Spotting during second trimester
The Second Trimester of Pregnancy: Pain, Bleeding, and Discharge
Pain, bleeding, and discharge
Some pain or discomfort is normal during the second trimester of pregnancy. Spotting and very small amounts of blood may also be harmless. However, there are certain types of pain, bleeding, and vaginal discharge that you shouldn’t ignore.
Learn how to tell the difference between normal pregnancy problems and serious medical concerns.
Emergency medical symptoms during the second trimester
There are a number of situations during pregnancy that demand medical attention. If you experience the symptoms below, don’t hesitate to call your doctor or seek emergency care.
When to seek emergency medical attention
Always seek emergency care if you are experiencing the symptoms of a miscarriage. Symptoms of a miscarriage include:
- enough vaginal bleeding to soak more than one menstrual pad
- severe pain in the abdomen or pelvic region
- clots or clumps of tissue (typically gray or pink in color) passed from the vagina
If you pass clots or clumps from the vagina, try to save the tissue in a jar or plastic bag to give to the doctor for analysis. They may then determine the cause of the problem.
There are three types of miscarriage.
If a miscarriage has been threatened, there was bleeding before 20 weeks of pregnancy with no cervical dilation and no expulsion of any of the fetal parts.
If a miscarriage has been completed, there was complete expulsion of fetal parts from your body.
If a miscarriage has happened incompletely, there was partial expulsion of the fetal parts before 20 weeks. In the case of incomplete miscarriages, the next step may be to allow the remaining products of pregnancy to pass naturally or perform a dilation and curettage.
Note: If you have miscarried before and notice bleeding or cramping, you should seek emergency medical attention.
Always seek emergency care if you are experiencing the symptoms of an ectopic pregnancy (a pregnancy outside the uterus). Symptoms of an ectopic pregnancy include:
- cramps and colicky (spasmodic) pain with associated tenderness
- pain that starts on one side and spreads across the belly
- pain that worsens with taking a bowel movement or coughing
- light bleeding or spotting that is brown in color, is either constant or intermittent, and precedes the pain by weeks
- one of the above symptoms combined with nausea and vomiting, pain in the shoulder, weakness or lightheadedness, or rectal pressure
- rapid and weak pulse, clamminess, fainting, and sharp pain (these symptoms may arise if the ectopic pregnancy is in the fallopian tube and the tube ruptures, causing septic shock)
When to call your doctor
Emergency care isn’t always necessary. However, some signs require a doctor’s evaluation. Always call your doctor for advice if you’re experiencing signs of miscarriage. Early signs of miscarriage include:
However, some signs require a doctor’s evaluation. Always call your doctor for advice if you’re experiencing signs of miscarriage. Early signs of miscarriage include:
- cramps and pain in the center of the abdomen with vaginal bleeding
- severe pain or pain that lasts for more than a day (even without bleeding)
- bleeding that is as heavy as a period
- spotting or staining that lasts for three days or longer
Pain
Although you may not experience an emergency, there will probably be times during your pregnancy when you’re uncomfortable or in pain. Many women have pain during the second trimester even when nothing is medically wrong.
Abdominal pain, back pain, headaches, leg cramps, and hand pain don’t always signal a problem. Learning to identify and relieve these normal discomforts will help you throughout your pregnancy.
Abdominal pain
Abdominal pain can either be a normal symptom of pregnancy or a sign of something serious, like preterm labor or ectopic pregnancy. It’s important to tell your doctor when you feel any type of abdominal pain, because of the potential for a serious complication.
It’s important to tell your doctor when you feel any type of abdominal pain, because of the potential for a serious complication.
When you feel pain in your abdomen during the second trimester, it’s usually related to the tension on the ligaments and muscles in the pelvis. These get stretched as the uterus expands to hold the growing baby.
If you move quickly, you can “pull” a ligament or muscle. This may feel like a painful pang in your pelvis or a cramp down your side that can last for several minutes. This kind of pain isn’t harmful to you or your baby.
Sometimes abdominal pain is related to past pregnancies or surgeries. If you’ve had surgery for infertility or other types of abdominal surgery, you may experience pain from the pulling of the remnants of scar tissue (adhesions).
Pregnant women can also have the same types of abdominal infections that other women develop. Infections that can cause abdominal pain include:
- cholecystitis (inflamed gallbladder)
- appendicitis (inflamed appendix)
- hepatitis (inflamed liver)
- pyelonephritis (kidney infection)
- pneumonia (lung infection)
Sometimes these diseases are harder to diagnose during pregnancy because the location of pain characteristic to each has been shifted. This happens when the growing uterus pushes nearby organs out of its way.
This happens when the growing uterus pushes nearby organs out of its way.
If you’re experiencing serious pain that doesn’t feel like it’s in your uterus, show or tell your doctor exactly where the pain is located. If you have one of the above infections, you may need antibiotics or surgery to fix the problem.
Warning: If you’re experiencing regular or painful contractions in the pelvis or abdomen, call a doctor immediately. These may be a sign of preterm labor.
Back pain
Back pain is very common during pregnancy. Pregnancy hormones cause the joints in the pelvis to become soft and lax in preparation for childbirth. As your uterus gets bigger in the second trimester, your center of gravity changes.
You begin to carry yourself differently to accommodate the weight. In addition, your abdominal muscles may separate as the uterus presses up against them, weakening the abdominal wall. All of these factors can contribute to back pain, strain, and discomfort.
Here’s how you can improve back pain:
- Practice good posture while standing (shoulders back, pelvis in) and sitting (elevate feet slightly and try to avoid crossing your legs).
- Get up every once in a while when you’re sitting for long periods.
- Lift heavy objects by bending at the knees, rather than the waist.
- Try not to reach for things over your head.
- Sleep on your left side, bending at your hips and knees, and place a pillow between your legs to reduce pressure on your back.
- Strengthen your stomach muscles. One of the keys to a strong back is a strong abdomen.
- Talk to your doctor. You may need to use a back brace or some other form of support to relieve the pressure on your back.
Warning: If you’re experiencing lower back pain accompanied by painful urination, you may have a bladder or kidney infection. Low, dull, consistent back pain may be a sign of preterm labor. Severe back pain coupled with vaginal bleeding or discharge may also indicate a serious problem. Call your doctor immediately if you experience any of these symptoms.
Severe back pain coupled with vaginal bleeding or discharge may also indicate a serious problem. Call your doctor immediately if you experience any of these symptoms.
Headaches
Many women experience frequent headaches during pregnancy. You still may be experiencing headaches that started during the first trimester, or they may be just beginning now.
Hormonal changes, tension, fatigue, hunger, and stress are all culprits. Try to relax, stay rested, and eat regularly. You can also try to relieve headaches in the following ways:
- If you have a sinus headache, apply warm compresses to aches in the sinus areas of your head. These include both sides of the nose, the middle of the forehead, and the temples.
- If the headache is due to tension, try applying cold compresses to aches along the back of your neck.
- Learn relaxation exercises, like closing your eyes and imagining yourself in a peaceful place. Reducing stress is a key component of a healthy pregnancy.
 Consider calling a counselor or a therapist if needed.
Consider calling a counselor or a therapist if needed.
Speak with a physician before you begin using pain relievers. This is important even if you took over-the-counter medications for pain before you were pregnant.
Common headache medicines include ibuprofen (Motrin), aspirin (Bufferin), acetaminophen (Tylenol), and naproxen sodium (Aleve).
Acetaminophen is probably the safest option during pregnancy, but don’t take pills during pregnancy unless your doctor has specifically told you to do so.
Warning: Call your doctor if the headache is particularly severe or lasts for more than a few hours. Also note whether your headache comes with a fever, swelling in the face and hands, dizziness, nausea, or changes in vision. These may be signs of preeclampsia or another serious complication.
Leg cramps
Although no one knows exactly what causes them, leg cramps are common in the second and third trimester. Possible causes may be that you don’t consume enough calcium, have too much phosphorous in your diet, or are tired.
Possible causes may be that you don’t consume enough calcium, have too much phosphorous in your diet, or are tired.
It may be that the uterus is pressing on the nerves that go to the legs. Regardless of the cause, you may wake up in the middle of the night with bothersome cramps.
You can avoid or get rid of cramps by:
- exercising your calves
- staying hydrated
- alternating between sitting and standing
- wearing support hose
- wearing comfortable, supportive shoes
- flexing the ankle and toes upward with a straightened knee to stop the cramping
- massaging or applying a warm compress to the leg that is cramping
- talking to your doctor about reducing the amount of phosphorous in your diet by cutting down on foods like milk or meat
- making sure you get enough calcium (by eating fortified cereal or spinach) and magnesium (by eating beans or semisweet chocolate)
Warning: Tell your doctor if the cramps feel particularly painful, fail to go away, cause swelling, feel warm to the touch, or change the skin color of your leg (to white, red, or blue). You may have a blood clot in a leg vein that needs to be treated. This is known as deep vein thrombosis, and without treatment it can be deadly. Consult a doctor immediately.
You may have a blood clot in a leg vein that needs to be treated. This is known as deep vein thrombosis, and without treatment it can be deadly. Consult a doctor immediately.
Pain and numbness in the hand
Numbness and pain in the thumb, index finger, middle finger, and half of the ring finger can be a sign of carpal tunnel syndrome.
Usually this condition is diagnosed in people who regularly perform repetitive tasks such as typing or piano playing, but it’s also common in pregnant women.
During pregnancy, the tunnel that surrounds the nerve to these fingers can become swollen, causing tingling, numbness, and pain. In the evening, after your arm has been dangling by your side all day, your symptoms may worsen due to gravity.
Shaking out your arm when you experience the carpal tunnel symptoms may help. Alternatively, you may want to talk to your doctor about splinting your wrist or taking vitamin B-6.
Numbness and tingling in the hand can also be caused by poor posture. If your shoulders droop and your head is thrust forward, you put pressure on the nerves under your arms, causing tingling.
If your shoulders droop and your head is thrust forward, you put pressure on the nerves under your arms, causing tingling.
Practice standing up straight with your head and spine erect. A supportive bra and proper bed rest are also important.
Bleeding
Bleeding can be a scary symptom during pregnancy. In some cases, bleeding can be harmless. It can happen when pregnancy hormones cause you to develop more sensitive, expanded blood vessels.
In other cases, bleeding can indicate a serious problem with the pregnancy. If you experience any bleeding, call a doctor for advice.
Vaginal bleeding
Light bleeding or spotting (which can be brown, pink, or red) during the second and third trimester isn’t usually cause for concern. It typically occurs as a result of interference with the cervix during sex or a vaginal exam.
Pink mucus or brownish discharge may both occur during the second trimester. It’s caused by small amounts of blood leaving your body with normal discharge.
Vaginal bleeding that’s like a period, however, can be a worrisome sign that needs immediate medical attention. Clots of blood or clumps of tissue in the blood may be symptoms of a miscarriage.
For this reason, you should never be the judge of what is normal or abnormal bleeding. Instead, call your doctor.
If the bleeding is heavy or if it’s accompanied by pain, call your doctor immediately. If it’s spotty, you can make the call sometime that day. Serious bleeding is most commonly caused by placenta previa, premature labor, or late miscarriage.
Rectal bleeding and hemorrhoids
Rectal bleeding isn’t as worrisome as vaginal bleeding and is generally a sign of either hemorrhoids or anal fissure. Rectal bleeding could also be a sign of something more serious. You should speak with your doctor if you’re experiencing this symptom.
Rectal bleeding may mean you have hemorrhoids, either external or, less commonly, internal. Hemorrhoids occur in up to half of all pregnant women. They are varicose veins of the rectum and can cause pain, itching, and bleeding, often made worse by constipation.
They are varicose veins of the rectum and can cause pain, itching, and bleeding, often made worse by constipation.
Hemorrhoids are caused by progesterone acting on the walls of the rectal veins, causing them to relax and expand. As you advance in your pregnancy and the uterus presses on these veins, blood flow slows down and the veins dilate even more.
Squeezing and constipation can make hemorrhoids worse. Laughing, coughing, straining, and going to the bathroom may cause hemorrhoids to bleed.
If rectal bleeding isn’t caused by hemorrhoids, it may be caused by an anal fissure — a crack in the skin that lines the anal canal. Anal fissures are usually caused by constipation. Fissures are very painful, particularly during the strain of taking a bowel movement.
Hemorrhoids and anal fissures can cause brown, pink, or red bloodstains to appear on your underwear or toilet paper. If the bleeding is heavy or continuous, call a doctor for advice.
If you’re diagnosed with hemorrhoids or an anal fissure, you should do the following:
- Try to avoid constipation by remaining well hydrated and eating a diet high in fiber.
- Try to alleviate pressure on the veins in the rectum by sleeping on your side, not standing or sitting for long periods of time, and not taking too long or straining when going to the bathroom.
- Take warm sitz baths up to two times a day. Sitz baths are basins that fit on your toilet and are filled with warm water in which you can soak your anus.
- Soothe the hemorrhoids with ice packs or witch hazel, and only use topical medications if your doctor prescribes them. Your doctor may also prescribe stool softeners or a laxative.
- Practice good hygiene by wiping thoroughly after bowel movements (from front to back) and keeping yourself clean.
- Use only white, unscented toilet paper.
- Perform Kegel exercises to improve the circulation to the area.
Warning: Massive rectal bleeding can be a serious problem. It can be caused by ectopic pregnancies or serious internal problems. Seek medical care immediately if you’re bleeding heavily from the anus.
Nosebleeds and nasal congestion
Like many of the complaints of pregnancy, nasal stuffiness and nosebleeds are believed to be due in large part to estrogen and progesterone. These hormones cause increased blood flow and swelling of the blood vessels in the mucus membranes.
Particularly in cold, dry weather, this can mean that you feel more congested than normal. You may also experience nosebleeds more often than you did before getting pregnant.
You may want to try the following to ease your nasal symptoms:
- Use a humidifier to help with the dryness that can make symptoms worse.
- Blow your nose gently by closing one nostril while you blow through the other.
- Curb nosebleeds by leaning forward and applying gentle pressure to the nose. Try squeezing it with the thumb and forefinger for five minutes. Repeat if necessary.
- Call your doctor if the bleeding doesn’t stop, or is heavy or frequent.
- Seek emergency medical care if nasal congestion makes it hard to breathe.

The same changes in hormones and blood vessels that cause nasal bleeding can cause sensitive gums. If you experience bleeding when flossing or brushing your teeth, try using a softer toothbrush.
Visit a dentist if you bleed a lot or have a lot of pain when flossing or brushing your teeth. Serious dental problems can be a sign of other health concerns that can complicate pregnancy.
Discharge
Many women experience different types of discharge during the second trimester. Pay attention to the color, smell, amount, and frequency of vaginal or anal discharge. Some types of discharge may indicate an infection that needs medical attention or treatment.
Vaginal discharge
As the pregnancy progresses, you may notice increasing vaginal discharge. Typically, it looks like egg whites and is milky and a bit odorous. It may remind you of premenstrual discharge, only a bit heavier and more frequent.
This discharge is totally normal and is just another change your body goes through in response to the pregnancy hormones and the increased blood flow to the area. You can wear panty liners or change your underwear more often than usual if you find the discharge bothersome.
You can wear panty liners or change your underwear more often than usual if you find the discharge bothersome.
Though the kind of discharge described above is normal, there are some types of discharge that may mean you have an infection.
Vulvovaginal candidiasis, or yeast infection, is very common during pregnancy. Signs include a thick, cottage cheese-like discharge accompanied by itching, redness, and burning, as well as painful intercourse and urination.
Sexually transmitted infections (STIs) may also occur during pregnancy, and because many of them can affect the fetus, it’s important that they be treated.
You may have a condition that requires treatment if any of the following is true:
- The discharge looks like pus.
- The discharge is yellow, green, or has a foul odor.
- You notice a burning sensation when you urinate.
- Your labia are red, swollen, or itchy.

Unlike signs of infection, clear or pinkish watery discharge may be a sign of premature rupture of the amniotic sac.
Rupture of the sac may cause a trickle of watery discharge or a rush of lots of watery fluid from the vagina. This is commonly known as having the water break before labor begins.
Warning: If you experience a steady trickle or a rush of watery discharge during the second trimester, call a doctor immediately. It may be a sign of premature labor or a tear in the amniotic sac.
Rectal discharge
In addition to bleeding from the rectum, some women may experience anal discharge during pregnancy. Rectal discharge may be caused by STIs, bowel and gastrointestinal problems, or physical wounds in the rectum. If you’re experiencing rectal discharge, consult a doctor.
Gonorrhea, chlamydia, and other infections that can be transmitted through sexual contact can cause an infection in the anus. These infections can cause lesions or sores that bleed. In addition, they may lead to discharge that’s foul-smelling, green or yellow, and thick.
In addition, they may lead to discharge that’s foul-smelling, green or yellow, and thick.
It may be painful to wipe or go to the bathroom. If you have these symptoms, discuss them with a doctor. Left untreated, they may cause serious problems for the baby. Most STIs can be treated with antibiotics.
Some pregnant women may experience anal discharge due to bowel problems or gastrointestinal disorders. These may result in mucus or watery discharge from the anus.
Certain gastrointestinal problems or food poisoning may also cause frequent diarrhea or fecal matter with unusual colors or textures. Tell your doctor about any unusual characteristics of your bowel movements. Some conditions require immediate treatment.
Finally, if you have a hemorrhoid or anal fissure that has become infected, you may notice unusual rectal discharge. Infected wounds may cause brown, yellow, green, or white discharge.
Such a wound may or may not have a foul smell. Infected sores are often very painful and require medical attention. Consult a doctor for treatment if you experience anal discharge of this nature.
Consult a doctor for treatment if you experience anal discharge of this nature.
Nipple discharge
Many women experience discharge from one or both nipples during the second trimester of pregnancy. Breast tenderness and changes in nipple color are also common during pregnancy.
Discharge is most common in women who have previously given birth. Nipple discharge is often clear, milky, or yellowish in color.
Discharge from the nipples is normally not a sign of a problem, unless the following symptoms are present:
- The nipple changes in size or becomes inverted.
- The nipple is dry, cracked, or painful.
- The nipple has a rash or new bumps.
- The discharge is foul-smelling, bloody, green, or brown.
If you aren’t sure whether your nipple discharge is normal, call a doctor to discuss your symptoms.
Bleeding During Pregnancy, What’s Normal?
Whether you’re early on in your pregnancy or about to pop, vaginal bleeding of any kind can be very scary and worrisome. Is this normal spotting or should you be concerned about your unborn baby?
Is this normal spotting or should you be concerned about your unborn baby?
In many cases, bleeding during pregnancy is normal. Where you are in your pregnancy and the severity of bleeding – whether light spotting or heavy bleeding – provide clues as to whether what you’re experiencing is normal or cause for concern.
Is there a difference between spotting and bleeding?
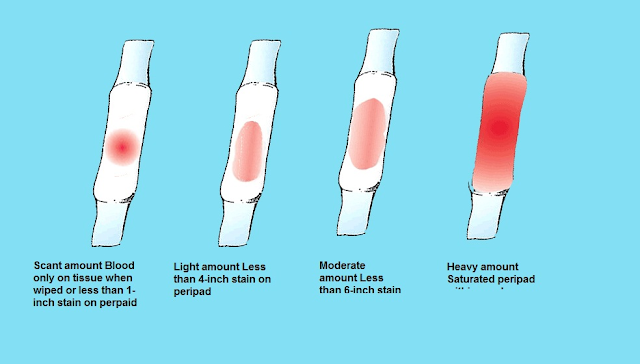
Spotting is light bleeding—the type of bleeding that wouldn’t cover a panty liner. Whereas bleeding is a flow of blood that’s greater than a drop here and there. It’s heavier in nature and would require a liner or pad to keep the blood from soaking through your underwear.
You should always let your provider know if you’re experiencing any type of spotting or bleeding, but the timing of when to seek help is key.
When should I seek help for vaginal bleeding during pregnancy?
If you notice pink, red or dark brown ‘spots’ smaller than a dime on undergarments or when you wipe, you can generally wait until your health care provider’s office opens to call and schedule an appointment.
“However, bleeding that soaks through a pad within an hour, and continues, requires urgent evaluation in the emergency room during the first trimester and early second trimester. Patients in mid-second trimester and beyond should go directly to the triage room in labor and delivery,” said Celia Valenzuela, MD, an OBGYN at Banner Health in Tucson, AZ. “Bleeding that is similar to your period in the third or mid to late second trimester always warrants evaluation.”
It’s important to know your blood type as some blood types may require special medication. If your blood is Rh negative, you’ll likely need medicine called Rh immunoglobulin or RhoGAM. Your provider can guide you through the timing of this. Learn more about Rh factor.
[Call 911 if you’re also experiencing intense cramping, a fever of 100.4 or higher, dizziness or thick vaginal discharge along with heavy bleeding.]
While it’s natural to go to worst case scenario at the sight of blood, read on to learn the potential causes for bleeding during the first trimester, second trimester and third trimester.
What are the most common causes of bleeding in the first trimester?
While seeing blood in your underwear can be unnerving, it’s not uncommon during the first trimester. While estimates can vary, about 1 in 4 pregnant people experience bleeding during the first trimester.
One of the most common causes of bleeding in early pregnancy occurs in the first few weeks during implantation, when the fertilized egg implants on the uterine wall.
“During pregnancy, pregnancy hormones can alter a person’s cervix, making it more sensitive and more susceptible to bleeding when touched,” Dr. Valenzuela said. “It’s not uncommon then to notice spotting or light bleeding after sex, insertion of a speculum, collection of a cervical specimen for pap test or culture and cervical examination for dilation.”
Problems that can cause bleeding in early pregnancy can include:
- Pregnancy loss or miscarriage: Roughly half of people who experience spotting in early pregnancy do miscarry, however this means half of women who spot, do not.
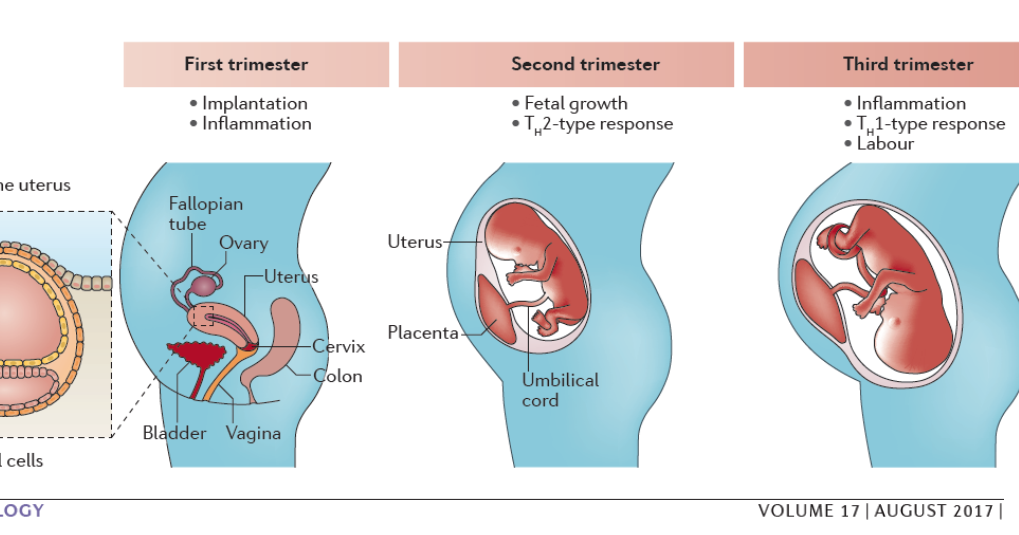
- Ectopic pregnancy: Usually, an ectopic pregnancy happens when a fertilized egg implants outside of the uterus. Symptoms of an ectopic pregnancy may include spotting or light bleeding and pelvic or belly pain. This is rare in pregnancies but is considered a medical emergency. “The amount of bleeding that you may experience can vary, though generally it is light prior to diagnosis,” Dr. Valenzuela said. “After an ectopic pregnancy is treated, you may have heavier bleeding as hormone levels decrease.”
- Molar pregnancy: A molar pregnancy is rare but occurs when abnormal tissue grows inside the uterus, instead of an embryo. You may think you’re pregnant, but an ultrasound shows no fetal heart rate. “Frequently, molar pregnancies are discovered during an ultrasound during the first trimester before bleeding has started,” Dr. Valenzuela said.
- Cervical or vaginal infections: Any infection of the cervix, vagina or a sexually transmitted infection like chlamydia, gonorrhea or herpes can cause bleeding.

- Cervical polyps: A harmless growth on the cervix that can result in bleeding during pregnancy.
“Many people frequently worry about miscarriage when they experience bleeding in the first trimester, and as a provider, we worry about this as well,” Dr. Valenzuela said. “Call your health care provider, so they can do the appropriate blood or ultrasound tests to identify the cause.”
What are the causes for vaginal bleeding later in pregnancy?
Like the first trimester, light bleeding or spotting during your second or third trimester may occur after sex or a cervical exam. It can also be due to a “bloody show,” a sign that labor is starting.
Problems that can occur later in pregnancy can be caused by placental abnormalities, such as placental abruptions or placenta previa.
“Placenta abruptions occur when the placenta separates partially from the uterine wall often resulting in very heavy bleeding,” Dr. Valenzuela said. “Placental previas occur when the placenta is placed over the opening of the cervix. Both require timely medical care.”
Both require timely medical care.”
Bottom line
Not all spotting and bleeding are a cause for concern during pregnancy, but it’s best to get evaluated by your health care provider.
If you’re experiencing abdominal pain, cramping, unusual vaginal discharge, contractions, fever or soreness in the uterus, seek emergency care. These symptoms could be a sign of a serious problem or may even signal preterm labor.
Also read:
- Prenatal Screenings and Tests, What to Expect Every Trimester
- Is a Headache During Pregnancy Something to Worry About?
- Expect the Unexpected: How Your Body Changes During Pregnancy
Women's Health Gynecology Pregnancy
Join the Conversation
What is it? Normal and abnormal discharge during pregnancy
Today we will talk with Elena Yurievna Romanova, an obstetrician-gynecologist at the Expert Center for Pregnancy Management at the Mother and Child Clinic, about what discharges during pregnancy should be feared and what discharges from the genital tract are regarded as normal.
Increased vaginal discharge during pregnancy is natural
Normal pregnancy discharge is milky white or clear mucus without a strong odor (although the smell may change from before pregnancy), this discharge does not irritate the skin and does not cause discomfort to the pregnant woman. The discharge can have a different color - from completely colorless (most often) to whitish and yellowish. The consistency of discharge at the beginning of pregnancy resembles raw chicken yolk - they are thick, jelly-like, often released in the form of clots.
With normal discharge, it is enough to use panty liners or change underwear twice a day.
Due to the activity of progesterone in the first 12 weeks of pregnancy, the discharge will be scarce and viscous.
Due to the increase in estrogen activity from 13 weeks, the discharge becomes less viscous and more abundant.
By the end of the pregnancy, vaginal discharge becomes more and more abundant. Each time you need to evaluate the nature of the discharge, change the gasket. If the fluid continues to ooze, this may mean leakage of amniotic fluid and the need to contact an obstetrician-gynecologist in the emergency department of a hospital with a maternity ward. There are auxiliary tests, thanks to which, as well as obstetric ultrasound, leakage of water can be excluded.
Each time you need to evaluate the nature of the discharge, change the gasket. If the fluid continues to ooze, this may mean leakage of amniotic fluid and the need to contact an obstetrician-gynecologist in the emergency department of a hospital with a maternity ward. There are auxiliary tests, thanks to which, as well as obstetric ultrasound, leakage of water can be excluded.
Not all discharge in pregnant women is the norm.
For example, a white, thick, crumbly, odorless discharge that itchs and burns the skin and causes discomfort during intercourse is likely a sign of a yeast infection (candidiasis).
White or grayish discharge, the smell of which after sex begins to resemble the smell of fish, is the main symptom of bacterial vaginosis, vaginal dysbacteriosis.
A yellowish or greenish discharge that has a strong unpleasant odor usually occurs with nonspecific vaginitis, and a foamy discharge is a sign of trichomoniasis, a sexually transmitted disease.
In all these cases, contact your doctor immediately. It should not be treated with over-the-counter drugs and folk remedies. According to some external signs, a diagnosis cannot even be made by a doctor, in addition, infections in pregnant women should be treated especially carefully and only by a professional. After proper treatment, the discharge returns to normal. There is no need to get rid of the usual discharge for pregnant women. After childbirth, they will stop naturally, and before that they are a sign of the normal course of pregnancy.
Allocations can change their nature and amount under the influence of irritants or intolerance to a particular substance, for example, when using panty liners. Such secretions are transparent and abundant, they stop when the irritant is removed.
"Thrush" is a disease caused by fungi of the genus Candida, present in small quantities in all women. During pregnancy, immunity decreases and fungi begin to actively multiply, causing inflammation, abundant white flocculent discharge with a sour smell, burning and itching in the vulva. The disease can manifest itself throughout pregnancy.
The disease can manifest itself throughout pregnancy.
Bloody discharge in the first half of pregnancy usually indicates a lack of the hormone progesterone, which can lead to spontaneous miscarriage. Discharge may be accompanied by pain in the lower abdomen and lower back. In the treatment of the threat of abortion, the appointment of progesterone drugs, such phenomena disappear.
If bleeding from the vagina appeared during pregnancy during the second or third trimester, then this is a sign of a formidable complication, namely, placenta previa or its premature detachment. With improper attachment of the placenta in the uterine cavity and overlapping of the placental tissue with the area of the internal pharynx, they speak of placenta previa. In this case, spotting occurs in a third of pregnant women. This most often occurs between 28 and 30 weeks, when the lower segment of the uterus is most prone to stretching and thinning. The discharge is repeated, the woman does not experience any pain, so it may be too late to see a doctor for an examination. This threatens the child with a lack of nutrients and oxygen, because it is through the placenta that the fetus is nourished. For a pregnant woman, this is fraught with acute placental abruption and severe bleeding, which is always problematic to stop, especially at home.
This threatens the child with a lack of nutrients and oxygen, because it is through the placenta that the fetus is nourished. For a pregnant woman, this is fraught with acute placental abruption and severe bleeding, which is always problematic to stop, especially at home.
Bloody discharge during pregnancy should force a woman to immediately contact her obstetrician-gynecologist.
Brown discharge during pregnancy also indicates the threat of termination of pregnancy, or bleeding "erosion" (decidual polyp) of the cervix. Therefore, you should not understand these issues on your own; when brown discharge appears, it is better to consult your doctor.
Brown discharge during a delay in menstruation as a sign of an ectopic pregnancy is very dangerous. This condition requires immediate surgical care, as the growing embryo can rupture the wall of the fallopian tube at any time and cause internal bleeding. Therefore, with pain in the lower abdomen, which is accompanied by brown discharge from the genital tract and delayed menstruation, you should immediately call an ambulance.
When the vagina becomes inflamed, the mucous discharge acquires a mucopurulent character, a greenish-yellow color, an unpleasant odor, burning and itching appear in the genital area. This is how chlamydia, mycoplasmosis, ureaplasmosis, trichomoniasis manifest themselves. Is it necessary to treat the infection during pregnancy, or is it better to do it after childbirth?
All sexually transmitted infections in pregnant women require treatment, as they can pass to the fetus and cause intrauterine infection (IUI). IUI is very dangerous for a child - it leads to his death or serious illness. Infection of a child during childbirth can lead to such serious complications as pneumonia, severe damage to the brain, kidneys, liver, and blood poisoning (sepsis).
Today, obstetricians and gynecologists have learned to treat any infection in pregnant women in accordance with special guidelines for the timing of pregnancy, so that it is effective and safe for mother and fetus. It is not the treatment that should be feared, but the infection itself and its consequences.
It is not the treatment that should be feared, but the infection itself and its consequences.
Medicines that are used to treat pregnant women have passed the necessary clinical trials, during which it was proved that they do not have a negative effect on the pregnant woman and the fetus, including that they do not have a teratogenic effect (do not cause deformities in the fetus).
Sometimes the discharge is mucous in nature, occurs upon contact with an irritant or allergen. It can be synthetic tight underwear, allergies to fabrics, toiletries, personal care products. If irritation and allergens are not eliminated in time, then an infection that lives on the mucous membranes of the genital organs will definitely join.
Hygiene measures are mandatory for pregnant women. Twice a day you need to take a warm shower, using special gels for pregnant women to wash the genitals. Be sure to monitor the cleanliness of the whole body and underwear - it must be changed daily. Pads (but not tampons!) can be used for discharge. The oral cavity can become the source of infection, so you need to monitor your teeth, brush them twice a day and get an examination by a dentist. Good nutrition strengthens the immunity of a pregnant woman. The diet should contain fresh vegetables and fruits, lean meats and fish, daily dairy products, vegetable oil, a variety of cereals.
Pads (but not tampons!) can be used for discharge. The oral cavity can become the source of infection, so you need to monitor your teeth, brush them twice a day and get an examination by a dentist. Good nutrition strengthens the immunity of a pregnant woman. The diet should contain fresh vegetables and fruits, lean meats and fish, daily dairy products, vegetable oil, a variety of cereals.
A mobile lifestyle, therapeutic exercises and maximum exposure to fresh air are very important. Hiking is useful even at the very end of pregnancy - they will help not only maintain immunity, but also strengthen the muscles that will be required during childbirth. Be healthy!
Pregnancy discharge | What are the discharge during pregnancy? | Blog
In the absence of menstruation, girls usually suspect that conception has occurred. However, during pregnancy, the female body may continue to secrete a secret of a different color and character. We recommend that you keep a close eye on everything that happens so as not to miss the development of adverse events. We will talk about how to recognize problem situations during pregnancy in the article.
We will talk about how to recognize problem situations during pregnancy in the article.
What secretions can occur during conception
Many women note that immediately after the delay and in the later stages, the nature of the secretion changes. It can be:
- With or without scent.
- Depending on the color - transparent, white, cream, yellow, greenish, bloody.
- By consistency - thick, liquid, cheesy.
- As a symptom for assessing the state of health - threatening, safe.
During ovulation, the egg is released from the ovary, its membrane is blown away, a small amount of fluid is released - so it becomes ready for fertilization. At this time, the thick mucus that fills the cervical canal of the cervix becomes less viscous. This makes it easier for the spermatozoa to penetrate and move further into the tubes for fertilization. At this time, you may notice an abundance of clear mucous secretions.
After the fusion of the egg with the spermatozoon, movement into the uterus begins, which should end with implantation in the inner layer. During penetration, its slight detachment may occur - this causes damage to the blood vessels that abundantly penetrate the muscular layer of the uterus. You may see light brown discharge, which is common during pregnancy. The color is due to the fact that the blood has time to clot.
Sometimes the discharge is brightly colored and some women mistake it for early menses. But in this case, a short duration is characteristic, a different shade (dark or scarlet), a slight mark on the linen.
With some features of the structure of the female genital organs (for example, with a bicornuate uterus), after implantation of the embryo in one part, rejection of the endometrium may begin in the other, as is usually the case with menstruation. This rarely happens.
Characteristics of discharge in case of threatened miscarriage
Spontaneous abortion is the rejection of an embryo in the early stages after conception. If at the first signs of pregnancy, you notice spotting, there is a high probability that a miscarriage begins.
If at the first signs of pregnancy, you notice spotting, there is a high probability that a miscarriage begins.
Also, miscarriage symptoms include:
- pulling or pressing on the lower abdomen, sacrum, lower back;
- the muscles of the uterus are tense.
The woman may experience cramps. This continues all the time or intermittently. From the vagina there are scarlet or brown discharge during pregnancy, which was previously confirmed. Sometimes the period may be still small, and the first signs did not have time to appear.
After 22 weeks, this phenomenon is called preterm labor. The child in this case is still weak, the organs are not sufficiently developed, and there is little chance of survival.
The following factors increase the risk of miscarriage:
- various diseases;
- progesterone deficiency;
- nervous and physical strain;
- pathologies in the genitals;
- fetal developmental defects.

To confirm the diagnosis, the doctor prescribes an ultrasound scan. If it shows that the fetal heart rate is disturbed, the tone of the uterus is increased, its size differs from normal for this period, hospitalization will be recommended to maintain pregnancy.
What discharge during pregnancy is considered normal
This secretion does not pose a threat to health:
- transparent;
- whitish;
- yellowish;
- odor free;
- mucous;
- without itching, burning, redness of the genitals.
Clear fluid on underwear is a symptom of ovulation. During pregnancy, the activity of ongoing processes in the body increases, so the amount of secretion secreted may increase. However, a violation of the norm is the leakage of amniotic fluid. You can determine the problem with the help of special diagnostic tests that the doctor will prescribe if he has suspicions.
White color, small amount, homogeneous structure should also not cause concern.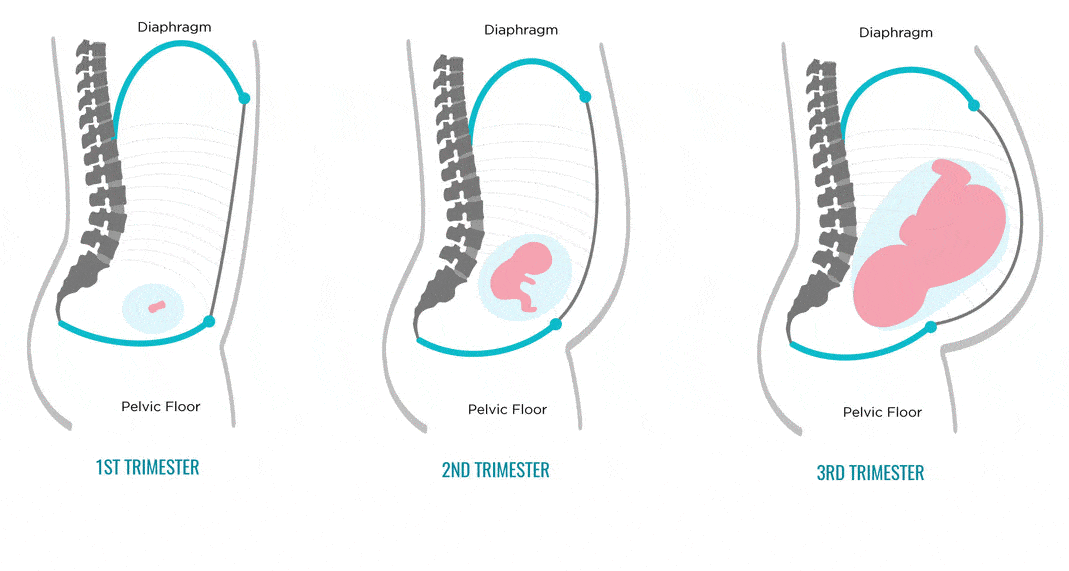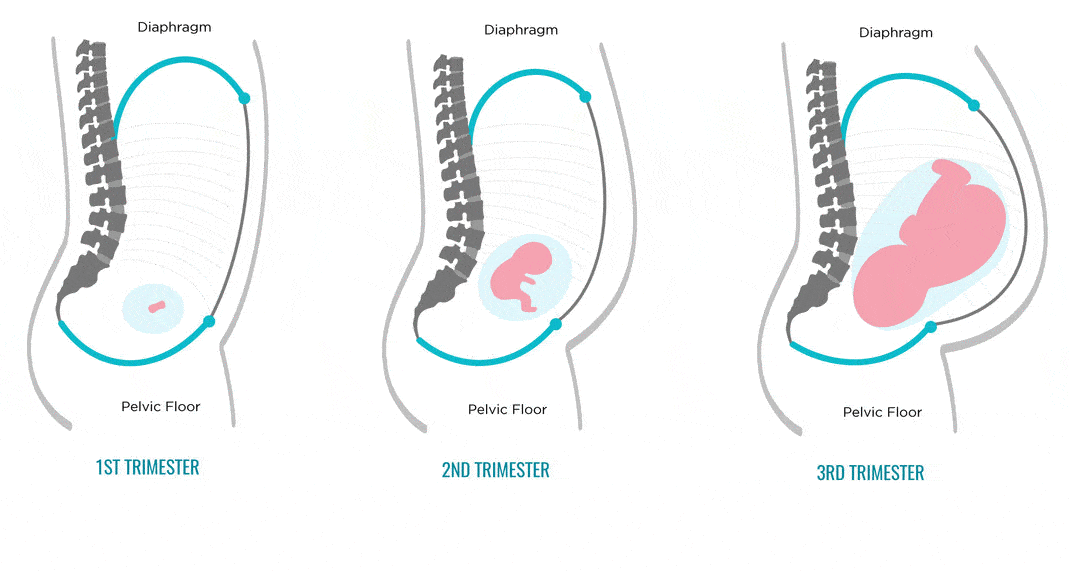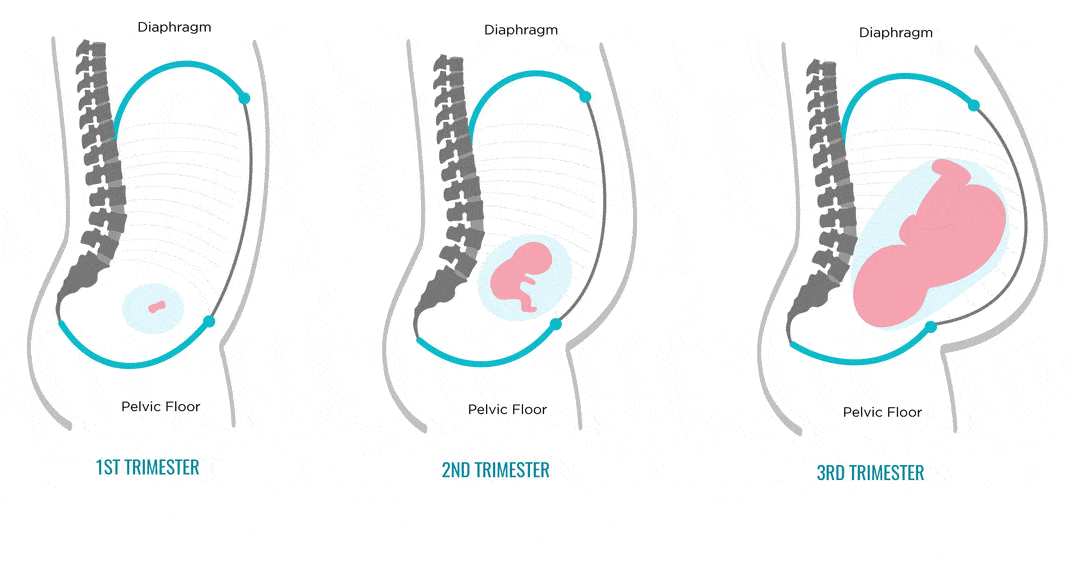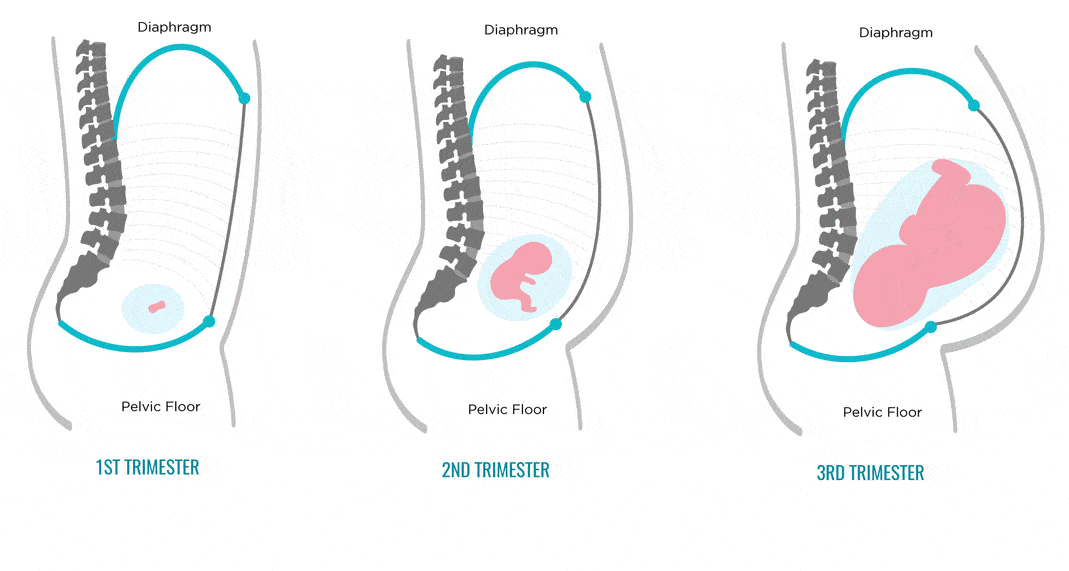 The increased volume of fluid in this case is associated with increased hormonal activity.
The increased volume of fluid in this case is associated with increased hormonal activity.
One of the variants of the norm is mucous discharge, which smells of slight sourness. If there is no pain, discomfort, there is nothing to worry about.
Yellow discharge, there are signs of pregnancy, there is no unpleasant odor - you are all right. Some women had this color before conception, only they did not pay attention. Now there are more of them, therefore more noticeable.
Sometimes a woman observes that the laundry gets wet and there is a smell of urine. This may indicate incontinence due to the constant pressure of the growing uterus. In this case, it is recommended to go to the toilet more often, change underpants twice a day.
What discharge during pregnancy is considered a sign of infection?
White discharge during pregnancy with a cheesy texture is a symptom of thrush (candidiasis). In pregnant women, it is diagnosed quite often - the reason is a change in hormonal levels. The disease is accompanied by itching, redness of the vulva, a strong sour smell. Sometimes external manifestations are not detected, then treatment is not carried out.
The disease is accompanied by itching, redness of the vulva, a strong sour smell. Sometimes external manifestations are not detected, then treatment is not carried out.
Infection is indicated by pain, pain, skin irritation, ulcers, smell of rot or fish, gray or green color, frothy discharge, increased nervousness, large inguinal lymph nodes. The reason may lie in sexually transmitted infections. This includes syphilis, gonorrhea, trichomoniasis, chlamydia and others. They are dangerous because they cause premature birth and fetal developmental defects.
What kind of discharge during pregnancy should I pay special attention to and should I consult a doctor?
The following indicates that pregnancy is at risk:
- Severe pain in the perineum, bleeding, difficulty defecation, convulsions - these may be injuries to the vaginal mucosa.
- Nausea, profuse vomiting, edema, headaches, cough, hypertension, bright red secretion are symptoms of hydatidiform mole (abnormal development of the embryo).
- A drop in blood pressure, pallor, weakness, sweating, pulling sensations, bleeding during pregnancy against the background of a lack of growth of hCG in the blood - this is how an ectopic attachment manifests itself.
- Discharge of clots, sharp pain, vomiting, diarrhea may indicate a frozen fetus.
If you experience any of these symptoms, contact your doctor immediately.
It is also necessary to contact the clinic if you have been physically abused, had rough sex, had an accident, fell, hit. The likelihood that the situation will be resolved successfully is much higher if you do not delay the visit, listen to the symptoms and take good care of your health.
Remember, despite the fact that pregnancy is a normal state of health of the female body, the diagnosis and treatment tactics are still different, due to the many restrictions on manipulations and medications during pregnancy. That is why diagnosis and treatment during pregnancy should take place only under the supervision of a physician.