Engorged breasts when milk comes in
What is breast engorgement? | Engorged breasts
Some new mums experience breast engorgement when their milk starts ‘coming in’ a few days after the birth. It’s usually temporary and easily treated – read on to find out how
Share this content
Sioned Hilton, health visitor, neonatal nurse and lactation consultant:
Mum-of-three Sioned has been supporting families with babies and young children for more than 30 years. As well working with breastfeeding and expressing mothers, both in hospitals and the community, she contributes to parenting magazines and conferences, and delivers workshops for healthcare professionals.
When you first start breastfeeding your baby, your breasts produce colostrum in small amounts that gradually increase over the first few days. But after around two to four days they start making much larger quantities of milk – a change known as your breast milk ‘coming in’. 1
One of the signs milk is coming in is your breasts become fuller and firmer. This swelling is not just caused by the greater quantity of milk, but also by increased blood flow and extra lymph fluids in your breast tissue.2
For most new mums, if their baby is feeding well and frequently, these feelings of heaviness pass without problems. But some produce almost more milk than their breasts can hold, which makes them feel rock hard and uncomfortably full – a condition called engorgement. While this is usually only temporary, the 24 to 48 hours it typically lasts for can be painful.
What do engorged breasts feel like?
Engorgement can happen in one or both breasts. It may cause throbbing and swelling, sometimes extending as far as your armpit, and could make your breasts feel fairly hot or lumpy – this is because of all the activity going on inside. You may notice other breast engorgement symptoms, including the skin of your breasts looking shiny and feeling stretched, and your nipples becoming hard and flat. Engorgement may even cause your body temperature to rise to around 37.5 to 38.3 °C (99 to 101 °F).3
Engorgement may even cause your body temperature to rise to around 37.5 to 38.3 °C (99 to 101 °F).3
As well as being painful, breast engorgement can cause breastfeeding difficulties – which can, in turn, worsen the problem. Your baby might struggle to latch if your nipples are flatter and your breast tissue is harder, which can cause sore nipples. In addition, if your baby’s latch is poor she’s less likely to drain the breast well. This means that, if left untreated, engorgement can lead to blocked ducts, mastitis and reduced milk production.
What causes breast engorgement?
Engorgement usually occurs because a baby is not feeding frequently enough (at least eight times every 24 hours). It can happen to any new mum, but is more common in women who’ve had previous breast augmentation or other breast surgery.2 Pressure from a badly fitting bra or tight clothing can make the discomfort worse, and may lead to blocked ducts and possibly mastitis.
Breast engorgement can happen to women who don’t or can’t breastfeed, as well as those who do. The hormonal changes that follow delivery of the baby and placenta, which cause an increase in milk production, occur whether you breastfeed or not. Engorgement can also happen if you suddenly cut breastfeeds, perhaps because your baby is sick, sleeping longer, starting solids, or going into childcare.
The hormonal changes that follow delivery of the baby and placenta, which cause an increase in milk production, occur whether you breastfeed or not. Engorgement can also happen if you suddenly cut breastfeeds, perhaps because your baby is sick, sleeping longer, starting solids, or going into childcare.
How can I treat engorged breasts?
2The most effective breast engorgement treatment is a hungry baby! You should try to empty your breasts as much and as often as possible to help keep milk flowing – so feed on demand, between eight and 12 times every 24 hours.
Keep your baby in skin-to-skin contact with your chest for as long as possible throughout the day, and when you’re awake at night. This way she can smell the tempting aroma of your milk, has easy access to your breasts, and you’re more likely to spot her early hunger cues so you can ensure she feeds frequently. Let her take as much milk as she wants from one breast before offering the other.
It’s also well worth getting your baby’s latch and positioning checked by a lactation consultant or breastfeeding specialist, to make sure she’s feeding effectively and draining your breasts properly. The tips below may also help relieve symptoms.
The tips below may also help relieve symptoms.
Tips for engorgement relief2
- Ensure you’re breastfeeding a minimum of eight times every 24 hours.
- Check that your baby has a good breastfeeding latch.
- Try breastfeeding in different positions.
- Massage your breasts gently while feeding to help the milk drain effectively.
- Express a little milk, either by hand or with a breast pump before breastfeeding to help soften your nipple so it’s easier to latch on to.
- If your breasts are still very firm and full after a feed, express again until you feel comfortable.
- If your baby is unable to breastfeed, replace the feeds with expressions. Pump your breasts until they feel much softer – a minimum of eight times every 24 hours.
- Try ‘reverse pressure softening’, a technique that can move excess fluid from the breast. A lactation consultant or breastfeeding specialist can show you how to do this.

- If your breasts are leaking milk, try a warm shower or applying a warm, wet flannel just before breastfeeding or expressing to soothe them and help milk flow. Don’t do this for more than a couple of minutes, as too much heat may worsen swelling.
- If your breasts aren’t leaking, apply a cold compress, chilled gel pad, or even frozen peas wrapped in a cloth, to your breasts for ten minutes after a feed to reduce swelling and relieve pain.
- Tuck clean cabbage leaves inside your bra. Yes, really! Many mums find they help reduce swelling and discomfort, and there’s scientific evidence to back this up.4
- Take anti-inflammatory painkillers. Paracetamol and ibuprofen can be used while breastfeeding, although ibuprofen has contraindications for asthmatic mums. Always consult a healthcare professional and follow the manufacturer’s and pharmacist’s guidance. It’s generally best to avoid aspirin – for more on which medicines you can take while breastfeeding, read Breastfeeding while sick.

- Wear a properly fitted nursing bra and avoid underwires, or you may prefer not to wear a bra.
- Don’t skip feeds or stop breastfeeding suddenly as you could make the engorgement worse.
Seek medical advice if you develop a fever5 of around 38 °C (101°F) or above, or if your baby is unable to breastfeed because of the engorgement.
Finally, try to be patient. Your body is still getting used to making milk and feeding your baby. The engorgement should soon subside as you both get used to breastfeeding.
References
1 Pang WW, Hartmann PE. Initiation of human lactation: secretory differentiation and secretory activation. J Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
2 Berens P, Brodribb W. ABM Clinical Protocol# 20: Engorgement, Revised 2016. Breastfeed Med. 2016;11(4):159-163.
3 Affronti M et al. Low-grade fever: how to distinguish organic from non-organic forms. Int J Clin Pract. 2010;64(3):316-321.
4 Boi B et al. The effectiveness of cabbage leaf application (treatment) on pain and hardness in breast engorgement and its effect on the duration of breastfeeding. JBI Libr Syst Rev. 2012;10(20):1185-1213.
The effectiveness of cabbage leaf application (treatment) on pain and hardness in breast engorgement and its effect on the duration of breastfeeding. JBI Libr Syst Rev. 2012;10(20):1185-1213.
5 NHS Choices. How do I take someone’s temperature? [Internet]. UK: NHS Choices; updated 2016 June 29. Available from: www.nhs.uk/chq/pages/1065.aspx?categoryid=72
Breast engorgement | Pregnancy Birth and Baby
Breast engorgement | Pregnancy Birth and Baby beginning of content3-minute read
Listen
What is breast engorgement?
Once your baby is born, your breasts are given a signal to start full milk production. Blood flows to your breasts, and your milk usually comes in 1 to 4 days after the birth. Breast engorgement is when the breast tissue overfills with milk, blood and other fluids and is a common problem in the early days and weeks of breastfeeding.
What are the symptoms of breast engorgement?
Engorgement can make your breasts feel very full, hard, swollen and painful.
Your nipples can become flat and tight. This can make it difficult for your baby to attach to the breast.
What causes breast engorgement?
Breast engorgement can happen if:
- your baby is not feeding and attaching well and your breasts aren’t drained well during a feed
- you are making more milk than your baby needs
- your baby misses a feed or is feeding infrequently
Breast engorgement can occur at any time you are breastfeeding, especially when your baby’s feeding pattern changes and they feed less.
Engorgement is usually temporary — eventually you will produce just as much milk as your baby needs.
How to prevent breast engorgement
To reduce the chance of breast engorgement:
- Feed your baby often and on demand (not by the clock) from birth, with at least 8 to 12 feeds in the first 24 hours.
 It helps to sleep in the same room as your baby to keep up the feeds.
It helps to sleep in the same room as your baby to keep up the feeds. - Wake your baby for a feed if your breasts become full and uncomfortable (especially at night time).
- Don’t limit your baby’s time at the breast.
- Avoid giving your baby any fluids other than breastmilk unless needed for a specific medical reason.
- Ensure your baby is positioned and attached correctly, to maximise the amount of milk they are getting.
How to relieve breast engorgement
If your breasts become engorged, there are things you can do to relieve the discomfort.
The best way to is to empty the breast, either by feeding your baby at the breast, or by expressing your milk. It’s okay to wake your baby and offer a breastfeed day or night if your breasts become full and uncomfortable between feeds.
The following tips might also help:
- Apply a warm washer to the breast, or have a warm shower before a feed, for comfort and to help the milk flow.

- Remove your bra before breastfeeding (and leave it off).
- Hand-express a little milk before feeding your baby, or try ‘reverse pressure softening’ (applying pressure around the nipples to push fluid back into the breasts).
- Gently massage the breast in a downward motion from the chest wall toward the nipple while your baby is feeding.
- Use a cold compress, like a cool gel pack from the fridge, or a chilled washed cabbage leaf over the breast to relieve inflammation.
- Express milk after a feed, either by hand or with a breast pump, if your breasts still feel full.
Sometimes, if the engorgement does not improve, a complete ‘pump out’ with an electric pump may be necessary to relieve the milk pressure that is causing increased blood and fluid within the breast tissue (ask your lactation consultant or doctor for help).
If you are still uncomfortable, ask your doctor for appropriate pain relief.
For help with breast engorgement prevention and treatment, contact a health professional, including your doctor, lactation consultant or breastfeeding counsellor, child health nurse, or call Pregnancy Birth and Baby on 1800 882 436.
Sources:
Raising Children Network (Breast milk oversupply and engorgement), Australian Breastfeeding Association (Engorgement), HealthyWA (Engorgement), myDr (Engorgement and mastitis)Learn more here about the development and quality assurance of healthdirect content.
Last reviewed: December 2020
Back To Top
Related pages
- Expressing and storing breast milk
- Breastfeeding your baby
Need more information?
Engorgement and mastitis - MyDr.com.au
If you experience difficulties with breastfeeding seek the advice of a midwife, lactation consultant, the Australian Breastfeeding Association or your doctor.
Read more on myDr website
Engorgement | Australian Breastfeeding Association
What is engorgement?You may find that your breasts become larger and feel heavy, warmer and uncomfortable when your milk ‘comes in’, usually about 2–6 days after your baby is born. This is normal. It does not affect milk flow or the ability of your baby to attach to your breast.
This is normal. It does not affect milk flow or the ability of your baby to attach to your breast.
Read more on Australian Breastfeeding Association website
Breastmilk oversupply & breast engorgement | Raising Children Network
Breastfeeding mums can have breastmilk oversupply and breast engorgement. Check feeding patterns, techniques and positions. Hand-expressing can also help.
Read more on raisingchildren.net.au website
Breastfeeding
Breastfeeding is learnt over the first weeks and months of your child’s life. It is a unique and special experience for families as no two mothers or babies are the same.
Read more on Karitane website
Blocked ducts | Australian Breastfeeding Association
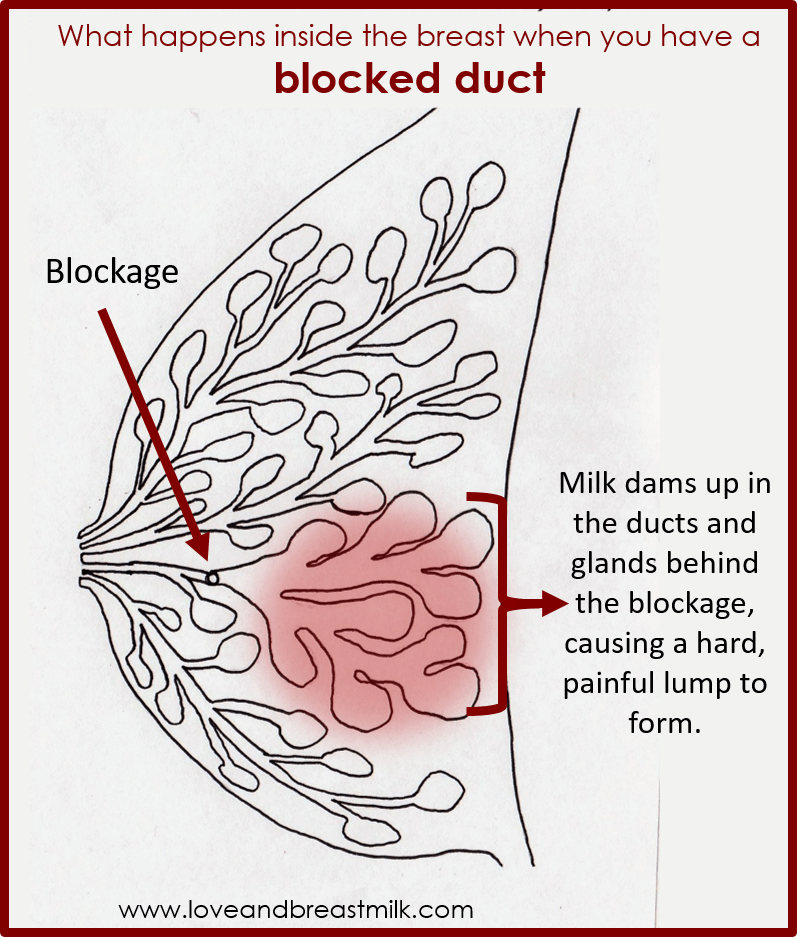
What are blocked ducts?Ducts carry the milk from deep in the breast to the nipple openings. Sometimes these ducts can become blocked. Milk builds up behind the blockage, a lump forms and your breast begins to feel sore. Your breast may become engorged in one area and might also look red.Occasionally, a mother with a blocked duct may notice a white spot on her nipple too.
Sometimes these ducts can become blocked. Milk builds up behind the blockage, a lump forms and your breast begins to feel sore. Your breast may become engorged in one area and might also look red.Occasionally, a mother with a blocked duct may notice a white spot on her nipple too.
Read more on Australian Breastfeeding Association website
Breastfeeding | Sydney Children's Hospitals Network
Breastfeeding is not always easy and you may have trouble breastfeeding your baby
Read more on Sydney Children's Hospitals Network website
Weaning: stopping breastfeeding | Raising Children Network
Whether weaning is led by you or baby, you can make the process of stopping breastfeeding easier if you take it slowly to start with. Get more tips.
Read more on raisingchildren.net.au website
Breastfeeding challenges - Ngala
Many new mothers experience breastfeeding challenges
Read more on Ngala website
Too much milk | Australian Breastfeeding Association
Some mothers make more milk than their babies can easily cope with. This is quite common in the first few weeks of breastfeeding, but for some mothers it can continue for longer.
Read more on Australian Breastfeeding Association website
Breastfeeding your baby
Breastfeeding is the most natural way to feed your baby, providing all the nutrition your baby needs during the first six months of life and a loving bond with your baby.
Read more on Pregnancy, Birth & Baby website
Disclaimer
Pregnancy, Birth and Baby is not responsible for the content and advertising on the external website you are now entering.
OKNeed further advice or guidance from our maternal child health nurses?
1800 882 436
Video call
- Contact us
- About us
- A-Z topics
- Symptom Checker
- Service Finder
- Linking to us
- Information partners
- Terms of use
- Privacy
Pregnancy, Birth and Baby is funded by the Australian Government and operated by Healthdirect Australia.
Pregnancy, Birth and Baby is provided on behalf of the Department of Health
Pregnancy, Birth and Baby’s information and advice are developed and managed within a rigorous clinical governance framework. This website is certified by the Health On The Net (HON) foundation, the standard for trustworthy health information.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
This information is for your general information and use only and is not intended to be used as medical advice and should not be used to diagnose, treat, cure or prevent any medical condition, nor should it be used for therapeutic purposes.
The information is not a substitute for independent professional advice and should not be used as an alternative to professional health care. If you have a particular medical problem, please consult a healthcare professional.
Except as permitted under the Copyright Act 1968, this publication or any part of it may not be reproduced, altered, adapted, stored and/or distributed in any form or by any means without the prior written permission of Healthdirect Australia.
Support this browser is being discontinued for Pregnancy, Birth and Baby
Support for this browser is being discontinued for this site
- Internet Explorer 11 and lower
We currently support Microsoft Edge, Chrome, Firefox and Safari. For more information, please visit the links below:
- Chrome by Google
- Firefox by Mozilla
- Microsoft Edge
- Safari by Apple
You are welcome to continue browsing this site with this browser. Some features, tools or interaction may not work correctly.
What is breast swelling? | Breast swelling
Some mothers experience breast swelling when milk begins to flow in the first days after childbirth. Usually this phenomenon is temporary and easily eliminated. Read our article to find out how to help yourself.
Share this information
Sioned Hilton, health visitor, neonatal nurse and lactation consultant:
Schoned, a mother of three, has been supporting families with newborns and young children for over 30 years. She provides advice on breastfeeding and pumping, both in clinics and at home. In addition, Schoned writes articles for parenting magazines, attends conferences, and conducts seminars for attending physicians.
She provides advice on breastfeeding and pumping, both in clinics and at home. In addition, Schoned writes articles for parenting magazines, attends conferences, and conducts seminars for attending physicians.
When you start breastfeeding, you first produce a small amount of colostrum, which gradually increases over the first few days. After about two to four days, production increases significantly. This phenomenon is called the "arrival" of milk. 1
One of the signs that milk is starting to come in is a change in the breast - it fills up and becomes firmer. This is due not only to an increase in the amount of milk, but also to increased blood flow and additional lymphatic fluid to the breast tissues. 2
If the child eats well and often, then for most mothers this feeling of heaviness disappears over time without any complications. However, some women produce so much milk that their breasts fill up and become painful and very hard. This condition is called breast swelling. And although everything usually passes in a day or two, this period can be quite painful.
And although everything usually passes in a day or two, this period can be quite painful.
How does breast swelling manifest itself?
Swelling may affect one or both breasts. It can cause swelling, sometimes down to the armpits, and a throbbing sensation. The chest becomes quite hot, sometimes lumps are felt in it. All this is due to the fact that a huge number of processes take place inside. You may also notice other symptoms, such as the skin on your breasts becoming shiny and tight, and your nipples becoming hard and flat. Swelling of the mammary glands can even cause a temperature to rise to 37.5–38.3°C (99–101°F). 3
In addition to painful sensations, breast swelling is also dangerous because it can make breastfeeding difficult, and this, in turn, will worsen the situation even more. If the baby finds it difficult to latch on because the nipples are flat and the breast tissue is firmer, nipples may become inflamed. In addition, in the event of a poor grip, he will not be able to completely empty the chest. Thus, if left untreated, swelling of the mammary glands can lead to blockage of the milk ducts, mastitis, and reduced milk production.
Thus, if left untreated, swelling of the mammary glands can lead to blockage of the milk ducts, mastitis, and reduced milk production.
What causes breast swelling?
Usually breast swelling is due to the fact that the child does not feed often enough (less than eight times a day). In principle, this can happen to any mother, but women who have undergone various breast surgeries, including breast augmentation, are more prone to swelling of the mammary glands. 2 Wearing a bra that is the wrong size or that is too tight can increase discomfort and lead to clogged milk ducts and even mastitis.
Breast swelling can occur in both breastfeeding mothers and mothers who are not or cannot breastfeed. The hormonal changes that occur after the birth of a baby and the release of the placenta and increase milk production are independent of whether you are breastfeeding or not. Swelling can also occur if the number of feedings is drastically reduced, for example, if the child becomes ill, sleeps longer, starts eating solid foods, or goes to nursery.
How to treat breast swelling?
2The best cure for swollen breasts is a hungry baby! Try to empty your breasts as much and as often as possible to facilitate the release of milk. To do this, feed your baby on demand, preferably eight to twelve times a day.
Maintain skin-to-skin contact with your baby, cuddling as often as possible during the day and at night when you are awake. This will allow him to smell the attractive smell of your milk and have easy access to the breast, and you will be able to better monitor signs that he is hungry and, accordingly, feed more often. Let the baby eat enough from one breast before offering the second.
It's a good idea to see a lactation consultant or specialist to check if your baby is properly grasped and positioned. It depends on how well he will eat and empty his chest. The tips below will also help you relieve the symptoms of breast swelling.
Tips for relief of breast swelling 2
- Breastfeed at least eight times a day.

- Make sure your baby is latching on well.
- Try other feeding positions.
- Gently massage your breasts during feeding to improve the flow of milk.
- Express some milk by hand or with a breast pump before feeding to soften the nipple and make it easier for your baby to latch on.
- If your breasts are still firm and full after a feed, pump more until you feel better.
- If your baby cannot breastfeed, express milk for him. Pumping must be continued until the breast becomes softer, and do this at least eight times a day.
- Try the areola pressure softening technique. This helps to remove excess fluid from the breast. A lactation consultant or specialist will show you how to do this.
- If milk leaks, try taking warm showers or applying warm flannel to your breasts just before feeding or pumping to soften your breasts and make it easier for your milk to flow. You should not, however, warm the chest for more than two minutes, as this can only increase swelling.

- If your milk isn't leaking, try applying cold compresses, chilled gel pads, or even frozen green peas wrapped in a towel for ten minutes after feeding to reduce swelling and relieve pain.
- Put clean cabbage leaves in your bra. Yes Yes! For many moms, it really helps reduce swelling and discomfort, and there are scientific explanations for this. 4
- Take an anti-inflammatory pain reliever. While breastfeeding, you can take some medications, in consultation with your doctor. Always consult your doctor, follow the drug manufacturer's instructions and the pharmacist's recommendations. To learn more about medications and breastfeeding, read our article on breastfeeding when sick.
- Wear an appropriately sized and comfortable nursing bra, avoid underwire or no bra at all.
- Do not skip feedings or stop breastfeeding abruptly as this may increase breast swelling.
Seek medical advice if your 5 temperature rises above 38 °C or if your baby is unable to suckle due to breast swelling.
And in any case, try to remain calm. Your body is just getting used to producing milk and feeding your baby. Breast swelling should go away on its own soon after you both get comfortable with breastfeeding.
Literature
1 Pang WW, Hartmann PE. Initiation of human lactation: secretory differentiation and secretory activation. J Mammary Gland Biol Neoplasia. 2007;12(4):211-221. - Pang, W.W., Hartmann, P.I., "Lactation initiation in the lactating mother: secretory differentiation and secretory activation." G Mammary Gland Biol Neoplasia. 2007;12(4):211-221.
2 Berens P, Brodribb W. ABM Clinical Protocol# 20: Engorgement, Revised 2016. Breastfeed Med . 2016;11(4):159-163. - Behrens P, Brodrhibb W, "AVM Clinical Protocol #20: Engorgement, 2016 edition". Brestfeed Med (Breastfeeding Medicine). 2016;11(4):159-163.
3 Affronti M Low-grade fever: how to distinguish organic from non-organic forms. Int J Clin Pract. 2010;64(3):316-321. - Affronti M. et al., "Subfebrile temperature: how to distinguish organic from non-organic cases." Int Zh Klin Prakt. 2010;64(3):316-321.
Int J Clin Pract. 2010;64(3):316-321. - Affronti M. et al., "Subfebrile temperature: how to distinguish organic from non-organic cases." Int Zh Klin Prakt. 2010;64(3):316-321.
4 Boi B et al. The effectiveness of cabbage leaf application (treatment) on pain and hardness in breast engorgement and its effect on the duration of breastfeeding. JBI Libr Syst Rev . 2012;10(20):1185-1213. - Boys B. et al., "Effectiveness of cabbage leaf (as a drug) for breast pain and engorgement, and its effect on the duration of breastfeeding." JBAi Libr Sist Rev. 2012;10(20):1185-1213.
5 NHS Choices. How do I take someone's temperature? [Internet]. UK: NHS Choices; updated 2016 June 29. Available from : www.nhs.uk/chq/pages/1065.aspx?categoryid=72 - NHS Choice. "How to measure the temperature?" [Internet]. United Kingdom: NHS Choice, 29 June 2016 edition Article linked: www.nhs.uk/chq/pages/1065.aspx?categoryid=72
United Kingdom: NHS Choice, 29 June 2016 edition Article linked: www.nhs.uk/chq/pages/1065.aspx?categoryid=72
Breast engorgement: symptoms and first aid
search support iconSearch keywords
Home ›› How to relieve the unpleasant symptoms of breast engorgement
Home ›› How to relieve the unpleasant symptoms of breast engorgement
↑ Top
One of the most common breastfeeding problems faced by mothers is breast engorgement. While occasional engorgement while breastfeeding is normal, it can be uncomfortable and lead to other problems if not addressed and dealt with. It is important for mothers to understand what breast engorgement is and how to alleviate it.
Let's look at all the important issues, including prevention, symptoms, and help with engorgement.
What is breast engorgement?
Engorgement is an increase in the size of the mammary glands, in which the breast becomes painful and sensitive. This condition is associated with increased blood flow and increased milk production, so it very often occurs during the first few days after childbirth. In addition, engorgement may develop within one to two weeks after childbirth or at any time during breastfeeding. Although this is quite normal during breastfeeding, it can be uncomfortable and sometimes lead to other complications. Therefore, the main thing is to deal with engorgement of the mammary glands immediately when it occurs.
This condition is associated with increased blood flow and increased milk production, so it very often occurs during the first few days after childbirth. In addition, engorgement may develop within one to two weeks after childbirth or at any time during breastfeeding. Although this is quite normal during breastfeeding, it can be uncomfortable and sometimes lead to other complications. Therefore, the main thing is to deal with engorgement of the mammary glands immediately when it occurs.
How long does engorgement last?
All women are different, and, accordingly, the duration of this condition may vary. Some experience mild symptoms for only one day, while others may experience this condition for up to two weeks.
Breast engorgement occurs for various reasons. The most common:
- Skipping a feeding or pumping session.
- Making more milk than the baby eats.
- Insufficient outflow of milk (improper latching on to the breast by the baby).
- Inflammation.
Breast engorgement symptoms
Breast engorgement symptoms vary, but the most common are:
- Breasts become hard or firm.
- Breasts become sore or warm to the touch.
- Breasts become heavy and swollen.
- Breasts become lumpy and swollen.
Although engorgement and mastitis may appear similar, they are actually completely different conditions. How can a mother determine what exactly she has: engorgement or mastitis? Mastitis is an inflammation of the breast that typically results in fever (>38.5°C) and reddening of the breast, while engorgement is the result of excessive milk production and incomplete emptying of the breast. Engorgement can lead to problems such as blockage of the milk ducts or infection of the mammary glands, so it is important to start treating engorgement at the first sign of engorgement.
Prevention of engorgement
There are several ways to prevent this condition. Prevention of breast engorgement in the first days after childbirth can be difficult as the mother's body adapts to the changes. But you can try to avoid it as follows:
Prevention of breast engorgement in the first days after childbirth can be difficult as the mother's body adapts to the changes. But you can try to avoid it as follows:
- Check the mammary glands. Moms should schedule breast checks before the baby is born. The doctor will be able to recommend corrective measures, if needed, to make breastfeeding more comfortable, as well as explain how to distinguish engorgement from mastitis and how to relieve breast engorgement.
- After your baby is born, feed on demand or express milk regularly if you are separated from your baby. Breastfeeding mothers produce milk regularly, so it is important to breastfeed or express milk frequently. Moms should try to feed their baby at least eight times a day and make sure that their breasts are completely empty each time. If a mother is unable to breastfeed her baby, she should express milk with a breast pump.
The electronic breast pump will help you to comfortably and efficiently express the right amount of milk between feedings, if necessary, or instead of feeding when the mother is away from the baby.
3. Make sure that the baby latch on correctly. To learn how to properly breastfeed a baby, a mother can seek advice from a breastfeeding specialist. Proper gripping of the breast during feeding is important for complete emptying of the breast. It also helps prevent other problems such as sore, irritated or cracked nipples.
4. Wean the baby gradually. When it's time to stop breastfeeding, moms shouldn't do it abruptly. It is best to wean the baby gradually, gradually reducing the number of daily feedings. This will gradually slow down milk production and prevent breast engorgement.
Helping with breast engorgement
Breastfeeding with engorgement is not only safe, but essential to prevent worsening of symptoms and provide relief. While the body is learning how to produce the right amount of milk, moms can use the Philips Avent bra pads to absorb excess milk and prevent stains on clothes all day long.
Philips Avent
Philips Avent 2-in-1 thermal pads can both warm and cool your breasts to both stimulate and soothe your breasts after feeding. Mom only needs to place them in a bra for 15-30 minutes before or after feeding (depending on the desired result).
Mom only needs to place them in a bra for 15-30 minutes before or after feeding (depending on the desired result).
Philips Avent
Multifunction thermal pads
SCF258/02Overall rating / 5
- review review reviews Reviews
-
-{discount-value}
- Pictures It is important to achieve optimal outflow of milk during feedings. To stimulate the outflow of milk, during feeding, you can gently massage the breast.
- Express milk. There are situations when a nursing mother cannot be with the baby during feeding. It is important to empty your breasts by expressing milk to prevent engorgement and other problems.
- When feeding, change positions and rotate the mammary glands. Changing your position while breastfeeding can be beneficial, as it improves the outflow of milk from different parts of the mammary glands. In addition, mothers can change their breasts during one feeding so that the baby can empty both of them.
Remember that minor pain and discomfort is completely natural during breastfeeding, but if these symptoms persist or worsen, the mother should consult a doctor.
Philips Avent Articles & Tips
Baby+ App
Download the app and track your baby's development and growth with trackers and keep those special moments forever.
Download app:
Pregnancy+ app
Download one of the world's best pregnancy tracking apps for weekly helpful information, articles and tips about pregnancy and baby development.
Download app:
You are leaving the Philips Healthcare (“Philips”) official website.