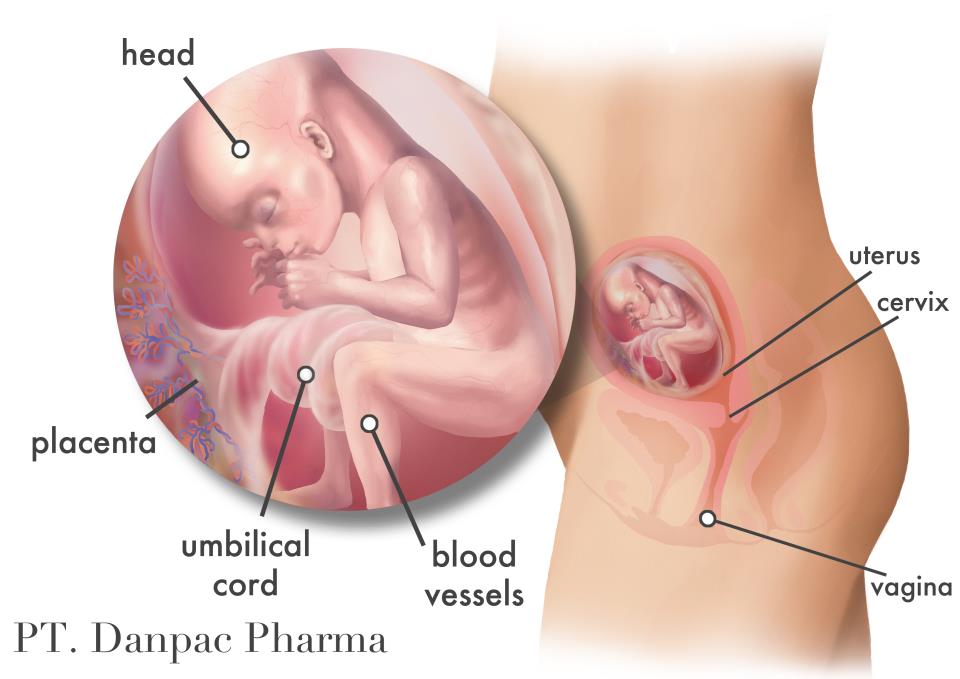
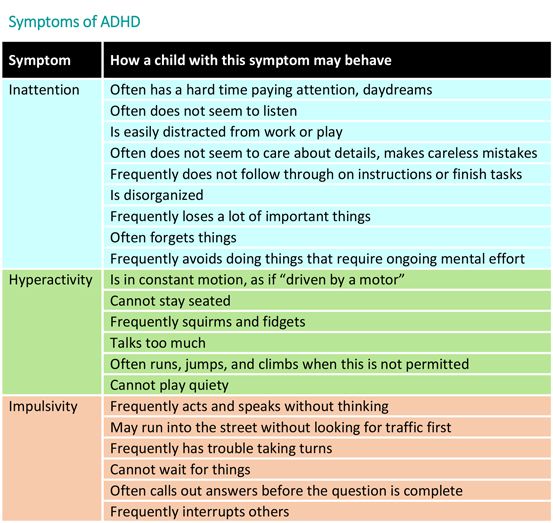
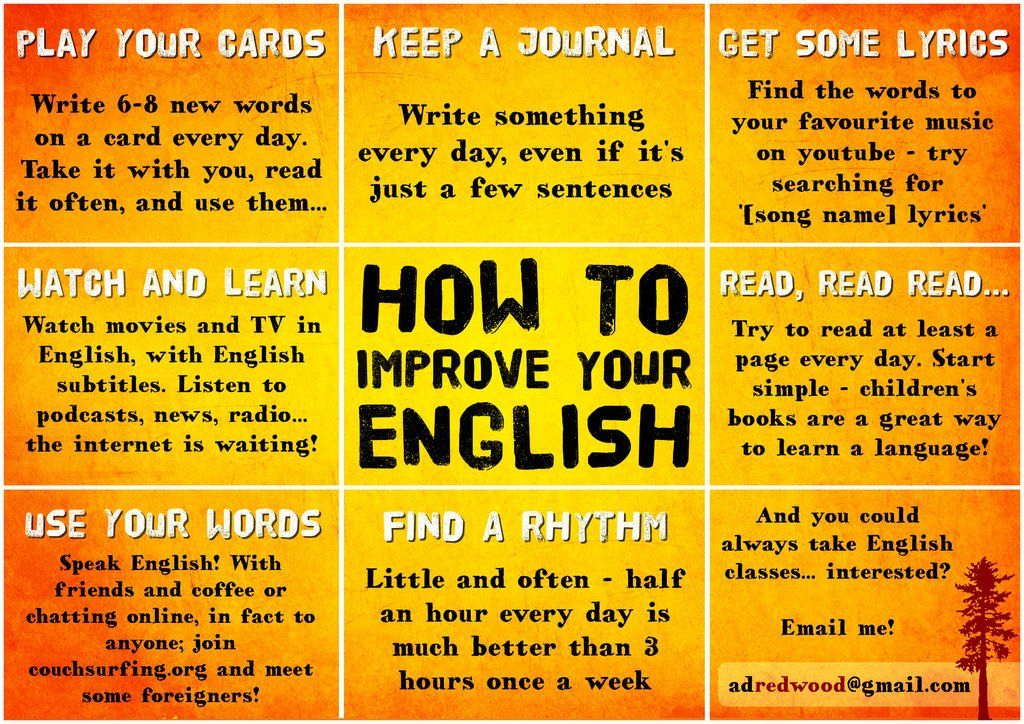
Blindness in newborns
Severe Visual Impairment and Blindness in Infants: Causes and Opportunities for Control
Middle East Afr J Ophthalmol. 2011 Apr-Jun; 18(2): 109–114.
doi: 10.4103/0974-9233.80698
,1,2,3 and 4
Author information Copyright and License information Disclaimer
Childhood blindness has an adverse effect on growth, development, social, and economic opportunities. Severe visual impairment (SVI) and blindness in infants must be detected as early as possible to initiate immediate treatment to prevent deep amblyopia. Although difficult, measurement of visual acuity of an infant is possible. The causes of SVI and blindness may be prenatal, perinatal, and postnatal. Congenital anomalies such as anophthalmos, microphthalmos, coloboma, congenital cataract, infantile glaucoma, and neuro-ophthalmic lesions are causes of impairment present at birth. Ophthalmia neonatorum, retinopathy of prematurity, and cortical visual impairment are acquired during the perinatal period. Leukocoria or white pupillary reflex can be cause by congenital cataract, persistent hyperplastic primary vitreous, or retinoblastoma. While few medical or surgical options are available for congenital anomalies or neuro-ophthalmic disorders, many affected infants can still benefit from low vision aids and rehabilitation. Ideally, surgery for congenital cataracts should occur within the first 4 months of life. Anterior vitrectomy and primary posterior capsulotomy are required, followed by aphakic glasses with secondary intraocular lens implantation at a later date. The treatment of infantile glaucoma is surgery followed by anti-glaucoma medication. Retinopathy of prematurity is a proliferation of the retinal vasculature in response to relative hypoxia in a premature infant. Screening in the first few weeks of life can prevent blindness. Retinoblastoma can be debulked with chemotherapy; however, enucleation may still be required. Neonatologists, pediatricians, traditional birth attendants, nurses, and ophthalmologists should be sensitive to a parent’s complaints of poor vision in an infant and ensure adequate follow-up to determine the cause.
 If required, evaluation under anesthesia should be performed, which includes funduscopy, refraction, corneal diameter measurement, and measurement of intraocular pressure.
If required, evaluation under anesthesia should be performed, which includes funduscopy, refraction, corneal diameter measurement, and measurement of intraocular pressure.
Keywords: Childhood Blindness, Congenital Anomalies, Congenital Cataract, Retinopathy of Prematurity
Visual impairment and blindness in children pose a special problem for ophthalmologists, as many eye care practitioners are not familiar with performing pediatric eye examinations and measuring visual acuity in infants. Infants are unable to verbalize their complaints, and history from parents and care takers may lack important details. The first year of life is also the time when the visual system develops and binocular vision is formed.1 If a visual deficit at this age is not treated in a timely manner, amblyopia and permanent visual deficit can occur. Hence, early diagnosis and prompt treatment is essential. The burden of blindness measured in blind-person years due to childhood blindness is second only to cataract – the most common cause of avoidable blindness in childhood. 2 Studies worldwide show that many of the causes of blindness in children are either preventable or treatable (ie, avoidable).3 Even children who have visual loss that cannot be clinically treated, can be helped with low vision devices and rehabilitation. Childhood blindness affects the individual, their family, and the community. Blindness also has implications for infants’ development, education, and future social, marital, and economic prospects. Nearly 75% of early learning comes from vision. Early onset visual loss can have profound consequences on a child’s motor, social, emotional, and psychological development.4
2 Studies worldwide show that many of the causes of blindness in children are either preventable or treatable (ie, avoidable).3 Even children who have visual loss that cannot be clinically treated, can be helped with low vision devices and rehabilitation. Childhood blindness affects the individual, their family, and the community. Blindness also has implications for infants’ development, education, and future social, marital, and economic prospects. Nearly 75% of early learning comes from vision. Early onset visual loss can have profound consequences on a child’s motor, social, emotional, and psychological development.4
The World Health Organization (WHO) classifies the causes of childhood blindness according to the anatomical site most affected and the underlying etiology.5 Visual loss in infants can be either prenatal (ie, occurring at the time of conception or during the intrauterine period) or postnatal (during or after birth). Prenatal causes are congenital anomalies – anophthalmos, microphthalmos, and coloboma; congenital cataract, retinal dystrophies such as Leber’s congenital amaurosis, infantile glaucoma, and congenital cloudy cornea. In the perinatal period (ie, from the 28th week of gestation through to 1-4 weeks after birth), the following conditions can occur: cortical impairment from birth asphyxia, ophthalmia neonatorum, and retinopathy of prematurity. Postnatal conditions (ie, those acquired after birth) are unusual during infancy. As retinoblastoma can be inherited as an autosomal dominant condition, it is considered a prenatal condition for the purposes of this paper.
In the perinatal period (ie, from the 28th week of gestation through to 1-4 weeks after birth), the following conditions can occur: cortical impairment from birth asphyxia, ophthalmia neonatorum, and retinopathy of prematurity. Postnatal conditions (ie, those acquired after birth) are unusual during infancy. As retinoblastoma can be inherited as an autosomal dominant condition, it is considered a prenatal condition for the purposes of this paper.
Leukocoria may be seen in early infancy can be due to congenital cataract, retinopathy of prematurity (ROP), persistent hyperplastic primary vitreous (PHPV) – anterior or posterior – retinoblastoma or rare genetic disorders such as Norrie’s disease. A leukocoria detected by parents in later infancy may be due to developmental cataract or retinoblastoma. Retinoblastoma is the most common childhood tumor presenting at the age of 12-15 months in bilateral cases and 18-24 months in unilateral cases; it can also develop much later in childhood. It is essential to examine children presenting with leukocoria under anesthesia due to the potentially serious underlying causes.
It is essential to examine children presenting with leukocoria under anesthesia due to the potentially serious underlying causes.
Congenital anomalies
Anophthalmos and microphthalmos are congenital anomalies in which the entire eyeball is entirely absent or smaller than normal from birth. Typical complete uveal coloboma is the most common congenital anomaly in which the embryonic fissure does not close completely by the sixth week of intrauterine life. Coloboma can cause severe visual loss if the defect involves the macula and/or optic nerve. Surveys from schools for the blind in many parts of Asia show that these congenital eye anomalies are a leading cause of blindness and severe visual impairment in children.6–9 These are difficult to research, even in countries with the best healthcare systems and expertise. In the majority of cases, even with in-depth molecular genetic testing and detailed investigation, no cause can be identified.10 This is because these anomalies are likely to be due to genes controlling eye development (which are largely unknown) and possibly, gene-environment interactions, reflecting similar processes elucidated for folic acid and spina bifida. 11 Even if an environmental agent (eg, folate) could be identified, the intervention would have to been extremely broad to have a measurable effect, be inexpensive and safe (as it would need to be given to large numbers of people) and be nonteratogenic – a difficult proposition in developing countries.
11 Even if an environmental agent (eg, folate) could be identified, the intervention would have to been extremely broad to have a measurable effect, be inexpensive and safe (as it would need to be given to large numbers of people) and be nonteratogenic – a difficult proposition in developing countries.
Medical therapy or surgery are rarely effective in congenital cases; however, refraction and low vision aids can help many of these cases.12 Many children with congenital defects can be taught to read print with low vision aids instead of Braille.
PHPV is a congenital anomaly in which the primary vitreous, which extends from the optic disc to the vitreous base at the posterior pole of the lens, persists into childhood.13 This anomaly can cause severe visual loss, and may be associated with microphthalmos. PHPV is usually unilateral, although bilateral cases can occur. Early vitrectomy can be attempted in eyes where the surrounding vitreous is clear and the retina fairly developed; however, the visual outcomes are often suboptimal. 14
14
Infantile glaucoma
Infantile glaucoma can result in blindness without early intervention.15 Surgery followed by medication and optical aids is the treatment of choice. Numerous genes have been implicated and genetic counselling is essential if more than one sibling is affected.
Retinal dystrophies
Retinal dystrophies have variable genetic inheritance and are common in communities with high rates of consanguinity. Although the dystrophy may only give visual symptoms later in life, this is a common cause of blindness in children worldwide, particularly in Middle Eastern countries.16,17 Low vision aids are effective for navigation and reading for individuals affected with retinal dystrophies. Genetic counselling is required if more than one sibling is involved.
Leber’s congenital amaurosis is an autosomal recessive condition that manifests in infancy. The fundus may be normal or show peripheral chorioretinal atrophy and granularity with nystagmus. Oculodigital syndrome, in which the infant constantly rubs or presses on the eyes, which leads to enophthalmos, is common. Other common features include learning disability, deafness, and epilepsy. In Knobloch syndrome nystagmus, high myopia and late retinal detachment are seen. Oculocutaneous albinism, which may be X-linked or autosomal recessive, is detectable at birth. Ocular albinism affects only male infants due to the X-linked inheritance and is usually diagnosed at infancy. Achromatopsy is a rare autosomal recessive heterogeneous group of stationary retinal dystrophies characterized by reduced central vision, poor color vision, and normal fundus. The usual presentation is reduced vision, marked photophobia, and nystagmus in infancy. A macular cherry red spot could be due to Tay-Sachs disease, which is fatal by the second year of life or due to Niemann-Pick disease or Sandhoff disease.
Oculodigital syndrome, in which the infant constantly rubs or presses on the eyes, which leads to enophthalmos, is common. Other common features include learning disability, deafness, and epilepsy. In Knobloch syndrome nystagmus, high myopia and late retinal detachment are seen. Oculocutaneous albinism, which may be X-linked or autosomal recessive, is detectable at birth. Ocular albinism affects only male infants due to the X-linked inheritance and is usually diagnosed at infancy. Achromatopsy is a rare autosomal recessive heterogeneous group of stationary retinal dystrophies characterized by reduced central vision, poor color vision, and normal fundus. The usual presentation is reduced vision, marked photophobia, and nystagmus in infancy. A macular cherry red spot could be due to Tay-Sachs disease, which is fatal by the second year of life or due to Niemann-Pick disease or Sandhoff disease.
Congenital cataract
The birth prevalence of cataract is 3-5/1,000 live births.18 While monogenetic abnormalities, syndromes, metabolic disorders, genetic disorders, and congenital rubella syndrome are recognized causes of this condition, in the majority, the cause is unknown. 19 The importance of congenital cataract is increasing as a cause of blindness among children in developing countries, with other causes declining. There can be 2 years delay from cataract diagnosis to presentation for surgery.20 Early recognition and referral is essential to prevent development of dense amblyopia. However, the timing of intraocular lens (IOL) implantation remains controversial.21 Many experienced surgeons are implanting IOLs in very young children, ie, 12 months or older. While children with unilateral cataract have undergone IOL implantation at as early as 6 months of age, it is better to wait until 2 years of age for implanting IOLs in children with bilateral cataracts.21,22 In \ children where the risk of general anesthesia very high, bilateral surgery at the same visit is advisable; however, this should be an exception rather than the rule. There is almost a hundred percent posterior capsular opacification in pediatric eyes.
19 The importance of congenital cataract is increasing as a cause of blindness among children in developing countries, with other causes declining. There can be 2 years delay from cataract diagnosis to presentation for surgery.20 Early recognition and referral is essential to prevent development of dense amblyopia. However, the timing of intraocular lens (IOL) implantation remains controversial.21 Many experienced surgeons are implanting IOLs in very young children, ie, 12 months or older. While children with unilateral cataract have undergone IOL implantation at as early as 6 months of age, it is better to wait until 2 years of age for implanting IOLs in children with bilateral cataracts.21,22 In \ children where the risk of general anesthesia very high, bilateral surgery at the same visit is advisable; however, this should be an exception rather than the rule. There is almost a hundred percent posterior capsular opacification in pediatric eyes. Experts recommend primary posterior capsulotomy and anterior vitrectomy in children up to the age of 6-7 years. At 6 years or older, the child can sit on a slit lamp for Nd:YAG laser capsulotomy after surgery, if required.21 The anterior vitrectomy removes the almost solid vitreous base, which can act as a scaffold for migrating lenticular cells. The pars plana approach has the advantage of keeping the primary incision and the anterior chamber free of vitreous, but this is technically demanding for anterior segment surgeons. Moreover, there is an exaggerated fear of suprachoroidal hemorrhage.23 Vitrectomy through limbal side ports is easier but the surgeon has to be meticulous in removing vitreous from the anterior chamber. The primary posterior capsulotomy can be performed before or after inserting the intraocular lens. There is a risk of the capsulotomy extending during the implantation of a foldable lens. An MVR blade may be used to make a ’nick’ below the implanted lens to later enlarge the opening with a vitrectors.
Experts recommend primary posterior capsulotomy and anterior vitrectomy in children up to the age of 6-7 years. At 6 years or older, the child can sit on a slit lamp for Nd:YAG laser capsulotomy after surgery, if required.21 The anterior vitrectomy removes the almost solid vitreous base, which can act as a scaffold for migrating lenticular cells. The pars plana approach has the advantage of keeping the primary incision and the anterior chamber free of vitreous, but this is technically demanding for anterior segment surgeons. Moreover, there is an exaggerated fear of suprachoroidal hemorrhage.23 Vitrectomy through limbal side ports is easier but the surgeon has to be meticulous in removing vitreous from the anterior chamber. The primary posterior capsulotomy can be performed before or after inserting the intraocular lens. There is a risk of the capsulotomy extending during the implantation of a foldable lens. An MVR blade may be used to make a ’nick’ below the implanted lens to later enlarge the opening with a vitrectors. 23 A-scan biometry and keratometry need to be performed under anesthesia. Hydrophobic acrylic or poly-methyl-methacrylate IOLs are best for infants. Generally, the target postoperative refraction is emmetropia by the age of 5-6 years. Aphakic glasses have to be corrected for near vision.
23 A-scan biometry and keratometry need to be performed under anesthesia. Hydrophobic acrylic or poly-methyl-methacrylate IOLs are best for infants. Generally, the target postoperative refraction is emmetropia by the age of 5-6 years. Aphakic glasses have to be corrected for near vision.
Pediatric cataract surgery is one step in a series of interventions required to rehabilitate vision.24 Postoperative management includes frequent steroid eye drops with cycloplegia, followed by early, accurate, and repeated refractions and treatment of amblyopia by patching the better seeing eye. Late complications of pediatric IOL implantation include opacification of the visual axis and glaucoma, the latter being particularly difficult to treat. Parents must be counselled about the need for regular ophthalmic examination, refraction, and intraocular pressure measurement. It is important to remember that aphakic/pseudophakic children need correction for near as well as distance, and many are able to tolerate executive bifocals very well. 21,24
21,24
Retinoblastoma
Retinoblastoma is the most common intraocular malignancy in early childhood. It usually presents after infancy as leukocoria, esotropia, or masquerades as uveitis. Lesions detected early can be treated with chemotherapy with preservation of the globe; however, larger lesions may need enucleation.25,26 A prosthesis needs to be implanted in the child’s eye to prevent the contracture of the socket. A mule’s implant wrapped in a sclera shell or dermal fat grafts may be used for this purpose. Management with specialist tertiary oncology services is also advisable.
Ophthalmia neonatorum
This is an eminently preventable condition in which the eyes of the infant become infected in the birth passage during delivery. Credé’s prophylaxis and antenatal testing or treatment of sexually transmitted diseases during pregnancy can prevent the condition. Credé’s prophylaxis entails cleaning the infants’ eyes immediately after birth with instillation of a topical antibiotic (eg, tetracycline eye ointment) or antiseptic (eg, 2. 5% povidone iodine). Traditionally, a 2% solution of silver nitrate was used for Credé’s prophylaxis. The agent used depends on the local epidemiology of sexually transmitted diseases and the organism’s sensitivity to antibiotics. Treatment of ophthalmia neonatorum must entail systemic as well as topical treatment, to ensure treatment of extraocular sites of infection (eg, pneumonia).
5% povidone iodine). Traditionally, a 2% solution of silver nitrate was used for Credé’s prophylaxis. The agent used depends on the local epidemiology of sexually transmitted diseases and the organism’s sensitivity to antibiotics. Treatment of ophthalmia neonatorum must entail systemic as well as topical treatment, to ensure treatment of extraocular sites of infection (eg, pneumonia).
Retinopathy of prematurity
Retinopathy of prematurity (ROP) is responsible for up to 15% of all causes of blindness in developed countries and up to 60% in middle income countries.27 A number of risk factors are implicated in the development of ROP. However, the most commonly identified risk factors are the degree of immaturity measured by birth weight (BW), gestational age (GA), and prolonged exposure to supplementary oxygen.28 Paradoxically, the hyperbaric oxygen that saves an infant’s life, if not properly controlled and tapered, can cause blindness. There are several trials seeking to define safe upper and lower limits of arterial oxygen saturation. 29 The improvement in neonatal care can lead to an increase in survival rates of premature infants in middle-income countries and major metropolises of even poorer countries. As a consequence, ROP has become a very important cause of childhood in these developing economies, where quality of neonatal care still needs to improve. The disease is classified by severity (stages I-V), by site (zones 1-3), and by extent (clock hours 1-12). While most developed countries screen infants by BW < 1,500 g,30 middle income and developing countries need larger BW criteria as infants weighing up to 2,500 g are developing severe ROP.31,32 Appropriate screening protocols ensure early detection in the first weeks of life so that treatment (peripheral ablation of avascular retina) with laser or cryotherapy can be provided. So far, there is no evidence provided by clinical trials that surgery is beneficial for cases in stages IV and V. Anti-vascular endothelial growth factors (VEGFs) are promising drugs for treatment of retinal proliferative diseases in adults.
29 The improvement in neonatal care can lead to an increase in survival rates of premature infants in middle-income countries and major metropolises of even poorer countries. As a consequence, ROP has become a very important cause of childhood in these developing economies, where quality of neonatal care still needs to improve. The disease is classified by severity (stages I-V), by site (zones 1-3), and by extent (clock hours 1-12). While most developed countries screen infants by BW < 1,500 g,30 middle income and developing countries need larger BW criteria as infants weighing up to 2,500 g are developing severe ROP.31,32 Appropriate screening protocols ensure early detection in the first weeks of life so that treatment (peripheral ablation of avascular retina) with laser or cryotherapy can be provided. So far, there is no evidence provided by clinical trials that surgery is beneficial for cases in stages IV and V. Anti-vascular endothelial growth factors (VEGFs) are promising drugs for treatment of retinal proliferative diseases in adults. However, extreme caution is warranted in infants, as these drugs interfere with the normal development of vasculature elsewhere in the body and may impede development of the lungs and alveoli of the lungs, which are VEGF-sensitive and develop at the same time as does ROP.33 Premature infants are at increased risk of developing refractive errors, strabismus, amblyopia, and low vision; hence, long-term follow-up is recommended.
However, extreme caution is warranted in infants, as these drugs interfere with the normal development of vasculature elsewhere in the body and may impede development of the lungs and alveoli of the lungs, which are VEGF-sensitive and develop at the same time as does ROP.33 Premature infants are at increased risk of developing refractive errors, strabismus, amblyopia, and low vision; hence, long-term follow-up is recommended.
Optic nerve lesions and cerebral visual impairment
Optic nerve lesions and cerebral visual impairment are the most common causes of visual impairment in many developed countries34 where these are often a consequence of preterm birth.35 Birth asphyxia, which causes cerebral palsy, may affect the optic nerve and cause cortical visual impairment. Little can be done by way of medical treatment. Low vision aids and rehabilitation are often the only recourse. Often, such children are severely handicapped, which makes assessment and management even more challenging.
Keratomalacia cause by acute deficiency of vitamin A is very unusual in the first year of life, and most infants before the age of 9 months (when they are immunized) will have protective measles antibodies received from their mother. The common causes of blindness in childhood such as vitamin A deficiency, measles, trauma, and trachoma are uncommon in infancy. Unless the refractive error is very large [>3-4 diopter (D)], or is causing strabismus, spectacles are not required in infants. However, if the infant has low vision, even small refractive errors may need correction.
While evaluation of a visually impaired infant may seem challenging for the general ophthalmologist, the task is not that difficult. Infants are best examined in the position they are most comfortable – on their parents’ shoulders, in their laps, or cribs. We recommend not making the infant and parents wait in a busy waiting area. A separate area for breastfeeding is welcome, as this puts the mother and child at ease. The infant can be examined for fixating and following of the flashlight. The ophthalmologist should also have a quick look at the cornea, anterior chamber, lens, and pupillary reflex. A handheld slit lamp is the best instrument for this component of the evaluation. The red reflex should be examined to rule out congenital cataract, advanced ROP, and other causes of leukocoria. If the child is uncooperative or distressed, the examination can be repeated after a few hours or next day after instilling atropine eye ointment to dilate the pupil. However, the drug may affect the pupil for a week. Cyclopentolate 0.1%, tropicamide 0.1%, and phenylephrine 2.5% eye drops may also be instilled, though there is a risk of toxicity due to systemic absorption. Cyclopentolate and tropicamide are parasympatholytic agents acting on sphincter pupillae, whereas phenylephrine is sympathomimetic acting on the dilator papillae muscle. The child can also be given 2.5 ml of phenergan syrup (properazine – a mild sedative and antihistamine combination) and then breastfed to lull it into sleep.
The infant can be examined for fixating and following of the flashlight. The ophthalmologist should also have a quick look at the cornea, anterior chamber, lens, and pupillary reflex. A handheld slit lamp is the best instrument for this component of the evaluation. The red reflex should be examined to rule out congenital cataract, advanced ROP, and other causes of leukocoria. If the child is uncooperative or distressed, the examination can be repeated after a few hours or next day after instilling atropine eye ointment to dilate the pupil. However, the drug may affect the pupil for a week. Cyclopentolate 0.1%, tropicamide 0.1%, and phenylephrine 2.5% eye drops may also be instilled, though there is a risk of toxicity due to systemic absorption. Cyclopentolate and tropicamide are parasympatholytic agents acting on sphincter pupillae, whereas phenylephrine is sympathomimetic acting on the dilator papillae muscle. The child can also be given 2.5 ml of phenergan syrup (properazine – a mild sedative and antihistamine combination) and then breastfed to lull it into sleep. This allows more detailed fundus and external ocular evaluation, and measurement of intraocular pressure by non-contact or Perkins (more accurate) tonometer. If a serious lesion such as retinoblastoma is suspected, an evaluation under anesthesia is essential for detailed examination of the fundus. The opportunity must be utilized not just to examine the fundus but to also perform tonometry, refraction, measurement of corneal diameter, and axial length.
This allows more detailed fundus and external ocular evaluation, and measurement of intraocular pressure by non-contact or Perkins (more accurate) tonometer. If a serious lesion such as retinoblastoma is suspected, an evaluation under anesthesia is essential for detailed examination of the fundus. The opportunity must be utilized not just to examine the fundus but to also perform tonometry, refraction, measurement of corneal diameter, and axial length.
Orthoptic evaluation of an infant requires patience. Jampolsky’s dictum of “one toy-one look” should be used to examine the infant’s ocular motility in the nine cardinal directions of gaze. An assortment of soft toys, brightly colored objects, and even mobile phones can be used to arouse the child’s interest. The objects should not make noise as the child will be attracted through the auditory and not the visual signals, which would defeat the purpose of the examination. Visual acuity can be formally assessed using forced preferential looking tests (eg, Cardiff cards), with the child sitting comfortably on a parent’s lap. The test is based on the psychological percept that humans are attracted to novel stimuli. If the child is shown a line drawing at one end of the card sheet and the other end is kept blank, the child will divert its eyes to the drawing rather than the blank area. The line drawings are made progressively finer to estimate higher orders of form vision. Worth’s ivory fall test and small sweets commonly used to decorate cakes, “hundreds and thousands”, can also be used. The child picks up the small sweets if it is able to see them. At first, bilateral vision is tested followed by monocular testing. The mother should be asked to occlude the infant’s eyes one at a time, and report on the infant’s response. If the infant objects to occlusion of one eye, this may indicate the visual acuity of the other eye is poor.
The test is based on the psychological percept that humans are attracted to novel stimuli. If the child is shown a line drawing at one end of the card sheet and the other end is kept blank, the child will divert its eyes to the drawing rather than the blank area. The line drawings are made progressively finer to estimate higher orders of form vision. Worth’s ivory fall test and small sweets commonly used to decorate cakes, “hundreds and thousands”, can also be used. The child picks up the small sweets if it is able to see them. At first, bilateral vision is tested followed by monocular testing. The mother should be asked to occlude the infant’s eyes one at a time, and report on the infant’s response. If the infant objects to occlusion of one eye, this may indicate the visual acuity of the other eye is poor.
There is a narrow window of opportunity in treating a visually impaired infant. Binocular single vision develops by 6 months of life and a visual deficit, if not detected and treated in time, may leave the child bereft of stereopsis. The amblyopia that develops from visual deprivation of early onset, irrespective of the cause, can be dense and difficult to treat.
The amblyopia that develops from visual deprivation of early onset, irrespective of the cause, can be dense and difficult to treat.
Pediatricians, general practitioners, and midwives should be educated and encouraged to perform the red reflex test. Using the direct ophthalmoscope, they should be taught to detect any opacity seen in the infant’s red reflex. All healthcare personnel working for the care of the infant should be sensitized to the eye conditions in infancy and on the causes of childhood blindness and visual impairment. Their training curricula should emphasize on the importance of early detection and treatment of such children. Training of midwives, traditional birth attendants, healthcare workers working for child health and immunization would be of immense help in early detection of such children.
The major barrier to accessing eye care services for infants is the absence of trained personnel who can diagnose a problem early. Developed countries have established referral systems between family practitioners, health visitors, neonatal units, and pediatric ophthalmology and retina specialist. However, pediatric eye care centers are rare in developing countries. There are financial and geographic barriers for many parents from poorer communities. Diagnostic, curative, and rehabilitative services may not be available in the region. Pediatric eye care interventions are also more expensive than adult treatment. For example, general anesthesia is often required for examination and treatment. This entails liaison with other medical practitioners such as pediatricians, anesthetists, and neonatologists. Another significant barrier is the lack of knowledge on the part of healthcare providers. Many healthcare workers, including physicians ask parents to wait until the child is older before any treatment can be given. Some physicians are unsure about what needs to be done. Others believe that the problem may resolve, as the child grows older or that a unilateral condition does not matter as long as the other eye is healthy. Due to these misconceptions, appropriate referral may too late if dense amblyopia has occurred.
However, pediatric eye care centers are rare in developing countries. There are financial and geographic barriers for many parents from poorer communities. Diagnostic, curative, and rehabilitative services may not be available in the region. Pediatric eye care interventions are also more expensive than adult treatment. For example, general anesthesia is often required for examination and treatment. This entails liaison with other medical practitioners such as pediatricians, anesthetists, and neonatologists. Another significant barrier is the lack of knowledge on the part of healthcare providers. Many healthcare workers, including physicians ask parents to wait until the child is older before any treatment can be given. Some physicians are unsure about what needs to be done. Others believe that the problem may resolve, as the child grows older or that a unilateral condition does not matter as long as the other eye is healthy. Due to these misconceptions, appropriate referral may too late if dense amblyopia has occurred.
Even when the infant has been referred for treatment appropriately, many parents believe that their infant is too small to undergo surgery or wear spectacles and, in some communities, visual loss in infants is not considered a priority for the family, especially for females.
However, a child who cannot be helped by medicine or surgery may still benefit from use of spectacles and/or low vision aids. Completely and irreversibly blind children can benefit by rehabilitation and special school education. This should be emphasized during parent counselling. Ophthalmologists should be nonjudgmental and empathetic while breaking the news about a potentially blinding condition. Ocular conditions, which have a genetic or familial basis, may be blamed on one of the parents. The ophthalmologist should spend some time with the parents to reassure, counsel, and suggest various alternatives that are available for the infant. It may take the parents some time to come to terms with their child’s visual loss. Frequent ophthalmic visits to confirm the level of vision and make a definitive diagnosis can be difficult for parents. A social worker or counsellor can establish a rapport with the parents or caretakers to ensure that they comply with the treatment as much as possible.
Frequent ophthalmic visits to confirm the level of vision and make a definitive diagnosis can be difficult for parents. A social worker or counsellor can establish a rapport with the parents or caretakers to ensure that they comply with the treatment as much as possible.
Blindness and severe visual impairment in infants is not that difficult to detect and diagnose. With proper care, most of these infants can be helped and formation of dense amblyopia prevented. Even if the ophthalmologist may not be able to help medically or surgically, optical aids and rehabilitation can help children reach their full capacity.
Source of Support: Nil
Conflict of Interest: None declared.
1. Day S. Normal and abnormal visual development. In: David T, editor. Pediatric ophthalmology. Section 1. Chapter 2. Oxford UK: Blackwell Science; 1997. pp. 13–28. [Google Scholar]
2. Rahi JS, Gilbert CE, Foster A, Minassian D. Measuring the burden of childhood blindness. Br J Ophthalmol. 1999;83:387–8. [PMC free article] [PubMed] [Google Scholar]
Br J Ophthalmol. 1999;83:387–8. [PMC free article] [PubMed] [Google Scholar]
3. Gilbert C, Rahi JS, Quinn GE. Visual impairment and blindness in children. In: Jhonson GJ, Minassian D, Weale RA, West SK, editors. Epidemiology of Eye Disease. 2nd ed. London: Arnold publishers; 2003. pp. 260–86. [Google Scholar]
4. Dale N, Salt A. Early support developmental journal for children with visual impairment: The case for a new developmental framework for early intervention. Child Care Health Dev. 2007;33:684–90. [PubMed] [Google Scholar]
5. Gilbert C, Foster A, Negrel AD, Thylefors B. Childhood blindness: A new form for recording causes of visual loss in children. Bull World Health Organ. 1993;71:485–9. [PMC free article] [PubMed] [Google Scholar]
6. Gogate P, Deshpande M, Sudrik S, Kishore H, Taras S, Deshpande M. Changing pattern of childhood blindness in Maharashtra, India. Br J Ophthalmol. 2007;91:8–12. [PMC free article] [PubMed] [Google Scholar]
7. Njuguna M, Msukwa G, Shilio B, Tumwesigye C, Courtright P, Lewallen S. Causes of severe visual impairment and blindness in children in schools for the blind in eastern Africa: Changes in the last 14 years. Ophthalmic Epidemiol. 2009;16:151–5. [PubMed] [Google Scholar]
Causes of severe visual impairment and blindness in children in schools for the blind in eastern Africa: Changes in the last 14 years. Ophthalmic Epidemiol. 2009;16:151–5. [PubMed] [Google Scholar]
8. Gogate P, Kishore H, Dole K, Shetty J, Gilbert C, Ranade S, et al. The pattern of childhood blindness in Karnataka, South India. Ophthalmic Epidemiol. 2009;16:212–7. [PubMed] [Google Scholar]
9. Sitorus RS, Abidin MS, Prihartono J. Causes and temporal trends of childhood blindness in Indonesia: Study at schools for the blind in Java. Br J Ophthalmol. 2007;91:1109–13. [PMC free article] [PubMed] [Google Scholar]
10. Shah SP, Taylor AE, Sowden JC, Ragge NK, Russell-Eggitt I, Rahi JS, et al. Anophthalmos, micophthalmos and typical coloboma in the United Kingdom: A prospective study of incidence and risk. Invest Ophthalmol Vis Sci. 2011;52:558–64. [PubMed] [Google Scholar]
11. Hornby SJ, Ward SJ, Gilbert CE. Hypothesis: Eye birth defects in humans may be caused by a recessively-inherited genetic predisposition to the effects of maternal vitamin A deficiency during pregnancy. Med Sci Monit. 2003;9:HY23–6. [PubMed] [Google Scholar]
Med Sci Monit. 2003;9:HY23–6. [PubMed] [Google Scholar]
12. Hornby SJ, Adolph S, Gothwal VK, Gilbert CE, Dandona L, Foster A. Requirements for optical services in children with microphthalmos, coloboma and microcornea in southern India. Eye. 2000;14:219–24. [PubMed] [Google Scholar]
13. Shastry BS. Persistent hyperplastic primary vitreous: Congenital malformation of the eye. Clin Exp Ophthalmol. 2009;37:884–90. [PubMed] [Google Scholar]
14. Walsh MK, Drenser KA, Capone A, Jr, Trese MT. Early vitrectomy effective for bilateral combined anterior and posterior persistent fetal vasculature syndrome. Retina. 2010;30:S2–8. [PubMed] [Google Scholar]
15. Mandal AK, Bhatia PG, Bhaskar A, Nutheti R. Long-term surgical and visual outcomes in Indian children with developmental glaucoma operated on within 6 months of birth. Ophthalmology. 2004;111:283–90. [PubMed] [Google Scholar]
16. Kotb AA, Hammouda EF, Tabbara KF. Childhood blindness at a school for the blind in Riyadh, Saudi Arabia. Ophthalmic Epidemiol. 2006;13:1–5. [PubMed] [Google Scholar]
Ophthalmic Epidemiol. 2006;13:1–5. [PubMed] [Google Scholar]
17. Cetin E, Yaman A, Berk AT. Etiology of childhood blindness in Izmir, Turkey. Eur J Ophthalmol. 2004;14:531–7. [PubMed] [Google Scholar]
18. Rahi JS, Dezateux C. British Congenital Cataract Interest Group. Measuring and interpreting the incidence of congenital ocular anomalies: Lessons from a national study of congenital cataract in the UK. Invest Ophthalmol Vis Sci. 2001;42:1444–8. [PubMed] [Google Scholar]
19. Rahi JS, Dezateux C. Congenital and infantile cataract in the United Kingdom: Underlying or associated factors. British Congenital Cataract Interest Group. Invest Ophthalmol Vis Sci. 2000;41:2108–14. [PubMed] [Google Scholar]
20. Mwende J, Bronsard A, Mosha M, Bowman R, Geneau R, Courtright P. Delay in presentation to hospital for surgery for congenital and developmental cataract in Tanzania. Br J Ophthalmol. 2005;89:1478–82. [PMC free article] [PubMed] [Google Scholar]
21. Wilson ME, Pandey SK, Thakur J. Paediatric cataract blindness in the developing world: Surgical techniques and intraocular lenses in the new millennium. Br J Ophthalmol. 2003;87:14–9. [PMC free article] [PubMed] [Google Scholar]
Paediatric cataract blindness in the developing world: Surgical techniques and intraocular lenses in the new millennium. Br J Ophthalmol. 2003;87:14–9. [PMC free article] [PubMed] [Google Scholar]
22. Ram J, Brar GS, Kaushik S, Sukhija J, Bandyopadhyay S, Gupta A. Primary intraocular lens implantation in the first two years of life: safety profile and visual results. Indian J Ophthalmol. 2007;55:185–9. [PubMed] [Google Scholar]
23. Gogate P. Complications of pediatric cataract surgery. Highlights Ophthalmol. 2009;37:12–5. [Google Scholar]
24. Gogate P, Khandekar R, Srisimal M, Dole K, Taras S, Kulkarni S, et al. Cataracts with delayed presentation. Are they worth operating upon? Ophthalmic Epidemiol. 2010;17:25–33. [PubMed] [Google Scholar]
25. Shields CL, Honavar SG, Meadows AT, Shields JA, Demirci H, Naduvilath TJ. Chemoreduction for unilateral retinoblastoma. Arch Ophthalmol. 2002;120:1653–8. [PubMed] [Google Scholar]
26. Honavar SG. Emerging options in the management of advanced intraocular retinoblastoma. Br J Ophthalmol. 2009;93:848–9. [PubMed] [Google Scholar]
Br J Ophthalmol. 2009;93:848–9. [PubMed] [Google Scholar]
27. Gilbert C, Fielder A, Gordillo L, Quinn G, Semiglia R, Visintin P, et al. ; For the International NO-ROP Group. Characteristics of babies with severe retinopathy of prematurity in countries with low, moderate and high levels of development: Implications for screening programmes. Pediatrics. 2005;115:e518–25. [PubMed] [Google Scholar]
28. McColm JR, Fleck BW. Retinopathy of prematurity: Causation. Semin Neonatol. 2001;6:453–60. [PubMed] [Google Scholar]
29. Carlo WA, Finer NN, Walsh MC, Rich W, Gantz MG, Laptook AR, et al. Support Study Group of the Eunice Kennedy Shriver NICHD Neonatal Research Network. Target ranges of oxygen saturation in extremely preterm infants. N Engl J Med. 2010;362:1970–9. [PMC free article] [PubMed] [Google Scholar]
30. Wilkinson AR, Haines L, Head K, Fielder AR. UK retinopathy of prematurity guideline. Early Hum Dev. 2008;84:71–4. [PubMed] [Google Scholar]
31. Vinekar A, Dogra MR, Sangtam T, Narang A, Gupta A. Retinopathy of prematurity in Asian Indian babies weighing greater than 1250 grams at birth: Ten year data from a tertiary care center in a developing country. Indian J Ophthalmol. 2007;55:331–6. [PMC free article] [PubMed] [Google Scholar]
Retinopathy of prematurity in Asian Indian babies weighing greater than 1250 grams at birth: Ten year data from a tertiary care center in a developing country. Indian J Ophthalmol. 2007;55:331–6. [PMC free article] [PubMed] [Google Scholar]
32. Shah PK, Narendran V, Kalpana N, Gilbert C. Severe retinopathy of prematurity in big babies in India: History repeating itself? Indian J Pediatr. 2009;76:801–4. [PubMed] [Google Scholar]
33. Darlow BA, Gilbert C, Quinn GE, Azad R, Ells AL, Fielder A, et al. Promise and potential pitfalls of anti-VEGF drugs in retinopathy of prematurity. Br J Ophthalmol. 2009;93:986. [PubMed] [Google Scholar]
34. Rudanko SL, Laatikainen L. Visual impairment in children born at full term from 1972 through 1989 in Finland. Ophthalmology. 2004;111:2307–12. [PubMed] [Google Scholar]
35. Rudanko SL, Fellman V, Laatikainen L. Visual impairment in children born prematurely from 1972 through 1989. Ophthalmology. 2003;110:1639–45. [PubMed] [Google Scholar]
What Causes Blindness at Birth? | For Eyes
People of all ages can endure issues with their eyesight, even infants. From obstacles during pregnancy to developmental problems, the reasons behind vision loss in babies can vary.
From obstacles during pregnancy to developmental problems, the reasons behind vision loss in babies can vary.
To find out more about what causes blindness at birth, keep reading. For Eyes is here to help.
What causes blindness at birth?
Like other age groups, newborns are not immune to blindness. Your little one’s eyes will need to be inspected from the time they’re born, such as for congenital cataracts, which may appear as unpigmented spots on your child’s eyes.
Congenital cataracts are a potential cause of vision loss in infants that can sometimes go undetected until your child is older, which is why every child needs an eye exam by 6 months of age. (The next eye exam should be at 3 years old and then again at age 6, with an appointment every year after into adulthood.)
What else causes blindness at birth? Issues with your child’s eye development or problems with the portion of the brain that controls vision may impact your child’s eyesight.
Another one of the potential causes of blindness in infants is retinopathy of prematurity (ROP), which affects the blood vessels in the retina. It most often impacts premature babies who are less than three pounds. When an infant is born early, their retina and blood vessels may not finish developing, which can inhibit oxygen absorption around the retina.
It most often impacts premature babies who are less than three pounds. When an infant is born early, their retina and blood vessels may not finish developing, which can inhibit oxygen absorption around the retina.
Due to this, the retina may be alerted to create new blood vessels. These can be delicate, and they tend to leak fluids, which can create marks and scars. The scars can yank on the retina as your child grows, which can make the retina move from its place behind the eye. Even if retinal detachment does not occur, your little one’s vision can still be impacted, usually making their direct line of sight blurry at the least.
According to the American Optometric Association (AOA), if your child has other health issues, they may have a higher chance of developing ROP. However, how much your little one weighs and when they’re born are some of the most significant risk factors.
What are the symptoms of blindness in babies?
From the day your child is born, it’s a good idea to watch for symptoms of blindness. In babies, the way to do so is to work with an eye doctor, who will inspect how your child’s eyes function together and apart. They may also look at how your child’s eyes respond to light, which can indicate a vision concern if the light doesn’t seem to affect them.
In babies, the way to do so is to work with an eye doctor, who will inspect how your child’s eyes function together and apart. They may also look at how your child’s eyes respond to light, which can indicate a vision concern if the light doesn’t seem to affect them.
Here are some other common symptoms of blindness in babies and children:
- Discolored pupils
- Eye movement issues
- Light sensitivity
- Red eyes
- Touching the eyes often
Remember: These symptoms don’t always indicate oncoming blindness. When your little one is young, it can take time for their eyes to develop. If you notice any symptoms happening more often than usual, consult an Independent Doctor of Optometry in your area.
Summary: Blindness in Babies
Monitoring symptoms of blindness in babies and children is the best way to detect eye issues early on and get your child the right treatment. If your child exhibits any signs of eye issues, such as discoloration in the pupils or light sensitivity, we encourage you to reach out to an optometrist.
Are you curious about what causes blindness at birth? Two of the main conditions to watch for are congenital cataracts and ROP.
While these issues are by no means the only ones that can affect your baby’s eyes, they’re some important ones to monitor. By ensuring your little one gets a comprehensive eye exam by 6 months old, you can usually catch these conditions before they progress too much.
Book your eye exam at For Eyes
Have you had your annual comprehensive eye exam? Schedule an appointment with an Independent Doctor of Optometry at your local For Eyes.
Book an Exam
Kids Eye Health Eyeglasses eye doctor eye exam Eye Health eye pain question eye doctor symptoms eye eye eyewear routine eye exam birth BlindnessVision in infants: the formation of the visual system after birth.

From All About Vision
Your heart skips a beat when your newborn baby opens its eyes and looks at you for the first time.
Don't worry if it doesn't happen right away. In newborns, the visual system develops gradually.
In the very first week of life, a child sees the world differently: indistinctly and in shades of gray.
Only a few months after birth, the baby's visual system will work to its full potential. Knowing the key milestones in the development of the eyes of a newborn baby (and how to help them along) will help you understand that your baby is developing normally and enjoying life.
Baby's eye development begins during pregnancy
Your baby's visual system begins to develop even before birth. Therefore, how you take care of yourself and your body during pregnancy is important and affects the development of the body and mental abilities of the child, including the eyes and visual centers in the brain.
Be sure to follow the nutritional advice your doctor gives you. Be sure to take your prescribed supplements and vitamins, and get enough rest.
Be sure to take your prescribed supplements and vitamins, and get enough rest.
Do not smoke or drink alcohol during pregnancy, as toxins can cause many health problems for the baby, in particular vision problems.
Smoking is especially dangerous during pregnancy. Cigarette smoke contains about 3,000 different chemicals (such as carbon monoxide or carbon monoxide) that can harm a person.
Even regular aspirin can be dangerous: it increases the risk of having a low birth weight baby and complications during childbirth. Low body weight, in turn, can contribute to vision problems.
Always check with your doctor before taking any medication during pregnancy. This also applies to over-the-counter drugs, herbal supplements, and other over-the-counter medications.
Eye Condition at Birth
Shortly after birth, your pediatrician or neonatologist will examine your baby's eyes for congenital cataracts or other serious neonatal eye problems in newborns.
Although such diseases are rather an exception, it is better to detect and treat them at an early stage in order to reduce the pathological impact on the development of the infant's visual system.
To protect the child's eyes from pathogenic bacteria and microorganisms that could enter them during the passage through the birth canal and cause eye infection , an antibiotic ointment is placed in them. Early prevention of possible eye infections is very important for the normal development of the visual system.
ARE YOU CONCERNED WITH YOUR BABY'S VISION? Find an optometrist nearby .
At birth, your baby sees objects only in black and white and in shades of gray. This is due to the fact that the nerve cells in the retina and brain that are responsible for color perception are not yet fully developed.
A newborn baby is not yet able to focus on nearby objects (disturbance of accommodation). Don't worry if you notice that your baby is unable to "focus" on objects or on your face. It will take time for him to acquire this ability.
Don't worry if you notice that your baby is unable to "focus" on objects or on your face. It will take time for him to acquire this ability.
Despite all these features, studies have shown that just a few days after birth, the baby is able to distinguish the mother's face from the face of a stranger.
Scientists believe that the baby recognizes the mother's face thanks to the contrasting hairline. (During the study, women covered their hair with a scarf or swimming cap, and the baby could not tell the mother's face from that of a stranger.)
Therefore, to encourage eye contact, during the first weeks of a child's life, do not change the hairstyle or appearance.
You may also notice that babies have rather large eyes. This is because usually a child's head grows first, and then the rest of the body. At birth, a baby's eyes are 65% the size of an adult's eyes!
Baby's eyes in the first month of life
In the first month of life, the baby's eyes are not highly sensitive to light. By the way, in order for a child who is 1 month old to understand that there is light in the room (the threshold of sensitivity to light), the light must be 50 times brighter than normal.
By the way, in order for a child who is 1 month old to understand that there is light in the room (the threshold of sensitivity to light), the light must be 50 times brighter than normal.
Don't be afraid to leave a light on in the nursery, because it won't disturb the baby's sleep and you won't trip over the furniture when you go to visit him at night!
Very quickly the baby acquires the ability to distinguish colors. A week after birth, the baby can see red, orange, yellow and green. A little later, he will be able to distinguish between blue and purple. This is because blue light is the shortest wavelength, and there is only one type of receptor in the retina that can "see" blue light.
Don't worry if you notice that your baby's eyes are looking in different directions. One eye may sometimes be slightly averted to one side or the other. This is fine. But if the baby's eyes squint to the side, consult an optometrist immediately.
Tips: Paint your baby's room in bright, cheerful colors to stimulate his eyesight. Furniture or interior details should be of contrasting colors and shapes. Hang a bright, colorful hanging piece above or next to your crib. It is important that it be multi-colored and consist of different geometric shapes.
Furniture or interior details should be of contrasting colors and shapes. Hang a bright, colorful hanging piece above or next to your crib. It is important that it be multi-colored and consist of different geometric shapes.
Development of the organs of vision: 2nd and 3rd month of life
Significant changes occur in the baby's visual system during the second and third months of life. During this period, visual acuity increases , functional strabismus (if it was) disappears. Now your child is able to follow moving objects and tries to fix his eyes on them.
A bright, bright room with lots of colors and shapes to help stimulate your baby's vision development.
Moreover, the baby learns to look from one object to another only with his eyes, without moving his head. Also, the child's eyes become more sensitive to light: at the age of 3 months, the threshold of sensitivity to light decreases. Therefore, during sleep, the light should be dimmed.
Tips: To stimulate the eyesight of a 2-3 month old baby:
-
Add new objects to the room or change their position frequently to enrich the baby's experience.

-
Leave a night light on to stimulate vision when your baby is awake in the crib.
-
Place the baby on its back during sleep to reduce the risk of sudden infant death syndrome (SIDS). However, when the baby is awake and under supervision, put it on the tummy. This posture stimulates the development of visual perception and motor skills.
Development of the organs of vision: Months 4-6
By 6 months, the visual centers of the baby's brain are quite well developed. The child sees more clearly and can follow moving objects with quick and precise eye movements.
Visual acuity improves from about 20/400 (6/120) at birth to 20/25 (6/7.5) at 6 months. Color perception reaches the level of an adult; the child can distinguish all the colors of the rainbow.
At the age of 4-6 months, the child's hand-eye coordination becomes more perfect, which allows him to quickly find and pick up objects with his hands, as well as accurately guide the bottle (and more!) into his mouth.
Six months is an important milestone in life, as this is when you should have your baby's first eye exam.
If necessary, a qualified eye specialist will examine a child at 6 months of age. But routine eye exams are usually recommended after kindergarten age (3-4 years and older).
If you have any concerns, you can also consult your doctor for further advice.
For a thorough examination of your six-month-old baby's eyes, see an optometrist who specializes in children's vision and eye development.
Eye Development: Months 7-12
Your baby is now moving around a lot, crawling and covering distances you never dreamed possible. He is getting better at estimating the distance to objects, more precisely grabbing and throwing them. (Beware!)
This is an important period in your child's development. At this stage, the baby feels his whole body better and learns to coordinate vision and movement.
Now you have to pay more attention to the baby to keep him out of harm's way. It is not uncommon for bumps, bruises, eye injuries and other serious injuries when the baby explores the world around him.
It is not uncommon for bumps, bruises, eye injuries and other serious injuries when the baby explores the world around him.
Close cabinets with household chemicals with a padlock, place special railings in front of stairs.
Don't worry if your child's eyes start to change color. Most babies are born with blue eyes because at birth there are not enough dark pigments in the iris. Over time, there will be many more of them, so your baby's eyes may change color from blue to brown, green, gray or swampy.
Tips: To stimulate your child's hand-eye coordination, you can lie on the floor with him and invite him to crawl to an object. Put your baby's favorite toy away and invite him to get to it. You can also offer to disassemble and assemble various objects and toys.
Strabismus problems
Pay close attention to how your child's eyes move, either together or separately. Strabismus is a term for a misalignment of the eyes. It is very important to detect and treat it at an early stage so that the child's vision develops properly.
It is very important to detect and treat it at an early stage so that the child's vision develops properly.
Left untreated, strabismus can lead to amblyopia or "lazy eye."
It may take months for a child to achieve joint eye movement. But if you notice that one of the baby's eyes is squinting or moving separately from the other, contact an optometrist immediately.
Vision problems in premature babies
The average duration of a normal pregnancy is approximately 40 weeks (280 days). According to the WHO, a baby born before 37 weeks is considered premature.
Compared to full-term babies, premature babies are at greater risk of developing eye problems. And the shorter the period, the more serious the complication.
The following visual problems associated with preterm birth are characteristic:
Retinopathy of prematurity (RP)
This is a disease in which fibrous changes and blood vessels develop in the thickness and on the surface of the retina. ROP is often accompanied by retinal scarring, poor vision and retinal detachment . In severe cases, retinopathy of prematurity can lead to blindness.
ROP is often accompanied by retinal scarring, poor vision and retinal detachment . In severe cases, retinopathy of prematurity can lead to blindness.
All premature babies are at risk of ROP. Extremely low birth weight is an additional risk factor, especially when the baby is placed in a high oxygen incubator immediately after birth.
If your baby was born prematurely, ask your obstetrician for a referral to a pediatric ophthalmologist for an eye exam to rule out ROP.
Nystagmus
These are involuntary oscillatory eye movements.
In most cases, nystagmus manifests itself in the form of involuntary eye movements in various directions, with different frequencies and amplitudes of "oscillation". Eye oscillations are pendulum in nature, horizontal, diagonal and rotational movements are observed.
Nystagmus may be congenital or may develop over several weeks or months. Risk factors include optic nerve hypoplasia, albinism, and congenital cataracts. By the amplitude of eye oscillations, you can determine how badly the baby's visual system is damaged.
By the amplitude of eye oscillations, you can determine how badly the baby's visual system is damaged.
If the child shows signs of nystagmus, consult an optometrist immediately.
Remember that smoking during pregnancy greatly increases the chance of preterm labor.
Page published on Monday, November 16, 2020
Page updated on Monday, April 19, 2021
norm and pathology - Articles
Vision is the most informative and at the same time the most fragile external analyzer. It is with the help of the eyes that a person receives most of the information about the world around him. The visual centers are connected and have a strong influence on almost all vital structures of the brain (vision is involved in the digestive, motor, vestibular, sexual and other activities of the body). Especially important in the formation and development of vision is the first year of life, when the eyes and the child's body as a whole are easily susceptible to various harmful effects of both internal and external factors.
If at this age the visual organ is damaged, then the child develops movement coordination disorders, the baby experiences fear of the outside world, which often leads to a significant lag in the development of the child, since the rest of the senses are not able to fully compensate for the lack of information.
In the first year, the child's vision develops very intensively. The almost complete blindness of a newborn baby (non-directional light perception) in a few months develops into the ability to analyze objects and their movement, evaluate and compare objects according to their various characteristics, including color. Therefore, it is especially important for parents to understand the basic principles of vision development in children of the first year of life and to be aware of the early signs of the onset of eye pathology.
Development of the visual system
There are several periods in the development of the organ of vision. The most important of them is the laying and intrauterine formation. At this stage, the action of damaging factors can lead to catastrophic consequences (developmental anomalies - hypoplasia of the optic nerves, congenital cataract, glaucoma; inflammation of the membranes of the eye; etc.). The next period is from birth to 1 year. At this time, areas of the visual cortex of the brain are actively developing, receiving information about the world around them. The simultaneous movement of the eyes is trained, the visual control of the movement of the hands is formed, the "library" of visual images is filled. If at this stage there is a restriction in the flow of light to the retina (violation of the transparency of the optical media of the eye), a violation of the focus of objects (the presence of myopia or a high degree of hyperopia) or a deterioration in the perception of visual images (damage to the optic nerves, visual centers of the brain), then vision may stop at the initial stage of development and not form to a normal level.
At this stage, the action of damaging factors can lead to catastrophic consequences (developmental anomalies - hypoplasia of the optic nerves, congenital cataract, glaucoma; inflammation of the membranes of the eye; etc.). The next period is from birth to 1 year. At this time, areas of the visual cortex of the brain are actively developing, receiving information about the world around them. The simultaneous movement of the eyes is trained, the visual control of the movement of the hands is formed, the "library" of visual images is filled. If at this stage there is a restriction in the flow of light to the retina (violation of the transparency of the optical media of the eye), a violation of the focus of objects (the presence of myopia or a high degree of hyperopia) or a deterioration in the perception of visual images (damage to the optic nerves, visual centers of the brain), then vision may stop at the initial stage of development and not form to a normal level.
Immediately after birth, the child is only able to perceive the presence or absence of a light source. In the first months of life, various objects of the surrounding world appear in front of the child, as if from a fog. At first, the baby only fixes his gaze on large objects (the first month), then he tries to trace their movement in space - he studies the parents passing by, follows the moving toys (3-4 months). At this age, you should not hang toys directly in front of your eyes - place them on the sides of the child or on your feet. At 6 months, the child's visual acuity allows him to observe small objects, visually recognize "their own", grab and throw toys, while learning the three-dimensionality of space. Place rattles and "rattles" in the area of the movement of the child's hands to facilitate their capture.
In the first months of life, various objects of the surrounding world appear in front of the child, as if from a fog. At first, the baby only fixes his gaze on large objects (the first month), then he tries to trace their movement in space - he studies the parents passing by, follows the moving toys (3-4 months). At this age, you should not hang toys directly in front of your eyes - place them on the sides of the child or on your feet. At 6 months, the child's visual acuity allows him to observe small objects, visually recognize "their own", grab and throw toys, while learning the three-dimensionality of space. Place rattles and "rattles" in the area of the movement of the child's hands to facilitate their capture.
A one-year-old baby is already collecting “little rubbish” on the floor, actively moving towards a bright toy. Use distant objects to attract attention. Receiving powerful visual stimuli, the baby begins to strive for the objects of interest to him, makes attempts to stand up and takes his first steps. Only by the age of 6-7 years does the child's vision reach the level of an adult (according to special tables, he names the 10th line).
Only by the age of 6-7 years does the child's vision reach the level of an adult (according to special tables, he names the 10th line).
Parental control
Even in the maternity hospital, a visual examination of a newborn can reveal signs of some congenital eye diseases. A cataract is a clouding of the lens that appears as a grayish glow instead of a black pupil. The most common treatment is surgical removal of the cloudy lens. The prolonged existence of interference with the passage of light into the eye will lead to a significant delay in the development of vision (obscurative ambiopia). After such an operation, the child wears special glasses or a contact lens that replaces the lens. Recently, the technique of early implantation of an artificial lens has been widespread. Some types of translucent cataracts are not operated on in early childhood. In such cases, periodic courses of stimulating treatment are carried out (exposure to the eye with light and laser radiation, electric and magnetic fields, classes on special computer programs) and delayed surgical intervention is performed at an older age.
External manifestations similar to cataracts can be detected in a more dangerous disease - retinoblastoma (retinal tumor). In the early stages, the tumor can be affected with the help of special radiation applicators - plates with a radioactive substance applied to them. They are sutured directly to the sclera at the site of the projection of the tumor, the shadow of which is determined during the operation, transilluminating the sclera with a diaphanoscope (a device similar to a flashlight). The radioactive material of the applicator destroys the tumor through the sclera. In the later stages, when there is a danger of the tumor spreading outside the eye, there is only one way - removal of the affected eye.
Congenital glaucoma is an eye disease characterized by an increase in intraocular pressure due to congenital disorders in the formation and outflow of intraocular fluid. As a result, the child's eye stretches and increases in size, moving forward (up to limiting the complete closure of the eyelids). Also, with glaucoma, there may be clouding of the cornea (leukoma). Since this disease is associated with structural changes in some parts of the eye, the treatment is mainly surgical. The purpose of the operation is to ensure the normal outflow of intraocular fluid from the eye cavity. If by the time of the operation the cornea and optic nerve are not affected, then it is possible to preserve and develop full vision.
Also, with glaucoma, there may be clouding of the cornea (leukoma). Since this disease is associated with structural changes in some parts of the eye, the treatment is mainly surgical. The purpose of the operation is to ensure the normal outflow of intraocular fluid from the eye cavity. If by the time of the operation the cornea and optic nerve are not affected, then it is possible to preserve and develop full vision.
Inflammatory diseases (conjunctivitis - inflammation of the outer shell of the eyes, covering the back surface of the eyelids and the anterior surface of the eyeball to the cornea, dacryocystitis - inflammation of the lacrimal sac, uveitis - inflammation of the choroid, etc.). The main signs of this group of eye diseases are redness of the eye, watery eyes, swelling of the eyelids and conjunctiva, and profuse discharge from the eyes. In such cases, only an ophthalmologist should determine the means and methods of treatment, since improper treatment can aggravate inflammation and complicate the process. Unreasonably prescribed antibiotics often lead to allergization of the mucous membrane of the eye, and their long-term use disrupts the vital activity of the normal bacterial flora.
Unreasonably prescribed antibiotics often lead to allergization of the mucous membrane of the eye, and their long-term use disrupts the vital activity of the normal bacterial flora.
In infants during the first months of life, mucous discharge from the eyes, similar to pus, may appear. There is a blockage of the lacrimal system. Often, in order to cope with the banal "festering of the eyes", ordinary hygiene procedures in the form of washing and massaging the area of the lacrimal ducts are enough. First, using a cotton pad moistened with boiled water, remove mucous membranes and crusts from the surface of the eye. Then use your little finger to massage several movements of the inner corner of the eye towards the nose. After that, pour a puddle of boiled water into the inner corner of the eye (the child should lie on his back) and try to make the child blink. When blinking, there is an active washing of the nasolacrimal ducts, which helps to improve the outflow of tear fluid. If necessary, repeat this procedure after each sleep, when the outflow of tears is blocked by tightly squeezing the eyelids.
In case of inflammatory diseases of the eyes, breast milk should not be instilled into them - this is an excellent breeding ground for harmful microorganisms, moreover, the fat contained in milk disrupts the outflow of tears.
The most common external manifestations of eye pathology that can be detected during a non-specialized examination of a newborn include: that is, the eye cannot fixate on an object and therefore sees its details as “blurry”). The cause can be both various eye diseases (high degree of myopia, lesions of the central retina, etc.) and brain damage;
 If such a problem does not interfere with the baby, he is able to view toys at different distances with this eye and he does not have strabismus, the issue of surgical intervention can be postponed to a later date, since surgical assistance in this case will be needed only for cosmetic purposes. To maintain the normal functioning of the eye in this case, it is necessary to conduct special training.
If such a problem does not interfere with the baby, he is able to view toys at different distances with this eye and he does not have strabismus, the issue of surgical intervention can be postponed to a later date, since surgical assistance in this case will be needed only for cosmetic purposes. To maintain the normal functioning of the eye in this case, it is necessary to conduct special training. Parents or an ophthalmologist during a physical examination may detect strabismus in a baby (a change in the correct position of one or both eyes in the palpebral fissure). It occurs due to visual impairment in one or both eyes, a change in the muscle tone of the oculomotor muscles, lesions of the oculomotor nerves, etc. The object in question is focused not on the central part of the retina, but on the neighboring area, where visual sensitivity is significantly lower, which creates a threat to the formation of binocular vision in a baby. Binocular vision - vision with two eyes with a combination of images simultaneously received by them, which allows you to localize objects in direction and in their relative distance. In this case, it is necessary to start treatment as soon as possible. A “curtain” of a gauze napkin is glued onto the non-squinting eye with the help of a patch (in the case of bilateral strabismus, a napkin with a patch is attached alternately on each eye), while the “problem” eye is trained. The only exceptions are cases when visual acuity in both eyes is sharply reduced and gluing can lead to inhibition of vision development in the eye that sees better.
In this case, it is necessary to start treatment as soon as possible. A “curtain” of a gauze napkin is glued onto the non-squinting eye with the help of a patch (in the case of bilateral strabismus, a napkin with a patch is attached alternately on each eye), while the “problem” eye is trained. The only exceptions are cases when visual acuity in both eyes is sharply reduced and gluing can lead to inhibition of vision development in the eye that sees better.
If the angle of deviation of the eye is large enough, surgical correction of strabismus cannot be dispensed with. This in no way cancels the application of patches and stimulating treatment. With the help of these measures, by the time of the operation (most often it is performed at the age of 4–5 years, so that before school there is an opportunity to form binocular vision), it is possible to reduce the angle of strabismus and maintain good visual acuity. And this contributes to a smaller amount of surgical intervention, a better postoperative effect and makes it possible to further normalize visual functions.
Specialized examination by an ophthalmologist
When examining a baby in a maternity hospital (and for premature babies - in the departments of nursing premature babies), an ophthalmologist can identify other eye diseases that do not have external manifestations in the early stages. The most formidable of them today are retinopathy of prematurity and atrophy of the optic nerves.
Retinopathy of prematurity is a disease of the retina, in which the normal development and growth of its vessels stop, and pathological vessels begin to develop that do not fulfill their function of delivering oxygen to the retina. The vitreous body becomes cloudy and thickens, which causes tension and retinal detachment, and if not adequately treated, this can lead to irreversible loss of vision. Unfortunately, outwardly this disease does not manifest itself in any way, and only at the last stage, when it is no longer possible to help the child, the gray glow of the pupil becomes noticeable. The disease in the early stages can only be diagnosed by an experienced ophthalmologist. Mild stages of retinopathy may leave behind minor changes that do not significantly affect vision. But when the 3rd threshold or 4th stage of the disease is reached, the child needs to be operated on urgently.
The disease in the early stages can only be diagnosed by an experienced ophthalmologist. Mild stages of retinopathy may leave behind minor changes that do not significantly affect vision. But when the 3rd threshold or 4th stage of the disease is reached, the child needs to be operated on urgently.
Optic nerve atrophy is a lesion of the nerve fibers that conduct visual signals from the eye to the visual centers of the cerebral cortex. The main reason is various lesions of the structures and the ventricular system of the brain. If the atrophy of the optic nerve is complete (which is rare), then vision may be completely absent. In the case of partial atrophy, visual acuity is determined by the degree and location of damage to the optic nerve. In case of atrophy of the optic nerves, stimulating functional treatment is used with the help of special devices, nootropic (improving metabolic processes in the brain) and vasodilating therapy.
Dynamic monitoring of the child
After the maternity hospital, parents should carefully monitor the development of their baby, paying attention to the formation of visual functions.
It is important that the first examination by an ophthalmologist is carried out in the first 3 months of a baby's life (during this period, most congenital diseases can be diagnosed in the early stages, which is the key to successful treatment). If there is no pathology at the initial examination, the next visit to the doctor is needed when the child is six months old (the maturation of the main structures of the eye responsible for the correct focusing of the image on the retina).
Primary examination is carried out according to the following algorithm:
Determination of sharpness (at 1 month - by the reaction of fixation on the object, at 2-3 months - by tracking a bright toy 15-20 cm in size on a light plain background, at 4-5 months - according to the tracking clarity up to a distance of 3-5 m) and fields of view (field of view - the maximum space inspected by one eye.). Fields of vision are determined approximately - the doctor moves the toy forward from behind the child's head until the baby's reaction to the object appears. At the same time, the appendages of the eye are examined: muscles, lacrimal ducts, eyelids (eye movements in different directions, patency of the lacrimal ducts, the fullness of opening and closing of the eyelids), as well as the optical media of the eye and fundus using an ophthalmoscope and a slit lamp (devices that send a slit-like or a round beam of light through the optical media of the eye).
At the same time, the appendages of the eye are examined: muscles, lacrimal ducts, eyelids (eye movements in different directions, patency of the lacrimal ducts, the fullness of opening and closing of the eyelids), as well as the optical media of the eye and fundus using an ophthalmoscope and a slit lamp (devices that send a slit-like or a round beam of light through the optical media of the eye).
The ophthalmologist also measures refraction using skiascopy (shadow test with optical rulers) or refractometry (a special apparatus is used).
If visual acuity cannot be determined (the baby has a fuzzy fixation or tracking reaction), then a study of brain impulses in response to visual stimuli (visual evoked potential method) is performed. Based on its results, one can judge the presence of functional and structural lesions of the visual analyzer or a delay in its development.
At 6 months, at the examination by an ophthalmologist, in addition to the standard examination of the child, the dynamics of refraction of the eye is monitored, that is, the newly obtained and primary data of this study are compared. In most children at 6 months, refraction fluctuates between +1–+2.5 diopters. Sometimes at this age there may be a shift towards negative refraction, which indicates the baby's predisposition to the development of myopia. In this case, it is necessary to limit visual loads - remove small and close-hanging toys, focus on distant and moving objects. If myopia is detected more than 2 D, especially if, along with this, the child's visual acuity decreases and strabismus appears, vision correction with the help of glasses is prescribed as soon as possible. Glasses, if necessary, can be prescribed as early as 6 months (sometimes, with large degrees or severe asymmetry between the eyes, vision correction is used using contact lenses).
In most children at 6 months, refraction fluctuates between +1–+2.5 diopters. Sometimes at this age there may be a shift towards negative refraction, which indicates the baby's predisposition to the development of myopia. In this case, it is necessary to limit visual loads - remove small and close-hanging toys, focus on distant and moving objects. If myopia is detected more than 2 D, especially if, along with this, the child's visual acuity decreases and strabismus appears, vision correction with the help of glasses is prescribed as soon as possible. Glasses, if necessary, can be prescribed as early as 6 months (sometimes, with large degrees or severe asymmetry between the eyes, vision correction is used using contact lenses).
Even if in 6 months no pathology of the organ of vision was revealed at the preventive examination, in the future it is supposed to be examined by an ophthalmologist every six months, since during this time the refractive indices of the eyes may begin to change (myopia, astigmatism form), some genetic syndromes that occur with a sharp impairment of visual acuity.