How many abortion can you have in a year
Repeat Abortion, Repeat Unintended Pregnancy, Repeated and Misguided Government Policies
About half of all U.S. women having an abortion have had one previously. This fact—not new, but dramatically underscored in a recent report from the Guttmacher Institute on the characteristics of women having repeat abortions—may surprise and concern some policymakers, even prochoice ones. However, policymakers should be more disturbed by the underlying fact that the unintended pregnancy rate in the United States is so high, and that so many women experience repeat unintended pregnancies. Some of these pregnancies end in abortion and some end in unintended births. Indeed, it is not uncommon for a woman to experience both of these outcomes, as well as one or more planned births, during her lifetime.
Reducing repeat abortion must start with reducing repeat unintended pregnancy, which goes back to the basic challenge of helping women prevent unintended pregnancies in the first place. In that regard, the almost 7,500 family planning clinics across the country certainly are doing their share, given that unintended pregnancy prevention is their primary mission. Beyond that, both abortion providers and providers of services to women giving birth also contribute, since contraceptive counseling and the provision of a birth control method upon request are standard components of high-quality postabortion and postpartum care.
Strengthening the linkages between services and between providers would seem to be key, however, if the overall goal is to enable women to better manage their reproductive lives and better plan whether and when to have a child or another child. But fostering continuity of care between abortion clinics and contraceptive services programs might be easier said than done. The contentious politics of abortion and the culture wars associated with it have led to the isolation of abortion as a medical service and to the stigmatization of both abortion clients and providers. Indeed, particularly for young and low-income women among whom unintended pregnancy and recourse to abortion are especially common, state and federal government policies over the last 25 years have only exacerbated the situation, by consciously driving wedges between providers of publicly subsidized contraceptive services and facilities providing abortions.
Abortion vs. Repeat Abortion
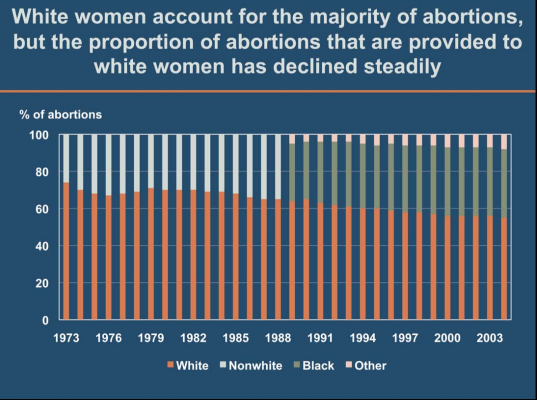
Although not widely recognized, the U.S. abortion rate reached its height in the early 1980s and has been drifting downward ever since. Over the last few years, however, the decline would appear to have stalled. At the current rate, about one-third of all U.S. women will have had an abortion by age 45. Certain groups are overrepresented among women having abortions: those who are young, poor or near-poor, black, Hispanic or unmarried, and those who already have had one child. Fifty-four percent of women having abortions used some method of contraception during the month they became pregnant. The tiny sliver of all sexually active women not practicing contraception (11%) accounts for the remaining half of all abortions.
According to the 2006 Guttmacher Institute report Repeat Abortion in the United States, women having a second or higher-order abortion are substantially different from women having a first abortion in only two important ways: They are more than twice as likely to be age 30 or older and, even after controlling for age, almost twice as likely to already have had a child. (Among all women having an abortion, six in 10 are mothers.)
(Among all women having an abortion, six in 10 are mothers.)
Just as with women having their first abortion, however, the majority of women having their second or even their third abortion were using contraceptives during the time period in which they became pregnant. In fact, women having a repeat abortion are slightly more likely to have been using a highly effective hormonal method (e.g., the pill or an injectable). This finding refutes the notion that large numbers of women are relying on abortion as their primary method of birth control. Rather, it suggests that women having abortions—especially those having more than one—are trying hard to avoid unintended pregnancy, but are having trouble doing so.
More effective conraceptive use would help women reduce their risk of unintended pregnancy, which in turn would lead to fewer abortions (including fewer repeat abortions) and fewer unintended births.
Moreover, according to the Guttmacher analysis, women at risk of having a repeat abortion share many of the same characteristics as women at risk of having a repeat unintended birth, including age, number of prior births, and race and ethnicity.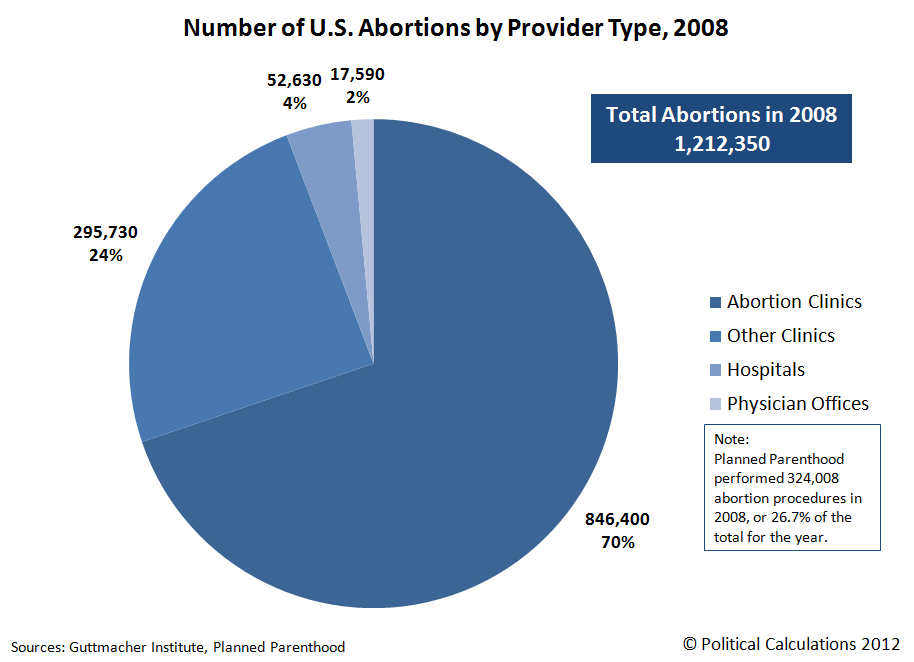 The associations with race and ethnicity, as well as poverty, are particularly striking among women having repeat unintended births: Almost half of black women and about 40% of poor and low-income women have had at least one unintended birth.
The associations with race and ethnicity, as well as poverty, are particularly striking among women having repeat unintended births: Almost half of black women and about 40% of poor and low-income women have had at least one unintended birth.
Indeed, unintended births are as common among U.S. women as is abortion: Almost one-third of all women aged 15–44 report having had at least one unintended birth. A minimum of four in 10 women of reproductive age have had at least one unintended pregnancy, whatever the outcome. Accordingly, as stated in the Guttmacher report, "it is possible, if not likely, that women who have had a prior abortion have also had other unintended pregnancies, some of which they carried to term."
Clearly, more effective contraceptive use would help women reduce their risk of unintended pregnancy, which in turn would lead to fewer abortions (including fewer repeat abortions) and fewer unintended births. To improve contraceptive use, a woman first needs good counseling, which will increase her chances of selecting the contraceptive method that is right for her at that particular time in her life. Then she needs easy and affordable access to her chosen method and to the necessary services to support her choice over time. Although having good access to contraceptive services is important for all sexually active women, it seems especially important for women having abortions and women giving birth (whether intended or unintended), who constitute a self-selected group—perhaps a high-risk one at that.
Then she needs easy and affordable access to her chosen method and to the necessary services to support her choice over time. Although having good access to contraceptive services is important for all sexually active women, it seems especially important for women having abortions and women giving birth (whether intended or unintended), who constitute a self-selected group—perhaps a high-risk one at that.
Walls of Separation
From the time that the U.S. Supreme Court legalized abortion nationwide in 1973, antiabortion activists inside and outside government turned their attention to making abortion services harder to obtain, rather than on making the unintended pregnancies that precede almost all abortions less likely. A central component of that effort, based on the notion that family planning clinics serve as funnels for abortion clinics, has been a doggedly pursued campaign to erect "walls of separation" between the two. At both the state and federal levels with varying degrees of success, antiabortion activists have sought to block organizations that receive public funds for family planning from providing problem pregnancy counseling that includes any discussion of the option of abortion, making abortion referrals even upon direct request, engaging in abortion rights advocacy and providing abortion services at all.
A spate of such separation requirements were enacted at the state level in the late 1970s but were blocked by the courts. With the election of Ronald Reagan in 1981, activists turned to the federal government and set their sights first on U.S. foreign policy, over which the president is given significant discretion. In 1984, the Reagan administration unveiled the "Mexico City" policy (named for the location of the international population conference at which it was first announced), which did not require congressional approval or even authority. The policy disqualifies indigenous organizations in developing countries from eligibility for U.S. family planning aid if they use other, non–U.S. government funds to provide abortions or abortion-related counseling, referrals or advocacy. In 1993, President Clinton rescinded the policy, which has come to be widely known as the global gag rule, but President Bush reimposed it in 2001.
Having successfully restricted international family planning programs, the Reagan administration in 1987 issued a similar gag rule for the Title X domestic family planning program. That regulation banned the "nondirective" problem pregnancy counseling that had been required in Title X programs, as well as abortion referrals for women who request them; it also called for physical and financial separation between a federally funded contraceptive services program and any privately funded abortion service. The courts blocked the domestic gag rule from going into effect until the U.S. Supreme Court upheld its constitutionality in 1991. The policy, however, was never fully implemented, and on his first day in office in January 1993, Clinton cancelled it (along with its international counterpart).
That regulation banned the "nondirective" problem pregnancy counseling that had been required in Title X programs, as well as abortion referrals for women who request them; it also called for physical and financial separation between a federally funded contraceptive services program and any privately funded abortion service. The courts blocked the domestic gag rule from going into effect until the U.S. Supreme Court upheld its constitutionality in 1991. The policy, however, was never fully implemented, and on his first day in office in January 1993, Clinton cancelled it (along with its international counterpart).
Just before leaving office, the Clinton administration replaced the Reagan-era regulation with guidelines that restored Title X's mandate to provide nondirective counseling and abortion referrals on request, but even these guidelines require Title X project activities to be "separate and distinguishable" from abortion-related services. In the intervening years, moreover, several states—notably, Colorado, Michigan, Ohio, Pennsylvania and Texas—have picked up where the federal government left off and have enacted laws or polices going much further than the Title X guidelines (see box).
Realities on the Ground
The putative goal of federal and state separation requirements is to sever ties going from family planning clinics to abortion providers. Indisputably, however, the consequences—both direct and indirect—have meant severed ties going in the other direction as well.
Both the National Abortion Federation (NAF) and Planned Parenthood Federation of America make clear through their respective clinical guidelines that an integral component of postabortion care includes the provision of information about contraception, as well as a contraceptive method, if requested. However, most free-standing abortion clinics (as opposed to Planned Parenthood clinics that also provide abortions), are not set up to provide ongoing, comprehensive contraceptive care. Rather, they have come to specialize in providing abortion-related care in response to the need that has arisen for this single-service approach. The reasons for this are several and interrelated, including the historic isolation of abortion services and providers by the "mainstream" health care system; the stigma associated with abortion, which deters women from wanting to return for ongoing health care; and the long distances many women must travel just to find an abortion provider.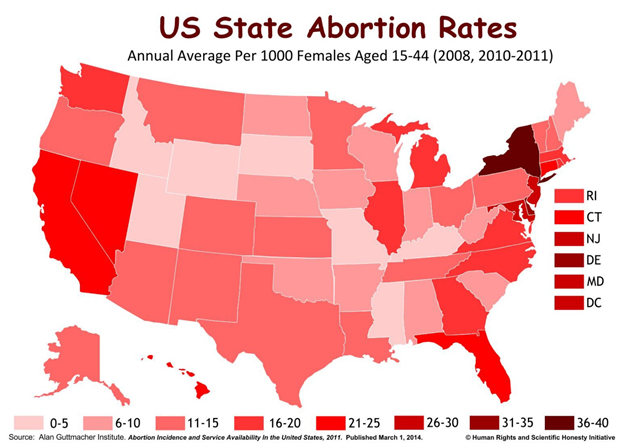
Basically, free-standing clinics are not comprehensive reproductive health care providers because of the lack of demand from their clients and because the existing providers, for better or worse, are doing all they can to keep up with the demand for abortion services. According to Rachel Falls, who directs NAF's abortion hotline, "a woman may be very pleased with the care she receives at the abortion clinic, but she is not there to build a relationship." Certainly, the stigma many women feel about having an abortion—emanating from family, friends, church, society at large or even themselves—can be a significant impediment to their wanting to return more than necessary.
'If only we didn't have these barriers, we would be able to provide an abortion patient with birth control on the spot, instead of her having to return for another appointment at our Title X clinic.'
Compounding the problem is the fact that the declining number of abortion providers has meant increasing numbers of women must travel longer distances to find one.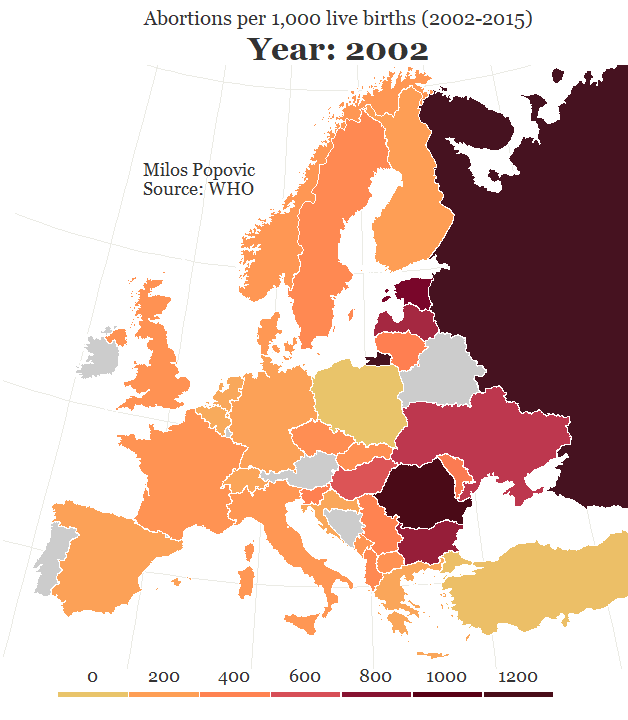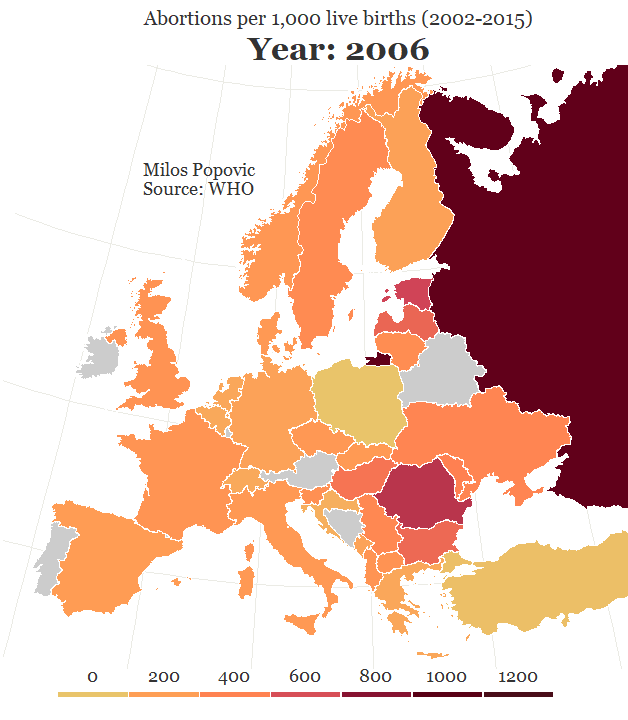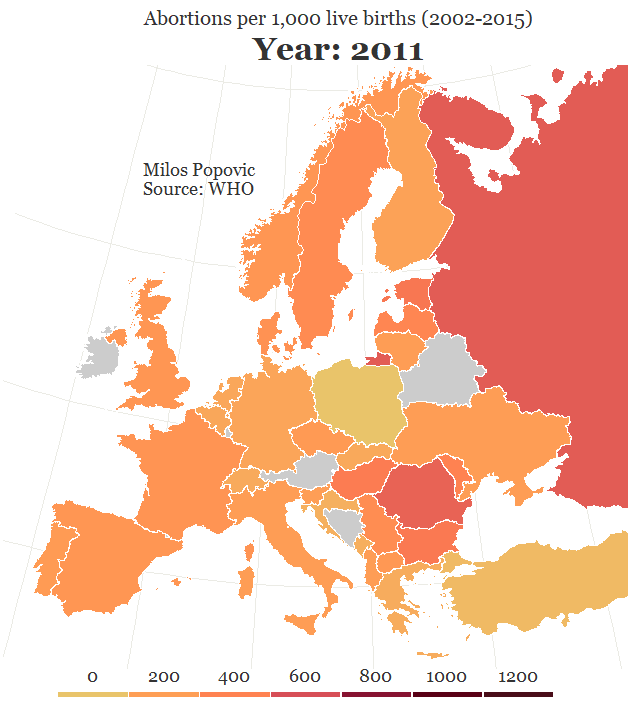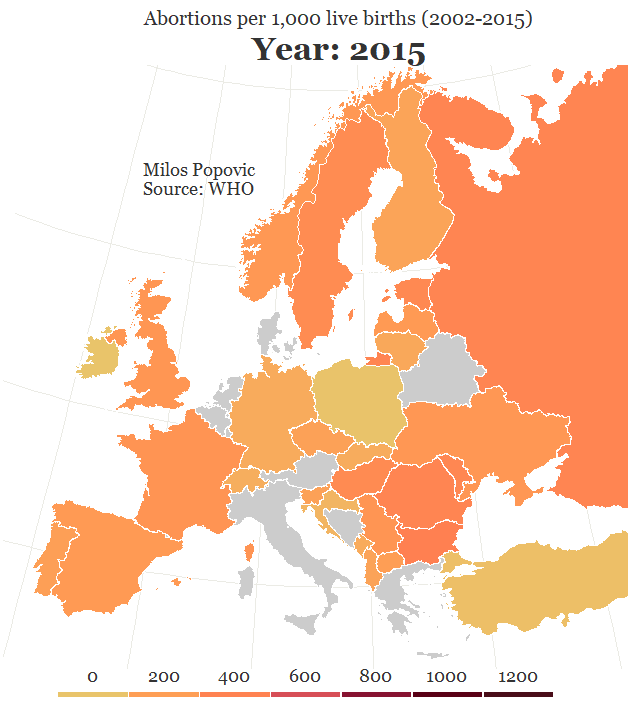 For example, in the case of the free-standing Hope Clinic for Women in Granite City, Illinois, more than half of the clients travel over 50 miles for abortion services, according to executive director Sally Burgess. The further a woman must travel (or for confidentiality reasons chooses to travel) to reach an abortion provider, the less practical it would be for her to consider that clinic for her regular source of reproductive health care.
For example, in the case of the free-standing Hope Clinic for Women in Granite City, Illinois, more than half of the clients travel over 50 miles for abortion services, according to executive director Sally Burgess. The further a woman must travel (or for confidentiality reasons chooses to travel) to reach an abortion provider, the less practical it would be for her to consider that clinic for her regular source of reproductive health care.
However, comprehensive models do exist, overwhelmingly among Planned Parenthood clinics. The Boulder Valley Women's Health Center in Colorado is a rare example of a comprehensive clinic not affiliated with Planned Parenthood that provides abortion services as well as Title X– funded contraceptive services. Executive Director Susan Levy observes that some abortion providers who might consider creating a family planning program are dubious about participating in Title X because of suspicion that the government rules would impinge on the quality of their abortion services program. Levy has managed to juggle both, she says, largely because she is operating in a favorable local political climate and because she has been able to garner additional public funding for her family planning program from local sources.
Levy has managed to juggle both, she says, largely because she is operating in a favorable local political climate and because she has been able to garner additional public funding for her family planning program from local sources.
Like the many Planned Parenthoods that both offer abortion services and operate Title X family planning programs, Boulder Valley has a strong commitment to overcoming political obstacles to make the system work for women as much as possible. Participating in the Title X program, however, does carry a cost. Levy notes, for example, that women who obtain an abortion at her agency must have a separate chart if they later return for ongoing, Title X–funded contraceptive services. The agency must scrupulously segregate the funds it uses for its abortion services and its Title X program.
Clearly, none of this promotes what should be an overriding interest in ensuring continuity of care, especially in the direction of helping a woman decrease her chances of having another abortion. "If only we didn't have these barriers," Levy explained, "we would be able to provide a low-income abortion patient with an appropriate and subsidized method of birth control on the spot, instead of her having to return for another appointment at our Title X clinic. We are operating our abortion clinic from a prevention mindset," she continued, "and that comes from being a family planning provider at the same time."
"If only we didn't have these barriers," Levy explained, "we would be able to provide a low-income abortion patient with an appropriate and subsidized method of birth control on the spot, instead of her having to return for another appointment at our Title X clinic. We are operating our abortion clinic from a prevention mindset," she continued, "and that comes from being a family planning provider at the same time."
Government's Role, for Good or Ill
Lebanon Valley Health Services in central Pennsylvania has been operating a prenatal clinic and a Title X–supported contraceptive services program at the same site since 1990. The agency's goal is two-fold: to facilitate early entry into prenatal care to improve pregnancy outcomes, and to ensure that their prenatal care clients, when returning for their postpartum visits, have direct access to a source of ongoing birth control information, services and support. The American College of Obstetricians and Gynecologists and the American Academy of Pediatrics encourage this approach. The federal Department of Health and Human Services embraces it too, noting in Healthy People 2010—the nation's official public health objectives—that "health care providers can help all new mothers understand that they can become pregnant again soon after delivery and should assist them with contraceptive education and supplies." By contrast, the federal government insists on separation between abortion and publicly subsidized contraceptive services.
The federal Department of Health and Human Services embraces it too, noting in Healthy People 2010—the nation's official public health objectives—that "health care providers can help all new mothers understand that they can become pregnant again soon after delivery and should assist them with contraceptive education and supplies." By contrast, the federal government insists on separation between abortion and publicly subsidized contraceptive services.
The historic isolation of abortion and abortion providers, which impedes continuity of care from abortion to contraception and which is reinforced by long-standing government policy, is clearly counterproductive.
This is short-sighted, at best. The fact is that for many if not most women, using contraceptives consistently and effectively over decades is not easy. But the records of other industrialized countries tell us that the United States can do much better than it is doing now. Indeed, it is challenging enough to design an approach to providing preventive health care that makes it easier for women—especially young and disadvantaged women—to be effective contraceptive users when life's other, more immediate priorities, such as housing, food, jobs and child care, often push contraception to the bottom of the list. The negative political climate surrounding abortion, contraception and sexuality in general in the United States does not help the situation.
The negative political climate surrounding abortion, contraception and sexuality in general in the United States does not help the situation.
Certainly, not every abortion provider needs to become a provider of comprehensive contraceptive services, or of Title X–supported subsidized services for low-income women. But the historic isolation of abortion and abortion providers, which impedes continuity of care from abortion to contraception and which is reinforced by long-standing government policy, is clearly counterproductive. Indeed, to the extent women are able to avail themselves of the services they need to help them prevent an unintended pregnancy, they benefit and society does too. This applies whether it is their first or a subsequent pregnancy and whether they are seeking services at an abortion clinic, in a postpartum care setting or at a family planning clinic. U.S. culture, politics and the health care system are all factors in how well this can ever work, but government has an important role to play as well. Ideally, it should be facilitating the linkages among these reproductive health and pregnancy-related services and providers. At a minimum, it should get out of the way.
Ideally, it should be facilitating the linkages among these reproductive health and pregnancy-related services and providers. At a minimum, it should get out of the way.
State 'Walls of Separation' Between Abortion and Contraceptive Services: Laws Currently in Effect
Colorado, Ohio and Pennsylvania
These three states have similar laws that ban the use of state funds for abortion counseling or referral. But they go far beyond that: They also disqualify entities from receiving any state family planning funds unless strict physical and financial separation exists between the family planning services and any abortion-related services. In Pennsylvania, hospitals and physicians participating in the Medicaid program are exempt from the requirement, however, leaving the law to apply mainly to Planned Parenthood affiliates.
Michigan
Michigan, likewise, bans any state funds from being used to counsel or refer for abortion, but Michigan has employed a unique twist to punish entities that use other funds for these purposes. Under Michigan's separation law, recipient agencies are ranked according to how many abortion-related "demerits" they have, with state and federal funding priority going to those with the fewest demerits. The offending activities include: providing abortion services (except to save a woman's life or in cases of rape or incest), providing abortion referrals, or maintaining in writing that "abortion is considered part of a continuum of family planning or reproductive health services."
Under Michigan's separation law, recipient agencies are ranked according to how many abortion-related "demerits" they have, with state and federal funding priority going to those with the fewest demerits. The offending activities include: providing abortion services (except to save a woman's life or in cases of rape or incest), providing abortion referrals, or maintaining in writing that "abortion is considered part of a continuum of family planning or reproductive health services."
Texas
In December 2006, the Texas Department of State Health Services received approval from the federal government to increase access to and participation in family planning services under the state's Medicaid program. The Texas legislature authorized the health department's waiver application, but not before adding a condition prohibiting any providers from participating in the Medicaid family planning expansion program that also "perform or promote elective abortions."
back to main text
Induced Abortion in the United States
Fact Sheet
Reproductive rights are under attack. Will you help us fight back with facts?
Will you help us fight back with facts?
Donate Now
The Guttmacher Institute recently published new data on abortion in the United States. As we work to update our fact sheets with the latest data, please be aware that some of the information below is out of date. In the meantime, please refer to the following resources for the most current facts on abortion in the United States:
Long-Term Decline in US Abortions Reverses, Showing Rising Need for Abortion as Supreme Court Is Poised to Overturn Roe v. Wade
Medication Abortion Now Accounts for More Than Half of All US Abortions
Roe v. Wade Overturned: Our Latest Resources
Lay of the Land: Abortion Policies and Access in the United States
- Eighteen percent of pregnancies (excluding miscarriages) in 2017 ended in abortion.1
- Approximately 862,320 abortions were performed in 2017, down 7% from 926,190 in 2014.
- The abortion rate in 2017 was 13.
 5 abortions per 1,000 women aged 15–44, down 8% from 14.6 per 1,000 in 2014.1 This is the lowest rate ever observed in the United States; in 1973, the year abortion became legal, the rate was 16.3.2
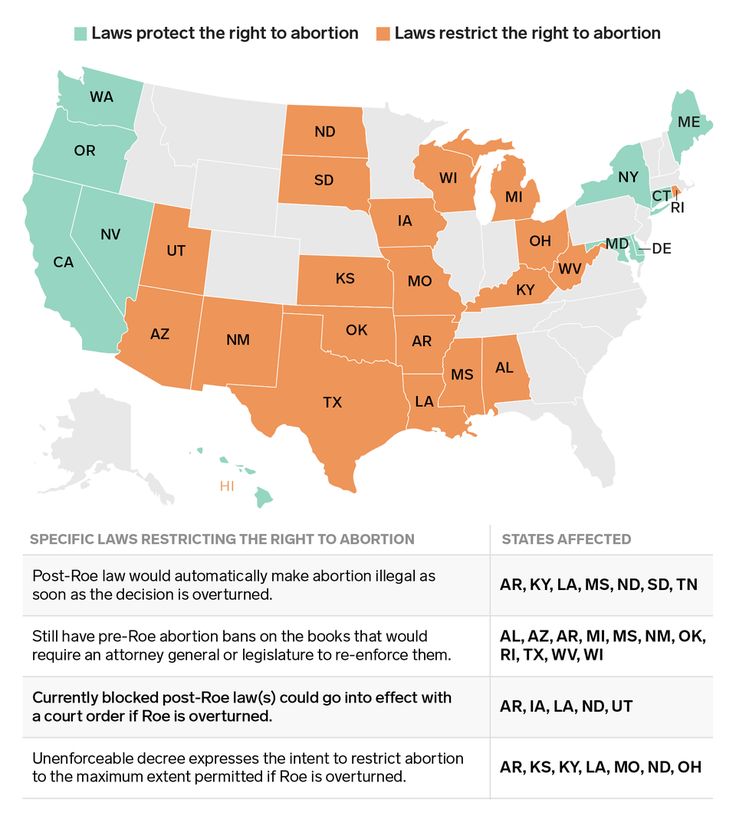
5 abortions per 1,000 women aged 15–44, down 8% from 14.6 per 1,000 in 2014.1 This is the lowest rate ever observed in the United States; in 1973, the year abortion became legal, the rate was 16.3.2 - As of September 1, 2019, 29 states were considered hostile toward abortion rights, 14 states were considered supportive and seven states were somewhere in between.3
- In 2019, 58% of U.S. women of reproductive age (nearly 40 million women) lived in states that were considered hostile to abortion rights. In contrast, 24 million women of reproductive age (35% of the total) lived in states that were supportive of abortion rights.3
WHO HAS ABORTIONS?
- At 2014 abortion rates, about one in four (24%) women will have an abortion by age 45.4
- More than half of all U.S. abortion patients in 2014 were in their 20s: Patients aged 20–24 obtained 34% of all abortions, and patients aged 25–29 obtained 27%.
 5
5 - Adolescents made up 12% of abortion patients in 2014: Those aged 18–19 accounted for 8% of all abortions, 15–17-year-olds for 3% and those younger than 15 for 0.2%.5
- White patients accounted for 39% of abortion procedures in 2014, black patients for 28%, Hispanic patients for 25%, and patients of other races and ethnicities for 9%.5
- Seventeen percent of abortion patients in 2014 identified themselves as mainline Protestant, 13% as evangelical Protestant and 24% as Catholic, while 38% reported no religious affiliation and the remaining 8% reported some other affiliation.5
- The vast majority (94%) of abortion patients in 2014 identified as heterosexual or straight. Four percent of patients said they were bisexual; 0.3% identified as homosexual, gay or lesbian; and 1% identified as "something else."5
- Fifty-nine percent of abortions in 2014 were obtained by patients who had had at least one birth.
 5
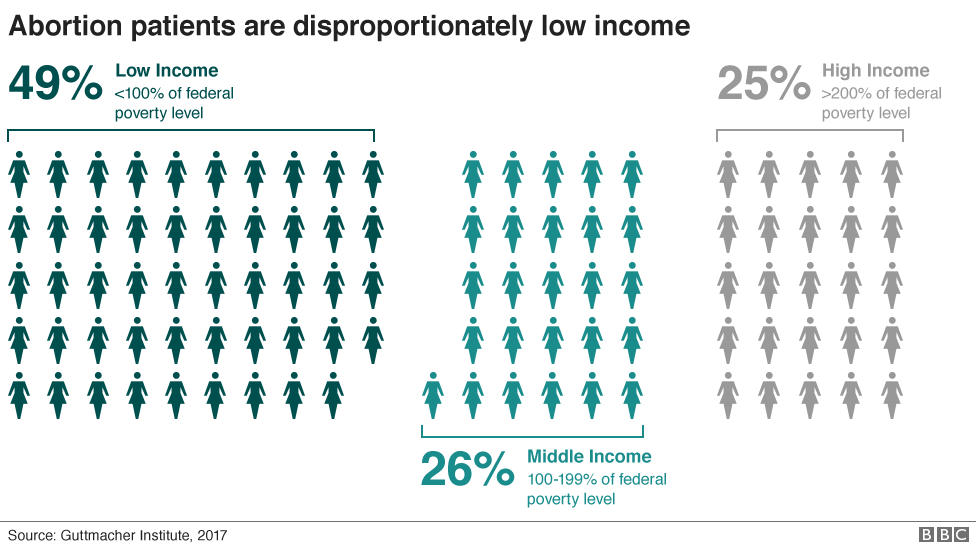
5 - Some 75% of abortion patients in 2014 were poor (having an income below the federal poverty level of $15,730 for a family of two in 2014) or low-income (having an income of 100–199% of the federal poverty level).5
- In 2014, 16% of patients who obtained abortions in the United States were born outside the United States, a proportion comparable to their representation in the U.S. population (17% of women aged 15–44).5
- In 2014, 51% of abortion patients were using a contraceptive method in the month they became pregnant, most commonly condoms (24%) or a short-acting hormonal method (13%).6
- In 2017, there were 808 clinics providing abortion services, a 2% increase from 2014. However, between 2014 and 2017, regional- and state-level disparities in abortion access grew: The number of clinics increased in the Northeast (by 16%) and the West (by 4%) and decreased in the Midwest (by 6%) and the South (by 9%).
 1
1 - Seventy-two percent of clinics offered abortions up to 12 weeks’ gestation in 2014, 25% up to 20 weeks and 10% up to 24 weeks.7
MEDICATION ABORTION
- In September 2000, the U.S. Food and Drug Administration approved mifepristone to be marketed in the United States for nonsurgical abortion. Currently, medication abortion is provided up to 10 weeks’ gestation.
- Medication abortions accounted for 39% of all abortions in 2017, up from 29% in 2014.1
- The majority of medication abortions were offered in specialized clinics and in high volume facilities. In 2017, 30% of clinics provided only medication abortion.1
- Medication abortions increased from 5% of all abortions in 2001 to 39% in 2017, even while the overall number of abortions declined.8
SAFETY OF ABORTION
- A committee of the National Academies of Sciences, Engineering and Medicine reviewed the available evidence and confirmed in a 2018 report that abortion is safe and effective.
 9
9 - Exhaustive reviews by panels convened by the U.S. and UK governments have concluded that there is no association between abortion and breast cancer. There is also no indication that abortion is a risk factor for other cancers.10
- In 2014, the average amount paid for an abortion with local anesthesia in a nonhospital setting at 10 weeks’ gestation was $508. The average paid for an early medication abortion (up to nine weeks’ gestation) was $535.7
- Most U.S. abortion patients had health insurance in 2014. Thirty-five percent had Medicaid coverage, while 31% had private insurance.5 However, insurance does not necessarily cover abortion services; even when it does, patients may not use their coverage for a variety of reasons (for example, because they do not know their plan covers it, they are concerned about confidentiality or their provider does not accept their plan).
 11
11 - Overall, 53% of abortion patients paid out of pocket for their procedure in 2014.5
- The Hyde Amendment currently bans the use of federal dollars for abortion coverage for people enrolled in Medicaid, the nation’s main public health insurance program for low-income individuals. Similar restrictions apply to other federal programs and operate to deny abortion care or coverage to people with disabilities, Native Americans, prison inmates, poor and low-income individuals in the District of Columbia, military personnel and federal employees.12
- Although the Hyde Amendment bars federal funds from being used to provide Medicaid coverage of abortion, states may use their own, nonfederal funds. Fifteen states have a policy requiring the state to provide abortion coverage under Medicaid.13
- In 2014, Medicaid was the second-most-common method of payment and was reported by 24% of abortion patients. The overwhelming majority of these patients lived in the 15 states that allowed state funds to be used to pay for abortion.
 5
5 - Fifteen percent of patients used private insurance to pay for the procedure. Most patients with private insurance (61%) paid out of pocket.5
- In 2014, 65% of abortion patients traveled less than 25 miles one way to obtain care, 17% traveled 25–49 miles, 10% traveled 50–100 miles and 8% traveled more than 100 miles.14
- Greater distances to abortion facilities are associated with increased burden on patients, including higher out-of-pocket costs for associated services such as food, lodging and child care; lost wages;15 increased difficulty getting to the clinic;16 delayed care;17 and decreased use of abortion services.18
- Abortion patients who lived in states with waiting period requirements and adolescents who lived in parental notification states traveled farther than those in states without such laws.14
- The proportion of abortion patients who traveled more than 100 miles for services was twice as high among those at or beyond 16 weeks of gestation as among those who were at 12 weeks’ gestation or less (14% vs.
 7%).14
7%).14 - If Roe v. Wade were overturned or weakened, increases in travel distances would likely prevent 93,500 to 143,500 individuals each year from accessing abortion care.19
- If Roe v. Wade were overturned or weakened, abortion patients’ average distance to the nearest facility would increase by 97 miles, from 25 to 122 miles.19
1. Jones RK et al., Abortion Incidence and Service Availability in the United States, 2017, New York: Guttmacher Institute, 2019, https://www.guttmacher.org/report/abortion-incidence-service-availability-us-2017.
2. Jones RK and Jerman J, Abortion incidence and service availability in the United States, 2011, Perspectives on Sexual and Reproductive Health, 2014, 46(1):3–14, doi:10.1363/46e0414.
3. Guttmacher Institute, State Abortion Policy Landscape: From Hostile to Supportive, 2019, https://www. guttmacher.org/article/2018/12/state-abortion-policy-landscape-hostile-supportive.
guttmacher.org/article/2018/12/state-abortion-policy-landscape-hostile-supportive.
4. Jones RK and Jerman J, Population group abortion rates and lifetime incidence of abortion: United States, 2008–2014, American Journal of Public Health, 2017, doi:10.2105/AJPH.2017.304042.
5. Jerman J, Jones RK and Onda T, Characteristics of U.S. Abortion Patients in 2014 and Changes Since 2008, New York: Guttmacher Institute, 2016, https://www.guttmacher.org/report/characteristics-us-abortion-patients-2014.
6. Jones RK, Reported contraceptive use in the month of becoming pregnant among U.S. abortion patients in 2000 and 2014, Contraception, 2018, doi:10.1016/j.contraception.2017.12.018.
7. Jones RK, Ingerick M and Jerman J, Differences in abortion service delivery in hostile, middle-ground and supportive states in 2014, Women’s Health Issues, 2018, doi:10.1016/j.whi.2017.12.003.
8. Jatlaoui TC et al., Abortion surveillance—United States, 2013, Morbidity and Mortality Weekly Report, 2016, Vol. 65, No. SS-12, https://www.cdc.gov/mmwr/volumes/65/ss/ss6512a1.htm.
9. National Academies of Sciences, Engineering and Medicine, The Safety and Quality of Abortion Care in the United States, 2018, http://www8.nationalacademies.org/onpinews/newsitem.aspx?RecordID=24950.
10. Boonstra HD et al., Abortion in Women’s Lives, New York: Guttmacher Institute, 2006, https://www.guttmacher.org/report/abortion-womens-lives.
11. Jones RK, Upadhyay UD and Weitz TA, At what cost?: payment for abortion care by U.S. women, Women’s Health Issues, 2003, 23(3):e173-e178.
12. Donovan M, In real life: federal restrictions on abortion coverage and the women they impact, Guttmacher Policy Review, 2017, 20:1–7, https://www.guttmacher.org/gpr/2017/01/real-life-federal-restrictions-abortion-coverage-and-women-they-impact.
13. Guttmacher Institute, State funding of abortion under Medicaid, State Laws and Policies (as of January 2018), 2018, https://www.guttmacher.org/state-policy/explore/state-funding-abortion-under-medicaid.
14. Fuentes L and Jerman J, Distance traveled to obtain clinical abortion care in the United States and reasons for clinic choice, Journal of Women’s Health, 2019, https://doi.org/10.1089/jwh.2018.7496.
15. Gerdts C et al., Impact of clinic closures on women obtaining abortion services after implementation of a restrictive law in Texas, American Journal of Public Health, 2016, 106:857–864.
16. Upadhyay UD et al., Denial of abortion because of provider gestational age limits in the United States, American Journal of Public Health, 2014, 104:1687–1694.
17. White K et al., Experiences accessing abortion care in Alabama among women traveling for services, Women’s Health Issues, 2016, 26:298–304.
18. Joyce T, Tan R and Zhang Y, Abortion before & after Roe, Journal of Health Economics, 2013, 32:804–815.
19. Myers C, Jones RK and Upadhyay UD, Predicted changes in abortion access and incidence in a post-Roe world, Contraception, 2019, https://doi.org/10.1016/j.contraception.2019.07.139.
Figure 1: Trends in abortion
The U.S. abortion rate reached a historic low in 2017.
Source: reference 1.
Figure 2: When women have abortions
In 2016, two-thirds of abortions occurred at eight weeks of pregnancy or earlier, and 88% occurred in the first 12 weeks.
Source: Calculated from the Centers for Disease Control and Prevention’s annual abortion surveillance summary, with adjustments for changes in states’ reporting data.
Figure 3: Medication abortion
As U.S. abortion numbers decline, the share that are medication abortions rises steadily.
Source: reference 1.
1. Jones RK et al., Abortion Incidence and Service Availability in the United States, 2017, New York: Guttmacher Institute, 2019, https://www.guttmacher.org/report/abortion-incidence-service-availability-us-2017.
2. Jones RK and Jerman J, Abortion incidence and service availability in the United States, 2011, Perspectives on Sexual and Reproductive Health, 2014, 46(1):3–14, doi:10.1363/46e0414.
3. Guttmacher Institute, State Abortion Policy Landscape: From Hostile to Supportive, 2019, https://www.guttmacher.org/article/2018/12/state-abortion-policy-landscape-hostile-supportive.
4. Jones RK and Jerman J, Population group abortion rates and lifetime incidence of abortion: United States, 2008–2014, American Journal of Public Health, 2017, doi:10.2105/AJPH.2017.304042.
5. Jerman J, Jones RK and Onda T, Characteristics of U. S. Abortion Patients in 2014 and Changes Since 2008, New York: Guttmacher Institute, 2016, https://www.guttmacher.org/report/characteristics-us-abortion-patients-2014.
S. Abortion Patients in 2014 and Changes Since 2008, New York: Guttmacher Institute, 2016, https://www.guttmacher.org/report/characteristics-us-abortion-patients-2014.
6. Jones RK, Reported contraceptive use in the month of becoming pregnant among U.S. abortion patients in 2000 and 2014, Contraception, 2018, doi:10.1016/j.contraception.2017.12.018.
7. Jones RK, Ingerick M and Jerman J, Differences in abortion service delivery in hostile, middle-ground and supportive states in 2014, Women’s Health Issues, 2018, doi:10.1016/j.whi.2017.12.003.
8. Jatlaoui TC et al., Abortion surveillance—United States, 2013, Morbidity and Mortality Weekly Report, 2016, Vol. 65, No. SS-12, https://www.cdc.gov/mmwr/volumes/65/ss/ss6512a1.htm.
9. National Academies of Sciences, Engineering and Medicine, The Safety and Quality of Abortion Care in the United States, 2018, http://www8. nationalacademies.org/onpinews/newsitem.aspx?RecordID=24950.
nationalacademies.org/onpinews/newsitem.aspx?RecordID=24950.
10. Boonstra HD et al., Abortion in Women’s Lives, New York: Guttmacher Institute, 2006, https://www.guttmacher.org/report/abortion-womens-lives.
11. Jones RK, Upadhyay UD and Weitz TA, At what cost?: payment for abortion care by U.S. women, Women’s Health Issues, 2003, 23(3):e173-e178.
12. Donovan M, In real life: federal restrictions on abortion coverage and the women they impact, Guttmacher Policy Review, 2017, 20:1–7, https://www.guttmacher.org/gpr/2017/01/real-life-federal-restrictions-abortion-coverage-and-women-they-impact.
13. Guttmacher Institute, State funding of abortion under Medicaid, State Laws and Policies (as of January 2018), 2018, https://www.guttmacher.org/state-policy/explore/state-funding-abortion-under-medicaid.
14. Fuentes L and Jerman J, Distance traveled to obtain clinical abortion care in the United States and reasons for clinic choice, Journal of Women’s Health, 2019, https://doi. org/10.1089/jwh.2018.7496.
org/10.1089/jwh.2018.7496.
15. Gerdts C et al., Impact of clinic closures on women obtaining abortion services after implementation of a restrictive law in Texas, American Journal of Public Health, 2016, 106:857–864.
16. Upadhyay UD et al., Denial of abortion because of provider gestational age limits in the United States, American Journal of Public Health, 2014, 104:1687–1694.
17. White K et al., Experiences accessing abortion care in Alabama among women traveling for services, Women’s Health Issues, 2016, 26:298–304.
18. Joyce T, Tan R and Zhang Y, Abortion before & after Roe, Journal of Health Economics, 2013, 32:804–815.
19. Myers C, Jones RK and Upadhyay UD, Predicted changes in abortion access and incidence in a post-Roe world, Contraception, 2019, https://doi.org/10.1016/j.contraception.2019.07.139.
Figure 1: Trends in abortion
The U. S. abortion rate reached a historic low in 2017.
S. abortion rate reached a historic low in 2017.
Source: reference 1.
Figure 2: When women have abortions
In 2016, two-thirds of abortions occurred at eight weeks of pregnancy or earlier, and 88% occurred in the first 12 weeks.
Source: Calculated from the Centers for Disease Control and Prevention’s annual abortion surveillance summary, with adjustments for changes in states’ reporting data.
Figure 3: Medication abortion
As U.S. abortion numbers decline, the share that are medication abortions rises steadily.
Source: reference 1.
Download Fact Sheet
Read More
ReportAbortion Incidence and Service Availability in the United States, 2017
State Laws and PoliciesAn Overview of Abortion Laws
Topic
United States
- Abortion
Geography
- Northern America: United States
Page not found - Narvskaya Clinic
REQUESTED
PAGE NOT FOUND
About clinic Patient Services Prices Stock Specialists Blog Contacts nine0004
- Flora smear
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- Contraception
- Hormonal contraceptives
- Intrauterine device
- Barrier contraception
- Natural contraception
Narvskaya, Narvsky pr., 18
Mon-Sun from 09:00 to 20:00
Card
call
- Gynecology
- Consultation of a gynecologist-esthetician
- Intimate contouring
- Abortion
- Consulting
- Diagnostics in gynecology
- Aesthetic gynecology nine0046 Small operations in gynecology
- Termination of pregnancy
- IV iron for anemia in pregnancy
- Laser treatment in gynecology
- Strengthening the pelvic floor muscles in women
- Installation of gynecological pessaries
- Comprehensive examinations for women
- Contraception nine0009
- Flora swab
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- Pregnancy management
- Pregnancy planning
- Management of pregnancy I trimester
- Management of pregnancy II trimester
- Management of pregnancy III trimester nine0009
- Pregnancy records
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
- Pregnancy record
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
- Colposcopy
Narvskaya, Narvsky pr., 18
Mon-Sun from 09:00 to 20:00
Card
call
- Daily monitoring
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- Stress ECG
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call nine0004
Narvskaya, 18 Narvskiy pr. call
- Urology
- Urologist's appointment
- Appointment with a urologist for the treatment of urolithiasis
- Diagnostics in urology
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call nine0004
- Ultrasound
- Pelvic ultrasound
- Ultrasound of the uterus
- Ultrasound during pregnancy
- Ultrasound to determine pregnancy
- Ultrasound to determine the sex of the child
- Folliculometry
- Comprehensive pelvic ultrasound
- Vaginal ultrasound
- Ultrasound in gynecology nine0009
- Screening ultrasound
- Thyroid ultrasound
- 4D ultrasound
- Breast ultrasound
- 3D ultrasound
- Fetal ultrasound
- Ultrasound screening 1 trimester
- Early pregnancy ultrasound
- Ultrasound screening 2nd trimester nine0008 Ultrasound screening 3rd trimester
- Ultrasound of the heart
- Ultrasound of the prostate
- Ultrasound of the scrotum
- Cervicometry
- Doppler
- Ultrasound in obstetrics
- Head vascular ultrasound
- Ultrasound of neck vessels
- Ultrasound of vessels of the upper extremities nine0009
- Ultrasound of vessels of the lower extremities
- Vascular ultrasound
- Ultrasound in urology
- Ultrasound of the kidneys
- Ultrasound of the kidneys and bladder
- Abdominal ultrasonography
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- STI (sexual infections)
- Testing for STIs in women
- Testing for STIs in men
- Treatment of sexually transmitted infections (STIs)
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
- Laser removal of neoplasms
- Dermatoscopy nine0008 Wart removal
- Mole removal
- Removal of papillomas
- Vessel removal
- Removal of genital warts
- Milia removal
- Atheroma removal
- Removal of angiomas
- Keratoma removal
- Callus removal nine0009
- Histological examination
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- Tests
- Oncocytology
- Spermogram with MAP test
- Blood test
- Testing for COVID-19
- Hormones nine0009
- Liquid oncocytology
- Urinalysis
- Tests for tumor markers
- Semen analysis (spermogram)
- Cervical cancer tests
- Cultures for bacterial isolation
- PCR tests
- Urethral swab
- hCG test nine0009
- Fecal tests
- Urinary stone analysis
- Tests for tumor markers in men
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
- Mammology
- Diagnosis of breast diseases
- Mammologist's appointment nine0010
- Cosmetology
- Cosmetologist's appointment
- Cosmetic cannula method
- Facial filler correction
- Wrinkle correction
- Biorevitalization
- Plasmolifting nine0009
- Leather cleaning
- Skin peeling
- Piercing
- Cardiology
- Diagnostics in cardiology
- Cardiologist's consultation
- ECG nine0008 stress ECG
- Daily monitoring
- Dermatology
- Dermatologist's appointment
- Mycologist's appointment
- Dermatovenerologist appointment
- Minor gynecological operations
- Labiaplasty (Labioplasty)
- Surgical defloration
- Hymenoplasty
- Aesthetic gynecology
- Intimate biorevitalization
- Clitoral augmentation (enlargement, filling)
- Plasmolifting in gynecology
- Intimate whitening
- Melsmon Injection
- Laennec Injections
- Diagnostics in gynecology
- Hysterosalpingoscopy
- Biopsy
- Colposcopy
- Consulting
- Consultation with a gynecologist on contraception nine0009
- Consultation with a gynecologist-oncologist
- Consultation of a gynecologist-endocrinologist
- Obstetrician-gynecologist consultation on pregnancy
- Gynecological consultation
- Gynecological appointment with ultrasound
- Andrology
- Andrologist's appointment
- Endocrinology
- Endocrinologist appointment
- Diagnosis of endocrine diseases
- Therapy
- General practitioner appointment
- Sick leave
- Help for sports
- Help to the pool
- Flora smear
- Contraception
- Hormonal contraceptives
- Intrauterine device
- Barrier contraception
- Natural contraception
- Gynecology
- Consultation of a gynecologist-esthetician
- Intimate contouring
- Abortion
- Consulting
- Diagnostics in gynecology
- Aesthetic gynecology nine0046 Small operations in gynecology
- Termination of pregnancy
- IV iron for anemia in pregnancy
- Laser treatment in gynecology
- Strengthening the pelvic floor muscles in women
- Installation of gynecological pessaries
- Comprehensive examinations for women
- Contraception nine0009
- Flora swab
- Pregnancy management
- Pregnancy planning
- Management of pregnancy I trimester
- Management of pregnancy II trimester
- Management of pregnancy III trimester nine0009
- Pregnancy records
- Pregnancy record
- Colposcopy
- Daily monitoring
- Stress ECG
- Urology
- Urologist's appointment
- Appointment with a urologist for the treatment of urolithiasis
- Diagnostics in urology
- Ultrasound
- Pelvic ultrasound
- Ultrasound of the uterus
- Ultrasound during pregnancy
- Ultrasound to determine pregnancy
- Ultrasound to determine the sex of the child
- Folliculometry
- Comprehensive pelvic ultrasound
- Vaginal ultrasound
- Ultrasound in gynecology nine0009
- Screening ultrasound
- Thyroid ultrasound
- 4D ultrasound
- Breast ultrasound
- 3D ultrasound
- Fetal ultrasound
- Ultrasound screening 1 trimester
- Early pregnancy ultrasound
- Ultrasound screening 2nd trimester nine0008 Ultrasound screening 3rd trimester
- Ultrasound of the heart
- Ultrasound of the prostate
- Ultrasound of the scrotum
- Cervicometry
- Doppler
- Ultrasound in obstetrics
- Head vascular ultrasound
- Ultrasound of neck vessels
- Ultrasound of vessels of the upper extremities nine0009
- Ultrasound of vessels of the lower extremities
- Vascular ultrasound
- Ultrasound in urology
- Ultrasound of the kidneys
- Ultrasound of the kidneys and bladder
- Abdominal ultrasonography
- STI (sexual infections)
- Testing for STIs in women
- Testing for STIs in men
- Treatment of sexually transmitted infections (STIs)
- Laser removal of neoplasms
- Dermatoscopy nine0008 Wart removal
- Mole removal
- Removal of papillomas
- Vessel removal
- Removal of genital warts
- Milia removal
- Atheroma removal
- Removal of angiomas
- Keratoma removal
- Callus removal nine0009
- Histological examination
- Tests
- Oncocytology
- Spermogram with MAP test
- Blood test
- Testing for COVID-19
- Hormones nine0009
- Liquid oncocytology
- Urinalysis
- Tests for tumor markers
- Semen analysis (spermogram)
- Cervical cancer tests
- Cultures for bacterial isolation
- PCR tests
- Urethral swab
- hCG test nine0009
- Fecal tests
- Urinary stone analysis
- Tests for tumor markers in men
- Mammology
- Diagnosis of breast diseases
- Mammologist's appointment nine0010
- Cosmetology
- Cosmetologist's appointment
- Cosmetic cannula method
- Facial filler correction
- Wrinkle correction
- Biorevitalization
- Plasmolifting nine0009
- Leather cleaning
- Skin peeling
- Piercing
- Cardiology
- Diagnostics in cardiology
- Cardiologist's consultation
- ECG nine0008 stress ECG
- Daily monitoring
- Dermatology
- Dermatologist's appointment
- Mycologist's appointment
- Dermatovenerologist appointment
- Minor gynecological operations
- Labiaplasty (Labioplasty)
- Surgical defloration
- Hymenoplasty
- Aesthetic gynecology
- Intimate biorevitalization
- Clitoral augmentation (enlargement, filling)
- Plasmolifting in gynecology
- Intimate whitening
- Melsmon Injection
- Laennec Injections
- Diagnostics in gynecology
- Hysterosalpingoscopy
- Biopsy
- Colposcopy
- Consulting
- Consultation with a gynecologist on contraception nine0009
- Consultation with a gynecologist-oncologist
- Consultation of a gynecologist-endocrinologist
- Obstetrician-gynecologist consultation on pregnancy
- Gynecological consultation
- Gynecological appointment with ultrasound
- Andrology
- Andrologist's appointment
- Endocrinology
- Endocrinologist appointment
- Diagnosis of endocrine diseases
- Therapy
- General practitioner appointment
- Sick leave
- Help for sports
- Help to the pool
Narvskaya, 18 Narvskiy pr. call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvsky pr., 18
Mon-Sun from 09:00 to 20:00
Card
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
Map
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call nine0004
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
Map
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Your message has been sent successfully, thank you! nine0004
We will contact you shortly.
Close
Page not found - Narvskaya Clinic
REQUESTED
PAGE NOT FOUND
About clinic Patient Services Prices Stock Specialists Blog Contacts nine0004
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvsky pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
Card
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvsky pr., 18
Mon-Sun from 09:00 to 20:00
Card
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call nine0004
Narvskaya, 18 Narvskiy pr. call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call nine0004
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr.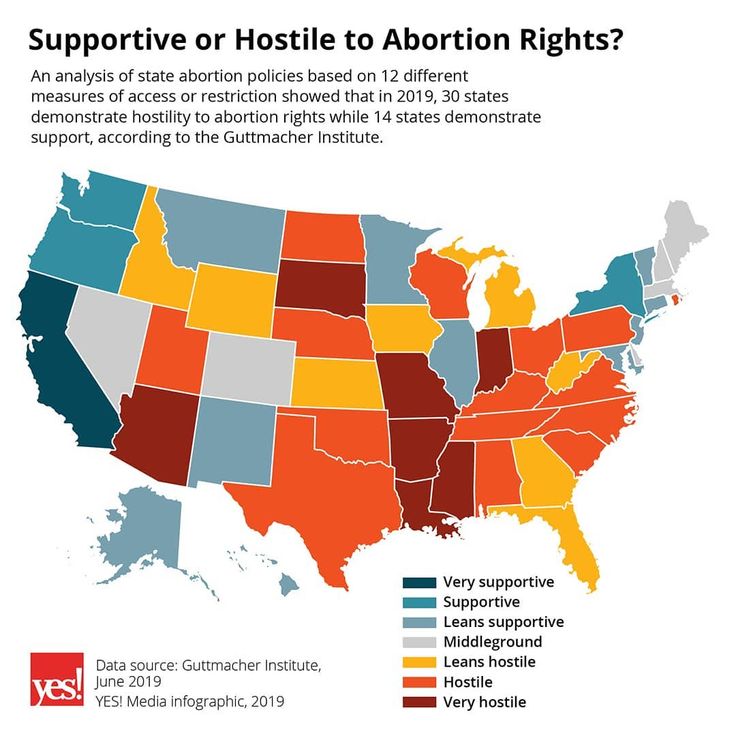 , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr. , 18
, 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, 18 Narvskiy pr. call
Narvskaya, Narvskiy pr. , 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvsky pr., 18
Mon-Sun from 09:00 to 20:00
Card
call
Narvskaya, Narvskiy pr. , 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
Map
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr. , 18
Mon-Sun from 09:00 to 20:00
call nine0004
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
call
Narvskaya, Narvskiy pr., 18
Mon-Sun from 09:00 to 20:00
Map
call
Narvskaya, Narvskiy pr.