerous anastomoses. The water membrane of each twin is separate, the septum between the fetal sacs consists of two water membranes (biamniotic twins).
Identical twins always belong to the same sex (both boys or both girls), look alike, have the same blood type.
In fraternal twins, the membranes in the septum are arranged as follows: amnion - chorion, chorion - amnion; with monozygotic amnion-amnion.
Important signs for the diagnosis are: blood type (and other blood factors), eye color, hair color, skin texture of the fingertips, shape and location of teeth. In identical twins, these signs are completely the same. Fraternal twins share the same similarities as normal siblings.
In identical twins, these signs are completely the same. Fraternal twins share the same similarities as normal siblings.
MULTIPLE PREGNANCY
With multiple pregnancy, increased demands are made on the woman's body: the cardiovascular system, lungs, liver, nights and other organs function with great stress. In this regard, multiple pregnancies are more difficult than single pregnancies.
RECOGNITION OF MULTIPLE PREGNANCY
Diagnosis of multiple pregnancy often presents significant difficulties, especially in its first half. In the second half, towards the end of pregnancy, the recognition of twins (triplets) is facilitated. However, diagnostic errors occur during the study at the end of pregnancy and even during childbirth.
When recognizing a multiple pregnancy, the following signs are taken into account:
Make an appointment
to the doctor - Arifullina Claudia Viktorovna
Clinical Hospital "AVICENNA" GC "Mother and Child"
GastroenterologyPediatric Gastroenterology
By clicking on the submit button, I consent to the processing of personal data
Attention! Prices for services in different clinics may vary. To clarify the current cost, select a clinic
Clinical Hospital "AVICENNA" Group of Companies "Mother and Child"Novosibirsk Center for Reproductive Medicine
All directionsGynecological proceduresSpecialist consultations (adults)Specialist consultations (children)Laboratory of molecular geneticsGeneral clinical studiesProcedure roomTherapeutic studiesUltrasound examinations for adults
.