Common baby rashes on face
Common childhood rashes | Pregnancy Birth and Baby
Most children experience a rash at one time or another, and many disappear without treatment. Others may be accompanied by fever, itchiness and other symptoms. Here is a guide to some common rashes in kids.
Meningitis rash
If you think your child might have meningitis rash, go to the nearest emergency department immediately. You can read more about serious childhood rashes here.
Rashes with no fever or itching
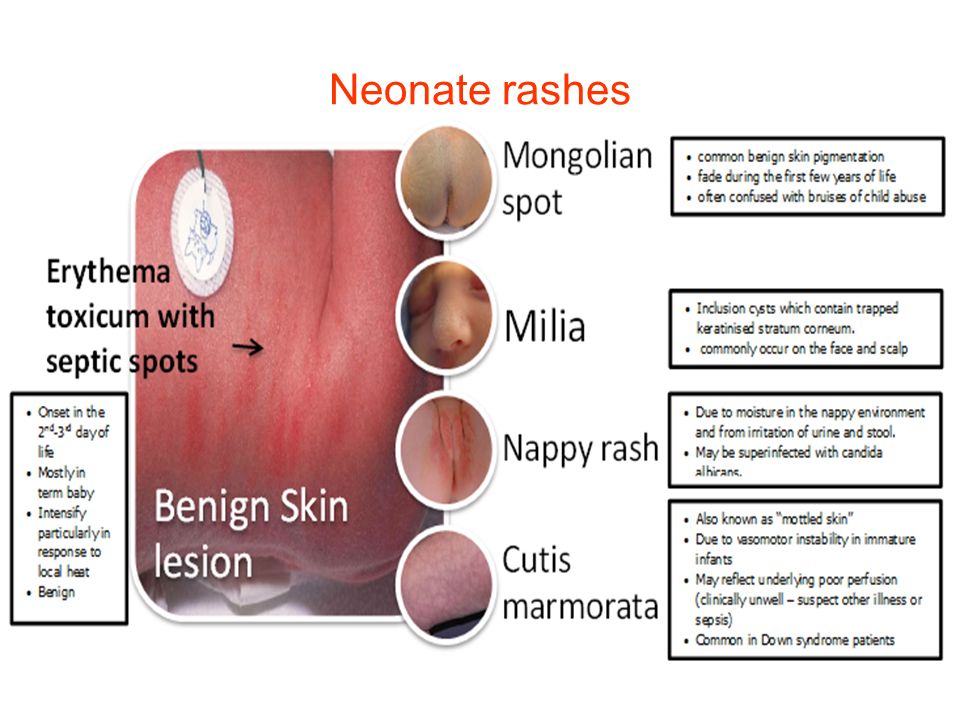
Milia (blocked oil glands)
Up to half of newborn babies develop small white spots called milia on their face, especially on the nose. These are just blocked pores, and they’re not itchy or contagious. They usually clear up without treatment within a few weeks.
Erythema toxicum
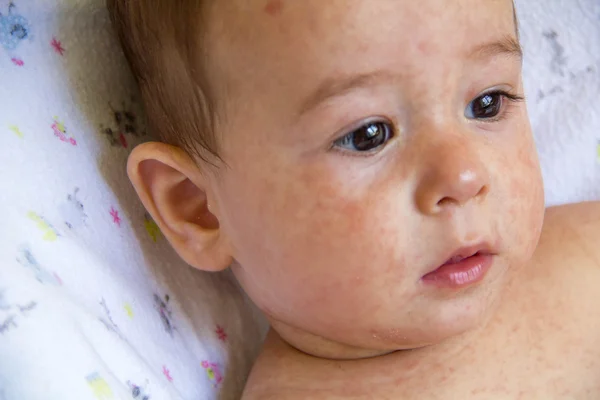
Many newborns develop a blotchy red skin reaction called erythema toxicum, which can appear between 2 days and 2 weeks after birth. Flat, red patches or small bumps often first appear on the face and spread to the body and limbs. The rash is harmless, not contagious, and will clear after a few days or a week.
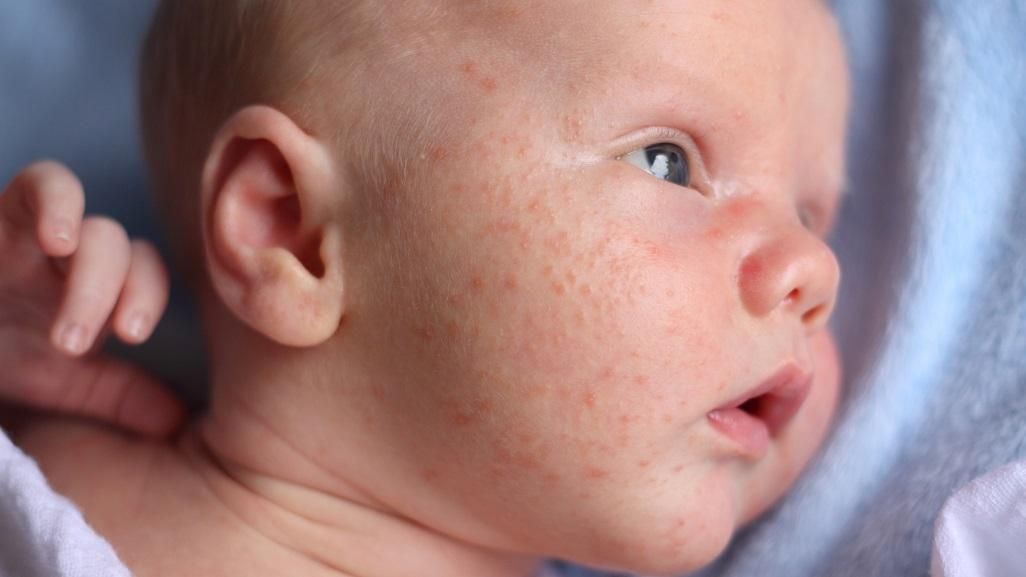
Baby acne
Some babies get acne on their cheeks and nose in the first few months of life. These pimples normally clear up without any treatment, usually in a few months, but sometimes it can take a year.
Nappy rash
Nappy rash is an inflammation of the skin in the nappy area that looks red, sore and inflamed. Nappy rash is caused by a number of things, including urine or poo irritating the baby’s skin.
To avoid nappy rash, keep the nappy area clean and dry with frequent nappy changes and nappy-free time. You can help protect the skin by putting on a barrier cream such as zinc or soft white paraffin at each nappy change.
Persistent nappy rash can be treated with a medicated cream. Don’t use talcum powder or antiseptics to treat nappy rash. If your baby’s skin has developed a fungal infection, you’ll need to use an antifungal ointment. Ask your doctor or pharmacist for advice.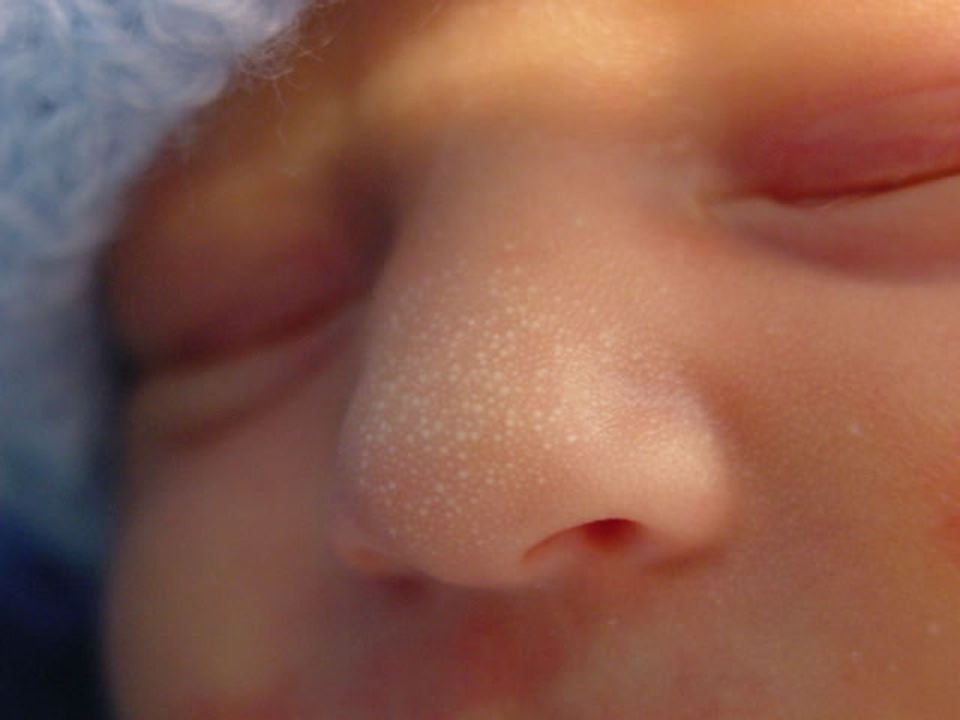
Erythema multiforme
Erythema multiforme is a rash triggered by an infection, medication or an illness. Red spots develop on the hands or feet before spreading across both sides of the body (over a day or so). The spots are not usually itchy, but might become raised or blistered.
Your baby might feel unwell or have a mild fever before the rash appears. Erythema multiforme is not contagious, and usually clears up without treatment in 3 to 6 weeks.
Keratosis pilaris (‘chicken skin’)
Keratosis pilaris is a harmless condition where the skin becomes rough and bumpy, as if permanently covered in goose pimples. These bumps most commonly occur on the upper arms and thighs. You can try several things to help the rash to clear up.
Rashes that might be itchy
Eczema
Eczema causes the skin to become itchy, red, dry and cracked, especially in the creases at the knees and elbows. It is usually treated with corticosteroid creams to reduce inflammation, and moisturisers to stop the skin from drying out.
Eczema is a long-term condition that can show up when babies are only a few months old. Certain triggers, such as viral infections, soap and pool chlorine, can cause symptoms to appear.
Ringworm (tinea)
Ringworm is a contagious, mild skin infection that causes a ring-like red rash with a clear centre. It can occur almost anywhere on the body, although the most common areas are the baby’s scalp, feet and groin.
Ringworm is caused by a fungus, not a worm, and is usually treated with over-the-counter antifungal creams. You should keep your child home from childcare or school until a day after you have started treatment to prevent spreading the infection.
Prickly heat (heat rash)
Heat rash might appear if your baby gets hot in a humid environment. The rash shows as tiny red bumps or blisters on the skin, which can be very itchy. Cooling your baby down and avoiding humidity is the best way to counteract heat rash, which usually clears within 2 to 3 days without treatment.
Impetigo (school sores)
Impetigo is a highly contagious bacterial infection of the skin. It causes red sores and blisters that form a yellow crust. It is very common in children aged 2 to 6, for whom it is not usually serious, but it can be dangerous for newborn babies. It is common in children who have scabies.
If your child has impetigo, you should see your doctor, who might prescribe an antibiotic cream, ointment or tablet. This should clear the infection within 7 to 10 days. You should keep your child home from childcare or school and away from young babies until the sores have dried up, usually a few days after treatment starts.
Hives (urticaria)
Hives is a raised, red, itchy rash that can appear on any part of the body at any time, but is common on the chest, stomach and back, as well as the throat and limbs. Hives usually disappears within a few days without any treatment. Your pharmacist can advise you about over-the-counter medications to treat hives. If the rash doesn't go away, you should see your doctor.
If the rash doesn't go away, you should see your doctor.
Pityriasis rosea
Pityriasis rosea is a mild skin rash that sometimes appears after a sore throat, cold or fever. It usually affects only children over 10.
It begins with a single pink or tan patch on the chest or back. Oval red patches then appear on the chest or back and limbs over the next weeks. They might be itchy, and your child might feel tired and unwell.
The exact cause of pityriasis rosea is unclear, and experts believe it is probably not contagious. The rash usually clears up within a couple of months without treatment.
If you are pregnant, pityriasis rosea can in rare cases lead to complications. See your doctor if you are pregnant and come into contact with a child who has pityriasis rosea.
Molluscum contagiosum
Molluscum contagiosum is a viral skin infection that is spread by skin-to-skin contact or by sharing swimming pool water or towels.
Molluscum contagiosum spots look like pimples and grow into round pearly white lumps, usually 2 to 5 millimetres in size. They can be itchy. Usually they heal without treatment within 6 months, but it might take longer.
They can be itchy. Usually they heal without treatment within 6 months, but it might take longer.
Rashes with fever
Slapped cheek disease (fifth disease)
Slapped cheek disease is a viral infection that mainly affects pre-school and school-age children. It typically causes a bright red rash on both cheeks that spreads as a ‘lacy’ rash on the body and limbs. Occasionally, it causes fever.
Slapped cheek disease is usually mild and clears up in a few days without treatment. The child is contagious before the rash appears, but not once it has appeared.
The virus can affect a pregnant woman, potentially causing a type of anaemia in her unborn baby. It can also cause miscarriage. If you suspect you or your child has slapped cheek disease, you should avoid contact with women who are, or might be, pregnant.
Hand, foot and mouth disease
Hand, foot and mouth disease is a mild but highly contagious viral illness that causes a rash on the palms of the hands and soles of the feet. It is not the same as the foot-and-mouth disease that affects farm animals.
It is not the same as the foot-and-mouth disease that affects farm animals.
The disease is common in childcare and kindergartens. Your child might feel unwell and have a fever and blisters on the hands and feet and in the mouth, and also in the nappy area, that last 7 to 10 days. Children with hand, foot and mouth disease should stay away from childcare or school until all the blisters have dried up.
Hand, foot and mouth disease usually resolves on its own without major problems but in rare cases it can be more serious especially in people whose immune system is not functioning normally or pregnant women. These rare problems include infections of the brain and heart muscle and miscarriage in pregnant women.
Roseola infantum
Roseola infantum is a contagious viral infection that can cause cold-like symptoms and a high fever. Kids with roseola infantum have raised pink spots that start on the chest, stomach and back and spread to the limbs. The child is contagious before the rash appears, but not after. The rash usually lasts 3 to 5 days.
The rash usually lasts 3 to 5 days.
The high fever may last for a few days. Roseola infantum can also cause some children to have a febrile convulsion. If your child has a convulsion (fit), call triple zero (000) immediately and ask for an ambulance. Febrile convulsions are scary to see but are generally not harmful.
When to seek help
Many babies develop a skin rash in their first days or weeks as their sensitive skin adapts to a new environment. Most rashes are harmless and go away on their own. But if your baby seems unwell, or if you’re worried, you should see your doctor. They can advise about the cause and whether treatment is necessary.
Whatever their age, you should take your child to the doctor if they have a rash and persistent high temperature, cold or cough symptoms or swollen neck glands.
Treatment of common childhood rashes
If you think your child might be contagious, they should stay at home. Keep them away from school, childcare and other children. You should also keep them away from women who are pregnant, or who might be pregnant, since some childhood infections can cause serious problems in unborn babies.
You should also keep them away from women who are pregnant, or who might be pregnant, since some childhood infections can cause serious problems in unborn babies.
You can use paracetamol or ibuprofen (in babies aged over 3 months) to reduce fever — read the packet instructions carefully to ensure your child receives the right amount for their age and weight.
Your pharmacist can advise you on treating the symptoms of common rashes. For example, you can use over-the-counter creams to prevent itchiness.
If you are concerned about your child, call Pregnancy, Birth and Baby on 1800 882 436 to talk to a maternal child health nurse, or call Healthdirect on 1800 022 022 to talk to a registered nurse. Alternatively, contact your doctor.
Learn more here about the development and quality assurance of healthdirect content.
Molluscum contagiosum - NHS
Molluscum contagiosum (MC) is a viral infection that affects the skin. Around 9 out of 10 cases happen in children although it can occur at any age.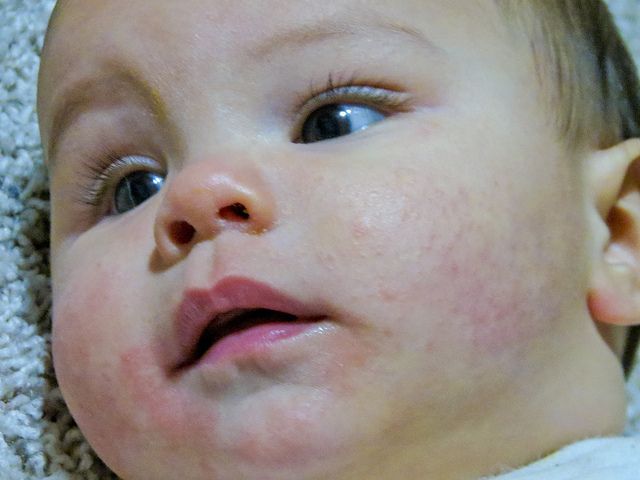
MC is generally a harmless condition that normally gets better in a few months without any specific treatment.
However, it's common for the condition to spread around the body, so it can take up to 18 months or more for the condition to clear completely.
Symptoms of molluscum contagiosum (MC)
Usually, the only symptom of MC is a number of small, firm, raised papules (spots) on the skin with a characteristic small dimple in the middle. The spots are not painful, but can be itchy.
The spots may develop in small clusters and can be spread across different parts of the body. They're most often found in the armpit, behind the knees or on the groin.
MC can affect a person on more than 1 occasion, but this is uncommon.
Credit:
DR P. MARAZZI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259439/view
MARAZZI/SCIENCE PHOTO LIBRARY https://www.sciencephoto.com/media/259439/view
When to seek medical advice
See a GP if you notice the spots associated with MC. They're usually easy to recognise, so they should be able to diagnose the condition without the need for further tests.
If the GP thinks the infection may be caused by something other than MC, they may want to:
- take a skin sample (biopsy) from one of the spots to test it for the molluscum contagiosum virus (MCV)
- refer you to a genitourinary medicine (GUM) clinic to be tested for sexually transmitted infections (STIs) – if you prefer, you can go to an STI clinic directly
They may refer you to a specialist in hospital if you have:
- spots on your eyelids, near your eye, or your eye is red or painful
- HIV and your symptoms are severe
- a weakened immune system for another reason – such as receiving chemotherapy
Causes of molluscum contagiosum (MC)
MC is caused by a virus known as the molluscum contagiosum virus (MCV).
This virus can be spread through:
- close direct contact – such as touching the skin of an infected person
- touching contaminated objects – such as towels, flannels, toys and clothes
- sexual contact – this includes intimate physical contact as well as sexual intercourse
If you become infected by the virus and spots appear on your skin, the virus can also spread to other areas.
It's not known exactly how long someone with MC is contagious for, but it's thought the contagious period may last up until the last spot has disappeared.
Treating molluscum contagiosum (MC)
Routine treatment for MC, particularly in children, is generally not recommended because:
- the infection usually clears up on its own
- the infection does not normally cause any symptoms other than the spots
- the infection does not usually interfere with everyday activities, such as going to work, swimming or playing sports
- treatments can be mildly painful and may cause scarring or damage to the surrounding skin
Treatment is usually only recommended for older children and adults when the spots are particularly unsightly and affect quality of life, or for people with weakened immune systems.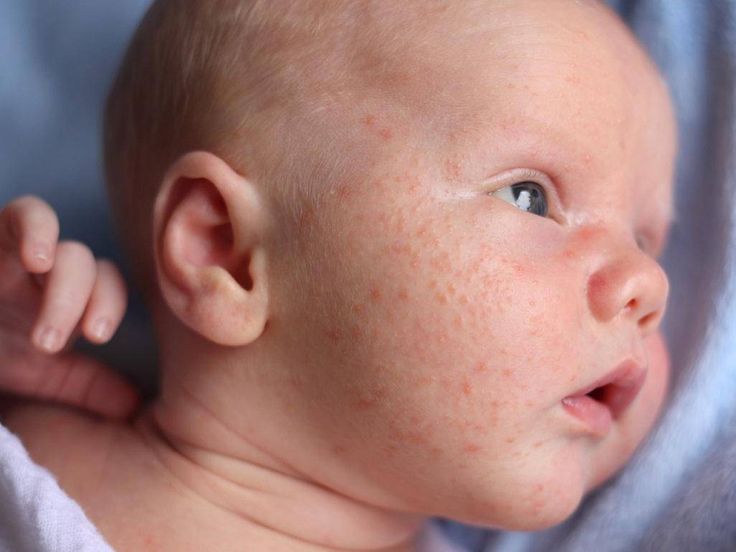
In such cases, treatments that may be offered include:
- liquids, gels or creams that are applied directly to the skin
- minor procedures such as cryotherapy (where the spots are removed by freezing them)
Preventing the spread of molluscum contagiosum (MC)
Although MC is infectious, the chance of passing it on to others during normal activities is small.
It's not necessary for you to stay away from work or your child to stay away from school or nursery, or to stop doing activities such as swimming if you have MC.
However, you should take some steps to avoid spreading the virus to other people. You should:
- avoid sharing towels, flannels and clothing
- avoid squeezing or scratching the spots – as well as increasing the risk of the infection spreading, this can cause pain, bleeding and can lead to scarring
- keep affected areas of skin covered with clothing whenever possible – a waterproof bandage can be put over the area if you go swimming
- avoid sharing baths
Using a condom while having sex can reduce the risk of passing on MC during sexual contact.![]()
Complications of molluscum contagiosum (MC)
MC rarely causes any other problems but complications can occasionally occur. These include:
- the spots may become infected by bacteria – which may require treatment with antibiotics
- scarring – after MC has healed and cleared, small patches of paler skin or tiny indented scars may be left behind; this is more likely if the spots became infected or after treatment
- eye problems – a secondary eye infection may develop, such as conjunctivitis or keratitis, which may cause your eyes to become sore and sensitive to light
See a GP if you suspect a bacterial infection or experience any eye problems such as eye pain or redness. Signs of a bacterial infection can include redness, swelling and pain in the skin and underlying tissue.
Page last reviewed: 03 September 2020
Next review due: 03 September 2023
Skin rash in children: analyze the causes
Features of children's skin
The skin, like most other organs and systems, gradually develops until puberty. In a child, it is functionally and structurally more sensitive to external influences and allergic reactions. At the same time, the sweat and sebaceous glands do not yet work properly, which is associated with insufficient development of skin innervation.
In a child, it is functionally and structurally more sensitive to external influences and allergic reactions. At the same time, the sweat and sebaceous glands do not yet work properly, which is associated with insufficient development of skin innervation.
At the same time, the skin from birth takes an active part in metabolism and respiration due to the many superficially located vessels. Because of this, skin diseases often greatly affect the general condition of the child.
Types of rash in children
Skin rash caused by a particular disease usually has its own characteristics. The most common types of rashes include:
- Papules. These are volumetric formations of a small size (up to 10 mm), which rise above the skin. The main color is red and pink. Occurs with lichen planus, roseola infantum, atopic dermatitis, etc.
- Vesicles. They are bubbles up to 5 mm in diameter, filled with a cloudy liquid. After opening, erosion is often left behind.
 May be a sign of chickenpox and other herpes infections.
May be a sign of chickenpox and other herpes infections. - Petechiae. A purplish skin eruption that does not go away with pressure. Its elements do not exceed 3 mm in diameter, do not rise above the skin and are not felt to the touch. As a rule, they indicate meningococcal infection, vascular damage (vasculitis), platelet deficiency.
- Erosion. This is a skin defect that does not penetrate deeper than the epidermis. It has the appearance of a rounded, somewhat in-depth formation of red color with a weeping surface.
- Peel. A secondary element formed by the drying of secretions from vesicles, erosions, or blood. Solid, has a dark red, brown color.
- Macula or spot. This is an area of discoloration that is on the same level as adjacent areas of the skin. It can be both an independent element in rubella, measles, roseola, and a residual phenomenon after papules, vesicles or erosions.
- Wheals or urticaria. A rounded element of a rash of pale pink, red or purple-white color, the size of which varies from 1-2 mm to tens of centimeters.
 Leaves no secondary elements behind. Meet with allergic reactions, urticaria.
Leaves no secondary elements behind. Meet with allergic reactions, urticaria. - Lichenification. These are areas of excessive thickening of the skin with increased skin pattern. Often a secondary element.
Diseases that cause skin rashes in children
Baby skin rashes can indicate various diseases, most often infections and allergic reactions.
Roseola infantum
Roseola infantum or sudden exanthema is a childhood infectious disease that occurs when infected with human herpesviruses type 6 or 7. Most often observed between the ages of 6 months and 2 years.
Sudden exanthema is accompanied by an increase in body temperature up to 39-40°C, which persists for 3-5 days, after which a bright red maculopapular rash appears on the child's skin. It occurs on the surface of the chest and abdomen, spreading throughout the body (Fig. 1). The elements of the rash, as a rule, are not felt by the fingers, but sometimes they can be raised. They disappear when the skin is stretched or when the glass of a glass is pressed on them.
They disappear when the skin is stretched or when the glass of a glass is pressed on them.
In roseola infantum there may be white rings around some elements of the rash. Often the rash is limited only to the trunk and, not having time to reach the face and limbs, disappears. The rash does not cause discomfort or itching, but children usually become sharply capricious and "unbearable" during this time; the rash lasts from several hours to several days, and then disappears, leaving no pigmentation or peeling. An excerpt from the book by Sergei Butriy “Child health: a modern approach. how to learn to cope with illness and your own panic.
Roseola infantum should be treated symptomatically, preferably with antipyretics and plenty of fluids. In immunodeficiency states (HIV infection, congenital disorders of the immune system), antiherpetic drugs are additionally prescribed.
Figure 1. Rash in roseola infantum. Source: WikipediaNo matter how hard baby roseola flows, it is perfectly safe.
Complications are extremely rare and are usually limited to febrile convulsions. An excerpt from the book by Sergei Butriy “Child health: a modern approach. how to learn to cope with illness and your own panic.
Enteroviral exanthems: chicken pox and enteroviral pharyngitis
The viral pemphigus, also known as turkish varicella, is caused by enterovirus 71 (EV-71). Enteroviral pharyngitis is caused by Coxsackie A16, B2, B5 viruses. They occur mainly among children under the age of 10 years, infection often occurs during holidays in southern countries.
The primary signs of pathologies are pain in the mouth and throat, because of which the child refuses to eat and does not even swallow saliva, but spits it out. Then the body temperature rises to 39°C. The fever persists for about 4 days and is accompanied by nausea and vomiting, loss of appetite and excessive irritability. With enteroviral pharyngitis, small white sores usually occur only on the palatine arches (Fig. 2), but Turkish chickenpox is a rash throughout the mouth, including the tongue, around the mouth, on the palms and feet. The rash on the skin may resemble chickenpox - red spots or blisters.
2), but Turkish chickenpox is a rash throughout the mouth, including the tongue, around the mouth, on the palms and feet. The rash on the skin may resemble chickenpox - red spots or blisters.
Symptomatic treatment:
- Oral hygiene and rinsing with antiseptic solutions.
- Non-steroidal anti-inflammatory drugs (NSAIDs) that help control pain while lowering body temperature.
- Plentiful warm fluids to prevent dehydration, cold drinks and ice cream may be given (these are more easily tolerated by sick children).
- Diet with the exception of mechanically hard, sour and salty foods.
- Enteroviral exanthems are self-limiting, the disease usually recedes after 3-7 days. However, the condition of the child during the illness must be monitored in order to consult a doctor in time in case of complications. The most common are dehydration and secondary bacterial infections.
 In the latter case, abscesses, yellow crusts appear on the skin, the skin swells. Rarely enterovirus infection leads to serous meningitis.
In the latter case, abscesses, yellow crusts appear on the skin, the skin swells. Rarely enterovirus infection leads to serous meningitis.
Chickenpox
Chickenpox or chickenpox is an infectious disease caused by the human herpesvirus type 3 (Varicella Zoster). People of any age get sick with it, but mostly it is children 5-9years.
The main symptom is skin rashes that have a certain sequence of development. Small pink spots appear first, quickly transforming into papules, and then into vesicles (Fig. 3) with reddening around. After a couple of days, they open or dry out, forming crusts of dark red, brown color on their surface. A characteristic feature is severe itching.
Figure 3. Development of a skin rash in chickenpox. Source: SlideToDoc
The total period of rashes lasts from 2 to 9days. At the same time, the general condition practically does not suffer, but fever may occur.
There are no drugs that can completely eliminate the virus, so the treatment tactics are aimed at eliminating the symptoms and normalizing the child's condition:
- Bed rest in the presence of fever.
- Treatment of elements of the rash with a solution of manganese, methylene blue or brilliant green (brilliant green).
- Antihistamines for itching.
- Antipyretics.
- Taking regular warm showers without using a washcloth or brush.
Complications of chickenpox occur against the background of suppression of the body's immune system. These include: inflammation of the lungs (pneumonia), lesions of the nervous system (neuralgia, meningitis, encephalitis, damage to the facial nerve), eyes (keratitis, conjunctivitis, uveitis), etc.
Important ! For the prevention of chickenpox, especially for adults, against the background of a weakened immune system and a high risk of complications, vaccination is recommended. It can also be carried out as an emergency prophylaxis up to 2 days from the moment of contact with a sick person.
Measles
Measles is a viral infectious disease. Often it occurs in unvaccinated children from 2 to 5 years and older.
Measles debuts with a sharp rise in temperature to 39-40°C, dry cough, runny nose, headache, hoarseness. Characteristic features are swelling and redness of the eyelids, pharynx and red spots in the sky. On the 2-3rd day of development, a symptom specific to measles occurs - Filatov-Belsky-Koplik spots. These are white spots with a red border, observed on the inner surface of the cheeks near the molars. On the 4-5th day from the appearance of the first signs of the disease, these spots disappear, and they are replaced by a skin rash.
The primary localization of measles papular rash is the outer surface of the elbow, knees, fingers. Further, it spreads throughout the body (Fig. 4). The elements of the rash are surrounded by red spots and tend to merge with each other. After 4 days from the moment they appear, the child's condition returns to normal, and the elements of the rash become darker and peel off. Residual effects and pigmentation disappear after 7-10 days.
Figure 4.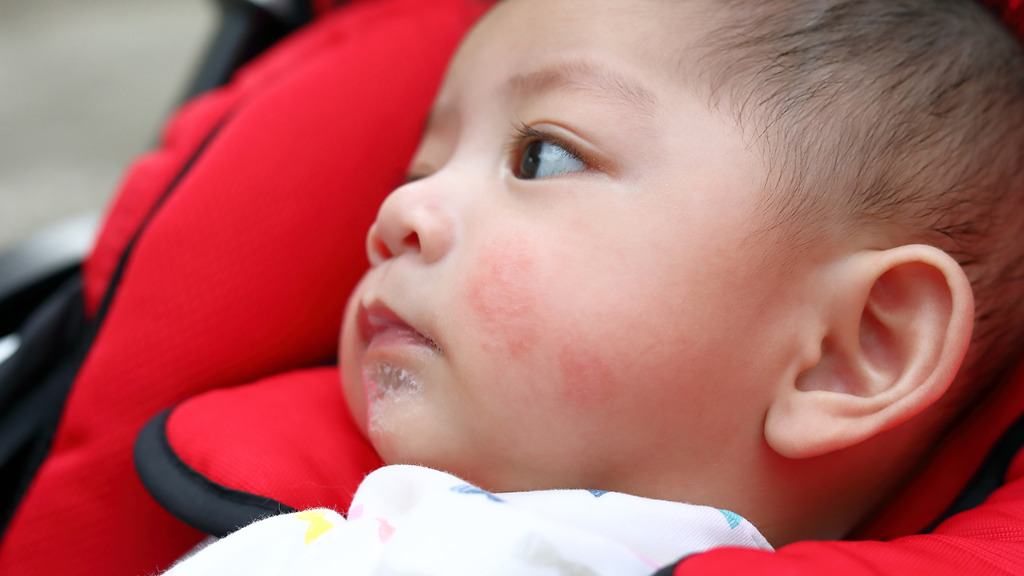 Skin rash in measles. Source: CDC
Skin rash in measles. Source: CDC
There is no specific treatment for measles; helping a child involves managing individual symptoms:
- NSAIDs to reduce body temperature.
- Expectorants for relief of coughs.
- Antiseptic mouth rinses.
- Topical treatment of rash elements with astringents or tea to relieve itching and soreness.
Measles is very dangerous. Possible complications of measles:
- Stenosis of the larynx - croup.
- Primary measles or secondary bacterial pneumonia.
- Inflammation of the respiratory tract - bronchitis, tracheitis, laryngitis, pharyngitis.
- Otitis media.
- Hepatitis.
- Encephalitis and subacute sclerosing panencephalitis.
Scarlet fever
Scarlet fever is a bacterial infection caused by group A beta-hemolytic streptococcus. Most cases occur in children between 3 and 7 years of age.
The first manifestation of scarlet fever is an intoxication syndrome - an increase in body temperature up to 38-39°C, headache, general weakness and loss of appetite.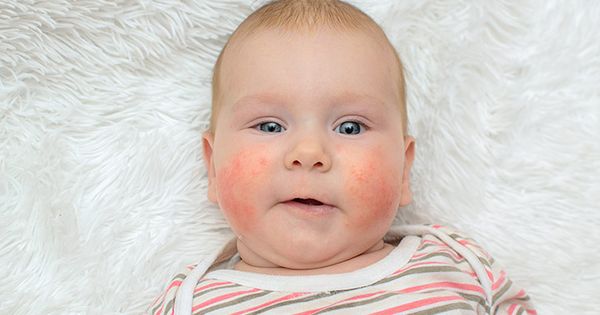 On the 2-4th day from the moment the first signs of the disease appear, one of the characteristic symptoms appears - "crimson tongue" (Fig. 5). It is manifested by pronounced graininess and bright red color of the surface. Angina also occurs - inflammation of the palatine tonsils.
On the 2-4th day from the moment the first signs of the disease appear, one of the characteristic symptoms appears - "crimson tongue" (Fig. 5). It is manifested by pronounced graininess and bright red color of the surface. Angina also occurs - inflammation of the palatine tonsils.
From the first days of scarlet fever, a characteristic red punctate rash appears, which does not disappear when pressed with glass, but becomes yellowish with effort. It is located on the flexion surfaces: the inner parts of the elbows, under the knees, in the inguinal pits, on the cheeks and sides of the body. It lasts up to 1 week, after which it disappears, leaving no pigmentation behind. A specific sign is the pallor of the nasolabial triangle.
Another characteristic feature of scarlet fever is the peeling of the skin that occurs after the rash has disappeared. At the same time, the skin "moves away" in whole layers in the area of the palms and feet, while in other areas - in small fragments.
Treatment is based on antibiotics from the penicillin group. Vitamin C and B vitamins, symptomatic preparations are used as adjuvants. Plentiful warm drink and bed rest are recommended. In severe cases, glucocorticosteroids and intravenous drip of glucose solutions and plasma substitutes are used.
The most common complications of scarlet fever: otitis media, sinusitis and frontal sinusitis (inflammation of the maxillary and frontal paranasal sinuses, respectively), cervical lymphadenitis (inflammation of the lymph nodes of the cervical region).
Rubella
Rubella is caused by Rubella virus. The majority of patients are children aged 3 to 9 years.
Rubella begins with an intoxication syndrome of moderate severity: fever up to 38-38.5°C, headache and increased fatigue, signs of pharyngitis and conjunctivitis, pronounced enlargement of the lymph nodes of the cervical and occipital region.
After 1.5-2 days from the onset of the disease, a skin rash appears in the form of spots, which spreads downward over several hours - appearing on the face, gradually moving to the trunk and limbs. Outwardly, the rash initially resembles measles, then scarlet fever. Itching and peeling are absent, and the spots, unlike measles, do not merge with each other. The bulk of the spots are located on the buttocks and lower back, the outer surface of the elbows and knees. After 3-5 days, the rash disappears without a trace.
Outwardly, the rash initially resembles measles, then scarlet fever. Itching and peeling are absent, and the spots, unlike measles, do not merge with each other. The bulk of the spots are located on the buttocks and lower back, the outer surface of the elbows and knees. After 3-5 days, the rash disappears without a trace.
There is no specific treatment for rubella, and the main actions are aimed at eliminating individual symptoms of the disease. Complications are very rare, as a rule - against the background of disorders of the immune system. In such cases, the development of pneumonia, arthritis, otitis media is possible.
Important ! Rubella is especially dangerous for pregnant women, as it causes problems in the fetus, so when planning a pregnancy, all unvaccinated people should be vaccinated against this infection.
Urticaria
Urticaria or urticaria is a type of dermatitis caused by allergies. The disease is very common among both children and adults. In total, about 20% of the adult population and 2-7% of children suffer from it.
In total, about 20% of the adult population and 2-7% of children suffer from it.
Medications (most often antibiotics), various foods, vaccines and physical influences: cold, sunlight, mechanical pressure can provoke the development of urticaria.
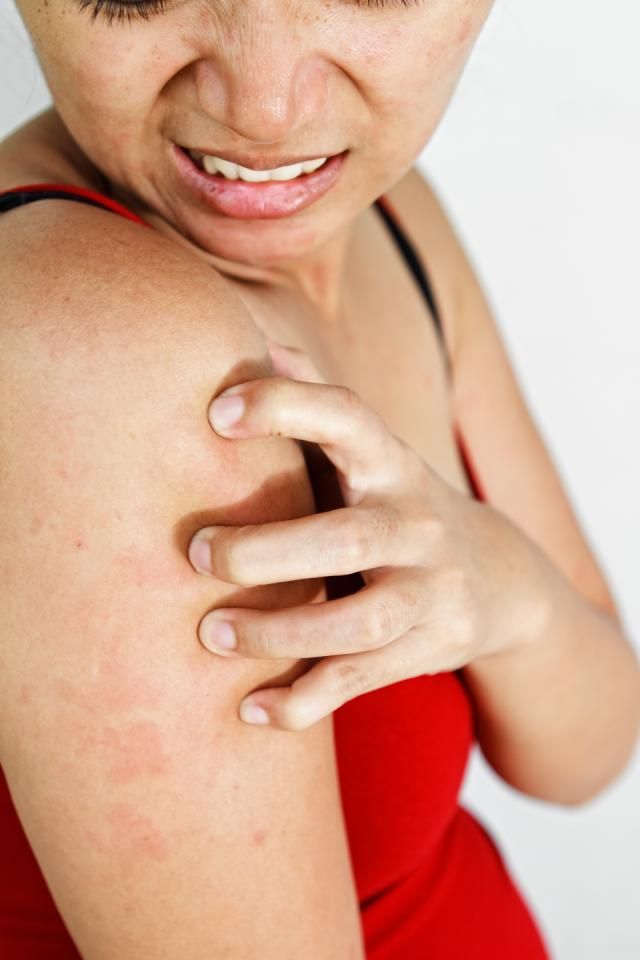
The leading symptom of the pathology is a skin rash in the form of dense red or pink vesicles or nodules 2-10 mm in diameter with clear edges, which become pale when pressed (Fig. 6). A characteristic feature is the sudden appearance and equally rapid disappearance of the elements of the rash without a trace, as well as severe itching.
Figure 6. Urticaria rash. Source: James Heilman, MD/Wikipedia
Treatment, depending on the form of the disease, is represented by antihistamines, histamine receptor blockers or glucocorticosteroids.
Complications occur in the absence of treatment and include angioedema, anaphylactic shock, heart and kidney damage in the form of myocarditis or glomerulonephritis, respectively.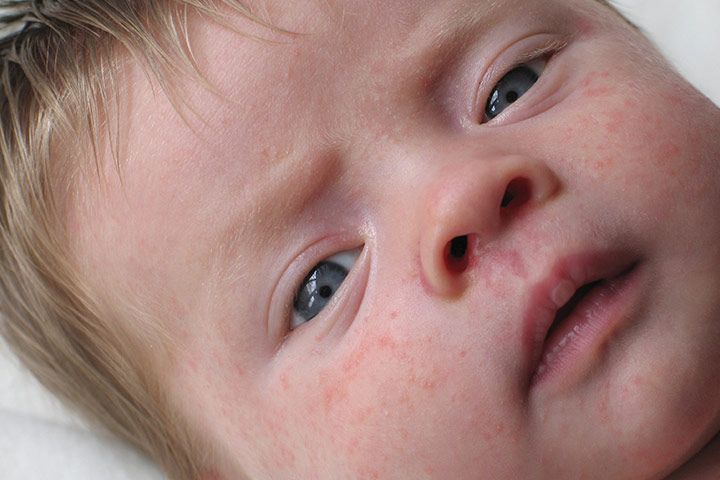
Lichen planus
Lichen planus is a chronic dermatitis of unknown origin. Most of the patients are people aged 30 to 60 years. However, about 5% of the total number of patients are children.
A typical form of the disease is accompanied by the appearance of gray-white papules up to 2 mm in diameter on the oral mucosa, namely: the inner surface of the cheeks behind the molars, on the lateral parts of the tongue and on the palate. Sometimes the rashes can merge, forming patterns.
In some patients, a rash also appears on the skin of the flexor surfaces of the limbs of the arms and legs, the inner thighs. It has the appearance of small papules of various shapes and pinkish-purple color with a shiny surface and a depression in the center.
Treatment includes diet with restriction of salt, smoked and fried foods, coarse food that irritates the mucous membranes. Glucocorticosteroids are prescribed as medical support.
Pityriasis rosea
Pityriasis rosea or Gibert's versicolor is a variant of a skin lesion whose cause has not been clearly identified. Exacerbations occur against the background of immune suppression - colds, hypothermia, chronic stress, etc. Most cases of this pathology are observed in people aged 20 to 40 years, as well as in adolescents.
Exacerbations occur against the background of immune suppression - colds, hypothermia, chronic stress, etc. Most cases of this pathology are observed in people aged 20 to 40 years, as well as in adolescents.
The disease begins with the formation of a primary scaly focus of pinkish or yellowish color from 1 to 10 cm in diameter with a clear rim. After 1-2 weeks, secondary plaques and smaller papules appear on the body and limbs - up to 2 cm (Fig. 7). Gradually, the elements of the rash turn pale, and the outer edge becomes rougher. The rash may be accompanied by itching, fever and other manifestations of the intoxication syndrome.
The disease tends to self-heal within 4-5 weeks. Treatment is mainly local in the form of ointments based on glucocorticosteroids, and antihistamines and NSAIDs are prescribed to combat itching and fever.
Figure 7. Skin rash with rosacea. Source: James Heilman, MD/Wikipedia
Atopic Dermatitis
Atopic dermatitis or eczema is a genetically determined inflammatory skin lesion of an autoimmune nature. Most often, children under 14 years of age living in large, industrial cities get sick.
Most often, children under 14 years of age living in large, industrial cities get sick.
Atopic dermatitis develops with a probability of 80% if both parents have a history of this pathology, and with a 50% probability if only one of them.
The first symptoms occur before the age of 2 years due to exposure to allergens, which can be food, plant pollen, dust and mold, cosmetics.
Typical symptoms are skin rashes, which vary depending on the stage of the disease. When exacerbated, red spots, papules and small vesicles appear, accompanied by severe itching. In infants, the typical site is the face, scalp, and neck. At an older age, the flexion surfaces of the limbs and the neck are affected. In the remission stage, they are replaced by foci of increased dryness of the skin, peeling and lichenification. During the year, on average, there are 2-4 exacerbations.
Ointments and creams based on glucocorticosteroids, calcineurin inhibitors, and zinc are used in the treatment. In severe cases, hormonal drugs are used in the form of tablets or intravenous injections. Antihistamines are also used to combat itching.
In severe cases, hormonal drugs are used in the form of tablets or intravenous injections. Antihistamines are also used to combat itching.
Infectious mononucleosis
Infectious mononucleosis is the result of infection with human herpesvirus type 4 (Epstein-Barr virus). It is believed that already before the age of 5, about 50% of children become infected with this virus, and its prevalence among adults reaches 95% of the population. Most often, clinical signs of pathology occur at the age of 14-18 years.
Typical symptoms of infectious mononucleosis include:
- General weakness and malaise.
- Sore throat and pain when swallowing
- Headache.
- Slight increase in body temperature.
- Sensation of aching in muscles and joints.
- Enlargement and soreness of the lymph nodes in the region of the lower jaw and neck.
Skin rash occurs in less than ¼ of patients. Most often, they occur on the 5th-10th day of the course of the disease against the background of the erroneously prescribed antibiotics ampicillin or amoxicillin.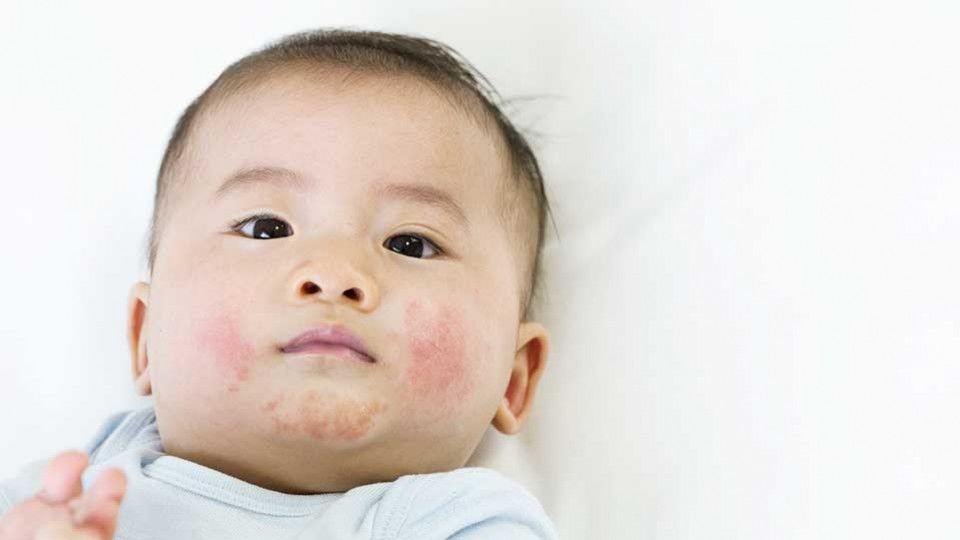 The rash is represented by spots and papules and is located in the face, trunk, thighs and shoulders. It is accompanied by swelling of the skin and itching, sometimes peeling. The rash disappears within 5-7 days.
The rash is represented by spots and papules and is located in the face, trunk, thighs and shoulders. It is accompanied by swelling of the skin and itching, sometimes peeling. The rash disappears within 5-7 days.
Since mononucleosis is of viral origin, antibiotic therapy is not used against it. Treatment of the disease involves the elimination of individual symptoms. In severe cases and with concomitant immunodeficiency, antiherpetic drugs are prescribed: ganciclovir, valaciclovir.
Prevention of rashes
In cases of infectious diseases, the only way to avoid rashes is to prevent infection, namely by limiting contact with sick people and practicing basic personal hygiene.
In case of allergic pathologies, it is important to exclude contact with triggers, and if this is not possible, take antihistamines or corticosteroids previously agreed with the attending physician in advance.
A series of recommendations to help avoid skin rashes of other origin for people with sensitive skin:
- Avoid direct skin contact with aggressive, irritating substances such as household chemicals.

- Limit skin exposure to sunlight, cold.
- Give preference to clothing and underwear made from natural fabrics.
- Avoid tight, uncomfortable clothing and mechanically rough objects such as washcloths.
- Use ointments or other skin care products recommended by a dermatologist or esthetician.
Conclusion
Skin rash is an important symptom of many diseases. She can tell you exactly what kind of disease you have to deal with. This, in turn, makes it possible to provide the right assistance before going to the doctor, avoiding mistakes or even coping with the problem on your own.
References
- Federal Clinical Guidelines. Dermatovenereology 2015. Skin diseases. Sexually transmitted infections. - 5th ed. revised and additional - M: Business Express, 2016. - 768 p.
- V.M. Kozin, Yu.V. Kozina, N.N. Yankovskaya "Dermatological diseases and sexually transmitted infections: Educational and methodological manual" - Vitebsk: VSMU, 2016.
 - 409 p.
- 409 p. - P.D. Walk. "Skin and venereal diseases: Textbook" - Grodno: Grodno State Medical University, 2003. - 182 p.
- Yu.V. Odinets, M.K. Biryukova “Atopic dermatitis, allergic rhinitis, urticaria in children: method. decree. for stud. and interns" - Kharkiv: KhNMU, 2015. - 52 p.
- S. A. Butriy “Child health: a modern approach. How to learn to cope with diseases and your own panic ”-“ Eksmo ”, 2018.
Rashes in infants | Rassvet Clinic
Babies are generous with various rashes. According to the "good" tradition, most of them are considered allergic with all the consequences - a strict diet for a nursing mother, transfer to artificial feeding, prescription of therapeutic mixtures, etc. In fact, true allergic rashes in infants are not so common. Allergic diseases affecting the skin in infants include: atopic dermatitis, acute urticaria and angioedema. Acute urticaria is extremely rare in infants - this is an acute allergic reaction in the form of peculiar rashes like blisters (as with a nettle burn, hence the name), which suddenly appear on the skin and just as suddenly disappear without leaving any trace, usually do not exist on the skin for longer than a day and are accompanied by severe itching, which manifests itself in the general anxiety of the child.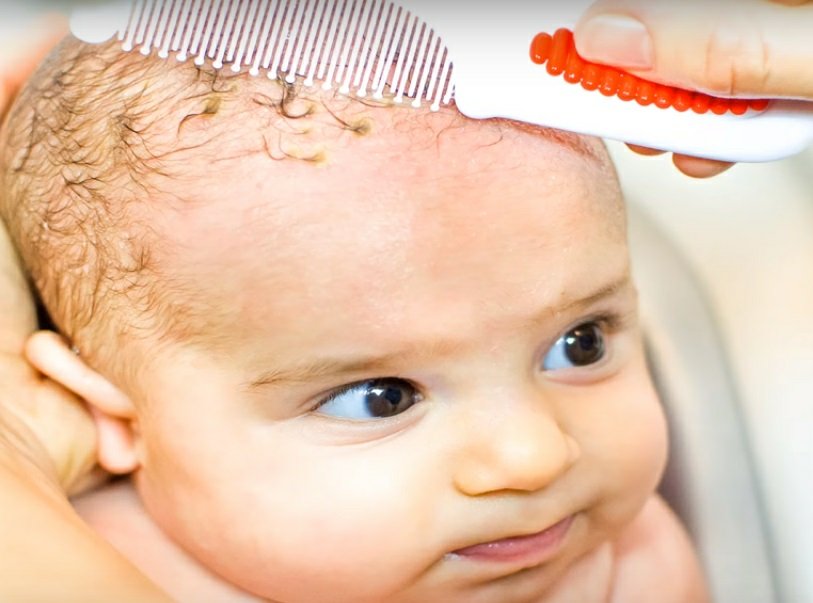 The most common causes are dietary proteins (such as cow's milk), viral infections, insect bites, and drugs (such as antibiotics). In severe cases, it may be accompanied by swelling and redness of the soft tissues of the face, neck, larynx, arms, legs, genitals or abdominal cavity - Quincke's edema, which requires immediate medical attention.
The most common causes are dietary proteins (such as cow's milk), viral infections, insect bites, and drugs (such as antibiotics). In severe cases, it may be accompanied by swelling and redness of the soft tissues of the face, neck, larynx, arms, legs, genitals or abdominal cavity - Quincke's edema, which requires immediate medical attention.
Let's look at what is most often undeservedly called an allergy:
Toxic erythema newborns - a transient benign rash, the exact cause of the appearance is unknown (possibly due to skin irritation by environmental factors).
Appears at birth or in the first 24-48 hours of life. Localization - face, trunk, limbs, except for the palms and soles. Disappears on its own within 5-7 days, sometimes 3 weeks. Does not require treatment.
Neonatal acne (acne infancy, neonatal pustulosis) is caused by androgen stimulation of the baby's sebaceous glands.
Peak rash falls on the 3rd week of life. It is localized more often on the face, sometimes spreads to the scalp, less often to the collar zone. They resolve spontaneously. The skin needs cleansing and moisturizing, in some cases, the application of
It is localized more often on the face, sometimes spreads to the scalp, less often to the collar zone. They resolve spontaneously. The skin needs cleansing and moisturizing, in some cases, the application of
treatment creams may be required.
Sweating rash , which occurs in poorly "ventilated" areas as a result of blockage of the sweat glands. May occur at any age.
Localization - skin folds, buttocks and back surface of the body, sometimes the face (after sleep). Depending on the depth of the lesion, it happens - crystal prickly heat, prickly heat, deep prickly heat (superficial).
The duration of the rash is from several hours to several days.
Treatment - cool water baths, air baths, prevention of overheating. Lotions containing calamine and creams with corticosteroids and antibiotics may be used to treat some cases of red and deep prickly heat.
Seborrheic dermatitis is a skin disorder that develops in areas rich in sebum.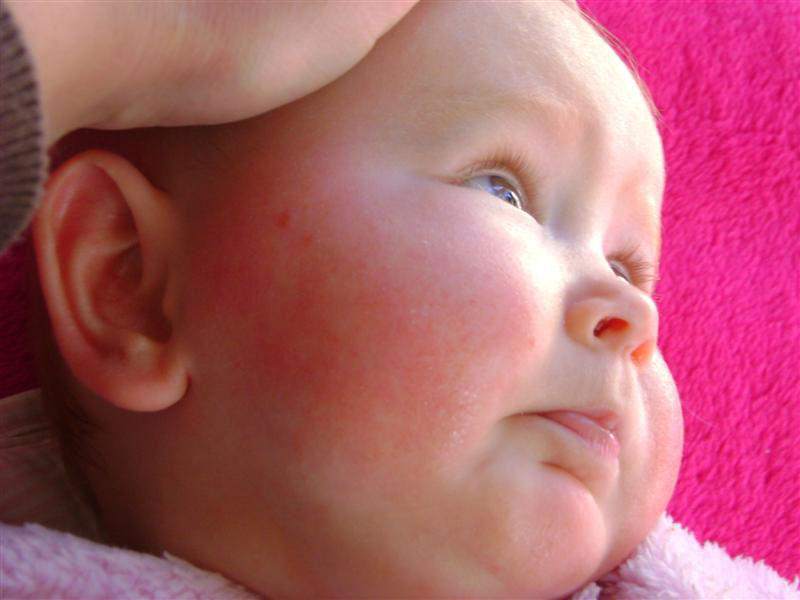 The exact cause is unknown (a certain role is assigned to the skin saprophyte - the Malassezia fungus, which grows well and multiplies in the sebaceous secretion).
The exact cause is unknown (a certain role is assigned to the skin saprophyte - the Malassezia fungus, which grows well and multiplies in the sebaceous secretion).
It can be foci or widespread, dermatitis with bran-like scales, which can form a crust (“cap”, gneiss) on the scalp.
Favorite localization - scalp, face, folds (!).
May begin at 1-2 weeks of age or later, resolve spontaneously within weeks or months.
Treatment consists of softening the crusts with oil or cream and then removing them, moisturizing the skin and, in some cases, applying antifungal and anti-inflammatory creams.
Simple contact dermatitis is a non-specific skin injury due to prolonged or repeated exposure to a variety of substances - saliva, fruit juices, foaming bath products, detergents (their residues on the walls of the bath), etc. In infants, saliva is often causes dermatitis in the area of contact with the nipple and in the folds of the neck.
As a rule, removal of the damaging agent and short-term use of anti-inflammatory creams leads to a quick recovery, but some children are so sensitive that it is almost impossible to identify the causative factor.
Diaper dermatitis (contact dermatitis prototype) is a skin lesion that occurs under the influence of physical (overheating), chemical, enzymatic (contact with sweat, urine and feces) and microbial factors. Localization - the area of the diaper or diaper fit.
Treatment is carried out using the abbreviation ABCDE (air, barrier, cleansing, diaper, education) - air, barrier, cleansing, diaper and parent education. Frequent diaper changes, washing the skin and drying it thoroughly help. Dermatitis is effectively prevented by the application to clean skin of products that completely cover it (Vaseline, zinc paste). In stubborn cases, medicated creams containing corticosteroids, antibiotics, or antifungals may be recommended.
And now a few words about AD:
Atopic dermatitis is a chronic allergic inflammation of the skin, genetically determined, associated with the loss of the skin barrier and, therefore, accompanied by dryness, itching and various rashes. In a third (!) of cases, it is combined with food allergies (the most common "culprits" are cow's milk, chicken eggs, wheat, fish, soy, nuts).
Starts more often not earlier than 3 months of life.
The most common localization up to 2-3 years is the face (cheeks, forehead, chin), convex parts of the limbs (extensor surfaces) and trunk, never in babies in folds (!).
Exacerbations are provoked by various factors - stress, dry air, sweat, food (histamine liberators), infections, contact with tobacco smoke, animal hair, coarse fabrics, detergent residues on clothing, etc.
Treated with careful skin care and using anti-inflammatory creams.
There are also:
Pseudo-allergic reactions are reactions that look similar to allergic reactions (for example, various rashes), but are not such, due to the non-immune mechanism of their development.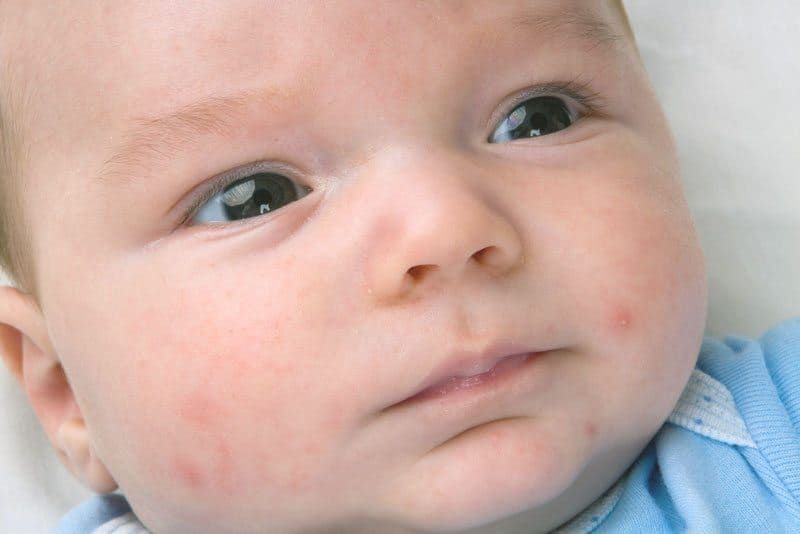
The reason is an increased content of histamine (tyramine, serotonin) in foods, or the ability of foods to increase the release of these substances in the body, or their increased absorption, due to the pathology of the gastrointestinal tract (fermentopathy, inflammation in the intestinal wall, etc.). ). Such products include chocolate, cocoa, strawberries, citrus fruits, honey, sauerkraut, marinades and spices, seafood, fish, caviar, pork, mushrooms, cheeses, nuts, smoked meats, preservatives, dyes and flavor enhancers.
Treatment includes dietary advice, skin care, and in some cases, antihistamines and anti-inflammatory creams.
Clinical manifestations of atopic dermatitis, simple contact dermatitis in highly sensitive children and the manifestation of pseudo-allergic reactions are very similar to each other, so the main task remains to create a "skin barrier" by constantly moisturizing the skin with the help of emollients, stopping exacerbation with anti-inflammatory creams and eliminating exacerbation-provoking factors .