Do braxton hicks cause dilation
Braxton Hicks Contractions - StatPearls
Deborah A. Raines; Danielle B. Cooper.
Author Information and Affiliations
Last Update: August 8, 2022.
Continuing Education Activity
Braxton-Hicks contractions, also known as prodromal or false labor pains, are contractions of the uterus that typically are not felt until the second or third trimester of the pregnancy. Braxton-Hicks contractions are the body's way of preparing for true labor, but they do not indicate that labor has begun. Because many pregnant patients have not been educated about Braxton-Hicks contractions, they often seek care and undergo unnecessary evaluation for these contractions. This activity reviews the evaluation and management of patients with Braxton-Hicks contractions and highlights the role of the interprofessional team in educating the patient about the condition.
Objectives:
Describe the etiology of Braxton-Hicks contractions.
Review the presentation of a patient with Braxton-Hicks contractions.
Explain how to evaluate a patient with Braxton-Hicks contractions.
Employ strategies to improve interprofessional communication, which will improve outcomes in patients with Braxton-Hicks contractions.
Access free multiple choice questions on this topic.
Introduction
Braxton Hicks contractions are sporadic contractions and relaxation of the uterine muscle. Sometimes, they are referred to as prodromal or “false labor" pains. It is believed they start around 6 weeks gestation but usually are not felt until the second or third trimester of the pregnancy. Braxton Hicks contractions are the body's way of preparing for true labor, but they do not indicate that labor has begun or is going to start.
Braxton Hicks contractions are a normal part of pregnancy. They may be uncomfortable, but they are not painful. Women describe Braxton Hicks contractions as feeling like mild menstrual cramps or a tightening in a specific area of the abdomen that comes and goes. [1][2][3]
[1][2][3]
Braxton Hicks contractions can be differentiated from the contractions of true labor. Braxton Hicks contractions are irregular in duration and intensity, occur infrequently, are unpredictable and non-rhythmic, and are more uncomfortable than painful. Unlike true labor contractions, Braxton Hicks contractions do not increase in frequency, duration, or intensity. Also, they lessen and then disappear, only to reappear at some time in the future. Braxton Hicks contractions tend to increase in frequency and intensity near the end of the pregnancy. Women often mistake Braxton Hicks contractions for true labor. However, unlike true labor contractions, Braxton Hicks contractions do not cause dilatation of the cervix and do not culminate in birth.
Etiology
Braxton Hicks contractions are caused when the muscle fibers in the uterus tighten and relax. The exact etiology of Braxton Hicks contractions is unknown. However, there are known circumstances that trigger Braxton Hicks contractions including when the woman is very active, when the bladder is full, following sexual activity, and when the woman is dehydrated. A commonality among all these triggers is the potential for stress to the fetus, and the need for increased blood flow to the placenta to provide fetal oxygenation.[4][5][6]
A commonality among all these triggers is the potential for stress to the fetus, and the need for increased blood flow to the placenta to provide fetal oxygenation.[4][5][6]
Epidemiology
Braxton Hicks contractions are present in all pregnancies. However, each woman's experience is different. Most women become aware of Braxton Hicks contractions in the third trimester, and some women are aware of them as early as the second trimester. Sometimes Braxton Hick contractions occurring near the end of the third trimester of pregnancy are mistaken as the onset of true labor. It is not unusual, especially in a first pregnancy, for a woman to think she is in labor only to be told it is Braxton Hicks contractions and not true labor.
Pathophysiology
Braxton Hicks contractions are thought to play a role in toning the uterine muscle in preparation for the birth process. Sometimes Braxton Hicks contractions are referred to as "practice for labor." Braxton Hicks contractions do not result in dilation of the cervix but may have a role in cervical softening.
The intermittent contraction of the uterine muscle may also play a role in promoting blood flow to the placenta. Oxygen-rich blood fills the intervillous spaces of the uterus where the pressure is relatively low. The presence of Braxton Hicks contractions causes the blood to flow up to the chorionic plate on the fetal side of the placenta. From there the oxygen-rich blood enters the fetal circulation.
History and Physical
When assessing a woman for the presence of Braxton Hicks contractions, there are some key questions to ask. Her response to these questions will assist the healthcare provider to differentiate Braxton Hicks contractions and true labor contractions.[7][8][9]
How often are the contractions? Braxton Hicks contractions are irregular and do not get closer together over time. True labor contractions come at regular intervals, and as time goes on, they get closer together and stronger.
How long are the contractions? Braxton Hicks contractions are unpredictable.
 They may last less than 30 seconds or up to 2 minutes. True labor contractions last between 30 to less than 90 seconds and become longer over time.
They may last less than 30 seconds or up to 2 minutes. True labor contractions last between 30 to less than 90 seconds and become longer over time.How strong are the contractions? Braxton Hicks contractions are usually weak and either stay the same or become weaker and then disappear. True labor contractions get stronger over time.
Where are the contractions felt? Braxton Hicks contractions are often only felt in the front of the abdomen or one specific area. True labor contractions start in the midback and wrap around the abdomen towards the midline.
Do the contractions change with movement? Braxton Hicks contractions may stop with a change in activity level or as the woman changes position. If she can sleep through the contraction, it is a Braxton Hicks contraction. True labor contractions continue and may even become stronger with movement or position change.
During the physical assessment, the provider may palpate an area of tightening or a "spasm" of the uterine muscle, but the presence of a uterine contraction in the uterine fundus is not palpable. The woman will be assessed for the presence of uterine bleeding or rupture of the amniotic membrane. An examination of the cervix reveals no change in effacement or dilatation as a result of the Braxton Hicks contractions.
The woman will be assessed for the presence of uterine bleeding or rupture of the amniotic membrane. An examination of the cervix reveals no change in effacement or dilatation as a result of the Braxton Hicks contractions.
Evaluation
There are no laboratory or radiographic tests to diagnose Braxton Hicks contractions. Evaluation of the presence of Braxton Hicks contractions is based on an assessment of the pregnant woman's abdomen, specifically palpating the contractions.
Treatment / Management
By the midpoint of pregnancy, the woman and provider should discuss what the woman may experience during the remainder of the pregnancy. Braxton Hicks contractions are one of the normal events a woman may experience. Teaching her about Braxton Hicks contractions will help her to be informed and to decrease her anxiety if they occur.[10][11][12]
There is no medical treatment for Braxton Hicks contractions. However, taking action to change the situation that triggered the Braxton Hicks contractions is warranted. Some actions to ease Braxton Hicks contractions include:
Some actions to ease Braxton Hicks contractions include:
Changing position or activity level: if the woman has been very active, lie down; if the woman has been sitting for an extended time, go for a walk.
Relaxing: take a warm bath, get a massage, read a book, listen to music, or take a nap.
Drinking water to rehydrate.
If these actions do not lessen the Braxton Hicks contractions or if the contractions continue and are becoming more frequent or more intense, the patient's healthcare provider should be contacted.
Also, if any of the following are present the healthcare provider should be contacted immediately:
Vaginal bleeding
Leaking of fluid from the vagina
Strong contractions every 5-minutes for an hour
Contractions that the woman is unable to "walk through"
A noticeable change in fetal movement, or if there are less than ten movements every 2 hours.

Differential Diagnosis
Amenorrhea
Ascites
Full bladder
Hematometra
Nausea
Ovarian cysts
Pseudocyesis
Uterine fibroids
Vomiting
Pearls and Other Issues
In addition to Braxton Hicks contractions, there are other causes of abdominal pain during pregnancy. Some normal reasons for abdominal pain during pregnancy, in addition to Braxton Hicks contractions and true labor contractions, include:
Round ligament pain or a sharp, jabbing feeling felt in the lower abdomen or groin area on one or both sides.
Higher levels of progesterone can cause excess gas during pregnancy.
Constipation may be a source of abdominal pain.
Circumstances in which abdominal pain is a sign of a serious condition that requires immediate medical attention include:
Ectopic pregnancy.
Placental abruption. A key symptom of placental abruption is intense and constant pain that causes the uterus to become hard for an extended period without relief.
Urinary tract infection symptoms include pain and discomfort in the lower abdomen as well as burning with urination.
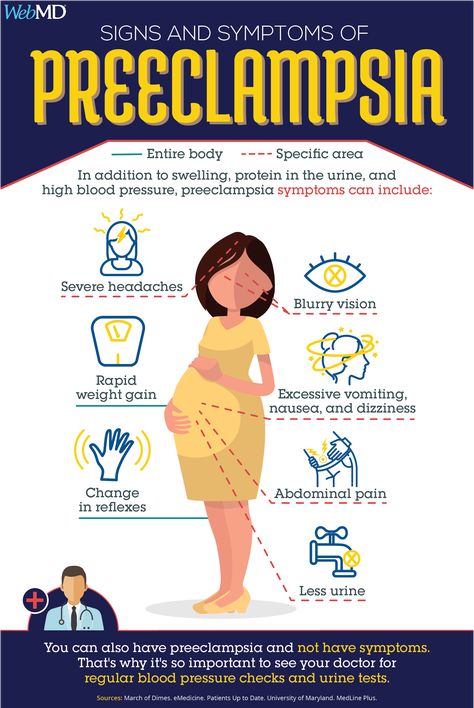
Preeclampsia is a condition of pregnancy occurring after 20-weeks gestation and characterized by high blood pressure and protein in the urine. Upper abdominal pain, usually under the ribs on the right side, can be present in preeclampsia.
If a woman is unsure if she is experiencing Braxton Hicks contractions or another condition, a discussion with a healthcare provider is needed. The healthcare provider may recommend a visit to the office setting or labor and delivery for an examination by a healthcare professional to determine the cause of the abdominal pain.
Enhancing Healthcare Team Outcomes
Braxton hicks contractions are fairly common and it is important for the emergency department physician labor & delivery nurse and nurse practitioner to be aware that this is not true labor. If there is any doubt, the obstetrician should be consulted. However, at the same time, the onus is on the healthcare workers to rule out true labor. Other organic disorders like appendicitis, urinary tract infection or cholecystitis must also be ruled out. With the right education, patients with braxton hicks contraction will not needlessly rush to the ED every time they sense a contraction.
If there is any doubt, the obstetrician should be consulted. However, at the same time, the onus is on the healthcare workers to rule out true labor. Other organic disorders like appendicitis, urinary tract infection or cholecystitis must also be ruled out. With the right education, patients with braxton hicks contraction will not needlessly rush to the ED every time they sense a contraction.
Review Questions
Access free multiple choice questions on this topic.
Comment on this article.
References
- 1.
Hanghøj S. When it hurts I think: Now the baby dies. Risk perceptions of physical activity during pregnancy. Women Birth. 2013 Sep;26(3):190-4. [PubMed: 23711581]
- 2.
MacKinnon K, McIntyre M. From Braxton Hicks to preterm labour: the constitution of risk in pregnancy. Can J Nurs Res. 2006 Jun;38(2):56-72. [PubMed: 16871850]
- 3.
Dunn PM. John Braxton Hicks (1823-97) and painless uterine contractions.
 Arch Dis Child Fetal Neonatal Ed. 1999 Sep;81(2):F157-8. [PMC free article: PMC1720982] [PubMed: 10448189]
Arch Dis Child Fetal Neonatal Ed. 1999 Sep;81(2):F157-8. [PMC free article: PMC1720982] [PubMed: 10448189]- 4.
Lockwood CJ. The diagnosis of preterm labor and the prediction of preterm delivery. Clin Obstet Gynecol. 1995 Dec;38(4):675-87. [PubMed: 8616965]
- 5.
Arduini D, Rizzo G, Rinaldo D, Capponi A, Fittipaldi G, Giannini F, Romanini C. Effects of Braxton-Hicks contractions on fetal heart rate variations in normal and growth-retarded fetuses. Gynecol Obstet Invest. 1994;38(3):177-82. [PubMed: 8001871]
- 6.
Kofinas AD, Simon NV, Clay D, King K. Functional asymmetry of the human myometrium documented by color and pulsed-wave Doppler ultrasonographic evaluation of uterine arcuate arteries during Braxton Hicks contractions. Am J Obstet Gynecol. 1993 Jan;168(1 Pt 1):184-8. [PubMed: 8420324]
- 7.
Lockwood CJ, Dudenhausen JW. New approaches to the prediction of preterm delivery. J Perinat Med. 1993;21(6):441-52.
 [PubMed: 8006770]
[PubMed: 8006770]- 8.
Rhoads GG, McNellis DC, Kessel SS. Home monitoring of uterine contractility. Summary of a workshop sponsored by the National Institute of Child Health and Human Development and the Bureau of Maternal and Child Health and Resources Development, Bethesda, Maryland, March 29 and 30, 1989. Am J Obstet Gynecol. 1991 Jul;165(1):2-6. [PubMed: 1677235]
- 9.
Oosterhof H, Dijkstra K, Aarnoudse JG. Fetal Doppler velocimetry in the internal carotid and umbilical artery during Braxton Hicks' contractions. Early Hum Dev. 1992 Aug;30(1):33-40. [PubMed: 1396288]
- 10.
Oosterhof H, Dijkstra K, Aarnoudse JG. Uteroplacental Doppler velocimetry during Braxton Hicks' contractions. Gynecol Obstet Invest. 1992;34(3):155-8. [PubMed: 1427416]
- 11.
Bower S, Campbell S, Vyas S, McGirr C. Braxton-Hicks contractions can alter uteroplacental perfusion. Ultrasound Obstet Gynecol. 1991 Jan 01;1(1):46-9. [PubMed: 12797102]
- 12.

Hill WC, Lambertz EL. Let's get rid of the term "Braxton Hicks contractions". Obstet Gynecol. 1990 Apr;75(4):709-10. [PubMed: 2314790]
Understanding and Identifying Braxton Hicks Contractions
- Home
- OB/GYN Knowledge Center
- Understanding and Identifying Braxton Hicks Contractions
The doctors and midwives at All About Women of Gainesville and Lake City, FL discuss how you can distinguish between Braxton Hicks vs. real labor contractions
Whether you're 22 or 35 weeks along, pregnant with your first baby or your third, Braxton Hicks contractions can take you by surprise and even trick you into thinking you're entering labor. Also called "warm- up" or "toning" contractions, Braxton Hicks contractions are your body's way of preparing the uterus for labor. And they can send even the most seasoned mother to the hospital – only for her to find out that her Braxton Hicks are causing "false labor."
And they can send even the most seasoned mother to the hospital – only for her to find out that her Braxton Hicks are causing "false labor."
Many women report having more of these contractions later in the day when they are tired or haven't had enough to drink. If you're having lots of Braxton Hicks contractions, don't stop your normal activities, but do make sure you stay well hydrated and take some time to get off your feet during the day.
Understanding Braxton Hicks contractions during pregnancy - when they occur, what they're like, and how to relieve them, as well as how your true labor contractions will differ - can help you interpret what is occurring in your body, and when it's really time to go to the hospital or call your OB doctor.
When Do Braxton Hicks Contractions Start During Pregnancy?
As with most all pregnancy matters, Braxton Hicks contractions are different for every woman. All pregnant women experience these contractions but not all expecting mothers are aware they occur. Some women don't feel any kind of contraction until delivery day, and that is completely normal. You don't need to worry if you haven't felt any warm-up contractions.
Some women don't feel any kind of contraction until delivery day, and that is completely normal. You don't need to worry if you haven't felt any warm-up contractions.
Many women, however, do feel their Braxton Hicks contractions, usually any time after the 20- week marker of pregnancy. While some women feel them this early, others may not experience any until the later weeks of pregnancy. In second and third pregnancies, some mothers say they're Braxton Hicks contractions start earlier.
What Do Braxton Hicks Contractions Feel Like?
Braxton Hicks contractions often begin very mildly, feeling like a tightening sensation across the uterus. They may become stronger in the later weeks of pregnancy. Their strength and recurrence is how expecting mothers confuse them with true labor contractions.
The job of a true labor contraction is to dilate the cervix. Braxton Hicks contractions, you may remember, work only to tone the uterus and do not cause the cervix to dilate. Of course, you can't tell if your cervix is dilated unless you go in and have your obstetrician or midwife check you, but Braxton Hicks contractions have other distinct characteristics like:
Of course, you can't tell if your cervix is dilated unless you go in and have your obstetrician or midwife check you, but Braxton Hicks contractions have other distinct characteristics like:
- Their intensity doesn't change. Braxton Hicks contractions usually remain fairly weak, while true labor contractions grow increasingly intense.
- They go away with a change in activity. If you're sitting down and having Braxton-Hicks contractions, they will usually go away if you get up and walk around. If you've been moving around, the opposite is true – try resting for a while and the contractions should go away. True contractions, on the other hand, do not go away with changes in activity.
- They feel like a tightening across the front of the uterus. True labor contractions, on the other hand, wrap from the top of the abdomen down, and wrap across the front of the abdomen and around the back.
- They are irregular.
 The length and frequency of Braxton Hicks contraction varies. True labor contractions occur at regular intervals and last at least thirty seconds. Real contractions will also grow longer and closer together.
The length and frequency of Braxton Hicks contraction varies. True labor contractions occur at regular intervals and last at least thirty seconds. Real contractions will also grow longer and closer together.
What Causes Braxton Hicks Contractions?
While they may occur without reason, there are some known life factors that cause women to have Braxton Hicks contractions:
- Strenuous exercise or activity
- Dehydration
- Sex, particularly orgasm
- Someone touching the mother's belly
Many women report having more of these contractions later in the day when they are tired or haven't had enough to drink. If you're having lots of Braxton Hicks contractions, don't stop your normal activities, but do make sure that you stay well hydrated and take some time to get off your feet during the day. A warm bath or a cup of tea can also help to relieve your contractions.
Accompanying Signs of Early Labor
If you are getting close to your due date and are experiencing contractions, you should be aware of the signs of early labor that accompany true labor contractions:
- Lower back ache, or pain in your abdomen or pelvis
- Loose stools
- Brown-tinged mucous
- Watery discharge
- Increased urination
If you experience any of these signs along with regularly occurring contractions, you are probably in labor. You may not need to go to the hospital right away, but you should contact your OB doctor or midwife to let them know what symptoms you are experiencing and how far apart your contractions are.
You may not need to go to the hospital right away, but you should contact your OB doctor or midwife to let them know what symptoms you are experiencing and how far apart your contractions are.
Braxton Hicks contractions present themselves so differently in successive pregnancies that even the most seasoned mothers can be confused , not to mention first-time mothers. The best way to have peace of mind about these contractions, besides educating yourself, is to stay in close contact with your OB doctor and midwife.
Florida's obstetricians and midwives at All About Women want you to feel confident with every step of your pregnancy. If you're concerned about contractions, or think you a re pregnant and need to ensure you and your baby are healthy, contact our Gainesville or Lake City office to schedule an appointment today.
Related KC and Blog Articles
Contact Us Knowledge Center
90,000 Braxton Hicks contractions. How to distinguish between false and real contractions? Braxton-Hicks contractions or false labor contractions are irregular contractions and relaxation of the muscles of the uterus as a way of preparing for true labor. They are thought to start around 6 weeks of gestation but are not usually felt until the 2nd or 3rd trimester.
They are thought to start around 6 weeks of gestation but are not usually felt until the 2nd or 3rd trimester.
False contractions are a normal part of pregnancy. They may be uncomfortable, but not painful. Women describe them as a feeling that feels like mild menstrual cramps or tightness in a specific area of the abdomen that quickly resolves.
They are also irregular in duration and intensity, occur infrequently, are unpredictable and not rhythmic, and are more uncomfortable than painful.
Braxton Hicks contractions tend to increase in frequency and intensity towards the end of pregnancy. Women often mistake Braxton Hicks contractions for real labor. However, unlike real contractions, they do not dilate the cervix and result in the birth of a baby.
Braxton Hicks contractions occur when the muscle fibers of the uterus contract and relax. The exact etiology of Braxton Hicks contractions is unknown. However, there are circumstances that can cause them:
- when the woman is very active,
- when the bladder is full,
- after sexual activity,
- when the woman is dehydrated.

Common among all these circumstances is the potential stress on the fetus and the need for increased blood flow to the placenta to provide oxygen to the fetus.
- Change position or activity level: if you were very active, lie down; if you have been sitting for a long time, go for a walk.
- Relax: take a warm bath, massage, read a book, listen to music or take a nap.
If you have Braxton Hicks contractions or if they continue and become more frequent and intense, you should see your doctor.
When assessing for Braxton Hicks contractions, there are a few key questions to ask yourself. We have prepared a table for you with questions, the answers to which will help you understand what kind of contractions you have:
| Braxton Higgs contractions | Real labor pains | |
|---|---|---|
| How often do contractions occur? | Irregular and do not increase over time. | Occurs at regular intervals and gets stronger over time. |
| How long do contractions last? | Unpredictable. They can last less than 30 seconds or up to 2 minutes. | Lasts 30 to 90 seconds and gets longer over time. |
| How strong are the contractions? | Usually weak and either stay the same or get weaker and then disappear. | Increase over time. |
| Where do contractions feel? | Often only felt in the front of the abdomen or in one specific area. | Begin in the middle of the back and wrap around the belly towards the midline. |
| Do abbreviations change with movement? | May stop if activity level changes or if woman's position changes. | Continue and may even get worse with movement or change of position. |
Back to the list of articles
Braxton Hicks contractions for how long - 25 recommendations on Babyblog.
For fifteen years now we have been living not just in a new century, but in a new millennium. For twenty years we have been using computers and the Internet everywhere. It would seem that with the progress of technology, people have enormous opportunities for the exchange of progressive information, knowledge and best practices. But the real picture is almost the opposite: false, untruthful information, often presented under the “sauce” of intimidation and deceit, is spread and accepted by people faster and easier than truthful and useful information.
The worst thing that is now observed in medicine is the filing of many conditions, including quite normal ones, and some diagnoses as something terrible and dangerous, threatening a person’s life, requiring aggressive and extensive treatment immediately. Obstetrics is no exception. On the contrary, in recent years this branch of medicine has grown in a number of countries into a kind of machine of deliberate harm to a pregnant woman and her unborn child.
The concept of "commercial diagnosis", introduced by me ten years ago, is no longer denied by many people and is even used by them in everyday life, conversations and discussions of the situation in the healthcare system. Both doctors and people of other specialties began to talk and write about obstetric aggression. Nevertheless, the number of fictitious diagnoses that do not exist in most countries of the world is striking not only by their backwardness, but also by the lack of a logical analysis of the situation, signs, and examination results when they are made (more precisely, invented).
INCOMPATIBILITY OF THE SPOUSES
Usually such a diagnosis sounds when:
- unsuccessful planning of pregnancy and infertility;
- loss of pregnancy, even the first or one;
- spontaneous habitual miscarriages;
- in exceptionally "striking cases" in the presence of one child or several healthy children.
If we talk about some kind of “spousal incompatibility”, then we can only talk about psychological incompatibility or sexual temperaments, but there is no other “incompatibility”.
Allergic reaction to semen is extremely rare in humans, but the diagnosis would be allergy, not incompatibility.
If a married couple cannot conceive, it may be infertility, which requires proper diagnosis. There are different types of infertility or infertility factors, which means that there will be a different approach to the examination of a married couple and treatment.
Very fashionable commercial HLA (human leukocyte antigen) testing in the world of progressive medicine is used in organ and tissue transplantation, to diagnose a number of autoimmune diseases, confirm paternity and monitor the effectiveness of the treatment of a number of diseases, but has nothing to do with conceiving children, carrying a pregnancy , and even more so with the "incompatibility of the spouses." "Genetic incompatibility of partners" is another invention for imposing an expensive examination and treatment.
If one of the partners has affected genes, that is, there are changes in the form of mutations, then such changes may be associated with problems in conceiving and bearing offspring, but this is not incompatibility. This may be a specific diagnosis (disease, syndrome) on the part of one or both partners. And the recommendations of some doctors to carry out IVF in such cases using the same sexual material, or to find a sexual partner outside of marital relations in order to conceive a child, do not always sound professional.
TOXICOSIS
The concept of "toxicosis" appeared in Soviet obstetrics in the early 1990s, when everyone in the world of progressive medicine had already completely abandoned this concept. Toxicosis means “a state of poisoning” (toxins are poison), and the logical conclusion is that this is pregnancy poisoning, that is, the embryo / fetus poisons the body, and therefore the life of the expectant mother. But doesn’t a mother poison her unborn child with poor-quality food, water, medication, smoking, and even drinking alcohol?
In the West, they quickly realized the absurdity of such a “diagnosis” and tried to switch to the concept of “preeclampsia”, that is, a condition associated with gestation (pregnancy). However, this definition was also abandoned very quickly, because the more science and medicine developed, the faster the exchange of advanced information and experience, the faster doctors began to understand that many “strange” phenomena during pregnancy are not diseases, but variants of the norm. and vice versa - all complications of pregnancy have specific specific names, which should appear as diagnoses.
In post-Soviet medicine, a completely normal phenomenon - nausea and vomiting at the beginning of pregnancy - is still called early toxicosis (in the rest of the world these are just unpleasant symptoms of this condition), and edema, which for the vast majority of women are normal, hypertension in pregnant women, preeclampsia, eclampsia and about ten other complications of pregnancy, which are independent diagnoses, and not a comprehensive mythical toxicosis.
Remember: there is no such diagnosis - toxicosis!
UTERINE TONE / HYPERTONE
For the first time, normal uterine contractions from the beginning of pregnancy to the end of childbirth were described by the English physician John Braxton Hicks in 1872. Mistakenly, such contractions are called "training bouts", which is not true. In the publication of this doctor, it was about normal uterine contractions throughout pregnancy, and not before childbirth.
The uterus is a muscular organ, therefore, just like any muscle, it has its own mode of contractions, which depends on many factors and can be observed both outside of pregnancy and during pregnancy.
The diagnosis of "tonus" or "hypertonicity" was invented by post-Soviet ultrasound doctors and the rest of the world does not exist in obstetrics, therefore it does not require treatment, and even more so inpatient, with the use of a large number of drugs that have also not been used in modern obstetrics for a long time ("Papaverine" , "No-shpa", "Viburkol", vitamin E, magnesia, etc.)
THREAT OF LOSS OF PREGNANCY
I have already raised the topic of "threat of abortion" more than once, especially since it is consonant with the topic of "preservation of pregnancy". In reality, the threat to a pregnant woman comes more from the medical staff than really from someone else or something (nature), because it is people who intimidate, put pressure on the psyche with negative scenarios, escalate the situation, harm with unsafe treatment.
The only diagnosis in obstetrics that has a word root consonant with “threat” is “threatened abortion”. This diagnosis is made according to strict criteria, and not because of “tone / hypertonicity of the uterus”, it does not require treatment, because there is no cure.
All other types of threats are fictitious diagnoses. In obstetrics, it is customary to talk about risk factors and determine the group or degree of risk for the development of one or another pregnancy complication (low risk, high risk). Against the background of the presence of various risk factors, pregnancy can proceed quite normally and end safely.
RH AND GROUP CONFLICT
In modern obstetrics there is no such concept or diagnosis as "Rh conflict" or "group conflict". Worst of all, such a “diagnosis” intimidates a married couple to such an extent that she refuses to conceive children: since it is absolutely impossible to get pregnant, then we are not trying. The presence of different blood types, as well as different Rh factors, is a normal phenomenon in human life and is not considered any conflict.
In modern obstetrics, there are more than 50 blood markers (antigens) for which antibodies (immunoglobulins) can be produced, and this condition is called alloimmunization, or sensitization.
During pregnancy, antibodies can be produced in the mother's body against fetal antigens, cross the placenta and destroy the fetal red blood cells, leading to anemia and fetal hemolytic disease. If hemolytic disease of the fetus occurs, then it will end either with the death of the fetus, or the birth of a child with hemolytic disease of the newborn. Unfortunately, many doctors do not understand the types of jaundice, do not know the current norm of bilirubin levels, so the diagnosis of "hemolytic disease of the newborn" in most cases turns out to be false, which means that aggressive treatment of such children is absolutely inappropriate.
If we talk about really rare "blood conflicts", then they arise not between a man and a woman, but between a mother and a fetus. Therefore, the enthusiasm of some doctors for the search for antibodies in the blood of a man is so surprising. Also depressing is the fact of searching for antibodies in the mother's blood after childbirth in order to make a diagnosis of "hemolytic disease of the newborn." And the use of such a dangerous procedure as plasmapheresis, supposedly to “cleanse the blood” of antibodies, is shocking. This procedure has passed into the category of commercial ones, because it is expensive and brings considerable income to those who carry it out.
For the prevention of Rh sensitization in the mother, vaccination with immunoglobulins (D-antibodies) has long been used, which is carried out in the absence of a woman's own antibodies during pregnancy, after childbirth, abortion, and a number of procedures. This prophylaxis does not protect the current pregnancy, but it does prevent hemolytic disease of the fetus and newborn in subsequent pregnancies. However, it is ineffective in preventing sensitization for all other blood markers.
HEREDITARY (GENETIC) THROMBOPHILIA
In post-Soviet obstetrics, over the past decade, there have been an extremely large number of positions of geneticists who do not understand prenatal genetic screenings and genetics in general, and hematologists (they are fashionably called hemostesiologists, hemastesologists), who do not understand blood and know absolutely nothing about normal changes in the composition of the blood, especially the blood coagulation system in pregnant women.
During pregnancy, blood viscosity increases despite an increase in blood (plasma) volume and a decrease in the concentration of many substances. Therefore, from the very first weeks, pregnancy is accompanied by a hypercoagulable state. It can persist for several weeks, not only after childbirth, but also after abortions and missed pregnancies. This is not a pathological condition, but normal physiological changes.
D-dimer, according to the level of which heparin is prescribed to all pregnant women in a row, is a derivative of fibrinogen. Both of these indicators increase from the first weeks of pregnancy, which is absolutely normal.
Commercially profitable genetic testing leads to the diagnosis of thrombophilia being overused, although several dozen diseases are known to be associated with disorders of the blood clotting process. There are several types of hereditary thrombophilia that have a clear name, and not just "genetic thrombophilia". There are also acquired thrombophilias, which often turn out to be not a separate diagnosis, but a laboratory and clinical symptom of other diseases.
The presence of genes and their combinations does not mean that a person has thrombophilia (and many other diseases). This may indicate a hereditary predisposition, but without clinical and laboratory confirmation, and even more so outside the state of pregnancy, such diagnoses are not made and blood thinning drugs are not prescribed.
Bed rest in hospitals, where pregnant women are kept for weeks and even months, is recognized as the most dangerous factor in the formation of blood clots. It is also surprising that before pregnancy, many women had no idea about their "genetic disease", they took hormonal contraceptives that are incompatible with thrombophilia, and then after giving birth they continue to take them, forgetting about the terrible diagnosis. However, doctors quickly forget about him too.
OLD PLACENTA
The diagnosis of "old placenta", which often sounds in conjunction with the diagnosis of "uteroplacental insufficiency", was born by the same ultrasound specialists.
The placenta is a dynamic organ that undergoes regular changes as pregnancy progresses. Therefore, we can safely say that not only the placenta is aging, but also the fetus itself. The woman also gets older by 9 months!
Placenta insufficiency can be spoken of only when it does not fulfill its function. Just as there is heart or liver failure, placental failure can also exist. But its presence can only be determined by the state of the fetus. If the fetus develops normally and does not lag behind in growth (for this, growth charts must be kept and the exact gestational age must be known), then what kind of placental insufficiency can we talk about?
But what is depressing in all these stories with placentas is that a woman is offered different schemes for "rejuvenation" of the placenta, which necessarily include two fuflomycins - "Kurantil" and "Actovegin". Remember: the placenta cannot be rejuvenated!
In addition, the diagnosis "placentitis" suddenly became fashionable, which was indeed used in veterinary medicine for a very long time, but never in obstetrics! Turning pregnant women into female animals?
oligohydramnios/polyhydramnios tendencies
When I hear or read about the diagnosis of oligohydramnios/polyhydramnios tendency, I want to respond with a great sense of humor: “You know, we all have a lot of tendencies. For example, there is a real tendency with age to get senile dementia. You can buy a lottery ticket - there will be a tendency to enrich. We sit in a car, drive along a highway - we tend to get into a traffic accident and even die. That's right, life tends to end. This means that pregnancy tends to end in term birth and the birth of a healthy baby.
The extremely common diagnosis of "trends" is often the product of ultrasound specialists who somehow do not use the logical thinking of obstetrician-gynecologists to ask a simple question: what kind of nonsense is this?
The state of amniotic fluid is only in the form of a norm, polyhydramnios and oligohydramnios, but there are no trends. These conditions are determined by measuring one pocket (column) of amniotic fluid in centimeters, but most often by the sum of four (namely four, not two or three) pockets, that is, by determining the amniotic index of amniotic fluid (AIF). After 20 weeks, the normal AIH ranges from 8 to 24 cm, of course, adjusted for the condition of the fetus and other ultrasound findings.
Oligohydramnios and polyhydramnios are practically not treated, therefore, volumetric regimens of antibiotics and fuflomycins, the same "Kurantil", "Actovegin", "Khofitol", "Viferon", "Tivorin" and other similar drugs, and with the obligatory presence of a pregnant woman in a hospital , is a manifestation of medical illiteracy.
fetal asphyxia
Most often, the diagnosis of fetal asphyxia appears in the conclusions of pathologists after pregnancy loss, as well as in stillbirth. Surprisingly, it is specialists who do not see the difference between hypoxia and asphyxia, who are just obliged to find out the cause of abortion and fetal death.
The baby is not breathing inside the uterus. His lungs don't work. Everything he receives from his mother in the form of nutrients and oxygen comes through the umbilical cord. The concept of hypoxia implies a violation of blood flow in the vessels of the fetus (impaired hemodynamics) due to the presence of usually two parallel conditions - anemia (anemia) and acidosis (increased acidity) due to oxygen starvation of tissues.