Acid reflux nausea pregnancy
Indigestion and heartburn in pregnancy
Indigestion, also called heartburn or acid reflux, is common in pregnancy. It can be caused by hormonal changes and the growing baby pressing against your stomach.
You can help ease indigestion and heartburn by making changes to your diet and lifestyle, and there are medicines that are safe to take in pregnancy.
Symptoms of indigestion and heartburn
Symptoms of indigestion and heartburn include:
- a burning sensation or pain in the chest
- feeling full, heavy or bloated
- burping or belching
- feeling or being sick
- bringing up food
Symptoms usually come on soon after eating or drinking, but there can sometimes be a delay between eating and developing indigestion.
You can get symptoms at any point during your pregnancy, but they are more common from 27 weeks onwards.
Things you can do to help with indigestion and heartburn
Changes to your diet and lifestyle may be enough to control your symptoms, particularly if they are mild.
Eat healthily
You're more likely to get indigestion if you're very full.
If you're pregnant, it may be tempting to eat more than you would normally, but this may not be good for you or your baby.
Find out more about a healthy diet in pregnancy and foods to avoid.
Change your eating and drinking habits
You may be able to control your indigestion with changes to your eating habits.
It can help to eat small meals often, rather than larger meals 3 times a day, and to not eat within 3 hours of going to bed at night.
Cutting down on drinks containing caffeine, and foods that are rich, spicy or fatty, can also ease symptoms.
Keep upright
Sit up straight when you eat. This will take the pressure off your stomach. Propping your head and shoulders up when you go to bed can stop stomach acid coming up while you sleep.
Stop smoking
Smoking when pregnant can cause indigestion, and can seriously affect the health of you and your unborn baby.
When you smoke, the chemicals you inhale can contribute to your indigestion. These chemicals can cause the ring of muscle at the lower end of your gullet to relax, which allows stomach acid to come back up more easily. This is known as acid reflux.
Smoking also increases the risk of:
- your baby being born prematurely (before week 37 of your pregnancy)
- your baby being born with a low birthweight
- sudden infant death syndrome (SIDS), or "cot death"
There's lots of help available to stop smoking.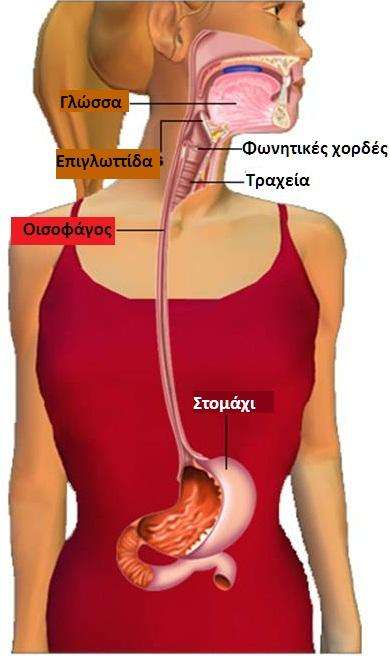 Talk to your midwife or call the NHS Smokefree helpline on 0300 123 1044. Find out more about stopping smoking in pregnancy.
Talk to your midwife or call the NHS Smokefree helpline on 0300 123 1044. Find out more about stopping smoking in pregnancy.
Avoid alcohol
Drinking alcohol can cause indigestion. During pregnancy, it can also lead to long-term harm to the baby. It's safest to not drink alcohol at all in pregnancy.
Find out more about alcohol and pregnancy
When to get medical help
See your midwife or GP if you need help managing your symptoms or if changes to your diet and lifestyle do not work. They may recommend medicine to ease your symptoms.
You should also see your midwife or GP if you have any of the following:
- difficulty eating or keeping food down
- weight loss
- stomach pains
Your midwife or GP may ask about your symptoms and examine you by pressing gently on different areas of your chest and stomach to see whether it's painful.
If you're taking prescription medicines
Speak to your GP if you're taking medicine for another condition, such as antidepressants, and you think it may be making your indigestion worse. They may be able to prescribe an alternative medicine.
Never stop taking a prescribed medicine unless you're advised to do so by your GP or another qualified healthcare professional who's responsible for your care.
Medicines for indigestion and heartburn
Medicines for indigestion and heartburn during pregnancy include:
- antacids – to neutralise the acid in your stomach (some are available over the counter from a pharmacist)
- alginates – to relieve indigestion caused by acid reflux by stopping the acid in your stomach coming back up your gullet
You may only need to take antacids and alginates when you start getting symptoms. However, your GP may recommend taking them before symptoms come on – for example, before a meal or before bed.
However, your GP may recommend taking them before symptoms come on – for example, before a meal or before bed.
If you're taking iron supplements as well as antacids, do not take them at the same time. Antacids can stop iron from being absorbed by your body.
If antacids and alginates do not improve your symptoms, your GP may prescribe a medicine to reduce the amount of acid in your stomach. 2 that are widely used in pregnancy and not known to be harmful to an unborn baby are:
- ranitidine – a tablet you take twice a day
- omeprazole – a tablet you take once a day
Causes of indigestion in pregnancy
Symptoms of indigestion come when the acid in your stomach irritates your stomach lining or your gullet. This causes pain and a burning feeling.
When you're pregnant, you're more likely to have indigestion because of:
- hormonal changes
- the growing baby pressing on your stomach
- the muscles between your stomach and gullet relaxing, allowing stomach acid to come back up
You may be more likely to get indigestion in pregnancy if:
- you had indigestion before you were pregnant
- you've been pregnant before
- you're in the later stages of pregnancy
Video: Eating well on a budget
In this video, a dietitian gives advice on how to eat healthily on a budget.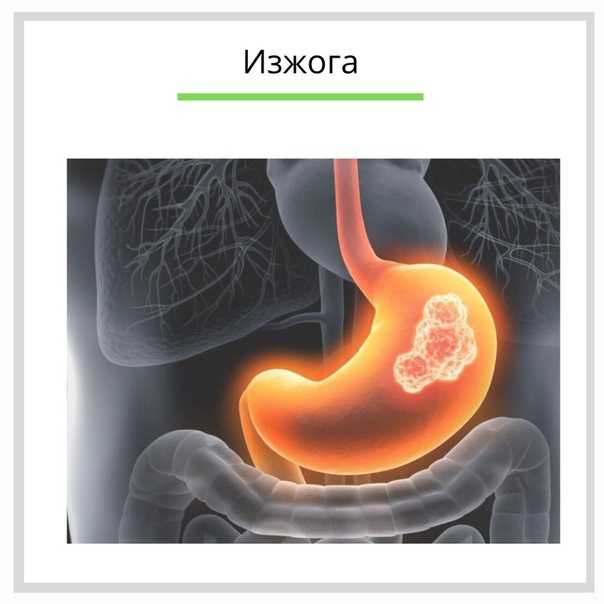
Media last reviewed: 13 January 2021
Media review due: 13 January 2024
Indigestion and Acid Reflux in Pregnancy (Dyspepsia)
In this series Common Side Effects of Pregnancy (Morning Sickness, Acid Reflux, Constipation) Nausea and Vomiting in Pregnancy (Morning Sickness)
Indigestion (dyspepsia) occurs at some point in around half of all pregnant women. It is usually due to acid reflux from the stomach into the gullet (oesophagus).
Indigestion in pregnancy is commonly due to acid reflux. Acid reflux occurs when acid from the stomach leaks up into the gullet (oesophagus). This may cause heartburn - usually felt as a burning pain which rises from the upper stomach behind the breastbone - and other symptoms. Attention to diet and lifestyle may help to ease symptoms. Antacids are commonly used. A medicine which prevents your stomach from making acid may be prescribed if symptoms remain troublesome.
What is indigestion?
Indiestion (dyspepsia) is a term which includes a group of symptoms (detailed below) that come from a problem in your upper gut. The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the gullet (oesophagus), stomach and the first part of the small intestine (duodenum). Various conditions cause dyspepsia.
The gut (gastrointestinal tract) is the tube that starts at the mouth and ends at the anus. The upper gut includes the gullet (oesophagus), stomach and the first part of the small intestine (duodenum). Various conditions cause dyspepsia.
Indigestion is really common in pregnancy - it occurs at some point in around half of all pregnant women. Indigestion in pregnancy is usually due to reflux of acid from the stomach into the oesophagus.
Understanding the oesophagus and stomach
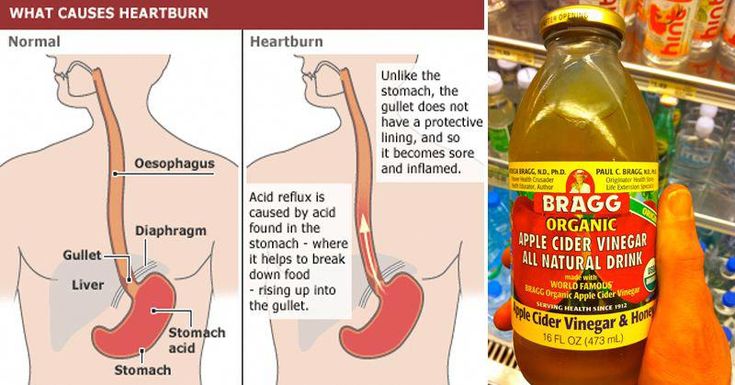
Acid reflux inflammation
When we eat, food passes down the gullet (oesophagus) into the stomach. Cells in the lining of the stomach make acid and other chemicals which help to digest food.
Stomach cells also make mucus which protects them from damage caused by the acid. The cells lining the oesophagus are different and have little protection from acid.
There is a circular band of muscle (a sphincter) at the junction between the oesophagus and stomach. This relaxes to allow food down but normally tightens up and stops food and acid leaking back up (refluxing) into the oesophagus.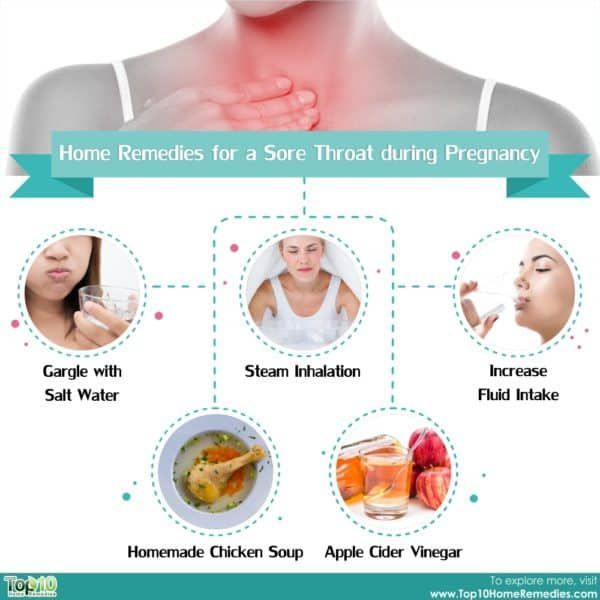 In effect, the sphincter acts like a valve.
In effect, the sphincter acts like a valve.
What causes acid reflux during pregnancy?
Acid reflux occurs when some acid leaks up (refluxes) into the gullet (oesophagus). The lining of the oesophagus can cope with a certain amount of acid. However, if more than the usual amount of acid refluxes, it may cause some inflammation on the lining of the oesophagus, which can cause symptoms.
The sphincter at the bottom of the oesophagus normally prevents acid reflux. It is thought that when you are pregnant:
- The increased level of certain hormones that occurs has a relaxing effect on the sphincter muscle. That is, the tightness (tone) of the sphincter is reduced during pregnancy.
- The size of the baby in the tummy (abdomen) causes an increased pressure on the stomach.
One or both of the above increase the chance that acid will reflux into the oesophagus. The indigestion usually settles on its own after the birth of your baby when your hormones change back to their non-pregnant state and the baby is no longer increasing pressure on your stomach.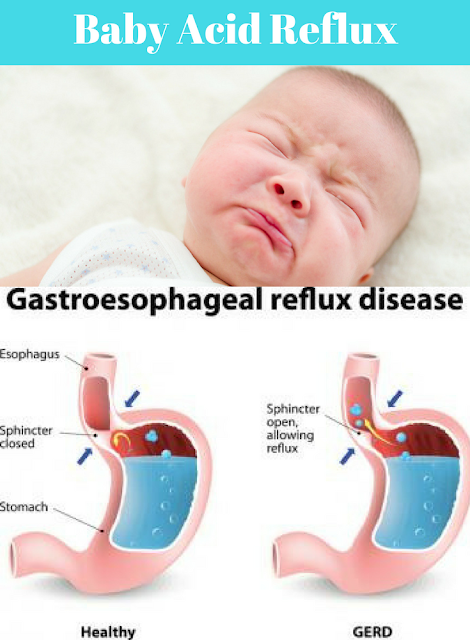
You are more likely to develop indigestion in pregnancy if you have previously had gastro-oesophageal reflux before you were pregnant.
What are the symptoms of acid reflux and indigestion in pregnancy?
Symptoms can vary from mild (in most cases) to severe. They can include one or more of the following:
- Heartburn. This is a burning sensation which rises from the upper tummy (abdomen) or lower chest up towards the neck. (It is a confusing term as it has nothing to do with the heart!)
- Waterbrash. This is a sudden flow of sour-tasting saliva in your mouth.
- Upper abdominal pain or discomfort.
- Pain in the centre of the chest behind the breastbone (sternum).
- Feeling sick (nausea) and being sick (vomiting).
- Bloating.
- Quickly feeling full after eating.
Symptoms tend to occur in bouts which come and go, rather than being present all the time. They may begin at any time during pregnancy but happen more often, or are more severe, in the last three months of pregnancy. As soon as the baby is born, indigestion due to pregnancy usually disappears quickly.
As soon as the baby is born, indigestion due to pregnancy usually disappears quickly.
Note: various other problems, associated with pregnancy and unrelated to pregnancy, are sometimes confused with indigestion. For example, pain in the right or left of the upper abdomen is not usually due to indigestion. Excessive vomiting is not usually due to indigestion. If symptoms change, or are not typical, or become severe, or are repeated (recurring), you should see your doctor.
Do I need any investigations?
Indigestion in pregnancy is usually recognised by your typical symptoms. Investigations are generally not needed.
Lifestyle changes that may help with indigestion symptoms
The following are commonly advised. There has been little research to prove how well these lifestyle changes help to ease acid leaking back up (reflux) and indigestion in pregnancy. However, they are certainly worth a try.
Consider avoiding certain foods, drinks and large meals
Some foods and drinks may make reflux worse in some people. (It is thought that some foods may relax the sphincter and allow more acid to reflux.) It is difficult to be certain to what extent specific foods contribute to the problem.
(It is thought that some foods may relax the sphincter and allow more acid to reflux.) It is difficult to be certain to what extent specific foods contribute to the problem.
Let common sense be your guide. If it seems that a food is causing symptoms, try avoiding it for a while to see if symptoms improve. Foods and drinks that have been suspected of making symptoms worse in some people include:
- Peppermint.
- Tomatoes.
- Chocolate.
- Spicy and fatty foods.
- Fruit juices.
- Hot drinks.
- Coffee.
- Alcoholic drinks. (Current advice is that you avoid all alcohol in pregnancy anyway.)
Also, avoid large meals if they bring on symptoms. Some women find that eating smaller meals more frequently is helpful.
Stop smoking if you are a smoker
The chemicals from cigarettes relax the sphincter muscle and make acid reflux more likely. Symptoms may ease if you are a smoker and stop smoking. In any case, it is strongly advised that pregnant women should not smoke for other reasons as well.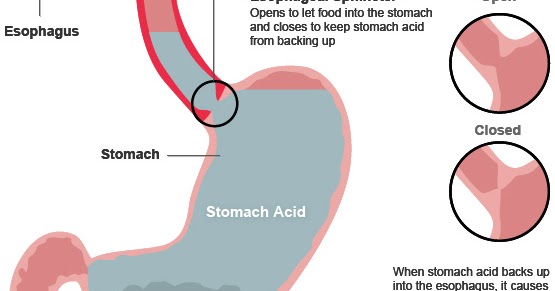 See the separate leaflet called Pregnancy and Smoking.
See the separate leaflet called Pregnancy and Smoking.
Have good posture
Lying down or bending forwards a lot during the day encourages reflux. Sitting hunched-over may put extra pressure on the stomach, which may make any reflux worse.
Bedtime
If symptoms return on most nights, it may help to go to bed with an empty, dry stomach. To do this, don't eat in the last three hours before bedtime and don't drink in the last two hours before bedtime. If you raise the head of the bed by 10-15 cm (with sturdy blocks or bricks under the bed's legs), this will help gravity to keep acid from refluxing into the gullet (oesophagus).
Consider any medicines that you are taking
Some medicines may make symptoms worse. Women are rarely prescribed these medicines during pregnancy. However, it's worth checking with your pharmacist or your doctor if you think medication you are on could be making your symptoms worse.
Is there any medication for indigestion in pregnancy?
For many women (especially if they have mild symptoms), making some lifestyle changes as above is enough to ease indigestion. However, if lifestyle changes do not help, medication may be needed to treat indigestion in pregnancy.
However, if lifestyle changes do not help, medication may be needed to treat indigestion in pregnancy.
Antacids and alginates
Antacids are alkaline liquids or tablets that neutralise the acid. A dose usually gives rapid relief. You can use antacids when you need them for mild or infrequent bouts of indigestion. Antacids containing aluminium or magnesium can be taken on an 'as required' basis. Those containing calcium should only be used occasionally or for a short period. Antacids that contain sodium bicarbonate or magnesium trisilicate should be avoided: this is because they may be harmful to your developing baby.
You can buy many different brands of antacids, and some are available on prescription. A doctor or pharmacist can advise. Some points about antacids are:
- They can interfere with the absorption of iron tablets. Therefore, they should be taken at a different time of day from any iron supplements you are taking. If possible, you should take your antacid at least two hours before or after you take your iron supplement.

- It is probably best to use an antacid with a low sodium content if you have high blood pressure or pre-eclampsia (a complication of pregnancy).
Alginates are often combined with antacids. Alginates help to protect the gullet (oesophagus) from stomach acid. They form a protective raft when they come into contact with stomach acid, blocking the acid from entering the oesophagus. Some alginates are specifically licensed for use in pregnancy. Again, your pharmacist can advise.
Acid-suppressing medicines
Omeprazole is an acid-suppressing medicine that is licensed for use in pregnancy to treat indigestion that is still troublesome despite any lifestyle changes and antacids. Omeprazole needs to be taken regularly to be effective.
Ranitidine is another medicine that can be used instead of omeprazole. This medicine works by reducing the amount of acid that the stomach makes. It usually eases the symptoms of indigestion quite well. Note: ranitidine is not licensed for use in pregnancy by the manufacturers. However, it has been used in pregnancy for many years with no reports of harm to the developing baby. It is generally considered safe to take. Ranitidine also needs to be taken regularly (and not just when you have indigestion symptoms) to be effective.
However, it has been used in pregnancy for many years with no reports of harm to the developing baby. It is generally considered safe to take. Ranitidine also needs to be taken regularly (and not just when you have indigestion symptoms) to be effective.
Note: only ranitidine and omeprazole, along with the antacids above, may be used if you are pregnant. Other medicines that are commonly used for heartburn, indigestion, acid reflux, etc, should not be used. For example, cimetidine, esomeprazole, lansoprazole and pantoprazole. It is not known whether these other medicines are safe to take during pregnancy.
90,000 GERD during pregnancy. What is GERD during pregnancy? IMPORTANT
The information in this section should not be used for self-diagnosis or self-treatment. In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor.
GERD during pregnancy is an acid-dependent disease of the esophagus caused by damage to the mucosa during the reflux of stomach contents, which has arisen or worsened under the influence of gestational factors. Manifested by heartburn, sour eructation, odynophagia, less often - nausea, vomiting, dysphagia, epigastric pain, cough, dysphonia, hypersalivation in sleep, taste perversions, depressed mood. It is diagnosed using alkaline and omeprazole tests, esophagoscopy, pH-metry, manometry. For treatment, alginates, antacids, selective histamine blockers, drugs that inhibit the proton pump, prokinetics are used. nine0006
ICD-10
K21 Gastroesophageal reflux
- Causes
- Pathogenesis
- Classification
- Symptoms of GERD during pregnancy
- Complications
- Diagnostics
- Treatment of GERD during pregnancy
- Prognosis and prevention
- Prices for treatment
General
GERD (gastroesophageal reflux disease, gastroesophageal reflux) is one of the most common diseases of the gastrointestinal tract, contributing to such a common symptom as pregnancy heartburn. According to the observations of specialists in the field of obstetrics and gynecology, from 30 to 95% of patients during the period of bearing a child experience heartburn, which some experts even consider a natural manifestation of pregnancy. In 21-80% of patients suffering from GERD, the disease debuted precisely in connection with gestation.
According to the observations of specialists in the field of obstetrics and gynecology, from 30 to 95% of patients during the period of bearing a child experience heartburn, which some experts even consider a natural manifestation of pregnancy. In 21-80% of patients suffering from GERD, the disease debuted precisely in connection with gestation.
Women who have given birth multiple times are more susceptible to the disease. The relevance of timely detection of gastroesophageal reflux is due to a significant deterioration in the quality of life of a pregnant woman and the need to prescribe pharmacotherapy to almost half of the patients.
GERD during pregnancy
Causes
Gastroesophageal reflux of acidic gastric contents develops with a weakening of the cardiac sphincter, impaired motility of the esophagus and stomach, increased gastric secretion, and a decrease in the protective properties of the esophageal mucosa. The occurrence of GERD is promoted by congenital and acquired hernia of the esophageal opening of the diaphragm with displacement into the posterior mediastinum of the abdominal esophagus, part or all of the stomach, smoking, dietary errors, and obesity. nine0006
The occurrence of GERD is promoted by congenital and acquired hernia of the esophageal opening of the diaphragm with displacement into the posterior mediastinum of the abdominal esophagus, part or all of the stomach, smoking, dietary errors, and obesity. nine0006
A certain role is played by the intake of nitrates, antidepressants, progestins, anticholinergics, calcium channel blockers and other drugs that cause transient relaxation of the esophageal sphincter. Specialists in the field of modern gastroenterology consider pregnancy as a separate prerequisite for the development of gastroesophageal reflux disease. The high incidence of GERD during gestation is associated with the action of factors such as:
- Increased progesterone levels. Under the action of progestins, the lower esophageal sphincter relaxes, the tone of which is restored only in the postpartum period. By reducing the tone of smooth muscle fibers and reducing the sensitivity of intestinal receptors to histamine and serotonin, physiological hyperprogesteronemia slows down gastrointestinal motility and impairs gastric emptying.
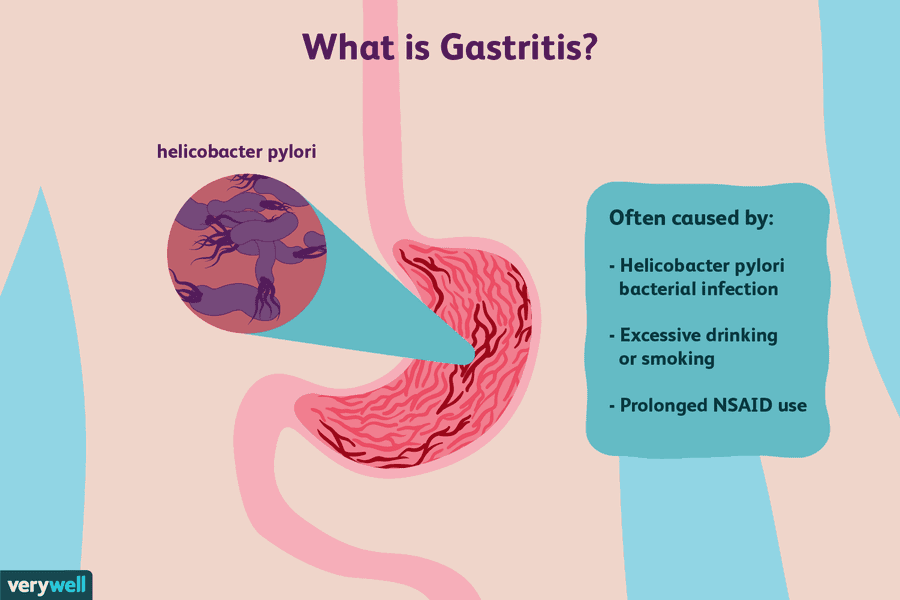 As a result, reflux occurs more frequently.
As a result, reflux occurs more frequently. - Increased intra-abdominal pressure. During pregnancy, the relative position of the internal organs of the abdominal cavity is disturbed, which is associated with the development of the fetus and the growth of the uterus. When the stomach is displaced towards the diaphragm, evacuation stagnation of its contents is formed faster and the risk of diaphragmatic hernia formation increases. The factor of increasing intra-abdominal pressure is most significant in carrying multiple pregnancies and large fetuses. nine0016
Pathogenesis
The mechanism of development of GERD during pregnancy is based on the reflux of aggressive stomach contents into the lower esophagus. Gastroesophageal reflux usually occurs when the pressure of the cardiac sphincter is less than 2 mm Hg. Art. or an increase in intragastric pressure of more than 5 mm Hg. Art. Both of these factors are found in pregnant women. Refluxate containing hydrochloric acid, pepsin, and in some cases bile acids, has an irritating effect on the epithelium of the esophagus, causes a local inflammatory reaction, and in some patients provokes the onset of erosive processes.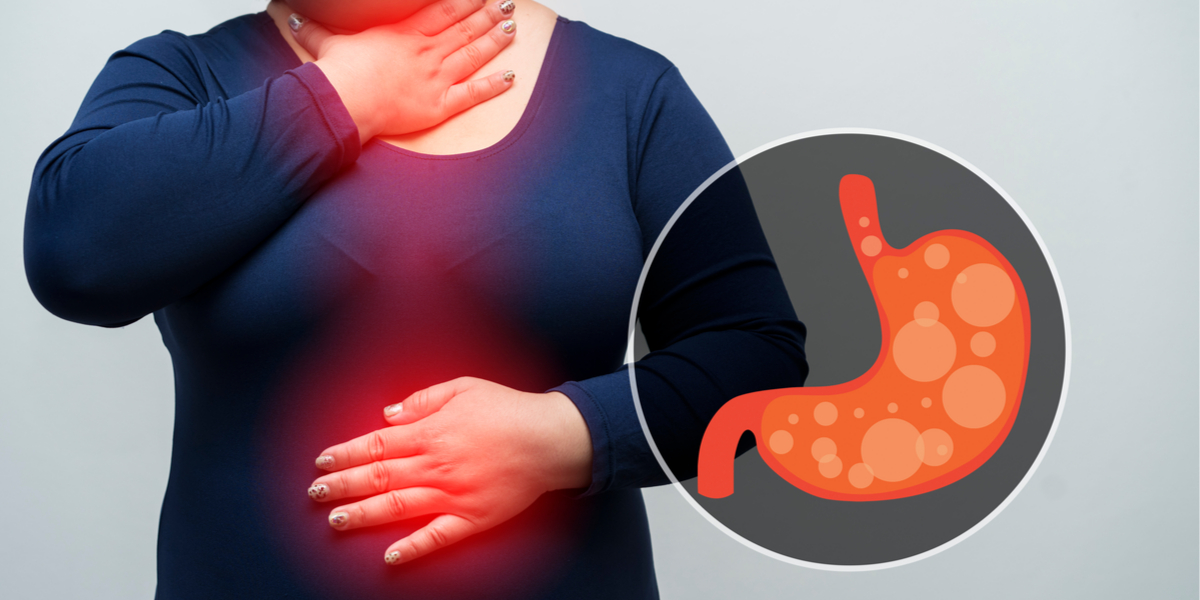 nine0006
nine0006
Classification
When systematizing the forms of GERD in pregnant women, the same criteria are taken into account as outside the gestational period - the nature of the course of the disease and the condition of the esophageal mucosa. This approach makes it possible to develop optimal medical tactics aimed at eliminating clinical symptoms and the morphological basis of their occurrence without the risk of negative effects on the fetus. Depending on the time of existence of the disorder, acute gastroesophageal reflux disease is distinguished, lasting up to 3 months, and a chronic process that exists for 3 months or more. Taking into account the characteristics of damage to the esophageal mucosa, such forms of GERD are distinguished as: nine0006
- Gastroesophageal reflux without esophagitis. With a non-erosive variant of the disorder, detected in 55-70% of patients, there are no endoscopic signs of damage to the epithelium. Although the likelihood of complications in this case is lower, the patient's quality of life deteriorates in the same way as in the presence of erosions.
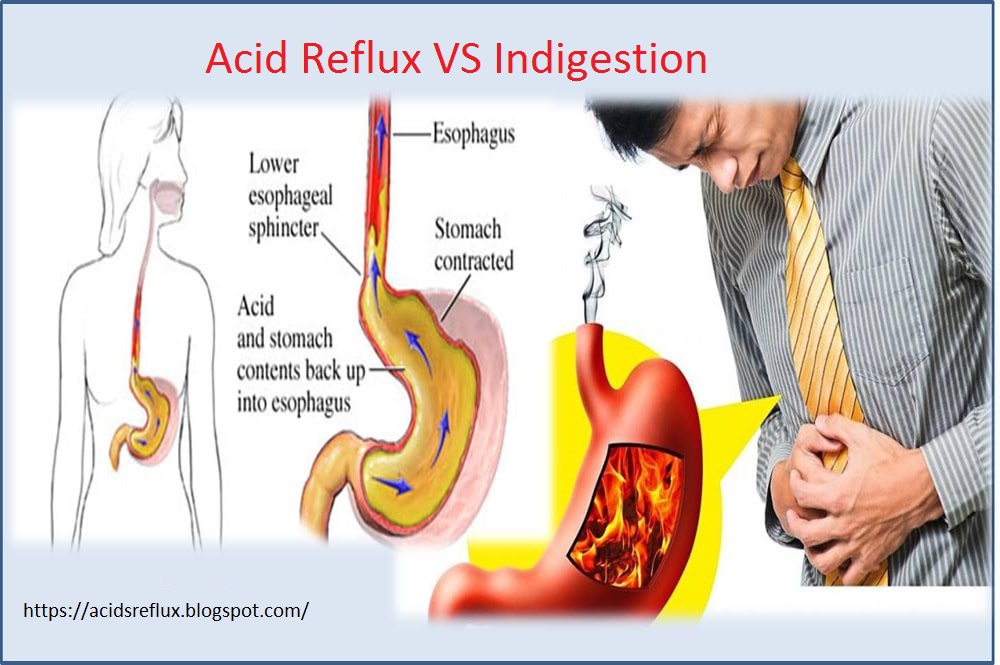
- Reflux esophagitis. In 30-45% of pregnant women with GERD during endoscopy, visible signs of esophagitis caused by the aggressive action of the contents of the stomach are determined. In the erosive form of gastroesophageal reflux, acute and long-term consequences of the disease are more often observed. nine0016
When predicting the outcome of GERD in a pregnant woman, the severity of the endoscopically positive variant of the disease according to the Los Angeles classification is also taken into account. The most favorable during pregnancy is reflux esophagitis A and B degrees, in which the defects extend to 1-2 folds of the mucosa, and their sizes, respectively, are up to or more than 5 mm. With C degree of GERD, less than 75% of the esophageal circumference is affected, and with D - 75% or more, which significantly increases the likelihood of a complicated course. nine0006
Symptoms of GERD during pregnancy
75% of patients with gastroesophageal reflux complain of heartburn, which gradually increases as labor approaches. Discomfort and burning behind the sternum often occur after eating spicy, fatty, fried foods, overeating, exercise, lying down and bending over. Heartburn attacks can recur several times a day and last from minutes to several hours. Pregnant women suffering from GERD may experience sour or bitter belching, sensation of a lump in the throat, retrosternal pain when swallowing with irradiation to the precordial region, neck, lower jaw, interscapular space. nine0006
Discomfort and burning behind the sternum often occur after eating spicy, fatty, fried foods, overeating, exercise, lying down and bending over. Heartburn attacks can recur several times a day and last from minutes to several hours. Pregnant women suffering from GERD may experience sour or bitter belching, sensation of a lump in the throat, retrosternal pain when swallowing with irradiation to the precordial region, neck, lower jaw, interscapular space. nine0006
Sometimes in the II-III trimesters, nausea and vomiting are noted, it is extremely rare that swallowing solid and then liquid food is difficult. Extra-esophageal manifestations of reflux disease during pregnancy are a feeling of fullness in the epigastrium, rapid satiety, repeated attacks of coughing and suffocation, a hoarse voice, sore throat, increased salivation during sleep, burning cheeks and tongue, taste perversion, bad breath. Often, pregnant women experience a sad, depressed mood. Rarely, GERD is asymptomatic.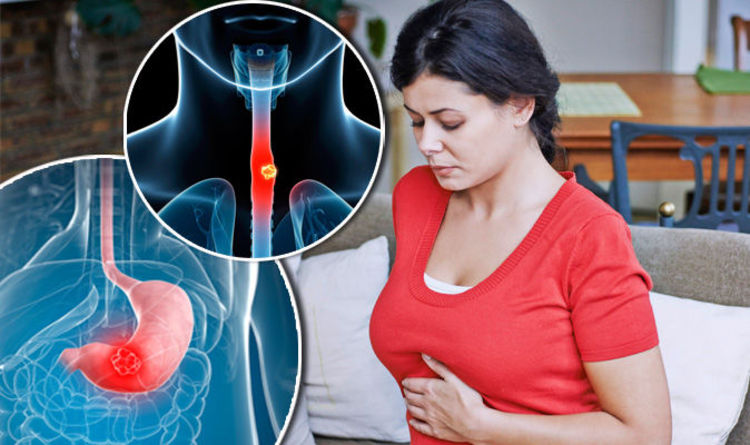 nine0006
nine0006
Complications
Usually, gastroesophageal reflux does not contribute to the occurrence of any obstetric complications, however, with extensive erosive damage to the esophagus, a more pronounced anemia of pregnant women may develop. In two thirds of patients, GERD worsens during pregnancy: in 10-11% of cases, a relapse occurs in the 1st trimester, aggravated by early toxicosis, in 33-34% - in the 2nd trimester, and in more than half of pregnant women - in the 3rd.
Rare specific complications that occur against the background of physiological immunodeficiency during pregnancy are acute esophagitis caused by candidal and herpes infections. There is a risk of ulceration of the mucosa with the development of esophageal bleeding. Long-term consequences of reflux disease are narrowing (strictures) of the esophagus, dysplasia and metaplasia of the epithelium (Barrett's esophagus) and esophageal adenocarcinoma. nine0006
Diagnostics
In pregnancy, the diagnosis of GERD is usually made on the basis of typical clinical symptoms with daily occurrence of heartburn. An obstetrician-gynecologist and a gastroenterologist are involved in the diagnosis. Instrumental methods traditionally used in the diagnosis of the disease are used to a limited extent in pregnant women due to the possible provocation of preterm labor and the aggravation of other complications (nephropathy, early toxicosis, preeclampsia, eclampsia). Recommended for diagnostic purposes: nine0006
An obstetrician-gynecologist and a gastroenterologist are involved in the diagnosis. Instrumental methods traditionally used in the diagnosis of the disease are used to a limited extent in pregnant women due to the possible provocation of preterm labor and the aggravation of other complications (nephropathy, early toxicosis, preeclampsia, eclampsia). Recommended for diagnostic purposes: nine0006
- Alkaline test. Reception of absorbable antacids quickly stops an attack of heartburn. The positive effect of alkaline preparations is associated with the neutralization of hydrochloric acid coming from the stomach into the esophagus. In the presence of extraesophageal manifestations, the study is supplemented with an omeprazole test aimed at eliminating symptoms by inhibiting gastric secretion.
- Endoscopy of the esophagus. Esophagoscopy is performed if extensive erosion, ulceration, esophageal bleeding, strictures are suspected, and neoplasia can be ruled out. In endoscopic examination, GERD is manifested by swelling and slight vulnerability of the esophageal mucosa, it is possible to identify areas of damaged epithelium.
 In some cases, it is possible to visualize the reflux of gastric juice. nine0016
In some cases, it is possible to visualize the reflux of gastric juice. nine0016 - Intraesophageal pH-metry. The method is effective in non-erosive forms of gastroesophageal reflux. Electrometric determination of the acidity of the contents of the esophagus is carried out using a flexible intraesophageal probe attached to an acidogastrometer. pH-metry allows you to identify episodes of reflux of gastric juice and determine the conditions for their occurrence.
- Manometry. Registration of pressure in different parts of the gastrointestinal tract using special catheters with strain gauges verifies the weakening of the cardiac sphincter and dysmotility. A manometric study also provides an objective assessment of elasticity, tone, contractile activity of the esophageal wall, and pressure profiling in the esophagus. nine0016
If necessary, the examination is supplemented with gastrocardiomonitoring, gastrointestinal impedancemetry, bilemetry. X-ray studies of the esophagus during pregnancy are not performed. GERD is differentiated from functional dyspepsia, gastric and duodenal ulcers, acute infectious esophagitis, benign tumors and esophageal cancer. If extraesophageal symptoms are detected, differential diagnosis with angina pectoris, bronchial asthma may be required.
GERD is differentiated from functional dyspepsia, gastric and duodenal ulcers, acute infectious esophagitis, benign tumors and esophageal cancer. If extraesophageal symptoms are detected, differential diagnosis with angina pectoris, bronchial asthma may be required.
Treatment of GERD during pregnancy
Therapeutic tactics are aimed at the rapid elimination of clinical symptoms, restoration of the esophageal mucosa, prevention of complications and relapses. In 25% of cases, the condition can be improved by non-drug methods. Pregnant women with mild GERD are recommended to stop smoking, correct diet and diet with frequent small meals, reduce the amount of high-protein and low-lipid foods, and exclude citrus juices, chocolate, caffeine-containing drinks, spices, mint, and alcohol. nine0006
Care must be taken when using drugs that transiently reduce the tone of the cardia. Efficient sleep with a raised headboard, chewing chewing gum with calcium carbonate.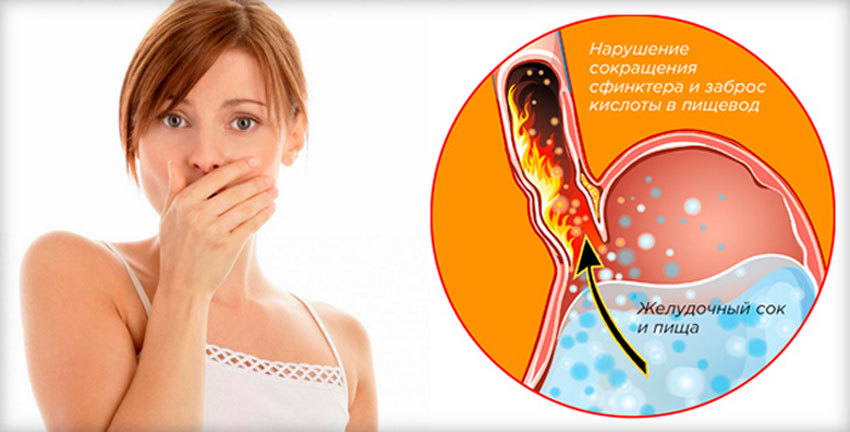 Identification of severe clinical symptoms requires the appointment of special drug therapy. During pregnancy, some of the drugs used in standard treatment regimens for gastroesophageal reflux are used with caution due to possible effects on the fetus or the occurrence of obstetric complications. Patients with severe GERD are shown: nine0006
Identification of severe clinical symptoms requires the appointment of special drug therapy. During pregnancy, some of the drugs used in standard treatment regimens for gastroesophageal reflux are used with caution due to possible effects on the fetus or the occurrence of obstetric complications. Patients with severe GERD are shown: nine0006
- Nonabsorbable antacids and alginates. Considered 1st line drugs for the treatment of gastroesophageal reflux disease in pregnant women. By neutralizing hydrochloric acid, reducing the digestive capacity of pepsin, adsorbing lysolecithin, bile acids, improving the evacuation of stomach contents, stimulating the secretion of prostaglandins, antacids reduce the damaging effect of refluxate. Alginates have a protective effect on the esophageal mucosa.
- Histamine h3 receptor blockers. They are used when antacid therapy for GERD is ineffective. The antisecretory activity of selective histamine blockers is due to the action on the receptors of the parietal cells of the stomach.
 Due to inhibition of secretion, the acidity and volume of gastric contents decrease, which helps to reduce its aggressiveness and pressure on the cardiac sphincter. The effect of h3-histamine blockers on the fetus is not well understood, which limits their use. nine0016
Due to inhibition of secretion, the acidity and volume of gastric contents decrease, which helps to reduce its aggressiveness and pressure on the cardiac sphincter. The effect of h3-histamine blockers on the fetus is not well understood, which limits their use. nine0016 - Proton pump inhibitors. High efficiency and rapid achievement of therapeutic results in the appointment of PPIs are based on blocking the secretion of hydrochloric acid at the level of the secretory tubules of parietal cells. The limited use of pump inhibitors is due to a decrease in the bactericidal properties of gastric juice, which, against the background of natural suppression of immunity, contributes to the development of food infections and impaired calcium absorption, which is necessary for the normal course of gestation. nine0016
As additional means, prokinetics that improve gastrointestinal motility and herbal enveloping preparations can be used. During gestation, surgical treatment of severe and complicated forms of GERD is not performed.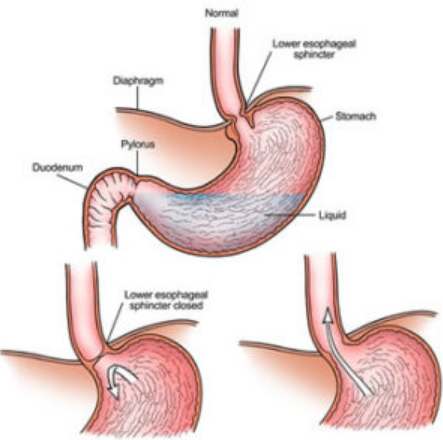 Pregnancy is recommended to be completed by natural childbirth at a physiological time. Caesarean section is performed when obstetric indications are identified.
Pregnancy is recommended to be completed by natural childbirth at a physiological time. Caesarean section is performed when obstetric indications are identified.
Prognosis and prevention
With the appointment of adequate treatment, the damaged mucosa of the esophagus usually fully recovers after 4-12 weeks, with non-erosive variants of the disease, improvement occurs within 4-10 days. Prevention of gastroesophageal reflux involves the normalization of diet and lifestyle: giving up bad habits, adequate rest and sleep, controlling weight gain with a tendency to obesity, eliminating foods that irritate the esophageal mucosa or stimulate gastric hypersecretion, taking drugs that can disrupt gastrointestinal motility, only as directed and under medical supervision. To prevent recurrence of GERD in a pregnant woman, a 1-3-day intake of alginates and antacids "on demand" is recommended when symptoms appear. nine0006
You can share your medical history, what helped you in the treatment of GERD in pregnancy.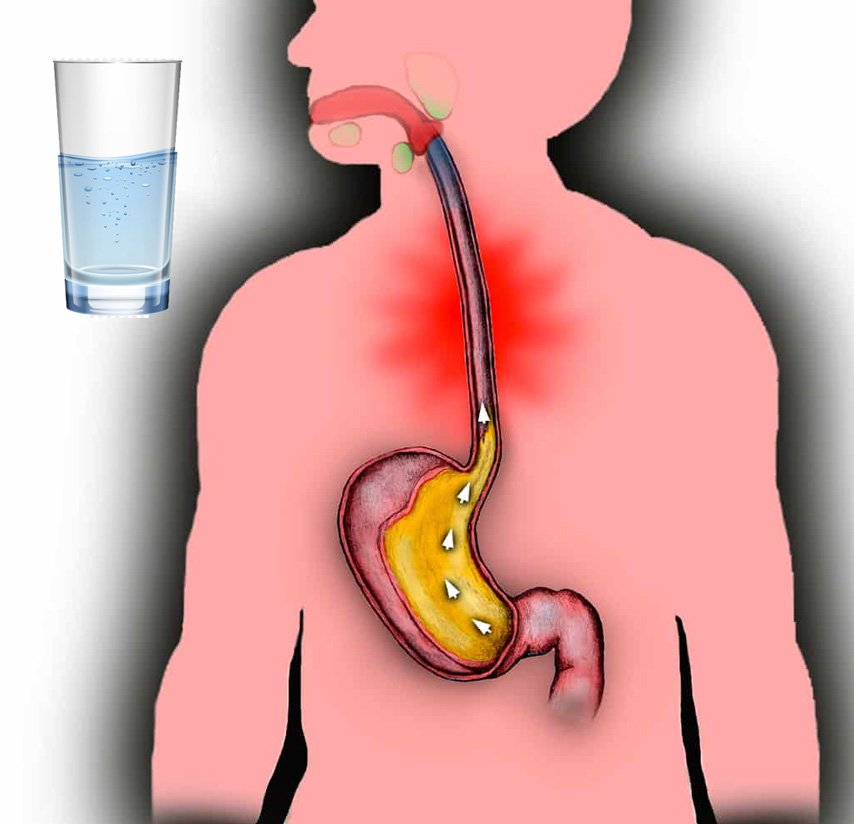
Sources
- Gastroesophageal reflux disease during pregnancy/ Elohina TB, Tyutyunnik VL// Experimental and clinical gastroenterology. - 2009 - No. 3.
- Pregnancy heartburn: an everyday trifle that must be endured, or gastroesophageal reflux disease that should be stopped? / Argunova IA// Gastroenterology. - 2015 - No. 3. nine0016
- Features of the course of gastroesophageal reflux disease in pregnant women/ Grishechkina IA, Kusakina AA, Miermanova MK// Young scientist. - 2015. - No. 13.
- Gastroesophageal reflux disease / Babak O.Ya., Fadeenko G.D. – 2000.
- This article was prepared based on the materials of the site: https://www.krasotaimedicina.ru/
IMPORTANT
Information from this section cannot be used for self-diagnosis and self-treatment. In case of pain or other exacerbation of the disease, only the attending physician should prescribe diagnostic tests. For diagnosis and proper treatment, you should contact your doctor. nine0006
nine0006
Acid related diseases in pregnancy | Rassvet Clinic
Heartburn during pregnancy is a very common complaint. It is known that up to 80% of pregnant women experience symptoms characteristic of gastroesophageal reflux disease (GERD) (heartburn, dysphagia, belching, and others), and the frequency of heartburn in the first trimester is 7.2%, in the second - 18.2%, in the third - 40%.
The main factors behind this high prevalence of GERD in pregnancy include hormonal changes such as hyperprogesteronemia (increased levels of the hormone progesterone) and hyperestrogenemia (increased levels of estrogen hormones), as well as increased intra-abdominal pressure due to uterine and fetal growth. nine0006
The action of gestational hormones in the first trimester of pregnancy is due to the fact that they, without affecting the basal tone of the lower esophageal sphincter (LES), reduce the increase in pressure of this sphincter in response to a variety of physiological stimuli, including food intake. In the second and third trimesters of pregnancy, progesterone and estrogen reduce the basal tone of the LES to 50% of the initial level, the maximum decrease occurs at 36 weeks of gestation. After a successful delivery, the tone of the LES in women who did not suffer from GERD before pregnancy, as a rule, returns to normal - in connection with this, this condition is called "pregnancy heartburn." nine0006
In the second and third trimesters of pregnancy, progesterone and estrogen reduce the basal tone of the LES to 50% of the initial level, the maximum decrease occurs at 36 weeks of gestation. After a successful delivery, the tone of the LES in women who did not suffer from GERD before pregnancy, as a rule, returns to normal - in connection with this, this condition is called "pregnancy heartburn." nine0006
Pregnancy heartburn usually does not lead to the development of esophagitis, complications of GERD (strictures, ulcers, bleeding) and does not require serious medical treatment.
If a woman had GERD before pregnancy, the complaints may worsen during pregnancy and require examination and medication.
The diagnosis of GERD during pregnancy is established primarily on the basis of complaints, medical history and physical examination. X-ray examination in pregnant women - due to possible damaging effects on the fetus - is not used, pH-metry and manometry can be used, but the need for its use is doubtful.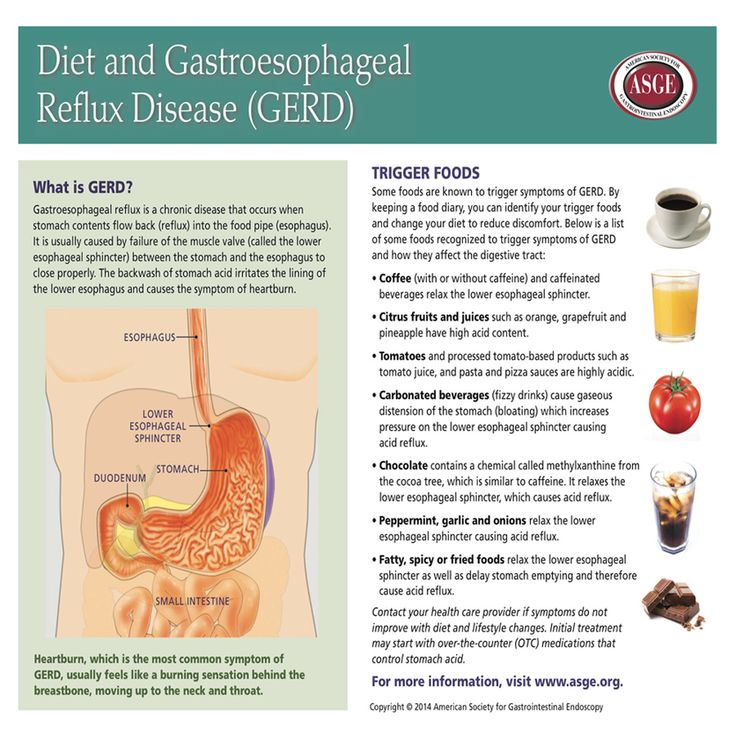 nine0006
nine0006
Esophagogastroduodenoscopy (EGD) is the method of choice for diagnosing GERD in pregnant women, but it should only be used for strict indications, such as a history of complications of GERD and the ineffectiveness of ongoing drug therapy.
Treatment of GERD in pregnant women should be based on changes in lifestyle and nutrition: exclusion of a horizontal position of the body immediately after meals, sleeping with the head end of the bed elevated (by 15 cm), exclusion of physical exertion that increases intra-abdominal pressure (including wearing corsets, tight belts, bandages). The last meal should take place no later than 3 hours before bedtime, you need to eat in small portions, pay special attention to the normalization of the stool. nine0006
First-line drugs for the treatment of GERD in pregnant women include antacids and alginates. With the ineffectiveness of these drugs, it is permissible to prescribe prokinetics (metoclopramide), blockers of histamine h3 receptors and (according to strict indications) proton pump inhibitors (PPIs).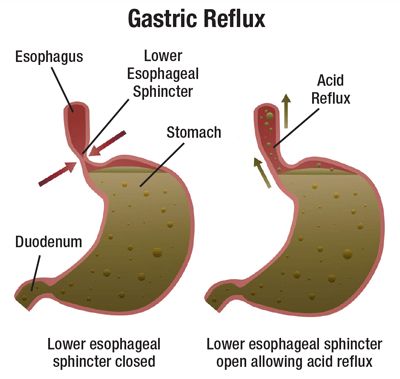
H2-histamine blockers are the most commonly prescribed group of drugs for pregnant women. They are classified as risk category B by the US Food and Drug Administration (FDA) ( "drugs that have been taken by a limited number of pregnant women without evidence of their effect on the incidence of congenital anomalies or damaging effects on the fetus") . In Russian instructions, only cimetidine and ranitidine are allowed with a caveat: use during pregnancy is possible only if the expected effect of therapy outweighs the potential risk to the fetus. Famotidine and nizatidine in the Russian Federation are contraindicated for pregnant women.
Although most PPIs are also classified by the FDA as risk category B, in Russia there are more stringent restrictions on the use of this group of drugs in pregnant women. So, lansoprazole is contraindicated in the first trimester, in the second and third trimesters it can be used only if the expected benefit of therapy outweighs the potential risk to the fetus. The use of pantoprazole and esomeprazole is possible only under strict indications, when the benefit to the mother outweighs the potential risk to the fetus. Rabeprazole during pregnancy is contraindicated. nine0006
The use of pantoprazole and esomeprazole is possible only under strict indications, when the benefit to the mother outweighs the potential risk to the fetus. Rabeprazole during pregnancy is contraindicated. nine0006
Pregnancy has a beneficial effect on the course of peptic ulcer disease: 75-80% of women experience remission of the disease, and it does not have a noticeable effect on its outcome. However, some patients may experience an exacerbation. This is most often observed in the first trimester of pregnancy (14.8%) and the third trimester (10.2%), as well as 2-4 weeks before the due date or in the early postpartum period. Uncomplicated peptic ulcer does not adversely affect the development of the fetus.
Treatment of peptic ulcer in pregnant women includes adherence to generally accepted "regime" measures and diet; taking in the usual therapeutic doses of non-absorbable antacids (1 sachet 3 times a day 1 hour after meals and adsorbents 1 sachet 3 times a day 1 hour after meals).