How to fix incontinence after childbirth
How to Handle Urinary Incontinence After Childbirth
Women who expect to leave all the pregnancy aches and pains behind them after childbirth soon find that postpartum symptoms can be almost just as bad.
These effects can take their tole in different ways and can last up to 6 weeks or longer. Soreness, depression, bleeding, fatigue, and constipation are just a few of the unpleasant outcomes women may experience after giving birth. One of the most common complaints from women is how to handle symptoms of urinary incontinence in the weeks following childbirth. Let’s explore some answers.
An Extremely Common Condition
Sorry to report this, but postpartum urinary incontinence is quite common. According to the latest research, women who give birth vaginally are more likely to experience these complications afterward. In some cases, issues of urinary incontinence can last up to a year, and smaller percentages of women are still living symptoms after 5 years.
Contributing factors include the fact that the bladder and pelvis muscles are weakened during childbirth. In addition, the uterus will begin to shrink back to its normal size, which causes repeated compressions on the bladder. Rapid changes in hormones also need to be considered as the body attempts to balance its female sex hormones after a child is born. Women over the age of 35 and those who are obese are also at a greater risk for urinary incontinence following childbirth.
All together, these influential factors lead women to face a much higher risk for urinary incontinence. The good news is that most women can recover with the proper precautions and effective treatment options recommended by Dedicated to Women.
Simple Lifestyle Changes
There are several ways to address your urinary incontinence without drastically altering your day-to-day routine, including:
- Reduce or completely give up caffeine, carbonated drinks, and alcohol. These beverages, along with spicy foods can cause the bladder to contract much more than what is necessary.
- Losing some weight will ease the pressure on your bladder and pelvic floor.
- Stop smoking if you haven’t done so already. Nicotine causes the muscles of the bladder to spasm, and persistent smoking often leads to a chronic cough that encourages bladder leakage.
- Don’t stop drinking water thinking that it will reduce your urge or need to urinate. You may only end up dehydrated or with a urinary tract infection.
Wear incontinence pads until the problem improves, and contact Dedicated to Women if additional care is needed.
Other Options to Treat Urinary Incontinence After Childbirth
Kegel exercises help to strengthen the pelvic floor muscles and can be performed anywhere. The simplest explanation to this easy exercise is to stop the flow of urine by squeezing the muscles tightly, holding for 5 seconds, and then continuing to urinate. Do these squeezes several times per day for maximum benefit.
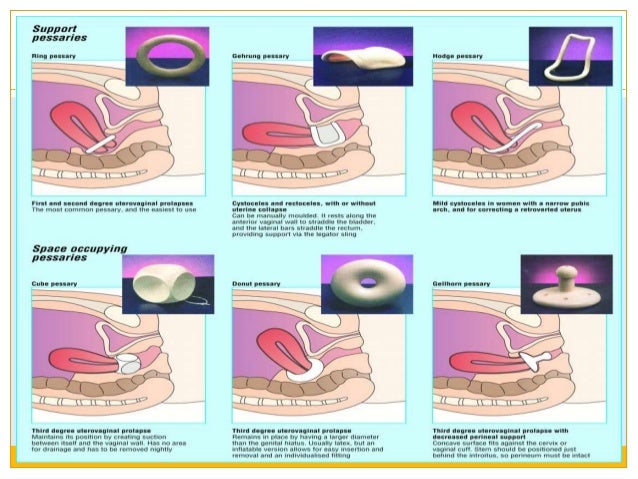
A pessary is a small silicone ring inserted into the vagina in the morning and removed each night. This device is designed to stop the flow from a woman’s urethra, and may remain in place all day or only during more strenuous activities if desired.
Sticking to a fixed bathroom schedule will help control your bladder. Try to stretch out the time between trips to the bathroom and build up your tolerance gradually.
Certain prescription medications can slow down an overactive bladder. Dedicated to Women ObGyn will be able to recommend and prescribe the medications they feel will work best for you and your specific symptoms of urinary incontinence.
There are other treatments that include both non-invasive and surgical methods to help women achieve relief from symptoms of urinary incontinence after childbirth.
Speak with Dedicated to Women if you still are having incontinence issues beyond 6 weeks after the birth of your child.
As always, if you have any further questions or would like to schedule an appointment, please call (302) 674-0223 today!
Incontinence After Childbirth | CU Urogynecology
Incontinence after childbirth at a glance
- During pregnancy and after childbirth, many women experience at least some degree of involuntary urination, called urinary incontinence.
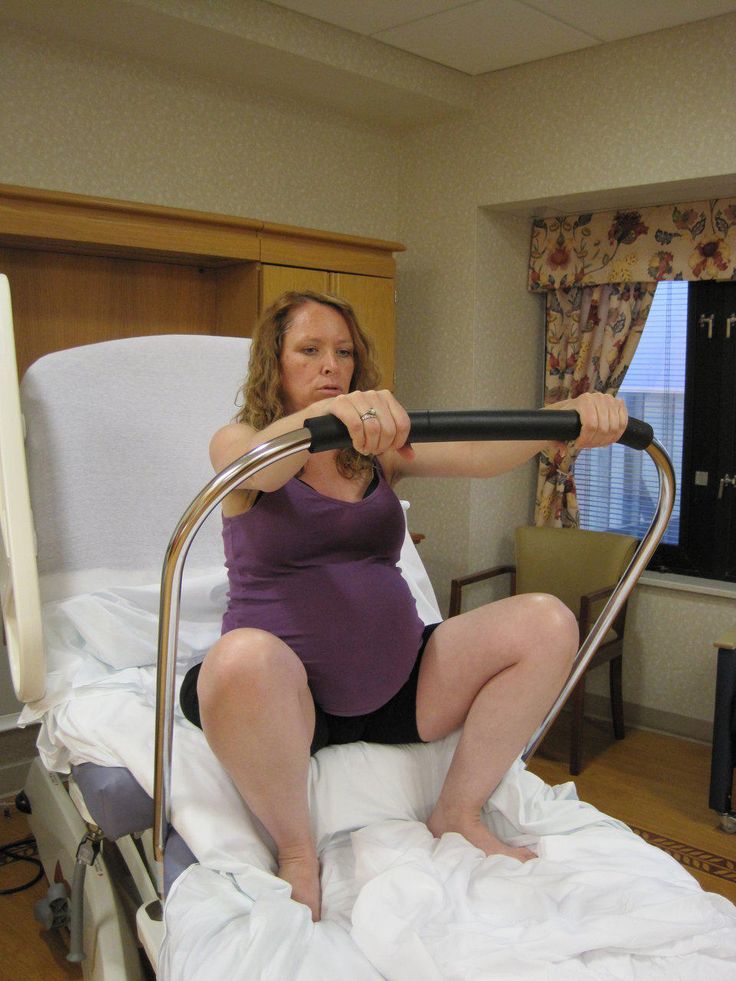
- Some women also experience bowel (fecal) incontinence, which is involuntary loss of fecal matter.
- Many factors can contribute to postpartum incontinence, including the baby passing through the birth canal during delivery, the increased weight of the uterus during pregnancy, and the unique hormones produced in pregnancy.
- Genetics and lifestyle factors, such as smoking, also play a role in a woman’s likelihood of developing incontinence after pregnancy.
- Women with a higher body mass index (BMI) during and after pregnancy have a higher chance of incontinence after childbirth.
- Women who delivered their child naturally have a 50% greater chance of developing incontinence after childbirth than women who had a Caesarean delivery.
- First line treatments for incontinence depend on individual circumstances, but can include strengthening exercises (Kegels), bladder training, nerve modulation, pelvic floor therapy, electrical stimulation to improve pelvic floor muscle contraction, or a pessary.

- If after childbirth symptoms have not resolved with first line treatments, surgery can be used to treat incontinence.
What is postpartum incontinence?
During and following pregnancy, as many as 4 in 10 women experience urinary incontinence, or the involuntary loss of urine. Despite the normalcy of incontinence after childbirth, many new mothers may feel shame or embarrassment about this change in their bodies.
The lack of dialogue about incontinence in many communities also leads some women to assume that this is an issue with no easy solutions. Truthfully, incontinence is not only very common, but also responds to a number of noninvasive treatment options that can greatly improve or eliminate symptoms.
There are several types of urinary incontinence, but most postpartum women experience stress incontinence. Laughing, coughing, sneezing, jumping and other activities can put extra pressure on the bladder sphincter, the muscular valve at the bottom of the bladder that controls urine flow. This pressure can lead to urine leakage, or stress incontinence, during those activities.
This pressure can lead to urine leakage, or stress incontinence, during those activities.
Giving birth is extremely tough on the body and can change a woman’s urinary control abilities. During pregnancy, the weight of the expanding uterus can weaken the strength of a woman’s pelvic floor muscles and cause urine to leak.
Giving birth can also affect those same muscles. Symptoms of incontinence may persist even after delivery. Hormones, genetics and other lifestyle factors, like smoking, can also make it more likely that a woman will experience incontinence after childbirth.
If you’re experiencing bladder control issues after pregnancy, our female pelvic health specialists can help you find relief.
Make an Appointment
The following conditions may also add to postpartum bladder control problems
- Damage to the nerves that control the bladder, rectum and pelvic floor muscles.
- Movement of the urethra and bladder from their usual position.

- Having an episiotomy or experiencing a tear in the pelvic floor muscle during delivery.
- Undergoing an assisted vaginal delivery with either forceps or a vacuum, which can damage the pelvic floor and anal sphincter, leading to urinary or fecal incontinence.
Read Stacy’s story on how surgery helped her return to running after giving birth to her son.
Incontinence is common in new moms but can also develop in the months and years after childbirth – some women don’t experience problems until their 40s. Whenever postpartum incontinence issues begin to develop, women should consider making an appointment with a female pelvic health specialist. We offer many treatment options that can improve the mother’s quality of life.
Sorry diamonds, Kegels are a girl’s best friend
Doing regular Kegel exercises will strengthen the pelvic floor muscles and can help to prevent urinary incontinence after childbirth. We have many resources all about Kegels including how to do them and how often, exercise tips and more.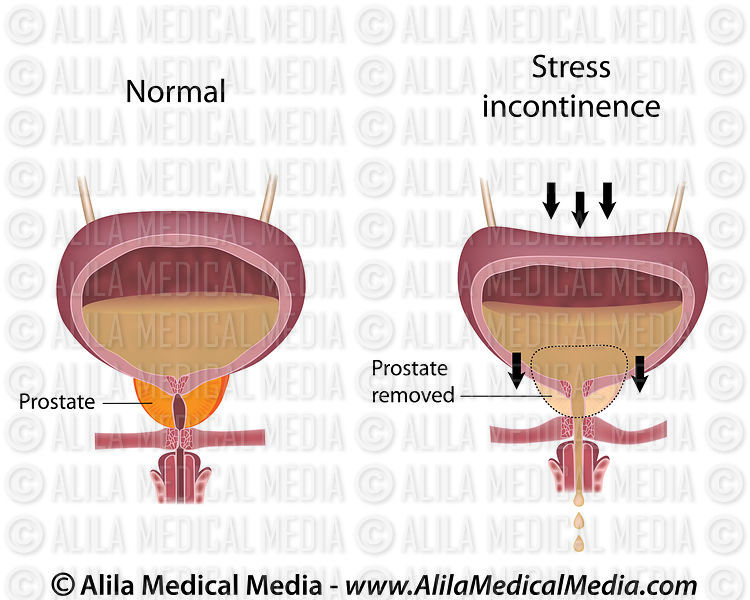
Visit the Kegel Corner
Risk factors for incontinence after childbirth
Women are more likely to have incontinence if they also had leakage problems during pregnancy, particularly in the first or second trimester. Women who also had long deliveries or needed forceps during labor are also more likely to experience urinary leakage.
According to the National Institutes of Health, women who have a natural delivery are 50% more likely to experience incontinence than women who deliver by C-section.
Women with a high BMI, or those who retain pregnancy weight gain after the birth of their child(ren), are more likely to experience incontinence and pelvic organ prolapse (POP) after giving birth. Postpartum weight loss decreases the risk of urinary incontinence, even if other risk factors such as age and/or type of delivery method exist.
When should women see a doctor about postpartum incontinence?
Women should talk to their doctor or a female pelvic health specialist six weeks after delivery if they had incontinence before, during or after pregnancy. Regular, unintended urine leakage may mean a woman has another medical condition. The loss of bladder control should be treated sooner rather than later, or it can become a long-term problem.
Regular, unintended urine leakage may mean a woman has another medical condition. The loss of bladder control should be treated sooner rather than later, or it can become a long-term problem.
Episiotomy considerations
We have a postpartum pelvic floor program uniquely designed to help women who experienced third- and fourth-degree anal sphincter lacerations during delivery. Women will meet with our pelvic floor physical therapists and begin therapy treatment 6-8 weeks post-delivery.
Make an Appointment
Postpartum incontinence treatments
The good news in regard to incontinence after childbirth is that there are many treatment options. Some common treatment options are listed below.
- Diet and exercise. Food and drinks such as coffee, citrus, spicy foods and soda can all irritate the bladder. Cutting back on or eliminating these foods may help improve incontinence symptoms. Keeping weight within a healthy BMI range, and/or focusing on losing pregnancy weight, can also help with bladder control.

- Special exercises. Kegels strengthen the pelvic floor, giving more control over urinary urges. Visit our Kegel Corner to learn more.
- Physical therapy. Pelvic floor physical therapy can also help build muscle memory and strength. The abdominal muscles, hip muscles and pelvic floor muscles work together when a woman performs strengthening exercises like Kegels. Physical therapists identify areas of weakness in those muscle groups to help a woman build a strong core and pelvic floor.
- Bladder training. The bladder is a muscle that should be regularly strengthened. Scheduling urination times and then gradually increasing the amount of time in between urination can increase bladder strength.
- Percutaneous tibial nerve stimulation (PTNS). PTNS is a nonsurgical treatment for overactive bladder and a form of neuromodulation therapy. During PTNS treatments, a doctor places a slim needle in the ankle where the tibial nerve is located.
 The needle delivers electrical impulses to the tibial nerve, which sends signals to the sacral nerves in the spine that control bladder and pelvic floor function. Over time, these pulses block nerve signals that are not working properly to lessen urinary incontinence symptoms.
The needle delivers electrical impulses to the tibial nerve, which sends signals to the sacral nerves in the spine that control bladder and pelvic floor function. Over time, these pulses block nerve signals that are not working properly to lessen urinary incontinence symptoms. - Evaluating lifestyle factors. Excessive coughing due to smoking or being overweight can put unnecessary strain on the pelvic floor muscles. Certain drugs such as antidepressants and antihistamines can also have an impact on urinary incontinence.
- Pessary. A pessary is a device inserted into the vagina to provide support for vaginal tissues, in turn, aiding in bladder incontinence.
- Surgical treatments. Surgical treatment options can help support the pelvic floor and may be recommended for women who have completed childbearing and have not had success with conservative therapy.
View all incontinence treatments at the bottom of our Urinary Incontinence page.
In many cases, women with postpartum incontinence see significant improvement after implementing a doctor’s recommended lifestyle changes. Women may also see their symptoms completely resolve by maintaining a healthy routine and losing any extra post-pregnancy weight.
The important thing for women to know is that incontinence after childbirth does not need to be a daily part of their lives as moms. There are attainable solutions, and all they often require is taking the first step of asking for help.
Urinary incontinence and other health issues after childbirth - Useful articles
There are two types of incontinence: in one case it is associated with an irresistible urge (as they say, "did not reach the toilet"), in the other case, involuntary urination occurs when intra-abdominal pressure increases during exercise , laughing, coughing, sneezing, etc. There may be mixed forms. The symptom of this disease is frequent urination more than 8 times during the day and 2 times at night, pain, leakage of urine and "urgency" - a feeling that urination will begin now. The causes of the disease can be different: inflammatory diseases of the pelvic organs, injuries after childbirth, concomitant neurological, endocrine and other somatic diseases.
The causes of the disease can be different: inflammatory diseases of the pelvic organs, injuries after childbirth, concomitant neurological, endocrine and other somatic diseases.
The problem in most cases is not resolved by itself, causing physical and psychological inconvenience and suffering (the need to walk around with pads and diapers) and reducing the quality of life, including intimate life. They are embarrassed to talk about it, and compared to how many people are prone to this problem, only a few seek help. Often they simply do not know who exactly to turn to - they go to a gynecologist, and to a therapist, and to a neuropathologist, while this should be done comprehensively and always with the participation of a urologist.
Therapeutic exercise for incontinence
In women after childbirth, disorders of vascular circulation and nervous regulation in the pelvic area are not uncommon. If there was a difficult birth, a large fetus, tears, stitches, then the prevention of incontinence should be started immediately, strengthening and restoring the muscles of the pelvic floor, nervous regulation and blood circulation. It is better, of course, to do this before pregnancy. Kegel exercises not only help to cope with involuntary urination, but also increase voluntary control over sexual reactions.
It is better, of course, to do this before pregnancy. Kegel exercises not only help to cope with involuntary urination, but also increase voluntary control over sexual reactions.
1. Slow contractions: tighten the muscles as if to stop urination, slowly count to three. To relax.
2. Contractions: tense and relax these same muscles as quickly as possible.
3. Push-ups: tense the perineum and abdominal muscles.
Special therapeutic exercises also help to strengthen the muscles of the small pelvis.
1. I.P. lying on your back. We exhale, draw in the stomach, pull the knees to the chest.
2. I.P. Same. Alternately raise straight legs and make circular movements out and in with full amplitude.
3. From the same position, on exhalation, pull up the chest with bent knees and clasp them with your hands.
4. Now raise the upper body and sit down, wrapping your arms around your knees.
5. At the expense of 1-2-3, lift the upper body and one leg, to which we reach with the same hand. We go down to count 4.
We go down to count 4.
6. Knees bent. At the expense of 1-2-3, we raise the pelvis, squeeze the buttocks, retract the anus. On the count of 4, lower the pelvis and relax.
7. From the same position, we lay bent knees to the right and left of the body.
8. I.P. standing, with support. On the inhale we rise on our toes, on the exhale we squat, holding on to the chair.
9. In the same position, holding onto the support, perform a roll from socks to heels and back.
10. I.P. On knees. Sit on your heels, stretch your arms up.
11. From the same position, alternately straighten the legs and pull them back. Shoulders-back-leg at the same time form one straight line.
12. Standing on all fours, alternately pull opposite arm and leg: straighten on the count of times, hold 2-3, return to the starting position on the count of 4. Be careful not to arch your back.
13. From the same starting position on count 1 stretch one leg back, on count 2-3 take it to the side parallel to the floor, bending at the knee, on count 4 return to the starting position.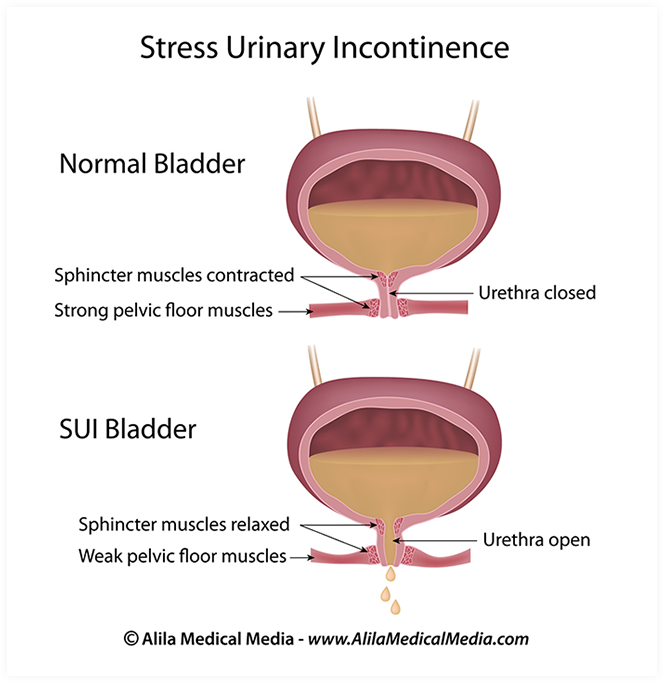
14. I.P. hands on the belt, one foot is on the chair. We lean forward and reach for the raised leg, bending it at the knee as much as possible.
There is no need to despair: although treatment is not a simple process due to the large number of components involved in the formation of this syndrome, it is very effective. In all cases, it begins with conservative methods: medicines, physiotherapy and, of course, the therapeutic exercises we have already mentioned. Refrain from activities that increase intra-abdominal pressure. If conservative treatment does not help, low-traumatic surgical methods come to the rescue in the form of imposing various types of loops.
Problems in the perineum
During childbirth, injuries to the soft tissues of the perineum are possible. Doctors pay special attention to this, but the woman herself should be engaged in prevention throughout the pregnancy. First of all, this is gymnastics, which prepares the muscles of this area for the birth load. Cure inflammatory processes that reduce the elasticity of the perineum (they include thrush), be careful with nutrition: an excess of sweet and starchy foods, especially in recent months, lead to an increase in the size of the fetus, increasing the risk of trauma, which then backfires problems in sexual life.
Cure inflammatory processes that reduce the elasticity of the perineum (they include thrush), be careful with nutrition: an excess of sweet and starchy foods, especially in recent months, lead to an increase in the size of the fetus, increasing the risk of trauma, which then backfires problems in sexual life.
Sometimes an episiotomy is done for the benefit of the baby and mother. Healing is very fast due to tissue matching and a powerful hormonal explosion. The main task of the mother, if she has stitches, is to keep them clean. This, of course, is hygiene (washing twice a day, from front to back, you can use a decoction of chamomile or a weak solution of potassium permanganate) and ensuring oxygen access. Associated with the latter is the ban on underwear and pads, which causes violent protest among women in maternity hospitals.
One should not underestimate such an important moment as the normalization of the stool on the third day after childbirth. Defecation does not provoke the divergence of the sutures, on the contrary, this stool retention can lead to trouble, so try to achieve a soft and spontaneous stool by the third day, and upon returning from the hospital, consult a doctor to make sure that the sutures are healing correctly, without divergence and suppuration.
Uterus and vagina
Some women who have recently given birth complain of vaginal gaping, even asking to "sew it up so that it was like before." Bringing the vaginal ring back to normal is really very important, but this process takes some time. During childbirth, the vagina stretches to let the baby through. Closing occurs within six months, which can be accelerated, for example, by the already mentioned Kegel exercise or the mixing-breeding of the legs.
Immediately after delivery, the uterus should empty well, so turn over, give a vertical load. This will improve blood flow, help her take a central position. Any exercises on the press are possible only after the complete cessation of secretions, otherwise an increase in intra-abdominal pressure increases the risk of resumption of bleeding. You can do it 6-8 weeks after giving birth in a prone position so as not to strain the muscles of the pelvic floor. But sitting in the hospital, especially if you have stitches, is not necessary - it is better to eat while standing, and to feed the baby - lying down.
The return of the tone of the soft tissues of the perineum will also be helped by sexual intercourse, which improves tissue nutrition. Please note: they are allowed when the placental site has been restored in the uterine cavity and there is no longer a risk of inflammation. If you feel pain during intercourse, do not hesitate to tell the doctor about it - he will find out the reason and advise the appropriate position.
Hemorrhoids
Another problem after the birth of a baby is hemorrhoids - a frequent manifestation of varicose veins. If hemorrhoids appear after childbirth, carefully observe them during the first days. Applying cold and topical application of anti-hemorrhoidal agents will help. Remember that the use of drugs after childbirth is limited, so it is necessary to deal with hemorrhoids that have appeared, if necessary, contacting a proctologist.
We hope that you will not be at a loss even if you encounter any of the above troubles and that you will definitely deal with them as soon as possible. Happy and trouble-free motherhood to you!
Happy and trouble-free motherhood to you!
Urinary incontinence in women after childbirth.
Article
Ilyina Irina Yuryevna
Acusher-gynecologist, candidate of medical sciences, the Department of Acusherity and Gynecology of the Moscow Faculty of the RSEM, chief physician of medical clinic ".
Urinary incontinence in women after childbirth.
The problem of urinary incontinence is one of the most common diseases among women.
The International Society for the Study of Urinary Continence (1974) defined urinary incontinence as a condition in which involuntary loss of urine is a social and hygienic problem and is objectively confirmed.
There are several types of urinary incontinence. In women after childbirth, stress urinary incontinence is most common, another name for this pathology is stress urinary incontinence. This is the involuntary release of urine that occurs when the pressure inside the bladder rises above the pressure in the urethra (urethra).
This is the involuntary release of urine that occurs when the pressure inside the bladder rises above the pressure in the urethra (urethra).
The cause of stress urinary incontinence is a violation of the function of the sphincter apparatus of the bladder and urethra, which occurs when their normal relationship changes.
Normally, in a standing woman, the bladder neck and the initial section of the urethra are located in the abdominal cavity above the pelvic floor, so the pressure in the urethra is equal to or greater than the pressure in the bladder. With various violations of the normal anatomical relationship between the bladder and the urethra, with an increase in intra-abdominal pressure (when coughing, sneezing, lifting weights), urine leakage is observed.
According to the severity of clinical symptoms, three degrees of urinary incontinence are distinguished (Kan D.V., 1986): mild (minimal symptoms of urinary incontinence with significant physical exertion), moderate (involuntary release of urine occurs during laughter, coughing or brisk walking) , severe urinary incontinence (involuntary excretion of urine occurs when changing body position or even during sleep).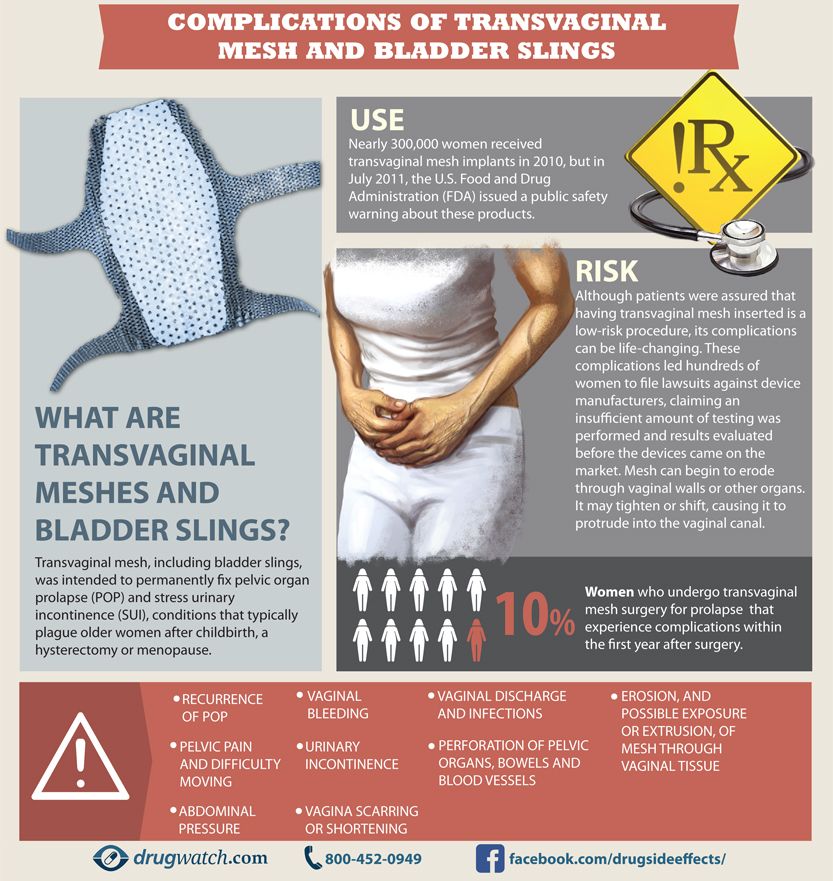
The most common cause of this pathology is pathological childbirth (rapid or protracted) - 51.1% - resulting in the development of traumatic and trophic disorders in the walls of the urethra and bladder neck (hematomas, areas of ischemia, tears of muscle fibers), in the future their atrophy and replacement with connective tissue occur, elastic properties are violated. Severe physical activity - 20.6%, associated with a prolonged increase in intra-abdominal pressure, leads to weakening of the ligamentous apparatus of the pelvic floor, disruption of anatomical and functional relationships. However, it should be emphasized that physical overexertion alone rarely leads to urinary incontinence. The disease arises from a number of other reasons, and under the influence of physical activity and inflammatory processes in the genitourinary organs progresses. Hormonal disorders - 15.6% - a decrease in estrogen synthesis that occurs in postmenopause. Operations on the pelvic organs - 12. 7% - traumatize muscle formations, develop cicatricial changes in tissues, leading to a shortening of the anatomical and functional length of the urethra.
7% - traumatize muscle formations, develop cicatricial changes in tissues, leading to a shortening of the anatomical and functional length of the urethra.
Thus, urinary incontinence is a serious medical and social problem that has an extremely negative impact on the psychological state of patients. Studying the psycho-emotional status of women suffering from urinary incontinence, Stanton (2000) noted that more than 38% of patients have a mental disorder of a functional nature. Emotional disturbances were manifested by increased irritability, depression and sexual problems.
Many women believe that urinary incontinence develops with age, and almost all experience these symptoms over the years. Indeed, the pelvic floor undergoes significant changes over the years, the urethra-bladder ratio changes, which can lead to the development of symptoms of urinary incontinence, but it is wrong to say that all women are prone to this condition.
Probably, at some stage in the life of every woman there is a change in the pelvic floor, which may be after childbirth, gynecological interventions or during menopause. This leads to changes in the relationship between the bladder and the urethra and it takes some time for the pelvic organs to adapt to the "new" anatomical situation. In the case when this does not happen, the development of symptoms of urinary incontinence is possible.
This leads to changes in the relationship between the bladder and the urethra and it takes some time for the pelvic organs to adapt to the "new" anatomical situation. In the case when this does not happen, the development of symptoms of urinary incontinence is possible.
Among the conditions associated with urinary incontinence, vaginal pelvic organ prolapse has the greatest clinical significance. The problem of prolapse and prolapse of the vagina and uterus continues to be relevant. Prolapse of the uterus is the position of this organ when the cervix is located below the interspinal line. When prolapsed, the uterus goes beyond the genital gap completely (complete prolapse) or partially, sometimes only the cervix (incomplete prolapse).
This disease is caused by congenital or age-related deficiency of the connective tissue, as well as failure of the pelvic floor muscles, which in most cases occurs due to damage to the muscles of the perineum and pelvic diaphragm during childbirth, with a prolonged increase in intra-abdominal pressure due to hard physical work, with chronic lung diseases, constipation . Surgical treatment.
Surgical treatment.
A thorough history and examination is essential in the diagnosis of urinary incontinence. It is important to clarify questions about the duration and severity of incontinence and past attempts to surgically eliminate stress urinary incontinence; it is important to find out the presence of any neurological diseases or diseases of the internal organs that underlie or contribute to urinary incontinence.
A questionnaire, voiding diary, is used, which is important for quantifying and documenting the amount of urine lost. The diary should record fluid intake and urine output, urination time, and any physical activity associated with episodes of urinary incontinence. A urination diary is kept for 48-72 hours.
| Time of day | Drinking volume (ml) | Excreted volume (ml) | Episodes of urine loss (ml) | What were you doing? |
|
|
|
|
|
|
Urodynamic studies play a significant role in the diagnosis of urination disorders and monitoring the effectiveness of treatment.
Severe to moderate stress urinary incontinence is treated surgically. With a mild degree of urinary incontinence, conservative treatment is possible. Therefore, it is very important to contact a specialist in time in order to start treatment in a timely manner.
The complex of conservative treatment of stress urinary incontinence includes training of the pelvic floor muscles. The key principle of this effect is repeated voluntary contractions of the pelvic floor muscles, which improves their tone, and also facilitates the muscle contraction reflex in response to an increase in intra-abdominal pressure. These exercises in some cases allow you to restore the pelvic muscles and minimize urine loss. The level of success depends on the severity and type of incontinence. The best results are achieved in patients with mild symptoms and well-preserved pelvic floor muscles. Their tone is assessed by a gynecologist during the study quite easily. You can also use specific vaginal cones. The kit includes several cones of various weights, as certain results of treatment are achieved, the mass of the applied cone gradually increases. Exercises are carried out 10 times for 30 seconds every hour. For an adequate assessment of the effectiveness of treatment, it must be carried out for at least 8-12 weeks. These are the treatments that a woman can independently carry out at home.
The kit includes several cones of various weights, as certain results of treatment are achieved, the mass of the applied cone gradually increases. Exercises are carried out 10 times for 30 seconds every hour. For an adequate assessment of the effectiveness of treatment, it must be carried out for at least 8-12 weeks. These are the treatments that a woman can independently carry out at home.
There are also other conservative treatments such as negative feedback pelvic floor muscle training, electrical stimulation.
Urinary incontinence is a complex medical, hygienic and social problem. Therefore, assistive devices used to correct incontinence play an important role in many situations - in preparation for surgical treatment, as well as during rehabilitation after it, when training the bladder and pelvic floor muscles. They enhance the social adaptation of this category of women and solve most of the hygiene problems caused by the negative effect of urine on the skin.
Modern devices (pessaries, urethral obturators) are effective means of preventing stress urinary incontinence for a long time. They do not have serious side effects and subjective inconveniences. However, there is a small percentage of violations of the integrity of the vaginal epithelium, including erosion and polyps, which can also sometimes lead to infection of the urinary tract.
They do not have serious side effects and subjective inconveniences. However, there is a small percentage of violations of the integrity of the vaginal epithelium, including erosion and polyps, which can also sometimes lead to infection of the urinary tract.
Women rarely turn to specialists because are embarrassed and many of them believe that this phenomenon is quite natural and every woman ever notes the symptoms of urinary incontinence. At the same time, some are skeptical about the possibility of treatment by a specialist, because. do not believe in the effectiveness of the treatment of this pathology. Lots of sick people put off
a visit to the doctor until the manifestations and severity of the disease interfere with their daily lifestyle and work.
Once again, we note that timely access to specialists and the early start of conservative treatment of urinary incontinence largely determines the success of treatment. In order to shorten the examination time and facilitate your first communication with the doctor, we suggest that you fill out the urination diary above and a questionnaire that includes 28 questions reflecting the possible causes of urinary incontinence, the nature of complaints, the duration of the disease, the number of births, their course, the effectiveness of conservative and surgical treatment (if any), the function of the bladder, urethra and rectum.